Self-care is a practice recognized by WHO and it aims at the establishment and maintenance of health1. It is estimated that more than 80% of medical symptoms are self-recognized and treated without professional interference2. The most obvious and frequently used form of self-care is self-medication3. In 1998, WHO defined self-medication as the autonomous decision to use a medication without medical advice in order to treat self-diagnosed symptoms1.
Self-medication mainly involves the use of non-prescription or over-the-counter (OTC) drugs4 . These drugs are safe enough and appropriate to be used without medical supervision for minor ailments and legally sold without a medical prescription5,6. In one consumer survey, more than 92% of respondents had used at least one OTC drug during the past year and 55% of them had used more than one3. The rational use of OTC drugs is characterized as responsible self-medication, and self-care is encouraged7.
However, the practice of self-medication includes not only the use of approved OTC drugs, but also traditional remedies and herbal medicines, non-compliance in the use of medically prescribed drugs, use of prescription medications without a prescription or use of prescribed medications that remain stored from previous use4. The practice of using a prescription-only medication as non-prescribed, without previous professional recommendation (prescription or suggestion)8, is characterized as irresponsible self-medication9. It constitutes an undesirable behavior that exposes patients at risk as it concerns the use of substances designed to be used only under medical surveillance10.
According to the literature, some people are willing to self-medicate whereas others are reluctant to do so11. Self-care orientation refers to the undertaking of self-care activities -including self-medication12 - by an individual in order to restore and promote his/her own health without professional assistance13,14. Self-care orientation concerns self-care actions based on attitudes more favorable towards self-care15, whereas self-management, a term commonly used in the literature, refers to the controlling or handling of these actions16. Two relevant cross-sectional surveys refer to self-care orientation. In a study by Isacson and Bingefors17, in the general population, approximately 60% of the respondents were self-care oriented, whereas in a study by Sawalha13 among university students, 33% were highly self-care oriented and approximately 99% of them had practiced self-medication. Self-care orientation has been found to be associated with positive attitudes towards drugs17 as well as with certain patterns of self-medication18 (eg the choice of medications used for self-treatment)13.
A number of factors make an individual more likely to self-medicate14. According to existing studies some of these factors are sociodemographic10,19-26; others include the existence of chronic disease27,28, perception of health27,29,30, healthcare variables20,24 and beliefs about symptoms22 and self-medication11.
According to predictors of irresponsible self-medication with prescription medicines, a few relevant studies show that this unwanted practice is related mainly to sociodemographic factors10,28,31,32. This practice is reinforced by pill sharing among family members and by accumulating previously prescribed drugs in home pharmacies, increasing the risk of accidents or adverse effects9,33,34.
The evaluation of self-care specifically in rural healthcare settings has been very limited, although self-care is a significant component of healthcare systems29 and research has shown that residents of rural areas rely on, or sometimes even prefer, informal to professional treatment35. The various problems associated with living in rural areas, such as economic restraints, problems of delivery and distribution of care, problems of access and use of health care36, as well as personal knowledge and habits37, may affect healthcare decisions. Because self-care orientation is an important personal factor related to the concept of self-medication13, it could be used to evaluate self-medication practices in rural areas. Also, there is little information about differences in self-care orientation between various population groups or users of various types of drugs13,17.
Therefore, a cross-sectional study design was used to evaluate self-medication practices in a rural community of northern Greece (Imathia). This community is a particularly interesting one in which to explore predictors of self-care and self-medication; the population is served by a visiting general practitioner once a week and the nearest permanent doctor is 5 km away. In Greece, health personnel are unequally distributed throughout the country38. The fragmented national healthcare system is often unable to provide enough healthcare professionals to attend to the population of rural areas, thus people in these areas have fewer options of health care39. However, in this rural area there is a community pharmacy reporting a high percentage of non-prescription medication use. The lack of relevant studies in Greece increases the interest of the results. The main objectives were to: (1) detect factors that determine the likelihood of self-care orientation, (2) study the impact of self-care orientation in the likelihood of using medical care and (3) detect factors that predict the likelihood of using prescription drugs without a doctor's prescription. The secondary objectives were to define the target population to provide appropriate information and education in order to correct misuse and promote rational use of medicines23,40.
Study design
The cross-sectional survey 'Study of attitudes and beliefs on self-medication and the use of over-the-counter drugs in a rural community of Imathia, Greece' was designed to evaluate the prevalence of self-care orientation and self-medication in this small rural area.
Setting and sample selection
The survey data collection phase was implemented during January and February 2011. Random sampling was used to identify study subjects among the 800 adult members of the community. The adult population consisted of 409 men and 391 women. The age distribution was as follows: 18-34 years (269 individuals, 33.6%), 35-59 years (314 individuals, 39.3%) and ≥60 years (217 individuals, 27.1%). All adult subjects (≥18 years) who were residents of this rural community were eligible to participate: the single community pharmacy reported that OTC drug use was approaching 90% during the month prior to survey implementation (December 2010). There were no exclusion criteria. Sample size calculation was based on the formula of simple random sampling:
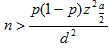
where a=0.05, d=5%, and p(self-medication)=90%. The sample size was calculated at n=119 adult individuals (≥18 years) and additional adults were identified to account for non-participation. Final participation exceeded estimates, with 150 adults providing data.
Instrument
Face-to-face interviews were conducted in the community pharmacy by using a research instrument with 46 questions. The basis for constructing the questionnaire was found in the international literature10,11,17,23,40,41 and included questions about self-rated health and the existence of chronic disease, self-medication behavior, use of prescription and non-prescription drugs and the sociodemographic characteristics42 of the respondents. The questions were selected and culturally adapted to a well-known rural population. Specific characteristics of the population were taken into account such as educational background and socioeconomic status. Finally, the questions were translated into Greek by a bilingual healthcare professional and then back-translated into the source language (English) by another healthcare professional. Appropriate corrections were also made43.
In this research, self-medication was measured by self-care orientation. The question was: 'In which of the following situations would you self-treat by using a medication without medical prescription (hypothetically)?' Self-care orientation was the basic question (variable) of the survey and was defined by the number of conditions that an individual reports that he/she would self-treat hypothetically by using a medicine (prescription or OTC drug) without a doctor's prescription or consultation. A self-care oriented individual would accept to self-treat in at least four of the following 13 conditions: headache; constipation or diarrhea; shortness of breath while at rest; skin rashes; back pain; persistent cough; sore throat; loss of weight without diet; dyspepsia or stomach upset; dizziness; common cold; problems of sleep; and fatigue17. Self-care orientation has been used in relevant surveys in the USA, Sweden12,17 and Israel13. In the final statistical analysis, the variable was dichotomized as 'no orientation' (0-3 conditions) or 'positive self-care orientation' (4-11 conditions).
The rational and irrational self-medication practice was estimated with the following open statement: 'Mention the medicine or medicines you have taken during the 3 last months for one or more symptoms of minor ailments (description) and if it was/they were taken with a doctor's prescription/suggestion or not'40. Undesirable self-medication was a secondary dependent binary variable (yes-no) defined as use of at least one prescription medication (based on the current Catalog of Prescription Medications in Greece) without a doctor's prescription for the period under study.
Per capita visits, which are one of the key variables of the present study, correspond to a recall period of 3 months according to Jones44 and O'Donnell and Van Doorslaer45.
Data analysis
Logistic regression was used to analyze the results. Binary logistic regression is a type of regression analysis used for predicting the outcome of a dichotomous variable based on one or more explanatory variables. The study of the effect of self-care orientation on the likelihood of medical care use was based on Fisher's exact test. The χ² test for independence evaluates the relationship between two variables. It is a nonparametric test that is performed on categorical data. Independent variables in the analysis were: age, gender, education, income, existence of chronic disease, self-rated health, marital status and occupation. Variable categories are shown in Table 1. Dummy variables were created to handle the multiple nominal categories of the variables 'marital status' and 'occupation'.
Models were evaluated for their goodness of fit using the Hosmer-Lemeshow test, and additional information for their appropriateness was checked with the link test. The explanatory value of the statistically significant variables was evaluated based on a receiver operating characteristic (ROC) curve. Finally, normality of deviance residuals and homoscedasticity of standardized deviance residuals were checked.
Statistical analysis was carried out using the STATA 9 statistical software package (StataCorp, http://www.stata.com).
Ethics approval
The study was approved by the Ethics Committee of the Hellenic Open University (#535, 09/24/2010).
Descriptive statistics
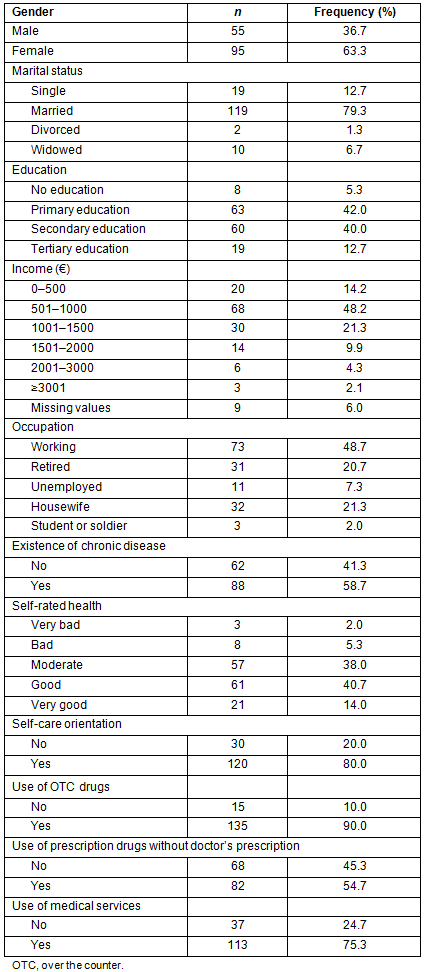
Sociodemographic, self-rated health and behavioral characteristics for the sample appear in Table 1. The mean age of the respondents was 48.3±15.9 years and the percentages of men and women were 36.7% and 63.3% respectively. The majority of respondents were married (79.3%), having primary or secondary education (82%), low income (48.2% reported income between 501 and 1000 ?) and employed (48.7%). An interesting contradictory finding was that 58.7% of this population group reported the existence of a chronic disease but also the majority (54.7%) reported a good or very good self-rated health status. Finally, 80% of the respondents were oriented towards self-care, 90% used OTC drugs, 54.7% used prescription medications without a prescription and 75.3% reported using some kind of medical service during the previous 3 months.
Table 1: Sample characteristics
Self-care orientation predictors
The orientation to self-care seems to be determined by gender, the existence of chronic disease and educational level (Table 2).
As shown in Table 2, women as well as more highly educated individuals are more likely to be oriented to self-care: the odds ratio (OR) is 3.44 times higher for women than men (OR: 3.44, 95% confidence interval (CI): 1.37-8.66) and 1.64 times higher for those of higher educational level than the less literate (OR: 1.64, 95% CI: 1.05-2.58). By contrast, individuals that have a chronic disease are less likely to be self-care oriented: odds ratios are 0.30 compared to those with no chronic disease (OR: 0.30, 95% CI: 0.09-0.92).
This specific model has an accepted goodness of fit of x2H-L=4.17, degrees of freedom (df)=7, p=0.76. Also, the link test gave satisfactory results: hat is statistically significant (p<0.05) and hat2 is non-statistically significant (p>0.05), which means that there is no specification error.
Additionally, the skewness and kurtosis test indicates that deviance residuals follow a normal distribution as p>0.05, whereas standardized deviance residuals according to the Brown-Forsythe test are homoscedastic, given that p>0.05.
The area under the ROC curve is 0.76, a relatively high explanatory value for the statistically significant values of the model (Fig1).
Table 2: Results of logistic regression for self-care orientation
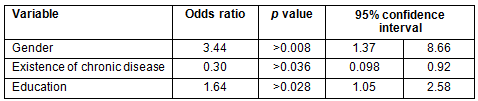
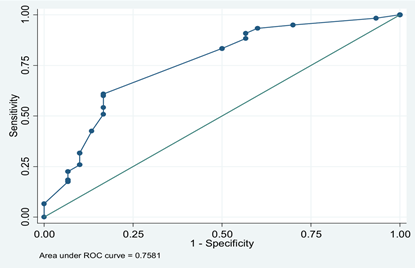
Figure 1: Receiver operating characteristic (ROC) curve for self-care orientation.
Medical care use
Regarding the use of medical care, 75.3% (n=113) of the sample had visited a doctor during the 3 months before the survey. However, self-care orientation was not found to affect the use of medical services: p(Fisher's exact test)>0.05.
Irrational self-medication predictors
With regard to using prescription medications without a doctor's prescription, the analysis revealed that a quite high percentage (54.7%, n=82) of the respondents used prescription medications without the prerequisite of prescription. The likelihood of this specific use is defined by self-care orientation and the self-rated health status (Table 3).
Based on the results shown in Table 3, the likelihood of using prescription drugs without a prescription is increasing in the case of individuals that are self-care oriented: the odds ratio is 6.16 times that of those who are not self-care oriented (OR: 6.16, 95% CI: 2.38-15.89). It is decreasing as the self-rated health is becoming better, having an odds ratio of 0.65 compared to those with worse health status (OR: 0.65, 95% CI: 0.42-0.99).
This specific model has accepted goodness of fit as x2H-L=2.49, df=4, p=0.65. Also, the link test is giving satisfactory results as hat is statistically significant (p<0.001) and hat2 is not statistically significant (p>0.05).
The skewness and kurtosis test indicates that deviance residuals follow a normal distribution (p>0.05), whereas standardized deviance residuals according to the Brown and Forsythe test are homoscedastic (p>0.05).
The area under the ROC curve was 0.69, a relatively high explanatory value for the statistically significant values of the model as indicated in Figure 2.
Table 3: Results of logistic regression for use of prescription drugs without doctor's prescription
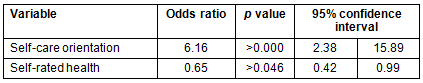
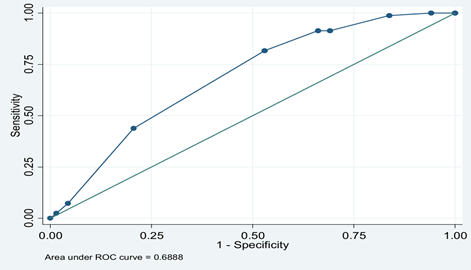
Figure 2: Receiver operating characteristic (ROC) curve for the use of prescription drugs without a doctor's prescription.
Discussion
According to the results the great majority (80%) of the respondents in this rural community are self-care oriented. Although there is a lack of similar surveys in Greece to make comparisons, the international literature shows studies with a high prevalence of self-medication among rural residents46,47. In rural areas health is significantly associated with ability to work35. This fact, combined with the financial, medical and geographical restrictions of rural areas36, may force residents to usually self-treat their health disorders.
The study identified three main predictors of self-care orientation by using a medication and consequently self-medication practices. The three predictors were gender, educational level and the absence of chronic disease.
The fact that women are more likely to self-medicate has been detected in previous surveys10,27. Additionally, other studies show high prevalence of medication use by rural female populations48,49. According to the literature, gender determines health maintenance behaviors50. So the fact that women have more symptoms than men51, possibly due to differences in their physiology but also in social roles21 and in combination with their greater sensitivity to symptoms, leads women in using medications more easily than men52 and makes them more strongly self-care oriented14. The latter may also be strengthened because women spend more time at home where drugs are stored14. Another reason for the extensive self-treatment among female residents of rural areas may be their active involvement both in agricultural and household activities. Being occupied most of the day explains why they do not have time to seek other medical care53. However there are contradicting articles showing that men self-medicate more often than women19,20, or even equally24, and also surveys indicating that women apart from their self-medicating inclination also consult a general practitioner more readily than men51,54,55.
It was also found that the likelihood of self-medication increases with increasing educational level. This finding is in accordance with the published literature10,22,27; individuals with higher education have more knowledge about medications as compared to the less educated, and may be more competent in self-medication56. Additionally they seem to perceive and evaluate symptoms differently54,57. According to Figueiras et al10 the more educated have more self-confidence in self-diagnosis and self-medication and less trust in doctors, particularly in the presence of an acute disorder, and they are more capable of selecting appropriate medications to attend to their symptoms, whereas less educated people prefer a medical consultation to self-medication because of lack of any knowledge about pharmaceuticals.
Individuals with a chronic disease are less likely to self-medicate. It seems that these individuals have established long-term rapport and a relationship with a doctor, and they may visit their personal doctor more often due to their illness or other symptoms28. In a study by Farmer et al37, rural patients had a stronger relationship with their doctors. Another explanation may be that they probably take prescription medications for their chronic disease, and due to risk of possible interactions58 they are afraid to self-medicate. Consequently they self-medicate less.
According to the results, self-care orientation does not seem to have an impact on use of medical services. People will utilize medical services even if they practice self-medication. This result is in accordance with previous findings that self-medication is not related to the frequency of medical consultation8. There are various possible explanations for this observation. It is possible that individuals use self-medication prior to or in addition to medical care and consult doctors to check or be reassured of their choices59. It is also possible that self-carers will visit a doctor if symptoms do not respond to self-medication60 or they may choose to self-treat certain less serious symptoms only and not others61.
In this survey, a worryingly high percentage (54.7%) of the respondents had used prescription-only medications without having been prescribed or recommended them by a doctor, in the months prior to the survey. According to the literature this undesirable practice (irrational self-medication) is a phenomenon usually present in rural areas either as use of non-prescribed antibiotics28,33,62, or as use of previously prescribed medications29. Kalomenidis et al63 found that the latter kind of drug consumption occurs more often in people insured by the Organisation of Agriculture Insurances, those who are mainly habitants in rural areas39.
The lack of sufficient self-care support and information about rational self-medication especially among the less literate64, in combination with the accumulation of previously prescribed medicines found in rural home pharmacies and high exchange prevalence between residents65, may lead individuals to irrational self-medication practices. Previous experience of drug effectiveness seems also to be an important factor in the selection of a substance during self-medication66. Another important attribute to the use of OTC drugs with or without previously prescribed and currently stored medications at home may be related to the cost of the medications; OTC drugs are not compensated by social medical insurance plans whereas prescription medicines are. Using prior prescriptions seems to be the least expensive choice, followed by obtaining a new prescription from a doctor. This practice is strengthened by the insufficient access to doctors in rural areas24.
Individuals with self-care orientation are more likely to use prescription medications without a prescription. A positive attitude towards self-care extends to the use of all medication categories (prescription and non-prescription)13.
In the present study there was a statistically significant association between use of prescription medications without a prescription and low self-rated health status. The literature around this subject is mixed. Studies show that self-medication practice is more frequent among healthier people with higher health status27-29, without however precluding the use of non-prescription medications in cases of low self-rated health30. According to Bartlomé et al29, individuals with low perceived health use more medications (prescription and non-prescription). Taking into consideration that the use of prescription medications increases with the severity of a disorder58, the use of prescription medications without a prescription possibly takes place when the symptoms people try to self-manage are serious enough to negatively influence health status. In fact, as the severity of the symptoms increase, irrational self-medication without the required medical consultation is becoming more risky67 and may lead to more negative influences in health status. The absence or inaccessibility of a permanent doctor may magnify the effect of this phenomenon. The degree of the severity of symptoms for which prescription medicines are used was not studied in the present study and requires future attention by healthcare services researchers.
Generally, safe practice of self-medication requires a specific level of knowledge about correct medicine usage68. Consequently, there is a need to educate individuals in the safe and rightful use of medicines40, especially in rural areas where medical sources are limited. Taking into consideration the preference of rural habitants for informal networks, the building of collaborations and a support network with healthcare professionals (physicians, pharmacists, nurses) may contribute to improvements in health status35 for the population of rural areas in Greece and elsewhere.
Strengths and limitations
The scarcity of studies regarding self-medication evaluation and non-prescription medication use in Greece and especially in rural areas makes the present study unique at the time it was conducted. However, certain limitations are acknowledged. Because the interest of the study is restricted to this specific rural community, the generalization of the results is not appropriate. However, it can orient other researchers in larger relevant studies for the extraction of safer conclusions according to self-care orientation and self-medication practices in rural areas. Undoubtedly self-medication is a common practice followed in urban areas as well, so further exploration is needed to determine predicting factors of such practices in rural areas compared to urban ones. Although many of the findings are in agreement with the international literature, comparisons are difficult because of the different methodologies and populations under study (different cultures, different environments)24. Besides, there is a lack of similar studies in Greece. Finally the impact of attitudes and beliefs towards medicines in general and OTC drugs specifically was not studied, although they are proven to be important in self-care orientation and self-medication inclination11,17.
According to this research, 80% of the residents of a rural community in Imathia, Greece, were self-care oriented. Factors that predict self-care orientation and consequently self-medication were female gender, the absence of chronic disease and higher educational level. Self-care orientation was not associated with the likelihood of using medical services. Finally, individuals who practice self-medication with prescription drugs are self-care oriented and they probably have lower self-rated health status. Future research is required in larger samples of rural and urban communities to understand specific patterns of self-medication either with OTC or prescription drugs. Research is also needed to design and evaluate educational interventions aimed to increase rational self-medication and to control irrational self-use of medications.
References
1. World Health Organization. The role of the pharmacist in self-care and self-medication. Report of the 4th WHO Consultative Group on the Role of the Pharmacist. The Hague, The Netherlands, 26-28 August 1998. WHO/DAP/98.13. Geneva: WHO, 1998.
2. Sobel DS. 'Patients as partners improving health and cost outcomes with self-care and chronic disease self-management'. NatPaCT Conference, The Brewery, London, 4 November 2003 (Online). Available: http://www.natpact.info/uploads/DavidSobel.ppt (Accessed 16 June 2013).
3. Wertheimer AI, Serradell J. A discussion paper on self-care and its implications for pharmacists. Pharmacy World & Science 2008; 30(4): 309-315.
4. Dean K. Lay care in illness. Social Science & Medicine 1986; 22(2): 275-284.
5. Commission of the European Communities. Directive for medicines classification. 92/26/EEC of 31 March 1992 concerning the classification for the supply of medicinal products for human use, OJ L 113, 30.4.1992, pp. 5-7 (Online) 1997. Available: http://eurlex.europa.eu/LexUriServ/LexUriServ.do?uri=COM:1997:0581:FIN:EN:PDF (Accessed 15 June 2013).
6. Kirch W (Ed). Encyclopedia of Public Health. New York: Springer, 2008.
7. Krishnan HS, Schaefer M. Evaluation of the impact of pharmacist's advice giving on the outcomes of self-medication in patients suffering from dyspepsia. Pharmacy World & Science 2000; 22(3): 102-108.
8. Chaiton A, Spitzer WO, Roberts RS, Delmore T. Patterns of medical drug use - a community focus. Canadian Medical Association Journal 1976; 114(1): 33-37.
9. Aljinovi?-Vuci? V, Trkulja V, Lackovi? Z. Content of home pharmacies and self-medication practices in households of pharmacy and medical students in Zagreb, Croatia: findings in 2001 with a reference to 1977. Croatian Medical Journal 2005; 46(1): 74-80.
10. Figueiras A, Caamaño F, Gestal-Otero JJ. Sociodemographic factors related to self-medication in Spain. European Journal of Epidemiology 2000; 16(1): 19-26.
11. James DH, French DP. The development of the Self-Medicating Scale (SMS): a scale to measure people's beliefs about self-medication. Pharmacy World & Science 2008; 30(6): 794-800.
12. Isacson D, Bingefors K. Epidemiology of analgesic use: a gender perspective. European Journal of Anaesthesiology 2002; 19(Supplement 26): 5-15.
13. Sawalha AF. A descriptive study of self-medication practices among Palestinian medical and nonmedical university students. Research in Social and Administrative Pharmacy 2008; 4(2): 164-172.
14. Levin LS, Idler EL. Self-care in health. Annual Review of Public Health 1983; 4: 181-201.
15. Saunders KW, Von Korff M, Pruitt SD, Moore JE. Prediction of physician visits and prescription medicine use for back pain. Pain 1999; 83(2): 369-377.
16. Taylor SG, Renpenning K. Self-care science, nursing theory and evidence-based practice. New York: Springer, 2011; 57.
17. Isacson D, Bingefors K. Attitudes towards drugs - a survey in the general population. Pharmacy World & Science 2002; 24(3): 104-110.
18. Almasdy D, Sharrif A. Self-medication practice with nonprescription medication among university students: a review of the literature. Archives of Pharmacy Practice 2011; 2(3): 95-100.
19. Shankar PR, Partha P, Shenoy N. Self-medication and non-doctor prescription practices in Pokhara valley, Western Nepal: a questionnaire-based study. BMC Family Practice 2002; 3(1): 17.
20. Martins AP, Miranda AdC, Mendes Z, Soares MA, Ferreira P, Nogueira A. Self-medication in a Portuguese urban population: a prevalence study. Pharmacoepidemiology and Drug Safety 2002; 11(5): 409-414.
21. Zadoroznyj M, Svarstad BL. Gender, employment and medication use. Social Science & Medicine 1990; 31(9): 971-978.
22. Saeed AA. Self-medication among primary care patients in Farazdak Clinic in Riyadh. Social Science & Medicine 1988; 27(3): 287-289.
23. Yousef AM, Al-Bakri AG, Bustanji Y, Wazaify M. Self-medication patterns in Amman, Jordan. Pharmacy World & Science 2008; 30(1): 24-30.
24. Nunes de Melo M, Madureira B, Nunes Ferreira AP, Mendes Z, Miranda AdaC, Martins AP. Prevalence of self-medication in rural areas of Portugal. Pharmacy World & Science 2006; 28(1): 19-25.
25. Habeeb GE Jr, Gearhart JG. Common patient symptoms: patterns of self-treatment and prevention. Journal of the Mississippi State Medical Association 1993; 34(6): 179-181.
26. Beitz R, Dören M, Knopf H, Melchert HU. [Self-medication with over-the-counter (OTC) preparations in Germany]. [in German] Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 2004; 47(11): 1043-1050.
27. Carrasco-Garrido P, Jiménez-García R, Hernández Barrera V, Gil de Miguel A. Predictive factors of self-medicated drug use among the Spanish adult population. Pharmacoepidemiology and Drug Safety 2008; 17(2): 193-199.
28. Berzanskyte A, Valinteliene R, Haaijer-Ruskamp FM, Gurevicius R, Grigoryan L. Self-medication with antibiotics in Lithuania. International Journal of Occupational Medicine and Environmental Health 2006; 19(4): 246-253.
29. Bartlomé JA, Bartlomé P, Bradham DD. Self-care and illness response behaviors in a frontier area. The Journal of Rural Health 1992; 8(1): 4-12.
30. Itterman R, Johnson J, Taylor J. Health Status and self-medication patterns in Alberta, Canada. Results from a population health survey. Journal of Social and Administrative Pharmacy 2003; 20(2): 43-52.
31. Grigoryan L, Haaijer-Ruskamp FM, Burgerhof JGM, Mechtler R, Deschepper R, Tambic-Andrasevic A, et al. Self-medication with antimicrobial drugs in Europe. Emerging Infectious Diseases 2006; 12(3): 452-459.
32. Mitsi G, Jelastopulu E, Basiaris H, Skoutelis A, Gogos C. Patterns of antibiotic use among adults and parents in the community: a questionnaire-based survey in a Greek urban population. International Journal of Antimicrobial Agents 2005; 25(5): 439-443.
33. Okumura J, Wakai S, Umenai T. Drug utilisation and self-medication in rural communities in Vietnam. Social Science & Medicine 2002; 54(12): 1875-1886.
34. De Bolle L, Mehuys E, Adriaens E, Remon JP, Van Bortel L, Christiaens T. Home medication cabinets and self-medication: a source of potential health threats? Annals of Pharmacotherapy 2008; 42(4): 572-579.
35. Weinert C, Long KA. Rural families and health care: refining the knowledge base. Marriage & Family Review 1990; 15(1-2): 57-75.
36. Escovitz A, Birdwell SW. Determining specific health care needs of rural communities. Journal of Health Care for the Poor and Underserved 1996; 7(4): 285-289.
37. Farmer J, Iversen L, Campbell NC, Guest C, Chesson R, Deans G, MacDonald J. Rural/urban differences in accounts of patients' initial decisions to consult primary care. Health & Place 2006; 12(2): 210-221.
38. Marketos S, Merikas G. Primary health care in Greece. World Health Forum 1981; 2(1): 69-71.
39. Oikonomou N, Tountas Y. Insufficient primary care services to the rural population of Greece. Rural and Remote Health 11(1): 1661 (Online) 2002. Available: www.rrh.org.au (Accessed 10 February 2012).
40. Cuzzolin L, Benoni G. Safety of non-prescription medicines: knowledge and attitudes of Italian pharmacy customers. Pharmacy World & Science 2010; 32(1): 97-102.
41. National Council on Patient Information and Education (NCPIE, USA). Attitudes and beliefs about the use of over-the-counter medicines: a dose of reality. A national survey of consumers and health professionals (Online) 2002. Available: http://www.bemedwise.org/survey/final_survey.pdf (Accessed 20 October 2010).
42. Pol LG, Thomas RK. The demography of health and health care, 2nd edn. New York: Kluwer Academic/Plenum Publishers, 2001.
43. Harkness, JA, Schoua-Glusberg A. Questionnaires in translation. ZUMA-Nachrichten Spezial 1998; (3): 87-127.
44. Jones ΑΜ. The Elgar companion to health economics. Cheltenham, GLOS: Edward Elgar Publishing, 2006.
45. O'Donnell Ο, Van Doorslaer Ε. Analyzing health equity using household survey data: a guide to techniques and their implementation. Washington, DC: World Bank Institute, 2007.
46. Phalke VD, Phalke DB, Durgawale PM. Self-medication practices in rural Maharashtra. Indian Journal of Community Medicine 2006; 31(1): 34-35.
47. Stoehr GP, Ganguli M, Seaberg EC, Echement DA, Belle S. Over-the-counter medication use in an older rural community: the MoVIES Project. Journal of the American Geriatrics Society 1997; 45(2): 158-165.
48. Glover DD, Rybeck BF, Tracy TS. Medication use in a rural gynecologic population: prescription, over-the-counter, and herbal medicines. American Journal of Obstetrics and Gynecology 2004; 190(2): 351-357.
49. Lassila HC, Stoehr GP, Ganguli M, Seaberg EC, Gilby JE, Belle SH, Echement DA. Use of prescription medications in an elderly rural population: the MoVIES Project. Annals of Pharmacotherapy 1996; 30(6): 589-595.
50. Dean K. Self-care components of lifestyles: the importance of gender, attitudes and the social situation. Social Science & Medicine 1989; 29(2): 137-152.
51. Wyke S, Hunt K, Ford G. Gender differences in consulting a general practitioner for common symptoms of minor illness. Social Science & Medicine 1998; 46(7): 901-906.
52. Verbrugge LM. Gender and health: an update on hypotheses and evidence. Journal of Health and Social Behaviour 1985; 26(3): 156-182.
53. Sharma RK, Dhawan S. Health problems of rural women. Health and Population Perspectives and Issues 1986; 9(1): 18-25.
54. Sharp K, Ross CE, Cockerham WC. Symptoms, beliefs, and the use of physician services among the disadvantaged. Journal of Health and Social Behaviour 1983; 24(3): 255-263.
55. Bertakis KD, Azari R, Helms LJ, Callahan EJ, Robbins JA. Gender differences in the utilization of health care services. Journal of Family Practice 2000; 49(2): 147-152.
56. Abosede OA. Self-medication: an important aspect of primary healthcare. Social Science & Medicine 1984; 19(7): 699-703.
57. Alberts JF, Sanderman R, Gerstenbluth I, van den Heuvel WJ. Sociocultural variations in help-seeking behavior for everyday symptoms and chronic disorders. Health Policy 1998; 44(1): 57-72.
58. Rabin DL, Bush PJ. Who's using medicines? Journal of Community Health 1975; 1(2): 106-117.
59. Punamaki RL, Kokko SJ. Reasons for consultation and explanations of illness among Finnish primary-care patients. Sociology of Health & Illness 1995; 17(1): 42-64.
60. Zola IK. Pathways to the doctor - from person to patient. Social Science & Medicine 1973; 7(9): 677-689.
61. Bell R. Over-the-counter drugs: factors in adult use of sedatives, tranquilizers, and stimulants. Public Health Reports 1984; 99(3): 319-323.
62. Skliros E, Merkouris P, Papazafiropoulou A, Gikas A, Matzouranis G, Papafragos C, Sotiropoulos A. Self-medication with antibiotics in rural population in Greece: a cross-sectional multicenter study. BMC Family Practice 2010; 11(1): 58.
63. Kalomenidis K, Mitropoulos G, Sissouras A. Demand and use of medicines from Greek population results of an empirical study in Achaia population. In: M. Gitona, G. Kyriopoulos (Eds), Politics and Economics of Medication in Greece. [in Greek]. Athens: Themelio/Society and Health, 1999; 163-181.
64. Pignone MP, DeWalt DA. Literacy and health outcomes: is adherence the missing link? Journal of General Internal Medicine 2006; 21(8): 896-897.
65. Tsiligianni IG, Delgatty C, Alegakis A, Lionis C. A household survey on the extent of home medication storage. A cross-sectional study from rural Crete, Greece. European Journal of General Practice 2012; 18(1): 3-8.
66. Hanna LA, Hughes CM. Public's views on making decisions about over-the-counter medication and their attitudes towards evidence of effectiveness: a cross-sectional questionnaire study. Patient Education and Counseling 2011; 83(3): 345-351.
67. Ruiz ME. Risks of self-medication practices. Current Drug Safety 2010; 5(4): 315-323.
68. World Health Organization. Guidelines for the regulatory assessment of medicinal products for use in self-medication. WHO/EDM/QSM/00.1. Geneva: WHO, 2000.
