Introduction
Since the 1950s in developed countries, there have been more suicides among farmers than among other professions1,2. Among farmers, suicide is characterized by an overuse of highly lethal means: firearms in the UK, Scotland and Australia3-5, hanging in France and Switzerland6-8, and ingestion of phytosanitary products in India and Taiwan9,10. Many researchers have tried to understand the reasons for this higher risk. Concerning the link between suicide and psychiatric pathologies, results vary between studies. Some suggest that it is not correlated with a higher prevalence of psychiatric disorders. In the UK, fewer psychiatric disorders were found to be diagnosed in farmers than in the general population11. In Norway, depression scores have been shown to be higher for farmers than for the general population, whereas anxiety scores were similar12. In study in the Midwest of the US, no link between increased depression or anxiety scores and increased suicide rate was found13. However, in Switzerland, Schmid et al found that farmers have a higher incidence of mental illness and addictive disorders than those in other professions14. The high suicide rate may also be associated with low level of education and the high percentage of single people in this population15. The multiplicity of individual, social and environmental factors could also be reported: isolation, low income, workload, divorce or family conflicts, fear of community stigmatization if help-seeking, ‘self-stigmatization’ (self-judgement, and being a ‘strong’ man as a limitation to seeking help)16.
Therefore, despite their many difficulties, farmers remain alone and do not seek help. In Australia, farmers are less likely to consult a GP or a psychiatrist17. In England, 22% of farmers who committed suicide had consulted a GP in the 3 months before the act3. Among them, 27% mentioned mental health difficulties, a rate not significantly different from that in the general population.
In France, farmers represent 1.8% of the working population, a percentage that has been declining. An exhaustive cross-sectional study in France from 2007 to 2011 found a higher suicide mortality rate than in all other active socio-professional categories, particularly for the dairy and beef cattle sectors6,18. All French farmers are affiliated to a compulsory social security system (Mutualité Sociale Agricole, MSA) that also collects their social security contributions. This organization has developed several schemes to help farmers in difficulty: discussion groups, retraining assistance, subsidy for a replacement, and an anonymous telephone helpline. Moreover, most farmers are registered with a GP and receive reimbursement for medical consultations and treatment costs. Yet, French farmers consult their GPs less often than other workers. A study found that 14.3% of French farmers decided not to see a doctor in the previous 12 months, mainly due to lack of time19.
In many countries, the suicide rate is higher among farmers than in the general population, but farmers seem to seek help less frequently. In this context, suicide attempts, which are often unique and lethal, are very difficult to prevent20.
No study has been carried out on French farmers’ perceptions about available help. Brittany is one of the French regions with the most developed agricultural sector and with a high suicide rate18. Within the region, one department, Ille et Vilaine, many farmers are in the dairy cattle sector. The aim of this study was to analyse the perceptions of farmers in this department about suicide and the help offered to farmers at risk of suicide.
Methods
Study design
This qualitative study investigated farmers’ perceptions using semi-structured interviews according to a reflexive thematic analysis in the framework of an inductive approach21.
Recruitment
The source population was farmers (cattle breeding) working in the Ille et Vilaine department.
To recruit them, flyers presenting the study were distributed at agricultural events. Emails were sent through farmers' organizations. Contacts were made with farmers in medical practices.
To be included in the study, each individual had to be a farmer in Ille et Vilaine and consent to the study's terms.
Farmers were recruited using various means in order to ensure a varied sample in terms of age, gender and farm type. The sample was enlarged by snowball sampling: interviewees were given the researchers' contact details, so that other farmers could contact them to take part in the study. Only one farmer responded to a written invitation by email; the other farmers were recruited by telephone call or direct contact. There was no set number of interviews before we started. As the interviews progressed, we tried to vary the sample (age, gender, farm type) in order to diversify the points of view.
Data collection
Data were collected in individual face-to-face interviews. An interview guide was prepared using a rigorous procedure based on the analysis of the existing literature and after exploratory interviews with two psychiatrists, an occupational physician and a farmer organization member22. It was validated by the entire research team (Appendix I).
The first questions concerned each farmer's professional background. Then, the farmer's health was discussed. The topic of suicide among farmers was raised in a general way, and then some questions focused on the help schemes known by the interviewees and that they would recommend.
Interviews took place in a quiet place chosen by the farmers, either at their home or at work. The two interviewers (ED and AP) were supervised by a senior researcher (LF).
Prior to each interview, written informed consent was obtained. Interviews were recorded and field notes were taken by the interviewers regarding silences and non-verbal communication. The interviewees were free to end the interview at any point during the interview.
Data analysis
The audio-recordings were transcribed verbatim, using Microsoft Word, taking into account silences, nuances and non-verbal communication. Data were anonymized at the transcription stage. Any information that could identify participants was removed during the transcription to ensure anonymity.
A thematic analysis following Braun and Clarke's inductive approach was conducted with their framework21. A verbatim analysis was carried out using the NVivo software. The transcripts were read by the two interviewers (ED and AP) at different times. Data familiarization is the first step of analysis, and both researchers performed the interviews. Each interview was transcribed in full by the researcher who conducted the interview. Each researcher coded the interviews manually and individually. Then, themes and subthemes were generated using the codes and they were reviewed by the research team. After an iterative process and discussions, in an inductive approach, a coding framework was constructed. After 24 interviews, sufficient and rich information was obtained to identify solid themes and to analyse the research question, as described in the Braun and Clarke approach21. The last two interviews reinforced the thematic analysis process23. The researchers considered that they had enough material after 26 interviews to write the report24.
Ethics approval
The study was approved by the Rennes University Hospital Ethics Committee, Rennes, France (18.112).
Results
Between January 2019 and March 2020, 26 interviews were conducted with farmers. Among them 19 were men and most were aged between 45 and 55 years. Their education level was heterogeneous (Table 1). To ensure participant anonymity, we assigned a French first name that corresponded to the interviewee's gender and age. All interviewed farmers had at least one parent who was a farmer. Moreover, they all knew a farmer who had committed suicide, either a relative or a colleague. The interviewed farmers spoke at length about their view on suicide, through their own or a colleague's experience of suicide.
The reflexive thematic analysis of the interviews highlighted three major themes that included subthemes (Table 2): (1) farmers' perceptions about suicide (2) suicide risk factors identified by the farmers and (3) perceptions about the available help schemes.
Table 1: Characteristics of the sample (n=26)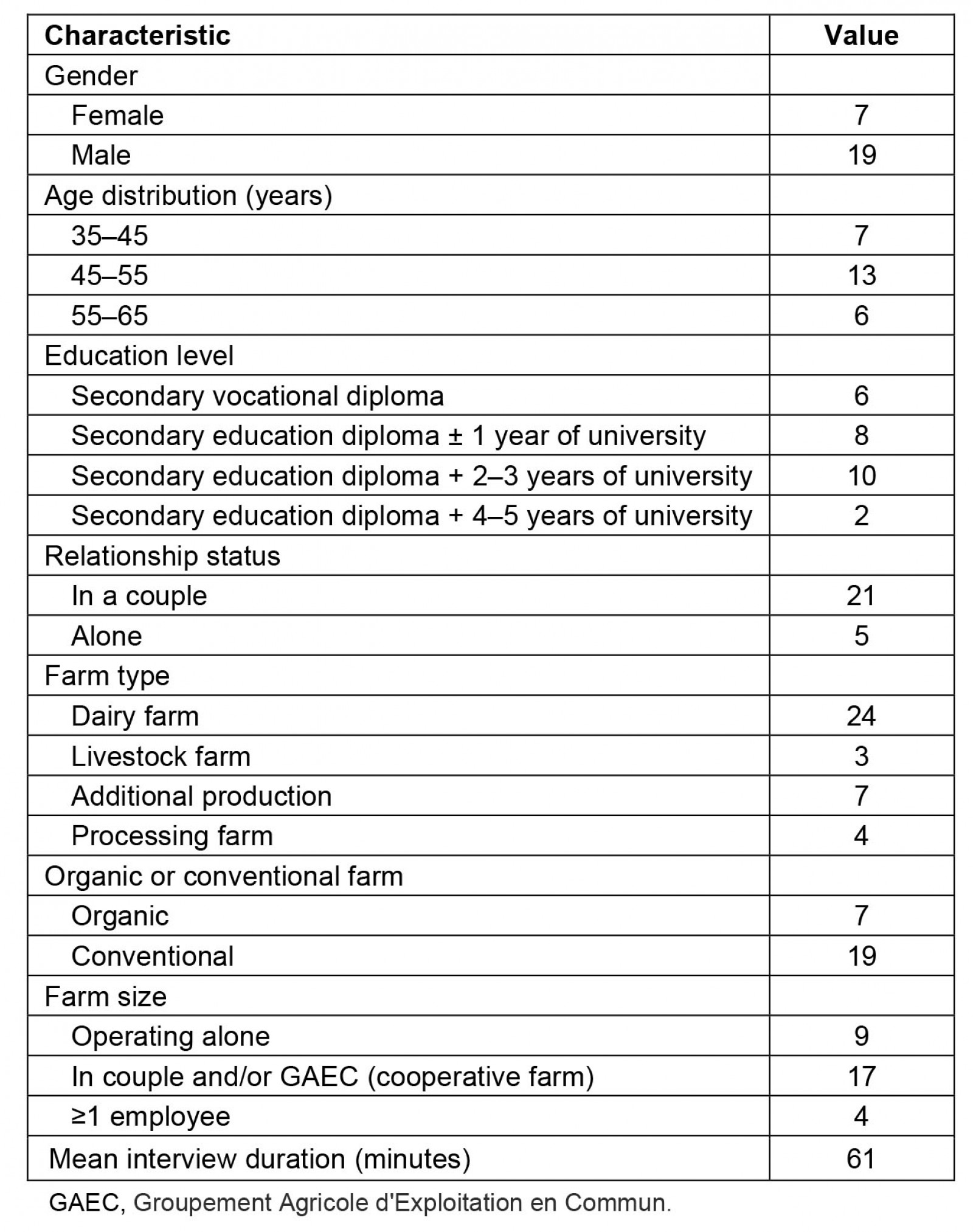
Table 2: Identified themes and subthemes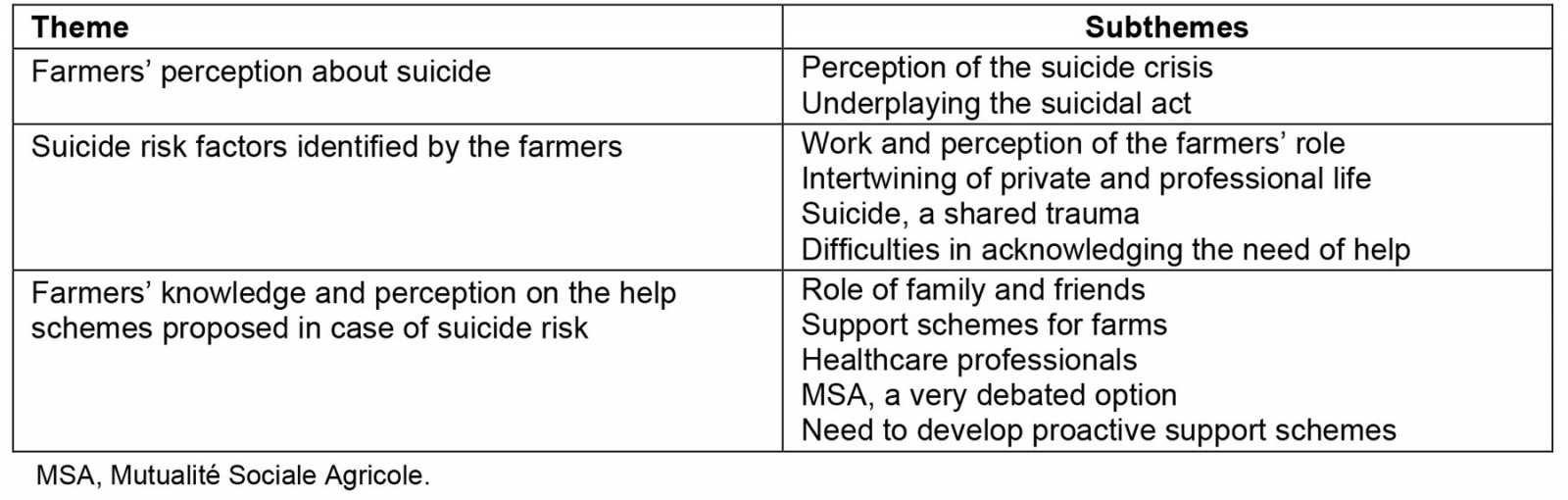
Farmers’ perceptions about suicide
Perception of the suicide crisis: The interviewed farmers demonstrated a strong understanding of the symptoms of suicidal crisis. They were often the initial witnesses, either experiencing the crisis themselves or observing it in someone close to them. Recurrent symptoms included fatigue and insomnia, while other psychological symptoms were occasionally mentioned, such as ‘stress’ and ‘aggressiveness’. They also evoked libido problems and various signs suggesting clinophilia or abulia. Some used the terms of ‘depression’ and ‘burnout’.
They identified common characteristics in relatives at risk of suicide or who committed suicide: personal and family psychiatric ‘history’, childhood trauma, ‘depression’ and ‘impulsivity’.
The coexistence of various characteristics was underlined, suggesting a multifactorial nature. Carelessness, increased alcohol consumption, suicidal conversations, disintegrating social ties, serenity before the act or abnormal behaviour were among the indicators that could have raised concerns before the event.
Underplaying the suicidal act: Far from considering it a taboo subject, the interviewed farmers understood that people can commit suicide. One male farmer (Vincent) told us, ‘The only solution they found is this one.’ Some confessed that they also had suicidal thoughts, for instance Olivier: ‘But, pfff ... I'll stop everything, I'll go over to the other side and that'll solve everything’. Sometimes, various scenarios were planned including hanging, insulin injection, car accidents, falling from heights and the use of firearms. Different perspectives were expressed: some believed that suicide was only for individuals with a ‘suicidal temperament’, while others denounced the occurrence of suicide among farmers.
Suicide risk factors identified by the farmers
Work and perception of the farmer’s role: Work was frequently linked with mental health in these discussions. A kind of destructive cycle existed between work and depression. Virginie, a female farmer, identified a link between the welfare of farm animals and her own health: ‘Your cows aren't well, you're not well’. When farmers' morale was low, it hindered their ability to work effectively. The burden of everyday tasks, along with feelings of weariness, created difficulty. Professional constraints were cited as the main cause behind an increased suicide risk, according to interviews conducted with farmers. The constraint of a low income was frequently mentioned, as well as the fear of losing essential subsidies.
The profession's lack of recognition by society was emphasised by Benoît, who stated, ‘No one really understands what we do’. Moreover, the increased significance of the insufficient recognition compared to the past was mentioned:
So, we're not recognized by society, we're full of debts, we're overworked, we have no income and on top of that we're told every day that we work badly because we pollute. (Chantal)
The criticism of ‘farmers, polluters’ seems to impact some farmers, such as Chantal. Nonetheless, a female farmer highlighted the positive developments in consumer expectations.
Intertwining of private and professional life: Among the interviewed farmers, the work and rest dimensions were often intertwined with many working as a couple or among several generations. This sometimes led to tensions, particularly when the farm was handed down from parents to children:
If we wouldn't have the boys who wanted to settle down or take over ..., we'd probably have less pain, less stress. (Jean)
Suicide, a shared trauma: Suicide was a shared trauma among the farmers, with each interviewee discussing the suicide of a colleague or loved one. After these experiences, the farmers felt a range of emotions including anxiety, anger, sadness, discouragement, powerlessness and guilt. Benoît reflected, ‘… maybe we didn't provide him with the help he needed, so we questioned ourselves.’ The farmers also expressed concern about the possibility of suicide being hereditary. Olivier said, ‘But in this case, it was hereditary: her son, who wasn't a farmer, also committed suicide’. According to a female farmer, the media coverage of suicides among farmers could be an additional risk factor.
Difficulties in acknowledging the need for help: Barriers to expressing psychological pain or suicidal ideas were identified. Some farmers appeared to downplay their own discomfort, as one farmer (Guillame) said: ‘I wasn't doing well compared to what I was before. But I hadn't gone downhill, I was still a long way from being really distressed’. Female farmer Chantal explained this apparent difficulty in verbalizing, stating, ‘So, I also think there's a bit of a model that in agriculture you can't complain ... Especially men, for that matter.’ The questioning of the purpose of verbalizing their pain was evident. One farmer (Virginie) expressed fatalism: ‘But when you get to that point, what do you want him to do? What? He's dead’. Additionally, discussing psychological distress was perceived as a possible aggravating factor, as Guillaume said: ‘Well, the problem is that you shouldn't always talk, ... because it's never good’. There was a great reluctance to seek help and discuss their difficulties. Finally, some farmers expressed uncertainty about resources, where they could go for guidance or support. One farmer (Jean) said, ‘But when you're in a bad way ... you don't know where to go sometimes’.
Farmers’ knowledge and perception of help schemes proposed in case of suicide risk
Paradoxically, while farmers described signs suggestive of distress or precursor to suicide, they did not know much about the help schemes and how to use them.
Role of family and friends: When asked about how to cope with psychological problems, farmers very often mentioned family members and friends, and especially their spouse, as the first source of support, as someone who ‘understands our problems well’. They helped them to share tasks in case of overwork, and also to spot difficulties.
Sometimes, the interviewed farmers said that they wanted to protect those around them who had already been deeply affected by suicide. ‘What's more, I made an effort not to show that I was mentally unwell’, said Nathalie. Others, such as Olivier, felt misunderstood: ‘People around you say you're depressed. But I'm not! You can't get demoralized!’
The neighbouring farmers had mixed feelings towards the farmer who was facing difficulties. While they could offer support, they could also benefit from the departure of the struggling farmer, such as expanding their own farm. As the saying goes, said Guillame, ‘Your own enemy is often your neighbour in agriculture!’ Additionally, pride in the profession may prevent farmers from seeking help from their peers, as Xavier notes: ‘There are hidden miseries’.
Support schemes for farms: The interviewed farmers linked improvement in their farm's financial situation to feeling better mentally. The role of the accountant and banker varied depending on the interviewee. They could provide assistance in a difficult financial situation by granting a life-saving loan. Estelle said, ‘The banker saved me’. However, others viewed them as an additional source of problems, worsening their debt burden. According to Virginie, ‘They lent money any way they could and pushed people ... into catastrophic situations!’
In times of difficulty, farmers turned to employees or agricultural contractors for support. Cooperatives that allowed for the sharing of farm equipment served as both a practical aid and a forum for exchanging with other farmers.
Training courses or meetings with colleagues were seen as helpful. According to Ludovic, it was the occasion to ‘think globally about production costs, organization, work efficiency ...’, as well as for motivation. All participants stressed the value of these different actors as a protection against loneliness, and as an alarm bell in case of extreme situations. For some farmers, associations specializing in supporting farmers in difficulty were the last option. Lastly, stopping farming was rarely seen as a solution. ‘Often, a farmer is a lifetime project’, said Stéphanie.
Healthcare professionals: Most farmers reported irregular visits to their GP, mainly due to limited access (low number of GPs, lack of time) and not feeling the need. The tendency to wait for illnesses to resolve on their own was noted; as Simon said, ‘We wait till it goes away’. They only consulted their GP for somatic problems that interfered with their work. ‘For me it's silly, but medicine is more physical’, said Estelle.
Some of the interviewed farmers said that they could discuss their distress with their GP. Michel said of his GP that he wanted to ‘find someone who listens to me’. It was also because the GP systematically asked about their wellbeing during the consultation. Laurent said, ‘And he always asks the right questions: 'Are things going well in your couple? In your job? ... Is it going well? Tell me about it.’’ Farmers appreciated the care offered and the time devoted by healthcare professionals. Laurent reported, ‘And my doctor at the time reacted extremely well ... we talked for one hour’.
Some farmers did not feel the need or interest to seek health care. Guillaume reported, ‘In other words, I still felt capable of coping with everything on my own’. Chantal explained this low healthcare utilization: ‘People who are treated are again the people who have the psychological means to go and see their doctor’. Additionally, some farmers did not trust the medical profession.
It is worth noting that most farmers did not consider psychiatrists or psychologists as a possible option. They said they found ways of coping with their bad feelings on their own. Nathalie explained, ‘And it's true that when things aren't going well, especially in spring when I'm tired, I go outside’.
Those who mentioned mental health care used negative language such as ‘internment’, ‘psychiatric patient’, ‘locking up’, ‘isolation’. Eric even said, ‘Psy means crazy, well, a bit disturbed’. Three farmers had already consulted a psychologist or psychiatrist. Some farmers had recognised the importance of their psychological wellbeing and the need for treatment.
Eric suggested regular check-ups: ‘I think that regular check-ups with a therapist may help to tidy up the clutter in the office and make it easier to empty the mind, and at least to find one's way around’.
MSA, a very debated option: According to interviews, the main role of MSA was to collect contributions; as Estelle said, ‘They're mainly there to take the dough’. They mentioned the low subsidies granted by MSA during sick leave. Some farmers felt cheated by contributions they found disproportionate relative to what they earned, especially given the low pensions in their profession.
Few farmers considered MSA as a possible option in case of psychological distress. The psychosocial hazard prevention unit and its various schemes were little known. Bernard highlighted the lack of communication: ‘I think that the MSA is really to blame, it's not normal that there isn't more communication, support, and help.’ Some farmers received benefits from one of the MSA support schemes on an ad hoc basis, which they appreciated (paid time off, free psychologist sessions). However, they still had a negative perception of this social security system. Some insisted on the lack of consideration shown by MSA doctors – particularly one, who was described as having ‘zero consideration’.
Farmers have complained about administrative difficulties in obtaining subsidies, lack of communication about the available help schemes, and long response times.
Need to develop proactive support schemes: The interviewed farmers proposed schemes to improve their quality of life. First and foremost, they wanted to be the primary actor in their wellbeing. Laurent said, ‘I need to find solutions for working less’. They expressed a desire to take time for themselves and identified isolation as a barrier to getting help. Chantal explained, ‘When you're ill, you think more about isolating yourself than going to see someone’. Therefore, it was emphasised that proactive interventions should be developed due to the low spontaneous demand for help from colleagues experiencing difficulties.
Discussion
This study on French farmers' perceptions about suicide and the available support schemes highlighted some novel results. Farmers had a good knowledge of suicide, its risk factors and the signs that precede the suicidal act. Paradoxically, while some expressed suicidal thoughts, they did not feel at risk of suicide because they did not have a ‘suicidal temperament’. In case of difficulties, farmers first sought support from those around them, particularly their spouse. An improvement in a farm's financial situation was an important factor to boost their mental health. Participation in groups or training courses was also an important help. Sometimes, they thought about seeing a healthcare professional, particularly their GP, but not everyone saw the usefulness of this approach. Mental health professionals (psychologists and psychiatrists) often had a bad reputation, like the MSA, despite the help offered. All participants spoke of the need to offer proactive help to farmers, aware of the low spontaneous help-seeking by colleagues in difficulty.
The interviewed farmers listed many anxiety–depressive symptoms, particularly fatigue and insomnia. In France, 75% of surveyed farmers found their work mentally tiring and 51% reported insomnia19. The importance of these physical symptoms can be visualized as a body reduced to being a mechanical tool. Symptoms are considered only when they impair the ability to work: ‘I’m no good. I can’t do anything’25. Conversely, other symptoms seemed to be minimized, particularly by male farmers. Indeed, expressing one's emotions contradicts the agricultural ideal of a strong, hard-working man who does not complain: ‘This stoicism, or manner of ‘hiding’ or ‘bottling up’ mental health struggles, particularly among men’26. This can be extended to the specific expression of depressive symptoms by men. When depressive symptoms are present, people may find other explanations for their presence. Depressive symptoms, fatigue and irritability are more likely to be related to possible physical problems27. In our study, this paradox was expressed by several farmers with the idea that suicide was something that occurred only to people with a predisposition, described by the term ‘suicidal temperament’, although they mentioned suicidal ideas. Suicide was seen to concern others, and to represent a form of weakness. These specific features in the description of psychological pain by farmers may partly explain the low prevalence of depressive symptoms11,13.
The interviewed farmers highlighted the difficulties inherent to their profession: isolation, new laws, financial difficulties, long working hours, longer time spent on administrative tasks, and reliance on subsidies16,19,28-30. Some of the interviewed farmers had suffered due to the consumers’ criticism concerning the use of phytosanitary products and livestock farming. One of the most important stress factors for dairy farmers in Finland is ‘the treatment of farmers in society and the media’31. These external factors can lead farmers to question their job, about which they are ‘passionate’, or lead to ‘cynicism’, one of the burnout components.
All interviewed farmers described the case of a colleague or relative who had committed suicide. The high prevalence of suicide among farmers and the intense professional and personal links among farmers in the same geographical area may explain this finding6,18. Experiencing the suicide of a colleague was a traumatic experience for the interviewed farmers, with psychological consequences. Indeed, the suicide of a family member or a colleague has negative health consequences: depression, post-traumatic stress disorder, psychiatric hospitalization and suicide depending on the relationship with the victim32. Suicide representations after this experience changed. Suicide becomes more real, or even a possibility. For others, the consequences for the loved ones might prevent them from attempting suicide33. In our study, some farmers understood why a close family member or a friend had committed suicide, but at the same time they were dismayed by the consequences for the family (financial burden and bereavement).
The experience of a farmer's relative committing suicide can serve as a basis for preventive actions. Actions targeted to the younger farmers seem promising. A study conducted among students at an agricultural high school in Brittany, France, suggests that mental health education could facilitate early treatment by breaking down barriers to healthcare utilization, particularly stoicism34. The interviewed farmers strongly asked to be autonomous and to take proactive actions, as shown by other studies35. Suicide prevention training sessions have been tested with active farmers. This system allows primary prevention by deconstructing the obstacles to help-seeking by the trained farmer, secondary prevention through the identification by the trained farmers (ie sentinels) of colleagues in distress and referring them to professionals, and postvention by limiting the feeling of powerlessness and guilt through the empowering of the farmer who witnesses distress36. The interviewed farmers highlighted their spouse's protective role. Studies indicate the dual function of family and friends: serving as support in challenging times, but also as a potential source of stress in case of conflict or divorce16,17. Investigating the interplay between professional and private life in business transfer or establishment can potentially optimise support by assigning a supplementary role to family and friends.
GPs are often the only healthcare contact for farmers. Healthcare foregoing was a reality, 14% for lack of time, fear of the diagnosis or lack of accessibility19. Yet, some farmers who committed suicide had consulted a GP before the act although often just for ‘physical’ symptoms (31%)3. GPs could improve the identification of farmers at high risk of suicide by conducting a targeted and systematic screening for mental health problems in this population. It is recommended that GPs receive training in questioning farmers.
Based on our study, prevention initiatives should be grounded in farmers' existing knowledge of suicide. This will help to break down preconceived notions, particularly regarding mental healthcare and build upon their current understanding through active education principles. Strengthening the role of families, especially spouses, is crucial for effective prevention initiatives.
Strengths and limitations
This study examines farmers' perceptions of suicide. The exchanges were lengthy and rich, and the quality of the farmers' welcomes demonstrated their interest. In terms of the population that was interviewed, the sample could have been more varied in terms of age and parental profession. It can be challenging to reach younger farmers, who may have less time or be less willing to discuss suicide. It would be interesting to explore this issue with farmers under the age of 35 years, as a greater proportion of young farmers do not have a family member who is also a farmer. The educational level could also be questioned.
To strengthen the internal validity of the study, the research team was involved in the analysis of the interview data. The two researchers who conducted the interviews, AP and ED, are GPs. Their profession could have limited the discussion with farmers. However, their familiarity with the farming community was an advantage in interviewing the farmers. This is their inaugural qualitative study. Although there may have been some biases, the reflexive team approach allowed them to remain as objective as possible.
Conclusion
This study shows that in Britany, farmers are well aware of suicide, its risk factors and the warning signs that precede the suicidal act. Yet help-seeking seemed difficult and healthcare professionals, particularly mental health professionals, were not regarded well. Proactive help schemes were mentioned as a tool for suicide prevention. The support schemes offered by the farmers’ social security system were also not regarded well. This raises the issue of proposing adapted support services outside these structures. The training of primary care professionals and of agricultural sector actors should be developed. Additional studies to assess the effect of specific training for primary care professionals are needed to better manage the farmers' physical and mental problems.
Acknowledgements
We would like to express our gratitude to all the farmers who participated in the interviews.
Funding
This article is supported by the French network of University Hospitals HUGO (Hôpitaux Universitaires du Grand Ouest). The authors thank Elisabetta Andermarcher for providing editorial assistance in the preparation of this article.
Conflicts of interest
No potential conflicts of interest were reported by the authors.




