Introduction
Skin cancer, both of the melanoma and non-melanoma skin cancer (NMSC) types are now the most common types of cancer in white populations across the globe1. In 2001, NMSC was both the most common cancer in Australia and the most expensive to treat2. Queensland, Australia, has the highest incidence of melanoma in the world3. Although the rate in younger Queenslanders is stabilising due to extensive health promotion programs, melanoma incidence in older people continues to rise rapidly across both metropolitan and rural locations4. As the key risk factor for melanoma and NMSC is ultraviolet sun exposure, those living and working in remote parts of Queensland, where outdoor work and leisure activities are common, are at increased risk compared with their metropolitan counterparts1.
Traditionally skin cancers in Australia of both the melanoma and NMSC types were managed by primary care doctors in general practice, supported by specialist services where appropriate5. With the dramatic rise in both the incidence and public awareness of skin cancer, there has been a concomitant rise in the development within the primary care health sector of dedicated skin cancer clinics. This is reflected in the rising proportion of all cause skin cancers managed by GPs who excise the majority of skin cancers6.
Remote medical practice is increasingly considered to have a different scope of practice and logistical structure from rural or metropolitan heath care services7. Apart from the lower number of practitioners per capita and issues of distance and isolation, remote primary care medical practice often requires novel funding arrangements to ensure viability. This requires consideration of population density below financial viability for generalist medical staff working full time in the community.
Health care services to the remote parts of the state of Queensland, Australia are primarily provided by Queensland Health, a state government agency and the Royal Flying Doctor Service of Australia (RFDS) Queensland Section, a not for profit non-government organisation. The RFDS has been providing healthcare services including aeromedical retrieval, telemedicine, telepharmacy and face-to-face primary care to people living in remote Queensland for more than 80 years. Over the last decade, there has been coordinated role delineation within face-to-face primary care service delivery across sites between these two organisations. In most instances, QH provides the resident nursing and ancillary staff and their appropriately equipped physical infrastructure, although in some locations the buildings are provided by local government. The RFDS provides a range of visiting health care staff including medical, nursing, mental health and allied health professionals. The primary care doctors in the communities considered in this study are RFDS staff members who visit each community on a regular, scheduled fly-in/fly-out basis for face-to-face clinics. Further particulars about the services provided by the RFDS are detailed elsewhere8,9.
The RFDS primary care medical services to remote locations are conducted in a traditional Australian general practice structure: a mixture of booked and walk-in patients present with a myriad of unselected problems to the doctor working in an office-based practice environment. All clinical services and pathology are provided free of charge to the patient, although in most locations regular and some acute medications must be paid for by the patient. The RFDS medical services have always included provision for the screening, diagnosis and management of skin cancers as this is an intrinsic component of Australian general practice10. However, in light of the well documented shortage of medical staff in remote areas, the amount of time available per patient for skin cancer management has to be balanced against other competing medical problems.
In recent years RFDS medical staff and management considered how best to increase service levels for skin cancer considering the limitations to medical staff time while at face-to-face clinics, the known higher rate of skin cancers in remote areas, increasing recognition of the benefits of prioritising screening for skin cancer, and the development in metropolitan areas of dedicated primary care skin cancer services. Key considerations were ensuring additional medical staff time was focussed on skin cancer care and that service delivery costs were minimised. The skin cancer clinic model chosen by RFDS was the addition of a second doctor with special expertise in skin cancer care to accompany the primary care doctor on regular scheduled visits where face-to-face primary care clinics were conducted. The key benefit envisaged from the addition of the skin cancer clinic was that the skin cancer care doctor could focus their entire attention on this area and direct any other intercurrent issues to the regular primary care doctor who was present in the adjacent office. The service would also allow for staff to develop their special interest in skin cancer work and consequently further develop skills in this area. Another important benefit of this model was that additional costs were essentially limited to the salary of the additional doctor and costs generated through treatment (eg equipment for skin excisions, histology, and referral where necessary). This was achieved through the additional doctor utilising existing air transport (whose costs were per aircraft, not per seat) and nursing or administrative staff already present in the clinics for the primary care clinic.
The aim of this study was to ascertain whether the RFDS skin cancer clinic could improve the skin cancer health outcomes for the target population while providing care at a level consistent with that documented for metropolitan skin cancer clinics.
Methods
The study was a retrospective longitudinal report. The intervention period was from 1 April 2006 to 30 June 2008, with the historical control period from 1 April 2001 to 31 March 2006.
Data sources
All data used in this study were obtained in a de-identified format from the RFDS databases and internal audit data that are regularly collected for internal and government reporting. Therefore there were no specific ethical requirements beyond institutional approval.
Population
The population under study was adult, non-Indigenous residents living and working in six distinct communities within one remote region in outback Queensland, Australia. The six communities all have employment and leisure options predominantly in outdoor activities with consequently significant long-term sun exposure. The 2006 census identified 1004 non-Indigenous adults aged over 18 years living in the region under study11. The RFDS medical staff provided a one day face-to-face primary care clinic on a fly-in/fly-out basis at each of the six study locations every 1 to 2 weeks. Each clinic provided approximately 6 hours of clinical time for the doctor to see the patients. There were no other doctors providing scheduled medical care to these communities.
Program
The RFDS skin clinic was supplied with standard equipment and a dermatoscope. A Siascope (Astron Clinica Pty Limited; Brisbane, QLD, Australia) which performed spectrophotometric intra-cutaneous analysis was donated to (rather than requested for) the RFDS clinic, and played a minor, peripheral role as appropriate for this form of technology in this context12.
The medical staff attending the RFDS primary care skin cancer clinic was shared over the study time between 6 different people. Ideally one or two staff would provide the entire service to ensure continuity of care but the realities of salaried staff taking study, sick or vacation leave, plus the natural cycle of staff turnover made this impossible. Nevertheless each staff member attending the skin cancer clinic had a special expertise in the service and received training in use of the Siascope.
The local resources regularly utilised in these six isolated communities were harnessed to advertise the service, including public noticeboards, community newspapers and word of mouth. The population were advised that the clinic would provide a diagnostic and treatment service for skin cancer, including comprehensive checking of an individual's skin for the presence of skin cancer.
Definitions
There are a number of different ways that outcomes are measured in relation to primary care skin cancer services. Recent Australian studies have developed three key indicators that have been used to objectively assess the quality of the service in standard general practice settings as well as dedicated primary care skin cancer clinics13,14. The consultation to biopsy ratio (CBR) equals the total number of consultations divided by total number of biopsies. Biopsy to treatment ratio (BTR) equals the total number of biopsies divided by total number of non-melanoma skin cancers (treated either surgically or non-surgically). Number needed to treat (NNT) equals the number of benign lesions (pigmented or non-pigmented) excised per melanoma, defined as number of benign lesions excised plus number of melanomas excised divided by number of melanomas excised.
Analysis methodology
Simple frequency analysis was performed using the Statistical Package for Social Sciences v 16 (SPSS Inc; Chicago, Il, USA). Categorical data were analysed using χ2 analysis. Continuous variables were analysed by analysis of variance. Statistical significance was defined as p<0.05.
Institutional review board approval
This study of de-identified data was approved by the Human Research Ethics Committees of both the University of Queensland and James Cook University.
Results
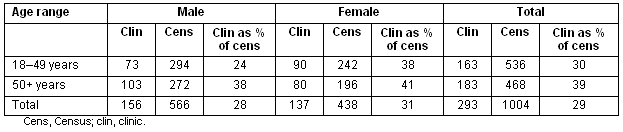
During the study period a total of 316 people were seen at the RFDS primary care skin cancer clinic (29% of the total non-Indigenous population) with 39% of those aged over 50 years seen. The male : female ratio was 1:0.9 and the average age was 48.5 +/- 16.7 years. The demographics of the population who attended this service clinic are detailed (Table 1).
Table 1: Age profile of the skin clinic population; source: 2006 census data for non-Indigenous adults11
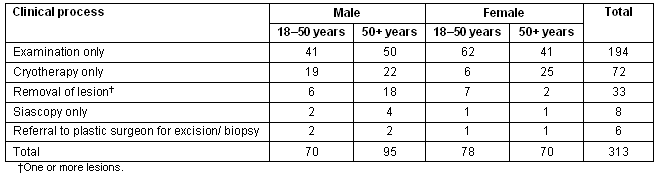
There was an average of 1.1 consultations per person (343 consultations in total), with a procedure performed in approximately one-third of consultations. Details of clinical processes are listed (Table 2). The demographic most likely to have a lesion removed were over 50 year-old males (p<0.0001).
Table 2: Clinical processes at the skin clinic
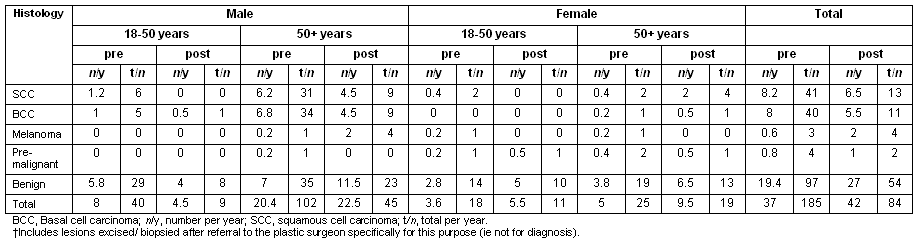
The histological findings by rate per year and absolute numbers of excised lesions are detailed (Table 3). This includes those lesions excised by the plastic surgeon after referral from the RFDS primary care skin clinic doctor who felt that the technical requirements of the excision were beyond the scope of the RFDS service. The rate of skin cancer detection was 15/1000 adults/year. The number of lesions removed/year increased from 37 to 42 after the intervention, with no statistically significant change in the percentage of excised lesions that were malignant (44%). The average age at removal of benign lesions was 52.1 +/- 16 years was statistically significantly younger than for malignant/pre-malignant lesions at 59.3 +/- 11.1 years (t = -4.333, p<0.0001). For over 50 year-old males, there was a statistically significant increase in the proportion of excised lesions that were melanomas (χ2 = 6.015; p = 0.013). This corresponded to a four-fold rise in melanoma detection from 0.2 /1000 people/year pre-intervention (a total of three in the 5 years before the clinic) to 2 /1000 people/year post-intervention (four in the 2 years of the skin cancer clinic's operation). There were no other statistically significant findings pre- and post-intervention across age and sex demographics.
Table 3: Histology results, pre- versus post-intervention
Discussion
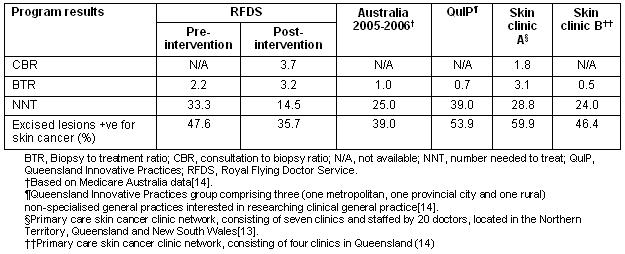
A comparison of the skin clinics' effectiveness compared with documented results from other Australian non-specialist skin cancer services is detailed (Table 4). There was a low number needed to treat for melanoma which is consistent with high diagnostic accuracy. This is also supported by a relatively high consultation to biopsy ratio. The biopsy treatment ratio and percentage of lesions that were malignant were similar to those seen in other Australian settings, suggesting that NMSC management was of a similar standard to those settings. In light of the trend for doctors working in metropolitan skin cancer clinics being required to have formal certification in skin cancer care, this is very reassuring. Although RFDS medical staff who work within the skin cancer clinic have a specific interest in this area, they are also clinically active in a variety of other clinical areas, including procedural areas such as aeromedical retrieval, and consequently have a considerable continuing medical education (CME) burden. Due to the difficulties experienced in sourcing all medical staff for remote Australia, the imposition of a formal requirement for specific training, certification and CME in skin cancer care would make it even more difficult to source medical staff for this clinic. A second benefit of the RFDS results being similar to metropolitan skin cancer clinics is that the patients who are the consumers of this clinical product can be reassured that their care is not being compromised by their geographical location.
Table 4: Comparison with published data on Australian non-specialist dermatology services
This study suggests an improved detection rate for melanoma although clinical relevance is compromised by the low numbers of patients and limited power of the study. Nevertheless, the suggestion of improved melanoma detection rates if confirmed by ongoing analysis of clinic results, would be of considerable import as people in remote areas have a higher rate of melanoma yet poorer health outcomes for melanoma15.
This study found that older males had the highest rate of melanoma, consistent with other studies16,17. This is not entirely surprising because the environment in which this study was conducted consists of outdoor work and leisure activities where consequent high sun exposure is the norm. Traditionally men would have been exposed to the sun for longer periods than women, and older males would have had significant ultraviolet exposure before the advent of modern sun protection advice.
The RFDS skin cancer clinic appeared to result in an increase in the detection rate of melanoma, a finding that will need to be confirmed by larger studies. However, it may be related to the increase in attendance by older males to this new clinical service. All new services undergo an accelerated period of interest when they begin and this may have accounted for a significant number of people coming to the skin clinic who were not seen previously. However, the service was provided over more than 2 years which would suggest this cause would have been mitigated. The other potential attraction to people who did not regularly attend health services was that this was advertised to the community as a dedicated skin cancer clinic. The advertising and positioning of the service may have duplicated the phenomenon that appears to make metropolitan dedicated primary care skin cancer clinics attractive to a segment of the population who may be otherwise reluctant to attend health services. This may be particularly relevant to older males who are known to be less likely to present for health care18.
Another possible reason for the apparent improved detection rate of melanoma is a change in the clinical acumen of the medical staff. This is consistent with the observed fall in the number needed to treat for melanoma diagnosis. This is low when compared with other contemporary Australian settings, and is also consistent with the high consultation to biopsy ratio, suggesting the medical staff felt confident in their clinical diagnostic acumen. These findings may be due to a change in medical staff skill, increased time per patient in the context of a skin cancer clinic when compared with a general clinic, or the addition of the diagnostic technology provided by the Siascope. The higher diagnostic acumen was not seen in NMSC where the biopsy to treatment ratio and the percentage of lesions that were benign were similar to other contemporary Australian settings19,20. These findings suggest that there was either differential enhancement of melanoma diagnosis or that the Siascope provided a distinct diagnostic input to the clinical process. Further studies would be required to define the relative importance of each of these distinct factors.
Limitations
A key limitation of this study was the use of historical controls. However, the geographical, demographic and service delivery nature of remote Queensland resulted in the absence of an appropriate formal control location. An important second issue was being unable to distinguish between the impact of advertising the new service and the consequent increase in interest and awareness about skin cancer and the actual delivery of skin cancer services within the clinic. However, advertising alone in the absence of an expansion of services would have simply increased pressure on the already busy primary care medical service. Consequently, there would have been little scope for expanding services to meet increased demand (eg increasing clinical skin cancer screening). Additionally, the timeframe over which the study was conducted suggested the ongoing success of the program, rather than an increase in visitation at onset, that would be expected with advertising a new service. A third issue is whether simply increasing resources would have resulted in an improvement. It would appear self-evident that this was so until one considers the rather unusual logistics and geography of remote parts of Queensland. The number of hours of face-to-face medical services is determined as much by aircraft logistics (flight times, aircraft loads) and prevailing weather (affecting both flight movements and ground transport for those living out of town to reach the clinic across roads subject to flooding etc), as by the availability of medical staff to provide services. The model reported in this article demonstrated a mechanism to enhance skin cancer services which minimised additional costs and the dilution of a new additional service through servicing other intercurrent clinical problems.
Conclusion
In conclusion, the RFDS skin cancer clinic outcomes were not dissimilar to outcomes seen in metropolitan skin cancer clinics, with a suggestion that clinical outcomes were enhanced. Further studies would assist in the further development of models for skin cancer clinics in remote areas.
Acknowledgements
The authors wish to acknowledge the financial support of the PHCRED program in conducting this study, and the support provided by the Royal Flying Doctor Service, Queensland Section. They also acknowledge the assistance of Dr Valmae Ypinazar in critiquing the manuscript. Astron Clinica provided one SIAscope at no cost to the Royal Flying Doctor Service Qld Section in 2006. Astron Clinica provided training to the medical staff in the use of this machine, specifically image and data collection. The Royal Flying Doctor Service Qld Section and the authors have not received any other support from Astron Clinica who have not had any influence over the clinical decision-making process in the RFDS primary skin care cancer clinic, analysis of the outcomes and results from the clinic or development of this manuscript.
References
1. Leiter U, Garbe C. Epidemiology of melanoma and nonmelanoma skin cancer--the role of sunlight. Advances in Experimental Medicine and Biology 2008; 624: 89-103.
2. Australian Institute of Health and Welfare. Health system expenditures on cancer and other neoplasms in Australia, 2000-01. Health and Welfare Expenditure series no. 22; AIHW cat no HWE 29. Canberra, ACT: AIHW, 2005.
3. Coory M, Baade P, Aitken J, Smithers M, McLeod GR, Ring I. Trends for in situ and invasive melanoma in Queensland, Australia, 1982-2002. Cancer Causes and Control 2006; 17(1): 21-27.
4. Whiteman DC, Bray CA, Siskind V, Green AC, Hole DJ, Mackie RM. Changes in the incidence of cutaneous melanoma in the west of Scotland and Queensland, Australia: hope for health promotion? European Journal of Cancer Prevention 2008; 17(3): 243-250.
5. Commens CA. Skin cancer: changing paradigms of practice and medical education. Medical Journal of Australia 2007; 187(4): 207-208.
6. Askew DA, Wilkinson D, Schluter PJ, Eckert K. Skin cancer surgery in Australia 2001-2005: the changing role of the general practitioner. Medical Journal of Australia 2007; 187(4): 210-214.
7. Smith JD, Margolis SA, Ayton J, Ross V, Chalmers E, Giddings P et al. Defining remote medical practice. A consensus viewpoint of medical practitioners working and teaching in remote practice. Medical Journal of Australia 2008; 188(3): 1591-61.
8. Margolis SA, Ypinazar VA, Muller R. The impact of supply reduction through alcohol management plans on serious injury in remote indigenous communities in remote Australia: a ten-year analysis using data from the Royal Flying Doctor Service. Alcohol and Alcoholism 2008; 43(1): 104-110.
9. Margolis SA, Ypinazar VA. Tele-pharmacy in remote medical practice: the Royal Flying Doctor Service Medical Chest Program. Rural Remote Health 8:937. (Online) 2008. Available: www.rrh.org.au (Accessed 18 February 2009).
10. Britt H, Miller GC, Charles J, Pan Y, Valenti L, Henderson J et al. General practice activity in Australia 2005-06. General practice series no 19; AIHW cat no GEP 19. Canberra, ACT: Australian Institute of Health and Welfare, 2007.
11. Australian Bureau of Statistics. 2006 Census data by comparison. (Online) 2008. Available: http://www.censusdata.abs.gov.au/ABSNavigation/prenav/PopularAreas?&collection=Census&period=2006&&navmapdisplayed=true&javascript=true&textversion=false (Accessed 6 May 2008).
12. Astron Clinica. Skin cancer screening. (Online) no date. Available: http://www.siascope.com (Accessed 27 June 2008).
13. Wilkinson D, Askew DA, Dixon A. Skin cancer clinics in Australia: workload profile and performance indicators from an analysis of billing data. Medical Journal of Australia 2006; 184(4): 162-164.
14. Byrnes P, Ackermann E, Williams ID, Mitchell GK, Askew D. Management of skin cancer in Australia - a comparison of general practice and skin cancer clinics. Australian Family Physician 2007; 36(12): 1073-1075.
15. Coory M, Smithers M, Aitken J, Baade P, Ring I. Urban-rural differences in survival from cutaneous melanoma in Queensland. Australian and New Zealand Journal of Public Health 2006; 30(1): 71-74.
16. Goldberg MS, Doucette JT, Lim HW, Spencer J, Carucci JA, Rigel DS. Risk factors for presumptive melanoma in skin cancer screening: American Academy of Dermatology National Melanoma/Skin Cancer Screening Program experience 2001-2005. Journal of American Academic Dermatology 2007; 57(1): 60-66.
17. Marks R. Epidemiology of melanoma. Clinical and Experimental Dermatology 2000; 25(6): 459-463.
18. McVittie C, Willock J. "You can't fight windmills": how older men do health, ill health, and masculinities. Quality in Health Research 2006; 16(6): 788-801.
19. Green AR, Elgart GW, Ma F, Federman DG, Kirsner RS. Documenting dermatology practice: ratio of cutaneous tumors biopsied that are malignant. Dermatological Surgery 2004; 30(9): 1208-1209.
20. Chren MM, Sahay AP, Sands LP, Maddock L, Lindquist K, Bertenthal D et al. Variation in care for nonmelanoma skin cancer in a private practice and a veterans affairs clinic. Medical Care 2004; 42(10): 1019-1026.
Abstract
Introduction:
The geography and logistics of living in remote Australia provide unique challenges in providing dedicated primary healthcare services to tackle the rising incidence of skin cancer. The aim of this study was to ascertain whether the Royal Flying Doctor Service (RFDS) skin cancer clinic could improve skin cancer health outcomes for the target population while providing care at a level consistent with that documented for metropolitan skin cancer clinics.Methods: This retrospective longitudinal report compared historical controls with a dedicated fly-in/fly-out primary care skin cancer outreach clinic provided by the RFDS. The clinic was run concurrently with the regular primary care medical service; the entire focus of this additional service was on skin cancer diagnosis and management. This model was used to minimise the additional costs of providing the service.
Results: During the study period a total of 316 people were seen at this skin cancer clinic (29% of the total non-Indigenous population) with 39% of those aged over 50 years seen. There was an average of 1.1 consultations per person (343 consultations in total), with a procedure performed in approximately one-third of consultations. The demographic most likely to have a lesion removed were over 50 year-old males (p<0.0001). The rate of skin cancer detection was 15/1000 adults/year. The number of lesions removed per year increased from 37 to 42 after the intervention, with no statistically significant change in the percentage of excised lesions that were malignant (44%). For over 50 year-old males there was a statistically significant increase in the proportion of excised lesions that were melanomas (χ2 = 6.015; p = 0.013). This corresponded to a four-fold rise in melanoma detection from 0.2/1000 people/year pre-intervention to 2/1000 people/year post-intervention. A comparison of the skin clinic's effectiveness with documented results from other Australian non-specialist skin cancer services demonstrated a low number needed to treat for melanoma which is consistent with high diagnostic accuracy. This is also supported by a relatively high consultation to biopsy ratio. The biopsy treatment ratio and percentage of lesions that were malignant were similar to those seen in other Australian settings.
Conclusion: The RFDS skin cancer clinic outcomes were not dissimilar to those seen in metropolitan skin cancer clinics. The small population and consequently low statistical power mitigated against certainty in concluding that clinical outcomes were enhanced. Further studies would assist in the future development of models for skin cancer clinics in remote areas.
Key words: primary care, remote, skin cancer, skin cancer clinic.

