Introduction
The health needs of rural communities have changed over time for a number of reasons including the ageing population, the ebbs and flows of market competition, and often rapid changes in the availability and application of information technology, and the 'passive patients' who have become active consumers1.
Consumers are becoming more informed of health and health service options and expect quality care. According to Swanson2 these changes must be considered when preparing nurses for the future. Additional skills are required to cater for the ever-increasing range of tasks expected of a nurse3. In turn, the changing needs in the community places additional requirements on universities to produce nurses who are able to match the growing demands.
An important part of this developmental process involves consideration of the views of stakeholders. One such important group of stakeholders in a rural setting is the local community.
The rural community, as consumers of health services, are in the best position to report their preferred type of new graduates4 who will best meet their specific needs. Sharpe5 states that patients should be able and allowed to comment on the quality of care they expect, and that this information should be used by health providers to guide the development of services. The focus of the current study concerns the rural community's perception of nurses and nurses' attributes. It identifies the kind of nurses the consumers expect. According to Kulig et al6, nurses working in rural areas hold the position of informal community leaders, have intimate knowledge of their communities and, therefore, have opportunities for policy involvement that will subsequently improve the health of the rural dwellers.
Currently in Australia, nurses are educated in tertiary institutions. According to the states/territories and Commonwealth Departments of Health and Education, the tertiary education of nurses has resulted in the evolution of new core qualities expected in nurses and midwives. The Australian Health Ministers' Advisory Council believes these core qualities of nurses and midwives are: professionalism, high-level qualifications and skills, versatility, excellent decision-making and management; team playing; caring; patient/client championing and communication7. It is not clear, however, whether these core qualities are equally important in urban and rural settings.
Australian research6,7 suggests nurses practicing in rural settings are different from those employed in metropolitan settings. Special issues for those in rural areas include a lack of anonymity; isolation from support services; knowledge of the community; and the requirement to care for relatives and friends. Due to the limited number of healthcare providers, rural nurses are required to have a very broad knowledge base, and often must extend their practice into other professionals' domains8. This view is not shared by Offredy9 who does not see metropolitan practitioners as different to rural. Offredy9 perceives that remote and rural practice is part of advance nursing practice and, therefore, the generic attributes include competencies, accountability, diagnostic pathology, prescribing medications, and referral procedures. Reid10 argues that the employing authorities want graduate nurses who possess generic skills in communication, cognitive attributes, knowledge, interpersonal skills, work context, and meta-attributes.
A Nursing Council of New Zealand11 report predicts graduate nurses' skills and attributes may become specialised for 2010 and beyond. According to the report, better education, increased availability of information, advances in information systems and information management, together with transformed medical technology will shape the attributes of the future nurse. Nurses will need to be flexible and adaptable, knowledgeable, culturally safe and will possess skills in clinical inquiry and people, health technology, information technology, along with business and management. The Australian Nursing Council's Competency Standards for Registered Nurses suggest that core graduate nurses' attributes include the following characteristics: critical analysis, problem solving, information literacy, knowledge transfer, interdisciplinary base knowledge, written communication skills, oral communication skills, sensitivity to multicultural issues, awareness of ethical issues and conduct, independent initiative and self-confidence, group team skills, discipline knowledge and basic computer skills12. Reid10 reviewed the literature and identified several core skills for all graduate nurses. These include effective interpersonal skills, verbal and written communication skills, analytical skills, leadership and management qualities, teamwork, problem identification and solving, creative and lateral thinking.
The Australian Nursing and Midwifery Council reviewed the competency standards for all Australian registered nurses in 2004/2005. This council has established the guidelines for assessment of registered nurse's competence prior to their annual renewal of license to practice in Australia13. These guidelines are also used by Australian universities when developing nursing curricula for undergraduate nurses in all settings. The guidelines expects the registered nurse to provide evidence-based nursing care to people of all ages and backgrounds, including the promotion of health and the prevention of illnesses and alleviation of suffering. The registered nurse must collaborate within the multidisciplinary healthcare team to achieve the goals and outcomes of individuals, groups, families and communities, in a wide range of settings. The registered nurse takes a leadership role in care coordination across different care contexts to optimize health outcomes. It is expected that the registered nurse contributes to lifelong learning, professional development of herself/himself and others, research activity, clinical supervision, healthcare policy and clinical guidelines.
Baron-Epel, Dushenat and Friedman14, asserts that, if the attributes are to serve the consumer in the most effective way, then the consumer should have input into in what they perceive to be essential characteristic. They identified the attributes rated highly by the consumers as the ability to provide 'answers to questions' and 'listening to problems'. Oermann and Templin15 identified important attributes of quality health care according to consumer perspectives as: keeping up-to-date and well informed; being able to communicate with the nurse; spending enough time with the nurse and not feeling rushed during visit; having a nurse teach about illness, medication, treatments, and staying healthy; and being able to call a nurse with questions. Bendall-Lyon and Powers16 identified attributes that consumers valued during their healthcare service to be responsiveness, friendliness, courtesy, competence and accessibility. They also found communication, interpersonal relationship between patient and caregivers, and caregiver expression of empathy, as important attributes in nurses. According to Webb17 consumers of health care want nurses who are responsive to their needs, congenial in their interactions, competent and educative.
The health care needs of rural people may not be adequately addressed by models that are generated from urban environments18. Input from the rural setting is also important. Weinert and Long19 emphasised that 'the need for those providing services to understand and work with rural people, rather than provide directives or advice based solely on professional knowledge'.
They further stressed that 'the health care programs, services, and practitioners will not be acceptable to, nor well utilized by, rural people unless they address relevant needs through methods congruent with rural life styles'19.
Studies have shown that there are several important characteristics of rural communities relevant here. The rural community, as compared with other population subgroups, is the most disadvantaged because of a relative lack of healthcare access20. Characteristics of the rural elderly include being independent, maintaining their dignity, valuing their privacy, self-sufficient and 'hardiness' (ie maintaining their perceived level of health despite the fact that they are ageing with chronic illness)21. Rural dwellers view 'health needs' are secondary to 'work needs', because they define health as being able to work (ie present time-oriented), or to being productive and performing their daily activities18. Rural residents may only seek health care, when they are very ill at the point of needing hospitalization, because they value independence and resist help from 'outsiders' or 'strangers'. This self-reliant nature of rural people to only seek help from family, relatives, close friends and resist help from people viewed as outsiders, is a healthcare challenge18. In some rural settings nurses are the sole healthcare provider, with little support22. As frontline healthcare workers, rural residents have an expectation of nurses to be both generalists and specialists, demonstrating excellent clinical skills at all times23,24.
The definition of the term 'rural' is very contextual
The second definition, the Accessibility/Remoteness Index of Australia (ARIA), is a measure of accessibility to services. This definition refers to remoteness according to access goods and services26. It refers to areas that are 'highly accessible', 'accessible', 'moderately accessible', 'remote - very restricted accessibility' and very remote - very little accessibility. The third definition, the Australian Standard Geographic Classification (ASGC), groups areas with similar characteristics. It includes major cities, inner regionals (those on the outskirts of major cities), remote, very remote and migratory27.
The aim of this article was to develop a questionnaire to be used to identify the key attributes (qualities and skills) that rural consumers expect in new nurse graduates in a RRMA 3 classified regional city.
Methods
The study was approved by the University of Melbourne Human Research and Ethics committee.
A questionnaire was designed to identify the importance attached to a set of attributes expected in nurse graduates. The items included in the questionnaire were derived from eight focus groups conducted with residents from rural communities in Victoria, Australia.
Focus groups
Thirty participants from four social organizations were included: (Returned Services League club n = 8; Nursing Mothers' group n = 10; local service club n = 10; skill training group n = 12. Participants from four professional sectors n = 34 were also included: (private hospital n = 11; health care public service department n = 7; post-registration undergraduate nurses group n = 18; and sub-acute public hospital n = 8). Ages of participants ranged from 18 to 80 years. The items generated from the focus groups included organisational practices, resource management, staff relations, quality assurance, implementation and change. These items from a wide range of members captured the cross-sectional views of a rural community's expectation of a graduate nurse, thus provided the framework for the questionnaire.
Questionnaire
The questionnaire was piloted with a separate non-professional focus group in another rural town in Victoria, and was modified following feedback from participants.
The final version of the questionnaire contained 38 items. Participants were asked to rate the importance of each item for the community on a five-point Likert scale (5 = extremely important, 4 = very important, 3 = moderately important, 2 = possibly important, 1 = not important at all). Additional demographic questions were included in the questionnaire, including gender, age and place of birth.
Procedure
One per cent of the 94 600 adults (≥16 years) of a regional city was surveyed using cluster sampling technique. The Australian regional city for the study is classified as RRMA 3 with some restriction to accessibility of some goods, services and opportunities for social interaction. Prior to sampling, each of the local government areas was divided into clusters of 15 to 17 households each. In total 946 questionnaires were hand delivered to the households and collected within one week by a team of five trained agents. If there were more than one adult in the household, the adult whose birthday was the closest to the day of the visit was requested to fill in the questionnaire. There were no exclusion criteria for the subjects, and all households within the clusters were sampled. Respondents with poor vision, literacy problems or other difficulties were assisted upon request during data collection. To safeguard anonymity, names and addresses of respondents were not recorded. Sealed envelopes were provided for the completed questionnaire by the respondents to ensure confidentiality of the responses. Surveys were completed and returned by 656 people, giving a response rate of 69%.
Statistical analyses
Exploratory factor analysis was performed on the 38 items using SPSS (SPSS inc; Chicago, IL, USA), after first confirming that the data were suitable for factor analysis. Principal components analysis (PCA) was used to extract the factors, followed by oblique rotation of the factors using Oblimin rotation (delta = 0). The number of factors to be retained was guided by Kaiser's criterion (eigenvalues above 1), inspection of the scree plot, and the interpretability of the items. Cronbach's alpha was used to assess the internal consistency of the subscales identified from the PCA.
Results
The majority of the 656 people who returned the questionnaire were female (68%), 30% were male, while 2% of the respondents did not identify their gender. There were 66.5 % of respondents between the ages of 21 and 60 years. The majority of the respondents (75.6%) were born in Australia, with 3.2% born in the UK and 1.7 % in the Netherlands.
Principal Components Analysis of the 38 items revealed five factors with eigenvalues exceeding one, accounting for 47.4% of the total variance. Table 1 shows the loading of items on the five factors. Items with loadings greater than + or - 0.3, that is, those items where approximately 10% of the common factor variance was associated with the factor in question, were used to characterise the factor solutions.
Component 1 was labelled Sympathetic/Patients' Welfare Factor. There were 11 items that loaded strongly on this factor, with loadings ranging from 0.71 to 0.33. The top four items within this factor were: 'Nurses should be sensitive to the emotional needs of patients' (loading of 0.71), 'Nurses should be good listeners' (0.70), 'Nurses should be sympathetic' (0.69) and 'Nurses should be compassionate' (0.67).
The second component, Contextual knowledge/Interpersonal skills, contained seven items with factor loadings from 0.69 to 0.52. The top two items were 'Nurses should be able to handle money and budgets well' and '...have knowledge of financial and social situations of their patients/employer/ community' with loadings of 0.69. Similarly, items 'Nurses should have good skills in resolving conflicts' and 'Nurses should have well developed counselling skills' had loadings of 0.61 and 0.55, respectively.
Component 3 was labelled Professionalism and contained ten items relating to professional behaviour. The top two items were: 'Nurses should be able to apply theory to practice in daily nursing' (loading of 0.77) and 'Nurses should be able to apply their knowledge to new circumstances' (loading of 0.73).
The fourth component was identified as Personal attributes, with seven items relating to personal appearance (neat and tidy), personality (cheerful, patient) and their skills (good organizational and time management skills). The item 'Nurses should be neat and tidy' had a high loading of 0.79.
The final component was labeled Accountability, containing only three items. The two top items were 'Nurses should be able to recognise their own limitations' (loading of 0.48) and 'Nurses should be aware of their legal rights and those of their patients' (0.47).
Table 1: Pattern matrix for principal components analysis with Oblimin rotation of five factor solution
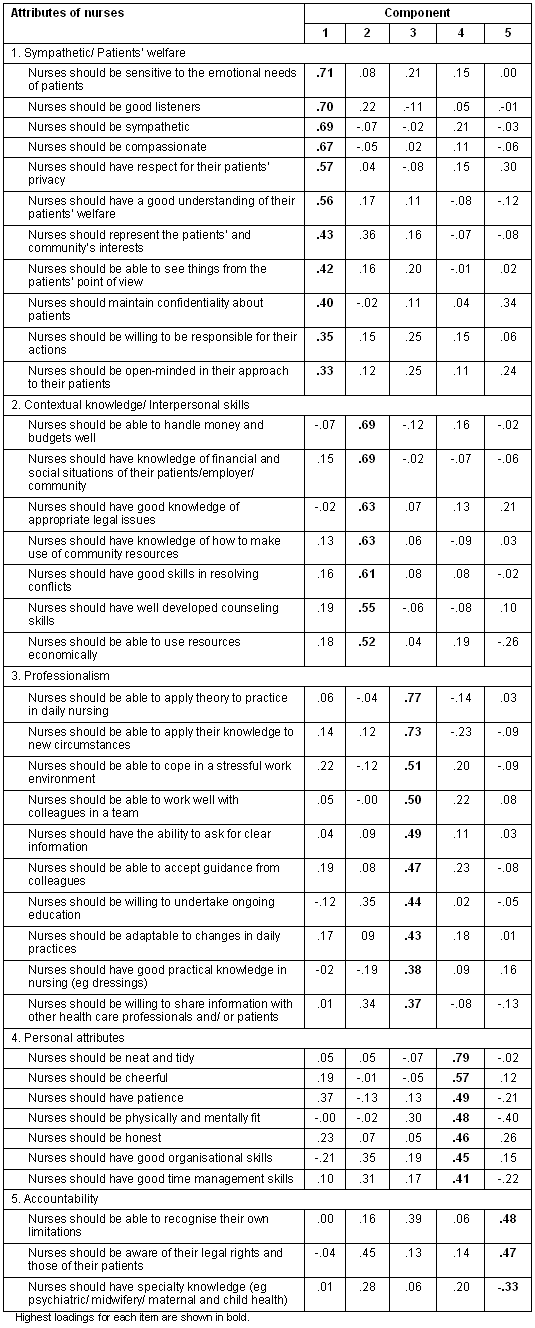
Cronbach alpha reliability coefficients were computed for each of the sub-scales identified from the PCA (Table 2). Four of the sub-scales recorded Cronbach alpha values exceeding .7, indicating satisfactory internal consistency. The Accountability subscale, fell below this value (alpha = .58) due to small number of items (n = 3).
Table 2: Cronbach's alpha values for each subscale

Discussion
The aim of the study was to identify the key attributes in new nurse graduates according to the community consumers. Psychometric analysis found support for five factors: Sympathetic/Patients' welfare, Contextual knowledge/interpersonal skills, Professionalism, Personal attributes, and Accountability.
The Sympathetic/ Patient's welfare component contains items that relate to being empathetic to clients. They indicate that nurses should listen to the client's point of view, understand what the clients are experiencing and be supportive. This component also relates to the notion of nurses being sensitive to the wellbeing of patients. One of the qualities the community expected, within the Sympathetic/ Patient's welfare component of the graduate nurse, is to be 'a good listener'. Orcajada28 states that many nurses enjoy talking too much and may even miss the message conveyed by the patients. On the other hand, some hospital personnel are 'too busy to just sit and listen to patients' and, therefore, may appear to show a lack of compassion towards the vulnerable and distraught patients29. Another important quality expected in graduate nurses within the Sympathetic/Patient welfare component was compassion. Compassionate care involves awareness of the patient's experience so as to share their burden and enable independence and dignity30. Compassion involves both insight and thoughtfulness and the ability to relate to a suffering individual in such a way as to alleviate the pain31. Von Dietze and Orb31 suggest compassion should be part of the integral component of nursing care. It is sometimes difficult for nurses to be compassionate in their caring when administrative and financial factors are challenging their practice. For example, a patient may be discharged early from hospital because the system cannot cope with daily hospital bed costs.
Patient privacy was also identified as an important item within the Sympathetic/Patient's welfare component.
Woogara32 argues that nurses need to be open with staff and patients while observing an accepted level of patient privacy as there is a delicate balance between assisting and intruding33. DiFillipo 33agrees and warns nurses to be careful of the boundary between 'assisting and intruding', as far as the patient privacy is concerned. Treating a person with dignity and respect is also an essential skill for nurses, within the patient welfare component. According to Douglas34, nurses are the patients' front-line advocates and failing here means they fail in their duty as a nurse. The current staff shortages increase nurses' workload and potentially affects the quality of care but, more importantly, impacts on the patient's welfare35. Items on this factor related to aspects of patients' welfare perceived to be important to the community. Other related items indicated that nurses should be sympathetic to the clients' concerns.
The second component consisted of two aspects identified as Contextual Knowledge/ Interpersonal skills. The first aspect indicated that it is preferred that nurses have a broad contextual knowledge of issues associated with practice of their profession such as finance, resources etc. The remaining items in this component relate to the requirement for nurses to have good interpersonal skills. The contextual knowledge is an important quality in graduate nurses because they are expected to manage resources and expenses in a climate of ever-increasing demand36. The nurse graduates who will move into management roles have to weigh up the competing demands on nursing resources. Nurses have to decide how to maximise health gain within the given circumstances. Nurses' decisions must be rational, defendable and transparent37. They need to familiarise themselves with economic evaluation to ensure resources are deployed to the best possible effect38.
The second aspect of the Contextual knowledge/ Interpersonal skills factor is the attribute that relates to interpersonal skills. Conflicts are inevitable at the workplace because of nurses' personal characteristics. Nurses' backgrounds can vary substantially in diversity of racial, social, cultural and political characteristics. If nurses are to function in a collegial manner, they must have developed skill in resolving conflicts and counselling39. The failure to manage conflict effectively is one of the most common causes that prevent nurses from developing to their fullest potential2. When conflict remains unresolved, trust and commitment do not exist2. These items also indicate that nurses should have a broad contextual knowledge on issues associated with practice. Items in this factor related to knowledge about finance, legal implications of malpractice, economic of health care, accessing resources and available social services, and to the need to maintain effective interpersonal skills. The growing demand for quality service and with limited hospital budget, emphasizes the need for strong interpersonal skills in new graduates.
The third component, Professionalism conveys a strong message that the community expects nurses to display professional characteristics. There is the belief that nurses should maintain a sound knowledge through continuing education, are able to share and apply that knowledge to work situations, ask questions when in doubt and accept guidance given by their colleagues. Within the component of Professionalism is the notion of being a team player or 'able to work well with colleagues in a team'. Being a team player in a healthcare setting is often challenging. The role of being an effective team player can be negatively influenced by a variety of factors including large team size, lack of familiarity with the team, regular changing of staff in a team, lack of a common purpose for the team and the physical layout of the work environment40. To overcome these challenges nurses are encouraged to seek support from each other in work settings, improve mutually beneficial relationships41 and promote collegiality. Grindel42 suggests it is possible for nurses to create a 'nurse-friendly' culture in the workplace so that they can achieve personal objectives and positive organisational outcomes. Nursing professional bodies can take an active part in developing the professionalism of nurses by bringing them together and empowering them43. Sullivan and Benner44 states that preparing nurses for the profession is to educate them in managing complex circumstances. This enables them to not only master the technical craft of the profession, but also develop analytical skills and learn the principles that make possible creative adaptations to new circumstances. Embedded within the component of Professionalism is the notion of coping in stressful work environments. Nurses must accept that nursing is a stressful occupation45. Some of the workplace stressors (such as dealing with patient communication, emotions when dealing with illness and death, working with other health professionals, shift work) can have immediate or long-term physical, emotional, and psychological problems for the nurse. When coping skills are not adequate, burnout may result46. There is an expectation by the rural community that nurses who are currently educated through the universities should be well equipped with theories and knowledge that should be applied to practice.
The fourth Personal attributes component relates to the concept that nurses should, apart from having good organisation skills, be physically and mentally strong and be presentable. The two items that have a high loading under this component were being 'neat and tidy' and 'cheerful'. LaSala and Nelson47 stressed that appearance, behaviour and dress play an important role in the image of a nurse. Clothing and hair should be neat and clean, jewellery should be kept to a minimum, tattoos should be covered during work hours, shoes should be clean and functional in the work setting, and makeup for women should be subtle47. There is an expectation that nurses are expected to set a clear professional standard, that is, come to work appropriately dressed48. The item within the factor of being cheerful is important and can lead to the creation of a positive work environment. Thompson48 acknowledges that nursing, being one of the roughest and most stressful jobs, can create tensions that become so overwhelming that laughing is the only alternative to crying. Humour can be the healthiest and most compassionate way to help staff and patients cope during very stressful situations. Manion49 found that being cheerful or joyful at work is an individual issue. She asserts that the organisation does not have an active role in influencing the experience of joy.
The fifth component, Accountability, captures the general notion of accountability to the public in nursing practice. The Accountability component relates to nurses being able to justify their actions and accept responsibility for them. Nurses are accountable not only to themselves, but to the public, the profession and also the employer. If nurses want to claim professional status, they must also be accountable50,51. The attributes of accountability were considered an integral part of satisfactory service. New graduate nurses when providing care 'should be able to recognise own limitations' otherwise, giving advice without an in-depth knowledge on issues can lead them to face the legal consequences52. It is sometimes difficult to work within their limitations when there is a shortage of staff. Melling and Hewitt-Taylor53 state that the British Department of Health supports nursing and other professions, allied to medicine, to increase their role flexibilities. The Department sees the benefits to doctors, in using non-doctors for a wider role. The help from non-doctors will assist in reducing the inpatient waiting times. Other benefits for nurses and allied health professionals can include a provision of more patient-centred care and cost-effectiveness (because one member can deliver the majority of aspects of care). Nurses, as members of one of the non-doctor health professions, may increase their job satisfaction with autonomous decision opportunities. Although medical associations may favour the expanded roles for nurses and recognise that nurses can and will do them, nurses should know their limitations and be aware that the more the nurse undertakes an expanded role, the greater his/ her legal accountability54,55. As stated by other studies, the Australian rural community expected that nurses 'should be aware of their legal rights and also those of the patients'56. Nurses have a responsibility to promote a safe working environment and should be aware of the obligations under current legislations57.
Implications of the study for nursing in rural settings
According to Lee21 nurses who want to work in a rural environment should have a working knowledge of the local resources, as was expected by the rural community in this study. But nurses must gain acceptance by and entry into the local network prior to gaining contextual knowledge, otherwise they will not share local information and be seen as 'outsiders'. A strategy by Weinert and Long22 to gain acceptance into the community 'circles' is for the nurse to be involved in informal diverse local recreational activities. Certainly this suggestion is useful but it raises the practical issue of overlapping relationship and, subsequently, the notion of maintaining confidentiality as was expected by the rural community in this study. Scopelliti et al58 stressed the point that in some isolated places, doctors, patients and nurses know each other outside the healthcare practice. Sometimes it may be difficult to discuss some sensitive health issues (eg mental illness or sexual health) with the consumer who is also a friend from the local club. Preparing nurses to work in a rural setting may need a planned and coordinated orientation program.
The current competency standards by the Australian Nursing and Midwifery Council (ANMC) do not specify personal attributes (such as being neat and tidy, cheerful and honest) as important. According to the ANMC these qualities may have been considered outdated, but the findings of this study clearly showed that they are still important24. It is, therefore, important for universities to encourage these qualities in their graduates, through a system of regular feedback from consumers to curriculum planners and employers.
One of the qualities of nurse expected by the rural community in this study is 'willing to undertake ongoing education'. According to Long and Weinert18 nurses in rural areas see themselves as separated from collegial support because of the distance. Although current modern technology (eg video - conferencing) allows nurses in some rural sites to link for professional support, this remains an issue in very remote and poorly resourced settings. Preparing nurses for rural work should encompass education and training to ensure versatility in information technology, in order to maintain professional links through electronic communication.
Good organisational and time management skills are essential qualities for nurses practising in rural settings, as identified in this study. These skills are highly relevant when dealing with rural people, many of whom are farmers. It should be understood23 that rural farming residents see work to be of a higher priority compared with their health. As such, the rural community is occupied with farm work, particularly during harvesting, and shearing seasons. Expecting rural dwellers to leave their farms, especially during such busy times, is impossible. As Nicholls23 asserts, rural health services (including nursing) must fit around the daily life of the rural residents, rather than expecting the resident to fit health care in with that life, as can be the case in urban or city settings. Therefore, employers must ensure that intending rural nurse practitioners are aware of this issue.
To deliver quality service in a rural community experienced nurses working in rural areas must have independence and self-direction24, unlike new graduates who still need to 'accept guidance from colleagues' and 'recognize their own limitations'. With the lack of rural workforce59, appropriate guidance for the new nurse graduate is not possible, unless they are supported by large centres. The nurse is required to function in several capacities, including supervisor, administrator, educator, care giver24 and, therefore, needs to have a broad range of qualities, as identified in this study. Although, these expectations may be over-optimistic at times and difficult to fulfill, it is important to understand that this is the consumer's perspective. In order to enable nurses to fulfill their clients' expectations, universities and employers need to capture these views through a client feedback system and promote and foster development of those qualities that are feasible.
Limitations of the study and further research
Although this study provides a useful rural consumer perspective, there are a number of factors that limit its generalizability. The rural community in this study is a large rural centre that has some restrictions to accessibility of some goods, services and opportunities for social interaction, and therefore may not truly reflect the issues of all rural places with smaller populations. Further investigation of this issue is needed in other rural and remote settings; and for comparative purposes, also in urban areas. The approach adopted here could also be expanded to explore community perceptions of important attributes of graduates from other courses, such as medicine, dentistry, pharmacy. A comparative study of the community expectations of attributes with professional competencies would be useful for curriculum decisions.
Conclusion
This study has identified key nurse attributes from an Australian rural community's perspective. The characteristics of rural healthcare settings impose challenges for quality nursing service provision. Preparing nurses to work in rural settings involves consideration of a number of factors including: educational programs; employer support; planned and coordinated rural orientation strategy; and rural support issues. The attributes identified in this study could be used to better guide the training of nurses for employment in rural settings.
References
1. Grbich C (Ed.). Health in Australia: sociological concepts and issues, 2nd edn. Sydney, NSW: Prentice Hall Australia, 1999.
2. Swanson J. Leadership is complex and uncertain times: Is nursing ready? American Academy of Ambulatory Care Nursing 2002; 24(2): 1.
3. Child R, Lingle G, Watson P. Managing diversity in the environment of care. Seminars for Nurse Managers 2001; 9(2): 102-109.
4. Calman L. Patients' views of nurses' competence. Nurse Education Today 2006; 26(8): 7197-25.
5. Sharpe A. A patient's view of nursing care - do we listen? Journal of Orthopaedic Nursing 2000; 4: 78-81.
6. Kulig JC, Nahachewsky D, Thomlinson E, Macleod MLP, Curran F. Maximizing the involvement of rural nurses in policy. Nursing Leadership 2004; 17(1): 88-96.
7. Australian Health Minister's Advisory Council - National Nursing & Nursing Education Taskforce. National review of Nursing Education - Our Duty of Care. (Online) 2002. Available: http://www.dest.gov.au (Accessed 17 August 2006).
8. Beatty R M. Continuing professional education, organizational support, and professional competence: dilemmas of rural nurses. Journal of Continuing Education in Nursing 2001; 32(5): 203-209.
9. Offredy M. Advanced nursing practice: the case of nurse practitioner in three Australian states. Journal of Advanced Nursing 2000; 31(2): 274.
10. Reid J. Nursing Education in Australian Universities: report of the National Review of Nurse Education Sector and Beyond. Canberra, ACT: Australian Government Publishing Service, 1994.
11. Klynveld, Peat, Marwick and Goerdeler. Strategic review of undergrduate nursing education. Final report to the Nursing Council. Wellington, NZ: KPMG, 2001.
12. Scoufis M. Graduate attributes projects: a focus for grass roots change in teaching and learning practices (Online) 2000. Available: http://lsn.curtin.edu.au/tlf/tlf2000/scoufis.html (Accessed 17 August 2006).
13. Council ANM. National Competency Standards for Registered Nurses. (Online) 2008. Available: http://www.anmc.org.au/docs/Competency_standards_RN.pdf (Accessed 8 July 2008).
14. Baron-Epel O, Dushenat M, Friedman N. Evaluation of the consumer model: relationship between patients' expectations, perceptions and satisfaction with care. International Journal for Quality in Health Care 2001; 13(4): 317-323.
15. Oermann M, Templin T. Important attributes of quality health care: consumer perspectives. Journal of Nursing Scholarship 2000; 32(2): 167-72.
16. Bendall-Lyon D, Powers TL. The impact of structure and process attributes on satisfaction and behavioural intentions. Journal of Services Marketing 2004 2004; 18(2): 114-121.
17. Webb B. A study of complaints by patients of different age groups in an NHS trust. Nursing Standard 1995; 12-18 July; 9(42): 34-37.
18. Long KA, Weinert C. Rural nursing: developing the theory base. Scholarly Inquiry for Nursing Practice: An International Journal 1999; 13(3): 257-268.
19. Weinert C, Long KA. Understanding the health needs of rural families. Journal of Family Relations 1987; 36: 450-455.
20. Kennedy V. Rural access to a regular source of medical care. Journal of Community Health 1979; 4(3): 199-203.
21. Lee HJ. Rural elderly individuals: strategies for delivery of nursing care. Nursing Clinics of North America 1993; 28(1): 219-230.
22. Weinert C, Long KA. Support systems for the spouses of chronically ill persons in rural areas. Journal of Family and Community Health 1993; 16: 46-54.
23. Nichols E. Response to: 'Rural nursing: developing the theory base'. Scholarly Inquiry for Nursing Practice: An International Journal 1999; 13(3): 271-274.
24. Bigbee JL. The uniqueness of rural nursing. Nursing Clinics of North America 1993; 28(1): 131-144.
25. Muula A. How do we define 'rurality' in the teaching on medical demography? Rural and Remote Health 7: 653. Available: www.rrh.org.au (Accessed 3 July 2008).
26. DoHaAC (DHAC). Measuring remoteness: Accessiblity remoteness index of Australia (ARIA). Canberra: ACT Information and Research Branch, Commonwealth Department of Health and Aged Care, 2001.
27. Glover J, Tenant S. Remoteness areas statistical geography in Australia: Notes on the accessibility/ remoteness index for Australia ARIA+ version working paper. Adelaide, SA: Public Health Information Development Unit: Adelaide, 2003.
28. Orcajada E, Rao L. The art of active listening. Nursing Spectrum (New York/New Jersey Metro Edition) 2005; 17A(21): 17,30.
29. Doherty L. A new focus on caring principles. Nursing Times 14-20 March 2006; 102(11): 13.
30. Abrams SE. Essentials of practice. Public Health Nursing 2006; 23(4): 295-296.
31. von Dietze E, Orb A. Compassionate care: a moral dimension of nursing. Nursing Inquiry 2000; 7: 166-174.
32. Woogara J. Privacy and dignity of cancer patients: a qualitative study of patients privacy in UK National Health Service patient care settings. Journal of Cancer Education 2005; 20(2): 119-123.
33. DiFilippo JA. How well do we ensure privacy? Rehabilitation Nursing 2003; 28(4): 103.
34. Douglas P. Profile: Pam Douglas nurse and whistleblower. Revolution 2000; 1(1): 9.
35. Yoder-Wise PS. A threat to the professionalism of nursing. Journal of Continuing Education in Nursing 2001; 32(4): 149.
36. Weaver D. Controlling expenditure and managing resources. Nursing & Residential Care 2005; 7(2): 64-65.
37. Douglas HR, Normand C. Economic evaluation: what does a nurse manager need to know? Journal of Nursing Management 2005; 13(5): 419-427.
38. Richardson G, Griffiths P. The costs of care; economic evaluation of treatments. Nursing Times 2000; 96(44): 44.
39. Burke LE, Fair J. Promoting prevention: skill sets and attributes of health care providers who deliver behavioral interventions. The Journal of Cardiovascular Nursing 2003; 18(4): 256-266.
40. Kalisch BJ, Begeny SM. Improving nursing unit teamwork. Journal of Nursing Administration 2005; 35(12): 550-556.
41. Hader R. Partnerships: thrive with a little help from your friends. Nursing Management 2006; 37(3): 6.
42. Grindel C. The nurse's responsibility in creating a 'nurse-friendly' culture in the workplace. MEDSURG Nursing 2006; 15(3): 125-126.
43. Campbell SL. Cultivating empowerment in nursing today for a strong profession tomorrow. Journal of Nursing Education 2003; 42(9): 423-426.
44. Sullivan W, Benner P. Challenges to professionalism: work integrity and the call to renew and strengthen the social contract of the professions. American Journal of Critical Care 2005; 14(1): 4, 78-80.
45. McGough G. Nurses have taken for granted the goodwill of the public for too long. Nursing Times 17-23 November 1999; 95(46): 45.
46. DiGiacomo M, Adamson B. Coping with stress in the workplace: implications for new health professionals. Journal of Allied Health 2001; 30(2): 106-111.
47. LaSala KB, Nelson J. What contributes to professionalism? MEDSURG Nursing 2005; 14(1): 63-67.
48. Thompson SA. The top 10 qualitites of a good nurse manager. Australian Journal of Nursing 2004; 104(8): 64C.
49. Manion J. Joy at work!: Creating a positive workplace. Journal of Nursing Administration 2003; 33(12): 652-659.
50. Rowe JA. Accountability: a fundamental component of nursing practice. British Journal of Nursing 2000; 9(9): 549-552.
51. Millar C. Maintaining professional and personal accountability. Nursing New Zealand 2002; 8(3): 25.
52. Halstead JA, Rains JW, Boland DL, May FE. Reconceptualizing baccalaureate nursing education: outcomes and competencies for practice in the 21st century. Journal of Nursing Education 1996; 35(9): 413-416.
53. Melling S, Hewitt-Taylor J. New flexible healthcare roles and the purpose of nursing. British Journal of Nursing 2003; 12(21): 1264-1270.
54. Tingle JH. Do guidelines have legal implications? Archives of Disease in Childhood 2002; 86(6): 387-388.
55. Taylor K. A nurse's duty of confidentiaility. The Lamp 2001; February: 17.
56. Goodman B. Ms B and legal competence: examining the role of nurses in difficult ethico-legal decision-making. Nursing in Critical Care 2003; 8(2): 78-83.
57. Blood R. Minimizing health and safety risks in the workplace. Nursing & Residential Care 2005; 7(5): 196.
58. Scopelliti J, Judd F, Grigg M, Hodgins G, Fraser C, Hulbert C et al. Dual relationships in mental health practice: issue for clinicians in rural settings. Australian and New Zealand Journal of Psychiatry 2004; 38: 953-959.
59. Taylor S, Foster M, Fleming J (Eds). Health Care Practice in Australia. Melbourne: Oxford University Press, 2008.
