Introduction
Most doctors believe they have a major role to play in promoting breastfeeding1-3 and consider worthwhile taking time to assist women to continue to breastfeed4. However, several studies have identified significant breastfeeding knowledge deficits among doctors1,5,6, and a lack of formal breastfeeding education at both the medical school and post-graduate level.3,7,8
Personal breastfeeding experience (either of themselves or their spouse) has been identified in some studies as an important source of breastfeeding information and practical experience for health professionals3,9. Additionally, health professionals with personal breastfeeding experience (often defined as breastfeeding for at least 2 weeks) are more likely to: perform better on breastfeeding knowledge surveys1,10,11; actively promote breastfeeding; and be more confident when assisting breastfeeding women1. Gender also appears to have an effect, with doctors who had breastfed their own infants being more confident than male doctors whose spouses had breastfed12. However, there are inconsistent results when comparing overall confidence of male and female doctors. Some studies suggest there is no difference between genders1,5 while others indicate that female doctors are likely to be more confident than their male counterparts12,13.
While it appears that a doctor's perceived breastfeeding attitudes and confidence are affected by both their gender and personal experience, there has been no previous qualitative research investigating these issues, nor has there been research carried out in an Australian setting. Additionally, the views of doctors working in rural and regional areas are of particular interest. Findings from previous studies conducted in the USA and Australia suggest that breastfeeding rates for women who live in rural and remote areas are lower than those for mothers living in urban areas14-16. Data from a recent study in Southern Queensland indicated that women living in rural and remote areas rather than a provincial city were: less likely to obtain breastfeeding information prior to or during pregnancy; more than twice as likely to think that 'formula is as good as breastmilk'; and more likely to introduce solids to their infant before 3 months of age17. Breastfeeding support services, such as lactation consultants and breastfeeding support groups, were significantly less available for women living in rural and remote areas, with doctors, child health nurses and pharmacy staff being the most commonly available resources. At both 3 and 6 months, mothers were more likely to have seen their doctor than any other breastfeeding support person or group17. Consequently, doctors in rural and regional areas may be expected to provide a greater degree of assistance and support for breastfeeding women than their counterparts in metropolitan areas.
This article reports some of the results of a qualitative descriptive study18 of eight GP registrars living in rural and regional areas in southern Queensland, Australia. An interview was conducted with each registrar and information obtained included the participants' perceptions of the effect their gender and personal breastfeeding experience had on their ability to assist breastfeeding women. This forms part of a larger mixed method study19 investigating the breastfeeding knowledge and skills of Australian GP registrars. Qualitative data collected from these interviews will inform the development of a questionnaire designed to ascertain the registrars' perceived breastfeeding attitudes and knowledge. Results from the qualitative and quantitative arms will be used to develop a tailored breastfeeding educational resource.
Method
Participants
Eight GP registrars practising within 250 km of Toowoomba, Queensland, Australia were purposively recruited to participate in the study. This geographic distribution ensured that the majority of participants came from rural or regional areas. The participants were then chosen for diversity in demographics and experiences. Two dichotomous variables, gender (male or female) and breastfeeding experience (self or spouse had breastfed/had not breastfed) were used in the sampling frame as previous quantitative research suggested an effect of gender and personal experience on doctors breastfeeding attitudes and confidence1,7,12. Participants with a range of ages were also identified with half being less than 34 years of age, the average age of GP registrars in Australia in 200520. While this sample is not statistically representative, the aim was to obtain a wide range of views, ideas and opinions of GP registrars18,21. By doing so the transferability of the results to similar groups is increased22.
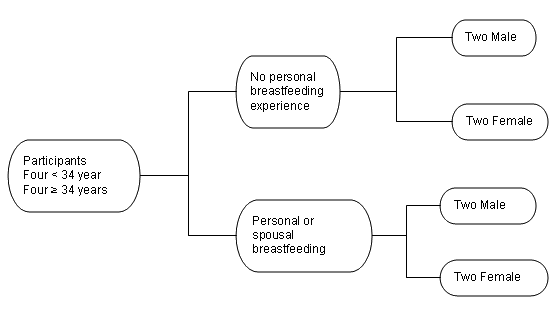
Figure 1: Selection matrix for interview participants.
Ethics approval
Ethics approval was obtained from the Behavioural and Social Sciences Ethical Review Committee, University of Queensland, Australia (clearance no 2005000456).
Materials
Semi-structured face-to-face interviews were conducted with the participants and information gathered included: their attitudes to breastfeeding and to assisting breastfeeding women in general practice; their breastfeeding knowledge needs and perceptions; their confidence in assisting breastfeeding women; and prior training about breastfeeding. Demographic variables also collected at interview included age, gender, years since graduation, years on the GP training program, whether they were parents, and if so whether the children were breastfed.
Procedure
Information regarding the study was sent to GP registrars in southern Queensland enrolled with the Rural and Regional Queensland Consortium, a provider of general practice training based in Toowoomba, and to other eligible registrars through the personal contacts of the researcher. Registrars interested in participating in the study were asked to contact the researcher and were recruited to participate if their socio-demographic profile filled positions on the selection matrix (Fig1). Interested registrars whose socio-demographic profiles were the same as registrars already participating in the study were not recruited. The participants were sent participant information sheets and mutually convenient times and places for an interview were arranged. All participants provided written consent at interview. The interviews, ranging in length from 21-36 min (mean = 28 min) were conducted between October 2005 and April 2006. They were recorded and transcribed with the transcripts being returned to the participants to verify accuracy before analysis began. Content analysis of each interview was undertaken by the researcher to identify emergent themes both within and among interviews. These results were then reviewed by two experienced qualitative researchers and changes were made until all parties were satisfied that the outcomes accurately reflected the content of the interviews. As this was a descriptive study18, no interpretation of the data was undertaken.
Results
Participants
Four participants were recruited via the Rural and Regional Queensland Consortium; the remainder were recruited from information given to personal contacts of the researcher. There were four male and four female participants with a mean age of 35 years (range 28-43). The children of the two male and two female participants who were parents, had been breastfed for more than 6 months. The years since graduation varied from two to 14 (mean = 7.5 years) and stage of GP training included basic GP terms (n = 3), advanced GP terms (n = 3) and subsequent GP terms (n = 2). Three participants had been born overseas, and had completed their medical training there. Four participants practised in small or other rural areas (RRMA 4 or 5). Three other participants practised in a large rural centre (RRMA 3). Only one participant practised in a large metropolitan area (RRMA 1) although she was about to commence working in an RRMA 4 designated area.
Specific questions relating to the effects gender and personal experience may have on breastfeeding attitudes or learning opportunities were not included in the interview outline. However, issues of gender and personal breastfeeding experience were a common thread through all eight interviews.
The influence of gender
Gender issues, particularly being male, affected the participants' views about breastfeeding and the role they played in assisting breastfeeding women. Male participants felt they were excluded from learning more about breastfeeding or developing practical breastfeeding skills by the attitudes of hospital nursing staff. These feelings resulted in them becoming distant and detached from any involvement with breastfeeding issues. One participant commented:
Certainly there are things that are regarded as women's business and actually intervening or even attempting to show an interest in some of those areas is discouraged, either passively or actively. [There]...isn't a lot of formal instruction in how to apply baby to the breast as a medical practitioner or particularly as a male practitioner. [Male, non-parent]
Participants considered that both women and other health professionals expected female doctors to be more knowledgeable and interested in breastfeeding than male doctors. Similarly, it was expected that male doctors were less knowledgeable about breastfeeding, particularly with practical issues and clinical skills.
I don't know how the men would help - or how male doctors could cope, really...Unless they've got wives who've had problems... [Female, parent]
These views led to the idea that the information female GPs gave was more likely to be trusted by mothers, even if their male counterpart was more knowledgeable and had had more experience.
... a female GP, she will be more believed by the patient, from her experience or her medical opinion will be more acceptable to a mum ... than a male GP. [Male, parent]
The perceived differences in breastfeeding knowledge between males and females reinforced the view that breastfeeding women would select a female practitioner within a general practice.
We're advantaged by having a female practitioner in the practice and there's a big trend I think nowadays to select towards the females. [Male, non-parent]
Some male participants believed that they needed minimal breastfeeding knowledge because they were unlikely to see breastfeeding women and were not the most appropriate people to assist or advise about breastfeeding.
I think it is valuable to encourage people, mums, to keep breastfeeding their babies, but I guess at this present moment in time whether I would be the most appropriate person to provide that instruction is the question that I would be asking. [Male, non-parent]
The influence of personal experience
The participants who were parents thought that they learnt more about breastfeeding from personal experience than from their medical program or subsequent work experience or training. They were disappointed that they needed personal experience to feel competent in this area of medical practice.
The most knowledge that I have is from my own experience. If it hadn't been for that I would know diddly squat really. [Female, parent]
Practical suggestions and clinical skills to help breastfeeding women were often neglected during the medical program and it was in these aspects where personal experience was thought to be especially useful.
I had the training more as theory but not as a practical and I have been trained as such on ... what the best technique and how you hold a baby and sort of latching ... That's come from personal experience later on in life. [Male, parent]
These participants also felt more confident discussing breastfeeding with women because they 'knew what they were talking about', could relate to problems the mothers might encounter and offer advice from their own experience.
I feel quite comfortable talking about breastfeeding only because I've breastfed myself. [Female, parent]
Participants who did not have children thought they were at a significant disadvantage to becoming more skilled and confident assisting breastfeeding women.
I guess not having had children myself or involvement there or practical experience in actually physically placing a baby on the breast... [Male, non-parent]
Additionally, there was concern that the information they gave was not reliable or valid because of their lack of personal experience.
I found it almost hypocritical in a way to try and explain things because I haven't breastfeed myself and ... I don't know that experience. [Female, non-parent]
They thought that having children of their own would improve their ability to manage breastfeeding problems.
Once I've had kids I'm sure I will be a lot more confident at dealing with not only breastfeeding and pregnancy, but also newborns and very young children which I don't feel confident at the moment. [Female, non-parent]
One participant was pregnant for the first time. Breastfeeding had become a much more important and personal issue. She found advice from others and reading lay books about breastfeeding and birth very informative and useful.
... [my increase in knowledge is] because of my own situation being pregnant myself. I've been reading about it myself and getting a lot of advice from people as you do when you're first pregnant. [Female, non-parent]
Discussion
By using purposive sampling to recruit participants who had different experiences with breastfeeding and thus provided diversity in the study population, one would expect to obtain a broad variety of responses. The fact that all participants independently broached the subject of gender and personal experience during the interviews underscores its importance for these registrars and increases the transferability of these finding to other groups.
Gender
Because breastfeeding is a female activity, the male participants thought women patients would assume that female doctors were more knowledgeable and better able to provide assistance with breastfeeding than male doctors. This perception became a self-fulfilling prophecy with male participants questioning whether it was necessary for them to have more than a basic knowledge about breastfeeding because women preferred to see female doctors with any breastfeeding concerns. Attitudes of female hospital staff towards medical students and doctors-in-training appeared to reinforce this view, with some male participants being discouraged from being involved with or learning about breastfeeding. If male doctors think that any breastfeeding knowledge or skills they have will not be used or valued, or that it will be inherently inferior, it is understandable that they may not see the value or need to become proficient in the subject.
While previous studies give conflicting results1,5 there is no convincing evidence that female doctors have increased confidence1 and knowledge23 about breastfeeding and lactation topics. Furthermore, being female does not automatically confer special breastfeeding knowledge to a person. Under the current training system, female doctors without children are only likely to have more knowledge than male doctors if they have seen more women with breastfeeding problems and learnt from experience, have a personal interest in the topic and/or have taken opportunities to learn about breastfeeding or consider that it is their responsibility to be able to assist women with breastfeeding difficulties. Freed et al.1 found that female family physicians did not consider that they were more confident or more knowledgeable than males. However, they were more likely to think their training about breastfeeding was insufficient and that there was not enough emphasis placed on helping and encouraging women to breastfeed. Female doctors may be more likely to acknowledge that they have a role to help and encourage breastfeeding women. They are also more likely to find breastfeeding a subject of personal interest when they become pregnant and have children of their own.
Personal experience
The participants in the present study found that personal experience with breastfeeding (either having breastfed themselves, or their spouse having breastfed) contributed substantially to their knowledge. This personal experience enabled them to feel confident and informed when discussing breastfeeding with women. In particular they found that practical aspects of breastfeeding, often not adequately covered in educational activities, provided a valuable insight into the concerns of breastfeeding women. The findings in this study are similar to finding in previous studies where doctors who were the parents of a child who was breastfed were more knowledgeable about breastfeeding1,6 and felt more confident counselling women with breastfeeding difficulties1. The role of gender and personal experience is less clear with one study suggesting that doctors who were mothers tended to have higher knowledge and confidence scores than doctors who were fathers12. In contrast, another study of general practice and paediatric trainees found no difference in knowledge or confidence between mothers and fathers6.
None of the parents interviewed in this study had had a negative breastfeeding experience - all breastfed for at least 6 months. However, a previous Australian study found that health professionals with negative personal breastfeeding experiences had lower breastfeeding knowledge scores than those with positive experiences or no personal experience at all24. Power et al.25 also found that male obstetricians whose spouses had not breastfed were least likely to have patients who were breastfeeding, compared with male obstetricians with no children and male obstetricians with breastfed children.
Nulliparous female participants felt that the information they gave mothers did not have the same authenticity as information provided by doctors who had breastfed. Similar sentiments expressed by other participants reflected the need to experience a situation before having sufficient knowledge and understanding to be able to help women. Dillaway and Douma26 also found that both paediatricians and nurses thought not having personal breastfeeding experience inhibited their ability to adequately assist breastfeeding women.
It is inevitable that doctors who have had a positive personal breastfeeding experience are more likely to have confidence when treating breastfeeding women. Nevertheless, doctors are called on to provide information, advice and treatment on a diverse range of conditions without the benefit of personal experience. Breastfeeding is not unusual in that regard, and it would be disappointing if doctors had to rely on personal breastfeeding experience to ensure they have the knowledge and expertise to be able to promote breastfeeding and encourage and assist breastfeeding women.
Doctors do not support breastfeeding women in isolation. Family, lay breastfeeding support groups and other health professionals also have a vested interest in providing support and assistance for breastfeeding women. Ideally a woman receives the benefit of encouragement and correct, consistent information from a number of different sources. Referring to people with more expertise was seen by this group of registrars to be a valid and important way of providing breastfeeding women with the help they needed27. Even so, women still attend their GP with breastfeeding problems and concerns. When working in rural and remote areas, doctors do not always have the luxury of being able to refer women to female practitioners, breastfeeding support services or others with breastfeeding expertise, and they may become the sole resource on which women rely.
Limitations to the study
There are a number of limitations to this study. There were no participants who had had negative personal breastfeeding experiences and these may have affected their views on the influence of gender and experiences on breastfeeding assistance. The findings of qualitative research are not representative of the whole population, so the views of this group of registrars may not be representative of the views of GP registrars in general, or of practising GPs. However, using a purposive sampling frame based on previous research increases the transferability of the results, and this is supported by congruence between some of this study's findings and those from large international quantitative studies.
Conclusions
The findings of this study provide valuable insights into the attitudes of a sub-sample of Australian male and female GP registrars with regard to their training about breastfeeding and their role with breastfeeding women. These attitudes need to be taken into account when discussing the role of GPs with breastfeeding women, and when designing and conducting breastfeeding training for medical students and registrars. For example, males as well as females need to be encouraged and supported to learn about breastfeeding and there should not be an assumption that female practitioners are knowledgeable and competent. Both male and female practitioners, regardless of personal or spousal breastfeeding experience, need sufficient breastfeeding knowledge and skills so that they can confidently provide encouragement, assess a woman with a breastfeeding problem and then treat or refer appropriately. Incorporating clinical experience and instruction on practical breastfeeding issues into training programs will ensure that these skills and knowledge are not only gained from personal experience. Additionally, GPs need to be aware of the breastfeeding support services available in their local area so that they can work in partnership to assist breastfeeding women.
The data from the results presented here will be used to design items to further elucidate the influence of gender and personal experience in a questionnaire investigating the attitudes and knowledge of GP registrars. Using triangulation of data, the interview results and results of the questionnaire will inform the development of a breastfeeding educational resource for GP registrars.
References
1. Freed GL, Clark SJ, Curtis P, Sorenson JR. Breast-feeding education and practice in family medicine. Journal of Family Practice 1995; 40: 263-267.
2. Pascoe JM, Pletta K, Beasley J, Schellpfeffer M. Best Start breastfeeding promotion campaign. Pediatrics 2002; 109: 170.
3. Finneran B, Murphy K. Breast is best for GPs - or is it? Breastfeeding attitudes and practice of general practitioners in the Mid-West of Ireland. Irish Medical Journal 2004; 97: 268-270.
4. Burglehaus MJ, Smith LA, Sheps SB, Green LW. Physicians and breastfeeding: beliefs, knowledge, self-efficacy and counselling practices. Canadian Journal of Public Health Revue Canadienne de Sante Publique 1997; 88: 383-387.
5. Williams EL, Hammer LD. Breastfeeding attitudes and knowledge of pediatricians-in-training. American Journal of Preventive Medicine 1995; 11: 26-33.
6. Guise J-M, Freed GL. Resident physician's knowledge of breastfeeding and infant growth. Birth 2000; 27: 49-53.
7. Schanler RJ, O'Connor KG, Lawrence RA. Pediatricians' practices and attitudes regarding breastfeeding promotion. Pediatrics 1999; 103: e35.
8. Arthur CR, Saenz R, Replogle WH. Breastfeeding education, treatment and referrals by female physicians. Journal of Human Lactation 2003; 19: 303-309.
9. Tennent R, Wallace LM, Law S. Barriers to breastfeeding: a qualitative study of the views of health professionals and lay counsellors. Community Practitioner 2006; 79: 152-156.
10. Ingram J. Multiprofessional training for breastfeeding management in primary care in the UK. International Breastfeeding Journal 1: 9. (Online) 2006. Available: http://www.internationalbreastfeedingjournal.com/content/1/1/9 (Accessed 14 June 2006).
11. Cantrill RM, Creedy DK, Cooke M. An Australian study of midwives' breast-feeding knowledge. Midwifery 2003; 19: 310-317.
12. Goldstein AO, Freed GL. Breast-feeding counselling practices of family practice residents. Family Medicine 1993; 25: 524-529.
13. Kim HS. Attitudes and knowledge regarding breast-feeding: a survey of obstetric residents in metropolitan areas of South Korea. Southern Medical Journal 1996; 89: 684-688.
14. Barton SJ. Infant feeding practices of low-income rural mothers. American Journal of Maternal and Child Nursing 2001; 26: 93-97.
15. Landers M, Hughes R, Graham K. The Darling Downs Breastfeeding Study. Toowoomba, QLD: Darling Downs Public Health Unit,1998.
16. Stamp GE, Casanova HT. A breastfeeding study in a rural population in South Australia. Rural and Remote Health 6: 495. (Online) 2006. Available: http://rrh.org.au (Accessed 10 January 2007).
17. Hegney D, Fallon T, O'Brien M, Plank A, Doolan J, Brodribb W et al. The Toowoomba infant feeding support service project: Report on phase 1 - A longitudinal needs analysis of breastfeeding behaviours and supports in the Toowoomba region. Toowoomba, QLD: University of Southern Queensland/University of Queensland, 2003.
18. Sandelowski M. Whatever happened to qualitative description? Research in nursing and health 2000; 23: 334-340.
19. Sandelowski M. Combining qualitative and quantitative sampling, data collection, and analysis techniques in mixed-method studies. Research in Nursing and Health 2000; 23: 246-255.
20. General Practice Registrars Australia Ltd. The future of general practice. (Online) 2004. Available: www.gpra.com.au/www/index.cfm?itemID=69 (Accessed 16 May 2007).
21. Sandelowski M. Sample size in qualitative research. Research in Nursing and Health 1995; 18: 179-183.
22. Malterud K. Qualitative research: standards, challenges, and guidelines. Lancet 2001; 358: 483-488.
23. Chen CH, Shu HQ, Chi CS. Breastfeeding knowledge and attitudes of health professionals and students. Acta Paediatrica Taiwan 2001; 42: 207-211.
24. Lowe T. Breastfeeding: attitudes and knowledge of health professionals. Australian Family Physician 1990; 19: 392-398.
25. Power ML, Locke E, Chapin J, Klein L, Schulkin J. The effort to increase breast-feeding. Do obstetricians, in the forefront, need help? Journal of Reproductive Medicine 2003; 48: 72-78.
26. Dillaway HE, Douma ME. Are pediatric offices "supportive" of breastfeeding? Discrepancies between mothers' and healthcare professionals' reports. Clinical Pediatrics 2004; 43: 417-430.
27. Brodribb W, Jackson C, Fallon AB, Hegney D. Breastfeeding and the responsibilities of GPs: A qualitative study of general practice registrars. Australian Family Physician 2007; 36: 283-285.



