Introduction
Medical imaging utilisation in rural populations is 85% of that of non-rural populations1, which may be a marker of poor access to medical imaging in rural areas. Access to appropriate services has implications for patient outcomes and for costs to the community in rural practice. For example, the use of ultrasound (US) in trauma may guide decisions regarding when (and how) to evacuate a patient from a rural setting; and its use in blunt trauma has had significant patient benefits2. In addition, computed tomography is associated with better patient outcomes for extradural haemorrhage3. Despite this, there is a projected shortfall of radiologists throughout Australia1 and in common with other medical services, it is likely that this will be felt disproportionately in rural communities. Currently only approximately 14% of radiologists are based outside metropolitan locations1. Therefore, the performance of radiology services by rural GPs and rural GPs' ability to access satisfactory radiology services by referral to third parties, in particular radiologists, are both important issues in the health care of rural communities.
Despite the acknowledged clinical importance of radiology, and there being an awareness of issues surrounding the rural radiology workforce and access to services and equipment, there is a paucity of information assessing the adequacy of rural radiology services in Australia. Assessing the satisfaction of rural GPs with the radiology services available to them is one way of assessing the adequacy of these services. To the authors' knowledge, there are no existing studies that identify the factors determining GPs' satisfaction with rural radiological services. In fact, few studies have assessed satisfaction at all. In Australia, McLean and Condon4 assessed satisfaction with mammography screening in Darwin using a global four-point satisfaction scale, finding that the program was well-accepted by GPs; a similar global satisfaction rating was used to assess bone densitometer services in the UK5. Neither of these studies assessed which specific factors influence satisfaction. Without this knowledge, it is difficult to assess rural GPs' perceptions of the adequacy or otherwise of the radiology services and the equipment available to them, or to identify how the provision of radiology services to rural GPs could be improved. This article aimed to identify the factors influencing GPs' satisfaction with rural radiology services, in terms of both the radiology GPs perform themselves and the radiological services to which GPs refer their patients.
Methods
Sample selection
In 9 May 2005, Tasmania had 135 GPs practising in rural areas (Rural, Remote and Metropolitan Area classification 5 to 76,7). We used purposive sampling from Tasmanian general practice workforce data7 to select male and female rural Tasmanian GPs of different ages from all three regions of Tasmania. This was performed using computer-generated random numbers with stratification by age (≤ 50 years or > 50 years), sex and region (north, northwest and southern Tasmania) with over-sampling of GPs practising in remote areas, due to their small numbers (n = 3). This sampling method ensured that the views of a diversity of rural GPs were obtained8,9. Recruitment was by letter of invitation followed by telephone contact. The study received ethics approval from the Human Research Ethics Committee (Tasmania) Network. Subjects were offered either face-to-face or telephone interview, and all subjects gave verbal informed consent according to the ethics committee approved consent processes.
Data collection
Interviews were performed in November 2005. The GPs participated in a semi-structured interview in which they discussed rural radiology services in their local area. Semi-structured interviews are an open-ended and exploratory qualitative technique where the interviewer is focused on a number of issues/questions to be explored8,10. The interviewer uses a list of possible questions or topics to guide the interview while allowing the conversation to flow naturally. The interview guide used is shown (Fig1). Interviews were conducted by phone by one author (BS) and were scheduled for a time suitable for the participating GP. The interview was recorded with permission of participants then transcribed in full. Interviewing ceased once 'theoretical saturation'11,12 was reached (ie once new themes emerging from interviews were minimal).

Figure 1: Interview guide.
Data Analysis
The transcribed interviews were analysed using an iterative and interpretive technique aimed at identifying major themes and providing insight into the issues raised by the research participants. The interviews were analysed progressively which enabled emerging insights to be incorporated into questioning in subsequent interviews. The interview guide served as a 'launching pad' for discussion and was used flexibly throughout the study8,13. A thematic analysis of the interview transcripts was undertaken, in which interviews were coded and the coded data used to identify the factors influencing GP satisfaction. Thematic analysis is 'part of an interpretive method that examines and seeks to explain the meanings that emerge from interview data'14.
Results
Twelve interviews were obtained from 15 approaches, but data from two interviews were lost due to equipment difficulties. Characteristics of the usable study sample (n = 10) are given (Table 1). Interviews ranged from 20 to 50 min in duration. Major factors influencing GPs' satisfaction identified from interviews are given (Fig2), and described below.
Table 1: Characteristics of participant GPs
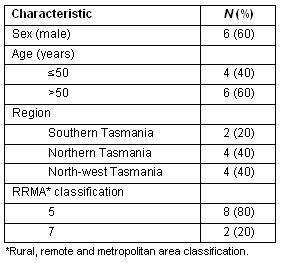

Figure 2: Major factors influencing GP satisfaction.
Access to service
Having to travel to obtain radiology services was seen as an inconvenience to the patient related to the distance that the patient had to travel 'compared to just popping... to the next suburb... it is a major inconvenience' (GP8). Travel also leads to greater indirect costs to the patient and community. The interviewees noted that patients not only incurred direct costs associated with the medical care and transport to and from the service, but that some also lost wages. They were also aware that some patients (such as those with a disability) faced great difficulties, particularly if they needed to be accompanied by their carer. The direct cost of services varied. Bulk billing, where the cost of the service is completely paid by the government, could be negotiated with radiology service providers in some cases. However, in some locations, costs of private radiology, particularly for after-hours services, had risen significantly.
GPs were acutely aware that there were limitations on the type of service that could be provided: '...small community, small utilisation, high capital cost of installation, high cost of running to maintain the service... it just is not cost efficient' (GP7) . It was acknowledged that radiology was one of many things that were more difficult to access in remote areas: '...we have a relatively good service, considering that the place is remote and difficult. It's easier to get an x-ray... than it is to get a lemon tree delivered' (GP8). These views depended to some extent on the degree of remoteness of the area in which the GP was practising:
I think we're extremely indulged and very spoilt in our access and availability of services... there are huge numbers of communities in mainland Australia which are faced with frightful travel, time and difficulties. (GP9)
Well, for the very remote communities like [name] Island.., it's a different situation to places like [town name] where you can just put someone in an ambulance and they can be in the hospital in half an hour... So I think it does need a higher level of local radiology support. (GP4)
Promptness and reliability of services
Responsiveness and reliability of services were frequently mentioned, and were often framed in terms of differences in level of service between private and public systems. One episode of care from a private provider was favourably described.
I had a person who I sent in for an x-ray, I saw them at my surgery at quarter past two, they drove straight in [to x-ray], I checked my email between 4, 4.30..., the report was there and I rang them [the patient] on their mobile and they were halfway home. (GP6)
In comparison experiences described from the public system were predominantly negative. Some of this was due to reporting delays:
I had one from [hospital name] this week which was really annoying, I had a patient who went up there with a knee injury on Saturday night and I sent a request through on Monday morning to records for the report... I haven't got it yet, they just sent a note to say that it hadn't been reported. (GP3)
Equipment
In their communities GPs had access to X-ray, US and mammography. For those GPs who performed their own imaging, X-ray equipment was the most common type of equipment used. The type and quality of this was very variable. A number of places had access to portable X-ray machines which GPs found convenient and those with access to them seemed relatively happy: 'It does the job, its mobile, its adjustable ... the accessories are probably , more in need, but you can manage with other things' (GP8).
Other GPs had used fixed X-rays and felt there were some benefits of these, in particular perceiving that they reduced radiation doses to patients. Some GPs felt that equipment was very poor: '...some of it came over with the first fleet' (GP7). One community was aware of issues with radiology equipment, with the GP describing fundraising efforts to replace it: 'The butchers here is running a collection... they give away bones for a donation for the new X-ray machine for the hospital' (GP8).
Maintenance also presented a challenge: 'We would report that it was malfunctioning, and wait for the health department to send a technician to repair it, which might be a week or two' (GP4).
Access to US equipment was limited to Doppler US which GPs used in obstetrics. Its use was limited by skills, GP experience and equipment. 'The ultrasound is very dicey... it's something that one of my colleagues got off EBay so that we could feel better about having people here in labour ' (GP2). There was interest in diagnostic US, but no GP interviewed reported access to this modality.
I think provision of an ultrasound would be a useful thing, and training for the local general practitioners in its use and interpretation of the results. That's not an expensive thing... (GP4)
Although GPs did not use mammography equipment, mammography was available locally through the mobile mammography service. In general this was considered an effective and useful service.
Assistance with X-ray interpretation
Most people surveyed found getting help with interpretation relatively easy. However opinion varied and some found it more difficult. This rural GP found it a challenge to get help.
Sometimes we ... send it [the X-ray] down on the bus to [town] with a note saying please take this to fracture clinic and have them call us... if we want immediate assistance on it, we might ask a relative to drive it to town. (GP2)
Access to training and skill levels
Some GPs had a sense of satisfaction with taking their own X-rays:
It's good doing it yourself, and it's really quite good when you can read it properly too. It keeps your skills up tremendously compared to what happens with the standard general practice. (GP8)
Of the GPs who operated equipment, their confidence in their ability to do so varied. One GP stated 'I'm pretty satisfied with my ability to handle the equipment I've got and I'm used to' (GP5). However, another GP reported:
I have only tried to do it [operate equipment] once... the first weekend I was on ... I told the person look I haven't operated this machine and she said yeah go for it... I didn't get a good film and I haven't used the machine since. (GP2)
The GPs' confidence in interpreting results also varied, ranging from definite discomfort: 'I don't do it really often enough to become confident, or to stay confident' (GP10); through to 'I'm comfortable with my limitations. I think I'm aware of my limitations' (GP8).
The GPs expressed the view that training courses for operating equipment were not relevant to their situation.
'I did a re-accreditation course ... when I came here which was absolutely useless to using our machine, I learnt by reading the instruction booklet that comes with the machine and practising, used some road kill actually to try it out. (GP8)
GPs believed courses were not well publicised and some seemed unsure of how to attend courses for licensing.
Access to training for interpreting images was also an issue.
A lot of CPD [continuing professional development]...used to occur at lunchtimes because that suited the suburban GPs... The ones that rural workforce agency put on twice a year... they're value because they have a spouse and family program, they're a good thing. (GP6)
The GPs were interested in further training in areas including taking X-rays of limbs, shoulders, pelvic girdle and chests, taking and interpreting X-rays in children, chest XR interpretation, general X-ray interpretation, use of US and how to choose the best way to use radiology services.
Challenges presented in accessing after hours radiology
The processes to access radiology after hours were consistently complex. One GP talked about her experience of having to make pragmatic adjustments to her clinical practice when she started work in a rural location.
We get a lot of broken bones on athletic weekends especially, and so Saturday is really busy. And when I first came here I sort of thought oh you get an X-ray when people come in with an injured limb, but I was persuaded that you could put a back slab on it and wait until Monday most of the time. (GP2)
The GPs were aware of difficulties faced by their communities in accessing after-hours care. At times when the radiology service was not available people from some communities had to travel long distances to a major public hospital or wait until the resumption of service. This was an inconvenience to the patients and could result in treatment delay.
This weekend I had somebody with a bowel obstruction who didn't want to go to [town name], and it turned out... Monday when we got the X-ray he actually was quite constipated... had we known that we could have done something...over the weekend. (GP2)
If a decision was made to transfer the patient to access radiology then a number of logistical problems could present themselves including coordinating services and arranging transportation.
...if we had an after hours problem... it would have to go to [town name]. So there would be a question of liaison with the radiology or the emergency service team...And then of course if it was significant enough to require an after hours X-ray you'd almost certainly involve the ambulance service which would necessitate getting volunteer... so there'd be a lag time of [up to] two to three hours before you could arrange even the transport, so it might be four to five hours before the patient actually hit the X-ray. (GP7)
Difficulty accessing results after hours was also a factor affecting GPs' satisfaction with after-hours services.
It all works well until you hit six o'clock or weekends, and then the whole thing just disintegrates. ...A few years ago I really needed an important report, and I wrote it on the report that it was important and that I wanted the result, and nine o'clock I realised that I hadn't got it and I actually had to get the radiographer on call to go in and open up the building and get the report and phone me back. (GP3)
Not all GPs found after hours service difficult.
It's actually easier to do an X-ray out of hours [at the hospital] because we haven't got another line up of patients waiting... if they come into the rooms ... then you're twenty minutes behind. (GP8)
Discussion
This study identified key factors influencing rural GPs' satisfaction with the radiology services available to meet their needs and the needs of their communities. These include accessibility for their patients, the quality of after-hours services, promptness and reliability of services, equipment quality and availability, access to training and skill levels. To the authors' knowledge, this is the first research addressing this important issue for rural GPs and provides novel and important insights into this significantly under-researched area.
An issue of great concern identified by this study is that of after-hours radiology services. Radiology services were either less or not at all available and with private services there could be increased expense associated with using them. Using public services often involved treatment delays, more travel with associated costs and inconvenience to the patient, and were often delivered through hospital emergency departments with the associated issues of waiting time for the patient. Rural GPs were presented with a dilemma. They needed to rely heavily on their clinical acumen to decide if the problem required urgent attention that needed treatment in the public hospital system immediately, or could it be 'patched up' and wait until the service resumed? The dilemma the GP faced could be compounded by the patient who may be resistant to traveling long distances. The GPs did not mention the potential for using rural radiographers as a source of advice on radiological reporting, though this model has been proposed for rural areas15. Once a decision to transfer a patient was made, a number of logistical problems needed to be overcome. In addition, further treatment delays could arise because of poor communication of x-ray results. Provision of after-hours care is an important part of general practice care in a rural community. The barriers to accessing appropriate radiological services may affect the ability to provide timely appropriate treatment. For example, could clinical acumen be relied on to differentiate between a perilunate dislocation and a distal radius fracture? The urgency of treatment is vastly different.
The GPs certainly understood that clinical practice in rural areas required that they take into consideration that they were practising in smaller communities in more isolated areas. Therefore they did not expect access to the same facilities as their urban counterparts. Their communities also understood this and took it into consideration. Nonetheless, the GPs described important factors influencing their satisfaction with services, many of which did point to elements which could be addressed to improve services. These concerns with providing service to their community have been previously identified as one reason for GPs performing their own radiological services16.
Access to training was an important issue highlighted by our study results, and is consistent with previous research suggesting that rural GPs Australia-wide would like better radiology education. A broad study of satisfaction with Australian GPs' own level of competence indicated that 25% of GPs felt that continuing education in radiology was under serviced17. A second Australia-wide study that investigated rural GPs' continuing medical education (CME) needs for self reported radiology confirmed the perceived CME under-service18 and found that GPs were least confident at reporting chest, cervical spine and skull radiology. Moreover, the varying levels of self-reported competence at producing radiographs described in our study is consistent with other data suggesting that GPs were aware that they did not produce the same quality of radiographs as radiographers16,19. However, in that study, GPs were less concerned about X-ray quality as long as the image was sufficient for them to make a diagnosis and initiate treatment. Rural health practitioners need additional knowledge and skills to provide secondary level care20. Ultrasound is likely to be increasingly relevant to rural clinical practice2,21. Obstetric US has been identified as a high need in continuing professional development21. Education in this area is currently variable between states21. Our study identified a number of problems with the training programs for GPs hoping to operate their own equipment in rural areas. These included training on equipment that was not relevant to them, and accessibility of courses. These are issues that should be considered by course planners.
This study has some limitations. It is a purely descriptive study. We made no attempt to quantify responses. However, this open-ended, inductive methodology is ideally suited to exploring this issue. More structured quantitative approaches, such as surveys, run the risk of the content reflecting preconceived ideas22,23 in a situation such as this when there is little if any relevant literature to inform questionnaire design. This study was undertaken in a small sample of GPs and the sample size precluded attempting to correlate differences in responses with any demographic characteristics of GPs. However, our sampling methodology ensured GPs from a variety of different demographic and geographic backgrounds participated. Nonetheless, the results need to be interpreted and used cautiously in light of differences that will be seen in different settings, for example across different healthcare systems in different countries. Further research is also required to quantify overall levels of satisfaction in rural GPs and more clearly assess which issues have the highest priority among rural GPs.
Conclusion
In conclusion, these data provide new insights into rural radiology services. They can help to inform the diverse stakeholders in the provision of rural health services, including policy makers and funding bodies responsible for rural radiology services, of issues requiring further consideration. Private radiology service providers who either already undertake work in rural areas, or are considering expanding into rural areas could also use this data to improve their services. This qualitative contribution to the creation of an evidence base provides a platform for further research and for the development of strategies to further assess and improve radiology services for rural communities.
References
1. Jones DN. 2002 Australian Radiology Workforce Report. Australasian Radiology 2002; 46: 231-248.
2. Freeman P. The role of ultrasound in the assessment of the trauma patient. Australian Journal of Rural Health 1999; 7: 85-89.
3. Jones NR, Molloy CJ, Kloeden CN, North JB, Simpson DA. Extradural haematoma: trends in outcome over 35 years. British Journal of Neurosurgery 1993; 7: 465-471.
4. McLean MJ, Condon JR. A single issue program in an isolated area: mammography screening in Darwin, NT. Australian and New Zealand Journal of Public Health 1999; 23: 357-361.
5. Madhok R, Kirby P, Fordham J, Stamp P, Green S, Cooper C. Bone densitometry at a district general hospital: evaluation of service by doctors and patients. Quality in Health Care 1996; 5: 36-43.
6. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications, AIHW cat no: PHE 53. Canberra, ACT: AIHW, 2004.
7. Tasmanian General Practice Divisions. 2005 Census of Tasmanian general practitioners. Hobart, Tas: Tasmanian General Practice Divisions, 2005.
8. Hansen EC. Successful qualitative health research: a practical introduction. Sydney, NSW: Allen and Unwin, 2006.
9. Patton MQ. Enhancing the quality and credibility of qualitative analysis. Health Services Research 1999; 34: 1189-1208.
10. Rice PL, Ezzy D. Qualitative research methods: a health focus. Melbourne, Vic: Oxford University Press, 1999.
11. Lewis-Beck MS, Bryman A, Futing Liao T. The Sage encyclopedia of social science research methods, vol 3. London: Sage, 2004.
12. Glaser BG, Strauss AL. The discovery of grounded research: strategies for qualitative research. New York: Aldine De Gruyter, 1967.
13. Rubin H, Rubin I. Qualitative interviewing: the art of hearing data. London: Sage, 1995.
14. Whelan J, Willis K. Problems with provision: barriers to drinking water quality and public health in rural Tasmania, Australia. Rural and Remote Health 7: 627. (Online) 2007. Available: www.rrh.org.au (Accessed 4 April 2008).
15. Smith TN, Baird M. Radiographers' role in radiological reporting: a model to support future demand. Medical Journal of Australia 2007; 186: 629-631.
16. Smith T, Jones P. Remote x-ray operator radiography: a case study in interprofessional rural clinical practice. Journal of Interprofessional Care 2007; 21: 289-302.
17. Booth B, Lawrance R. Quality assurance and continuing education needs of rural and remote general practitioners: how are they changing? Australian Journal of Rural Health 2001; 9: 265-274.
18. Glazebrook R, Chater B, Graham P. Rural and remote Australian general practitioners' educational needs in radiology. Journal of Continuing Education for Health Professionals 2001; 21: 140-149.
19. Smith T. 'Skill transfer' and interprofessional boundaries in rural and remote radiography. Australian Journal of Rural Health 2007; 15: 273-274.
20. Smith J, Hays R. Is rural medicine a separate discipline? Australian Journal of Rural Health 2004; 12: 67-72.
21. Glazebrook R, Manahan D, Chater B, Barker P, Row D, Steele B et al. Educational needs of rural and remote Australian non-specialist medical practitioners for obstetric ultrasound. Australian Journal of Rural Health 2004; 12: 73-80.
22. Pope C, Mays N. Researching the parts other methods cannot reach: An introduction to qualitative methods in health and health services research. BMJ 1995; 311: 42-45.
23. Sale JEM, Lohfeld LH, Brazil K. Revisiting the quantitative-qualitative debate: Implications for mixed-methods research. Quality and Quantity 2002; 36: 43-53.


