Background
The international rural medical education movement has gathered strength over the last 20 years to become a broadly based coalition of interests that shares experiences and expertise in the delivery of medical education for rural practice. The strength of the movement lies in North America and Australia, where rural communities are recognised as having specific healthcare needs, and initiatives have been introduced to improve rural health status. It is also where much of the initiative has been found for doing things differently, including developing rural medical education, either through broad national approaches or through the development of medical schools that focus on rural health. However, in Europe the need for a different approach in rural health is less well recognised, and therefore rural medical education is less well developed. This article explores the relevance to Europe of developments elsewhere, aiming to translate and contextualise key messages into information that is relevant to Europe.
Common themes in rural health
At the heart of the rural health education agenda is that rural people have different healthcare needs and reduced access to services1. By most definitions, rural people live in smaller communities some distance from major population centres. The local economies are more dependent on primary production, such as farming and mining. These industries are often associated with substantial economic transition, due to globalisation of food production and mineral processing. Rural populations tend to have different disease profiles to those of urban populations; in Australia this includes higher rates of heart disease, mental health problems, accidents, suicide and several other major diseases2. Populations and workloads in rural tourist destinations can fluctuate with the temporary addition of visitors. The healthcare access behaviour of rural people, particularly males, is affected by cultural and social values, such that they tend to present with more advanced disease3. Many young rural people move to larger centres to improve education and employment options, leaving an ageing population. All of these factors contribute to a sense of isolation and difference in rural communities.
Rural health professionals face additional isolation issues. Isolation from professional support requires a broader scope of practice, more training and stronger support networks4. Their partners face reduced local education and employment opportunities. If they are not from the local community, they may also be isolated from family and friends; it may take years to become accepted as 'part' of rural communities. The combination of different practice, training and support requirements has resulted in problems with both recruitment and retention of rural health professionals5,6. The rural health and education themes that are shared by many countries are listed (Fig 1).

Figure 1: Common international themes in rural medical education
Developments in North America and Australia
These are nations that combine longstanding Indigenous cultures with more recent European immigrant populations, secondary and tertiary industry, and European-style political concepts and structures. There are population groups, often comprising Indigenous peoples, that have markedly worse health status than other citizens. Distances can be vast and population density low, in comparison with Europe, from which the basics of healthcare systems may have been imported. In the more successful and wealthier of these new nations, rural communities expect equal access to healthcare services compared with urban communities. The health status of their rural populations appears to be better than in developing nations, but still worse than that of their own urban populations.
Much of the success in North America and Australia has come from two features that are less obvious elsewhere. The first is that there is an expanding research evidence base that supports the development of policy change and initiatives to address identified problems. The second is that there are well organised groups that have found the ear of government and achieved policy changes that resulted in funded initiatives to address shared concerns. As an example, in Australia there is both a strong coalition of rural interests in the National Rural Health Alliance and strong rural doctor associations7,8. Largely due to their effort, there has been a wide range of incentives for students and professionals to work in rural communities9, and the establishment of rural professional organisations and rural-oriented medical schools10,11.
The situation in Europe
Although European countries illustrate similar rural health education themes, there is considerable diversity amongst them in the degree to which rural health is considered as important. The UK represents one extreme in the spectrum, as a relatively compact and wealthy nation that provides comprehensive health care to its citizens. Distances are usually small and poor access to health care is often regarded as being due to factors other than distance and rurality. Whereas rural populations in North America and Australia have higher rates of almost every health problem and worse healthcare outcomes than urban people, health research in England suggests that rural people have slightly better mental health and no significant difference in overall mortality from ischemic heart disease (except in remote communities), renal dialysis or breast cancer12-15. In Scotland, rural people are happier than urban people with their health care services, despite having high expectations of a quality service16. While some research has produced different results17, the only major health statistics in common with the rural Australia are an increase in road traffic accident mortality and suicide among rural males18,19. Rural residence is frequently regarded as being synonymous with healthier and wealthier lifestyles.
However, in almost all UK research about rural-urban health inequalities, comment is made about a confounding variable that appears to dominate any data analysis: deprivation. In the UK, deprivation is seen as predominantly an inner urban phenomenon, as poor, unhealthy people congregate in communities that have endured post-industrial collapse. These people live closer to health services, and so have no genuine geographical access problems, but have higher rates of most indicators of disadvantage than people in outer urban and surrounding rural communities17. Hence the unit of measurement in rural-urban research may be misleading.
Elsewhere in Europe the situation is more mixed. The more established and wealthier nations appear to be more like England, although Norway and Scotland have genuine remoteness based on distance and climatic conditions. In some of the 'newer' European Economic Association (EEA) nations, national economies are less robust and rural areas are the main focus of deprivation. The word 'rural' is sometimes even regarded as a denigrating term, associated with poverty and peasantry.
However no European nation, except perhaps Norway, appears to recognise rural health workforce education as a priority. Many medical schools do not have academic primary care or general practice departments or academic staff, and relatively few require clinical placements in rural communities, although these are increasing in frequency and popularity with students (verbal comment, anonymous, EURIPA section, WONCA Europe Conference 2006).
Issues to be resolved
Many European rural doctors are frustrated by the lack of progress made in furthering the rural health education agenda. However, in comparison with North America and Australia, there are some key differences, and these need to be explored as part of making progress. Developing and collating an evidence base is important if a strong argument is to be made for change. The issues that require resolution are listed (Fig 2).

Figure 2: Issues to be resolved to further European agenda
Defining rural, regional and remote
Agreeing on a definition of 'rural' is difficult within a single country, let alone across a collection of countries. A key problem is that rurality is probably defined more by how larger cities are described than on firm criteria. The rational approach relies on categorisation of data, often collected for other purposes, such as local government boundaries, population numbers and density, distance from services, and industrial activity. However, these data are used and combined differently, so there is no easy way of comparing measures of rurality across Europe.
The second approach relies on the perception of individuals and communities: do they identify as being rural? In an increasingly urban world, much of the way we see communities relates to relative position from large cities into which essential services are centralised. In several European countries there is a large, central city, containing the centre of government, politics, finance, commerce, major educational institutions and major health care facilities. Transport systems are designed to move people rapidly between the dominant cities and outer centres. Modern high-speed mass transit systems bring communities up to 160 km within commuting distance; twice the Australian rural health access benchmark of 1 hour travel time (80 km) from services4. For these commuters, access to services during work time is the same as for urban people. They are in their home communities only overnight, and have little connection with the local people and services.
This urbanisation of rural communities leads to the perception that rural residents are no different from urban people. But this is almost certainly not correct. Not all rural people are commuters. There remain substantial populations of young and old people, local business people and farmers who are in rural communities all day. Even the commuters are there when not at work. What is clear is that the old notions of rural and urban are no longer uniformly relevant. There is an urgent need for a clear, current and measurable set of European definitions to facilitate more rational, informed and perhaps persuasive debate with professional groups and politicians.
Further, the definition of rural medical practice needs to be reconsidered. In Australia it does not include only primary care and general practice20. Narrower specialists in regional centres may face similar issues of professional isolation from colleagues in major centres. Taking a more inclusive approach would increase the support for rural-regional medical education, which can be about developing an entire workforce for regional areas. The situation in Europe may be similar.
Deprivation
In much of Europe, deprivation is regarded as an inner city issue. However, deprivation knows no geographical boundaries, and should be tackled everywhere. There is also substantial rural deprivation, even if it is sometimes less obvious17,21. The recent immigration of substantial populations of political and economic refugees from Asia and Africa has introduced new, isolated and often unwell population groups into many rural communities. The most useful strategy would be to work with researchers and policy makers to see that the powerful deprivation debate includes urban and rural communities.
Impact of a changing workforce context
The medical workforce is becoming part of a global health economy, with an international shortage of medical graduates and increased movement across national boundaries for education, economic and political reasons. Despite agreements about the ethical position22, the net migration appears to be in favour of wealthier nations. Further, the barriers posed by EEA regulations to external medical immigration may be increasing the movement of doctors from Eastern to Western Europe. Expanding medical education may simply provide more emigrant doctors, but also has the potential to preferentially select and retain local graduates through rural medical education. The latter is a more persuasive political argument.
Evidence of successful educational strategies
Successful rural medical education elsewhere has been built with the assistance of a research evidence base that indicates the educational and workforce benefits of expanding rural medical education. There is evidence, at least in North America, Australia and Japan23-26, to support: preferential selection of rural background students; providing positive rural placements; facilitating student connection with rural communities; and providing students with successful rural professional role models. New rural-oriented medical schools have been established11,27,28, combining several layers of strategies to develop a clear, coherent and evidence-based approach to rural medical education that attempts to maximise the effect of the initiatives. However, apart from the pioneering work in northern Norway29, there is little evidence of success of any such strategies in Europe.
The characteristics of successful rural medical education are listed (Fig 3)30. These should to be applied such that all strategies reflect immersion in community partnership and the mission of the school, as depicted (Fig 4). The whole package may currently be beyond the short-term reach of European rural health movement, but it may be unnecessary to establish stand-alone rural medical schools. If more mainstream medical schools could be encouraged to expand rural medical education, then there will be benefits. As examples, the WWAMI program in north-western USA shows how a traditional urban medical school can be a world leader at rural medical education31. Further, the Australian strategy of making all medical schools introduce rural medical education appears to be having a positive effect, although it is too early for longer-term outcome data. The driver for European rural medical education development may be the expansion of medical education, as urban health facilities are struggling to cope with increased student numbers. This is an opportunity for rural medicine to offer clinical teaching capacity in return for greater curriculum involvement.
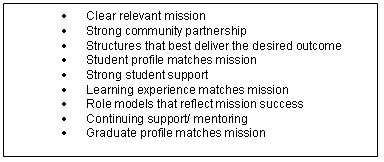
Figure 3: Characteristics of successful regional/rural medical education30.
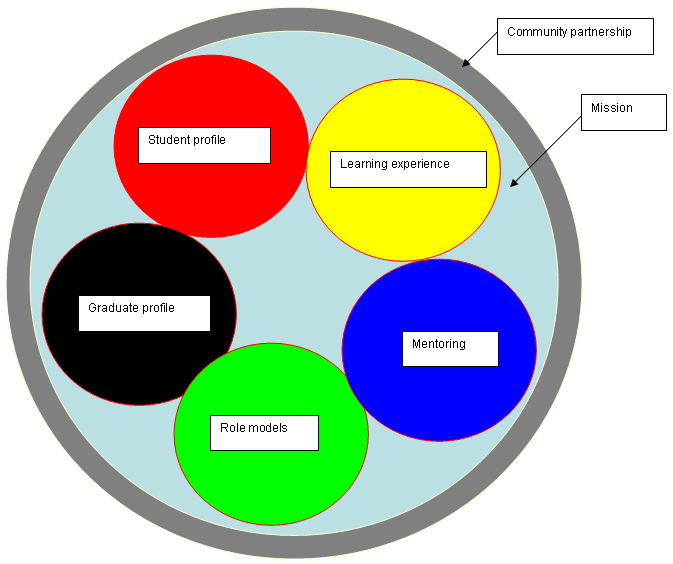
Figure 4: Congruence between strategies.
Rural professional and community leadership
At this stage there does not seem to be the broad coalition of professional, community and political interests found in Australia and North America. The rural medicine movement is primary-care based and regarded as a small part of much larger professional organisations. Primary care organisations in some European countries have rural practice interest groups, and EURIPA is the most active pan-Europe rural practice advocacy group32. However, it is unclear just how influential these organisations are within either the profession or the broader community. Enhancing this influence is not easy, but may follow more easily if there are clearer definitions and an evidence base.
Conclusion
The impetus for rural-regional medical education development, and much of the success, has taken place outside of Europe, based on a combination of evidence about rural health status, evidence supporting educational intervention, strong rural professional and community leadership, and governments that have listened to the resulting powerful argument. There is a clear case for the development of academic rural medicine within Europe, to act as a vehicle for the intellectual debates about definitions and roles, and for gathering the educational research necessary evidence to support initiatives that can make a difference to health care and workforce problems. As happened elsewhere, the best strategy may be to start with carefully designed initiatives in several European nations, gradually gathering momentum based on evidence and success.
Acknowledgement
This article is based on a keynote presentation to the EURIPA section of the WONCA Europe 2006 Conference, Florence, August 2006.
References
1. Veitch PC, Sheehan MC, Holmes JH, Doolan T, Wallace DA. Barriers to the use of urban medical services by rural and remote area households. Australian Journal of Rural Health 1996; 4: 104-110.
2. Strong K, Trickett P, Titulear I, Bhatia K. Health in rural and remote Australia - The first report on the Australian Institute of Health and Welfare on rural health. Cat no PHE 6. Canberra: AIHW, 1998; vi-vii.
3. Strasser R. Rural health around the world: challenges and solutions. Family Practice 2003; 20: 457-463.
4. Hays RB, M Craig, Wise A, Adkins P, Mahoney P, Sheehan M et al. A sampling framework for rural general practice. Australian Journal of Public Health 1994; 18: 273-276.
5. Whitcomb ME, Myers WW. Physician manpower for rural America: summary of a WAMI region conference. Academic Medicine 1990; 65: 729-732.
6. Committee of Inquiry into Medical Workforce and Medical Education into the 21st Century. Australian Medical Education and Workforce into the 21st Century. Canberra: AGPS, 1988.
7. National Rural Health Alliance. (Online) http://www.ruralhealth.org.au (Accessed December 2006).
8. Rural Doctors Association of Australia. Rural Doctors Association of Australia home page. Available: http://www.rdaa.com.au (Accessed 1 December 2006).
9. Holub L, Williams B. The general practice rural incentives program, development and implementation: Progress to date. Australian Journal of Rural Health 1996; 4: 117-127.
10. Australian College of Rural and Remote Medicine. Australian College of Rural and Remote Medicine home page. Available: www.acrrm.org.au (Accessed 1 December 2006).
11. Hays RB. Rural Initiatives at the JCU School of Medicine. Australian Journal of Rural Health 2001; 9: S2-S5.
12. Levin KA, Leyland AH. Urban-rural inequalities in ischemic heart disease in Scotland, 1981-1999. American Journal of Public Health 2006; 96: 145-151.
13. Weich S, Twigg L, Lewis G. Rural/non-rural differences in rates of common mental disorders in Britain: prospective multilevel cohort study. British Journal of Psychiatry 2006; 188: 51-57.
14. O'Riordan E, Lambe D, O'Donoghue DJ, New J, Foley RN. Variation in dialysis patient mortality by health authority. QJM 2003; 96: 739-745.
15. Maheswaran R, Pearson T Jordan H, Black D. Socioeconomic deprivation, travel distance, location of service and uptake of breast cancer screening in North Derbyshire. UK. Journal of Epidemiology and Community Health 2006; 60: 208-212.
16. Farmer J, Hinds K Richards H, Godden D. Urban vs rural populations' views of health care in Scotland. Journal of Health Services Research and Policy 2005; 4: 212-219.
17. Baird G and Wright N. Poor access to care: rural health deprivation? British Journal of General Practice 2006; 56: 567-568.
18. Levin KA, Leyland AH. Urban/rural inequalities in suicide in Scotland, 1981-1999. Social Sciences and Medicine 2006; 60: 1877-1890.
19. Hewson P. Deprived children or deprived neighbourhoods? A public health approach to the investigation of links between deprivation and injury risk with specific reference to child road safety in Devon County, UK. BMC Public Health 2004; 4: 15.
20. Smith JD, Hays RB. Is rural medical practice a separate discipline? Australian Journal of Rural Health 2004; 12: 67-72.
21. Jordan H, Roderick P, Martin D. The Index of Multiple Deprivation 2000 and accessibility effects on Health. Journal of Epidemiology and Community Health 2004; 58: 802.
22. WONCA. Melbourne Manifesto. Available: http://www.globalfamilydoctor.com/aboutWonca/working_groups/rural_training/melbourne_manifesto.htm (Accessed 1 December 2006).
23. Pathman DE, Konrad TR, Ricketts TC. The comparative retention of National Health Service Corps and other rural physicians. JAMA 1992; 268: 1552-1558.
24. Rabinowitz HK. Recruitment, retention and follow-up of graduates to a program to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1993; 328: 934-939.
25. Veitch C, Underhill A, Hays RB. The career aspirations and location intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation. Rural and Remote Health 6: 537. (Online) 2006. Available: http://rrh.org.au (Accessed 30 January 2007).
26. Matsumoto M, Okayama M, Inoue K and Kajii E. Factors associated with rural doctor's intention to continue a rural career: a survey of 3072 doctors in Japan. Australian Journal of Rural Health 2005; 13: 219-225.
27. Northern Ontario Medical School. Northern Ontario Medical School home page. Available: www.normed.ca (Accessed 1 December 2006).
28. Tesson G, Strasser R, Pong RW, Curran V. Advances in rural medical education in 3 countries: Canada The United States and Australia. Rural and Remote Health 5: 397. (Online) 2005. Available: http://rrh.org.au (Accessed 30 January 2007).
29. Magnus JH, Tollan A. Rural doctor recruitment: Does medical education in a rural area recruit doctors to rural areas? Medical Education 1993; 27: 250-253.
30. Hays RB. Guiding principles for the successful innovation in regional medical education. Rural and Remote Health 6: 516. (Online) 2006. Available: http://rrh.org.au (Accessed 30 January 2007).
31. Norris TE, Coombs JB, House P, Moore S, Weinrich MD, Ramsey PG. Regional solutions to the physician shortage: the WWAMI experience. Academic Medicine 2006; 81: 857-862.
32. EURIPA. About EURIPA. Available: http://www.euripa.org/about.htm (Accessed 1 December 2006).
Abstract
The drive to increase recognition of the different health care needs of rural communities has been more successful in North America and Australia than in Europe. This success has translated into political support for a range of education, workforce and service model initiatives that appear to be effective in providing a better prepared and supported healthcare workforce in rural communities, providing services through specifically developed delivery models, all with the aim of improving the quality of health care for rural people. The reasons for the differences between Europe and nations with greater success appear to relate to: the absence of a clear, shared definition of rurality across a very diverse group of nations within Europe, and a weaker coalition of interests advocating rural health issues. As a result, although very similar rural health issues are present in Europe, governments are not particularly supportive of initiatives aimed specifically at rural health and so rural medical education is much less well developed. This article explores how the rural health movement in Europe might build on success elsewhere to develop and successfully promote localy relevant models of rural medical education.
Key words: Europe, quality, rurality.
You might also be interested in:
2010 - Building capacity for acute care in developing countries

