Introduction
The purpose of this study was to assess rural health care managers' understanding of rural community wellbeing. Specifically, definitions were sought for rural, community, health, wellbeing, and healthy rural community. Rural areas in many parts of the world are facing issues such as economic restructuring, environmental degradation, aging, and depopulation. These issues impact the health and wellbeing of the people living in rural communities. While research has attempted to better understand the constructs of rural1-4, determinants of health5,6, and models of rural health7-9, there is a gap in the understanding of the relationships between rural health and rural community. This research was concerned about how the individuals who administer healthcare services in rural areas define the areas they serve (rural, community), the conditions they seek to address (health, wellbeing), and the relationships between the two (healthy rural community). This research is rooted in the assumption that the development of healthy rural communities will be facilitated through an understanding of not only rurality, but also dimensions of good health10,11. In this context, it is important to examine how rural healthcare managers, those individuals in decision-making positions, construct and integrate various concepts such as rural, health, rural community, and their relationships.
Defining rural and community has been an ongoing debate in the social sciences since Hillery12 (1955) first documented over 90 definitions of community in the academic literature13. Developing models of health and wellbeing are also many and varied10,14. Factors affecting health and wellbeing are also well-established, particularly with respect to the determinants of health literature15,16. In a Canadian prairie context, the focus of this work has addressed both social capital as a determinant of health17,18 and indicators of, and factors affecting, rural community wellbeing19. Specific health issues have also been addressed; most recently, the impacts of living with HIV/AIDS in rural Alberta20. Previous research in southwestern Manitoba, Canada, undertook similar assessments based on focus group analysis of rural community members13,21. While community member perceptions are useful, it is also important to understand how the individuals who manage and allocate healthcare resources define such terms.
Although Canada is the second largest country in the world, 80% of its inhabitants live in urban centres. The Province of Manitoba represents the national average. According to Statistics Canada22, the 2001 population of the Province of Manitoba was 1.17 million people with two-thirds of this total living in the capital city of Winnipeg (Fig1). This two-thirds, unfortunately, suffer from the ('tongue in cheek') urban health problem of 'perimeteritis', a condition caused by living within the perimeter highway that bounds Winnipeg. As the second largest community in Manitoba, the City of Brandon (population 43 000) serves as a service centre for southwestern Manitoba. These services include manufacturing and retail, a university, community college, a full-service hospital with emergency and surgical services, and specialized health clinics. The rural region surrounding Brandon is served by 20 healthcare facilities located in smaller communities that range in size from 300 to 3300 people. This spatial pattern and density is analogous to that found in various Prairie and Great Plains jurisdictions of North America (eg Nebraska and Kansas in the United States; southern Saskatchewan in Canada). Healthcare delivery in the Province of Manitoba is managed through Regional Health Authorities (RHAs). Southwestern Manitoba (Fig1) is served by two health authorities. The Brandon RHA (BRHA) serves the city of Brandon. The Assiniboine RHA (ARHA) serves the rural areas and communities that surround Brandon. This article focuses on the ARHA, the more rural of the two. The following analysis examines how healthcare centre managers interpret subjects and concepts related to the context of their work: rural, community, wellbeing, health, and healthy rural community. The article concludes by relating these interpretations to the distinct rural-urban dichotomy that exists in the Province of Manitoba.
Methods
The research reported here builds on previous initiatives that included focus groups21, cognitive mapping13, secondary data analysis23, and in-depth interviews19. From this previous research, it was evident that healthcare managers represent an important dimension to social capital in rural communities in southwestern Manitoba. This has informed the current work that seeks to better understand the connections between the notions of rural, community, health, wellbeing, and healthy rural communities. This qualitative approach seeks to develop a more detailed understanding than a quantitative approach would offer, by giving voice24, to key actors in the healthcare decision-making process in rural communities. Seeking detailed descriptions and definitions of these key concepts is consistent with inductive logic and the use of in-depth interviews utilizing an open-ended format25, to facilitate a better understanding of commonalities and discrepancies among healthcare managers.
The research reported in this article is based on a set of interviews with each of the 20 healthcare professionals who either managed healthcare centers or administered specialized programs in rural healthcare centres in the ARHA. There were no refusals to participate, although one respondent terminated the interview at the halfway point. In addition, several respondents have shared responsibilities across communities. Because of the small numbers, issues specific to a particular community are not identified. The interviews used a semi-structured question format allowing for open-ended responses26,27. This approach was adopted to obtain respondents' knowledge of a range of terms and concepts related to rural community wellbeing (eg definitions of rural and community, indicators of rural community wellbeing, factors affecting rural community wellbeing, and prospects for the future). Because of the small number of respondents, information about rural roots, age, or previous life experiences was not obtained. Thus, it is not possible to assess the experiential concept of place or their sense of belonging to place. Respondents were asked, however, to provide their view on the prospects for the future of the community in which they worked. Most had concerns, including two who felt the community would not exist in 20 years19.
The interviews were conducted from February to April 2003. Interviews ranged from 30 min to 2 hours. All interviews were tape recorded and transcribed. No probing techniques were used to elicit information beyond that freely offered, as this would have affected the intentions of the interviews (ie, to obtain personal views on definitions and descriptions). Further, not using probes ensured that respondents were free to answer in the direction of their choice. The research conducted for this project was approved by the Brandon University Research Ethics Committee (BUREC). Due to the small number of respondents, in approving the project, BUREC expressed sensitivity regarding any reporting based on background information such as age, sex, education and rural roots. Having said this, it is possible to state that all but one of the respondents were female, and most were Manitoban and had varying levels of post-secondary education.
Results
Respondents were thoughtful and philosophical in their responses, but at the same time contextualized their comments within their professional responsibilities. This produced a rich array of definitions of rural, community, health, wellbeing, and healthy rural community. In doing so, the struggles for rural communities in southwestern Manitoba were highlighted.
Rural
Respondents provided a range of definitions of rural. To aid in the analysis, these have been categorized into two types: spatial community and community of interest11,13,28. The 'spatial community' is that which is defined by geography (eg municipal boundary, health region). A 'community of interest' is defined not by space, but by some common bond (eg feeling of attachment) or entity (eg farming, church group). Fourteen of the 20 respondents defined rural based on being outside a large urban centre. For example, Respondent 3 states that rural is:
...anything outside of the larger urban centres. I know that sometimes Brandon is considered rural, but I am not sure that it is rural anymore...it is more of a city. So anything outside a fairly big population base. Northern Manitoba does not seem to fit rural, it has a unique quality in itself, it is not rural to me but something different.
Similarly, Respondent 11 stated that rural is:
...an area that is outside of the city. Most people consider Winnipeg as the only city in Manitoba, but I also consider Brandon to be a city and Portage to be cities [sic] or some of those bigger areas that have a lot more amenities than the rural areas.
Others felt that Brandon was rural (Respondent 4). Three respondents specified distinctions relative to Winnipeg, the capital city of Manitoba, and four noted the importance of being 'outside of the perimeter'. That is, these seven respondents defined rural by stating it did not include Winnipeg or areas inside the perimeter. As noted in the introduction, approximately two-thirds (670 000) of the 1.17 million Manitobans lives in Winnipeg. A divided highway (ie, freeway or ring road) surrounds the city, and is known colloquially as 'the Perimeter Highway.' 'Perimeteritis' has recently been defined as people living in Winnipeg who lack awareness that anything exists in Manitoba, outside of Winnipeg29.
Not surprisingly, most specialized healthcare services are located in Winnipeg, with some specialized services located in Brandon. Respondent 16, for example, stated: 'I guess as much as there is "perimeteritis" one way or another it is anything outside of the perimeter of Winnipeg or outside of Brandon.' The reference to Brandon is consistent with previous research where rural residents noted that a smaller-scale 'perimeteritis' existed around Brandon13. The remaining six respondents offered interest-based definitions of rural, albeit each has a spatial element. Two respondents each described rural based on economic/employment aspects, the specific healthcare region and the service boundary. For example, Respondent 20 stated: 'rural is defined as any small group of people that live and work and play and serve in an area.'
Community
Whereas the definitions of rural focused on the spatial aspect, and tended to be brief, more variety and a greater level of detail was provided for definitions of community. The 20 definitions were placed into three categories: (i) spatial; (ii) interest and combinations of spatial; and (iii) interest. The spatial definitions were more basic in nature and degree, relating to specific boundaries and size. For example, respondent 10 stated: 'community can be geographic area. Sometimes [it is] referred to as a census community which is when people are working together as well'. A jurisdictional and spatial definition was also provided: '...community is every person living in this area or the area that the hospital would serve' (Respondent 13). Another, while more ambiguous, did refer to municipal designations: 'community defined from the health centre point of view includes the region ... the village and the surrounding municipalities' (Respondent 1). Further, this same respondent noted that community was: 'the town and surrounding areas. It goes a bit broader with regionalization and of course it is really broad now because we are Assiniboine, so our region, is all of Westman.' The regionalization of a range of services, including health, education, policing and emergency services is now common across rural Canada. Westman is a colloquialism referring to the southwestern corner of Manitoba (Fig1).
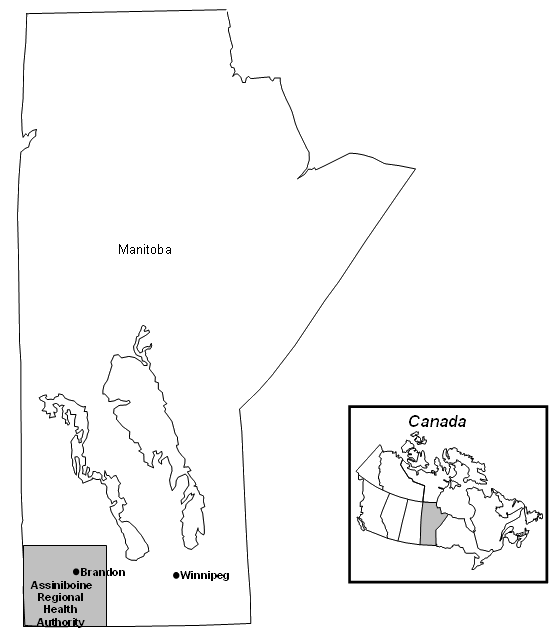
Figure 1: Map of the area discussed.
Interest-based definitions of community were similar to core aspects found in the literature, including sense of belonging, coming together for a common purpose, and feelings of closeness. For example, Respondent 16 described community as the following:
...to me, [community] is any grouping of individuals however big or small that come together for a purpose whether it be a community in your work, a community in your faith or a community in any organization. Community is people working together and multigenerational and in our rural areas we end up seeing much more of a multigenerational focus to that community.
Similarly, another respondent focused on family and place:
I look at community in various ways. I think that community can be the environment that you work in, the place that you live, community can be the household that you live in and just your family members. I define community in different ways or all of those ways. (Respondent 11)
Respondent 12 placed her definition of community within the health service context:
It is a place in which people live together to promote wellness in the community. The community is run by different organizations in order to make it work properly. A community is togetherness.
Other respondents noted both geographic and interest-based aspects in their definitions of community. For example, Respondent 8 noted that:
...a community can be any size. It is a group of individuals that make up various organizations that work towards the common good of everyone in the community. There is an old saying that it takes a community to raise a child and I believe that because a community is a variety of people, be it your teachers, your coaches, your daycare workers, your babysitters, the people at the grocery store. I believe that a community is a group of people that have a common interest and work towards achieving that.
Another stated: '...in some ways it is just a group of people that live in a specific geographical region, like a town or city...but it is also a sense of belonging to some place or some group' (Respondent 3). Similarly, Respondent 4 noted:
I guess it is a group of people with something in common, quite often that is location but it could also be extended beyond that to smaller groups. It could be a community of people like a church setting, a community program like the Lion's Club; it is defined differently for every person I think.
While it is common to believe that every individual has a distinctly different definition of community, as this research shows, definitions tend to be structured as either spatial or interest based.
Health
Following the descriptions of rural and community, respondents were asked the question: 'How do you define or describe health?' As indicated in the methods section, no prompts were used. Respondents had difficulty providing a comprehensive definition of health, with one respondent noting in her definition:
...health is an individual definition so health cannot be easily defined. My personal definition of health is one's mental, spiritual and physical ability to function. I practice my work holistically so health is a balance between the mental, spiritual and physical parts of a person. (Respondent 20)
While some respondents provided standard biomedical definitions, most referred to broader aspects such as wellbeing, determinants of health, and healthcare delivery. The simplest definitions included: '...health is a state of physical and mental wellbeing' (Respondent 10); 'The way that one feels or your general wellbeing' (Respondent 6); and '[health] is a person's wellbeing, which is physical, mental, and social' (Respondent 14).
Others related health to determinants, including the conditions in which people live (Respondent 17) and more specifically as a measure of determinants of health as articulated by Respondent 15:
There is the government things and the determinants of health that are all integrated and it depends on your economic background, your genetic background, and your financial situation. Health is a feeling of wellbeing without illness at the time.
Most respondents, however, included a range of elements to the definition of health, for example that articulated by Respondent 5:
There are many, many ways that it can be defined. It used to be absence of disease but that is no longer where it is at because we look at all the determinants of health. They are everything from having a job to having clean water to having knowledge and education and those kinds of things. I guess that health is a balance in life.
The notion of lifestyle was also present in several definitions, including gambling, smoking, diet, and exercise.
Wellbeing
Given that most respondents referred specifically to wellbeing in their definitions of health, is not surprising that there was repetition in responses to the question: 'How do you define or describe wellbeing?' Responses included specific definitions related to aspects of condition, including spiritual, mental, social, economic, physical. Others noted levels of satisfaction in life. Still others articulated specific determinants of health in impacting individual wellbeing. While most articulated individual measures of wellbeing, others felt '...it is personal thing. It is a feeling of being at peace with whatever your circumstances' (Respondent 5). More specifically, Respondent 1 stated that, wellbeing is, 'being able to have food, a place to live, a job and enough money to be able to feel that you are able to cope.' The overlap between health and wellbeing was also noted, for example:
Some of it is already what I have said in defining health. Wellbeing is how you perceive not how someone else perceives it. It is your own sense of how you feel. It encompasses all those things, not just physical but also mental, spiritual, social and even financial. For example if things are a little tight after Christmas your wellbeing might be affected because you are concerned about your financial affairs. It encompasses a lot of things but is mainly what an individual feels about it not what someone else tells them to feel. (Respondent 11)
This definition is useful as it takes a particular event that affects most people in southwestern Manitoba, Christmas, and illustrates how financial implications from the event can impact individual and family wellbeing. Together, respondents illustrated the complexities of wellbeing as a concept to which measures are applied.
Healthy rural community
The definitions of 'healthy rural community' were more detailed, apart from Respondent 7 who noted: 'I feel I have already answered that if you put together my answers to the previous questions.' Whereas definitions of health and wellbeing focused on condition and determinants of condition, definitions of healthy rural community tended to include actions to affect change. Respondents noted a range of determinants that require attention, including environment, education, economy, recreation, employment, health promotion, physical infrastructure, healthcare services, safety, religion, kinship, and basic needs (food, water, shelter). Whereas there were trends in definitions of wellbeing and health, each of the 20 definitions of healthy rural community proved to be unique. For example, Respondent 2 focused on leadership, recreational opportunities and young people:
I think healthy rural communities need some governance, be it your town or your RM [rural municipality] that is interested in making sure that their people have the dimensions that are affecting their wellbeing. Some of it starts with the people that you elect to look after you. I am more of a socialist in that I feel that there needs to be recreations for all, not just one specific group. It needs to be an affordable community to live in for all. I think it needs to look like we care about the babies and how they are being fed, the little kids and how their school bit is going. Sports teams for those who want to play on them. For teenagers a place to hang out. A healthy community needs to not just be a great place for seniors to live but a great place for everyone to live.
While Respondent 8 included recreational opportunities, the context of her definition began with creating a smoke-free environment:
It would be one that is absolutely smoke-free. A community that works towards the health of everyone be it smoke-free facilities for the children and everyone else. You have recreational activities for people to participate in, churches for people to participate in and attend for spiritual wellbeing, the economic resources for people to find and sustain employment that pays well enough for them to sustain a healthy lifestyle and obtain nutritious food, clothing and housing. I don't believe that simply having a facility [healthcare] bricks and mortar gives you a healthy community. It is the people in the community working towards a healthier outcome. Community health is very important in health promotion and disease prevention and communities need to work towards that and support those types of activities.
The future of rural communities was inherent in many of the definitions, which for some hinged on broader notions of social capital and rural development. For example, Respondent 15 described elements of inclusiveness, leadership and economic opportunity in her definition:
A healthy rural community is one that functions together for the general good of the entire community. They have volunteers that help out in various areas for the good of the community. A healthy community has excellent leaders who can make a team work rather than acting as a dictator. A healthy community is progressive looking and is always trying to find ways to bring economic development to their town or to improve what development they have. A healthy rural community encourages and welcomes newcomers and has available housing at reasonable prices. I guess that a healthy rural community is a community that thinks that it is a positive place to live and is not afraid to say it.
Service provision was also an element described to foster a healthy rural community, including religion (Respondent 20), and housing (Respondents 8 and 20). It was surprising that only six respondents specified healthcare services (Respondents 4, 5, 13, 16, 17 and 19). This emphasizes the fact, as noted above by Respondent 8, that a healthy rural community is more than the healthcare facility.
Implications for research
One concern about this study is the question: can these results be generalized to other rural areas? While we are confident in the results for southwestern Manitoba and we are confident that they provide cases useful to other rural areas, we do not believe they should be generalized to the rural world. Caution is always prudent in these areas. At the same time, it is clear to us that this research carries with it implications for health policy development, health program delivery, and healthy rural communities. For example, distinctions between metropolitan and rural areas need to be addressed in the context of overarching health policies, specific health program delivery options and in rural medical practice. For example, in recognizing the importance of healthcare services in rural areas, two communities within the ARHA, both struggling to maintain healthcare services, have recently articulated an agreement to pursue developing one larger healthcare facility and related services. This issue is substantially different from the Winnipeg Health Authority case that deals with issues such as whether to build new facilities or renovate older ones.
These implications are visible in issues such as rural healthcare centres closing and the difficulty in attracting healthcare professionals to rural areas. While these implications are beyond the scope of this study, it is our plan to address these issues in future research in light of the context established here.
Conclusions
The future of many rural communities in the Canadian prairies, particularly in southern Saskatchewan and Manitoba, is in question. Continually increasing farm size, and concurrent urbanization since the 1950s, has resulted in fewer people living in rural areas. Communities struggle to keep viable institutions (eg hospitals, schools, post offices) and businesses (eg hardware stores, gas stations, grocery stores). This study was a follow up to one that employed focus groups to obtain rural resident perceptions of rural, community, wellbeing, and health in southwestern Manitoba. The study reported on here argued that the specific views of healthcare managers were necessary to further illustrate the complexities in understanding definitions of community and condition. The results are consistent with previous research on this topic in southern Manitoba13,21 and the recent literature in that there are no universally accepted definitions of rural2,3, community30, wellbeing19,31, or health10,11,19. Further, the study illustrated that professionals charged with managing healthcare services in rural Manitoba maintain very broad definitions of health and wellbeing. Most significantly, the determinants of health and wellbeing were central to defining individual and community condition and quality of life. To reiterate, the views of healthcare manager are important because these are 'the' individuals responsible for making decisions that will contribute to healthier rural communities.
In returning to the title 'Perimeteritis and Rural Health', Manitoba is not unique. Examples can be found around the world, including the M25 around London, England, the outer perimeter highway of Atlanta, Georgia, and the North Perimeter Freeway around Perth, Australia. Healthcare issues, including healthcare delivery, certainly vary between metropolitan centres and their rural surroundings. What is perhaps unique in Manitoba is to have one city so dominant in population, and thus in services provided. This research has illustrated that living outside of Winnipeg has an impact on how people perceive boundaries, connections, health, and wellbeing. Because of these differences, understanding the issues and solutions also vary. This topic has been addressed in other Canadian jurisdictions32. A future extension of the research reported on in this article would be to conduct a direct comparison between urban and rural healthcare managers, healthcare practitioners and/or citizens concerned about healthcare services and delivery. That is, there are health issues distinct to rural areas. For example, there are challenges to providing services in depopulating regions and addressing individual and community health concerns specific to rural issues such as environmental change and condition. Responses to such challenges vary from cooperation between communities to merge their two small healthcare facilities into one larger, full-service facility, to the closure of rural health care facilities and demands to centralize.
References
1. Hoggart K. Let's do away with rural. Journal of Rural Studies 1990; 6: 245-257.
2. Halfacree K. Locality and social representation: space, discourse, and alternative definitions of rural. Journal of Rural Studies 1993; 9: 23-37.
3. Troughton M. Redefining 'rural' for the twenty-first century. In: W Ramp, J Kuling, I Townshend, V McGowan (Eds). Health in rural settings: contexts for action. Lethbridge, Alberta: University of Lethbridge Press, 1999; 21-38.
4. Ryan-Nicholls KD, Racher FE. Investigating the health of rural communities: toward framework development. Rural and Remote Health 4: 244. (Online) 2004. Available: www.rrh.org.au (Accessed 29 November 2007).
5. Hartley D. Rural health disparities, population health and rural culture. American Journal of Public Health 2004; 94: 1675-1678.
6. Frankish CJ, Moulton GE, Qantz D, Carson AJ, Casebeer AL, Eyles JD et al. Addressing the non-medical determinants of health: a survey of Canada's health regions. Canadian Journal of Public Health - Revue Canadienne de Sante Publique 2007; 98: 41-47.
7. Clarke L, Miller M. The character and prospects of rural community health and medical care. In: A Luloff, L Swanson (Eds). American rural communities. Boulder: Westview Press, 1990; 74-150.
8. Leduc E. Defining rurality: a general practice rurality index for Canada. Canadian Journal for Rural Medicine 1997; 2: 125-131.
9. Humphreys J. Delimiting 'rural': implications of an agreed 'rurality' index for healthcare planning and resource allocation. Australian Journal of Rural Health 1998; 6: 212-216.
10. Ramsey D, Smit B. Rural community wellbeing: models and application to changes in the Ontario Tobacco-belt. Geoforum 2002; 33(3): 367-384.
11. Kearns R, Joseph A. Restructuring health and rural communities in New Zealand. Progress in Human Geography 1995; 21: 18-32.
12. Hillery DA. Definitions of community: areas of agreement. Rural Sociology 1955; 20: 111-123.
13. Ramsey D, Annis B, Everitt J. Rural Community in Westman: theoretical and empirical considerations. In: R Blake, A Nurse (Eds.) The trajectories of rural life: new perspectives on rural Canada. Regina: Canadian Plains Research Centre, University of Regina, 2003; 1-10.
14. Wan T, Gill Odell B, Lewis D. Promoting wellbeing of the elderly: a community diagnosis. New York: Haworth Press, 1982.
15. Hamilton N, Bhatti, T. Population health promotion: an integrated model of population health and health promotion. Ottawa: Health Promotion Development Division, 1996.
16. Hancock T, Labonte R, Edwards R. Indicators that count! - measuring population health at the community level. Ottawa: Health Canada, 1999.
17. Gauthier DA, Diaz P. Rural adaptation and social cohesion for sustainable development of the prairies. Prairie Forum 2005; 30: iii.
18. Gauthier DA, Weiss S. Assessing performance: indicators, social cohesion and community sustainability. Prairie Forum 2005; 30: 313-328.
19. Ramsey, D, Beesley, K. Rural community wellbeing: the perspectives of health care managers in Southwestern Mantioba, Canada. Journal of Rural and Community Development 2006; 2: 86-107.
20. Groft JN, Robinson Vollman A. Seeking serenity: living with HIV/AIDS in rural Western Canada. Rural and Remote Health 7: 677. (Online) 2007. Available: www.rrh.org.au (Accessed 29 November 2007.
21. Ramsey D, Annis B, Everitt J. Definitions and boundaries of community: the case of focus group analysis in Southwestern Manitoba. Prairie Perspectives 2002; 5: 187-201.
22. Statistics Canada. Census of population, 2001. Ottawa: Supply and Services Canada, 2003.
23. Annis R, Racher F, Beattie M. Rural community health and wellbeing: a guide to action. Brandon: Rural Development Institute, Brandon University, 2004.
24. Ragin CC. Constructing social research. Thousand Oaks, CA: Pine Forge Press (Sage Publications), 1994.
25. Creswell JW. Research design: qualitative, quantitative, mixed methods approaches. Thousand Oaks, CA: Pine Forge Press (Sage Publications), 2003.
26. Iarossi G. the power of survey design: a user's guide for managing surveys, interpreting results and influencing respondents. Washington, DC: World Bank, 2006.
27. Peterson RA. Constructing effective questionnaires. Thousand Oaks, CA: Sage Publications, 2000.
28. Goldschmidt W. Large-scale farming and the rural social structure. Rural Sociology 1978; 43: 362-366.
29. Great Plains Staff. Perimeteritis. Encyclopedia of Manitoba. Winnipeg, Manitoba: Great Plains Publications, 2007. 529.
30. Wilkinson K. The future of the community in rural areas. In: K Pigg (Ed.). The future of rural America: anticipating policies for constructive change. Boulder: Westview Press, 1991; 73-90.
31. Larson J. The measurement of social wellbeing. Social Indicators Research 1993; 28: 285-296.
32. Pampalon R, Martinez J, Hamel D. Does living in rural areas make a difference for health in Québec? Health and Place 2005; 12: 421-435.

