Introduction
Rising health care costs and the need to consolidate expertise in tertiary services have led healthcare providers in some countries to reconsider how health services are provided and to move towards more centralised services1,2. The effects of such changes are hotly debated with some arguing that centralisation reduces the quality of care, due to increased patient volume or by placing additional burdens regarding access on the patient2-4. Others suggest that higher-volume hospitals have been found to have better outcomes, notably in studies of complex surgical procedures5. Maternity services, both in Europe6-8 and North America9, have struggled to find a balance between the need to centralise acute services and ensuring that women have access to care as close to their locality as possible. A key consideration has been ascertaining that health professionals have the skills to competently and confidently provide maternity services. Much discussion has focused on the challenges of attaining and maintaining competence in rural areas which may be geographically isolated and where health professionals may only care for a small number of pregnant women each year7,10-13. Although no association has been found between number of deliveries attended and maternal or perinatal outcomes11, there is evidence that health professionals who see low numbers of women tend to refer more readily11, perhaps indicating a lack of confidence. Practitioners in rural locations have been found to exhibit more caution regarding referral, often referring more readily than would have been indicated by national guidelines14. In Scotland the definition of 'rural' has been based on: (i) degree of remoteness; (ii) population density; (iii) settlement patterns; (iv) demographic profiles; and (v) economic profiles15. In 2005 the Scottish Executive defined rural as 'settlements with a population of less than 3,000 inhabitants'16. These settlements could be either remote rural (areas with 'a greater than 30-minute drive time to the nearest settlement with a population of greater than 10,000') or accessible rural (areas with a 30-minute or less drive time).
In the UK, it is midwives who have been most affected by maternity service changes as obstetric and anaesthetic services have been centralised in tertiary units. Many rural units have moved towards becoming midwife-led, requiring changes both in the organisation of the service and in the culture of the unit17-18. Professional development programs, involving training in advanced life support, have been used with the aim of developing the competence and confidence of the midwives to work as autonomous practitioners18.
Defining competence in midwifery has proved difficult, with definitions ranging from those that take a narrow performance-based approach (the ability to perform a particular skill or activity) to more detailed definitions that include a combination of knowledge, attitudes, skills and behaviour19. Some reports document the general activities of a midwife20, while specific midwifery competencies are more usually spoken about in relation to the essential skills and knowledge required of a practitioner to enter into midwifery practice21-23 or to achieve midwifery registration24. The International Confederation of Midwives (ICM) identifies six broad-based competencies, underpinned by specific skills and knowledge25. Some argue that such statements or standards are often too broad and do not present competence in a way that allows objective and independent measurement and assessment26. As a consequence, research has tended to focus on midwives' ability to carry out specific skills, such as suturing a perineum, siting an intravenous (IV) infusion, or managing an obstetric emergency27-29. However, even measuring this more narrowly-defined interpretation of competence has been far from straightforward. Fleming et al. used a four-point Likert-type rating scale, based on the Glasgow Royal Maternity Skills Inventory27, to elicit midwives' own reports of their competence for individual skills29. The categories used were 'I don't have these skills yet', 'I require a lot of practice', 'I require some practice' and 'I am fully competent'. Thus, the scale appeared to include an indicator of the quality of the performance, and it could be argued that this might raise the issue of confidence in the mind of the respondent. There is some evidence that practitioners are uncertain about whether competence is about being adequate or being expert30. A response of 'I require some practice' could therefore be interpreted as an indicator of lack of confidence rather than a lack of ability. The scale used by Persad et al. ranged from 'unwilling' to 'very competent'28 and was criticized for a similar reason; 'because "unwilling" does not necessarily mean "incompetent", there were immediate concerns about the validity of the scale' 29 p296. If a wider definition of competence is accepted, that is, one which considers not only performance but also capability19, then clearly confidence has a role to play. However, developing confidence in a skill often requires practice and thus, for some skills which can only be practised in a simulated situation (eg managing an obstetric emergency), it is arguable whether this is possible. Given these uncertainties, we considered it important to assess competence and confidence separately.
Background
In 2002 the Expert Group on Acute Maternity Services (EGAMS) in Scotland conducted a review of national and international approaches to intrapartum care to assist National Health Service (NHS) Boards 'to plan and configure their acute maternity services' and to 'identify the range of professional skills required by the Scottish maternity workforce'31 p3. The work was conducted by a multi-professional group including midwives, obstetricians, anaesthetists, paediatricians, GPs, paramedics, nurses and allied healthcare professionals. The result was a detailed report which included a list of 'skills and competencies' that EGAMS identified as essential for professionals to have in order 'to provide effective and safe care for low-risk women and to manage obstetric emergencies within remote and non-specialist units'31 p22. These 'skills' are listed (Fig1).

Figure 1: Core skills or competencies identified by Expert Group on Acute Maternity Services as being necessary for staff providing intrapartum care. Skills included in the questionnaire are shown in bold. IV, Intravenous.
A commissioned study explored the challenges that health professionals in remote and rural areas of Scotland face in the provision of maternity care, intrapartum care in particular, and asked the professionals to self-report their competence and degree of confidence with regard to some of these 'skills'12,32. As a follow up we undertook a sub-group analysis of the rural midwives' responses and a survey of midwives working in three urban units to examine whether confidence and competence assessments differed between rural and urban areas. This article reports the comparison.
Methods
Objective
Our objective was to compare the views of midwives in rural and urban settings regarding their competence and confidence with respect to the competencies identified by the EGAMS as being essential for all maternity care providers.
Design
The Scottish study of remote and rural maternity care was conducted in three phases: (i) mapping of units; (ii) site case studies with staff interviews; and (iii) questionnaire survey12,32. The data reported here are the responses from midwives in the questionnaire phase. The questionnaire was subsequently sent to a convenience sample of midwives in urban units to enable the comparisons to be made.
Questionnaire development
The questionnaire was developed using key themes identified from 72 interviews with staff in remote and rural areas12,32 and the policy questions identified by the EGAMS31. It contained seven sections:
- the individual's experience and the area in which s/he worked
- protocols and procedures for transfer in that area
- training
- skills and competence
- skills and confidence
- continuing professional development (CPD)
- maternity care in rural areas.
Most of the questions were closed-ended to help improve response rates, for ease of coding and data entry. This paper reports findings from sections D to F.
Respondents were asked to indicate their competence and confidence with respect to skills or 'competencies' that the EGAMS had highlighted as essential. Some skills noted in the EGAMS report were very broad (eg communication) and were therefore excluded in this study. Fifteen key skills required to support practice in rural and remote settings were selected for the questionnaire survey. These key skills were identified through triangulating the literature review, interviews, and input from experts in the advisory group and within the research team. The skills ranged from skills in a defined procedure (eg IV cannulation) to complex skills (eg basic obstetric life support). The skills are listed in bold in Figure 1. The literature suggests that competence is usually conceptualised either as a person 'being competent' or 'not' or as 'being half way along a continuum' (ie, adequate but not outstanding)30. Given the challenges of measuring competence previously discussed, we decided to use the simple question: 'Are you competent to do this?' for each item, offering respondents the option of 'yes' or 'no'. Confidence was assessed using a separate five-point Likert-type rating scale ranging from 'Not at all confident' to 'Very confident'. Respondents were also offered a separate box to tick if they felt that the skill was not applicable to their post. The next section presented a number of barriers to CPD, which had been identified from the interviews. Respondents were asked to rate these barriers as 'not important', 'important' or 'very important'. They were also given the opportunity to add additional barriers that were not listed.
Respondents could make additional comments on the final page of the questionnaire. The questionnaire was reviewed by the researchers and the steering group for content validity. Pilot testing (involving two midwives, two general practitioners and two obstetricians) led to some minor amendments being made.
Sample
Questionnaires were sent to two groups in 2003:
- Rural midwives - Midwives involved in the study of remote and rural maternity care (n = 82), identified by senior midwives in a stratified sample of units. The units were identified from routine data as those with low annual deliveries (<300) or small district general hospitals with large rural catchments (annual deliveries of approximately 1200)12,32.
- Urban midwives - Midwives from three urban units in Scotland, which have 'alongside' midwife-led units (n = 107), identified by heads of midwifery. The heads of midwifery in urban units were asked to apply a sampling ratio to staff establishment lists to avoid selection bias. All three units had more than 3000 deliveries per annum7.
Ethical approval was obtained from the appropriate local research ethics committees and permission to contact participants was obtained from heads of midwifery. Participants gave informed consent at two levels: (i) verbal consent to the interview was obtained from each individual participant in the rural group; (ii) implied consent to the questionnaire survey was assumed through return of the questionnaire in both groups. For the questionnaire survey, the cover letter provided participants with details of the study, the researchers involved and an assurance of confidentiality. Participants were informed that there was no obligation to participate in the study.
Data collection and analysis
Questionnaires were posted direct to study participants along with a pre-paid envelope to facilitate return. Each questionnaire contained a unique identifying number to enable reminders to be sent after 3 weeks. However, participants were assured that all data would be anonymised and that neither the participant nor the unit would be identifiable in the reporting of the results.
Data were collated and analysed using the statistical package SPSS for Windows33 (SPSS Inc; Chicago, IL, USA). Data checking revealed a data entry error rate of 0.35%. These errors were corrected prior to data analysis. Descriptive statistics were produced for all variables. Categorical variables were analysed using the χ2 test and continuous variables with a normal distribution by the Student's t-test. Results were considered to be statistically significant at the 5% level.
Results
The response rate from midwives in rural settings was considerably higher (85%; 70/82) than from midwives in the three urban settings (60%; 64/107).
Respondent characteristics
Midwives in urban settings were predominantly hospital based, while those in rural settings were more likely to work in both hospital and the community (Table 1).
Table 1: Demographic data
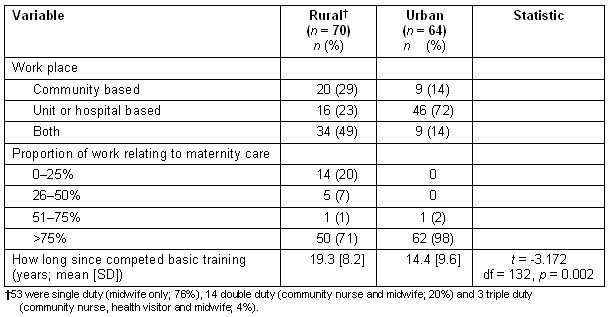
Of the urban midwives, only 16 (25%) were currently working within the delivery suite. Others worked in antenatal or postnatal wards (n = 18), clinics (n = 4), day care and ultrasound departments (n = 4), neonatal units (n = 1) and community midwifery (n = 13). Eight midwives did not specify the area in which they worked. The majority of urban midwives (92%) spent more than 75% of their time involved in maternity care. In contrast, more than a quarter of the rural midwives spent 50% or less time on maternity care. In most cases, these respondents had double or triple duty posts (n = 16/19); that is they also held a post as a community nurse or health visitor (in remote and rural areas of Scotland the community midwife has traditionally been a key health professional and the role has usually been carried out in combination with a nursing role - community nurse [double duty], community nurse and health visitor [triple duty])34. Rural midwives in this study had been qualified for significantly longer than urban midwives.
Competence
For many of the competencies, the proportion of midwives who reported that they were competent was similar in the two groups, for example repair of perineal trauma (Table 2). Although self-reported competence in emergency situations was consistently higher in the rural group, this was only statistically significant for breech delivery. Significantly more urban midwives reported competence in skills more commonly conducted in hospital, such as IV fluid replacement and initial and discharge examination of the newborn. Competence in prescribing drugs was also reported to be higher in the urban group.
Confidence
Respondents' ratings of confidence followed a similar pattern to competence (Table 3), but the differences between urban and rural groups with respect to emergency situations were less marked. The only statistically significant difference was with respect to initial and discharge examination of the newborn.
Table 2: Proportion of midwives who reported that they were competent to carry out skill
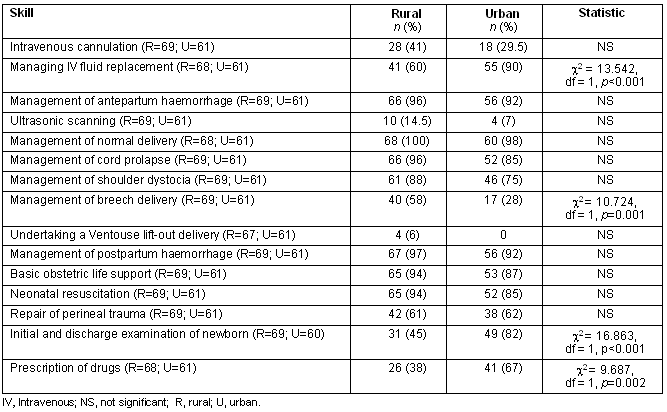
Table 3: Proportion of midwives who were confident or very confident to carry out skill
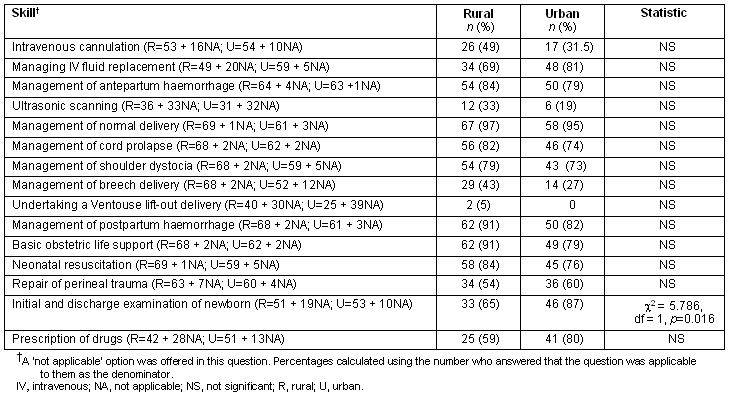
Continuing professional development
Significantly more respondents in the rural group (59%; 41/69) than the urban group (22%; 14/64) had attended a CPD event within the last month (χ2 = 21.793, df = 3, p<0.001). Barriers to attending CPD events were similar in the two groups (Table 4), but lack of time was reported to be a significantly greater barrier by urban midwives, whereas distance to training was a greater barrier for rural midwives. Lack of motivation or interest was significantly greater among midwives in urban units. Of the respondents who reported lack of motivation to be a barrier, 50% in the rural group and 90% in the urban group spent more than 75% of their time involved in maternity care.
Table 4: Barriers to continuing professional development
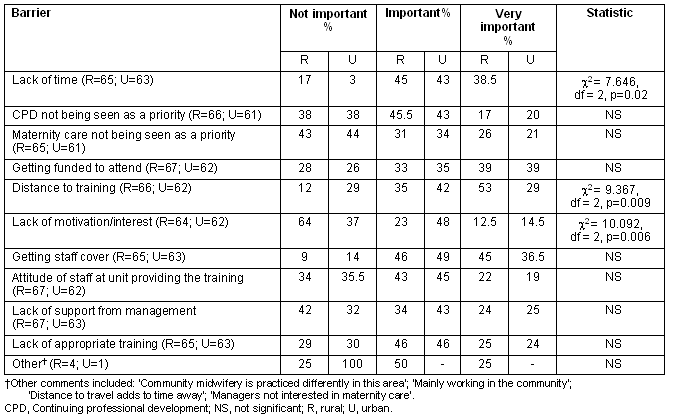
Discussion
This was an exploratory study and therefore has a number of limitations. The data on rural midwives were obtained as part of a larger survey of the views of health professionals involved in remote and rural maternity care in Scotland12 and the comparison with urban units was opportunistic, being conducted as an ad hoc survey afterwards. The sample size was not calculated with a view to making comparisons, but was purposively chosen in the rural areas to ensure views from representative sample of units and staff12,32 and was one of convenience in the urban units. The sample size was small and it is possible that the study did not have the adequate power to detect differences in competence and confidence. A larger sample size would also have allowed exploration of the relative importance of other factors, such as length of experience and current place of work. The different sampling methods could have resulted in differences between the groups other than those reported in Table 1; thus, caution must be exercised in interpreting the results. Data on the number of deliveries were available at unit level only and it cannot be assumed that midwives in units with larger throughput actually had greater exposure to relevant events than those in smaller units.
We attempted to measure competence and confidence separately; however, the two aspects are clearly related. Identifying exactly what is meant by the term 'competence', and how it can be determined, has long challenged health care13,19,35-38 as well as other professional groups30. One of the main reasons for this seems to be the range of different definitions or terminology, which may be used differently even within the same professional group19,30,37. Although it has been suggested that there is a distinction between competence and the performance of a skill39, identifying the features involved in making a practitioner competent is not straightforward. Worth-Butler et al. suggest that performance relates to something a person is capable of doing in some situations (the quality of the performance may vary), while competence draws on multiple performances19. This implies that confidence may play an important role, as repeated performances will increase familiarity with the result that the practitioner is more likely to report that they are competent. However, it also raises the question of whether a practitioner can ever really develop competence in rare events.
Various tools exist to measure the competence of nursing and midwifery students; however, two recent systematic reviews have raised concerns about their use37,40. Problems include the fact that little consideration has been given to validity and reliability when developing such instruments37,40 and the finding that the potential for subjectivity when carrying out the assessment has not been addressed37. Assessment of competence of qualified practitioners has tended to rely on self-report28,29 and this was the method used in this study. There is limited research into the validity and reliability of self-report measures37, and no evidence of their transferability to actual practice. A recent study used non-participant observation and interviews to observe competency elements as part of a validation of competency standard41. However, the study was concerned with validating that the competency standards were applicable to midwifery practice, rather than assessing whether midwives met these standards.
Our study is unique in comparing confidence and competence assessments from practitioners in rural and urban areas. Previous studies of midwifery competence have focused on midwives as a single group28 or compared them by type of training29. Thus, despite these limitations, the findings of this study can usefully contribute to the debate on the centralisation of maternity services.
Previous research into maternity services suggests that health professionals who see low numbers of women11, and practitioners in more rural practices14 tend to refer more readily. The reasons for these associations are not clear, but might be thought to be due to a lack of confidence. However, our findings suggest that confidence is not low among midwives in rural Scotland. Self-reported competence and confidence with regard to emergencies was as high among rural midwives as among urban midwives, despite the fact that more emergencies are seen in tertiary units in urban areas. Indeed, for breech delivery, now often viewed as an emergency situation, rural midwives appeared to feel significantly more competent than their urban colleagues. It is unclear why this should be. Some have suggested that the medicalisation of childbirth and an over-reliance on medical technology have led to the de-skilling of midwives42,43 and, because this is more likely to occur in urban units, it could be argued that this is one reason for the lower reports of competence in this group with regard to breech delivery.
The limitation of the study design means that place of practice is confounded by a number of factors, including job description and time spent providing maternity care. However, notably only a quarter of the midwives in the urban group were actually working within the delivery suite at the time of the survey and, thus, lack of recent experience in obstetric emergencies could have been an issue in both groups. Because these events are rare, even in tertiary units, maintaining competence could have been an issue even for those currently working in the delivery suite.
Continuing professional development is often relied upon to maintain competence and confidence with regard to rare events. Government reports have recommended that CPD events, in particular life support training, be used to maintain competence with regard to obstetric emergencies44; however a recent systematic review found little evidence about whether such courses can improve the actual management of obstetric emergencies45. The review did find that all studies reported participants had a significant increase in confidence in handling obstetric emergencies, and one study found that this was maintained for 12 months after the course45. In our study more rural than urban midwives had recently undertaken CPD, which may explain the increased confidence regarding breech delivery.
Staff in remote and rural areas face significant challenges in maintaining their skills. In some countries this has led to a substantial reduction in the number of midwives who are able to demonstrate that they are competent and, therefore, can renew their authorization to practice10. However, our findings indicate that there may also be significant challenges to maintaining competence in urban maternity units. Although CPD courses are more readily available to those in tertiary units, urban respondents reported that it was difficult to find time to access such courses. Indeed, the comments indicated that for many urban midwives, even attending mandatory update sessions was difficult. An unexpected finding was that more urban midwives reported lack of motivation or interest to be a barrier to CPD. This was despite the fact that a greater proportion of rural midwives had commitments other than maternity care. The picture is complicated by the fact that many rural units in Scotland, including small district general hospitals, are in a period of transition and undergoing considerable change in order to remain viable. The move towards community maternity units that are midwife-led has put considerable pressure on practitioners to maintain and update their skills18, and this could explain the rural midwives' more recent attendance at CPD events. However, it has been suggested that job dissatisfaction and disillusionment are higher in tertiary units43, and this needs further investigation.
Not surprisingly, the urban group reported greater competence with skills more commonly associated with care of the high-risk woman, such as IV fluid replacement and prescribing of drugs. Confidence was lowest in both groups with regard to ultrasonic scanning and Ventouse delivery. However, these competencies were ones which the EGAMS states should be considered as a 'team competency' and thus achieved by at least one team member in remote areas31. Training courses in these aspects are now being made available to staff in remote units in Scotland.
Conclusions
It might be assumed that midwives working in rural areas, with fewer deliveries, will be less competent and confident in their practice. Our exploratory study tentatively suggests that the issue of competence is far more complex and deserves further attention, especially in light of recruitment and retention problems in rural areas, and the re-design of maternity services.
Acknowledgements
The study was funded by NHS Education for Scotland and the work conducted through the Centre for Advanced Studies in Nursing and the Dugald Baird Centre for Research in Women's Health, University of Aberdeen, Scotland. However, the views expressed in this article are those of the authors. The authors would like to thank the midwives who participated in the study and provided the data for this article.
References
1. Hemmelgarn BR, Ghali WA, Quan H. A case study of hospital closure and centralization of coronary revascularization procedures. Canadian Medical Association Journal 2001; 164: 1431-1435.
2. Mungall IJ. Trend towards centralisation of hospital services, and its effect on access to care for rural and remote communities in the UK. Rural Remote Health 5: 390. (Online) 2005. Available: http://www.rrh.org.au/ (Accessed 19 June 2007).
3. Bindman AB, Keane D, Lurie N. A public hospital closes. Impact on patients' access to care and health status. Journal of the American Medical Association 1990; 264: 2899-2904.
4. Baird AG, Donnelly CM, Miscampell NT, Wemyss HD. Centralisation of cancer services in rural areas has disadvantages. BMJ 2000; 320: 717.
5. Webster P. Time to evaluate why high-volume hospitals have better surgical outcomes. Canadian Medical Association Journal 2005; 173: 2.
6. Holt J, Vold IN, Backe B, Vollnes M, Oian P. Child births in a modified midwife managed unit: selection and transfer according to intended place of delivery. Acta Obstetricia et Gynecologica Scandinavica 2001; 80: 206-212.
7. Scottish Executive Health Department. Expert Group on Acute Maternity Services Reference Report. Edinburgh: Scottish Executive, 2002.
8. Department of Health. The Report of the Maternity and Neonatal Workforce Group to the Department of Health Children's Taskforce. London: Department of Health, 2003.
9. Klein MC, Johnston S, Christilaw J, Carty E. Mothers, babies and communities. Centralizing maternity care exposes mothers and babies to complications and endangers community sustainability. Canadian Family Physician 2002; 48: 1177-1179.
10. Monaghan J, Walker J. Delivery in the bush: maintaining workforce in rural and remote Tasmania. In: Proceedings, 6th National Rural Health Conference. 4-7 March 2001; Canberra, ACT, Australia. 2001.
11. Klein MC, Spence A, Kaczorowski J, Kelly A, Grybowski S. Does delivery volume of family physicians predict maternal and newborn outcome? Canadian Medical Association Journal 2002; 166: 1257-1263.
12. Kiger A, Tucker J, Bryers H, Caldow J, Farmer J, Hundley V et al. Sustainable maternity service provision in remote and rural areas of Scotland: The scoping of core multidisciplinary skills and best practice in the development and maintenance of skills. Edinburgh: NHS Education for Scotland, 2003.
13. Ireland J, Bryers H, van Teijlingen E, Hundley V, Farmer J, Harris F, Tucker J, Kiger A, Caldow J. Competencies and skills for remote and rural maternity care: a review of the literature. Journal of Advanced Nursing 2007; 58: 105-115.
14. Tucker J, Farmer J, Stimpson P. Guidelines and management of mild hypertensive conditions in pregnancy in rural general practices in Scotland: issues of appropriateness and access. Quality and Safety in Health Care 2003; 12: 286-290.
15. Scottish Office. Scottish rural life - an update. A revised socio-economic profile of rural Scotland. Edinburgh: Scottish Office, 1996.
16. Scottish Executive. Rural definitions map. (Online) 2005. Scottish Executive, Edinburgh. Available: http://www.scotland.gov.uk/Topics/Rural/rural-policy/16780/6661 (Accessed 19 June 2007).
17. Turner M. Helme Chase Maternity Unit: experiences of a stand alone midwifery led unit in rural Cumbria. MIDIRS Supplement, MIDIRS Midwifery Digest 2004; 14: S22-S24.
18. Leatherbarrow B, Winters P, Macleod L, Nicoll A, McNicol K et al. From vision to reality: the development of a community maternity unit. RCM Midwives 2004; 7: 212-215.
19. Worth-Butler M, Murphy RJL, Fraser DM. Towards an integrated model of competence in midwifery. Midwifery 1994; 10: 225-231.
20. Office for Official Publications of the European Communities. Council Directive 21 concerning the coordination of provisions laid down by law, regulation or administrative action related to the taking up or pursuit of the activities of midwives. (80/155/EEC). Office for Official Publications of the European Communities. Online (1980; amended 1989 and 2001). Available: http://europa.eu.int/eur-lex/en/consleg/pdf/1980/en_1980L0155_do_001.pdf (Accessed 19 June 2007).
21. The Australian Nursing and Midwifery Council. National Competency Standards for the Midwife 2006. Online (no date). Available: http://www.anmc.org.au/ (Accessed 19 June 2007).
22. College of Midwives of British Columbia. Competencies of Registered Midwives (revised June 2005). Vancouver: College of Midwives of British Columbia, 1997. Available: http://www.cmbc.bc.ca (Accessed 19 June 2007).
23. American College of Nurse-Midwives. Core competencies for basic midwifery practice. Silver Spring: ACNM, 2007. Available: http://www.acnm.org/siteFiles/descriptive/Core_Competencies_6_07_3.pdf (Accessed 1 August 2007).
24. Midwifery Council of New Zealand. Competencies for entry to the Register of Midwives. Midwifery Council of New Zealand. (Online) 2004. Available: http://www.midwiferycouncil.org.nz/main/Competence/ (Accessed 19 June 2007).
25. International Confederation of Midwives. Essential competencies for midwifery practice. The Netherlands: International Confederation of Midwives, 2002. Available: http://www.internationalmidwives.org (Accessed 19 June 2007).
26. Worth-Butler M, Murphy R, Fraser D. The need to define competence in midwifery. British Journal of Midwifery 1995; 3: 259-262.
27. The MDU Research and Midwifery Teams. The establishment of a Midwifery Development Unit based at Glasgow Royal Maternity Hospital. Glasgow: Glasgow Royal Maternity Hospital, Midwifery Development Unit, 1995.
28. Persad PS, Hiscock C, Mitchell T. Midwives' own perception of competence in obstetric procedures. British Journal of Midwifery 1997; 5: 706-708.
29. Fleming V, Poat A, Curzio J, Douglas V, Cheyne H. Competencies of midwives with single and dual qualifications at the point of registration in Scotland. Midwifery 2001; 17: 295-301.
30. Eynon R, Wall DW. Competence-based approaches: a discussion of issues for professional groups. Journal of Further and Higher Education 2002; 26: 317-325.
31. Scottish Executive Health Department. Implementing a framework for maternity services in Scotland. Overview Report of the Expert Group on Acute Maternity Services (EGAMS). Edinburgh: The Stationary Office, 2002.
32. Tucker J, Hundley V, Kiger A, Bryers H, Caldow J, Farmer J et al. Sustainable maternity services in remote and rural Scotland? A qualitative survey of staff views on required skills, competencies and training. Quality and Safety in Health Care 2005; 14: 34-40.
33. Norusis MJ. SPSS 11.0. Guide to data analysis. Upper Saddle River: Prentice Hall, 2002.
34. West JM, MacDuff C. Evaluating family health nursing through education and practice. Scottish Executive, Edinburgh, 2003. Available: http://www.scotland.gov.uk/Publications/2003/10/18442/28466 (Accessed 19 June 2007).
35. Girot EA. Assessment of competence in clinical practice: a review of the literature. Nurse Education Today 1993; 13: 83-90.
36. Manley K, Garbett R. Paying Peter and Paul: reconciling concepts of expertise with competency for a clinical career structure. Journal of Clinical Nursing 2000; 9: 347-359.
37. Watson R, Stimpson A, Topping A, Porock D. Clinical competence assessment in nursing: a systematic review of the literature. Journal of Advanced Nursing 2002; 39: 421-431.
38. McMullen M, Endacott R, Gray MA, Jasper M, Miller CML, Scholes J et al. Integrative literature reviews & meta-analyses. Portfolios & assessment of competence: a review of the literature. Journal of Advanced Nursing 2003; 41: 283-294.
39. Ashworth P, Saxton J. On 'competence'. Journal of Further and Higher Education 1990; 14: 3-25.
40. Norman IJ, Watson R, Murrells T, Calman L, Redfern S. The validity and reliability of methods to assess the competence to practice of pre-registration nursing and midwifery students. International Journal of Nursing Studies 2002; 39: 133-145.
41. Homer CSE, Passant L, Kildea S, Pincombe J, Thorogood C, Leap N et al. The development of national competency standards for the midwife in Australia. Midwifery 2007. (In press).
42. Walsh D. Midwives and birth technology: a debate that's overdue MIDIRS Supplement 2. MIDIRS Midwifery Digest 2001; 11: S3-S5.
43. House of Commons Health Committee. Provision of Maternity Services: Fourth report of session 2002-03. Vol 1 (HC464I). London: The Stationery Office Limited, 2003.
44. National Institute for Clinical Excellence, Scottish Executive Health Department, Department of Health, Social Services and Public Safety: Northern Ireland. Why mothers die 1997-1999. The Confidential Enquiry into Maternal Deaths in the United Kingdom. London: RCOG Press, 2001.
45. Black RS, Brocklehurst P. A systematic review of training in acute obstetric emergencies. British Journal of Obstetrics and Gynaecology 2003: 110: 837-841.









