Introduction ___________________________
The James Cook University (JCU) School of Medicine has recently graduated its first three cohorts. Founded in 2000, it was the first new medical school in Australia for 20 years, and had a mission to prepare graduates to meet the needs of northern Australia across a large geographical area1. It remains the only complete medical school in Australia's tropical north. The six-year undergraduate course recruited students who were predominantly school leavers, and had a major emphasis on rural, remote, Indigenous and tropical health. Strategies used to develop students' understanding of these key areas of the program included: the geographic location of the school; student selection and support; rural orientation of curricula, experiences and teachers; establishment of a multidisciplinary rural student club; and the provision of postgraduate training and career opportunities locally. All students completed the core subject in year 2, 'Rural, Remote, Indigenous and Tropical Health', which provided a theoretical foundation for these strands of the course2,3.
Additional experiences throughout the program included cross-cultural courses and structured rural placements in years 2 (4 weeks), year 4 (8 weeks) and year 6 (8 weeks). Each of the three core rural placements had different learning objectives. The year 2 rural placement formed the first major clinical experience of the course. Students had a wide choice of placements in rural and remote locations. Learning objectives included development of clinical skills, an appreciation of the importance of the basic sciences in clinical medicine, and developing a deeper understanding of rural and remote communities and the healthcare system. The year 4 placement was more structured. Placement sites were defined with more limited choice. Students were expected to work in pairs studying clinical skills and pathology under the supervision of a clinical tutor. Some teaching was provided by distance education techniques2,3.
The third core rural placement was in year 6, by which stage students had completed the final major summative examinations in the course (at the end of year 5). Students undertook five rotations of 8 weeks each in year 6: aged care and rehabilitation; critical and crisis care; multidisciplinary adult health; the rural internship; and an elective/corrective. The focus of these rotations was vocational preparation, ensuring that students had the necessary knowledge, skills and attitudes to prepare them for their intern year4. The learning objectives are summarized (Fig 1). Assessment was via a learning portfolio across the whole year (50%), and in-rotation assessment. Year 6 students were based at the clinical schools in Mackay, Townsville, Cairns and Darwin.

Figure 1: Learning objectives for year 6 students.
Methods
The rural internship was designed to allow students to develop and practise clinical skills in a rural context in small rural hospitals. Students undertook full-time inpatient and outpatient responsibilities under supervision, being rostered for after-hours work with appropriate support. The state government health department (Queensland Health) was closely involved in the planning and implementation of the program in the first year, through its Northern Zone Workforce Unit and the newly created position of JCU liaison officer. A set of guiding principles was developed regarding supervision and legal sign-off (Fig 2).

Figure 2: Guiding principles for the rural internship.
Care was taken to ensure that both the students and preceptors were aware of the students' limitations and boundaries in regard to accepting responsibility for care. Concern for patient safety was paramount, and guidelines were developed to ensure that patient care was not compromised; informed consent was obtained from all patients; and clinical decisions and the time to definitive care was not influenced by involvement of the student. At all times students were under the supervision of the medical superintendent or delegate, who was responsible for checking and verifying all student tasks. Some aspects of student involvement were determined locally such as completion of clinical records and pathology forms. Other issues that were resolved in conjunction with Queensland Health included accommodation, access to information technology resources, and access to pathology and radiology systems.
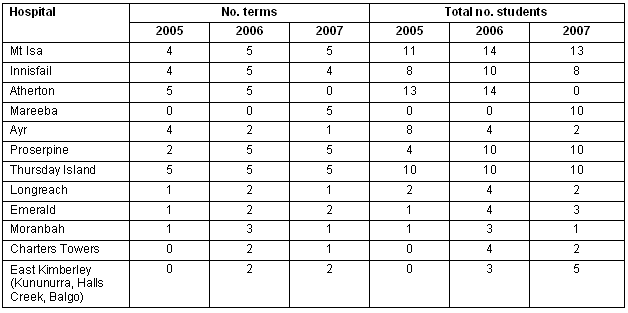
Sites were chosen for placements on the basis of demonstrated capacity to supervise and teach. A strong rural teaching network had been developed in the region at undergraduate and postgraduate levels since the North Queensland Clinical School was established in the early 1990s5. The majority of sites had a strong record of teaching medical students and general practice registrars, and were well known to staff at the school. Most were 2-4 doctor hospitals in rural/remote communities (rural, remote and metropolitan area [RRMA] classifications 4-7), although one larger hospital (Mt Isa, 35 doctors) and one smaller hospital (Moranbah, one doctor) were used6. Supervision was provided by experienced rural doctors (medical superintendents and senior medical officers), holding a Fellowship of the College of Rural and Remote Medicine (FACRRM) or equivalent. Sites used are listed (Table 1).
Table 1: Student numbers at rural internship sites, 2005-2007
Teleconferences were held with Medical Superintendents and key Queensland Health staff before and after the first rotation and at the end of each year. These provided an opportunity for two-way communication about the program and provided useful feedback. In addition, a program of site visits was undertaken.
Learning activities were centred around the clinical work, which was largely hospital-based, working as part of a clinical team. Most rotations involved experiences in Indigenous health, including time in an Aboriginal community-controlled health service, and in Indigenous communities. Other venues in which the students could gain experience varied between communities, including: private practices, visiting specialists, community health and volunteer groups, nursing homes, ambulance services, visiting allied health professionals, and aeromedical services such as the Royal Flying Doctor Service. Students were also encouraged to develop a deeper appreciation of their community through involvement with service clubs, giving talks to high school students, visits to local industry, and essential services. These activities served to emphasize the multidisciplinary nature of this rotation, with a wider focus than just medicine or health care.
The range of experiences available allowed students to apply, integrate and consolidate learning from all areas in a rural context, both vertically (across all years of the course with the opportunity to revise and apply principles of basic science) and horizontally (across all disciplines). Where students from different year levels overlapped in the same community, the senior students were expected to mentor the junior students.
Implementation of the rural internship included a compulsory pre-placement briefing, at which students were provided with copies of the student handbook and a checklist to work through ahead of time. Previous work at the school had demonstrated the critical importance of ensuring adequate preparation of the students, preceptors and the sites as perhaps the most important predictor of a successful rural placement7. Students who failed to attend this briefing were assigned a make-up activity. Communication with students during the rotation was by means of email, electronic discussion boards and two teleconferences in each rotation. Students were required to participate in a debrief session at the end of the rotation and to present their population health project to the remainder of their group.
Assessment during the rotation comprised 20% of the final mark for the year and contributed to the final grade. Fifty percent of the mark was derived from the student's learning portfolio, which included ratings by peers and supervisors (multi-source feedback or a '360 degree tool') and logs of procedures and clinical skills. The remaining 50% of the mark was rotation-specific and included a population health project (40%) and a telephone referral exercise (10%). Students working in groups of two to three had to complete a mock application for funding for a population health project relevant to their community, using an application template. This exercise involved considerable research and consultation to determine an appropriate choice of topics. Students had to submit the written proposal and prepare a brief oral submission (10 min presentation with a further 10 min for questions) to their peers. The telephone referral involved two parts. Students initially had to discuss an emergency case in which they had been involved with a staff member as a role play, in which they were discussing management of the case with the appropriate registrar or consultant at the base hospital. Students then had to generate an appropriate referral letter.
Evaluation of the program was largely qualitative, including student questionnaires, site visits and interviews, and follow-up teleconferences with preceptors. All students were required to complete a two-page questionnaire at the compulsory debrief session. A copy of the questionnaire appears in Appendix I. This feedback was used by the school, along with additional information obtained from students in the course of teleconferences and email communication as part of a quality assurance process.
All sites were contacted on a number of occasions each academic year by telephone, email and in person. An action research approach was adopted, whereby information was fed back to preceptors and staff as it was obtained, and incorporated into a quality improvement process. Data from students, preceptors and staff were used both to modify the program, and to develop insights into the learning activities and education impact of the rotation. The principles of grounded theory were used during the data collection process, building theory from data using the participants' own words and experiences8. This work was based on earlier research into the quality of rural placements and preceptors' supports needs7,9. These studies formally explored issues around rural placements in the earlier years of the course in similar communities across north Queensland.
Advice was received from the James Cook University Ethics Review Committee that formal ethics approval was not required, because data was de-identified and not able to be linked to an individual.
Results
The rural internship appeared to be an outstanding success, providing senior medical students with valuable experience by participation in the healthcare team. Students had an excellent, rich and varied clinical experience. They were made to feel welcome in each community, and worked closely with health professionals as part of the healthcare team. Feedback from supervisors was that students were able to contribute to the workforce under supervision, and that they enjoyed a positive clinical experience in a rural state health facility.
Students felt well prepared for their placements, with a number of positive comments on the helpfulness of the staff and the documentation. Preparation of the placement site and supervisor were also considered to be adequate, with a few initial teething problems noted in the first year that were then addressed. In particular, some information technology problems were rectified with local support and ingenuity, and some issues arose with last-minute change of supervisors, again resolved locally. Infrastructure and accommodation were regarded in all sites as at least satisfactory. Changes made in response to feedback included provision of bicycles on Thursday Island, where the accommodation was some distance from the hospital.
Students identified a number of successes and satisfactions with the placement. The staff in the rural sites were described by the students as great clinicians, committed teachers and inspiring role models. A number of preceptors were singled out by name for praise, while other students nominated groups of staff members (for example, registered nurses in the emergency department) as being particularly supportive. Students valued the chance to participate as a team member, thereby furthering their understanding of healthcare teams, and being able to accept some responsibility and manage patients with some independence. All students felt adequately supported and supervised, with an appropriate balance between supervision and independence.
Students also valued the excellent clinical experience and opportunities for learning. In particular, there were many opportunities to perform practical procedures and attend clinics and theatre sessions with visiting specialists. Students valued the many hands-on opportunities, and the ability to participate in health care, rather than just watch. The chance to implement a population health project, for example, developing clinical guidelines for use locally, was appreciated by some students.
Finally, a number of students commented on the warm welcome they had received from the healthcare team and the community, and how this contributed to a positive holistic experience that was much broader than clinical medicine. They appreciated the diverse opportunities available in rural medicine and the scenic beauty of many of the locations. A number commented that this was the best placement they had ever undertaken, and indicated positive influences in terms of career choices.
There were relatively few concerns expressed by students. Some related to initial difficulties with technology and accommodation, which were not unexpected in a new program and were managed locally. Other feedback was conflicting, for example, two students expressed dissatisfaction with accommodation at one site, while other students raised no concerns and thought it was satisfactory. Some students discussed concerns with staff about allocation to some of the more remote placements; once these concerns were addressed no student reported a negative experience. While the expectations of preceptors and academic staff of student workload was high (essentially, participation on the medical roster on a full-time basis), no students expressed concern about this aspect.
Supervisors were very supportive of the program . Some initially struggled with the concept of supervision of senior students who required less formal teaching and were able to contribute to patient care in a delegated way. Once these issues had been dealt with, staff were able to develop local models to keep the students busy with useful learning experiences that did not demand too much staff time. All preceptors were keen to accept more rural interns, with specific feedback from medical superintendents demonstrating rural interns were not a burden to the system in terms of teaching time and other resources. In most cases the students were making such a significant contribution to patient care that they were actually saving time for other staff.
Academic staff felt that the learning objectives of the program were met. Initially, considerable time and effort went into preparation of the sites and monitoring progress, although this diminished as the year progressed. The quality of the population health projects impressed staff: students understood the concept, were engaged, and developed a number of interesting and relevant project proposals that were of immediate practical use locally.
In summary, the rural internship program allowed students to accept limited supervised responsibility and further their ability and confidence to undertake the role of the intern. Importantly, they proved not to be a burden to the system. This rotation, therefore, appears to meet educational needs without compromising the local workforce (and indeed may add to it).
Discussion
This model extends and enhances the traditional apprenticeship-style approach by its rural focus, the distributed nature of the program, and involvement of the entire cohort of students. Students were able to meet the learning objectives of the rotation, and found the rural internship to be one of the most important clinical experiences of the final year of the course. In addition, students had opportunities to further develop clinical skills, and a deeper understanding of healthcare teams, and of rural communities. Students felt confident at the end of this rotation to undertake the role of an intern, and a number felt that the experience had influenced their choice of final career.
A distinguishing feature of the rural program at JCU is that all students spend at least 20 weeks on placement in rural towns and remote communities (RRMA 4-7). One of the main concerns for academic programs and clinical preceptors alike is the extent to which the clinical teaching load might compromise service delivery in rural settings, which are often overstretched.
In this respect, the experience with the sixth year rural internship in small rural hospitals has been gratifying. Both clinical supervisors and nursing staff report that students make a net contribution to the team and are missed when there are gaps between rotations. Placements of registrars and senior medical students in such settings on an ongoing basis appears to transform the role of the experienced rural medical practitioner to one of consultant, with teaching, team supervision and management of complex or difficult cases replacing some of the face-to-face patient care. The 'teaching health service' model appears highly appropriate to rural communities and is a key strategy for addressing future rural health workforce needs.
As the third major rural placement undertaken by all students in the course, the rural internship appeared to build on students' previous experiences. Students were well prepared for rural placements, being oriented to rural communities, and used to self-directed learning and working in teams. Careful planning of placements had to occur in order to ensure that accommodation and capacity to teach were not overloaded, and that preceptors had a balanced workload.
Preparation of the students, the preceptors and the communities again emerged as a key element of success. This is consistent with other literature, and reinforces the need for staff, rural sites and students to communicate and deal with issues that arise in a quality improvement framework7,9. Provision of written material ahead of the placement, including a pre-placement checklist, and insistence that all students participate in the pre-placement briefing, appear to be sound strategies.
Assessment strategies in this rotation were deliberately kept to a minimum, with a focus on students' immersion in their clinical duties, and documenting these. The population health project appears to have been successful in encouraging students to think more broadly about clinical problems at a population as well as individual level. The emergency referral also appears to have been a useful assessment task, encouraging students to develop an important skill without demanding too much student or staff time.
While the early evaluation of this program is positive, more formal evaluations need to be done in other settings. Much of the early evaluation has relied on self-reports; further evaluations could examine changes in knowledge, skills and attitudes, and on choice of career. In addition, further work needs to be done to determine if the issues relating to quality of rural placements and the training need of preceptors that arose in previous evaluations7,9 are still relevant in the context of the year 6 placement, with increasing student numbers and teaching load.
Conclusion
The rural internship model offers opportunities for students to have a high quality clinical experience in a rural setting. Students valued the opportunity for supported independent practice allowing the enhancement of clinical skills and confidence in preparation for deployment as an intern. The students also highlighted the importance of mentoring and supervision, the establishment of resources and networks on which they might be able to draw at a later time within their career, the acceptance and integration within the community - both the health community and the wider social community within the locations - and the fact that their input was valued. Students clearly expressed the view that this experience was of critical importance in supporting the developing confidence in their own ability, and in the training they had received, in order to be able to work effectively as part of the healthcare team.
This approach also provides a means to address an emerging paradox: rural preceptors and communities are keen to teach students and appreciate the long-term workforce implications, but are increasingly constrained by resources, particularly time. In addition, the contribution to patient care by senior students and junior doctors may lead to a consultant-registrar-resident model, in which experienced rural doctors function as consultants providing advice, support and tuition rather than predominantly face-to-face patient care10. This type of model means that students' clinical and educational needs can be met without placing undue pressure on an already stretched rural workforce. Similar innovative approaches should be explored in other settings.
Acknowledgements
This article is based on a paper presented at the 2006 General Practice Education & Training Conference, Hobart, Tasmania, Australia, and published in the conference proceedings.
References
1. Hays RB, Wronski I, Veitch J, McCloskey T. Intern choices for the first graduates of the James Cook University. Medical Journal of Australia 2006; 184: 94.
2. Sen Gupta TK, Grant M, Alberts V, McKenzie AJ, Veitch PC, Murphy B et al. The role of medical schools in recruitment and retention - rural, remote, Indigenous and tropical health at the James Cook University School of Medicine. In: Proceedings, ACRRM Scientific Forum/RWAV Victorian Rural General Practice Conference. 30 April 2002; Melbourne, Vic; 2002.
3. Hays RB. Rural Initiatives at the James Cook University School of Medicine: a vertically integrated regional/ rural/ remote medical education provider. Australian Journal of Rural Health 2001; 9(Suppl): S2-S5.
4. James Cook University School of Medicine program outline. Online (2007). Available: http://www.jcu.edu.au/medicine/programs/index.htm (Accessed 20 July 2007).
5. Hays RB, Sen Gupta T, Arlett K. Integrating general practice medical education - the North Queensland model. Medical Journal of Australia 1994; 160: 388-389.
6. Government of Australia. The rural, remote and metropolitan area (RRMA) classification system. (Online) 2006. Available: http://www.health.gov.au/internet/wcms/publishing.nsf/content/work-bmp-where-rrma (Accessed 20 July 20 2007).
7. Sen Gupta TK, Gupta S, Jukka C, Woolley T, Taylor L. Going bush - a chance of a lifetime. Key factors in ensuring the quality of 4- and 8-week rural placements for medical students. Report to the Rural Undergraduate Support and Co-ordination Program, Department of Health and Ageing, Commonwealth of Australia. Canberra, ACT: Department of Health and Ageing, 2004.
8. Glaser BG, Strauss AL. Discovery of grounded theory: strategies for qualitative research. Chicago: Aldine, 1967.
9. Woolley T, Sen Gupta TK, Thistlethwaite J. Effective and enthusiastic rural preceptors. What they need to know and what they need to have. An integrated approach to the support and training of rural clinicians who teach medical students on placement. Report to the Rural Undergraduate Support and Co-ordination Program, Department of Health and Ageing, Commonwealth of Australia. Canberra, ACT: Department of Health and Ageing, 2005.
10. Sen Gupta TK, Murray RB. Rural Internships for final year students. Medical Journal of Australia 2006; 185: 54-55.
Appendix I: Rural placement student feedback form

Abstract
Introduction: The James Cook University School of Medicine is the only complete medical school in northern Australia, and it has a mission to prepare graduates to meet the unique needs of the region with a particular emphasis on rural, remote, Indigenous and tropical health. Eight-week 'rural internships' have been undertaken by all sixth-year medical students at James Cook University since 2005. Each student had previously completed at least 12 weeks of structured rural placements in years 2 and 4, as well as other core teaching in rural health including the year 2 subject, 'Rural, Remote, Indigenous and Tropical Health'. Students worked in rural hospitals across northern Australia developing and practising clinical skills under the supervision of senior staff. Students undertook full-time inpatient and outpatient responsibilities under supervision, being rostered for after-hours work with appropriate support. Assessment involved a learning portfolio, including multi-source feedback from peers, supervisors and patients, and a population health project and a telephone referral exercise.
Methods: This article describes the development, implementation and assessment of the first years of the program, from 2005 to 2007. Evaluation included student questionnaires, site visits and interviews, and follow-up teleconferences with preceptors.
Results: The rural internship provides senior medical students with valuable experience by active participation in the healthcare team. Students reported a rich and varied clinical experience. Students accept limited supervised responsibility and further their ability and confidence to undertake the role of the intern. Importantly, they proved not to be a burden to the system. This rotation therefore appears to meet educational needs without compromising the local workforce (and indeed may add to it). Students felt welcomed by their communities and enjoyed the social and cultural aspects of their attachment, as well as the clinical aspects and the opportunity to further their understanding of rural communities, rural health care and the healthcare team. Preparation of the students, the preceptors and the communities emerged as a key element of success.
Conclusion: This model extends and enhances the traditional apprenticeship model by its rural focus and distributed nature, and involvement of the entire student cohort. In addition, the contribution to patient care by senior students and junior doctors enables a consultant-registrar-resident model, in which experienced rural doctors function as consultants providing advice, support and tuition rather than predominantly face-to-face patient care. This approach also provides a means to address an emerging paradox: rural preceptors and communities want to teach students, appreciating the long-term workforce implications, but are increasingly constrained by resources, particularly time. Similar innovative approaches should be explored in other settings.
Keywords: assessment, Australia, rural workforce, undergraduate medical education.
You might also be interested in:
2010 - Analysis of enhanced pharmacy services in rural community pharmacies in Western Australia
2010 - A tribute to John A J MacLeod
2006 - Funding sources and consequences: the subverting of an Indigenous community outreach program





