Introduction
Only 23% of doctors in Australia practice in rural areas and the number of doctors in significant shortage areas, per head of population, is only 54-65% of that in metropolitan Australia1-3. It is well known that medical graduates with rural backgrounds are more likely to practise in rural communities4, but unless all rural students choose rural medicine, we must recruit metropolitan students to rural practice as well. Most western medical schools offer clinical rural 'electives,' and some offer extended clinical rural placements to select groups of students. Such rural exposure at both the undergraduate and postgraduate level increases interest in rural health careers5, and experience shows that understanding rural health practice in the context of rural placements for medical students is important6. However, participants who elect rural coursework may be biased and thus studies based on elective experiences have intrinsic limitations.
In 2003, the Melbourne University Department of Rural Health (UDRH) developed the 'Rural Health Module' (RHM) as a required course for all University of Melbourne medical students, as part of Australian Commonwealth program initiatives to address rural doctor shortages in Australia7,8. This logistically ambitious program aimed to expose all medical students at a metropolitan-based medical school to a substantial rural health experiential course, embedded in a contextual framework based on five key concepts: (i) social determinants of health: (ii) confidentiality; (iii) access; (iv) cultural safety; and (v) team practice9. Additionally, because of the shortage of rural GPs and specialists, it also attempted to engage students in community rural health and Indigenous health activities without requiring significant GP teaching time.
The purpose of this article was to report student feedback on their experience of the RHM and their attitudes about undertaking rural practice in the future.
Course structure
Each four week rotation begins at the School of Rural Health (SRH), based in Shepparton, North East Victoria, which is ethnically diverse with large Indigenous and refugee populations. Two days of lectures and discussions, focussing on the five key themes precede the start of community placements. Students also attended a 1 day workshop on Indigenous cultural safety issues during the course. Pairs of students attend a short-term community placement (3 days), an Indigenous placement (3 days) and a small rural community placement (2 weeks). Indigenous placements were developed using a community consultation model developed by the school and Indigenous community in partnership10,11. The SRH Senior Indigenous Liaison officer organised the Indigenous placements. Shortterm placements in Shepparton included health service agencies such as district nursing, community health services, aged care assessment teams (n = 12). Examples of Indigenous community agencies included Aboriginal-controlled health services and child/aged care services (n = 10). Twenty-four rural towns and health services in Victoria and New South Wales volunteered to accept students. Time with GPs was limited due to the shortage of GP practices able to take students. Supervisors for community placements were recruited by the SRH team; most were health professionals (not doctors) identified by the participating agencies.
Course assessment included: (i) an oral presentation on the students' experiences, framed as an analysis of rural/urban differentials of the five key concepts; and (ii) a written examination paper.
Methods
Overall, 393 students participated in the RHM during the initial period: 132 students in 2003 (three rotations) and 261 students in 2004 (six rotations). Students completed an optional evaluation, developed by the course committee, at the end of the RHM (Appendix I). The evaluation asked for feedback on placements and RHM educational activities, and the effect of the experience on students' attitudes toward rural training or practice. To maintain confidentiality, no personal information was collected, and all data were grouped before analysis. The evaluation team (authors/researchers) had no access to rotation schedules or identifying data. Approval was obtained from the University of Melbourne Human Research Ethics Committee.
Data analysis
Five point ordinal (Likert) scale responses were analysed using SPSS v 11.0.1 and 12.0 (SPSS Inc, Chicago, IL, USA). Discrete variables and means of different groups were compared using χ2 tests and t-tests, respectively. Statistical significance was set at 5% and all tests were two-tailed. Qualitative analysis of open-ended questions used standard qualitative methods12, with common response themes identified and coded independently by two researchers. Final coding was based on review of discrepancies and common agreement.
Results
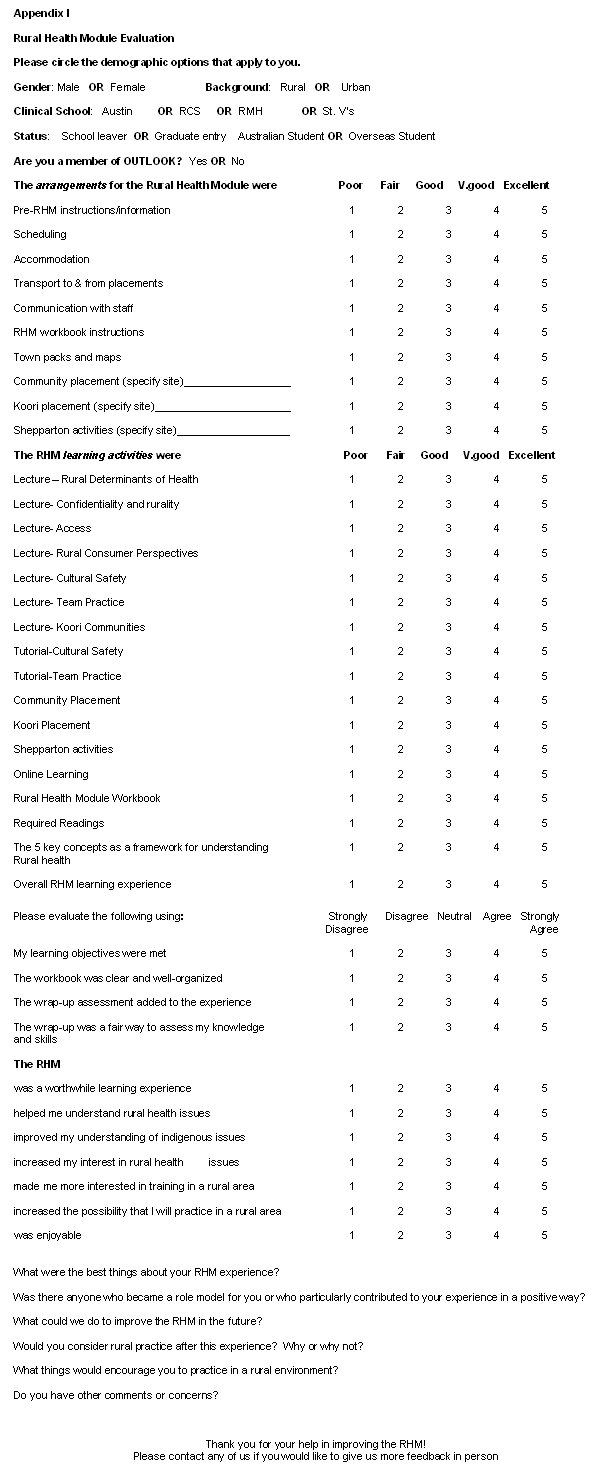
The RHM evaluation was completed by 368 students (93%) of 393 RHM participants. Some respondents did not answer all questions. Thus, analysis was done on the basis of a varied n (range: 122 to 368). Since no significant demographic differences were found amongst the nine rotations of students (Table 1), the data from all rotations were combined. Of all participants, 57% were female, and most (86%) had come from urban backgrounds. The majority (79%) were school leavers; 63% were Australian students; and 21% reported belonging to the student 'OUTLOOK' rural health club. (OUTLOOK is a multidisciplinary student organisation committed to raising awareness of the health needs of under-resourced communities. Such communities include rural and Iindigenous Australia and developing countries. Members of OUTLOOK represent all health disciplines taught at The University of Melbourne, including physiotherapy, dentistry, nursing and medicine).
Table 1: Demographics of Medical Students Participating in the Rural Health Module.
Educational Activities
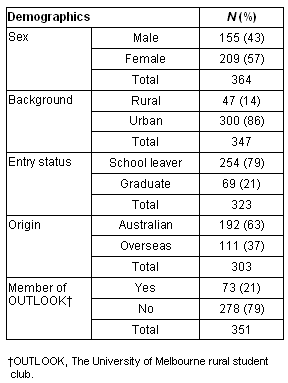
Students rated the lectures and tutorials introducing the five key concepts (Table 2) from 'fair' (2) to 'very good' (4), with a mean of 2.96. The majority of participants rated their placements as 'good' or better, with a mean of 2.93. Seventy-five percent of students rated their rural community placement 'good' to 'excellent', and 59% rated their Indigenous placements similarly. Sixty-nine percent of students reported a 'good' to 'excellent' understanding of the five key concepts. However, only 35% percent of students agreed that their learning objectives were met 'well' or 'very well' (4-5 on a 5-point scale).
Table 2: Student Perceptions of the Rural Health Module
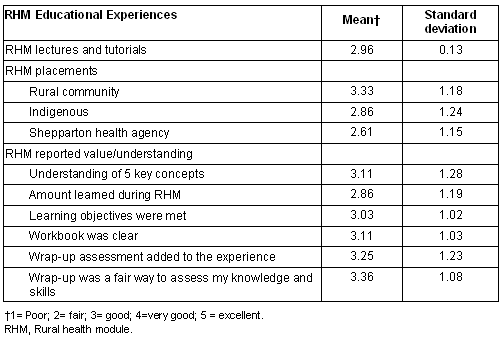
The RHM learning experience (Table 3) was rated with a 5 point Likert scale. Students reported that the RHM helped them understand rural health issues 'well' and that it increased (their) interest in rural health issues; 60% rated this in the top two categories (4 or 5). Fifty-three percent of students rated their learning experience as worthwhile (4-5); 49% identified that they would be interested in training in a rural area. Importantly, only 12% of students said that the RHM did not increase their interest in rural practice 'at all' (1); 40% reported that the RHM increased the possibility that they would practice in a rural area 'a little bit' or 'somewhat' (2 or 3) and 48% agreed that it increased the possibility that they would practice rurally (4 or 5).
Table 3: Students Attitudes about the RHM and Rural Health

Qualitative results
Open-ended questions addressed topics such as: how to improve the RHM; how the experience affected their consideration of rural practice; and what factors that would encourage them to practice in a rural environment. Respondents made multiple comments. Fifteen themes were identified from 553 comments (n = 342) identifying the 'best things' about the RHM. Welcoming/community experiences and community integration (37%), community placements (33%); and first hand experience of rural practice (20%); Indigenous placements (18%), rural life (12%), and understanding rural health (10%) were identified most frequently.
Positive role models were listed by 285 respondents (340 comments). Twenty-nine percent (n = 107) of students identified a rural GP or doctor as someone who enhanced their experience and served as a positive role model. Other health care workers (15%), community nurses (10%), hospital managers/staff (5%), local elderly (4%) and school of rural health staff (4%), were also listed as positive role models. Specific suggestions were made (n = 328 respondents; 559 comments) about improving the RHM. Importantly, many students (35%) wanted more contact with doctors, for example GP activities (n = 115). Given the workforce shortage issues relating to Indigenous health, it is notable that 26 students requested more time with Indigenous communities. Comments included: 'more Koori and small town, less regional centre placements'; and 'lengthen the period in the Koori community.'
The question, 'Would you consider rural practice after this experience? Why or why not?' generated 397 responses from 284 respondents: 49 participants (13%) said they had always considered rural practice, while 93 respondents (25%) said that they would consider rural practice for a short period of time, and another 49 (13%) would consider rural practice in the future. Students' reasons for considering rural practice included: rural lifestyle/small community (8%), to improve/contribute to rural/community health (7%), the breadth of rural practice (5%) and wanting to be near family and friends (3%). Only 7% of students who made comments stated that the RHM had not changed their thoughts about pursuing rural practice. Reasons cited for not considering rural practice in the future included: the slow pace of life; fewer specialist training opportunities; perceived pressure from the community to perform; lack of employment opportunities for spouse; and that the rural community was not welcoming. One student identified the 'lack of infrastructure e.g. swimming pool, gym, movies' in the small town and that 'the community was not welcoming of newcomers - I spoke to a counsellor who had come from Melbourne and she said it took a long time to make new friends'. Another student commented that 'the lifestyle just does not suit me' and a student identified the experience as 'overwhelming' when explaining why she would not consider rural practice. Of the 47 students from a rural background undertaking the RHM, 8% identified that they had enjoyed the rotation.
When asked, 'What things would encourage you to practice in a rural environment?' 282 participants made 448 comments. Of 35 identified themes, the most important were: community support, social opportunities and a friendly environment (20%); financial incentives and compensation (11%); rural lifestyle (11%); collegial/professional support (10%); diversity of experiences/careers (9%); professional development and training opportunities (9%); and the presence of family and friends (6%).
Discussion
Student responses in this study showed that a required 4 week rural experiential health course, with a theoretical framework, increased students' self-reported understanding of rural health. Almost half of respondents (47%) indicated that the course increased their interest in rural practice, and over half of the students (51%) indicated that they plan to practise rurally, would consider it for a short time or seriously consider it in the future. These findings are remarkable because all participants are from a metropolitan university that has historically emphasized research, and most students taking this required course identified as having urban backgrounds (86%). Only one previous study has examined the quantitative effects of a required rural undergraduate 'clerkship' (clinical rotation)13. Their first two cohorts were 'unhappy' that the course was required (anecdotally, many students in our cohort felt similarly) and the authors did not show an increased preference toward rural practice in the first 2 years (9.1% vs 11.8% reporting a rural preference prior to the course, vs national preferences of 15.3%)13. Thus, our findings of 13% saying they had always considered rural practice with another 38% saying they would practise rurally for a short time or consider it strongly in the future, after the RHM, are encouraging compared with the only published standard available. The same study states that students required to do a rural course were more likely to rate their experience in 'public health and community medicine' as 'excessive'13. Since RHM placements are largely community based, rather than clinically based, one might expect significantly less enthusiasm from our students who do the RHM during their clinical years.
Our data regarding students' suggestions about what would encourage them to want to practise rurally are consistent with those from other studies5,14,15. Students' comments highlight the importance of rural- and GP-associated clinical experiences, as well as the need for positive role models and welcoming communities.
As Australian medical student numbers increase, rural health placements, especially in general practice (and Indigenous health placements), will become an increasingly scarce resource. Due to concern about the stress the RHM student load might place on GPs, the RHM originally used only community health agency placements. Despite limited access to doctors, 29% of RHM students identified a rural doctor as a positive role model. Since the inception of the course, increases in the Practice Incentive Payment (PIP) have enabled GPs to offset the costs of teaching more appropriately, and they are now more willing to have students in their practices. Lack of infrastructure (rooms for teaching and consultation) in rural practices is a major barrier to further implementation of such a course for large numbers of students.
The strengths of this study include a high response rate. The limitations include single-institution data that may not be representative. However, a report from another metro-based university in Australia notes that students 'valued the experiences and the insights into rural practice issues obtained through the [rural] attachments'5 with the major differences being the required nature and non-doctor oriented nature of our program. Self-reported data were collected only at the end of the course, and thus despite asking students whether their attitudes had been changed by the module, their responses theoretically reflect only single point attitudes, which may not represent the effect of the course or lead to more students truly considering or choosing rural practice.
In response to student feedback, the course is being modified to become: (i) more clinically focussed; (ii) community- or research-project oriented; and (iii) the course has recently begun to require cultural safety workshops for all students (anecdotally reported as one of the best things about the course).
Conclusion
Requiring all medical students at a major metropolitan medical school to complete a community-based rural health course can improve their reported interest in rural health, and in rural training and practice. However, significant barriers to sustaining such a course exist, including lack of rural clinical placements and concern remains about placement fatigue for both GPs and Indigenous communities. The course was expensive and logistically difficult to implement and, thus, may not be the best way to increase numbers of students choosing rural practice. Further research is needed to investigate whether the investment of time and effort into a required course, including students who do not elect or want a rural health experience, is justified. This must be compared with outcomes from more accepted strategies, such as recruiting students from rural origins into medicine or providing clinical electives for students interested in rural health.
References
1. Morey S. Workforce Committee of the Royal College of Physicians. Sydney: Royal College of Physicians, 2005.
2. Rural Workforce Agency Victoria. Proceedings, Rural Workforce Agency Victoria Statewide Forum. 27 August 2003; Melbourne; 2003.
3. Australian Government, Department of Health and Ageing. General Practice in Australia 2004. Australian Government, Department of Health and Ageing, 2005.
4. Han GS, Mahnken J, Belcher S. More rural and Aboriginal students for health related university courses - are we making progress? Australian Health Review 2003; 26: 73-77.
5. McAllister L, McEwen E, Williams V, Frost N. Rural attachments for students in the health professions: are they worthwhile? Australian Journal of Rural Health 1998; 6: 194-201.
6. Sturmberg JP, Reid A, Khadra MH. Community based medical education in a rural area: a new direction in undergraduate training. Australian Journal of Rural Health 2001; 9(Suppl 1): S14-18.
7. Cameron I. Retaining a medical workforce in rural Australia. Medical Journal of Australia 1998; 169: 293-294.
8. Wakerman J, Humphreys JS. Rural health: why it matters. Medical Journal of Australia 2002; 176: 457-458.
9. Bourke L, Sheridan C, Russell U, Jones G, DeWitt D, Liaw ST. Developing a conceptual understanding of rural health practice. Australian Journal of Rural Health 2004; 12: 181-186.
10. Henderson R, Simmons DS, Bourke L, Muir J. Development of guidelines for non-indigenous people undertaking research among the indigenous population of north-east Victoria. Medical Journal of Australia 2002; 176: 482-485.
11. Liaw ST, McGrath B, Jones G, Russell U, Bourke L, Hsu-Hage B. A compulsory experiential and inter-professional rural health subject for undergraduate students. Rural Remote Health 5: 460. (Online) 2005. Available: www.rrh.org.au (Accessed 1 June 2007).
12. Weinberg D. Qualitative research methods. Malden, MA: Blackwell, 2001.
13. Jones AR, Oster RA, Pederson LL, Davis MK, Blumenthal DS. Influence of a rural primary care clerkship on medical students' intentions to practice in a rural community. Journal of Rural Health 2000; 16: 155-161.
14. Jensen CC, DeWitt DE. The reported value of rural internal medicine residency electives and factors that influence rural career choice. Journal of Rural Health 2002; 18: 25-30.
15. DeWitt DE, Migeon M, LeBlond R, Carline JD, Francis L, Irby DM. Insights from outstanding rural internal medicine residency rotations at the University of Washington. Academic Medicine 2001; 76: 273-281.
_________________________________