The difficulties accessing health and medical services in rural Australia are well documented1,2. Road quality, high travel costs, inconvenience and family disruptions are cited as affecting access and utilisation of medical services3-8. In spite of these barriers and the presence of local hospitals with resident doctors and visiting specialists, many rural patients bypass local health services.
Studies of rural patient movement for hospital and health care suggest consumer preferences, perceptions of services, location of general practitioner (GP), service fees, adequacy of equipment, consulting with the same physician and the type of service required all influence service seeking behaviour9-13. The demographic and socioeconomic profiles of hospital and health care 'out shoppers' have also been described in the literature. Typically they are younger, more affluent, well educated and privately insured9,11,14.
Many rural hospitals in Western Australia (WA) are threatened by low patient volumes, loss of services and declining revenues. Health administrators and service providers need to understand the reasons for out migration if this trend is to be reversed. This study identifies the demographic and service characteristics of health consumer behaviour in rural WA, with an emphasis on specialist surgical services.
Method
Eight focus group discussions15 were held in four regional WA towns between May and June 2000. Towns had a combination of resident and visiting medical services related to population and proximity to the metropolitan area (Table 1).
Table 1: Characteristics of the four regional Western Australian towns where the focus groups were held
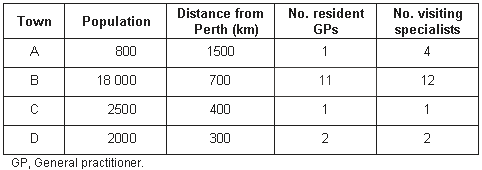
Town A is an isolated mining town, with an impressive number of visiting services. Town B on the state's southern coast has the largest population and number of resident medical services. The agricultural towns C and D are reliant on visiting services for anything other than basic care.
A standardised discussion guide was designed to identify factors affecting the migration of rural Western Australians from local health and medical services. Discussions encompassed local service quality, treatment preferences, visiting specialist service utilisation and characteristics of a quality service. Two groups were undertaken in each town, one male and one female. Groups were single sex to ensure the identification of male and female issues. Subjects were recruited from local government A-Z resident lists obtained from the WA Electoral Commission, current for 11 February 2000. Fifty names and addresses were randomly selected from each community to ensure a minimum group size of six participants. Recruitment occurred 2 weeks prior to scheduled focus groups and consisted of a short telephone interview. Individuals were recruited provided they had lived in the town for at least 2 years, they or an immediate family member had used a health service in WA during the last 2 years and they were the first or second person contacted in their age category (25-34 years; 35-49 years; 50-64 years; > 65 years).
On arrival, subjects completed a short data sheet providing basic demographic and background information. Sessions were facilitated by a researcher and audiotaped for transcription and analysis.
Results
Forty-eight rural residents, male : female ratio 1:1 and mean age 47 years (SD = 14) participated in the study. All age categories were well represented (25-34 years, n = 11; 35-49 years, n = 16; 50-64 years, n = 12; and > 65 years, n = 9) with an average attendance of six subjects per group. Subjects travelled a mean distance of 10.2 km to attend groups (Table 2).
Table 2: Demographic characteristics of subjects according to their town of residence
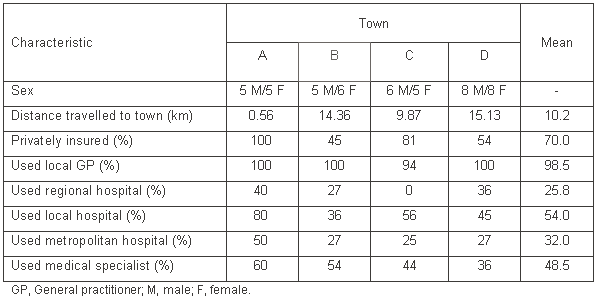
Perception of local services
Men and women demonstrated similar awareness levels of local health and medical services with the exception of gender specific services. Knowledge of visiting services was poor in comparison to resident services, and influenced by prior personal or family use.
Generally participants thought themselves 'lucky' compared with other rural communities in the availability of local services they rated as above average. In spite of this rating men and women agreed that local services were only adequate for basic care, noting consistently the lack of specialist and allied health services. Men and women commented on the lack of weekend cover for GPs and the need to 'wait until Monday' for treatment. The local hospital, whilst being important in terms of emergencies and as a major employer for the town, was perceived to lack specialist equipment and services.
Treatment preferences
Local health services, in particular the GPs, were preferred by all groups for basic care; colds and flu, renewal of prescriptions, childhood illnesses and 'minor' ailments. In cases of emergency, the local hospital in conjunction with the GP was the primary treatment option. Females were more likely than males to access visiting services. Participants voiced strong migration tendencies to regional or metropolitan centres for severe or major illnesses. Local health services were bypassed for GP referral, medical transfers, second opinions, anonymity and for services unavailable locally. Treatment seeking behaviour was also influenced by individual perceptions of the quality of local care and equipment regardless of severity. Interestingly, only one group (male) mentioned a preference for local services to save time and money.
Specialist service utilisation
A unanimous response to the question of individual specialist or specialist service choice, identified GP referral, specialist reputation, location (in terms of convenience to the patient and family support) and the cost of treatment as major factors affecting the decision of where to access care. Less dominant factors were prior history with a particular specialist, the availability of an appointment and severity of illness.
When asked to consider using a visiting specialist surgical service for a consultation, men and women differed in their responses. Although important to both, men rated knowledge of the visiting specialist's reputation and qualifications higher than women who were more concerned with the cost of accessing the service. The sample identified several advantages of visiting specialist services likely to increase utilisation (Table 3).
Table 3: Perceived advantages of using visiting specialist services
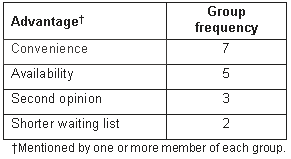
A preference for visiting services was indicated for non-urgent conditions provided the service was regular and connected to local services.
Existing illness and prior association with a specialist were positively associated with migration for specialist care as was the bad reputation of a visiting service. Over booking and a rushed approach to the patients negatively impacted on service utilisation. Some participants were concerned with the risks of procedures performed in the rural setting and whether appropriate follow up would be available. If a condition was urgent or serious, participants indicated they would bypass the visiting service to access care immediately.
Safety concerns were paramount in the decision to use a visiting specialist service for a surgical procedure in local hospitals. Diagnostic tests and day procedures were considered acceptable provided the procedure risk was the same as in larger centres. Participants indicated a willingness to undergo operations locally if standard safety, anaesthetic and sterilisation procedures were in place. Some reservations were expressed for elderly and high-risk individuals.
Quality service
Participants were asked to indicate which aspects of a health service or hospital most influenced their decision to use it, accessibility, quality or distance/cost. All three were considered important with quality exerting the greatest influence. The characteristics of a quality service defined by the sample were similar for men and women (Table 4).
Table 4: Quality service as characterised by participants
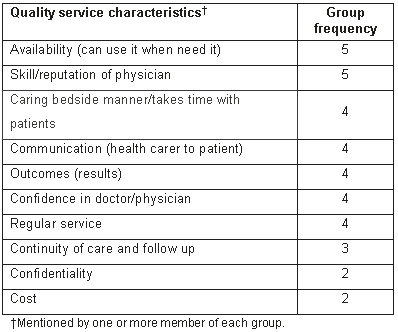
Discussion
Participants accepted the number and standard of health services available in their respective towns. The main criticisms were for greater access to specialist care and allied health services. Factors influencing the migration of the sample for health care were similar to other rural populations5,8,9,13. Local services were preferred for basic and emergency care whilst regional or metropolitan centers were favoured in the event of major or severe illness. Typically local services were bypassed to access 'better' care and equipment, services unavailable locally and obtain a second opinion. In this study, GP recommendation and referral were the major influence on service selection.
The sample embraced the concept of visiting specialist services. They indicated a willingness to use them provided they were informed of specialist's reputation, service outcomes and the service was integrated into the local health care setting and supported by their GP. The need for community awareness programs to be incorporated with visiting specialist services was evident by the participants' poor knowledge of visiting services in comparison to resident services.
Modern techniques and equipment allow a number of surgical and medical services to be safely performed in rural hospitals. Visiting specialist services increase the perception of quality care and viability of rural hospitals with increased patient throughput and revenues. The economic consequences of this are far reaching as rural hospitals generate many employment opportunities and attract other industry and services3,8.
The tendency for rural residents to bypass local services is not limited to health care, they have been migrating for retail, education and banking services for years. Unless mechanisms are put in place to encourage rural patients to 'shop' local, it is likely more and more will bypass local services for those in regional and metropolitan centres.
Conclusion
Service utilisation is determined by the need for a service, the ability to access the service, in terms of cost and distance, and the perception of the service itself. In order to understand the patterns of rural health consumers, it is necessary to know their attitudes towards local, regional and metropolitan health services. Community consultation was used in this study to determine rural resident perceptions and attitudes towards local health and visiting specialist services. It is hoped that the findings of this and follow up studies will impact on rural policy makers and the delivery of health and medical services in rural WA.
References
1. Humphreys JS. Super-clinics or a country practice? Contrasts in rural life and health service provision in northern NSW. In: DJ Walmsley (Ed.) Change and Adjustment in Northern NSW. Armidale: University of New England, 1990; 73-84.
2. Lonsdale RE, Holmes JH. Settlement systems in sparsely populated regions: the United States and Australia. New York: Pergamon Press, 1981.
3. Humphreys JS, Weinand HC. Health care preferences in a country town. Medical Journal of Australia 1991; 154: 733-737.
4. Walmsley DJ. The influence of distance on hospital usage in rural New South Wales. Australian Journal of Social Issues 1978; 13: 72-81.
5. Veitch PC, Sheehan MC, Holmes JH et al. Barriers to the use of urban medical services by rural and remote households. Australian Journal of Rural Health 1996; 4: 104-110.
6. Haynes RM, Bentham CG. Accessibility and the use of hospitals in rural areas. Area 1979; 11: 186-191.
7. Trott P, Blignault I. Cost evaluation of a telepsychiatry service in northern Queensland. Journal of Telemedicine and Telecare 1998; 4(S.1): 66-68.
8. Strasser RP, Harvey D, Burley M. The health service needs of small rural communities. Australian Journal of Rural Health 1994; 2: 7-13.
9. Borders TF, Rohrer JE, Hilsenrath PE et al. Why rural residents migrate for family physician care. Journal of Rural Health 2000; 16: 337-348.
10. Taylor SL. Outshopping: the battle between rural and urban medical services. Marketing Health Services 1997; 17: 42-44.
11. Finlayson SRG, Birkmeyer JD, Tosteson ANA et al. Patient preferences for location of care: implications for regionalization. Medical Care 1999; 37: 204-209.
12. Rayburn J. Outshopping for hospital obstetrical services. In: VA Richmond VA (Ed.) Annual meeting of the Southern Marketing Association. Southern Marketing Association, 1991; 438-442.
13. Andrus D, Kohout FJ. The effect of rural consumer satisfaction on outshopping for medical services. Marketing Ambulatory Care Services 1985; 20: 171-184.
14. Buczko W. Bypassing of local hospitals by rural medicare beneficiaries. Journal of Rural Health 1994; 10: 237-246.
15. Krurger RA. Focus groups: a practical guide for applied research, 2nd edn. San Diego, CA: Sage, 1994.
Published 22 August 2002; style modified 13 May 2003.
Abstract
Introduction and Objectives: The purpose of the study was to identify the demographic and health service characteristics impacting on rural residents' utilisation of health and visiting specialist services in Western Australia.
Method: Focus group discussions were held with an age-stratified, randomly selected group of forty-eight residents in four rural Western Australian towns between May and June 2000.
Results: Discussions revealed a preference to use local health services for basic care and to travel for the treatment of major or severe illnesses. The focus group participants supported visiting specialist services, indicating a willingness to use them for consultations, diagnostic and minor procedures. Utilisation of visiting services was conditional on the provision of information on specialist reputation, service outcomes, integration of the service into local facilities, and recommendation by the local general practitioner.
Conclusion: Numerous factors influence the service-seeking behaviour of rural patients. These factors need to be recognised and considered in the design and promotion of resident and visiting specialist services if the migration for health care is to be rationalised.
Key words: service-seeking behaviour, visiting specialist services, Western Australia.
You might also be interested in:
2006 - Medical students' assessments of skill development in rural primary care clinics
2001 - The impact of health system reform on remote health in Cambodia and the Philippines
