Introduction
Allied health professionals comprise a substantial proportion of the health workforce and make a significant contribution to the health and wellbeing of the Australian population. According to the Australian Institute of Health and Welfare (AIHW)1 the allied health professions form approximately 18% of Australia's health workforce, while medical practitioners comprise approximately 12% and nurses 63%.
Despite the acknowledged importance of allied health services, there is remarkably little information detailing the existing allied health workforce, particularly in rural areas. Available studies are dated, based on a small sample size, geographically limited or report important inconsistencies2. For example, the conclusions of Victorian3 and Tasmanian4 studies about the value of student placements for rural recruitment are not in agreement. Peer reviewed publications exploring Australian rural allied health workforce issues are also sparse5,6. The need for data collection regarding the current allied health workforce has been repeatedly mentioned in the literature2,7,8.
However, workforce data are robust for nurses and medical practitioners, including many peer-reviewed publications and major governmental reports9-10. The AIHW 2006 report provides a small amount of detail about the national allied health workforce based on 2001 Australian Bureau of Statistics census data1. More recent reports have concluded that there is a lack of data about the Australian allied health workforce, particularly for rural and remote areas11.
The Rural Allied Health Workforce Study (RAHWS) is ongoing in Tasmania and New South Wales (NSW). This report describes the development of a method to obtain workforce information using a cross-sectional survey instrument of high validity which has the capacity to provide a large scale but detailed profile of the allied health workforce in regional, rural and remote Australia. The data produced may inform future public health and primary care policy development, as well as generating a deeper understanding about the recruitment and retention of rural allied health professionals. The work is the product of a collaboration of three Australian Government funded University Departments of Rural Health (UDRHs)12.
Background and rationale
Allied health professionals provide a broad range of diagnostic and therapeutic services in both the public and private healthcare systems. For example in aged care, physiotherapists, occupational therapists and social workers contribute to both speedy discharge from hospital and the prevention of readmission. Podiatrists, exercise physiologists and dietitians are key team members in managing chronic conditions such as diabetes. Audiologists and speech therapists provide screening of and therapy for children with developmental disabilities. Medical laboratory scientists and radiographers provide essential diagnostic services, and psychologists help to address the rising prevalence of mental illness. Allied health professionals often work in multidisciplinary models of care, with an emphasis on preventive services and are well placed to provide interprofessional health education and health promotion services.
Because of the diversity of roles, defining 'allied health' is difficult. In 2007, Lowe, Adams and O'Kane examined the manner in which different jurisdictions, organisations, purchasers of allied health services and professional groups used the term 'allied health'13. The following criteria were derived from their analysis:
- are tertiary qualified, having completed an accredited entry level qualification permitting them to obtain either state or territory registration, a license or accreditation to practice, and/or to join the relevant professional body
- apply their skills and knowledge to restore and maintain optimal physical, sensory, psychological, cognitive and social function
- use clinical reasoning skills in working directly with patients to restore and optimise function on an individual basis
- are 'allied' or aligned to each other and other members of the health professional workforce, working together as part of a multidisciplinary team
- are 'allied' or aligned with health consumers, the consumer's family and other carers, and with the community.
It is well known that there is a national shortage of allied health professionals and that this problem is worse in rural areas14. An analysis of 2001 ABS census data undertaken by Services for Australian Rural and Remote Allied Health (SARRAH) in 2004 demonstrated that people living in outer regional centres have access to only about half as many allied health professionals as people living in metropolitan centres. This figure decreases to less than a quarter in some remote locations(Fig1). The per capita reduction of allied health services associated with increasing rurality has implications for the healthcare needs of rural and regional residents. In particular, the ageing population could stretch the already sparse allied health workforce beyond the ability to cope with the expected increased demand for services.
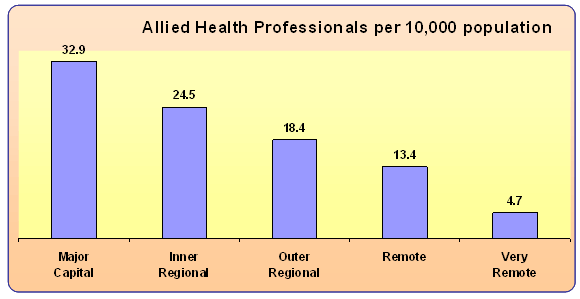
Figure 1: The allied health workforce by degree of rurality and remoteness.
In a climate of health workforce shortages, the Productivity Commission has recently suggested service innovations, such as the use of supervised therapy assistants and extending the scope of health professional practice on a competency basis15. The need for innovative service delivery models is particularly acute in rural areas where practitioners' ingenuity is frequently tested in meeting the healthcare needs of the population.
In 2006, the Australian Health Workforce Official Committee (AHWOC) developed a checklist to assess the impact of new initiatives on the health workforce16. The Committee advises that new projects must take into account future workforce requirements, the distribution and work contexts of existing workforce, training arrangements and workforce roles and scope of practice. The absence of data profiling the existing allied health workforce renders such analysis impossible.
The questionnaire
The RAHWS survey instrument (Appendix I) is the result of a comprehensive consultation with clinicians in the public and private healthcare system, allied health academics from three Australian universities, and public healthcare administrators. A pilot survey was performed in the Hunter-New England region of northern NSW in 20052. The questionnaire was well accepted by allied health professionals in that region and opportunities for a larger scale study soon eventuated.
The RAHWS questionnaire was expanded from the pilot version to include further questions in three broad categories: background information; current employment; and education and professional development. The added questions target issues related to recruitment and retention and were constructed with reference to the literature, including that of the nursing and medical workforce9,10,17-19.
The face validity of the revised RAHWS questionnaire was evaluated by allied health clinicians who volunteered to complete it and provide feedback. Generally, they took approximately 15 min to complete the questionnaire and reported that the questions were relevant, requesting only relatively minor modifications. Concurrent validity was assessed by comparing the content of the RAHWS survey items with that of the 1999 SARRAH survey20. It matched 89% of the topics included in the SARRAH survey. Further comparison found 38 items not included in the SARRAH data that are included in the RAHWS questionnaire.
Most of the questionnaire's 74 questions can be answered by selecting from a menu of 'tick box' choices, making it possible to develop the instrument for online delivery, with immediate entry of responses into a database. The convenience and cost advantage of the online response option is considerable. However, allied health professionals are both widely dispersed and difficult to locate and so the option remains of distributing the questionnaire in hardcopy. To achieve maximum penetration it is recommended that both online and hardcopy options are used, depending on the means of distribution. Ideally, the survey will be mailed or distributed electronically through registration boards and licensing authorities. However, not all allied health professions are subject to either registration or licensing. Other distribution pathways include professional associations, employers and by word of mouth. Private practitioners may be identified by searching telephone and business directories.
Conclusions
Accurate and current information about the rural health workforce is essential to future policy development, and yet there is remarkably little known about allied health professionals in regional, rural and remote Australia. Developing a meaningful national data-set requires a uniform sampling process across the allied health population, in spite of the challenges involved. The RAHWS survey instrument has been specifically developed to meet the need for detailed, large-scale and uniform data collection. Good concurrent and face validity of this instrument have been demonstrated and its design allows for flexible methods of data collection, using either online or hard copy modes of delivery. The data collected can be easily analysed for a wide range of variables with cross-correlation of responses. The results can be used to answer a large number of research questions about recruitment and retention, professional education and service delivery.
The RAHWS survey has been performed in Tasmania and non-metropolitan parts of NSW. Other states have also expressed strong interest in using the same survey instrument and methodology. It is hoped that data collection will take place across the whole of Australia on a state-by-state basis over a sampling period of approximately 12 to 18 months. If this can be achieved it will create the largest repository of data about the allied health workforce ever available in this country.
References
1. Australian Institute of Health and Welfare. Australia's health 2006. AIHW catalogue no AUS 73. Canberra, ACT: AIHW, 2006. Available: http://www.aihw.gov.au/publications/index.cfm/title/10321 (Accessed 26 November 2008).
2. Smith T, Cooper R, Brown L, Hemmings R. A profile of the rural allied health workforce in northern New South Wales. Australian Journal of Rural Health 2008; 16: 156-163.
3. Belcher S, Kealey J, Jones J, Humphreys J. The VURHC rural allied health professionals recruitment and retention study. Melbourne, VIC: Victorian Universities Rural Health Consortium, 2005. Available: http://catalogue.nla.gov.au/Record/3410622/Holdings?&#details (Accessed 26 November 2008).
4. Department of Health and Human Services. Allied health professional workforce status report. Hobart, TAS: Department of Health and Human Services, 2003.
5. Collins K, Jones ML, McDonnell A, Read S, Jones R, Cameron A. Do new roles contribute to job satisfaction and retention of staff in nursing and professions allied to medicine? Journal of Nursing Management 2000; 8(1): 3-12.
6. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14(1): 14-19.
7. Australian Health Workforce Advisory Committee. The Australian allied health workforce - an overview of workforce planning issues. AHWAC report 2006-1. Sydney, NSW: Australian Health Workforce Advisory Committee, 2006. Available: http://www.nhwt.gov.au/publications.asp (Accessed 26 November 2008).
8. Services for Australian Rural and Remote Allied Health. 2006 National SARRAH conference recommendations. Canberra, ACT: SARRAH, 2006. Available: http://www.ruralhealth.org.au/conferences/sarrah2006/RecsProcess.htm (Accessed 26 November 2008).
9. Australian Institute of Health and Welfare. Medical labour force 2006. AIHW cat. no. HWL 42. Canberra: AIHW, 2008. Available: http://www.aihw.gov.au/publications/index.cfm/title/10620 (Accessed 26 November 2008).
10. Australian Institute of Health and Welfare. Nursing and midwifery labour force 2005. AIHW cat. no. HWL 40. Canberra, ACT: AIHW, 2008. Available: http://www.aihw.gov.au/publications/index.cfm/title/10475 (Accessed 26 November 2008).
11. Australian Government Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia. Canberra, ACT: DoHA, 2008. Available: http://www.aihw.gov.au/publications/index.cfm/title/10620 (Accessed 26 November 2008).
12. Humphreys JS, Lyle D, Wakerman J, Chalmers E, Wilkinson D, Walker J et al. Roles and activities of the Commonwealth Government University Departments of Rural Health. Australian Journal of Rural Health 2000; 8(2): 120-133.
13. Lowe S, Adams R, O'Kane A. A framework for the categorization of the Australian health professional workforce. Canberra, ACT: Services for Australian Rural and Remote Allied Health, 2007. Available: http://www.sarrah.org.au/site/index.cfm?display=65820 (Accessed 26 November 2008).
14. Services for Australian Rural and Remote Allied Health. National allied health workforce report. Canberra: SARRAH, 2004. Available: http://www.sarrah.org.au/site/index.cfm?display=65820 (Accessed 26 November 2008).
15. Productivity Commission. Australia's health workforce research report. Canberra, ACT: Productivity Commission, 2005. Available: http://www.pc.gov.au/projects/study/healthworkforce/docs/finalreport (Accessed 26 November 2008).
16. Australian Health Workforce Officials Committee. Health workforce impact checklist and guidelines: informing the decision making process. Sydney, NSW: Australian Health Workforce Officials Committee, 2006. Available: http://www.nhwt.gov.au/documents/Publications/2006/Health%20workforce%20impact%20checklist.pdf (Accessed 26 November 2008).
17. Stagnitti K, Schoo A, Reid C, Dunbar J. Access and attitude of rural allied health professionals to CPD and training. International Journal of Therapy and Rehabilitation 2005; 12(8): 355-362.
18. Stagnitti K, Schoo A, Dunbar J, Reid C. An exploration of issues of management and intention to stay: allied health professionals in South West Victoria, Australia. Journal of Allied Health 2006; 35(4): 226-232.
19. McCarthy G, Tyrrell MP, Lehane E. Intention to 'leave' or 'stay' in nursing. Journal of Nursing Management 2007; 15(3): 248-255.
20. Services for Australian Rural and Remote Allied Health (SARRAH). A study of allied health professionals in rural and remote Australia. Canberra, ACT: SARRAH, 2000. Available: http://www.sarrah.org.au/site/index.cfm?display=65820 (Accessed 26 November 2008).
______________________________
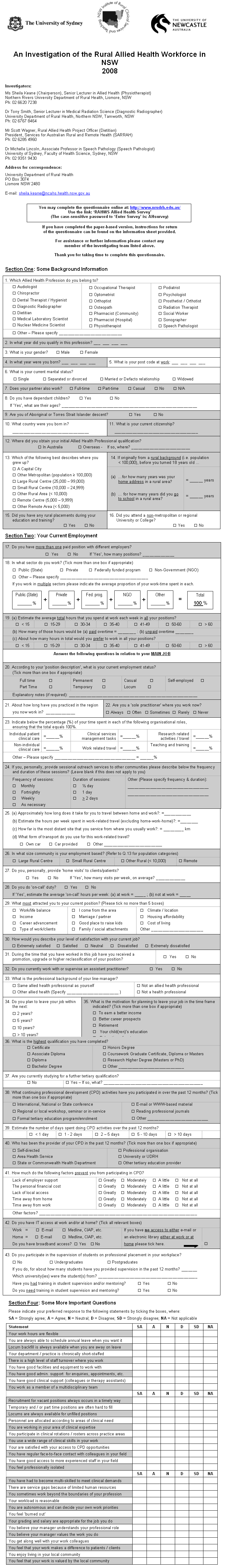
Appendix I: The Rural Allied Health Workforce Study survey instrument