Introduction
The death certificate is the formal document in which a physician records the time, cause and circumstances of the death of an individual. Morbidity and mortality statistical studies are mainly based on the analysis of these certificates1-3. Consequently, inaccuracies in the completion of death certificates may lead to biased estimation of several epidemiological parameters4,5.
Almost every physician will have to complete at least one death certificate in his career. However, teaching the precise wording and formulation of causes of death is not usually included either in undergraduate or in postgraduate medical education6-9. Weeramanthri et al. estimated the impact of an educational intervention on physicians' improvements in completing death certificates10. They showed a non-significant reduction in the error rate10. Following this, Myers and Farguhar examined the impact of an interactive learning method on error rates in the completion of death certificates, reporting a statistically significant decrease in errors11.
It is obvious that errors in the completion of death certificates present a problem from the legal standpoint, as well as for the purposes of collecting relevant vital statistics data from which to draw conclusions. Accordingly, every effort must be made to ensure that the completion of death certificates is performed in the most specific, accurate and complete fashion.
The goal of the present study was to review all death certificate records during an eight year period in a rural region of western Greece, as well as to evaluate the quality of cause-of-death statistics.
Methods
A retrospective study was conducted in an effort to determine the frequency and type of errors observed during the completion of a death certificate. The study was approved by the director of Erymantheia's Health Center, Greece. All original death certificates archived in the municipality of Tritaia during the period 1999-2006 were examined.
Two authors of the present study (PFK and MK), independently verified all death certificates to discover the type of any error in each. In the case of four documents, the two authors classified the error according to different types but achieved consensus after discussion.
The structure of death certificate
All death certificates should be completed in accordance with the World Health Organization (WHO) standard structure12. Briefly, such a certificate is generally composed of two segments:
- The demographic characteristics of the decedent.
- Part I. The sequence of events that led to the death, starting from the final disease or condition that resulted in death. Each condition in this part is caused by the condition stated before it. The final entry in this sequence is the specific cause of death, which should be stated in order to avoid any doubt about the etiology of death.
Part II. Any significant condition, disease or injury that contributed to death but did not lead to the underlying cause is stated.
Types of error
This study did not validate the cause-of-death diagnoses because no medical records or autopsy information were available. However, the death certificates were examined for inaccuracies in their completion. For this purpose, we adapted the classification system used by Leadbeatter et al and Lu et al13,14. The errors encountered were classified into four categories:
- Error A: the mechanism but not the cause of death is given.
- Error B: multiple causal statements are given.
- Error C: a single but non-precise cause is given.
- Error D: a single causal sequence with incorrect order is given.
Associated factors
The certifying doctors were classified into two groups: (i) primary health care physicians working in the regional health centre (Group A); and (ii) private physicians and physicians working in hospitals (Group B). The demographic data (sex and age) of the decedent were obtained from death certificates.
Statistical analysis
Statistical analysis was performed using SPSS 14.0 for Windows (SPSS Inc; Chicago, IL, USA), Microsoft Office Excel 2003 and MIM 3.2 (http://www.hypergraph.dk). Age was expressed as median and range. A comparison of the results was made by comparing the proportions of the unpaired case. More specifically, the null hypothesis was tested approximately by taking
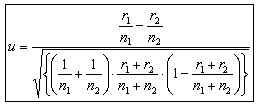
as a standardized normal deviate15.
With regard to the state of independence among the variables 'gender', 'error type', 'age' and 'doctor origin', investigation was performed by considering the class of discrete graphical models16. According to this method, a graph is formed consisting of nodes; each node represents a variable. The presence of connecting lines (undirected edges) between the nodes can be interpreted in terms of conditional independence between them. With regard to the evaluation of dependence between the different variables, we started from the saturated model that represents the model of no independence between any two nodes, and we performed statistical significance tests in order to examine whether a simpler model could fit the data within acceptable limits. The tests were based on the Akaike Information Criterion (AIC) score, which takes into consideration quality of fit, as well as the model's complexity. This procedure, called backward selection, attempts to delete existing edges in a stepwise manner. The process ends when no significant reduction of ΑIC score is achieved and the model chosen best fits the data. MIM 3.2 was used for the analysis. The significance level was set at 0.05.
Results
Frequencies of error
A total of 516 death certificates were examined in the present study; 5.6% (11 males and 18 females) were excluded because of insufficient demographic data. The remaining 487 death certificates were finally analyzed (51.5% males, 48.5% females: median age 82 years, range 5-103 years; and 83 years, range 0-104 years, respectively). In 20.1% (98/487) of the death certificates, the certifier was a regional health centre physician; whereas, the remaining 79.9% were certified by private physicians or physicians working in hospitals.
In all, 39.4% (192/487) were correctly completed. From the certificates presented with an error, in 168 (34.5%) only the mechanism of death was given (Error A); in 72 (14.8%) multiple causal sequences were given (Error B); in 22 (4.5%) a single but non-precise cause was given (Error C); and in 33 (6.8%) a single causal sequence with incorrect order was given (Error D).
Factors associated with errors
The different types of error according to the characteristics of the decedent and the certifying physician are given (Table 1).
Table 1: The frequency distribution of the errors by age and sex of the deceased and by the specialty of the certifying physician
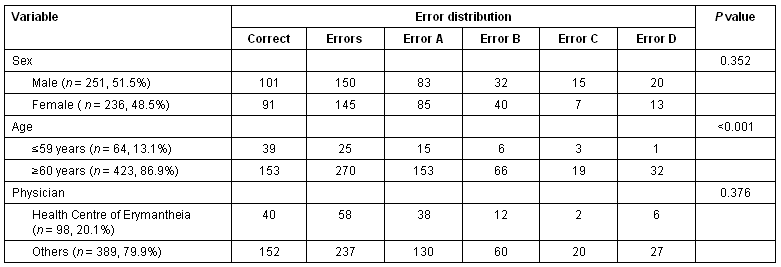
Gender was not associated with the presence of errors (p = 0.352). In contrast, the probability of inaccuracy rose as the age of the deceased increased. Errors were present in 63.8% (270/423) of the death certificates in deceased individuals ≥60 years of age, and in 39.1% (25/64) in individuals ≤59 years (p<0.001).
In 19.7% (58/295) of the erroneously completed death certificates, the certifier was a physician working in primary health care (p = 0.376). In 1999, 74.6% (50/67) of the death certificates contained with errors; whereas, in 2006 the error rate had decreased to 51.8% (29/56) (p = 0.004).
Figure 1 shows the final model that was produced from the analysis of dependence among the variables using MIM 3.2. The 'model selection' procedure of the log-linear analysis of SPSS 14.0 gave similar results.
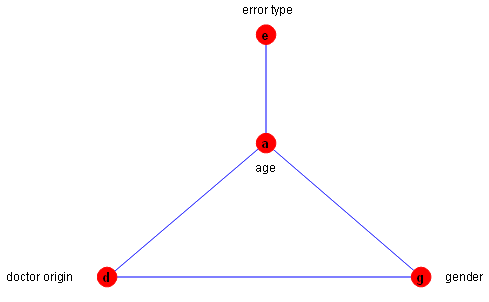
Figure 1: The best-fit model, selected by backward selection using ΑIC criterion.
What is evident from the graph is that the 'error type' is directly dependent on 'age', while its dependence on the rest of the variables passes through 'age'. In other words, 'error type' is rendered independent of the other variables, provided that we have knowledge of 'age'.
Discussion
The present study was an attempt to estimate the accuracy of death certificate completion in a region of western Greece, using the data from death certificates over an 8 year period. Almost two-thirds of the death certificates (60.6%) were erroneously completed. The most frequent type of error was Error A, where the mechanism but not cause of death was given. It is encouraging that during these 8 years there has been a statistically significant decrease in the presence of error.
Types of error
The most serious errors in death certificates, according to cause-of-death statistics, are Errors A and B. The rate for Error A was 34.5% (168/487) in our study, which is relatively high compared with other reports of rates ranging from 7% to 29%6,14,17. Physicians usually confuse the cause of death with the mechanism of death; probably because the target of the medical treatment is more often the mechanism2,14. The cause of death is a distinct entity and etiologically specific. However, the mechanism is a physiologic derangement or a biochemical disturbance produced by the cause of death. With this understanding, diabetes mellitus is a possible cause of death, but cardiac arrest is a mechanism of death. The mechanism is not etiologically specific and for this reason it should not appear on death certificates. Nevertheless, it is not always easy to identify a definite cause of death, especially for dying patients who are sent to hospital without information about their medical history. In such cases, it is easier for the certifier to determine the mechanism, rather than the cause of death.
The rate of Error B was 14.8% (72/487), and second most frequent in our study. Physicians tend to report causes of death according to their severity, as well as being the main reason for admission14. Increased life expectancy has led to a multivariate cause of death, and it is increasingly likely that death is due to conditions affecting multiple organ systems (eg cardiovascular-renal disease). As a result, the assignment of a single cause of death will result in the loss of diagnostic information. For this reason, a new form of death certificate with the option of recording multiple diagnoses should be developed.
The rate of Error C was 4.5% (22/487). This type of error does not change the ranking of the leading causes of death if the two-digit codes of the International Classification of Diseases, 9th revision (ICD-9) are used18.
Error D was observed in 6.8% (33/487) of the death certificates. This is relatively low when compared with the literature6,14,17. Death certificates with this type of error contain insufficient information for epidemiological studies. For example, in a deceased patient who suffered from diabetes mellitus and coronary artery disease, diabetes should be entered second to coronary artery disease in the certificate's cause of death sequence. The opposite sequence would incorrectly suggest that the coronary artery disease caused the diabetes.
The classification of errors used in this study was previously proposed and tested in the literature13,14. Another way of analyzing the death certificates would be through the rule system described in the ICD-1012. In this system, five rules are proposed in order to correct errors occurring in completion of the main conditions that lead to death. Reviewing death certificates using this system, observed errors could be easily corrected. However, the adoption of this system was not feasible during our study.
Associated factors
The most important factor associated with the rate of errors is the age of the deceased. As age advances, co-morbidity increases, and this makes it difficult for a physician to distinguish a single causal sequence14. This is consistent with our results.
The specialty of the certifier plays an important role as well. Family physicians are reported to perform better in death certification accuracy than other specialists6,7,10. This may be attributed to their training in this task, and to their familiarity with their patients. It was not possible to estimate the performance of family physicians in death certificate completion in our study. The group of physicians working in the health centre, particularly during the first years of our study, consisted of both specialized family physicians and unspecialized doctors. In addition, the low number of death certificates completed by family physicians during the study period may have lead to inaccurate conclusions.
The age of the certifier is another significant factor to consider. According to James et al, the incidence of errors decreases as the age of the certifier increases19. Unfortunately, such data was not available in our case.
Finally, in our study we report a decrease in the presence of errors in death certification between the years 1999 and 2006. This may be because greater efforts have been made to improving physicians' certifying skills. However, further and on-going educational intervention is required.
Study limitations
Despite our analysis, a potential pitfall is the lack of medical records and autopsy results. However, the primary goal of this study was to detect physicians' certifying errors, rather than identify the cause of death itself. Furthermore, these data could not be obtained at the time of the study. Another limitation is the absence of the classification system ICD-10, which categorizes errors in the completion of death certificates into five groups. However, this system has not been widely used in the studied region and physicians are not yet familiar with it.
Conclusion
In conclusion, the efforts of both trainers and physicians are required in order to improve the quality of diagnostic information in death certificates. In this way, more accurate cause-of-death statistics derived from death certificates will lead to better health planning.
References
1. Smith Sehdev AE, Hutchins GM. Problems with proper completion and accuracy of the cause-of-death statement. Archives of Internal Medicine 2001; 161: 277-284.
2. Kircher T, Anderson RE. Cause of death: proper completion of the death certificate. The Journal of American Medical Association 1987; 258: 349-352.
3. Crowcroft N, Majeed A. Improving the certification of death and the usefulness of routine mortality statistics. Clinical Medicine 2001; 1: 122-125.
4. Messite J, Stellman SD. Accuracy of death certificate completion: the need for formalized physician training. The Journal of American Medical Association 1996; 275: 794-796.
5. Armour A, Bharucha H. Nosological inaccuracies in death certification in Northern Ireland. The Ulster Medical Journal 1997; 66: 13-17.
6. Jordan JM, Bass MJ. Errors in death certificate completion in a teaching hospital. Clinical and Investigative Medicine 1993; 16: 249-255.
7. Peach HG, Brumley DJ. Death certification by doctors in non-metropolitan Victoria. Australia Family Physician 1998; 27: 178-182.
8. Lionis C, Sasarolis S, Kasotakis GI, Lapidakis GM, Stathopoulos AI. Investigation of accuracy of death certificate completion and implications on mortality statistics in Greece. European Journal of Epidemiology 2000; 16: 1081.
9. Slater DN. Certifying the cause of death: an audit of wording inaccuracies. Journal of Clinical Pathology 1993; 46: 232-234.
10. Weeramanthri T, Beresford W, Sathianathan V. An evaluation of an educational intervention to improve death certification practice. Australian Clinical Review 1993; 13: 185-189.
11. Myers KA, Farquhar DRE. Improving the accuracy of death certification. Canadian Medical Association Journal1998; 158: 1317-1323.
12. World Health Organization. International Statistical Classification of Diseases and Related Health Problems Vol 2, 10th revision, 2nd edn. Geneva: WHO, 2004.
13. Leadbeatter S. Semantics of death certification. Journal of the Royal College of Physicians of London 1986; 20: 129-132.
14. Lu TH, Shau WY, Shih TP, Lee MC, Chou MC, Lin CK. Factors associated with errors in death certificate completion. A national study in Taiwan. Journal of Clinical Epidemiology 2001; 54: 232-238.
15. Armitage P, Berry G, Matthews JNS. Statistical methods in medical research. Oxford: Blackwell Publishing, 2001.
16. Whittaker J. Graphical models in applied multivariate statistics. Chichester: Wiley 1990.
17. Zumwalt RE, Ritter MR. Incorrect death certification-an invitation to obfuscation. Postgraduate Medicine 1987; 81: 245-254.
18. World Health Organization. Manual of the international statistical classification of diseases, injuries, and causes of death. Vol 1, 9th revision edn. Geneva: WHO, 1977.
19. James DS, Bull AD. Death certification: is correct formulation of cause of death related to seniority or experience? Journal of the Royal College of Physicians of London 1995; 29: 424-428.



