Introduction
Since 1990 several airway devices have become available to assist in difficult intubation. Multiple surveys have assessed difficult airway equipment (DAE) availability in anaesthetic departments and emergency departments internationally, allowing comparison with available recommendations1-3. In Australia, only adult emergency departments have been surveyed regarding airway equipment4.
The population distribution in Queensland, Australia results in a concentration of healthcare services. Outside secondary and tertiary centres elective and emergency airway management is performed by non-vocationally trained anaesthetists. Their practice is unique in both its multidisciplinary nature and geographical isolation5.
All general practitioners who perform anaesthesia in rural and remote Queensland were surveyed to assess the availability of DAE and whether this was related to practice location or involvement in continuing professional development (CPD) activities. The results may influence future training opportunities and provision of DAE in remote areas.
Methods
Following approval by the Royal Brisbane and Women's Hospital Human Research Ethics Committee, the survey was sent to all rural general practitioners listed with Health Workforce Queensland (HWQ) as proceduralists performing general anaesthesia in rural locations. The HWQ is a rural workforce agency whose key activities are 'to facilitate the recruitment, retention and quality of general medical practitioners and primary health care teams in rural and remote Queensland communities'6. Our sample included proceduralists in hospitals categorised as Rural, Remote and Metropolitan Area (RRMA) classification 4 to 7.
The RRMA system is a remoteness classification that divides Australia into areas according to city status, population, rurality and remoteness7. The scale is 1 to 7 with 7 being most remote (Fig 1). The working brief of Rural Workforce Agencies includes locations classified RRMA 4 to 7. The HWQ information is updated annually and is confidential. The authors were blinded to the personal details of the practitioners and mailing was coordinated by HWQ. Returned surveys were de-identified and numbered. Seventy-nine surveys were distributed. An incentive prize was advertised to enhance the response rate.
The first section of the survey covered demographic information including CPD activities specifically related to airway management skills. The next section identified equipment currently available to the practitioner. This was based on the American Society of Anesthesiologists' (ASA) suggested contents of a portable storage unit for difficult airway management8 (Fig2). The availability of on-site assistance was surveyed, with additional space for general comment on the subject.
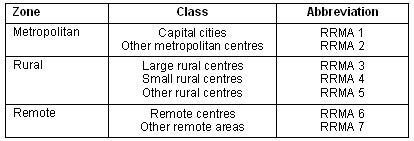
Figure 1: Structure of the RRMA Classification7.

Figure 2: Suggested contents of the portable storage unit for difficult airway management - ASA Taskforce on Difficult Airway Management8.
The received data were entered into a Microsoft Excel spreadsheet and analysed in Statistical Package for Social Sciences v15.0 (SPSS Inc; Chicago, IL, USA) using the frequencies and crosstabs functions. Due to small cell counts, some categories were combined. Some variables were transformed and re-analyzed as binary variables but this did not always resolve the problem of small cell counts. The Fisher's exact test was used. A p-value of less than 0.10 was considered noteworthy and a p-value of less than 0.05 was considered to be significant. In many cases there were several respondents from each hospital, therefore results were analysed as per respondent, rather than per hospital.
A statistical comparison was made between the known demographics of the target population (n = 79) and the survey responders (n = 35)9,10. The known demographics were derived from the Health Workforce Queensland (HWQ) database and included age, gender, practice location and practitioner type. Accurate data for level of experience (in years) was not available.
Results
Thirty-five surveys were returned (response rate of 44%). Respondents from 21 hospitals returned their surveys. The demographics of the target population and survey responders were compared to determine if the survey results were representative. There was no statistical difference between the two groups in terms of age and gender. There was no statistical difference in terms of practice location, although the small percentage responding from RRMA 6 was notable. There was a difference between the groups in terms of practitioner type. The responder group consisted of 38% hospital based and 62% Queensland Health salaried. The target population consisted of 58% hospital based and 42% Queensland Health salaried. This was statistically significant (p = 0.0002).
Demographic data are summarised (Table 1). Hospitals classified as RRMA 5 were the most frequently represented (50%). The respondents were experienced practitioners with 25 out of the 35 (71%) having greater than 10 years experience. There was wide variation in number of anaesthetics performed.
Thirty-four out of the 35 (97%) had attended at least one CPD activity specific for airway skills in the last year. Practitioners in the more remote locations were less likely to have attended an event such as conference, workshop or skills training laboratory (p = 0.058) (Table 2). These were the most commonly attended activities (91%), as shown in Table 3.
Most practitioners had no expert assistance available to them in elective cases (60%) or emergency cases (63%). In the absence of assistance, 13 of the 35 (37%) utilised telephone assistance from larger institutions. There was no relationship between the RRMA category and availability of expert assistance.
Data pertaining to equipment is summarised (Table 4). Eighty per cent of respondents stated that they had appropriate DAE. Regarding intubation aids, 26% and 20% reported no access to intubating stylet and gum-elastic bougie, respectively. In contrast, surgical airway equipment was present in 86% of cases.
Table 1: Respondents' demographic data (n = 35)
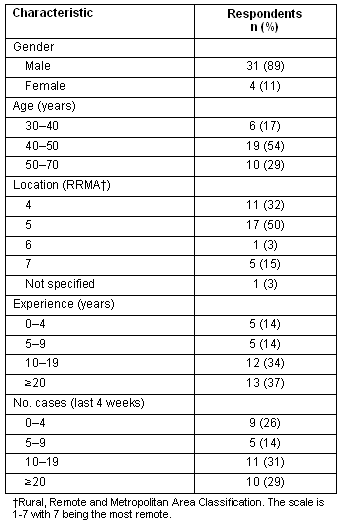
Table 2: Relationship between the practice location and attendance at a continuing professional development activity, such as conference, workshop or skills training laboratory

Table 3: Participation in airway-related continuing professional development activities
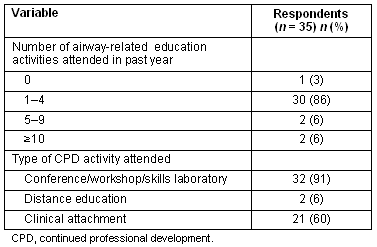
Table 4: Equipment availability (per respondent; n = 35), based on the suggested contents of the portable storage unit for difficult airway management - ASA Taskforce on Difficult Airway Management8
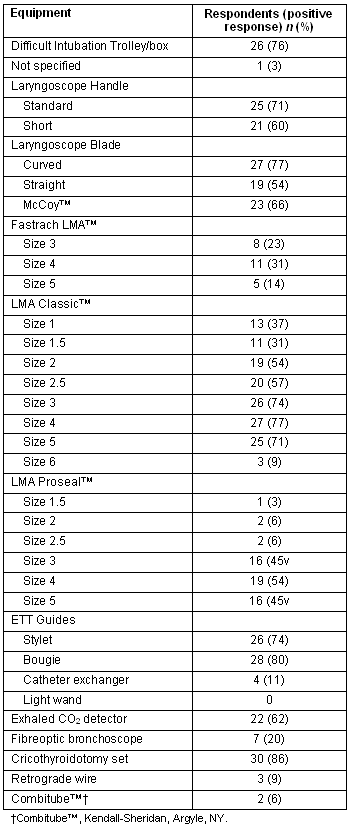
Availability of the Fastrach Laryngeal Mask Airway (LMA; LMA North America Inc; San Diego, CA, USA) in all sizes was low. Seven out of the 35 (20%) reported the availability of a fibreoptic bronchoscope with one stating an inability to use it and another noting difficulty in obtaining and maintaining skills.
Discussion
The majority of rural general practitioner anaesthetists in Queensland felt they have appropriate DAE. This is not reflected in the data collected. Predominantly, there was no relationship between the availability of equipment and the remoteness of the practice location. The isolated nature of rural anaesthetic practice is highlighted with limited on-site assistance for an elective or emergency difficult airway.
Surgical airway devices were the most readily available (86%). Less invasive devices (bougies, stylets) used prior to surgical airway were not commonly present, or known by the respondents to be present.
Access to intubating LMA of sizes 3, 4 and 5 was limited. This non-surgical method allows more efficient ventilation than a classic LMA and provides a means of subsequent intubation. Minimum training is required for this technique11.
The ASA Guidelines for Management of the Difficult Airway recommend using alternative laryngoscope blades in an unanticipated difficult airway. Our survey revealed that straight and McCoy blades were less frequently available than curved blades. The use of a McCoy blade utilises pre-existing skills, is non-surgical and has been shown to improve laryngoscopy views in 50% of patients12. The infrastructure involved in maintenance is similar to that of standard laryngoscope blades.
Size one classic LMA was available in 37% of cases. The use of an LMA in newborn resuscitation was discussed in the most recent resuscitation guidelines13. Wider access to size one LMA may be warranted, especially in the setting of obstetric anaesthesia.
Access to a fibreoptic bronchoscope was higher than expected (7 of 35) and this was not related to remoteness. Comments reflected difficulties in achieving and maintaining bronchoscopy skills in rural anaesthetic practice. The cost of maintaining equipment could be prohibitive14.
The relatively low response rate may limit the strength of our data. The possibility of non-responder bias is mitigated by the demonstration that the responder group is largely representative of the target population. Responders to our survey were representative of the Queensland rural anaesthetists in terms of gender and age. They were somewhat representative of practice location, with RRMA 6 being under-represented. The group was less reflective of practitioner type with hospital based practitioners under-represented. This statistically significant difference introduces the potential for non-responder bias. The responder data for this variable may be skewed, however, due to the structure of the survey tool. Of the survey responders, 17% selected the option 'other' which does not appear on the HWQ database.
The HWQ report that rural GPs are a widely surveyed group. This is likely to negatively impact our response rate. A high response rate does not preclude non-responder bias, hence survey results with both high and low response rates need to be interpreted carefully15. Certain surveying techniques have been proven to improve response rate16. Such techniques could be used in future data collection, however others infringe on respondent confidentiality. Within the confines of available information, our data remains important. It indicates an urgent need for reviewing available equipment for difficult airway management in rural centers.
Discrepancies in the data suggest poor awareness of local resources - respondents from the same institution reported the availability of different equipment. This may reflect unfamiliarity with equipment that is used infrequently and is an important finding. The low reported availability of an end-tidal CO2 detector may be attributed to an alternative location (emergency department or anaesthetic monitor).
The ASA makes recommendations regarding DAE for operating theatre complexes. Rural anaesthetists manage airways in a unique environment and anaesthesia may comprise a small part of their overall practice. The applicability of the ASA guidelines to small, remote operating theatres is questionable. Indeed the ASA list addendum states it should be 'customized to meet the specific needs, preferences, and skills of the practitioner and the healthcare facility'8.
Recently, an initiative to standardise equipment in rural and remote hospital emergency departments has commenced in the Southern Area of Queensland Health (Dr P Thomas, pers. comm., 19 February 2008). Our findings support a similar approach to the provision of DAE for rural anaesthetists. Standardisation of medical practice and equipment is a well accepted principle in improving patient safety17. Rural doctor turnover is well documented18 and may contribute to unfamiliarity with difficult airway management devices.
Conclusions
Further study is required to strengthen the validity of the data. However, based on our current analysis we suggest a standardised collection of user-friendly difficult airway equipment for rural anaesthetists. Expert use of this equipment could be supported by more widely available airway workshops. Simple equipment should be universally available. Provision of fibreoptic bronchoscopes and retrograde intubation kits should be reviewed carefully due to the high cost and difficulty in maintaining skills. Standardising equipment would recognise the specialised environment of rural anaesthetists and has the potential to improve patient safety. Information pertaining to critical incidents in rural anaesthesia and the relationship to available equipment remains an area for future research.
Acknowledgements
The authors thank Health Workforce Queensland, especially Ms Sarah Constantine, for their assistance. Also thanked are Dr Peter Thomas for his advice and Ms Heather Reynolds (Research Assistant) for her assistance in preparing this manuscript. Conflict of interest declaration: Dr Keith Greenland and Dr Victoria Eley are casual employees of Medical Education Solutions (MES) as difficult airway workshop facilitators. Health Workforce Queensland subcontract workshops to MES on a regular basis.
References
1. Rosenblatt WH, Wagner PJ, Ovassapian A, Kain ZN. Practice patterns in managing the difficult airway by anesthesiologists in the United States. Anesthesia and Analgesia 1998; 87: 153-157.
2. Jenkins K, Wong DT, Correa R. Management choices for the difficult airway by anesthesiologists in Canada. Canadian Journal of Anaesthesia 2002; 49: 850-856.
3. Baker PA, Hounsell GL, Futter ME, Anderson ME. Airway management equipment in a metropolitan region: an audit. Anaesthesia and Intensive Care 2007; 35: 563-569.
4. Rochford M, Skippen B, Duffy M. Difficult airway equipment in Australian adult emergency departments. Emergency Medicine Australasia 2008; 20: 184-185.
5. Smith JD, Margolis SA, Ayton J, Ross V, Chalmers E, Giddings P et al. Defining remote medical practice: a consensus viewpoint of medical practitioners working and teaching in remote practice. Medical Journal of Australia 2008; 188: 159-161.
6. Health Workforce Queensland. Health Workforce Queensland homepage. (Online) no date. Available: http://www.healthworkforce.com.au/ (Accessed 11 March 2008).
7. Australian Rural and Remote Workforce Agencies Group. ARRWAG Minimum Data Set Report - 30 November 2002. Appendix 2: Rural, Remote and Metropolitan Area Classification (RRMA) and Accessibility/Remoteness Index of Australia (ARIA). Canberra, ACT: ARRWAG, 2003.
8. American Society of Anaesthesiologists Task Force on Difficult Airway Management. Practical guidelines for management of the difficult airway. Anesthesiology 2003; 98: 1269-1277.
9. Lenth RV. Java applets for power and sample size. (Online) 2006. Available: http://www.stat.uiowa.edu/~rlenth/Power (Accessed 26 August 2008).
10. Hossein A. Measuring dependency of two variables from categorized data. (Online) 2008. Available: http://home.ubalt.edu/ntsbarsh/Business-stat/otherapplets/Catego.htm (Accessed 26 August 2008).
11. Choyce A, Avidan MS, Patel C, Harvey A, Timberlake C, McNeilis N et al. Comparison of laryngeal mask and intubating laryngeal mask insertion by the naïve intubator. British Journal of Anaesthesia 2000; 84: 103-105.
12. Chisholm DG, Calder I. Experience with the McCoy laryngoscope in difficult laryngoscopy. Anaesthesia 1997; 52: 906-908.
13. The International Liaison Committee on Resuscitation. The International Liaison Committee on Resuscitation (ILCOR) Consensus on Science With Treatment Recommendations for Pediatric and Neonatal Patients: Neonatal Resuscitation. Pediatrics 2006; 117: e978-e988.
14. Mason RA. Learning fiberoptic intubation: fundamental problems Anaesthesia 1992; 47: 729-731. (Editorial)
15. Barclay S, Todd C, Finlay I, Grande G, Wyatt P. Not another questionnaire! Maximizing the response rate, predicting non-response and assessing non-response bias in postal questionnaire studies of GPs. Family Practice 2002; 19: 105-111.
16. Edwards P, Roberts I, Clarke M, DiGuiseppi C, Pratap S, Wentz R et al. Increasing response rates to postal questionnaires: systematic review. BMJ 2002; 324: 1183.
17. Walton M. Australian Council for Safety and Quality in Health Care National Patient Safety Education Framework July 2005. Table 4.2 Working Safely: Understanding Human Factors. Canberra, ACT: Australian Council for Safety and Quality in Health Care, 2005; 111.
18. Health Workforce Queensland. Medical Practice in rural and remote Queensland: Minimum Data Set (MDS) Report as at 30th November 2007. Brisbane, QLD: HWQ, 2008.