Introduction
The expected impact of climate change on the health of residents in the Australian desert and surrounding regions and the possible responses to that impact are discussed in this article. With less than 3% of the population, the desert region consists of arid and semi-arid lands that extend over 70% of Australia1. Characterised as hot, with poor soils, low biological productivity and a highly variable and uncertain climate, it is far removed from both political decision-makers and markets2.
The direct impacts on health, such as increased temperature, are important. But so too are the secondary impacts that will occur as a result of the impact of climate change on the natural environmental and on the interlinking social and economic systems3. The consequence of these secondary impacts will appear as changes in the incidence of disease and infections, and on the psychosocial determinants of health4,5.
We use a holistic approach as the basis for this analysis, as a means of interlinking the environmental, social and economic systems, and in recognition that different approaches will be required in different regions of this vast area. The content and approach taken in the article is based on the breadth of knowledge and experience of the authors, who have had an extensive involvement in these regions, together with a broad search of the recent climate change literature.
Responding to the health impacts of climate change in the Australian desert will require a high degree of collaboration among federal, state and local jurisdictions, including the integration of health services over all jurisdictions, and involvement of the private sector. The latter range from local commercial operators serving the local and tourist population to large mining industry corporations, as well as including community and individual responses.
Current environmental and health status
The introduction of domestic and feral grazing animals, weeds and the loss of traditional land management practices due to the disconnection of Aboriginal people from their country following European settlement have had a negative impact on the desert environment6,7. This has resulted in a loss of biodiversity and an increase in wildfires, soil erosion and dust storms8. There has been an overall increase in temperature and decreased effective rainfall since the 1950s9.
Of the total population of 584 000 (0.11 persons km-2), more than half are located in the five major service centres10, with the remainder scattered across more than 400 Aboriginal settlements and 3000 pastoral properties11. Aboriginal people make up 45% of the population in very remote areas11, although such areas do extend beyond the Australian desert. Due to the non-Aboriginal population's relatively lower birth rate and their outward migration, Aboriginal people are expected to make up an increasing proportion of the very remote regional population10.
Death rates in regional and remote areas are reported to be 10% to 70% higher than that observed in the major cities12. The higher rate in very remote areas is strongly influenced by the higher death rate of Aboriginal people13. The nature of the gap between Aboriginal and non-Aboriginal people and the expected increased costs and resources necessary to bridge this gap is well documented14,15.
We suggest that the national health delivery model currently operated by the Commonwealth, State and Territory governments is inadequate for those living in the desert region and, in particular, for Aboriginal people12. A commitment has been made by the Commonwealth government to closing this health gap16.
The impact of climate change
The major impact of climate change in the Australian desert is expected to revolve around higher mean temperatures, decreasing effective rainfall and an increased occurrence of extreme climatic conditions17. Increased temperatures will have a direct effect, causing increased heat stroke, cramps, heat exhaustion, and deaths18; while temperature increase is likely to result in increased skin cancer. These impacts will profoundly affect the need for preventive, primary level and hospital levels of care.
Those most vulnerable to climate change are the young, the elderly, the chronically ill - particularly those suffering from cardio-respiratory diseases - and the socio-economically disadvantaged who have less access to the resources to handle the increasing climatic extremes19. Vulnerability is compounded by inappropriate and inadequate housing, inadequate fresh water, poor access to essential services such as health, limited food supplies, power for cooling systems, and decreased participation in those social, cultural and economic activities most likely to be impacted by climatic change. On this basis, Aboriginal people will be the most disadvantaged, while those tied to natural resource-based industries such as pastoralism, or those otherwise required to work outside are also at greater risk. The implications for areas of health, welfare, aged care, housing, and other areas are apparent.
A variety of indirect risks are likely to be affected by climate change. Shallow groundwater supplies may dry up and become contaminated more often during dry periods. Decreased water availability could result in more cases of dehydration, increased water-born diseases, exacerbated impacts of poor household hygiene, and skin diseases through the lack of personal hygiene and swimming in infected and biotoxin-contaminated waterholes. Likewise, increasing temperatures coupled with poor living conditions could promote flies and other pests affecting food, and food poisoning caused by organisms such as Salmonella and Campylobacter. The changed conditions could also lead to an increase in meningococcal (epidemic) meningitis20. The health impacts of poor living conditions and infectious disease will be compounded, particularly among children. There is the potential for higher incidences of diarrhoeal disease, acute respiratory and skin infections and increased hospitalisation, particularly among Aboriginal infants and children aged less than 5 years. As with the factors noted above, it is clear that there will be multiple service implications of climate change in the desert, extending also to the interests of local government in their public health and safety responsibilities.
Climate change is also likely to lead to the loss of plant and animal refuge areas for relic species and decreased biodiversity21, and the potential loss of native foods and traditional medicines. Increased atmospheric carbon dioxide and higher temperatures will contribute to changing vegetation composition, favouring woody plants in some regions, and increasing wildfire risk in grass-dominated regions. The spread of the introduced buffel grass (Cenchrus ciliarus) will lead to hotter fires and the release of greenhouse gases through the loss of woody plants in some environments. Fires can also lead to injury and death, decreased ground cover and more extreme dust storms.
Fire smoke and increased dust storms and suspended fine particulate matter will increase the frequency of cardio-respiratory disease and asthma, among other diseases. In addition to the physical irritants of siliceous dust, such storms can carry fungus, viruses and bacteria. Research carried out elsewhere shows the movement of such aeroallergens to have serious health effects22,23. Dust-storms originating in the Australian desert can extend to either the west coast or to the east coast. The easterly extending storms have ranged as far north as Cairns and as far south as Sydney24, with implications for health promotion and the prevention and treatment of health conditions within and beyond the Australian desert.
Similarly, beyond the evident physical health corollaries of climate change, there will be multiple mental health effects. People will be under increased mental stress with the higher level and increased incidence of climatic extremes25. Health concerns extend beyond the more obvious bio-medical impacts with increased variability and environmental uncertainty, adding to the overall stress level. Potential reductions in incomes and social connections would also impact mental health. Although suicide rates are known to be higher among men living in rural areas, there is a paucity of data on the likely impact of climate change on residents in rural and remote areas, including among Aboriginal people26. The need for mental health resources is, however, clear.
There are additional low probability but high impact risks of rapid, threshold environmental changes that tip the global climate and, hence, local ecosystems to new states. Factors outside the Australian desert, such as changes in sea and atmospheric currents, could radically impact the desert climate, and further exacerbate the need for substantial responses to meeting health and other service provisions.
In summary, changes will result in a less productive environment that will affect natural systems, cultural resources, grazing and human activity. These will contribute to environmental and economic pressures against living in central Australia. People (including tourists) may be less tempted to visit or stay in the region; although, at the same time, the world will increasingly value open space. With increasing transport costs, there may be increased costs of production and lower returns from beef and native food production, tourism and local sales of Aboriginal arts and crafts. At the same time, individual demands for health and complementary inputs such as housing, water and waste management, and employment opportunities would increase supply costs.
Responses
We have suggested that environmental, social and economic structures are intimately linked to the health impacts of climate change. To be successful and cost effective, the prevention and mitigation of climate change impacts will require working with these and other interlinking structures. Any such response will also need to accommodate the high degree of risk and uncertainty associated with these links2.
It is our contention that a first step in dealing with this uncertainty is to apply a framework for identifying and categorising key variables. We suggest that it is important to recognise that remote Australia encompasses a diversity of environments, biophysically and socially27,28, that may require differentiated responses. Holmes27 classified 29 regions of remote Australia into seven types of regional trajectories (with 4 regions being unclassifiable); these have stood the test of time29, so we adopt these types as a first effort to consider differentiated responses (Table 1, Fig 1).
Table 1: A classification of current trajectories of remote regions
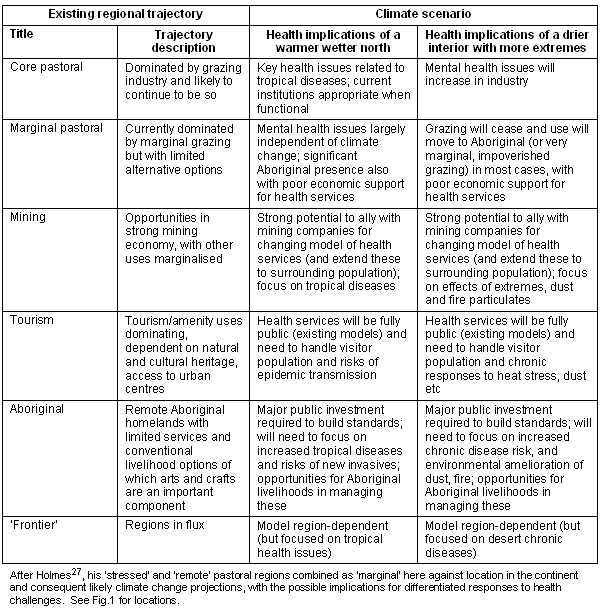
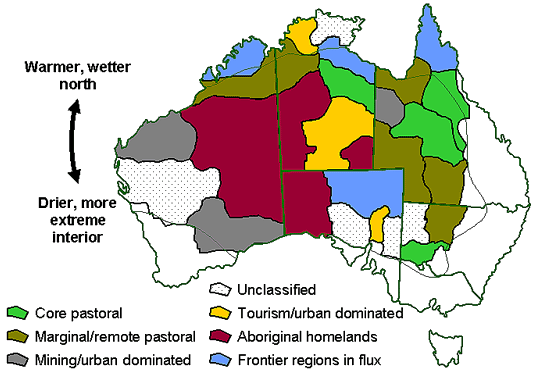
Figure 1: Locations of the different types of regions in remote Australia as defined by Holmes27. See his original work for the names, more detailed characterisations, and the likely major divergent effects of climate change.
The per capita demands for the full spectrum of health related services are likely to increase as a result of climate change - but in different ways in different regional types (Table 1). The total demand on health services will also depend on net migration and on the closure of the gap in health outcomes between Aboriginal and other Australians. The engagement of Aboriginal people in broader social and economic systems is vital to closing this gap and to the future management of remote Australia.
Uncertainty about future trends creates investment doubts, which are exacerbated by considering remote Australia as a single entity. By analysing social and climatic trends at a regional scale, it is possible to create a much more certain regional investment environment. Economic activity in the private sector, particularly mining and tourism, will drive opportunities in some regions. The effect that this will have on residents in the region will depend on the employment strategy used by the companies involved, and the preparedness of government and industry to negotiate new models of health support. If personnel and servicing are contracted outside of the region and flown in, there will be minimal positive impact in the region. Integration of the resident population with mining activities would be expected to have positive income and resulting health outcomes.
In regions not dominated by mining or tourism, there will be opportunities arising from the demands placed on the public sector as a result of climate change. These will include the need to stabilise existing vegetation to retain greenhouse gas (eg through biosequestration and soil stabilisation). This will, in part, involve the control of wild fires through spot burning, the control of weeds and feral animals, and the maintenance of biodiversity. One approach is to work with Aboriginal people to re-engage in traditional land management practices, while another is the engagement of pastoralists on marginal properties in stewardship activities on behalf of society. Both can have additional benefits in the joint supply of improved health outcomes and environmental services with justifiable public funding to the degree that the public good benefits of health and biodiversity would otherwise be under supplied. Such support for local engagement in natural resource management, together with negotiating with mining companies to enhance regional engagement with their activities, are appropriate policy actions because of their immediate benefits regardless of climate change impacts.
Our key observation is that each region requires a different combination of actions, encompassing public policy, engagement of private enterprise, community involvement and personal responsibility. There is, therefore, a need for a systematic analysis that: (i) considers whether the regionalisation we use in this analysis is the most appropriate; (ii) collates relevant information about each region; (iii) engages the community and businesses in each region (or at least each region type) in a discussion of future needs, in order to obtain their ownership of the solutions, and then (iv) proposes the appropriate balance of private responsibility and public investment for each region. This will result in far more efficient and effective outcomes than if there is an attempt to deliver to remote Australia as if one size fits all.
Conclusion
We have shown that addressing the health impacts of climate change in the Australian desert will involve working with how altered environmental, social and economic conditions interact with existing health conditions. We note that responding to the impacts of climate change on health in the Australian desert will involve the active participation of a variety of interest groups ranging from local to state and federal governments and a range of public and private agencies, including those not traditionally defined as within the health sector. The modes of engagement required for this process need to be innovative, and will differ among regions on different trajectories. To this end, we have attempted a first classification of these trajectories. This classification may require considerable refinement; however, we emphasise, it suffices to show that some form of sensible disaggregation is required to make progress in this vast and under-resourced heartland of Australia.
This large region is significant to Australia for its cultural, biodiversity and natural resources and deserves a greater degree of engagement regarding this issue than has occurred to date. Improved information and the integration of such information based on Australian and shared overseas experiences and research will assist in minimising the level of uncertainty and in defining future responses.
Acknowledgements
Acknowledgement is given to Penny Greenslade and Melissa Lindeman for their assistance, and three anonymous reviewers for their constructive thought and consideration. The work reported in this publication was jointly supported by funding from the Australian Government Cooperative Research Centre Program through the Desert Knowledge CRC and the Centre for Remote Health. The views expressed herein do not necessarily represent the views of Desert Knowledge CRC, the Centre for Remote Health or its participants.
References
1. Australian Bureau of Statistics. Year Book Australia 2006. Canberra, ACT: ABS, 2007.
2. Stafford Smith M. The 'desert syndrome' - causally linked factors that characterise outback Australia. The Rangeland Journal 2008; 30: 3-14.
3. McMichael AJ. Global climate change and health: an old story writ large. In: AJ McMichael, DH Campbell-Lendrum, CF Corvalán, KL Ebi, AK Githeko, JD Scheraga et al. Climate change and human health: risks and responses. Geneva: World Health Organisation, 2003.
4. Carson B, Dunbar T, Chenhall RD, Bailie R (Eds). Social determinants of Indigenous health. Sydney, NSW: Allen & Unwin, 2007.
5. Cass A, Cunningham J, Snelling P, Wang Z, Hoy W. Exploring the pathways leading from disadvantage to end-stage renal disease for Indigenous Australians. Social Science & Medicine 2004; 58: 767-785.
6. Lunt ID, Eldridge DJ, Morgan JW, Witt BG. A framework to predict the effects of livestock grazing and grazing exclusion on conservation values in natural ecosystems in Australia. Turner review no 13. Australian Journal of Botany 2007; 55(4): 401-415.
7. Gale SJ, Haworth RJ. Catchment-wide soil loss from pre-agricultural times to the present: Transport and supply-limitation of erosion. Geomorphology 2005; 45: 417-430.
8. Knight AW, McTainsh GH, Simpson W. Sediment loads in an Australian dust storm: implications for present and past dust processes. Catena 1995; 24: 195-213.
9. Australian Department of the Environment. Water, Heritage and the Arts. (Online) 2008. Climate trends. Available: www.climatechange.gov.au/impacts/trends/ (Accessed 13 March 2008).
10. Brown D, Taylor J, Bell M. The demography of desert Australia. The Rangeland Journal 2008; 30: 29-43.
11. Australian Institute of Health and Welfare. Rural, regional and remote health: a study on mortality. AIHW no PHE 45. Canberra, ACT: AIHW, 2008.
12. Australian Institute of Health and Welfare. Rural, regional and remote health: indicators of health status and determinants of health. AIHW rural health series no 9. Canberra, ACT: AIHW, 2008.
13. Vos T, Barker B, Stanley L Lopez A. The Burden of Disease and Injury in Aboriginal and Torres Strait Islander People: Summary Report. Brisbane, QLD: School of Population Health, The University of Queensland, 2007.
14. Deeble J, Agar JS, Goss J. Expenditure on health for Aboriginal and Torres Strait Islander peoples 2004-05. Health and welfare expenditure series no 32. Canberra, ACT: Australian Institute of Health and Welfare, 2008.
15. Ramsey J, Wakerman J, Jensen H, Farthing A. Central Australian Allied Health Planning Study. Alice Springs< NT: Centre for Remote Health, 2005.
16. Aboriginal and Torres Strait Islander Social Justice Commissioner and the Steering Committee for Indigenous Health Equality. ClosetheGap: National Indigenous Health Equality Targets. Outcomes from the National Indigenous Health Equality Summit. Canberra, ACT: Australian Government, 2008.
17. Hennessey K, Page C, McInnes K, Walsh K, Pittock B, Bathols J et al. Climate Change in the Northern Territory. Canberra, ACT: Northern Territory Department of Infrastructure, Planning and Environment by the Climate Change Group, CSIRO Atmospheric Research, 2004.
18. McMichael AJ, Woodruff R, Whetton P, Hennessy K, Nichols N, Hales S et al. Human health and climate change in Oceania: a risk assessment 2002. Canberra, ACT: Department of Health and Aging, Commonwealth of Australia, 2003.
19. McMichael AJ, Woodruff R. Climate change and risk to health. BMJ 2004; 329: 1416-1417.
20. Menne B, Bertollini R. The health impacts of desertification and drought. Down to Earth: The newsletter of the Convention to Combat Desertification 2000; 14: 4-8.
21. Hughes L. Climate change and Australia: trends, projections and impacts. Austral Ecology 2003; 28(4): 423-443.
22. Ichinose T, Yoshid T, Hiyoshi K, Sadakane K, Takona H, Nishikawa M et al. The effects of microbial materials adhered to in Asian sand dust on allergic lung inflammation. Archives of Environmental Contaminants and Toxicology 2008 (in press).
23. Kellogg CA, Griffin DW. Aerobiology and the global transport of desert dust. Trends in Ecology and. Evolution 2006; 21: 638-644.
24. Knight AW, McTainsh GH, Simpson RW. Sediment loads in an Australian dust storm: implications for present and past dust processes. Catena 1995; 24: 195-213.
25. Kovats R, Bouma M. Retrospective studies: analogue approaches to describing climate variability and health. In: P Martens, AJ McMichael (Eds). Environmental Change, Climate and Health. Cambridge: Cambridge University Press, 2002; 144-171.
26. McMichael AJ. Climate change, prolonged drought conditions and health: Implications for rural Australia, In: Proceedings, 9th National Rural and Remote Health Conference; 7-10 March 2007; Albury, Vic; 2007.
27. Holmes J. Diversity and change in Australia's rangelands: translating resource values into regional benefits. The Rangeland Journal 1997; 9: 3-25.
28. Maru YT, Chewings VH. How can we identify socio-regions in the rangelands of Australia? The Rangelands Journal 2008; 30: 45-53.
29. Holmes J. Impulses towards a multifunctional transition in rural Australia: gaps in the research agenda. Journal of Rural Studies 2006; 22: 142-160.
Abstract
Climate change is likely to have a significant effect on the health of those living in the 70% of Australia that is desert. The direct impacts on health, such as increased temperature, are important. But so too are the secondary impacts that will occur as a result of the impact of climate change on an uncertain and highly variable natural environment and on the interlinking social and economic systems. The consequence of these secondary impacts will appear as changes in the incidence of disease and infections, and on the psychosocial determinants of health. Responding to the impacts of climate change on health in desert Australia will involve the active participation of a variety of interest groups ranging from local to state and federal governments and a range of public and private agencies, including those not traditionally defined as within the health sector. The modes of engagement required for this process need to be innovative, and will differ among regions on different trajectories. To this end, a first classification of these trajectories is proposed.
Key words: Aboriginal, Australia, dust storms, environmental uncertainty, health risks, interlinking systems, primary health care.
You might also be interested in:
2014 - Investigating factors of self-care orientation and self-medication use in a Greek rural area






