Introduction
Malnutrition, defined as being underweight, is a serious public health problem linked to a substantial increase in the risk of mortality and morbidity1. Women and young children are most affected. Diets that place people at risk for malnutrition are those deficient in macronutrients (protein, carbohydrates and fat, leading to protein-energy malnutrition), micronutrients (electrolytes, minerals and vitamins, leading to specific micronutrient deficiencies) or both2,3.
In developing countries, the prevalence of bacterial and parasitic diseases contributes greatly to malnutrition2,4-6. Similarly, malnutrition increases susceptibility to and the severity of infections, and is thus a major cause of illness and death from disease2,7-9, and thus the most important risk factor for the burden of disease in developing countries2,7.
Poverty is the main underlying cause of malnutrition and its determinants2. However the degree and distribution of protein-energy malnutrition and micronutrient deficiencies among a population depend on many factors, including: the political and economic situation; the level of education and sanitation; the season and climate conditions; food production, cultural and religious food customs; breast-feeding habits; prevalence of infectious diseases; the existence and effectiveness of nutrition programs; and the availability and quality of health services10-12.
While rural disadvantage for childhood malnutrition in developing countries is established13-23, little attention has been paid to the rural-urban disparity among women. This research sought to address this imbalance in information by using meta-analysis techniques to examine the results of a number of studies, thereby increasing combined statistical power.
Knowledge of the disease burden of a population, and how that burden is distributed across different sub-populations (eg by gender or type of residence), is important information for defining strategies to improve public health. For policy-makers, disease burden estimates suggest the health gains achievable by targeting specific risk factors; and enable identification of the groups at highest risk and action priorities. This study used nationally representative data from 26 countries in sub-Saharan Africa in order to provide a reliable source of information about the prevalence malnutrition, and its rural-urban disparity among women.
Methods
Data and selected countries
The most recent data available was from October 2007 in the Demographic and Health Surveys (DHS)24 of 26 countries. The various data sets were selected according to the availability of women's anthropometric measurements, to allow comparative analysis. The DHS data sets are from nationally representative surveys of households with at least one woman of reproductive age, usually between 15 and 49 years. The data were collected by in-country research and from statistical agencies, with technical assistance from ORC Macro International. All eligible women in each selected household were surveyed. The surveys were based on two-stage sample designs. In the first stage, enumeration units or 'clusters' were selected from larger regional units within countries. Next, households were randomly selected from within clusters. Detailed information about the women, their male partner, and their children under either 3 or 5 years was gathered.
Measures
Body mass index (BMI) was used as the outcome for this study. Weight was measured by using a solar-powered scale with an accuracy of ±100 g, and height was measured with an adjustable wooden measuring board that is designed to provide accurate measurements (to the nearest 0.1 cm) in the context of a developing-country field situation24. In this study, malnutrition refers to BMI <18.5 using the WHO cut off for underweight25. Pregnant women and women 2 months postpartum were excluded because of weight gain during pregnancy26. Place of residence was defined as either rural or urban as defined administratively in each country.
Statistical analyses
Meta-analysis: Odds ratios (OR) were calculated to assess the association between prevalence of malnutrition and type of residence, comparing rural with urban residents. The techniques used to calculate pooled OR were the Mantel-Haenszel method27 assuming a fixed-effects model, and the DerSimonian-Laird method28 that assumes a random-effects model. The fixed-effects model relates to assembled particular studies, and the random-effects model is used when samples are drawn from a larger number of possible studies, leading to inferences about all studies in the hypothetical population. Cochran's Q test was used to evaluate whether the results were homogenous29. The quantity I2 describes the percentage variation across studies that have heterogeneity30,31. Negative values of I2 were adjusted to zero (no heterogeneity), to give an I2 between 0 and 100%, where larger values show increasing heterogeneity.
Subgroup analyses were performed to investigate the effects of the year of the study, sample size, and sub-region on the pooled odds ratio. To determine the stability of the results, a leave-one-country-out sensitivity analysis was also performed. This analysis evaluated the influence of individual studies by estimating the weighted average OR in the absence of each country.
Meta-regression analysis: An inverse-weighted linear meta-regression analysis investigated the impact of various study characteristics on OR estimates. The independent variable was the natural logarithm of the OR, and explanatory factors included the sample size, sub-region and the calendar year of the survey. This analysis accounted for aspects such as effect modifications of the explanatory factors by performing univariable linear regression analyses for each factor. Those with a p value of less than 0.2 were included in a multivariable regression. All tests were two tailed and p <0.05 was considered significant. Stata 10 (Stata Corp, College Station, TX, USA) software was used for analysis.
Results
This meta-analysis data from 26 DHS countries, years of data collection, and sample sizes are listed (Table 1). Prevalence estimates of underweight women is shown by type of residence (Fig1); the median prevalence for rural and urban women is 10.4% (range, 3.1% to 24.9%) and 6.0% (range, 1.4% to 13.7%), respectively.
Table 1: Description of data sets employed and study sample sizes
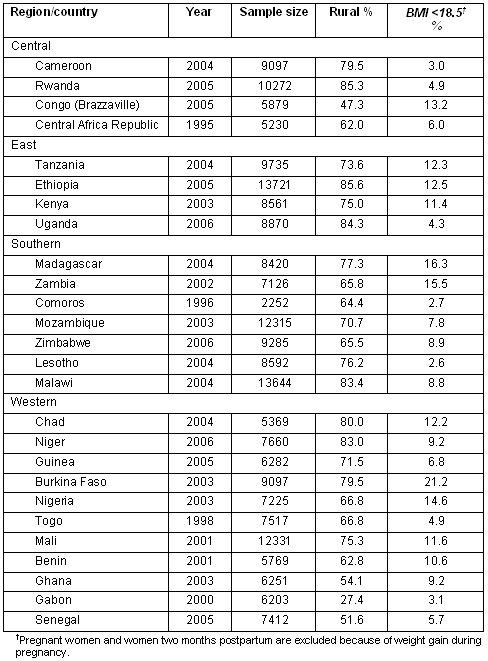
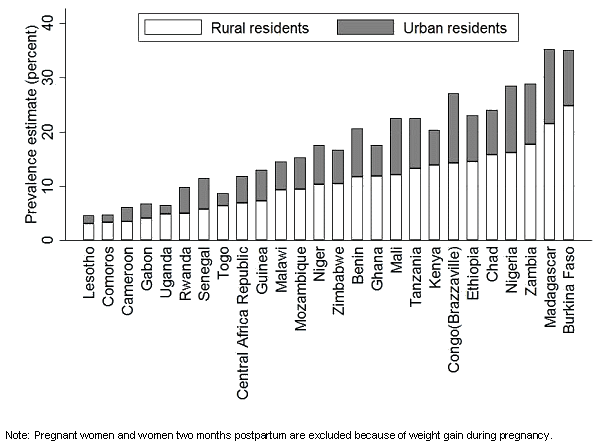
Figure 1: Proportion of women classified as underweight for selected countries included in the study by type of residence.
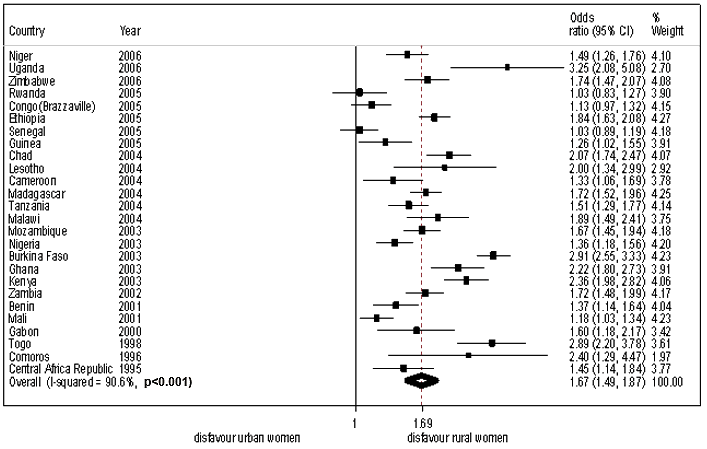
Figure 2: Forest plot of the meta-analysis of 26 studies indicating excess of malnutrition among women in rural areas compared to urban areas.
The OR and 95% CI from individual countries, and pooled results are shown (Fig2). The calculated effect estimates were identical, assuming either a fixed- or a random-effects model (OR 1.67; 95% CI 1.48-1.87) and (OR 1.62; 95% CI 1.57-1.68), respectively. The Cochran's Q test was p = 0.001 (Q = 265.33 on 25 degrees of freedom) and the corresponding I2 was 90.6%, both indicating statistically significant heterogeneity. Subgroup analysis was performed for the geographical sub-region of each the study. Stratification by geographical region reduced statistical heterogeneity within subgroups. Pooled OR for studies conducted in Southern Africa was 1.74 (95% CI 1.63-1.87); for those in Central Africa 1.21 (95% CI 1.05-1.39); for Eastern Africa 2.03 (95% CI 1.60-2.58); and for Western Africa 1.65 (95% CI 1.32-2.07). Statistical heterogeneity remained significant when the studies were stratified by sample size and calendar year (Fig3).
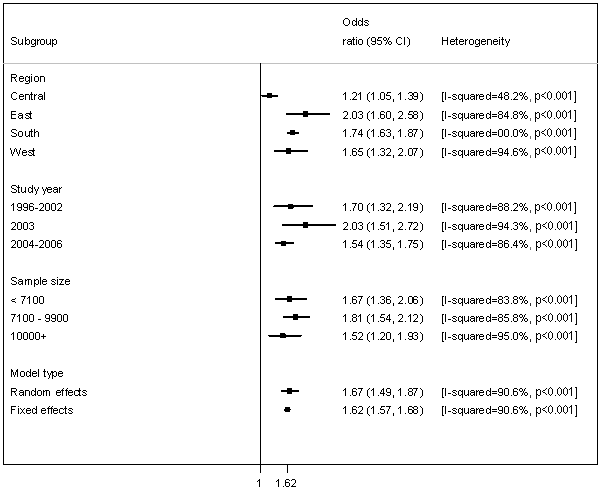
Figure 3: Subgroup analyses on the basis of year of study, sample size and sub-region.
In the leave-one-country-out sensitivity analysis to evaluate the stability of the results, overall effect size was calculated, removing one country at a time. The study conducted in Burkina Faso was found to have the single greatest effect on combined OR; and when omitted, the combined OR reduced to 1.62 (95% CI 1.46-1.80), within the overall estimate for all studies, confirming the stability results.
Meta-regression analysis
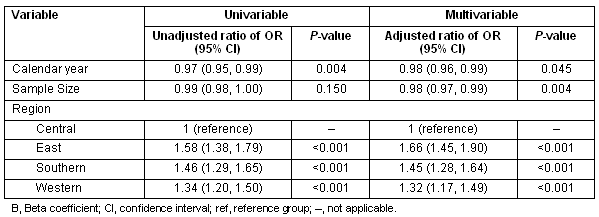
Table 2 shows the univariable and multivariable inverse-weighted linear meta-regression results. On meta-regression, the geographical sub-region where the study was conducted was a significant predictor of heterogeneity on both univariable analysis and when controlling for all variables.
The year of the study was was significant on univariable analysis and marginally significant when the other two factors were controlled for statistically. Sample size of the study was not a significant predictor of heterogeneity on univariable analysis. However, when geographical sub-region and calendar year was controlled for, the unadjusted effect became marginally significant.
Table 2: Inverse variance-weighted linear meta-regression for odds ratio
Discussion
This meta-analysis brought together evidence from 26 sub-Saharan Africa countries, collected between 1995 and 2006. On average, the nutritional status of urban women was better than that of rural women. This is consistent with other studies32-38. The pooled OR of rural women being more likely to be malnourished was 1.68, and at a country-level it was as high as 3.25 (95% CI 2.08 and 5.08). Use of analysis and meta-regression provided evidence that sub-region, sample size, and the year the study was conducted provide a way of partitioning the OR into homogenous groups.
Most studies show that the effects of conditions affecting health in developing countries are more favourable in cities than in rural areas16. In less developed countries, place of residence usually determines people's life-styles, their economic, social and cultural activities and, most importantly, their health conditions39. One explanation of urban health advantage is that cities have more developed healthcare systems, which facilitate public health interventions, such as epidemic diseases control, vaccination and maternal-and-child health programs.
Some studies suggest that the health facilities of rural areas are often ill-suited to delivering required primary health services, and that rural people have to travel a greater distance to obtain care39-41. The urban environment may be more affluent and so supportive of health. Furthermore, developed road and rail links facilitate the regular and abundant supply of foodstuffs to urban populations. Another presumption in the literature is that urban populations are advantaged in terms of water supply, housing and sanitation, and in social programming that directly affects health14. Cities are perceived as having a concentration of wealth, power and western culture, together with services and modern equipment, while villages represent poverty, underdevelopment and lack of services40,41.
Another possible explanation for the observed rural-urban disparity in women's malnutrition in this study is the impact of HIV on food security in rural communities. Of the 33.2 million people worldwide living with HIV/AIDS, an overwhelming 95% live in developing countries42. And within those countries, AIDS is becoming a greater threat in rural areas than in cities43. In absolute numbers, there are more people living with HIV in rural areas. The spread of the epidemic is affecting the remotest villages, cutting food production and threatening the very life of rural communities. In addition, rural communities bear a higher burden of the cost of HIV/AIDS because many urban dwellers and migrant labourers return to their village of origin when they become ill. While household expenditure rises to meet medical bills and funeral expenses, the number of dependents increases43, endangering both short- and long-term household food security. Young women in sub-Saharan Africa are at particularly high risk of HIV infection42 . Food shortages and malnutrition have combined with HIV/AIDS to bring some countries to the brink of crisis44.
Policy implications and future research
Hunger and malnutrition have been found to increase both the incidence and fatality rate of conditions that cause up to 80% of maternal death46. Women who are underweight prior to pregnancy and who gain little weight during pregnancy face are at increased risk of complications and death47. Malnourished mothers are more likely to give birth to low birth-weight babies who face a greatly increased risk of dying in infancy. They are also more likely to suffer stunting during childhood which will greatly increase their own risk of dying during childbirth or giving birth to another generation of low birth-weight babies. Improving nutrition for women and girls throughout their lives could accelerate progress to reducing the millennium development goal by three-quarters between 1990 and 2015, a maternal mortality ratio within reach.
This meta-analysis raises several questions for future research. While this study documents the better nutritional status of urban women, recent research suggest than urban malnutrition is on the rise14. Further research is needed to test for urban-rural differences in the strength of association between key socioeconomic determinants and women's nutritional status. Given established differences in the environment, choices and opportunities of urban and rural dwellers, understanding the relative importance of the various determinants of malnutrition among urban and rural women is the key to designing context-relevant, effective programs and policy responses to address malnutrition. There is also a need further research on the impact of HIV on women's nutritional status. This will provide support to policy-makers and those in public health to raise awareness about the links between poverty, nutrition, and HIV/AIDS, with the hopes of finding wider solutions.
Strengths and limitations of the study
There are a number of caveats to be considered when interpreting these results. The aggregation of different study findings, particularly those with different levels of methodological quality, have been questioned. Additionally, because meta-analysis does not allow casual inferences to be made, the findings must be interpreted with caution45. Significant heterogeneity among studies, indicating substantial variability not attributable to chance, suggests caution in interpreting pooled rural-urban OR. Heterogeneity among studies can be caused by methodological differences such as sample representativeness and rates of non-participation. Another potential source of heterogeneity in is rural/urban differentials. As in other studies, a major problem in these analyses centres on the classification of localities as urban or rural. Some countries classify in terms of administrative boundaries; and others in terms of agglomerations (the physical structure). Other criteria used include population size, population density, percentage of labour force in non-agricultural activities, or a combination of several of these criteria. And even for those which classify in terms of population size, the minimum size required for a locality to be classified as urban varies from one country to another (eg 5000 in Ghana and 20 000 in Nigeria)47. Although this variety of urban-rural classification undoubtedly weakens cross-country comparisons, a uniform definition cannot capture the large variety of urban and rural situations across countries with wide disparities in economic and social development, as in those used in this study. Another limitation of the present analysis relates to the use of BMI as the only measure of malnutrition. Due to the lack of appropriate data on dietary intake and food or calorie consumption, low body weight among rural women was used as proxy for malnutrition. Finally, cross-sectional data only allow observing associations; it is impossible to predict how the relationship between socioeconomic position and BMI may change over time.
Despite these limitations, the study results are significant. Meta-analysis has numerous strengths. It allows for a synthesis of study findings and comparison across multiple studies48. It allows conclusions that are more accurate and credible than those drawn from any one primary study49. In addition, meta-analysis can be used to highlight gaps or limitations in the research literature. The DHS have some important advantages over other surveys. They are often nationally representative, allowing for conclusions that apply to an entire nation50. In addition, numerical values are comparable across countries. Overall, the number of included studies and geographic and socioeconomic diversities constitute a good yardstick for the region, and help to strengthen the findings from the study.
Conclusions
This meta-analysis adds to our knowledge on rural-urban disparity in malnutrition among women in sub-Saharan Africa. The magnitude of the gap described in this study offers a baseline probability for use in evidence-based research that will assist clinicians, researchers and policy-makers in the detection, prevention and treatment of malnutrition among rural women. While these findings do not suggest a redirection of prevention programs from urban to rural areas, they do call for efforts to ensure that malnutrition prevention strategies are applied to all stratas of society.
Acknowledgements
The authors are grateful to the editor and referees for their helpful comments; and to Measure DHS for providing the data.
References
1. Blossner M, de Onis MG. Malnutrition: quantifying the health impact at national and local levels. WHO Environmental Burden of Disease series no 12. Geneva, Switzerland: World Health Organization, 2005.
2. Muller O, Krawinkel M. Malnutrition and health in developing countries. Canadian Medical Association Journal 2005; 173(3): 279-286.
3. Millward DJ, Jackson AA. Protein/energy ratios of current diets in developed and developing countries compared with a safe protein/energy ratio: implications for recommended protein and amino acid intakes. Public Health and Nutrition 2004; 7(3): 387-405.
4. Dickson R, Awasthi S, Williamson P, Demellweek C, Garner P. Effects of treatment for intestinal helminth infection on growth and cognitive performance in children: systematic review of randomised trials. BMJ 2000; 320(7251): 1697-1701.
5. Stoltzfus RJ, Chway HM, Montresor A, Tielsch JM, Jape JK, Albonico M et al. Low dose daily iron supplementation improves iron status and appetite but not anemia, whereas quarterly anthelminthic treatment improves growth, appetite and anemia in Zanzibari preschool children. Journal of Nutrition 2004; 134(2): 348-356.
6. de Onis M, Monteiro C, Akre J, Glugston G. The worldwide magnitude of protein-energy malnutrition: an overview from the WHO Global Database on Child Growth. Bulletin of the World Health Organization 1993; 71(6): 703-712.
7. Murray CJ, Lopez AD. Global mortality, disability, and the contribution of risk factors: Global Burden of Disease Study. The Lancet 1997; 349(9063): 1436-1442.
8. Rice AL, Sacco L, Hyder A, Black RE. Malnutrition as an underlying cause of childhood deaths associated with infectious diseases in developing countries. Bulletin of the World Health Organization 2000; 78(10): 1207-1221.
9. Black R. Micronutrient deficiency - an underlying cause of morbidity and mortality. Bulletin of the World Health Organization 2003; 81(2): 79.
10. de Waal A, Whiteside A. New variant famine: AIDS and food crisis in southern Africa. The Lancet 2003; 362(9391): 1234-1237.
11. Salama P, Spiegel P, Talley L, Waldman R. Lessons learned from complex emergencies over past decade. The Lancet 2004; 364(9447): 1801-1813.
12. Young H, Borrel A, Holland D, Salama P. Public nutrition in complex emergencies. The Lancet 2004; 364(9448): 1899-1909.
13. Lisa C, Smith MT, Ruel, Aida N. Why is child malnutrition lower in urabn than rural? Evidence from 36 developing countries. Washington, DC: International Food Policy Research Institute, 2004.
14. Fotso JC. Urban-rural differentials in child malnutrition: trends and socioeconomic correlates in sub-Saharan Africa. Health Place 2007; 13(1): 205-223.
15. Fotso JC, Kuate-Defo B. Household and community socioeconomic influences on early childhood malnutrition in Africa. Journal of Biosocial Sciences 2006; 38(3): 289-313.
16. Fotso JC. Child health inequities in developing countries: differences across urban and rural areas. International Journal of Equity in Health 2006; 5: 9.
17. Pongou R, Salomon JA, Ezzati M. Health impacts of macroeconomic crises and policies: determinants of variation in childhood malnutrition trends in Cameroon. International Journal of Epidemiology 2006; 35(3): 648-656.
18. Garrett J, Ruel MT. The coexistence of child undernutrition and maternal overweight: prevalence, hypotheses, and programme and policy implications. Maternal and Child Nutrition 2005; 1(3): 185-196.
19. Van de Poel E, O'Donnell O, Van Doorslaer E. Are urban children really healthier? Evidence from 47 developing countries. Social Sciences and Medicine 2007; 65(10): 1986-2003.
20. Kennedy G, Nantel G, Brouwer ID, Kok FJ. Does living in an urban environment confer advantages for childhood nutritional status? Analysis of disparities in nutritional status by wealth and residence in Angola, Central African Republic and Senegal. Public Health and Nutrition 2006; 9(2): 187-193.
21. Semba RD, de Pee S, Sun K, Sari M, Akhter N, Bloem MW. Effect of parental formal education on risk of child stunting in Indonesia and Bangladesh: a cross-sectional study. The Lancet 2008; 371(9609): 322-328.
22. Rajaram S, Zottarelli LK, Sunil TS. Individual, household, programme and community effects on childhood malnutrition in rural India. Maternal and Child Nutrition 2007; 3(2): 129-140.
23. Thang NM, Popkin B. Child malnutrition in Vietnam and its transition in an era of economic growth. Journal of Human Nutrition and Diet 2003; 16(4): 233-244.
24. Measure DHS Demographic and health surveys. (Online) 2007. Available: http://www.measuredhs.com (Accessed 10 June 2008).
25. Mishra V. Effect of obesity on asthma among adult Indian women. International Journal of Obesity and Related Metabolic Disorders 2004; 28(8): 1048-1058.
26. WHO. Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organisation Technical Report Service 2000; 894:i-xii, 1-253.
27. DHS Statistics. Children and Women's Nutritional Status: Women's Nutritional Status. (Online) no date. Available: http://www.measuredhs.com/help/Datasets/Women_s_Nutritional_Status.htm (Accessed 30 May 2008).
28. Mantel N, Haenszel W. Statistical aspects of the analysis of data from retrospective studies of disease. Journal of the National Cancer Institute 1959; 22(4): 719-748.
29. DerSimonian R, Laird N. Meta-analysis in clinical trials. Controlled Clinical Trials 1986; 7(3): 177-188.
30. Cochran W. The combination of estimates from different experiment. Biometrics 1954; 8: 101-129.
31. Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Statistical Medicine 2002; 21(11): 1539-1558.
32. Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ 2003; 327(7414): 557-560.
33. Teller CH, Yimer G. Levels and determinants of malnutrition in adolescent and adult women in Southern Ethiopia. Ethiopian Journal of Health Development 2000; 14(1): 57-66.
34. Mendez MA, Monteiro CA, Popkin BM. Overweight exceeds underweight among women in most developing countries. American Journal of Clinical Nutrition 2005; 81(3): 714-721.
35. Shafique S, Akhter N, Stallkamp G, de Pee S, Panagides D, Bloem MW. Trends of under- and overweight among rural and urban poor women indicate the double burden of malnutrition in Bangladesh. International Journal of Epidemiology 2007; 36(2): 449-457.
36. Ahmed SM, Adams A, Chowdhury AM, Bhuiya A. Chronic energy deficiency in women from rural Bangladesh: some socioeconomic determinants. Journal of Biosocial Sciences 1998; 30(3): 349-358.
37. Bharati S, Pal M, Bhattacharya BN, Bharati P. Prevalence and causes of chronic energy deficiency and obesity in Indian women. Human Biology 2007; 79(4): 395-412.
38. Belahsen R, Mziwira M, Fertat F. Anthropometry of women of childbearing age in Morocco: body composition and prevalence of overweight and obesity. Public Health and Nutrition 2004; 7(4): 523-530.
39. Subramanian SV, Smith GD. Patterns, distribution, and determinants of under- and overnutrition: a population-based study of women in India. American Journal of Clinical Nutrition 2006; 84(3): 633-640.
40. United Nations. Socioeconomic differentials in child mortality in developing countries. New York: Department of International Economic and Social Affairs, 1985.
41. Sastry N. What explains rural-urban differentials in child mortality in Brazil? Social Sciences and Medicine 1997; 44(7): 989-1002.
42. Lalou R, Legrand TK. Child mortality in the urban and rural Sahel. Population: An English Selection 1997; 9: 147-168.
43. UNAIDS. 2007 AIDS epidemic update. Geneva: Joint United Nations Programme on HIV/AIDS (UNAIDS) and WHO, 2007.
44. Food and Agriculture Organisation of the United Nations. HIV/AIDS: a rural issue. (Online) no date. Available: http://www.fao.org/FOCUS/E/aids/aids1-e.htm (Accessed 20 April 2008).
45. Kennedy N, Ramsay A, Uiso L, Gutmann J, Ngowi FI, Gillespie SH. Nutritional status and weight gain in patients with pulmonary tuberculosis in Tanzania. Transcripts of the Royal Society of Tropical Medicine and Hygiene 1996; 90(2): 162-166.
46. Hall JA, Rosenthal R. Interpreting and evaluating meta-analysis. Evaluation for Health Professionals 1995; 18(4): 393-407.
47. Food and Agriculture Organization of the United Nations. The state of insecurity in the world 2005. Rome: Food and Agriculture Organization of the United Nations, 2005.
48. United Nations. Socioeconomic differentials in child mortality in developing countries. New York: Department of International Economic and Social Affairs, New York, 1985.
49. Arriola KR, Louden T, Doldren MA, Fortenberry RM. A meta-analysis of the relationship of child sexual abuse to HIV risk behavior among women. Child Abuse and Neglect 2005; 29(6): 725-746.
50. Rosenthal R, DiMatteo MR. Meta-analysis: recent developments in quantitative methods for literature reviews. Annual Review of Psychology 2001; 52: 59-82.
51. Lawoko S. Factors associated with attitudes toward intimate partner violence: a study of women in Zambia. Violence and Victims 2006; 21(5): 645-56.
Abstract
Introduction:
Malnutrition is a serious public health problem, particularly in developing countries, linked to a substantial increase in the risk of mortality and morbidity. Women and young children are most often affected. Rural disadvantage is a known factor, but little attention has been paid to rural-urban disparity among women. To provide a reliable source of information for policy-makers, the current study used nationally representative data from 26 countries in sub-Saharan Africa to update knowledge about the prevalence malnutrition and its rural-urban disparities among women. The data sources were the demographic and health surveys of 26 countries conducted between 1995 and 2006.Methods: The methods included meta-analysis, meta-regression, sub-group and sensitivity.
Results: Overall, rural women were 68% more likely to be malnourished compared with their urban counterparts. In the meta-regression analysis, sub-region, sample size, and the year the study was conducted explained the observed heterogeneity.
Conclusions: This meta-analysis provided usable data for women in sub-Saharan Africa. The magnitude of rural-urban malnutrition disparity revealed provides a baseline that will be of assistance to clinicians, researchers, and policy-makers in the detection, prevention and treatment of malnutrition among rural women.
Key words: Africa, children, malnutrition, rural-urban, women.

