Introduction
Stroke is characterized by the sudden onset of clinical symptoms indicating a focal or global impairment of cerebral function. These symptoms persist for at least 24 hours or lead to death and have no discernible cause other than being related to blood vessels1. Globally, stroke stands as the primary contributor to disability, significantly reducing patients’ quality of life and placing a substantial burden on healthcare systems2.
Quality of life is crucial for stroke patients because it encompasses their perceptions of life within the cultural and value systems they exist in, along with their aspirations, standards, expectations, and concerns3. Self-efficacy refers to an individual’s confidence in carrying out a specific task or behavior. For stroke patients, high self-efficacy correlates positively with mobility and activities of daily living while also improving overall quality of life4. The examination of the factors that impact quality of life and self-efficacy is a crucial element for chronic diseases such as stroke, given their significance and influence5,6.
Residing in a rural locality is widely acknowledged to be an obstacle to obtaining healthcare services because of the distance, limited transportation, unfavorable weather conditions, a scarcity of health professionals, and inadequate healthcare coverage7. Living in rural areas often means longer travel distances, making it more challenging for individuals to access medical care. Consequently, people in these areas tend to see physicians less often and receive fewer referrals to specialists8. Evidence suggests that individuals from rural areas have lower odds of accessing stroke unit care, brain imaging within 24 hours, carotid imaging, and consultations from neurologists, physiotherapists, occupational therapists, and speech language pathologists. Additionally, they are less likely to be transferred to inpatient rehabilitation facilities9. Therefore, a patient’s place of residence could potentially influence their quality of life and self-efficacy.
Türkiye’s urban–rural profile is characterized by a combination of rural and transitional areas. While well-developed western regions boast deep rural characteristics, there are also scattered ‘prosperity spots’ in less-developed eastern regions10. The country has a significant rural population, with 26% of the total population residing in rural areas11. To the best of our knowledge, there has been no research on the disparities in quality of life and self-efficacy among stroke patients residing in rural and urban areas within Türkiye, despite available information about other countries12,13. In light of this background, this study aims to bridge this gap by examining the impact of residential location on the quality of life and self-efficacy levels of stroke patients in Türkiye.
Methods
Design
In this cross-sectional study, patients with stroke who were admitted to the physical medicine and rehabilitation outpatient clinic of Üsküdar State Hospital between 1 June 2023 and 1 September 2023 were evaluated. Patients aged 18 years and above with a confirmed stroke diagnosis of at least 1 year were eligible for inclusion. Patients experiencing mental or communication difficulties that prevented them from completing the questionnaire were excluded from the study.
Sample
Sample size was determined using the following formula:
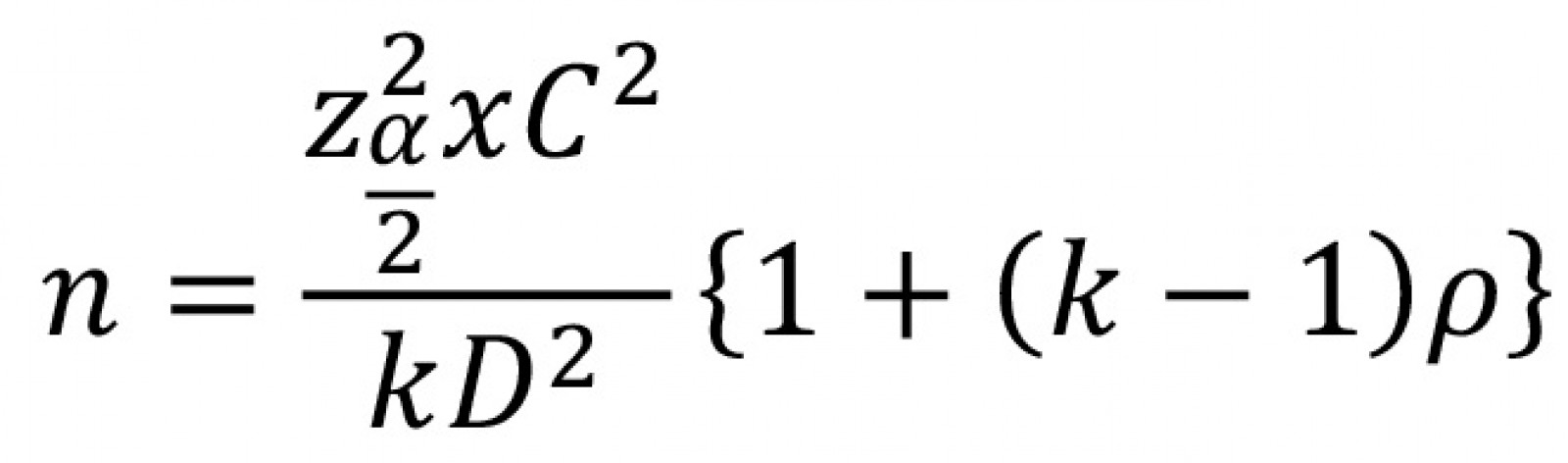
k represents the number of items on the Likert scale, specifically k=5 for the stroke-specific quality-of-life scale (SSQoL).
The pairwise correlation coefficient (ρ) was assumed to be 0.5, and the coefficient of variation (C) for each Likert-item scale was assumed to be 0.5. Additionally, D was set at 0.10, which represented a 10% relative tolerable error, where D=B/µ, B signified the bound of error, and μ was the sample mean. The value corresponded to the 100(1−α/2)th percentile of the standard normal distribution, and for a 95% confidence interval was assumed to be 1.9614. Consequently, the necessary sample size was determined to be 58 for each group. Allowing for a 10% dropout rate, the total number of participants aimed for was set at 64 for each group, totaling 128 patients in the study.
Setting and participants
According to Village Law No. 442 of the Turkish Republic, settlements with a population less than 2000 are classified as villages, those between 2000 and 20,000 are designated as towns, and those exceeding 20,000 inhabitants are termed cities. The areas identified as villages by this law were categorized as rural, while towns and cities were considered urban. Patients were segregated into two groups based on their places of residence7. During the study period, stroke patients admitted to the Üsküdar State Hospital were initially categorized according to their residence in either rural or urban areas. A combined total of 353 individuals from urban regions and 276 individuals from rural areas underwent screening to determine their eligibility. Among them, 92 patients residing in rural areas and 88 patients living in urban locations met the inclusion criteria and were subsequently admitted. As a result, 180 participants ultimately took part in the study.
Outcome measures and data collection
Data encompassing sociodemographic factors such as age, gender, marital status, and education level, along with details about where they lived and worked, and comorbid diseases, and specific questions regarding the individual’s disease (years since stroke, affected artery, affected side, whether the patient had rehabilitation) were gathered through interview. All participants took part in personal assessments using both the SSQoL and the stroke self-efficacy questionnaire (SSEQ). The hospital database was used to ascertain the frequency of visits to the emergency department, physical medicine and rehabilitation outpatient clinic, and general practitioner clinic with primary reason for visit being post-stroke related complaints and complications in the past year. Brunnstrom staging was performed by a physical medicine and rehabilitation specialist with 10 years of experience in staging.
The SSQoL scale is a tool designed to measure the health-related quality of life in individuals who have had a stroke. It consists of 49 items covering the 12 domains of mobility, energy, upper extremity function, work/productivity, mood, self-care, social roles, family roles, vision, language, thinking, and personality. Patients are asked to rate each item using a 5-point Likert scale based on their experiences during the past week. This allows for an up-to-date reflection of the patient’s wellbeing15. Yönt et al carried out the Turkish study to establish the reliability and validity of this scale16.
The SSEQ consists of 13 items and is a self-report scale designed to assess individuals’ confidence in their ability to function effectively after a stroke. Participants indicate their level of belief in achieving each item using a 3-point scale, where 0 represents ‘not at all confident’ and 3 represents ‘very confident’17. Topçu et al carried out the validation and reliability study for this questionnaire in a Turkish context18.
Motor recovery assessment in stroke patients was performed by using the Brunnstrom stages. In stage 1, patients demonstrate flaccidity and an inability to initiate limb movements. Stage 2 involves the emergence of basic limb synergies or their components, along with minimal voluntary movements and the onset of spasticity. During stage 3, there is voluntary control over movement synergies; however, not all components may develop fully, and spasticity becomes severe. At stage 4, non-synergistic movement combinations are mastered, leading to a decrease in spasticity. As patients progress to stage 5, more complex movement combinations are executed as basic limb synergies become less dominant. Finally, at stage 6, spasticity decreases, allowing for individual joint movements. This ordered framework offers a valuable clinical depiction of motor recovery post-stroke by highlighting the evolving interaction between spasticity and voluntary movements19. A physical medicine and rehabilitation specialist with a decade of expertise in the field conducted the Brunnstrom assessment.
Data analysis
Data analysis was conducted using Statistical Package for the Social Sciences v27 (IBBM Corp; https://www.ibm.com/products/spss-statistics). The categorical variables were presented as numbers and percentages, while the numerical variables were represented with mean and standard deviation values. Categorical variables were compared using the χ² test, and numeric variables in independent groups were assessed through the student’s t-test for normally distributed data or Mann–Whitney U-test when normality assumptions were violated. The significance level was 0.05, with a confidence interval of 95%.
Ethics approval
This research was granted ethics approval by the local Clinical Research Ethics Committee on 10 May 2023. The research followed the guidelines outlined in the Declaration of Helsinki and was registered with clinicaltrials.gov for transparency and accountability.
Results
The flowchart of the study is presented in Figure 1. Overall, the distribution of gender, age, and BMI was comparable between the two groups, with no statistically significant differences observed. Notably, rural participants had a slightly higher average BMI, although this was not statistically significant. The general demographic profile suggests a relatively balanced sample in terms of key baseline characteristics across rural and urban settings. Table 1 outlines the demographic and health characteristics of patients from rural and urban areas. There was a tendency for patients in urban areas to have experienced strokes a longer time ago (average 3.9 years) than those in rural areas (average 2.72 years), but this contrast did not show statistical significance (p=0.107). Urban patients had significantly fewer visits to an emergency department in the past year than rural patients (p<0.001); similarly, urban patients made fewer trips to physical medicine and rehabilitation clinics and family practitioner clinics over the last year than rural patients (p<0.001 and p<0.001, respectively).
Rural patients demonstrated lower SSEQ scores (20.31±9.38) in comparison to urban patients (23.17±8.71) (p=0.036). Furthermore, rural patients reported lower SSQoL scores (119.79±35.66) than urban patients (138.91±31.72) (p<0.001).
The analysis revealed a statistically significant difference in the utilization of physical medicine and rehabilitation services between patients residing in urban areas and those living in rural areas (p=0.027) (Fig2).
Analyses did not show any notable difference in the affected side, type of stroke, and affected artery (p=0.126, p=0.780 and p=0,527, respectively) (Figs3,4).
Statistical analysis revealed that there was no significant statistical difference in Brunnstrom stages among stroke patients residing in rural and urban areas (Table 2).
Table 1: Comparison of demographic and health characteristics between patients in rural and urban areas
| Variable | Characteristic |
Patients living in rural areas (mean±SD) |
Patients living in urban areas (mean±SD) |
p-value |
|---|---|---|---|---|
| Gender | Male | 50 | 44 | 0.654 |
| Female |
42 |
44 | ||
| Age (years) | 65.19±9.6 | 63.95±10.55 | 0.291 | |
| BMI | 28.53±5.19 | 28.17±5.19 | 0.459 | |
| Years since stroke | 2.72±3.66 | 3.9±5.89 | 0.107 | |
| Emergency department visits in last year | 4.15±3.93 | 2.15±1 | <0.001* | |
| PM&R polyclinic visits in last year | 5.10±2.41 | 1.7±0.91 | <0.001* | |
| Family practitioner visits in last year | 8.65±5.41 | 2.59±1.9 | <0.001* | |
| Stroke self-efficacy score | 20.31±9.38 | 23.17±8.71 | 0.036* | |
| Stroke-specific quality-of-life scale | 119.79±35.66 | 138.91±31.72 | <0.001* |
* Independent samples t-test.
BMI, body mass index. PM&R, physical medicine and rehabilitation. SD, standard deviation.
Table 2: Brunnstrom stages of patients living in urban and rural areas
| Variable | Characteristic | Brunnstrom stage | p-value | |||||
|---|---|---|---|---|---|---|---|---|
|
1 |
2 |
3 | 4 | 5 | 6 | |||
| Patients living in rural areas (%) | Hand | 10.9 | 16.3 | 19.6 | 25 | 28.3 | 0 | 0.823 |
| Patients living in urban areas (%) |
13.6 |
20.5 | 18.2 | 13.6 | 18.2 | 15.9 | ||
| Patients living in rural areas (%) | Upper extremity | 4.3 | 10.9 | 29.3 | 29.3 | 23.9 | 2.2 | 0.977 |
| Patients living in urban areas (%) |
9.1 |
29.5 | 13.6 | 9.1 | 6.8 | 31.8 | ||
| Patients living in rural areas (%) | Lower extremity | 6.5 | 10.9 | 32.6 | 20.7 | 29.3 | 0 | 0.849 |
| Patients living in urban areas (%) |
6.8 |
13.6 | 29.5 | 22.7 | 13.6 | 13.6 | ||
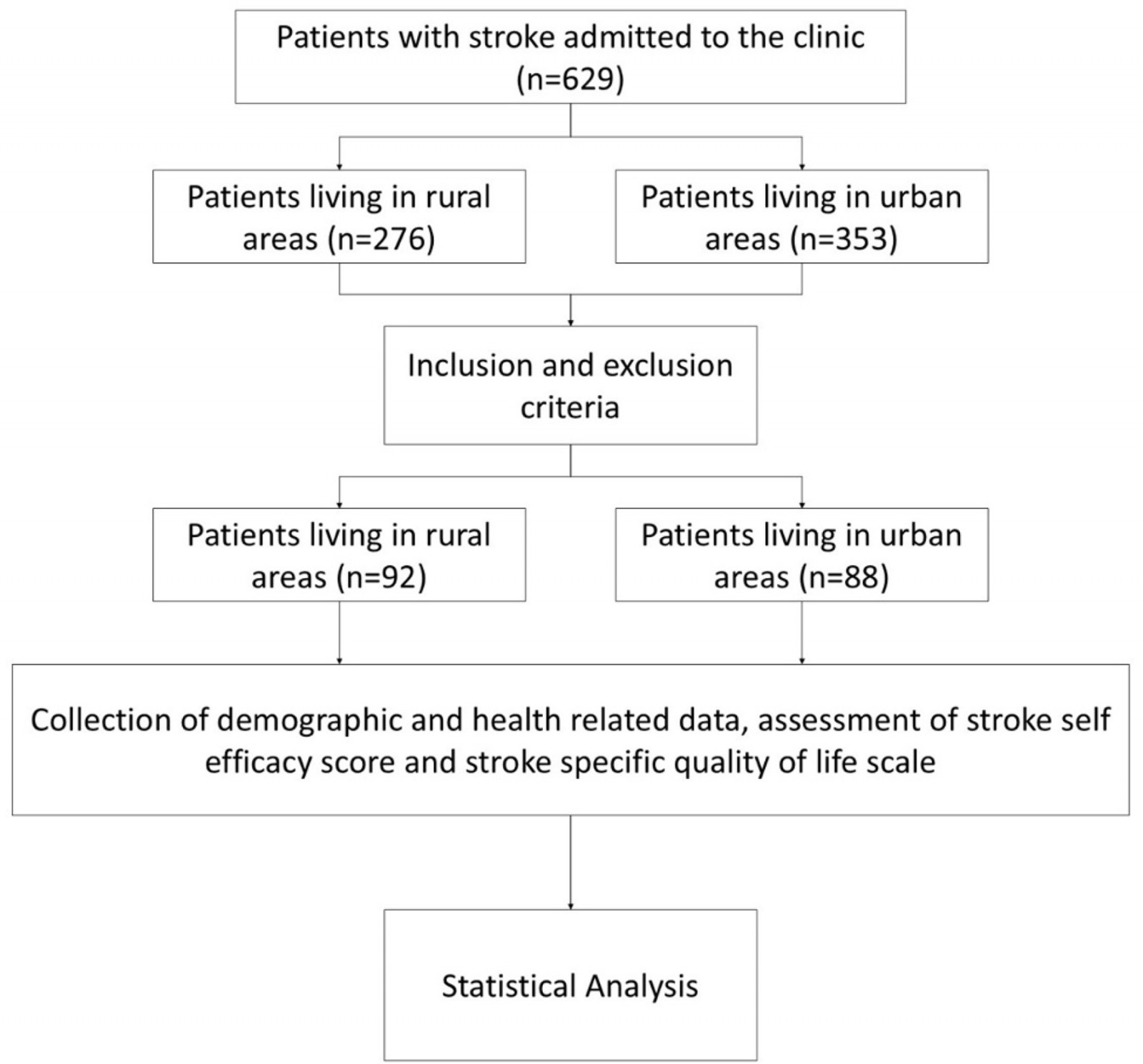 Figure 1: Flowchart of the study.
Figure 1: Flowchart of the study.
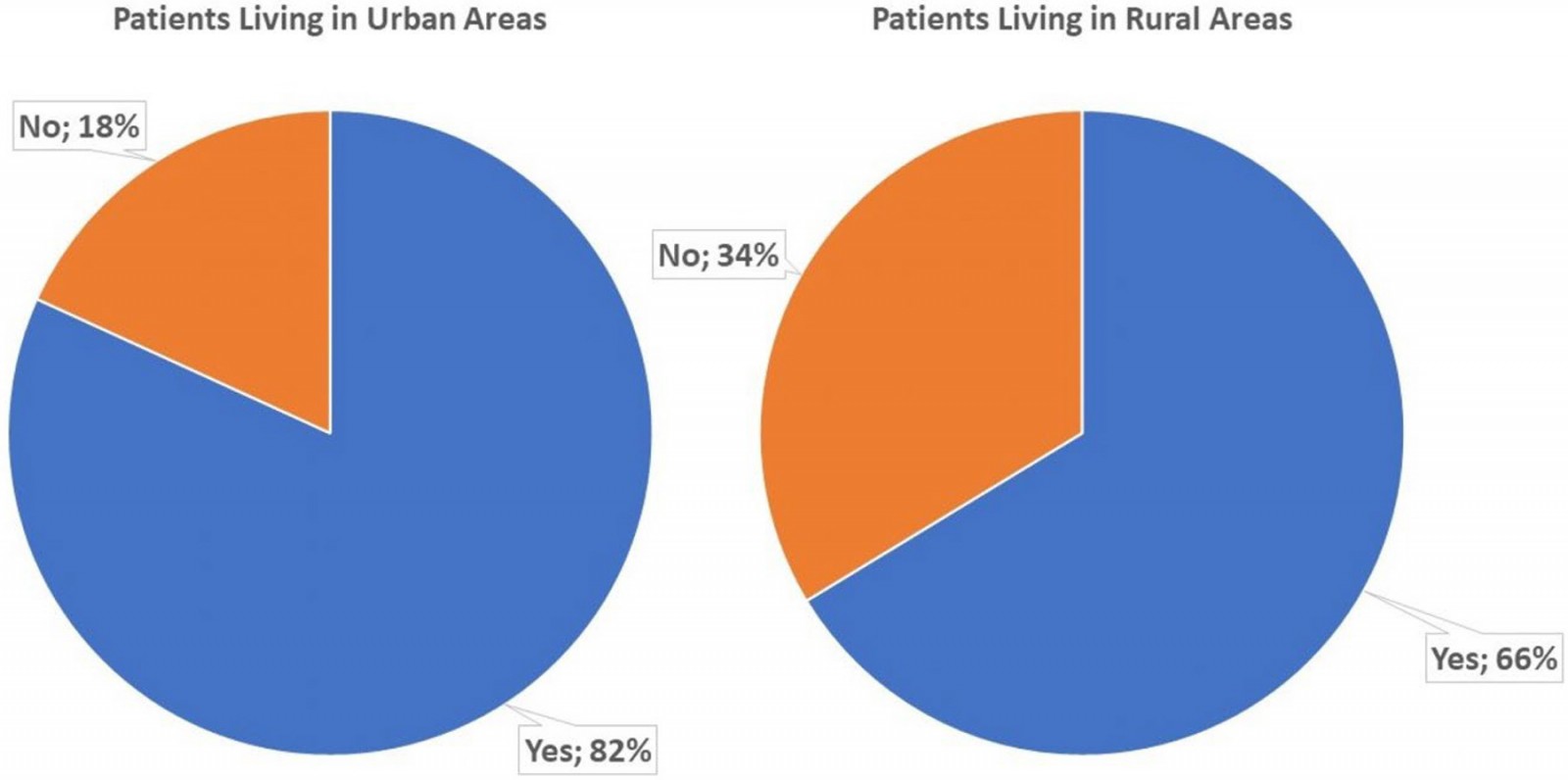 Figure 2: Whether a patient had prior rehabilitation compared to patient’s region of residence.
Figure 2: Whether a patient had prior rehabilitation compared to patient’s region of residence.
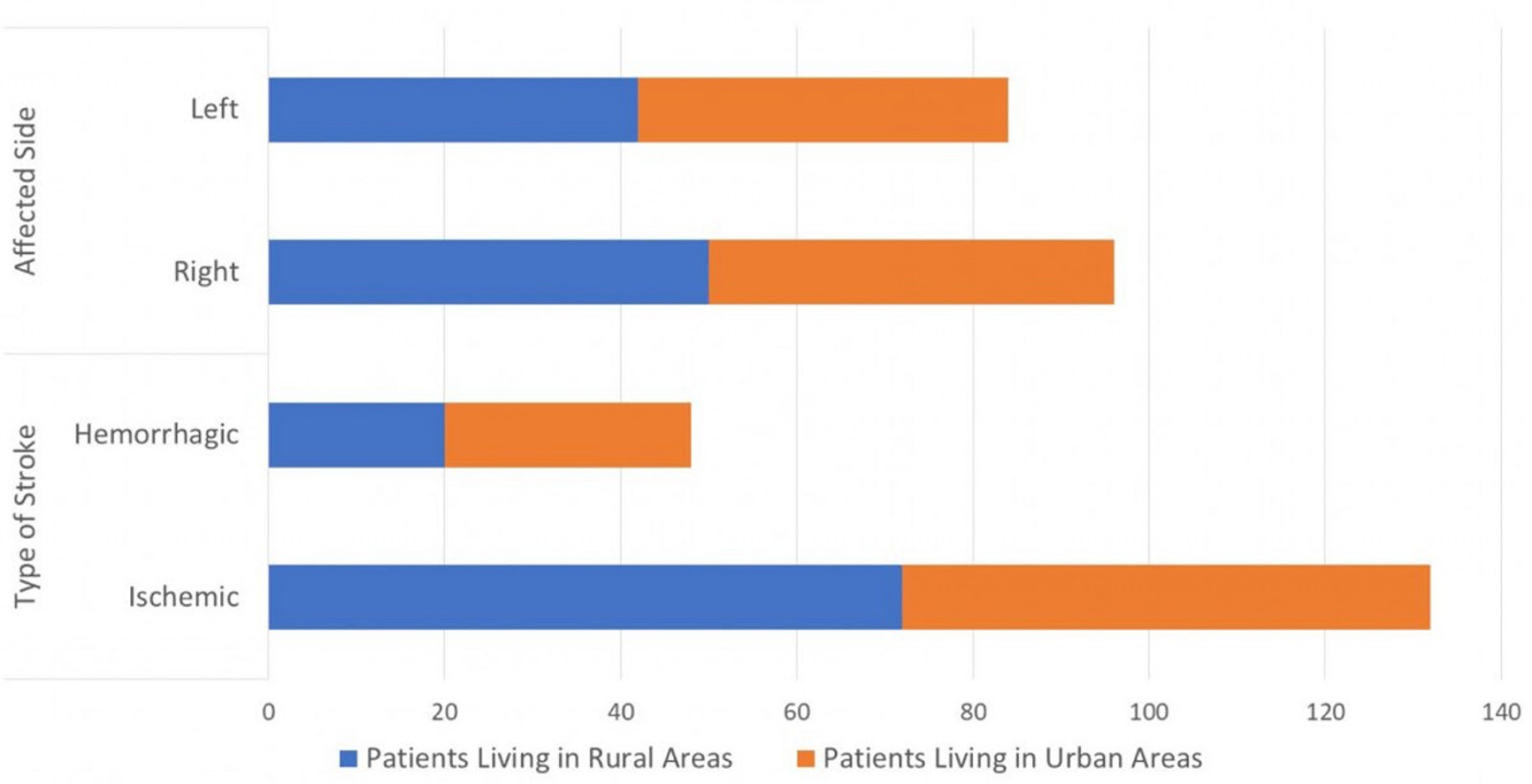 Figure 3: Affected side and type of stroke of patients living in rural and urban areas.
Figure 3: Affected side and type of stroke of patients living in rural and urban areas.
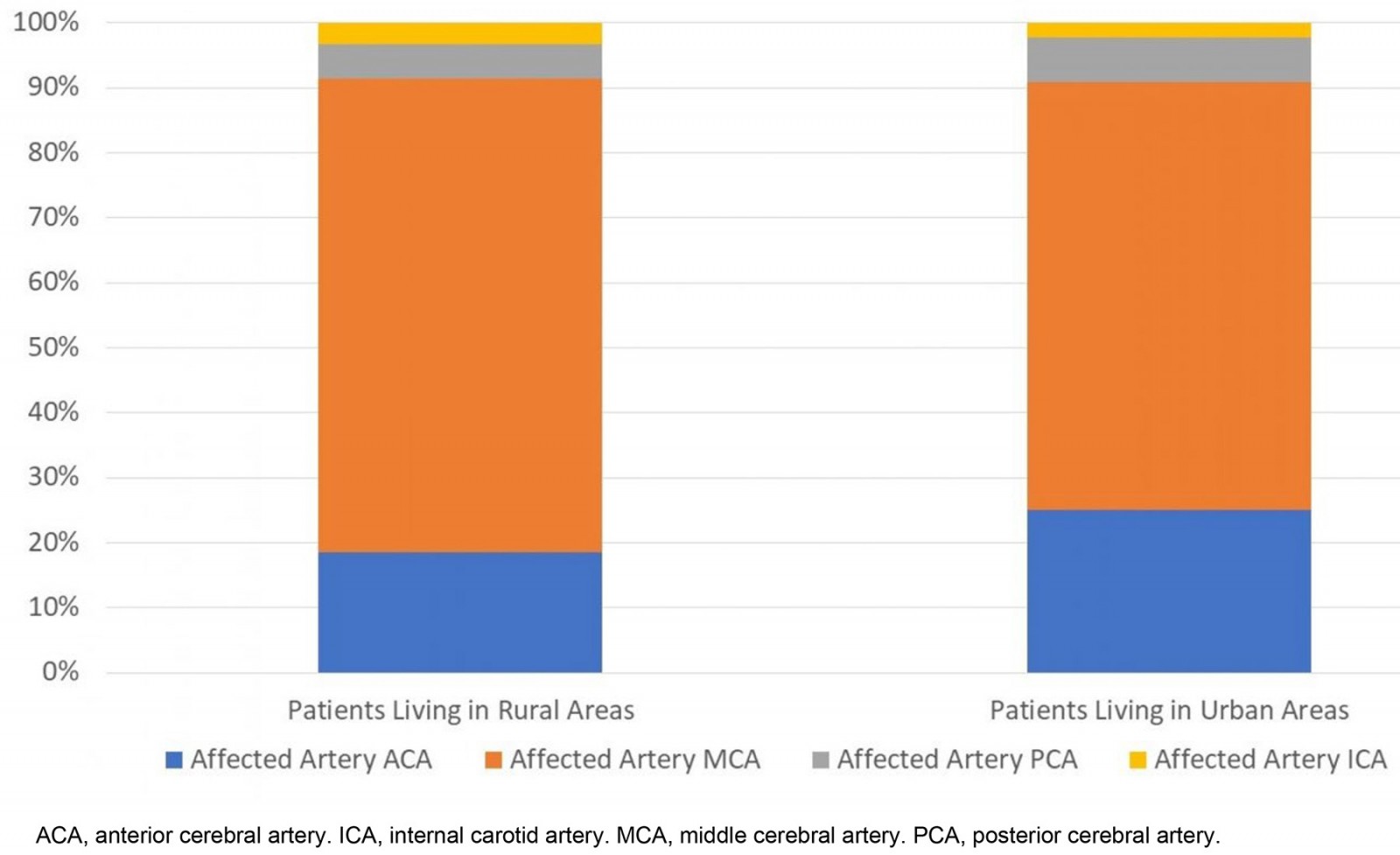 Figure 4: Comparison of the affected arteries between patients living in rural and urban areas.
Figure 4: Comparison of the affected arteries between patients living in rural and urban areas.
Discussion
As a result of this study, it was observed that stroke patients residing in rural areas exhibited significantly lower stroke-specific quality of life and self-efficacy than those living in urban areas, despite no significant difference being observed in Brunnstrom stages. Furthermore, it was noted that individuals from rural communities had significantly lower attendance at rehabilitation and were more inclined to seek medical advice from family physicians, physical medicine and rehabilitation specialists, and emergency clinics. This research represents the initial comparative study of stroke patient recovery outcomes, quality of life, self-efficacy, and healthcare utilization between rural and urban regions in Türkiye.
The study found that stroke patients in rural areas tended to seek medical assistance from family physicians, emergency physicians, and physical medicine and rehabilitation clinics more often than those in urban areas. Contrary to our findings, Jeyakumar et al’s research on ambulatory care for secondary prevention of stroke in rural versus urban areas in Ontario, Canada, indicated that individuals from rural areas who had previously suffered a stroke had fewer visits to physicians, received less screening for hyperlipidemia, and faced a slightly higher risk of experiencing another stroke20. Koifman et al determined in their research on the outcomes of stroke among rural residents that there is a lower likelihood of these individuals receiving critical interventions for stroke care following an episode9. The findings of our research could be connected to the challenges faced by rural hospitals, including limited staffing and infrastructure, resulting in suboptimal treatments and thus increased hospital visits. When this suboptimal treatment is combined with reduced quality of life and lower self-efficacy, rural stroke patients may tend to seek more advice and follow-up from a healthcare professional, regardless of subspeciality21.
Our research revealed that patients in rural areas tend to receive less rehabilitation than their urban counterparts, which aligns with previous studies. For instance, Merchant et al found that Australian rural stroke patients had lower access to rehabilitation than those living in metropolitan areas22. Similarly, Yan et al’s study on stroke patients in Chinese rural regions highlighted the insufficient availability of secondary prevention and rehabilitation services, often falling below evidence-based standards23. Additionally, Quigley et al reported that rural and remote stroke survivors face limited opportunities to achieve their full rehabilitation potential after being discharged from hospitals24. Personnel deficits, uneven distribution of healthcare staff, and challenges in recruiting and retaining personnel may be responsible for this gap in rural areas. To bridge this divide, telerehabilitation methods could be explored to overcome the challenges of providing rehabilitation in rural areas. It is also essential to advocate for policy reforms, enhanced funding, and revised reimbursement policies to drive positive changes.
Self-efficacy is a crucial factor for the wellbeing of stroke patients and plays a significant role in accurately assessing their functional abilities. It has been observed that individuals with high self-efficacy tend to perform better in their daily activities than those with low self-efficacy25. Our study revealed lower self-efficacy scores among stroke patients residing in rural areas, aligning with Ferri et al’s findings that reported greater dependency on others among stroke patients living in rural regions within Latin America, China, and India during their investigation into the burden of stroke26. This difference in self-efficacy levels in rural areas might be influenced by limited knowledge and education about the illness, insufficient self-care skills, and substandard disease control27. To enhance the self-efficacy of patients in rural areas, it may be advantageous to prioritize providing access to rehabilitation services, establishing realistic goals, delivering educational information, and promoting transparent communication within healthcare settings.
Quality of life is vital for stroke patients because it allows for the evaluation of their overall wellbeing and their responsiveness to changes in clinical status over time28. Studies conducted on the quality of life of stroke patients living in rural areas have indicated that they experience lower levels of quality of life. For example, Howitt et al reported that stroke patients in rural Tanzania had lower quality of life than controls29. Similarly, Mei et al found that stroke patients in rural China also experienced poor quality of life30. Jun et al’s investigation into a Korean community yielded similar findings to our research, showing that residents in rural areas reported a lower quality of life than those living in urban areas31. This difference may stem from restrictions in medical care and resources for people living in rural regions, higher occurrence of anxiety and depression among stroke patients residing in rural areas, as well as decreased social connections30,32. Enhancing the quality of life of stroke patients in rural areas may entail introducing telehealth services for distant appointments, local rehabilitation and assistance initiatives, caregiver support and education, as well as establishing community centers and support groups within the area.
As a result of the research, it was discovered that while patients residing in rural areas had notably lower quality of life and self-efficacy than those in urban areas, there were no significant differences observed in Brunnstrom stages. This could be attributed to insufficient access to treatment of stroke-related complications, decreased likelihood of receiving essential psychological and social support as opposed to urban settings, and potential challenges with treatment adherence among patients living in rural areas33-35. In addressing the acknowledged disparities, it may be advantageous to ensure accessibility of stroke treatments and rehabilitation services. Additionally, introducing community-based initiatives that enhance awareness, offer education, and establish tailored social support systems for the specific needs of rural stroke survivors could enhance their overall quality of life and dedication to treatment plans.
Strengths and limitations
This study has several limitations that should be considered when interpreting the results. First, as the research was conducted exclusively among stroke patients in Türkiye, the findings may not be generalizable to populations in other countries with different healthcare systems, socioeconomic conditions, and cultural contexts. Second, the study does not explore specific socioeconomic determinants such as income, education, or social support, which are likely to influence healthcare-seeking behavior and health outcomes, particularly in rural areas. The cross-sectional design limits the ability to assess changes over time, and future longitudinal studies would provide deeper insights into evolving factors affecting stroke recovery. Additionally, there is a potential selection bias due to the underrepresentation of patients with severe impairments or those who did not seek medical care, which may have influenced the observed levels of self-efficacy and quality of life. A further methodological limitation relates to the sample size calculation, which was based on a 5-point Likert scale item rather than a clinically meaningful difference in standardized stroke scale scores, potentially affecting statistical power. Finally, while the study references several relevant works, some are outdated, highlighting the persistent gap in up-to-date, high-quality research on rural–urban disparities in stroke care and outcomes.
Conclusion
This research emphasized the challenges faced by individuals living in rural areas, who experienced lower quality of life and self-efficacy in managing their stroke than those residing in urban areas. It was also found that rural stroke patients tended to seek medical assistance more frequently from family physicians, emergency clinics, and rehabilitation services. Addressing the limited availability of rehabilitation services, medical infrastructure, resources, and healthcare professionals for rural patients through policy reforms and innovative approaches such as telerehabilitation could potentially enhance the wellbeing and outcomes for stroke patients in these regions. Subsequent studies should explore specific socioeconomic factors using longitudinal methods to gain a comprehensive understanding of the influences on stroke recovery across diverse geographical locations.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflicts of interest
The authors declare no conflict of interest in the writing and/or publication of this article.


