There is a paucity of literature in the area of recruitment strategies for graduate nurses in rural and remote health care settings. This is despite a need for greater numbers of health professionals in rural and remote areas being repeatedly identified by rural health and government peak bodies, the National Rural Health Alliance and the Australian Health Department Healthy Horizons Policy1. Previous studies suggest that familiarity with the workplace is a positive influence on future work intentions2,3. However, a recent national survey of Australian rural nurses found only 8% had experienced any fieldwork in rural practice during their training4. This study is part of a larger project which aimed to provide evidence that student nurses who experience rural and remote health care settings during their studies are more likely to be recruited in their graduate year to rural settings.
A number of difficulties associated with rural clinical placements have been identified in the literature. Nominated restraints include family or carer responsibilities, the commitments associated with part-time employment, the financial burden and transport worries5,6. Concerns have been raised about the type of clinical experience available and distance from professional resources5,6. A study of rural placements in Georgia, USA, found that while some students believed they wouldn't obtain quality work experience, others worried about the level of independence or self-direction needed in a rural setting5. Social isolation and a lack of recreation facilities have also been reported as barriers to rural clinical placements6,7.
All final year nursing students at Queensland University of Technology (QUT), Queensland, Australia, are encouraged to select a placement of interest in first semester of their final year. The motivation of students to try something different is encouraged after two years of clinical placement in metropolitan clinical venues. Some students select to go overseas, others rural or remote and many stay within the usual confines of the metropolitan setting for a number of reasons.
Since 1996, a rural undergraduate clinical placement program has been available to student nurses at QUT. The Rural Clinical Support Scheme was comprised of a rural placement grant that assisted students with the cost of travel. The granting model was based on the number of kilometres from Brisbane, the State's capital city, and the funding ranged from $AU100 to $AU200 per student. Students were provided with a pre-briefing session prior to placement which addressed a number of important issues such as isolation, cultural differences, communication and information and documentation regarding the clinical venues. Students could access the information database on any of the clinical venues which provided them with details about travel options to the venue and within the town, accommodation availability, sporting events and other activities as well as tourist information. Collaboration with the clinical venue staff encouraged appropriate support for the students and preceptors through discussion of clinical site needs and the provision of guidelines for facilitation.
Anecdotal evidence indicates rural placements have a positive effect in raising awareness of the advantages of rural practice as a registered nurse. Although substantial numbers of student nurses have successfully undertaken a rural placement, available places go unfilled. To gain an understanding of the characteristics of students who select a rural placement, it was important to obtain information on factors influencing their choice of a rural or metropolitan clinical placement setting. It is hoped this information will lead to the development of successful recruitment strategies for graduate nurses in rural and remote areas.
Aims
This study was part of a larger research project, of which the aims were to:
- Evaluate the effectiveness of the Clinical Placement Support Scheme for final year Bachelor of Nursing students as a recruitment strategy for rural and remote health care services.
- Develop an increasing awareness in final year nursing students of the employment opportunities available for new graduates in rural and remote areas.
The following research questions were explored in this study:
- Did previous experience of living in a rural community have any impact on the choice of region of placement?
- Did the number of years lived in a rural area have any impact on the choice of region of placement?
- Did the choice of a region of placement have any relationship with having worked previously in a rural area?
- Did the choice of a region of placement have any relationship with other demographic factors?
Method
Design
This study utilised a descriptive survey design to collect pre-test data. A quasi-experimental pre-post test design was used for the larger project.
Population and sample
The population under study consisted of all final year Bachelor of Nursing students at Queensland University of Technology who undertook a clinical placement in 2000 (n = 212). One hundred and thirty-seven questionnaires were returned in the pre-test (response rate 65%).
Instrument
A questionnaire consisting of 24 items was developed by the researchers and contained a combination of open7 and closed8 questions. The questions related to demographics, previous experience of a rural lifestyle, previous work experience and issues of importance regarding the clinical placement experience. Piloting of the questionnaire was conducted prior to commencement of the study.
Procedure
Pre-test questionnaires were distributed to participants at a prebriefing session held at the university one week prior to commencement of clinical placements. Participants completed the questionnaire during the session and returned it anonymously to the researcher.
Ethical approval for the study was obtained from QUT Human Research Ethics Committee.
Data analysis
Quantitative data were analysed using an SPSS database. Frequency distributions, c2analysis (for nominal data) and ANOVA (for interval data) were used to describe differences between the characteristics of students choosing a rural or remote placement and students choosing a metropolitan placement.
Results
Demographics
The demographic characteristics of this sample are shown (Table 1.)
Table 1: Demographic characteristics of final year Bachelor of Nursing students
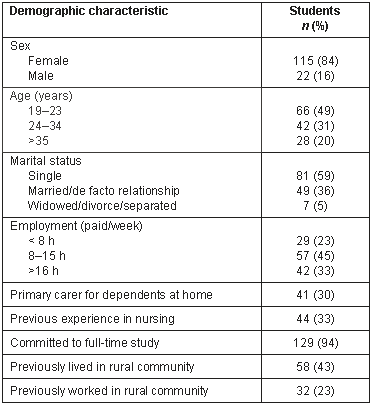
Characteristics of students who chose a rural placement: Thirty (22%) of the 137 students who responded chose a rural setting for their clinical placement.
Previous experience of a rural lifestyle Of the 58 students who had lived previously in a rural community, 19 (33%) chose a rural clinical placement and 39 (67%) chose a metropolitan setting. However, of the group of 30 students who chose a rural clinical placement, 19 (63%) had lived previously in a rural area. The proportion of rural clinical placement students who had lived previously in a rural area (63%) was significantly higher than the proportion of metropolitan clinical placement students who had lived previously in a rural area (37%), (c2 = 6.877, df = 2, p = 0.028).
Length of time lived in a rural community Of the students who had lived previously in a rural area and chose a rural clinical placement (one student did not respond to this question):
- 17% (n = 3) had lived in a rural community for less than 5 years.
- 39% (n = 7) had lived in a rural community for 6-10 years.
- 44% (n = 8) had lived in a rural community for more than 10 years.
In comparison, of the students who had lived previously in a rural area but chose a metropolitan placement:
- 41% (n = 16) had lived in a rural community for less than 5 years.
- 31% (n = 12) had lived in a rural community for 6-10 years.
- 28% (n = 11) had lived in a rural community for more than 10 years.
Worked previously in a rural community Of the 32 students who had worked previously in a rural community, 11 (34%) chose a rural clinical placement, while 21 (66%) chose a metropolitan placement. However, 37% of the students who chose a rural clinical placement had worked previously in a rural community, compared with 20% of the students who chose a metropolitan setting, a significantly higher difference (c2 = 5.873, df = 2, p = 0.048).
Financial/employment considerations Thirty-one students (28%) from the total student sample had applied for a rural scholarship, either from Queensland University of Technology, Royal College of Nursing Australia or Queensland Health. Major issues influencing application for a scholarship were financial reasons (42%) and the opportunity to gain diversity in clinical experience (33%). Reasons identified for not applying for a scholarship included financial/employment obligations in the local area (31%) and a lack of interest in working in a rural area (33%).
Respondents were asked to rate the importance of issues regarding their clinical placement experience on a scale from 1 to 5, from 'not at all important' to 'extremely important'. Analysis of results (using ANOVA) found rural students rated the importance of support for costs associated with placement significantly higher than students undertaking a metropolitan placement (rural students: M = 3.97, SD = 1.02; metropolitan students: M = 3.25, SD = 1.44; F = 6.125, df = 1, p = 0.015), while metropolitan students rated the importance of maintaining work commitments significantly higher than students undertaking a rural placement (rural students: M = 3.45, SD = 1.27; metropolitan students: M = 4.03, SD = 1.12; F = 5.77, df = 1, p = 0.018).
Home and family considerations Family issues were nominated by 57% of students as a reason for not considering future employment in a rural setting and by 24% of students as a reason for not applying for a scholarship to undertake a rural clinical placement. Students who had chosen a metropolitan placement rated the importance of family responsibilities significantly higher than students who selected a rural placement (rural students: M = 3.55, SD = 1.38; metropolitan students: M = 4.26, SD = 1.03; F = 9.292, df = 1, p = 0.003). Rural placement students also rated the provision of appropriate living conditions significantly higher than metropolitan placement students (rural students: M = 3.88, SD = 1.03; metropolitan students: M = 3.03, SD = 1.18; F = 11.02, df = 1, p = 0.001).
Discussion
The demographic information obtained in this study had implications on the students' choice of clinical practice site. Over half of the student sample were aged >24 years, with 31% aged 24-34 years and 20% aged >35 years. In fact, only approximately one-third of nursing students currently enrolled at QUT are recent school leavers, while approximately two-thirds are mature-age students. The high proportion of mature-age students at QUT is not an isolated case, as Queensland Tertiary Admissions Centre's figures show, many South-East Queensland universities have a similar proportion of mature-age nursing students. The high level of family, carer, financial and employment commitments identified in this study reflects the mature age of the group and the strong ties many students have to the local area.
Characteristics of students who chose a rural placement
Rural background: Possession of a rural background has been identified in previous studies as being positively associated with future employment in country areas9-13. It was interesting that of the 58 students who had lived previously in a rural community, only 19 (33%) chose a rural clinical placement setting. However, the proportion of rural clinical placement students who had lived previously in a rural area (63%) was still significantly higher than the proportion of metropolitan clinical placement students who had lived previously in a rural area (37%). A survey of Victorian rural nurses supports these findings, with 67% of the nurses reporting they had spent most of their childhood in a rural area11. These participants indicated that rural background and lifestyle issues were among the most important factors when considering recruitment to a rural area. It has been suggested that universities need to recruit greater numbers of students with rural backgrounds to the health care professions in order to take advantage of this trend14, and recent government initiatives aim to encourage this idea15.
Length of time in a rural community: When examining the number of years lived previously in a rural community, the data suggested that the longer a student had lived previously in a rural community, the more likely they were to choose a rural placement. Forty-four percent of the students who had lived in a rural community and chose a rural placement had lived in a rural area for over 10 years. In contrast, 41% of students who had lived previously in a rural area and chose a metropolitan placement had lived in a rural area for less than five years (28% for more than 10 years). However, the numbers involved were too small to detect any statistically significant differences.
Worked previously in a rural community: There was a significantly higher proportion of students who had worked previously in a rural community and chose a rural clinical placement than those who had worked previously in a rural community and chose a metropolitan clinical placement. This trend could be linked to the positive association between familiarity with the work environment and subsequent employment noted by Glover, Clare, Longston and De Bellis3 and Collins, Hilde and Shriver2. Providing students with some work experience in a rural area may encourage greater familiarity with possible employment settings. The nursing graduates surveyed by Collins et al.2 felt their site of clinical practice was an important influence on their choice of employment, with 28% beginning their careers in the same workplace.
Financial and family considerations: A considerable number of students indicated family (24%), financial or employment (31%) commitments influenced their choice of a clinical placement site. Students who chose a metropolitan clinical placement rated the importance of maintaining work commitments and family responsibilities significantly higher than students selecting a rural area for their placement, while provision of financial support for costs associated with the placement and appropriate accommodation was significantly more important to the rural clinical placement students.
Similar concerns have been identified in recruitment literature. In 1999, a national survey of rural Australian nurses reported that 'self, family or friends live in the area' and 'marriage commitments or family' were listed in the top four most frequent responses to essential factors influencing original recruitment to rural nursing4. Duffy, Siegloff and McGrail reported Victorian rural nurses indicated their partner's employment was the most important factor in recruitment to a rural location11. Providing infrastructure for the needs of nursing students' family obligations, such as the availability of employment opportunities, education facilities and social support for carers, are thus of vital importance when considering recruitment strategies for health professionals to rural areas.
Conclusion
This study supports earlier research demonstrating that students who have previously lived and/or worked in a rural area are more likely to choose a rural setting for clinical placements or postgraduate employment. However, considering nearly half of the students who choose a rural placement had no previous experience of a rural lifestyle, the value of rural clinical placements as a method of increasing awareness of employment opportunities in the rural setting is considerable. Family, financial and employment commitments were also found to influence students' choice of undertaking a rural clinical placement. These factors should be considered in the development of recruitment and retention strategies for health professionals to rural areas.
Acknowledgements
Funding for this research project was received from a Queensland University of Technology Scholarship in the Professions Grant. We would like to thank Ms Rekha Sharma for her assistance in the analysis of data for this project, and also the members of the Reference Committee for their valuable contribution.
References
1. Healthy Horizons. Healthy horizons: a framework for improving the health of rural, regional and remote Australians. Canberra: National Rural Health Policy Forum and the National Rural Health Alliance, 1999.
2. Collins P, Hilde E, Shriver C. Recruiting factors: rural and urban settings. Nursing Management 1993; 24: 97-98.
3. Glover P, Clare J, Longston D, De Bellis A. Should I take my first offer? A graduate survey. Australian Journal of Advanced Nursing 1998; 15: 17-25.
4. Stephenson J, Blue I, Petkov J. A National survey of Australian rural nurses. Whyalla Norrie, South Australia: The Association for Australian Rural Nurses, 1999.
5. McDonough JE, Lambert VA, Billue JS. A rural nursing practicum: making it work. Nurse Educator 1992; 17: 30-34.
6. Barney T, Russell M, Clark M. Evaluation of the provision of fieldwork training through a rural student unit. Australian Journal of Rural Health 1998; 6: 202-207.
7. Mitchell R. Perceived inhibitors to rural practice among physiotherapy students. Australian Journal of Physiotherapy 1996; 42: 47-52.
8. Queensland Tertiary Admissions Centre 2001. Brisbane, QLD: 2001.
9. Easterbrook M, Godwin M, Wilson R et al. Rural background and clinical rural rotations during medical training: Effect on practice location. Canadian Medical Association Journal 1999; 160: 1159-1164.
10. Huntley B. Factors influencing recruitment and retention: why RNs work in rural and remote area hospitals. The Australian Journal of Advanced Nursing 1995; 12: 14-19.
11. Duffy E, Siegloff LH, Siegloff LMF, McGrail M. Victorian Rural Nurse Project: workforce database final report - December 1999. Traralgon, Victoria: Monash University Centre for Rural Health, 2000.
12. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 210-211.
13. Wood D. Effects of educational focus on a graduate nurse's initial choice of practice area. Journal of Professional Nursing 1998; 14: 214-219.
14. Hays RB, Acklin F, Chan P et al. The University of Sydney Rural Careers Project. The Australian Journal of Rural Health 1993; 1: 23-25.
15. National Rural Health Alliance. Budget 2001 (Media Release, 22 May 2001). National Rural Health Alliance e-forum. (Online) 2001. Available from http://www.ruralhealth.org.au/22501.htm (Accessed 8 June 2001).
Published 30 October 2001; style modified 21 July 2003.

