Introduction
Medical schools around the world include a range of programs that expose their students to practice situations outside the classroom and teaching hospital. Community-based medical education gives students opportunities to learn about the health needs and demands of the people they will later serve while, at the same time, learning from practising health workers1,2. The training for doctors who will work in rural communities should include time spent in such communities during their period of study3-6. Rural training sites are appropriate for students to learn more about the range of social, political and economic forces that affect health in every society3,7. In Vietnam, the time and quality of study periods in the community were limited until the 1990s for several reasons. The curriculum was then still hospital-based, teachers lacked experience in organizing and conducting field teaching (FT) in the new social context, and extramural teaching was (and is) more costly than teaching in classrooms. In addition, most of the FT was aimed at serving the needs of the students, with little regard to the needs of the teachers, the local health services and especially the communities.
In 1990, the Vietnamese Government established a policy aimed at training medical doctors in a more community-oriented fashion (Decision 58/TTg of the Vietnam Government, dated 03/02/1994). They planned that by the year 2000 medical doctors would be available in 40% of the more than 10 000 commune health centers (CHC) in Vietnam (Resolution no. 37/CP of the Vietnam Government dated 20/06/1996). This target was met because more than 45% of CHC had doctors at the end of 2000 (Decision no. 35/2001/QD-TTg of the Vietnam Government dated 19/03/2001). A new target was set for 2010: 100% of the CHC in lowland and midland areas would have doctors, as well as 50% of the remaining CHC in mountainous and remote areas (Master Plan for the Domestic Health Care System between 2006 and 2010). Medical schools were asked to increase their attention to both community needs and practice, by making classroom teaching more community oriented, and by improving the teaching in the communities (FT or community-based education, CBE).
However, at the same time the introduction of the market economy and private enterprise in Vietnam began to create barriers to the community accepting large numbers of students, especially if community members could see no benefit for themselves. The market economy and the rise of private practice also reduced the enthusiasm of teaching staff for spending time in rural areas with the students. These changes presented the schools with serious challenges in implementing FT. However, from 1999 the eight main medical schools received support from a Dutch project that provided technical and financial assistance to strengthen community-oriented teaching, including FT.
The project aim was to enhance the capacity of the eight medical schools in community-oriented curriculum development and to improve the quality of the teaching. To be systematic, the program commenced with identifying the knowledge, attitude and skills (KAS) that a general medical doctor graduating from any medical school in Vietnam should have8. The KAS were first identified by teachers from the eight schools, then checked with newly practising doctors9 and final year students about to graduate from the eight schools10. From the agreed KAS came curriculum renovation, teaching/learning material development, then updating teaching/learning methods and student assessment tools to fit with the identified community-oriented KAS. One important aspect was to improve FT so that it would contribute more to the training of community-oriented doctors, who would then have a better understanding of the rural community's health needs, and better skills to meet those needs.
The method of curriculum evaluation designed by Coles and Grant11 includes three phases: first the written plan, then the actual teaching process and last the results, checking the latter two against the first. This approach has also been used to evaluate a community-based period in the medical curriculum by Kristina, Majoor and van der Vleuten12,13. In the present study a similar approach was used, but an additional phase was added to the preparation: a trial phase in which we explored the building of a community-university partnership model to identify appropriate ways to involve the community in FT. Finally, feedback from local health staff, communities and the students who participated in FT were collected to evaluate the program. Looking at the inputs and outputs through these phases, the eight medical schools could clearly recognize the benefits of involving all stakeholders actively and of working on the basis of commitment to an approach of mutual benefit. The factors affecting participation by all stakeholders are discussed here, based on theories of motivation. This approach produced more appropriate and effective FT programs in the context of the change in Vietnam.
The aim of this article is to identify strategies and approaches that were successful in involving different stakeholders effectively to improve FT in the eight medical schools. It is hoped that this case study will be useful to others developing similar initiatives in other settings.
Methods
The four steps in the intervention are outlined (Fig1). The baseline data were obtained during the first inter-school FT workshop in 2001 (before the intervention), from the pilot intervention and from experience as the project was implemented. Before the first workshop, a representative team from each school prepared a report on their existing situation, challenges and plans for FT. The reports also served for comparison among the schools. Stakeholder analysis identified the roles and needs of each stakeholder in each location, which lead to a plan to improve the FT programs in the eight medical schools.
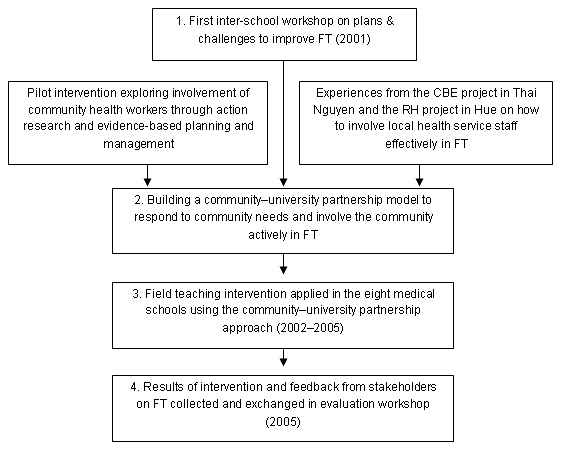
Figure 1: Four steps to improving field teaching in medical schools in Vietnam. CBE, Community-based education; FT, field teaching; RH, reproductive health.
One large challenge was to involve the local health staff and rural community effectively and in a way that motivated and satisfied them. Therefore, a pilot intervention was performed by Hanoi Medical University (HMU) at three communes in a rural district to explore a model of community-university partnership. At the same time, experiences from a project on CBE in Thai Nguyen Medical School and another project on FT for reproductive health (RH) in Hue Medical School (both with international financial and technical support) were also taken into consideration in completing the community-university partnership model. The interventions were then carried out in all eight medical schools from 2002 to 2005. To check the achievements and lessons learnt from the FT intervention, in 2005 the eight schools collaborated in a multi-centre survey. They interviewed 144 rural health staff involved in their FT programs as preceptors as well as 300 community members. They also conducted 12 focus group discussions (FGD) among local authorities at rural FT sites to obtain their opinions. Additional information came from a feedback survey performed by the HMU team using a structured questionnaire among 240 students who had just returned from their FT period in rural districts of nearby provinces.
Data collection and analysis
The research method used in this study is case study evaluation, in which data were collected from different sources (participatory stakeholder workshops, surveys, pilot interventions, project documents and reports) using different methods (semi-structured questionnaires, informal interviews, structured interviews using checklists, focus group discussions and participant observation), before and after interventions with experimental steps. The results and lessons were summarized, screened for frequently occurring or repeated terms and concepts as well as associations, then presented and compared in diagrams and matrices. The Herzberg motivation theory14 was also applied to identify factors that would motivate stakeholders' effective involvement in the FT program. Data from different sources and obtained by different methods were used to triangulate, in combination with participant observation and data from feedback surveys, to maximize the validity of the results.
Results
Challenges to field teaching before the intervention
Before 1986 (ie before the market economy was introduced in Vietnam), when all the training activities of medical schools were centrally subsidized and private practice by teaching staff was not allowed, it was relatively easy to carry out FT. Teachers in both preventive medicine and clinical departments had time and the willingness to go into the field with students; while people in the rural community at the FT sites were happy to receive both teachers and students, because it would offer them access to a higher quality of medical care. Since market mechanisms were introduced in 1986 and the private sector started to develop, budget allocation to medical schools became more decentralized, and teachers started to set up private practices and so were less willing to take the time to go with students for FT. Rural residents at the FT sites were also influenced by the market mechanism, having greater access to medical care on the one hand, and paying more attention to other kinds of benefits on the other. These changes made FT more difficult to organize. At the same time, the Ministry of Health (MOH) requested that the schools provide doctors with a more community-oriented background to prepare them better for service in the community.
At the first inter-school workshop in 2001, a number of key challenges and barriers were identified for all stakeholders (Fig 2).
For schools, FT was complicated and costly to organize because schools had to identify and prepare the rural FT sites, pay for transport, accommodation and mission allowances for teaching staff and organizers, and supervise students more carefully than in the university environment.
These difficulties had considerable influence on the practice of FT in Vietnam's medical schools. The quality of FT no longer met the needs and requirements of the MOH policy or of society (Fig3).

Figure 2: Barriers to field teaching in medical schools before 2001: results of stakeholder analysis. FT: Field teaching.
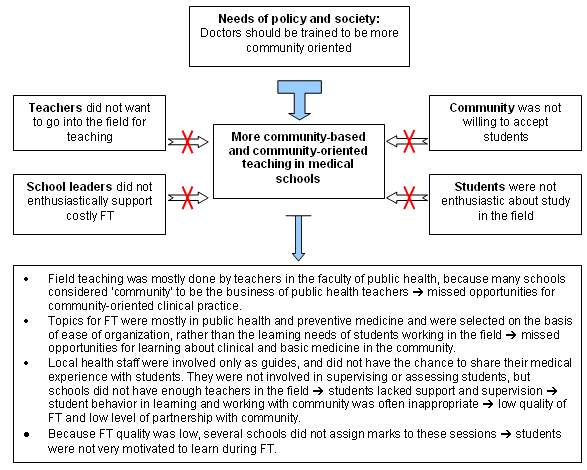
Figure 3: Barriers to field teaching and their effects on community-oriented learning before 2001. FT, Field teaching.
During the first workshop it became clear that improving partnerships among the stakeholders, respecting each one's need for benefits and motivating them would be the main approach to improve FT in the eight schools. The community-university partnership was especially targeted for improvement. Because most of the teachers in the medical schools were still inexperienced in ensuring that communities were actively involved in FT, a pilot intervention was planned to test an approach that could motivate and involve local health staff and communities.
Building a community-university partnership model
Senior and junior teaching staff of HMU worked with three communes in a densely-populated, urbanizing rural area near Hanoi to build a model that supported health staff and volunteers at community level in solving local health problems using an evidence-based planning approach.
First, the HMU and MOH staff visited the district and the three communes to discuss with them what they needed and what the university could provide. They agreed that the local people needed to be better able to analyze their own problems and find solutions for them, using the skills of action research. That was something the university could provide.
A pool of trainers was established, including HMU staff and staff from the Department of Science and Training, MOH, and a few experienced staff at provincial and district levels. The pool included both experienced and junior staff, to provide opportunities for learning and sharing experiences and to ensure supervision during action research and implementation of interventions. Together, the staff trained and supervised six staff of the CHC and 27 village health workers in three communes. The participants learned to identify problems and to collect data (existing and new) to describe and prioritize the problems and then look for solutions. They learned by participating in a series of training courses alternating with practice periods, as presented (Fig4). The participants selected three topics for action research and intervention: malnutrition in children under five; pesticide abuse by farmers; and traffic accidents in an urbanizing area. By participating in all project activities, staff from HMU learned how to work with community health workers and others in a participatory way. They also learned how to teach evidence-based planning and management for health workers at grassroots level. A pilot model for a community-university partnership was established that respected the needs of, and ensured benefits for, all partners15.
At the same time, experience from the other projects supporting community-based teaching in other medical schools was reviewed. In the Thai Nguyen Medical Faculty, for example, students were assigned to follow at least 10 households in their catchment area during their 6 years in the medical school; they helped the families improve their health, both in preventive and curative aspects. That project also shared the experience of how to guide learning for students at district hospitals and commune health centers, and how to ensure that local health staff had clear roles in the FT. In Hue Medical College, experience from the RH project and another project focused on FT contributed ideas about how to recruit, assess, train and reward district health staff for participation in training, supervising and assessing students. With all of these inputs, a model for community-university partnership was developed and adopted for intervention at all eight medical schools.
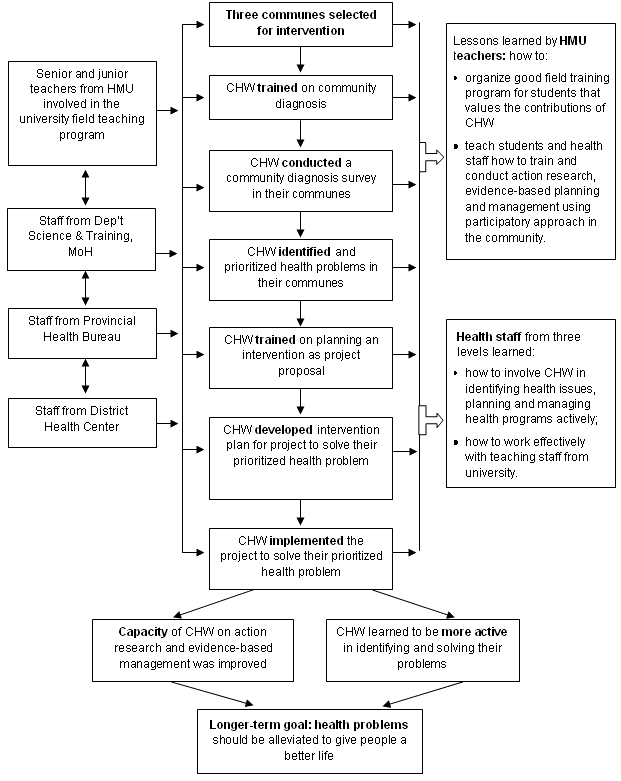
Figure 4: Process of evidence-based planning and project management and its achievements. CHW, Community health workers; HMU, Hanoi Medical University; MOH, Ministry of Health.
Main strategies and activities to improve field teaching in the eight schools
An important question as we developed new strategies and activities for FT was how to involve and motivate all stakeholders so that they could and would continue to contribute after the end of the project. Using the theories of motivation proposed by Herzberg14 and our experiences during the pilot intervention and from other projects, we analyzed the motivation of the four main stakeholders whose involvement was needed in the FT. Figure 5 shows the areas and activities identified for improvement of FT, and the roles of the different stakeholders.
The selection of the most appropriate strategies and activities for each stakeholder was based on the application of Herzberg's motivation theory14 as presented (Table 1). In this way, the FT program could ensure benefits and motivating factors for all stakeholders.
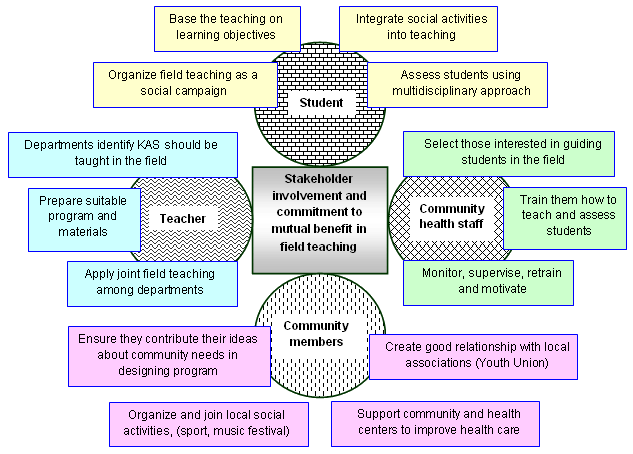
Figure 5: The role of each stakeholder in strategies to improve field teaching. KAS, knowledge, attitude and skills.
Table 1: The application of Herzberg's motivation theory to strategies for field teaching programs
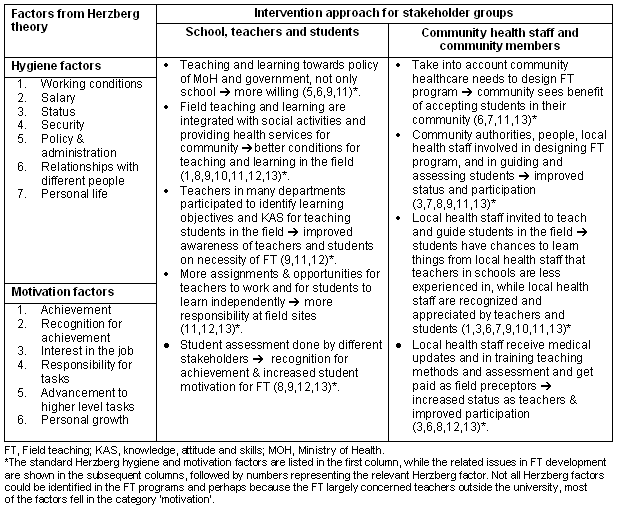
Once the plans were prepared, the intervention to improve FT programs began in the eight medical schools. The FT programs were not identical in each school because they were adapted to fit the local situation; however, all worked towards the community-university partnership with attention to and respect for the needs and benefits of all stakeholders.
Intervention activities for field teaching
The main activities of the intervention are summarized (Table 2).
Table 2: Relationships between aims and actions in field teaching
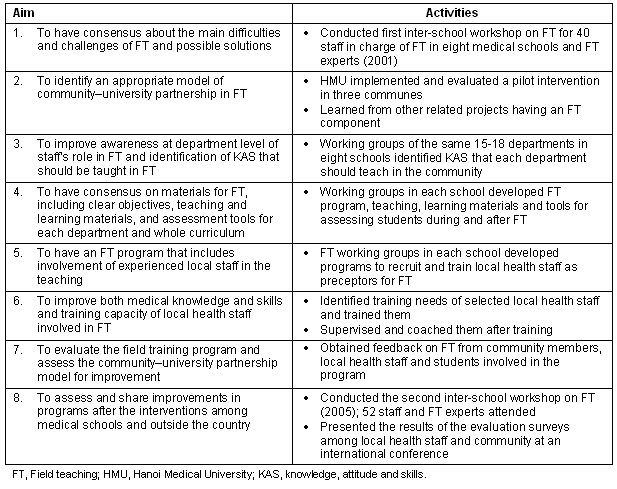
Results after interventions
The results and achievements of the intervention are summarized (Table 3), comparing columns according to the situation before and after intervention.
Table 3: Results and achievements of field teaching after the intervention
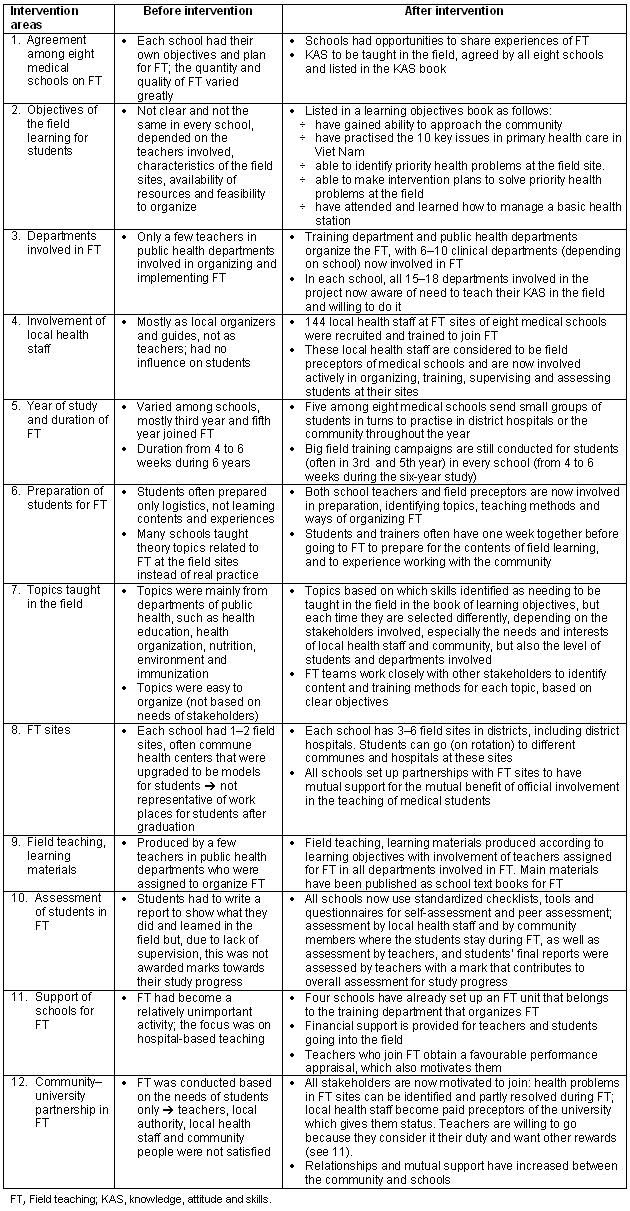
Evaluation of the intervention by different stakeholders
To evaluate the improvements in FT and achievements of the community-university partnership approach, surveys were performed among the three important FT stakeholders: (i) local health staff who now become preceptors for FT; (ii) community members and local authorities at the FT sites; and (iii) the students. The results of these surveys are summarized (Table 4).
Table 4: Feedback from the three important field teaching stakeholders
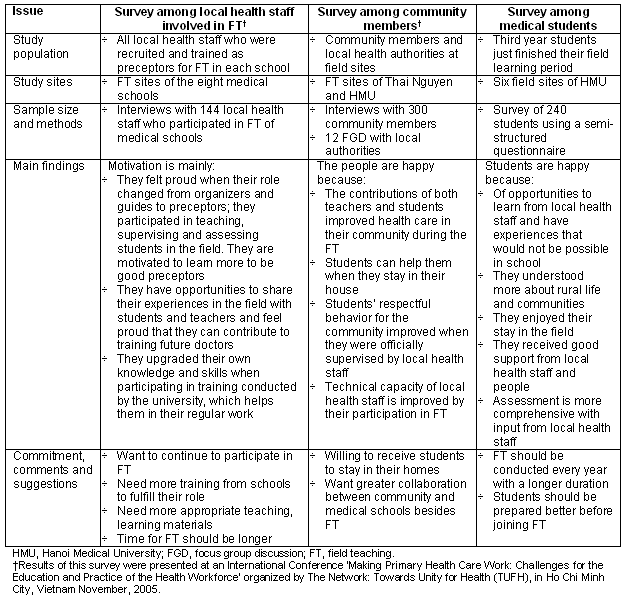
In addition to the direct benefits of FT for all stakeholders, the results of the surveys also revealed that the medical schools and their teachers gained many indirect benefits. Indirect benefits for the teachers included:
- Their KAS were improved by greater exposure to the community and by sharing experiences with local health staff when teaching in the field. They also shared duties in organizing and supervising students during FT.
- Student assessment was more objective with input from the local preceptors so the teachers have more confidence in it.
- The quality of teaching and learning in the field was much better using the new model that involved all stakeholders.
Indirect benefits for the schools included:
- It was easier to conduct FT when local health staff are actively involved and motivated.
- Local authorities paid more attention and assisted the students more in the field.
- The schools could reduce financial support for teachers and students because community members were willing to provide accommodation (due to the FT benefits for themselves and their community).
- The relationship between the community and schools was better when they shared planning and implementation as a collaboration.
Discussion
What we have learned
Field teaching has been applied widely in many medical schools, especially in developing countries and in countries where there is a need for medical practitioners in rural areas2,3,12,16-19. These periods are believed to develop students' ability to integrate their knowledge in the basic and behavioral sciences in relation to practice in a real situation20. It also helps students better understand the doctor-patient relationship, the decision-making processes in the real life context, and how the health care environment is changing21. As Kaufman said, 'If learning in medical schools is to be suitable for rural practice, students must receive early and sustained exposure to rural communities and to rural physician role models'7. Many programs aim to influence medical students to choose rural practice after graduation, although it is not yet clear whether that is always the program outcome1-3,20,22. There is evidence that FT can lead to better communication between the primary-care level and the referral levels and better community-based care for those with chronic conditions23. In Vietnam, FT at rural sites has a long history, but since 1986 when the market economy and private sectors were introduced to the country, medical schools faced many challenges in its implementation. The general objective of FT should be to expand the students' perception of community health problems and their learning through providing service and performing research in the community3,24. At the same time students should contribute to improving the health of the community in which the program is conducted.
In Vietnam, the eight medical schools worked together to build a community-university partnership in their FT programs that would benefit both the students and the communities. The greatest challenge was to motivate all stakeholders to be involved actively and effectively, especially the local health services and the community. Using the theories of motivation outlined by Herzberg14 and by Adams and Maslow25, we considered the motivation of different stakeholder FT participants (Fig5; Table 1).
In the case of the students and teachers, who already knew that FT was necessary and that they had to be involved, by applying Herzberg's theory we recognized a need to provide them with maintenance factors. These could be, for example, providing good learning and teaching environments, integrating the learning with social and entertainment activities, combining the learning and teaching in the field with implementing research and providing health services, thereby giving both students and teachers more opportunities to learn and to share their experiences. Motivation factors for teachers in FT started with giving them responsibility, first asking teachers from each department to identify and plan for the KAS that they should teach in the field. The departments and the faculties supported that request and the teachers felt responsible. The teachers could also learn from other stakeholders and get involved in community research and services; these actions would contribute to their career advancement and provide recognition and appreciation from students, local health staff, the community and their colleagues. For students, the opportunities for self-learning, enjoying life in the community with social activities, and the freedom to explore new areas were the main motivational factors. They were also motivated by their responsibilities and achievements, once we introduced a good supervision and assessment system with the participation of all stakeholders. Students gained the recognition of classmates, teachers and the community when they performed well in the field learning sessions. These benefits were recognized by students who had been on rural placements in other countries1,2,20,26.
Efforts to improve FT and make it sustainable included capacity building for individuals like teaching staff and students, and also for their organizations and institutions. In all eight medical schools, the teaching staff received support to produce the new FT program involving all stakeholders, with appropriate teaching and learning materials, including tools and procedures for student assessment. Once the systems were established and the materials available, maintenance costs were relatively low. Some schools set up an FT unit under their training department to coordinate all FT activities, but others have not yet made that move and have left FT to the public health department to organize and implement. It remains difficult to motivate the clinical and basic science departments to become involved. This may be in part because of financial losses they may incur by remaining rural, but it is also a attitudinal problem with a belief that there is not enough relevant work during a rural attachment. In the schools that made a specific effort to include clinical teaching in their rural FT periods there were a few key clinical departments (such as obstetrics or pediatrics), actively involved.
For the local authorities, health staff and community members, Adams' theory25 of job motivation may provide a better basis for analysis, because they may not consider FT their responsibility. To involve them actively, we had to consider the balance between what we wanted them to contribute to FT and the benefit they could gain from their involvement. In Tasmania, Australia, field preceptors felt excluded from the educational process until a program to provide them with training skills and more involvement with the students was instituted1,27. When the Vietnamese program was adapted to give the local health staff and others more responsibility and clearer benefits, the feedback from all community groups was very positive.
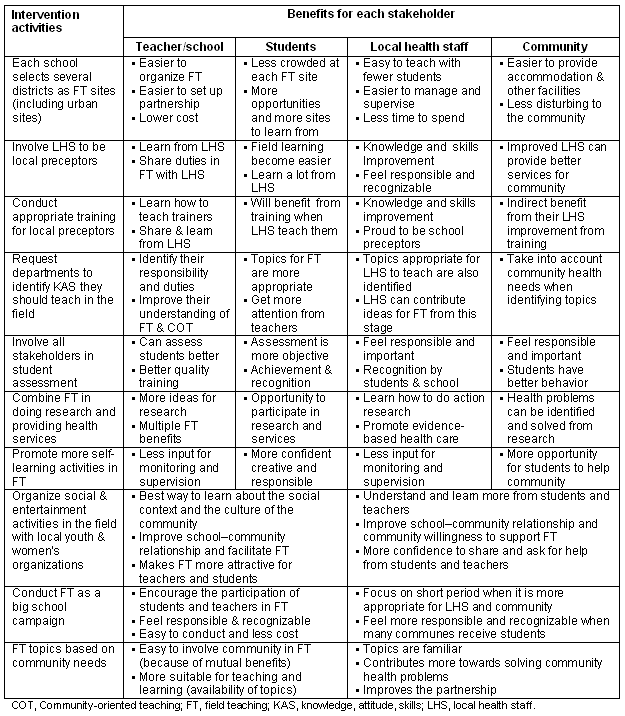
Using a multi-stakeholder approach that addressed appropriate motivating factors for each stakeholder, the FT project interventions appear to have been successful in gaining the support and involvement of all main stakeholders, as is illustrated (Table 5).
Table 5: Summary of benefits for stakeholders from each intervention in field teaching
Conclusion
Eight medical schools in Vietnam recognized a need to improve their rural FT programs and worked together to achieve this. The situation analysis guided the selection of issues to be addressed, then pilot FT interventions were carried out at rural field sites before applying them to all medical schools. The development of strategies for involving stakeholders at the field sites was informed by theories of motivation. This resulted in an effective community-university partnership model that satisfied all stakeholders. This step-by-step approach demonstrated a number of successful strategies to creating conditions for continued stakeholder contribution to FT. Such a 'win-win' approach to community-campus collaboration should be considered in every activity to maintain, develop and strengthen the community-university partnerships in FT in Vietnam and in other countries.
Acknowledgements
The authors acknowledge the essential contributions of the project teams, team leaders and other staff in the eight medical schools and their colleagues in the field, who contributed their experience, implemented activities and reported results. Also gratefully acknowledged is the support and leadership of the project directors, the late Professor Ton That Bach and Professor Nguyen Lan Viet; the Project Coordinator Dr Nguyen Thi Bach Yen, as well as the financial and moral support of the Royal Netherlands Embassy throughout the project, which ended in early 2006 (source of funding: project 'Strengthening Community-Oriented Medical Education in Eight Vietnamese Medical Schools', Royal Netherlands Embassy in Hanoi, 1999-2006). We also thank Professor J Ruitenberg and Professor G-J van der Wilt of the Vrije Universiteit, Amsterdam, for helpful discussion during preparation of the manuscript.
References
1. Dalton LM, Routley GK, Peek KJ. Rural placements in Tasmania: do experiential placements and background influence undergraduate health science student's attitudes toward rural practice? Rural Remote Health 8: 962. (Online) 2008. Available: www.rrh.org.au (Accessed 14 October 2008).
2. Shannon CK, Baker H, Jackson J, Roy A, Heady H, Gunel E. Evaluation of a required statewide interdisciplinary rural health education program: student attitudes, career intents and perceived quality. Education in Health (Abingdon) 2005; 18: 395-404.
3. Eley D, Baker P. Does recruitment lead to retention? - Rural Clinical School training experiences and subsequent intern choices. Rural Remote Health 2006; 6: 511.
4. Pathman DE, Steiner BD, Jones BD, Konrad TR. Preparing and retaining rural physicians through medical education. Academic Medicine 1999; 74: 810-820.
5. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809-814.
6. Woloschuk W, Tarrant M. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36: 241-247.
7. Kaufman A. Rurally based education: confronting social forces underlying ill health. Academic Medicine 1990; 65: S18-S21.
8. Hoat LN, Yen NB, Wright EP. Participatory identification of learning objectives in eight medical schools in Vietnam. Medical Teacher 2007; 29: 683-690.
9. Hoat LN, Dung DV, Wright EP. Practicing doctors' perceptions on new learning objectives for Vietnamese medical schools. BMC Medical Education 2007; 7: 19.
10. Hoat LN, Son NM, Wright EP. Perceptions of graduating students from eight medical schools in Vietnam on acquisition of key skills identified by teachers. BMC Medical Education 2008; 8: 5.
11. Coles CR, Grant JG. Curriculum evaluation in medical and health-care education. Medical Education 1985; 19: 405-422.
12. Kristina TN, Majoor GD, Van der Vleuten, CPM. Does Community-Based Education come close to what it should be? A case study from the developing world: students' opinions. Education in Health (Abingdon) 2006; 19: 179-188.
13. Kristina TN, Majoor GD, Van der Vleuten, CPM. Does CBE come close to what it should be? A case study from the developing world. Evaluating a programme in action against objectives on paper. Education in Health (Abingdon) 2005; 18: 194-208.
14. Herzberg F. One more time: how do you motivate employees? Harvard Business Review 2003; 81: 87-96.
15. Hoat LN. Grassroots Partnership in Vietnam. The Network Towards Unity for Health Newsletter; 27(1): 20.
16. Azila NM, Rogayah J, Zabidi-Hussin ZA. Curricular trends in Malaysian medical schools: innovations within. Annals of Academic Medicine Singapore 2006; 35: 647-654.
17. Habbick BF, Leeder SR. Orienting medical education to community need: a review. Medical Education 1996; 30: 163-171.
18. Kiguli-Malwadde E, Kijjambu S, Kiguli S, Galukande M, Mwanika A, Luboga S et al. Problem Based Learning, curriculum development and change process at Faculty of Medicine, Makerere University, Uganda. African Health Sciences 2006; 6: 127-130.
19. Kristina TN, Majoor GD, van der Vleuten CPM. A survey validation of generic objectives for community-based education in undergraduate medical training. Education in Health (Abingdon) 2006; 19: 189-206.
20. Wilson NW, Bouhuijs PA, Conradie HH, Reuter H, Van Heerden BB, Marais B. Perceived educational value and enjoyment of a rural clinical rotation for medical students. Rural Remote Health 8: 999. (Online) 2008. Available: www.rrh.org.au (Accessed 14 October 2008).
21. Shipengrover JA, James PA. Measuring instructional quality in community-orientated medical education: looking into the black box. Medical Education 1999; 33: 846-853.
22. Baillie S, Matena J, Yerxa J, Newbury J. Rural medical education: five medical students spend a year in rural Port Lincoln, Australia. Rural Remote Health 7: 586. (Online) 2007. Available: www.rrh.org.au (Accessed 14 October 2008).
23. Seabrook MA, Lempp H, Woodfield SJ. Extending community involvement in the medical curriculum: lessons from a case study. Medical Education 1999; 33: 838-845.
24. Magzoub ME, Schmidt HG. A taxonomy of community-based medical education. Academic Medicine 2000; 75: 699-707.
25. Lindner JR. Understanding employee motivation. Journal of Extension 1998; 36(3):. (Online) 1998. Available: http://www.joe.org/joe/1998june/rb3.html (Accessed 14 October 2008).
26. Schoo AM, McNamara KP, Stagnitti KE. Clinical placement and rurality of career commencement: a pilot study. Rural Remote Health 8: 964. (Online) 2008. Available: www.rrh.org.au (Accessed 14 October 2008).
27. Baker PG, Dalton L, Walker J. Rural general practitioner preceptors--how can effective undergraduate teaching be supported or improved? Rural Remote Health 3: 107. (Online) 2003. Available: www.rrh.org.au (Accessed 14 October 2008).

