Introduction
Previous observations have suggested a high prevalence of diabetes in the study area (District 32) in Italy at 6.5%, and poor control of type 2 diabetes mellitus with a mean HbA1c level of 7.5% ± 1.1 SD, with 62% of the population above 7.0%1. Inadequate blood pressure control and suboptimal management in both diagnosis and treatment of hypertensive type 2 diabetic patients has been described in several European countries2. To date there have been no substantial studies on quality indicators in rural areas of Southern Italy.
Research question
The research question for the present study was: 'Is the recording of patient data and the achievement of quality indicator targets satisfactory in rural Italy, or is there potential to improve the quality of care of patients with type 2 diabetes and hypertension through a quality and outcome incentivisation scheme?'
Methods
A subject information sheet with simple information about the research was given to all the patients and doctors involved. An informed consent form was signed by subjects who agreed to be involved.
This observational study was conducted in a rural practice context (in District 32) in the Province of Caserta, Campania, Southern Italy. Data were collected from the electronic files of patients with type 2 diabetes from the records of seven family doctors (GPs) in February 2008. Ten patients with type 2 diabetes and hypertension were randomly selected by each GP.
The exclusion criteria were chosen to minimize confounding factors:
- Treatment with steroids or major surgery in the last 3 months.
- Presence of dementia or other inability to give written, informed consent.
- Treatment with insulin.
The inclusion criteria ensured that the data were from a single, public quality assured laboratory to avoid bias due to differing testing methods.
Main outcome measures
The main outcome measures were: HbA1c optimal target ≤7%; LDL cholesterol target ≤100 mg/dL (2.6 mmol/L); systolic blood pressure target ≤130 mmHg, and diastolic blood pressure ≤80 mmHg. Patient characteristics included in the analysis were age, sex, and educational level. Behaviour-related risk factors such as smoking and body mass index, and presence or absence of comorbidities were also recorded. The comorbidities sought were cerebrovascular disease (stroke and transient ischemic attack), coronary artery disease (angina pectoris and myocardial infarction or equivalent such as coronary angioplasty or surgical revascularisation), and asthma or chronic obstructive pulmonary disease. Also examined were other relevant quality markers included in the Quality and Outcomes Framework3 (QoF). The software Epi Info v3.3 (CDC, Atlanta, GA, USA) was used for statistical tests.
Ethical issues
According to Italian requirements for ethical research, the approval of an ethics committee was not required because this was not an interventional study. There was no potential disadvantage to the patients or doctors involved because this was an observational study of patients receiving their usual care. Subjects' anonymity was ensured. The local medical association approved the study.
Results
Patient characteristics are shown (Table 1). The sample was an older population with overweight and/or obesity problems and poor control of diabetes; however, the presence of comorbidity was not high.
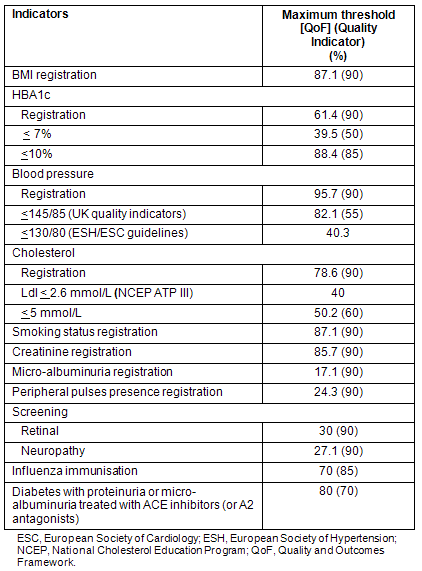
District 32 patients' data were compared with UK quality indicators (Table 2) and a poor level of registration was found for several important variables. An adequate level of registration and control was found for blood pressure. An acceptable level of control for HBA1c was also achieved (but there were missing data for many patients).
Table 1: Patients' characteristics
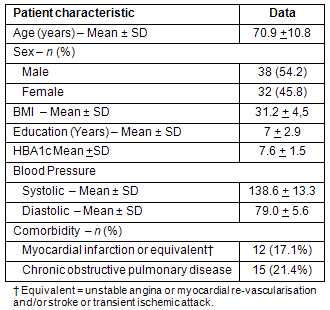
Table 2: Average achievement for each indicator in District 32
Discussion
A strategy that could be introduced easily to this rural area in Italy is the incentive scheme developed as part of the new General Medical Services contract in the UK4. After the introduction of this new system, the achievement of target levels in the UK has been universally high5. Khunti et al conducted a systematic review of published observational studies of quality in diabetes primary care in the UK, and compared the results with data from the QoF of the new General Practice Contract6. They found that the quality of care achieved by the QoF was highest.
Few indicators in the present study reached international standards. The target QoF threshold for HbA1c (50% diabetics at <7%) was not achieved (39.5% below target in the present study). However, the level of blood pressure registration was high (95.7%) and this may be due to the District's easy-to-use electronic medical records.
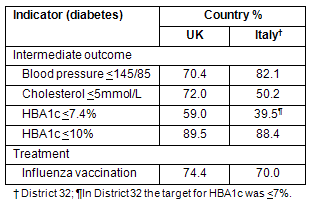
Tables 3 and 4 provide a comparison of the District 32 achievements with those of UK practices (according to McLean et al who studied primary medical care quality differences for cardiovascular disease and diabetes across the NHS after the new contract of 20057). District 32 performed comparatively poorly, particularly in process indicators; however, comparisons of intermediate outcome and treatment indicators were more favorable.
Table 3: Average achievement on each process indicator for UK vesus District 32 (Italy)
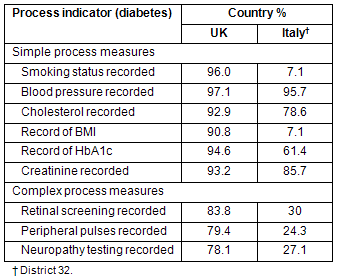
Table 4: Average achievement on each outcome and treatment indicator for UK versus District 32 (Italy)
Strengths and limitations of the study
This study provides data on the level of care in a rural area of Italy. It may contribute to a government assessment of the need to incentivise doctors to improve care (as in the example of the QoF in the UK), and the possible costs of doing so. However, it should be borne in mind that this was a small study that involved a small number of motivated family doctors.
Conclusion
The quality of care and level of control among patients with type 2 diabetes in the rural Italian area studied is not optimal and could be improved; this is especially so in terms of data registration. In the UK, many quality markers have been improved by an incentivisation scheme. Such a scheme may also improve the quality of care provided in rural Italy.
Acknowledgement
Funding was provided by the scientific society SNAMID (National Society for General Practitioners' Education) Caserta, Caserta, Italy.
References
1. Buono N, Petrazzuoli F, Carelli, F. Diabetes and Cardiovascular Risk: Role of the General Practitioner. In: Proceedings, Conference of The European Society of General Practice/Family Medicine Wonca Region Europe. 18-21 June 2003; Lubiana, Slovenia; 2003.
2. Berlowitz DR, Ash AS, Hickey EC, Glickman M, Friedman R, Kader B. Hypertension management in patients with diabetes: the need for more aggressive therapy. Diabetes Care 2003; 26: 355-359.
3. British Medical Association. Annex A: Quality indicators - Summary of points. (Online) 2007. Available: http://www.bma.org.uk/employmentandcontracts/independent_contractors/general_medical_services_contract/investinggp.jsp?page=9 (Accessed 10 December 2007).
4. Department of Health. Investing in General Practice: The New General Medical Services Contract. (Online) 2003. Available: www.dh.gov.uk/en/Publicationsandstatistics/ (Accessed 1 April 2008).
5. Doran T, Fullwood C, Gravelle H, Reeves D, Kontopantelis E, Hiroeh U et al. Pay-for-performance programs in family practices in the United Kingdom. New England Journal of Medicine 2006; 355: 375-384.
6. Khunti K, Gadsby R, Millett C, Majeed A, Davies M. Quality of diabetes care in the UK: comparison of published quality-of-care reports with results of the Quality and Outcomes Framework for Diabetes. Diabetic Medicine 2007; 24(12): 1436-1441.
7. McLean G, Guthrie B, Sutton M. Differences in the quality of primary medical care for CVD and diabetes across the NHS: evidence from the quality and outcomes framework. BMC Health Services Research 2007; 7: 74. DOI: 10.1186/1472-6963-7-74.




