Introduction
Acute coronary syndrome (ACS) includes a range of cardiac conditions including acute myocardial infarction (AMI) and angina1. Acute coronary syndrome is a major cause of morbidity and mortality and represents one of the most common causes of acute medical admissions in Australia2. Current Australian clinical guidelines1 recommend all patients with ACS should receive secondary prevention services that aim to maximise physical, psychological and social functioning, and enable people with ACS to lead fulfilling and productive lives2.
A comprehensive approach to secondary prevention should include a combination of pharmacological interventions (eg antiplatelet agents, beta-blockers, angiotensin-converting enzyme inhibitors, lipid lowing medications and nitrates) and lifestyle and behavioural interventions. This approach has been shown to significantly reduce the risk of future cardiac events and deaths2-4, and leads to fewer re-admissions to hospital, a shorter associated length of stay5-9, and enhanced medication management10. The National Heart Foundation Australia advocates a multidisciplinary approach to secondary prevention that includes nurses, doctors, physical therapists, dieticians, social workers and pharmacists working together to deliver therapeutic interventions and health behaviour advice for smoking cessation, physical inactivity, obesity, poor nutrition, high risk alcohol consumption, hypertension and dyslipidaemia2. In this case secondary prevention specifically aims to impact on cardiac risk factors and this differs from a primary prevention approach, which employs population health activities aimed at health promotion and disease prevention whereby it is more difficult to directly attribute impacts of primary healthcare activities and initiatives3.
Optimal patient outcomes rely on the timely and effective implementation of proven therapies11. Clinical guidelines for the management of ACS are readily available and are based on rigorous evidence11. However, the ability to implement these guidelines is dependent on the resources available in a particular region1,12. Rural and remote populations have a significantly higher incidence of cardiac mortality and morbidity than those in metropolitan areas2,13, yet they have poorer access to structured secondary prevention programs14,15 and are prescribed cardiovascular medications at half the rate of people living in major cities13.
The Riverland region of South Australia is a 3 hour drive north east of state capital Adelaide with a population of just under 35 000 people16. Cardiac related health services, including ad hoc secondary prevention, are provided by five hospitals and seven GP clinics in the region. In addition, patients have access to five visiting cardiologists who consult at the Riverland Regional Hospital's Berri Campus and the Loxton District Hospital (three consult monthly and two consult bi-monthly). Patients are also required to travel to Adelaide for additional services, including admission to a metropolitan hospital for percutaneous coronary interventions and cardiac surgeries, and for cardiologist review if they are referred to specialist who does not consult in the Riverland17.
With a Socio Economic Index for Areas rating (SEIFA) of 961, the Riverland Region is placed 0-5% below the non-metro average in terms of socio-economic disadvantage18. An Accessibility/Remoteness Index of Australia (ARIA) rating of 3.6301-4.5262 classifies the Riverland as 'moderately accessible', or significantly restricted with regards to accessibility of goods, services and opportunities for social interaction16,18,19. This is significant due to the strong link between lower socioeconomic status and increased rates of cardiovascular disease (CVD) mortality18. The rate of CVD in the Riverland is well above the state average and is the primary killer in the region, accounting for nearly one-fifth of the total mortality burden16. Despite this high risk profile, there is currently no structured approach in the Riverland to secondary prevention, including cardiac rehabilitation, for patients with ACS.
Much attention has been given in the literature to evaluating the scope, efficacy and adherence rates of structured secondary prevention services throughout Australia. However, we could find no evidence of studies reporting the scope and efficacy of unstructured secondary prevention services in rural Australia. Hence, the aim of this study was to examine initial assessment and ongoing secondary prevention of CVD risk factors for patients who have suffered AMI in a rural region of South Australia that does not offer structured secondary prevention services.
Methods
Study design and data collection tool
A retrospective medical records analysis was undertaken to examine assessment of CVD risk factors and documented evidence of secondary prevention interventions within a 12 month time period. Medical record review has been used previously in Australia20,21, and internationally by the EUROASPIRE II study22 and GRACE study23 to collect demographic and CVD risk factor data, and pharmacological interventions for CVD. The data abstraction tool, initially developed to evaluate an outpatient, hospital-based cardiac rehabilitation program in the USA24, was adapted for the current study to encompass current 'Australian Clinical Guidelines for the Management of Acute Coronary Syndromes'1,4. Data were pooled prior to analysis to preserve health service and patient anonymity.
Study participants and ethics approval
All patients admitted to hospital in the Riverland region between 1 July 2004 and 30 June 2005 with a primary diagnosis of AMI were eligible for inclusion in the study. Approval for the study was granted by the University of South Australia Human Research Ethics Committee.
The current study was undertaken in two separate phases.
Phase 1: The aim of phase 1 was to examine baseline assessment of CVD risk factors and implementation of current clinical guidelines for secondary prevention of ACS in the hospital setting. Permission to access medical records of eligible patients (n = 77) was sought from all five Riverland hospitals (Fig1). Three hospitals agreed (n = 48), and the internal ethics committees of the remaining two hospitals consented, providing the hospitals contacted eligible patients and obtained individual consent. The hospitals sent a written invitation to participate in the study to 29 patients, 7 of whom responded and consented (24% response rate). The medical records of 55 of a possible 77 (71%) patients were accessed in the hospital setting.
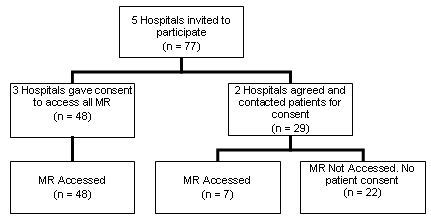
Figure 1: Phase One - hospital response rates and number of medical records accessed in the hospital setting. MR, Medical records.
Phase 2: The aim of phase 2 was to examine follow-up care and the implementation of current clinical guidelines for secondary prevention of ACS in the GP clinic setting for the 55 patients in phase 1. All seven GP clinics in the region were approached for permission to access the medical records of those same 55 patients. Five GP clinics granted access to relevant medical records, one of which required the researcher to gain written consent from each patient. Two GP clinics did not allow access to medical records. A total of 34 of a possible 55 medical records were accessed in the GP clinic setting (Fig2). Of the 21 records not accessed; five patients attended GP clinics that declined participation in the study, two patients were not Riverland residents, five patients died prior to follow up, and nine patients did not provide written consent.
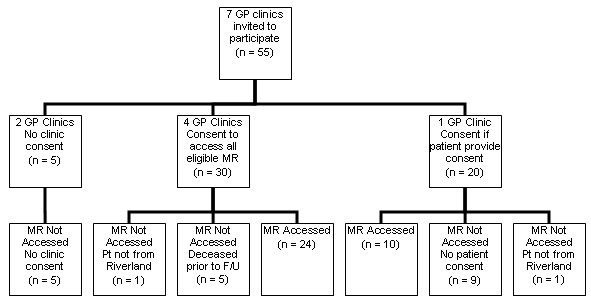
Figure 2: Phase 2 - GP clinic response rates and number of medical records accessed in GP clinic setting. F/U, Follow up; MR, medical records; Pt, patient.
Data collection
Categories in the data collection tool were: demographics, prescribed medications, previous AMI, biomedical risk factors (diabetes, hypertension, dyslipidaemia), and lifestyle and behavioural risk factors (obesity or overweight, physical activity, independence with activities of daily living, dietary habits, alcohol consumption, smoking status, living arrangements and social support).
Entries in the medical records were examined from the initial date of admission through to 12 months post-admission. Demographic and baseline CVD risk assessment data were collected in the hospital setting. Documented evidence of secondary prevention interventions, measurement of biomedical CVD risk factors, and deaths were collected in both the hospital and GP clinic setting,
Statistical analysis
Data were entered by hand on to the data abstraction tool and then entered into Microsoft Excel spreadsheets for analysis. Descriptive statistical analysis was used to calculate frequencies, mean values and range. Pharmacological and medical interventions in the current study refers to the assessment and measurement of biomedical risk factors, smoking and overweight/ obesity, referral to relevant health services, prescribing of recommended medications and the provision of a written action plan for chest pain.
Results
Demographic characteristics
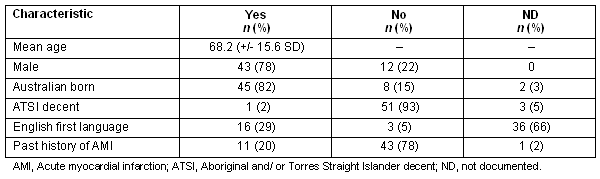
The mean age was 68.2 years (+/-15.5 SD), and 43 patients (78%) were male. Forty-five patients (82%) were born in Australia, and one patient (2%) was of Aboriginal or Torres Straight Islander decent. Demographic data is presented (Table 1).
Table 1: Demographic characteristics of patients (n = 55) assessed in the hospital setting
Baseline assessment of biomedical risk factors, smoking and obesity in the hospital setting
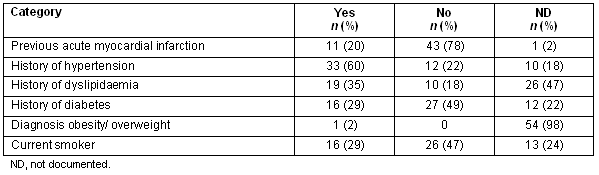
The majority of patients were assessed for previous AMI and history of biomedical risk factors in the hospital setting, as depicted (Table 2). The most poorly documented risk factor was obesity/overweight, with only one patient (2%) diagnosed as obese (GP entry on admission form). While 22 patients (40%) were weighed during hospital admission, there was no evidence of body mass index (BMI) assessment or waist circumference measurement for any patient in the study. Also poorly documented was a history of dyslipidaemia with only 29 patients (53%) assessed in this category.
Table 2: Baseline assessment of biomedical and behavioural risk factors in the hospital setting (n = 55)
Pharmacological and medical interventions
The proportion of patients referred to additional health services by hospitals and GP clinics was 89% and 62%, respectively. The most common referral in the hospital setting was to a metropolitan hospital (67%), and the most common referral in the GP clinic setting was for review by a cardiologist (62%). Six patients (11%) in the hospital setting and 10 patients (29%) in the GP clinic setting were not referred to any additional health services.
There was no evidence of interventions for smoking or obesity/ overweight in the hospital setting. In the GP clinic setting, five of 11 smokers (45%) received 'quit' advice and one smoker was prescribed nicotine replacement therapy. Sixteen of 34 patients (47%) followed up in the GP clinic setting had BMI assessed and 11 patients were diagnosed as overweight/ obese. Two of these 11 patients (18%) received weight loss advice.
The majority of patients had their medication regimen altered in both the Riverland hospital setting (96%) and GP clinic setting (97%). During the 12 month study period, a high percentage of patients were prescribed medications recommended for all patients with ACS1,4 pS23. However, prescribing rates were as low as 42% for some recommended medications at the time of discharge from hospital (Table 3).
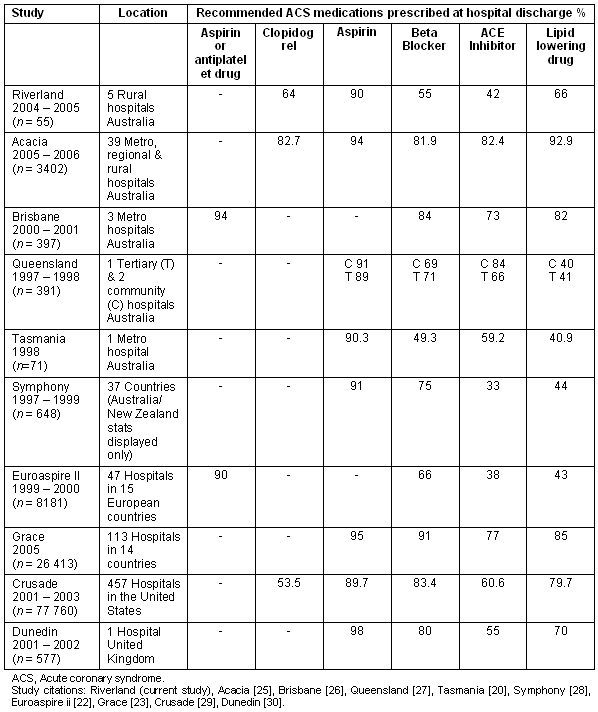
Prescribing rates at the time of hospital discharge in the current (Riverland) study were compared with 9 Australian and international studies (Table 4). Riverland prescribing rates for aspirin were similar to other studies. However, Riverland prescribing rate for beta blockers and ACE inhibitors were lower than most of the comparison studies. Prescribing rates for lipid lowering drugs varied widely between the comparison studies, with the Riverland having the sixth lowest rate.
Table 3: Recommended medications prescribed in the hospital setting (n = 55) and GP clinic setting (n = 34) during the 12 month study period
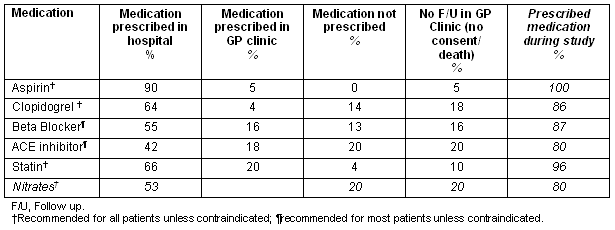
Table 4: Prescribing rates of recommended medications post acute coronary syndrome at the time of hospital discharge in the current (Riverland) study compared with 9 Australian and international studies20,22,23,25-30
Discussion
Results of the current study indicate prescribing rates for ACS at the time of hospital discharge are suboptimal. However, overall prescribing rates in the 12 month period post-ACS are 80% or higher, suggesting a good level of guideline knowledge relating to pharmacological interventions31. It is interesting to note the wide variation in hospital and GP clinic prescribing rates, despite the same GP usually overseeing patient care in both settings. Further investigation to determine the reason for this variation is warranted. Any intervention to increase the percentage of patients being prescribed recommended medications prior to discharge is likely to favorably affect patient outcomes32. For example, 96% of patients were prescribed lipid lowering medication during the 12 month study period; however, only 66% were discharged from hospital on lipid medication. Increasing this prescribing rate could enhance patient outcomes, as intensive statin therapy initiated immediately after ACS has been shown to reduce recurrent cardiovascular events and mortality33, and to improve the likelihood of patient adherence34.
Increasing the use of recommended drug therapies, however, will not in itself raise the standard of secondary prevention of CVD1,22. For secondary prevention to be successful, pharmacological interventions must be combined with the assessment of biomedical, and lifestyle and behavioural assessment and interventions to address identified risk factors1,22. For example, blood lipid analysis is recommended for all patients with ACS34. In the current study only 29% of patients were tested in the hospital setting. This finding is lower than previously reported testing levels internationally of 39%35, 48%36 and 52.5%37. It is interesting to note that a considerably higher number of patients who were transferred to a tertiary hospital underwent lipid analysis when compared with patients discharged home (42% vs 20%). This difference may be explained by the lower mean age of patients transferred to tertiary care (62 vs 80.5 years), as advanced age has been associated with lower rates of lipid testing37. A significantly higher proportion of patients underwent lipid testing in the GP clinic setting (76%), again despite the same GP usually overseeing patient care from hospital to GP clinic.
Several other recommendations were poorly met, including tight glycaemic control in patients with diabetes, screening all patients for type 2 diabetes, and assessment and interventions for smoking and obesity/overweight. In addition, no patients were provided with the recommended written action plan for chest pain1 which includes explanations about rest, administration of recommended medications and calling for assistance. These care deficits may indicate the level of knowledge of clinical guidelines31, or a lower importance placed on these interventions in comparison with other treatments38. Often, when patients with chronic illness are admitted to an acute care setting, medical attention is focused on treating the acute problem rather than discharge planning and long-term care37,39. Time constraints and inadequate staffing levels have also been cited as reasons for suboptimal assessment and intervention for biomedical risk factors38. A combination of some or all of these factors may have led to the deficits identified in the current study. We would also argue that the absence of a structured approach to CR in the region contributed to these results.
Study limitations
The retrospective nature of this study relies on the accuracy and completeness of original documentation. Documentation of risk factor assessment and measurement in the current study was incomplete, and the possibility that interventions were offered but not documented must be considered when interpreting the findings. The use of non-probability sampling and the small sample size limits generalisability to the wider population. However, the findings have potential relevance to other rural areas with similar populations. It is important to note that this study did not examine the appropriateness of medication class, dosage or adherence rates and, therefore, no determination can be made regarding this. It also important to note that pharmacological interventions were assessed for a period of 12 months post AMI, and no determination can be made regarding long-term prescribing rates.
Conclusions
Unstructured secondary prevention interventions are currently provided to many rural and remote communities in the absence of a structured program. However the unstructured nature of these services means there is variability in the implementation of services and evaluation of outcomes. Consequently the efficacy of unstructured CR and subsequent patient outcomes is also variable. The results of this study provide a valuable insight into the level of unstructured secondary prevention provided by rural health services in the absence of a formal program. Our findings demonstrate that unstructured secondary prevention services can provide some of the recommended elements. Nevertheless, we identified several deficits in care that have the potential to negatively impact patient outcomes in this already disadvantaged population. Future research needs to focus on the extent to which rural and remote health care services are working within current clinical guidelines for the management of ACS, the appropriateness of prescribed medications, long-term prescribing rates, and subsequent patient outcomes.
There is strong evidence to support the efficacy of secondary prevention programs in relation to CVD related morbidity and mortality. In addition, secondary prevention is likely to be most beneficial in rural and remote settings where usual care may be less than optimal14,40. Urgent consideration must, therefore, be given to the introduction and evaluation of a more structured and systematic approach in this and other rural and remote regions of Australia. The development of rehabilitation and prevention services that build on existing strengths and resources have the potential to widen access, enhance current services and ensure care is based on best practice guidelines. This, in turn, may reduce the burden of CVD and improve the overall health and quality of life for patients in rural and remote Australia.
References
1. Aroney C, Aylward P, Kelly A, Chew D, Clune E. Guidelines for the management of acute coronary syndromes 2006: on behalf of the Acute Coronary Syndrome Guidelines Working Group. Medical Journal of Australia 2006; 184(8): S1-S30.
2. Access Economics Pty Ltd. The shifting burden of cardiovascular disease: a report prepared for the National heart Foundation of Australia. Access Economics, 2005. Available: http://www.heartfoundation.org.au/document/NHF/cvd_shifting_burden_0505.pdf (Accessed 1 October 2008).
3. National Health Priority Action Council. National service improvement framework for heart, stroke and vascular disease. In: Ageing. Canberra, ACT: Australian Government Department of Health and Ageing, 2006.
4. National Heart Foundation and Australian Cardiac Rehabilitation Association. Recommended framework for cardiac rehabilitation 04. National Heart Foundation Australia, 2004. Available: http://www.heartfoundation.org.au/document/NHF/cr_04_rec_final.pdf (Accessed 1 October 2008).
5. Murchie P, Campbell N, Ritchie L, Simpson J, Thain J. Secondary prevention clinics for coronary heart disease: four year follow up of a randomised controlled trial in primary care. BMJ 2003; 326: 84-89.
6. Pearson S, Inglis S, McLennan S, Brenman L, Russell M, Wilkinson D et al. Prolonged effects of a home-based intervention in patients with chronic illness. Archives of Internal Medicine 2006; 166: 645-650.
7. Stewart S, Marley J, Horowitz J. Effects of a multidisciplinary, home-based intervention on unplanned readmissions and survival among patients with chronic congestive heart failure: a randomized controlled study. The Lancet 1999; 354(9184): 1077-1083.
8. Sundararajan V, Bunker S, Begg S, Marshall H, McBurney H. Attendance rates and outcomes of cardiac rehabilitation in Victoria, 1998. Medical Journal of Australia 2004; 180: 268-271.
9. Warrington D, Cholowski K, Peters D. Effectiveness of home-based cardiac rehabilitation for special needs patients. Journal of Advanced Nursing 2003; 41(2): 121-129.
10. Campbell N, Ritchie L, Thain J, Deans H, Rawles J, Squair J. Secondary prevention in coronary heart disease: a randomised trial of nurse led clinics in primary care. Heart 2006; 80: 447-452.
11. Chew D, Allan R, Aroney C, Sheerin N. National data elements for the clinical management of acute coronary syndromes. Medical Journal of Australia 2005; 182(9): S1-S15.
12. Huynh L, Phillips P, Chew D. Improving the management of acute coronary syndromes in Australia: translating evidence to outcomes. Internal Medicine Journal 2007; 27: 412-415.
13. Australian Institute of Health and Welfare. Rural, regional and remote health: mortality trends 1992 - 2003. Canberra, ACT: Australian Institute of Health and Ageing, 2006.
14. Clark A, Hartling L, Vandermeer B, McAllister A. Meta-analysis: secondary prevention programs for patients with coronary artery disease. American College of Physicians, Annals of Internal Medicine 2005; 143: 659-672.
15. Dollard J, Smith J, Thompson D, Stewart S. Broadening the reach of cardiac rehabilitation to rural and remote Australia. European Journal of Cardiovascular Nursing 2004; 3(1): 27-42.
16. Public Health Information Development Unit. Population health profile of the Riverland Division of General Practice: supplement, Population Profile Series: no 94a. Adelaide, SA: Public Health Information Unit, The University of Adelaide, 2007.
17. Government of South Australia Department of Health. Riverland Health. (Online) 2005. Available: http://www.riverland.health.com.au (Accessed 4 February 2008).
18. Australian Institute of Health and Welfare. Socioeconomic inequalities in cardiovascular disease in Australia: current picture and trends since 1992. Bulletin 37. Sydney, NSW: AIHW, 2006.
19. Department of Health and Aged Care. Measuring remoteness: accessibility/ remoteness index of Australia (ARIA); revised edition. Occasional papers: new series. 2001; Number 14. (Online) 2001. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/health-historicpubs-hfsocc-ocpanew14a.htm (Accessed 4 February 2008).
20. McNamara K, Peterson G, Frieson W. Changes in the management of acute myocardial infarction in Southern Tasmania. Journal of Clinical Pharmacy and Therapeutics 2000; 25: 111-118.
21. Scott I, Denaro C, Bennett C, Hickey A, Mudge A, Flores J et al. Achieving better in-hospital and after-hospital care of patients with acute cardiac disease. Medical Journal of Australia 2004; 180(Suppl): S83-S88.
22. Euroaspire II Study Group. Lifestyle and risk factor management and use of drug therapies in coronary patients from 15 countries. European Heart Journal 2001; 22: 554-572.
23. Goldgerg R, Spencer F, Steg P, Flather M, Montalescot G, Gurfinkel E et al. Increasing use of single and combination medical therapy in patients hospitalized for acute myocardial infarction in the 21st century. Archives of Internal Medicine 2007; 167(16): 1766-1773.
24. Paulus D. Performance of a process evaluation system in outpatient hospital-based cardiac rehabilitation. Blacksburg, VA: State University, 1997. Available: http://scholar.lib.vt.edu/theses/available/etd-71397-13485/unrestricted/PaulusDM.pdf (Accessed 1 October 2008).
25. Chew D, Amerena J, Coverdale S, Rankin J, Astley C, Brieger D. Current management of acute coronary syndromes in Australia: observations from the acute coronary syndromes prospective audit. Internal Medicine Journal 2007; 37(11): 741-748.
26. Scott I, Denaro C, Flores J, Bennett C, Hickey A, Mudge A. Quality of care of patients hospitalized with acute coronary syndrome. Internal Medicine Journal 2002; 32: 502-511.
27. Scott I, Heath K, Harper C, Clough A. An Australian comparison of specialist care of acute myocardial infarction. International Journal for Quality in Health Care 2003; 15(2): 155-161.
28. Kramer J, Newby L, Chang W, Simes R, Van de Werf F, Granger C et al. International variation in the use of evidence-based medicines for acute coronary syndrome. European Heart Journal 2003; 24: 2133-2141.
29. Roe M, Peterson E, Newby L, Chen A, Pollack C, Brindis R et al. The influence of risk status on guideline adherence for patients with non-ST segment elevation acute coronary syndromes. American Heart Journal 2006; 151(6): 1205-1213.
30. Tang E, Wong C, Wilkins G, Herbison P, Williams M, Kay P et al. Use of evidence-based management for acute coronary syndrome. The New Zealand Medical Journal 2005; 118(1233). Available: http://www.nzma.org.nz/journal/118-1223/1678/ (Accessed 4 February 2008).
31. Heidrich J, Behrens T, Raspe F, Keil U. Knowledge and perception of guidelines and secondary prevention of coronary heart disease among general practitioners and internists: results from a physician survey in Germany. European Journal of Cardiovascular Preventative Rehabilitation 2005; 12(6): 521-529.
32. Merenich J, Olson K, Delate T, Rasmussen J, Helling D, Ward D. Mortality reduction benefits of a comprehensive cardiac care program for patients with occlusive coronary artery disease. Pharmacotherapy 2007; 27(10): 1370-1378.
33. Barclay L. Early, intensive statin use may improve outcomes in acute coronary syndrome. Archives of Internal Medicine 2006; 166: 1814-1821.
34. National Heart Foundation and Australian Cardiac Society of Australia and New Zealand. Guidelines for preventing cardiovascular events in people with coronary heart disease. NHFA & CSANZ, 2004. Available: http://www.heartfoundation.org.au/document/NHF/ReducingRisk_HeartDisease_FullGuide_2007.pdf (Accessed 1 October 2008).
35. Feder G, Griffiths A, Eldridge S, Spence M. Effect of postal prompts to patients and general practitioners on the quality of primary care after a coronary event (POST): randomised controlled trial. BMJ 1999; 318: 1522-1526.
36. Minhas R. Statins in primary care: bridging the treatment gap. British Journal of Cardiology 2004; 11(6): 487-491.
37. Ko D, Alter D, Newman A, Donovan L, Tu J. Association between lipid testing and statin therapy in acute myocardial infarction patients. American Heart Journal 2005; 150(3): 419-425.
38. Clark A, Barbour R, MacIntyre P. Preparing for change in the secondary prevention of coronary heart disease: a qualitative evaluation of cardiac rehabilitation within a region of Scotland. Journal of Advanced Nursing 2002; 39(6): 589-598.
39. Williams A, Botti M. Issues concerning the ongoing care of patients with co-morbidities in acute care and post discharge in Australia: a literature review. Journal of Advanced Nursing 2002; 40(2): 131-140.
40. Bowman G, Bryar R, Thompson D. Is the place for cardiac rehabilitation in the community? Social Sciences in Health 1998; 4(4): 243-254.

