During January 2001, a mission to Somaliland was initiated by a comercial company. During their visit, a physician (MLA) was cordially invited by the Minister of Health (AADA), to evaluate the health care system and to find ways to assist the Somaliland authorities in health care delivery. The reason for this field trip was economical, but the health care aspect was seen as part of the project.
Methods
Meetings with several government officials were conducted, and apart from spending time in Hargeisa, we traveled to Berbera, Sheikh and Borau. We had the opportunity to visit several health care facilities in these places. This report is based on these experiences.
Country background
Somaliland is a self-declared state, not recognized by the nations of the world (Figure 1). Independence from the Republic of Somalia was declared 10 years ago, and fighting for independence has gone on for several years, resulting in the destruction of the infrastructure of the country. Currently, the country is run by a government headed by President Mohamed Haji Ibrahim Egal. The country is large and the terrain varies from desert coastal plains to high mountains and a high plateau (1700 m) with acacia bush, home to more than 7 million goats and sheep, and 5 million camels.
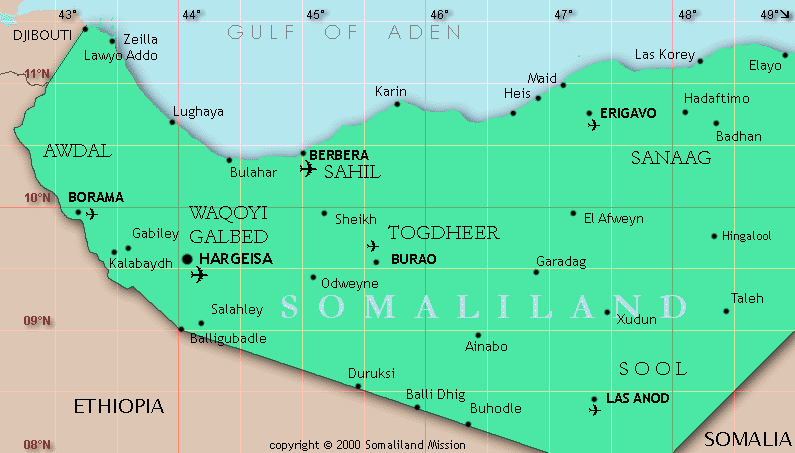
Figure 1: The self-declared State of Somaliland.
The Population
Somaliland has not had a census, and population estimates are difficult for the following reasons: Returning refugees1, internally displaced citizens, citizens of Somali ethnicity who reside in neighboring countries seek medical care and other benefits in this relatively newly established country. These factors are the reason for the diversity of figures quoted regarding the population size and composition. It is likely that Somaliland has approximately 3 million people, 30% of whom are semi-nomadic shepherds, 30% are small scale farmers, and 40% live in towns and cities2.
Economy
GNP (gross national product) and other data are not available. A recent report on the southern region reveals that people are poor, and they depend on livestock3.
Approximately 50-75% of the income of the poor is spent on basic food (including sugar, wheat flour, oil and meat) and non-food items. Calorie and protein intake are not always adequate. Other expenses include soap (8 pieces per month, approximately $30/year [all values are US$]), clothes ($35-45/year), schooling and, kerosene (approximately $35/year). Veterinary and human drugs are selectively purchased depending on available income at the time and the situation, but may range from $70-90/year. Tractor hire (8-15 hours at $4-6 per hour) represents $30-90 per year.
There may also be some expenditure on khat, which is an intoxicating leaf chewed by inhabitants of the Horn of Africa and Yemen, particularly on Thursday afternoons and Fridays. Details of expenditure on khat have not been assessed. In some areas money may also be spent on water for livestock in the dry season.
The economy is based on the export of live goat and sheep to Saudi Arabia, where they are slaughtered for sacrifice during the pilgrimage to Mecca (The Haj). A recent ban on livestock from Africa was instituted by the Saudi Government because of cases of Rift Valley Fever in East Africa, and the possible transmission through infected animals4.
Trade of small livestock usually is for one of the following purposes: gifts, payment of debts, rehabilitation of the house, purchase expensive clothes for women, marrying another wife, or payment to Koranic school teacher. Animals are slaughtered as part of the prayers and ceremony associated with the birth of a child, circumcision celebrations for boys and girls, visits by relatives, or religious festivals and holidays.
The average household size is between 6 and 8 people. A family will have 0.5-1.5 ha cultivated land, yielding 0.25-1.125 t staple food/year; 1-3 cows and 5-8 goats or sheep3.
Health care system
There is a public sector run by the ministry, and a private sector, which is independent. The exception is the maternity and pediatrics hospital in Hargeisa, which will be described in detail. The visit was to the public sector: the Hargeisa Group Hospital that serves as the national medical center. There are five district hospitals, each supervises 5-6 health centers, which have responsibility for a total of 125 health posts.
The country is served by 100 doctors (1:30 000 population, similar to the situation in other countries in the Horn of Africa). There are about 300 nurses (1:10 000), and currently there is no functional nursing school.
Major health care problems
Lack of trained manpower in all fields is a major issue5,7. There is limited access to medical services, especially among nomads, but also lack of means of transportation limit access to medical services. The nation has incomplete immunization coverage, resulting in frequent measles epidemics. Over-prescribing of medications, especially antibiotics, is common.
There is a high prevalence of malaria6, and childhood diarrhea is also a major cause of morbidity and mortality8. There is also a high prevalence of tuberculosis (TB)9,10. Direct Observed Treatment Schedule (DOTS), a new method for treating tuberculosis, is the preferred method of treatment, due to problems with compliance11. Human Immuno-Deficiency Virus-Acquired Immuno-Deficiency Syndrome (HIV-AIDS) is not a big problem, probably due to low rates of transmission of Sexually Transmitted Diseases (STD)12,13.
Results of the visits to the health facilities
The National Hospital, Hargeisa
This structure was built by the British in the 1950s. Little has changed since then regarding the physical structure. The hospital includes the four departments: medicine, pediatrics, obstetrics and gynecology, and surgery, with a total of 400 beds. There is also a 100 bed psychiatric ward but no trained psychiatric staff. Conditions for these patients are especially difficult. In addition to the usual rates of mental disease in a normal population, post traumatic stress syndrome and coping with returning from exile are additional issues, making psychiatric diagnosis and treatment difficult. Psycho-pharmaca are not used, except for tranquilizers.
Laboratory services are limited to the basics. The only functioning X-ray machine is an old mobile unit, not sufficient for the needs of the hospital. There is an ultrasound machine, which can examine the trunk only. This is used for abdominal, pelvic, and (rarely) chest examinations. There is no permanent record of the examinations because there is no recording paper.
There is no regular supply of bottles of oxygen for the hospital. Currently, all bottles are empty. The blood bank functions well. Given rates of positive tests on donated blood (mainly by patients' family members) were: hepatitis B surface Antigen (HbsAg) 15-20%, VDRL (for syphilis) 10%, and HIV <2%.
Tuberculosis Hospital, Hargeisa
This structure was the old British general hospital until they moved to the 'new' facility in 1958, and the old one became the Tuberculosis Hospital. It has 127 beds, and a large out-patient department (The Fisher Clinic), seeing approximately 700 people daily. Patients are all treated by the DOTS method, as in-patients for 2 months, and as outpatients for the remaining 4 months. Assuming full occupancy, the calculated number of new cases averages 63 per month, with a population catchement of 250 000, the annual incidence of 'open' TB is 3:1000. Record-keeping and reporting is meticulous and accurate. In the year 2000, 597 new cases of smear-positive TB, and 489 cases of smear negative TB were reported - of those 261 were extra-pulmonary TB. This total number gives an annual incidence of 5.4%. There were 30 cases of 'relapse'. Assuming all these are multi-drug resistant TB, the worst case scenario, this represents a 3% rate, which is acceptable. The laboratory performs approximately 250 smears per month of which 10-15% are positive (these are mostly new cases because many of the negatives are patients on DOTS). There are no facilities for culture or sensitivity.
Ms Edna Adan's Maternity and Children's Hospital
Although this structure was not finished at the time of the visit, it will hopefully be opened by April 2001. This charity hospital will have the goals of reducing maternal mortality by providing treatment for complicated pregnancies, and of reducing the mortality of children, especially from diarrheal disease. In preparation for the opening of the hospital there are currently 33 young women studying in a course organized and taught by Ms Edna, some nurses and guest teachers. They have succeeded in putting together a medical library which is a cornerstone for the nursing school.
Urban Health Center in Hargeisa
This urban health center serves 10-15 thousand families, many of them returning refugees. They provide DOTS to 17 tuberculosis patients. A committee elected by and representing the community is functioning at the center, participating in decision making and is finding additional resources. At this center, the system of patient cost sharing is piloted. So far this center has been a success due to community involvement. Under the previous regime health care was free, and explaining to the public why now it costs money is not easy.
Berbera Regional Hospital
During our visit, a board meeting of community members took place. The agenda was: a report from the District Medical Officer about his trip to Hargeisa; an operational plan for the hospital (guided by a specialist from Italy); follow up from last week's business; and the role of the municipality in running the hospital.
There are patients in four buildings, separated by a large compound that also houses the local high school: the general hospital (210 beds), the tuberculosis hospital (56 beds), the surgical hospital (80 beds), and the psychiatric hospital (42 beds, 37 of which are occupied by male patients). The hospital pharmacy is adequate, the director of the hospital encourages local production of formulae from existing medications, such as crushing pills and suspending the powder in syrup for pediatric use. He plans to manufacture intravenous solutions for fluid infusion, using glass bottles and an existing autoclave.
The budget is balanced due to donations from the Italian non-governmental organization (NGO) COPI, and cost-sharing by patients. The hospital has its own electrical generator that supplies more power than the hospital needs. The excess is sold to the city. The hospital works closely with the peripheral health centers, which in turn coordinate the work of health posts in the region.
Tuberculosis is a serious problem. The local laboratory performs 150-200 tests per month. Of these, 10-15% of tests are positive. Presumably all of these are new cases, because there are very few treatment failures. This makes an annual incidence of more than 200 cases for a population of less than 200 000, or more than 1:1000 smear-positive cases per year.
The surgical hospital serves as a referral center for the region beyond the district (Burao and beyond), and many cases of trauma are referred. A visiting consultant from Italy left a video library for surgical procedures, which is functioning and available in the doctors' lounge.
The mother and child health (MCH) clinics, sponsored by UNICEF, functions well, seeing approximately 20 children daily, all less than 5 years of age, and 15-20 anticipating mothers for antenatal care. The pregnant women are given tetanus toxoid vaccination. 'Polio vaccination days' are conducted door-to-door, with blue stickers placed on the door posts of houses visited to prevent duplication.
Burao regional hospital
This remote town was the center for livestock trade. Currently, the market is empty due to the ban of exports. The population of the region is approximately 250 000 people, most of whom are shepherds.
The hospital has 65 beds, and the TB hospital has 114. Patients are hospitalized for 2 months for TB, and the average stay in the general hospital is much shorter. The high number of beds needed for TB patients is impressive. Many of these patients are ethnically Somali, but came from Ethiopia (only 70 km away).
The hospital is staffed by seven doctors and 35 nurses, plus auxiliary staff. Burao born Somalilanders who live in Western countries have donated money and equipment for the local hospital. These efforts have resulted in the arrival of a brand-new X-ray machine, which has not been put to use due to the inability of the local electrical power to supply the 80 kW h needed for the machine. The hospital laboratory is currently paralyzed due to lack of reagents.
The hospital pharmacy needs upgrading and supplies are scarce. It serves 21 health posts and 10 MCH clinics, which requires physical means as well as managerial skills. The surgeons lack instruments. None of the instrument sets is complete.
The problem of childhood malnutrition is more severe in the town than in the rural population. This indicates that economical problems in the town of Burao are serious, so it was reassuring to see that a modern abattoir and a tannery are being built in the town.
The TB ward is run by a competent and energetic registered nurse who knows everything there is to know about this disease. Her laboratory performs many more tests than the others (280 in the month of January), and the rate of positives is lower (5.4% in January), indicating that follow up is tight, and that treatment is successful, because most of the tests are for follow up of patients under treatment.
Discussion
The health ministry is doing a remarkable job, with very limited resources and tremendous problems. They function under circumstances of permanent shortage, and seasonal calamities such as malaria outbreaks in the wet season, measles outbreaks every 3-4 years, and the constant burden of TB.
Tuberculosis is a major issue, and the disease is under-diagnosed. Living conditions are in close quarters, and cold nights contribute to the spread of the disease among family members of undiagnosed cases, augmented by borderline nutrition and emotional stress8. Fortunately the supply of anti-TB medications is not a problem due to UN agencies involvement.
The DOTS method is the best treatment method, because the patient takes the medication under the direct observation of a health-care worker who records and monitors compliance. Hospitalizing the patients for the first 2 months of treatment seems long, but this covers the critical period of therapy, when the patient has to take four medications, or 16 tablets per day. The employment of this method requires persistence and endurance for both the health-care worker and for the patient10. Prevention of further spread of the disease is paramount, and case finding, contact screening and treating are essential components of a good TB program.
When visitors and NGO want to contribute, the easy way is to contribute a piece of equipment, or a month's supply of an expensive medication. This is definitely not the best way to contribute. Sharing knowledge, teaching skills, and upgrading health-care professionals is an investment that will last for much longer, and will improve the wellbeing of the population.
'Prevention is better than cure', however public health is a formidable task. The cultural issues are not to be taken lightly: people who are nomadic by tradition do not have the habits of garbage or sewage disposal of people who have lived in urban centers for generations. It is important to provide health education in the school system so that the next generation will be able to live in a clean environment. Plastic bags do not carry disease but they are a marker of carelessness. The country is littered with millions of used plastic bags and this is a sign of poor garbage disposal.
Sewage disposal is not regarded as a serious issue but in Berbera open sewers run into the closed bay, contaminating the water. Berbera's drinking water comes from a series of springs, originating far from the city. The water flows to the city by gravity, and an efficient chlorinating system is in place. In Hargeisa, the city is supplied with drinking water from clean wells. The amount is 800 m3 per day, for about 200 000 people. The water is distributed to central taps in neighborhoods, from which water is carried by small donkey cart tankers and is sold to people at home. This gives an average of 400 L per day/person, not including city needs, small industries and other losses. Such amounts need a sewage system, with treatment to prevent contamination of the aquifer.
Summary Recommendations
- The public health sector of the Ministry of Health should be stronger. Professionals should be sent to Somaliland to teach local officials the skills and practice of public health.
- A nursing school is needed for the country. The current efforts do not meet the needs.
- The TB program in Berbera region should serve as a model for other regions in the country.
- Water resources must be developed and maintained, assuring safe water supply and safe wastewater disposal.
- Health education is a key issue in this developing nation. It should be incorporated in school curriculae.
References
1. Bisrat F, Berhane Y, Mamo A, Asefa E. Morbidity pattern among refugees in Eastern Ethiopia. East African Medical Journal 1995; 72: 728-730.
2. Sheik-Mohamed A, Velema JP. Where health care has no access: the nomadic populations of sub-Saharan Africa. Tropical Medicine and International Health 1999; 4: 695-707.
3. Maroodi J. Somaliland Household Food Economy Analysis. [No publication title] 1999; 13: Summer.
4. Eisa M. Preliminary survey of domestic animals of the Sudan for precipitating antibodies to Rift Valley fever virus. Journal of Hygiene 1984; 93: 629-637.
5. Spaulding HS. Can I make a difference? The challenge of teaching community health workers in Somalia. Journal of Christian Nursing 1994; 11: 28-31.
6. Bentley C. Primary health care in northwestern Somalia: a case study. Social Science in Medicine 1989; 28: 1019-1030.
7. Ledbetter E, Shallow S, Hanson KR. Malaria in Somalia: lessons in prevention 1995; 273: 774-775.
8. Ibrahim MM, Aden AS, Omar HM, Wall S, Persson LA. Diarrhoea among children in rural Somalia. Maternal perceptions, management and mortality. Annals of Tropical Paediatrics 1994; 14: 215-222.
9. Peltola H, Mohamed ON, Kataja M et al. Risk of infection with Mycobacterium tuberculosis among children and mothers in Somalia. Clinical Infectious Diseases 1994; 18: 106-111.
10. Agutu WO. Short-course tuberculosis chemotherapy in rural Somalia. East African Medical Journal 1997; 74: 348-352.
11. Aden Abdi Y, Gustafsson LL. Poor patient compliance reduces the efficacy of metrifonate treatment of Schistosoma haematobium in Somalia. European Journal of Clinical Pharmacology 1989; 36: 161-164.
12. Watts DM, Corwin AL, Omar MA. Hyams KC. Low risk of sexual transmission of hepatitis C virus in Somalia. Transcriptions of the Royal Society of Tropical Medicine Hygiene 1994; 88: 55-56.
13. Scott DA, Corwin AL, Constantine NT et al. Low prevalence of human immunodeficiency virus-1 (HIV-1), HIV-2, and human T cell lymphotropic virus-1 infection in Somalia. American Journal of Tropical Medicine Hygiene 1991; 45: 653-659.
Published 14 May 2001; style modified 22 July 2003.

