Introduction
Aboriginal people (an all encompassing term currently used to describe the Indigenous people of Canada, including First Nations, Inuit and Métis) comprise approximately 4% of Canada's population. The geographic span of Aboriginal communities reaches from arctic to Canada's temperate regions1. Although culturally very diverse, almost half of the over 700 Inuit and First Nations communities are remote or isolated2, and geographic isolation creates significant barriers to accessing health care. Aboriginal community health is also profoundly affected by the social determinants of health associated with colonial forces. These include the marginalization of traditional Aboriginal world views, culture, languages and lifestyles; assimilation policies such as the forceful removal of children and placement in residential school systems in the last century; and the suppression of traditional economies3-6. As a result, there are significant health disparities in Aboriginal communities when compared with mainstream Canadian communities.
E-health has been described as the 'health services and information delivered or enhanced through the Internet and related technologies' combined with a state of mind to enhance health care using information and communication technology (ICT)7 . E-health, therefore, embodies a critical potential to facilitate more equitable access to health services and health information, particularly in rural, remote and Aboriginal communities in vast countries such as Canada. As is the case with all Aboriginal health services, a culturally-based approach and Aboriginal control of the design and delivery of e-health services is essential to ensure effectiveness4,5,8.
While it is tempting to promote e-health as a solution to health disparities in rural and remote areas, the increasing use of ICT in health care also has the potential to further contribute to health disparities due to inequities in connectivity within and among countries, called the 'digital divide'9. Low income, residence in rural areas, being a member of an ethnic minority group and speaking a minority group language are all proven, significant barriers for individuals and communities to access and use digital ICT10. These obstacles are also characteristics associated with many Aboriginal communities in Canada. In fact, it is probable that much of Indigenous health care worldwide is considerably impacted by this digital divide. Furthermore, case studies in Canada show that even when the appropriate ICT infrastructure has been deployed and regions become technologically connected, timely access and better care through e-health applications do not necessarily follow. Instead, to ensure community uptake, the development of e-health initiatives must be tailored to fit the unique health and social needs of the users and their community11,12. In order to maximize the potential health and socio-economic benefits of e-health, it is essential to conduct research on how e-health and telehealth can be most effectively utilized in remote areas and Aboriginal communities.
In Canada, telehealth has been successfully implemented in a number of Aboriginal communities with subsequent improvements to access to health care, quality of life, quality of care and improved social support13. The academic literature has often treated Aboriginal e-health issues as part of a broader discussion related to rural and remote service provision. Published and peer-reviewed Aboriginal-specific e-health research is rare14. In addition, the existing literature on Aboriginal telehealth consists mainly of case and service-specific evaluations, which limits the generalizability of results2,15-20. Consequently, there are many knowledge gaps that limit the understanding of a broad range of Aboriginal e-health issues, including the specific e-health and technical needs of Aboriginal communities, cultural perspectives and community impact related to e-health implementation21. In short, a research agenda is urgently required.
The Aboriginal Telehealth Knowledge Circle (ATKC; pronounced 'At- Kay-See')22 is the national centre of excellence for Aboriginal telehealth and well positioned to conduct consultations to create and advocate for an Aboriginal e-health research agenda. The ATKC thus initiated the development of a research agenda to answer the question: 'What are the most significant information gaps related to Aboriginal telehealth/eHealth that compromise eHealth adoption and realization of related health benefits over the next decade?'
Methods
In the spring of 2007, the ATKC council began the year long process of developing an Aboriginal e-health research agenda through stakeholder consultation. One of the authors, an ATKC research portfolio holder (MM), facilitated this process. The research protocol received ethics review from the ATKC Council, based on rigorous Aboriginal health research ethics guidelines23. Using Indigenous research methods, a consensus methodology was developed to systematically identify priority areas for Aboriginal e-health research. All participating interviewees provided written consent authorizing the use of their interview data in the development of a research agenda. A participatory action research (PAR) approach was employed. To honor the spirit of community empowerment that is integral to Indigenous research methods as well as PAR, the Council was not merely consulted for input; instead, they collaborated in the research process. Council members monitored the project from beginning to end to ensure Aboriginal perspectives were paramount in the design, data collection, interpretation and dissemination. To ensure high quality, meaningful dialogue between the research leads and the Council, 7 distinct cycles of collaboration were developed which are described in this article.
Western consensus methods
Formal consensus methods have been used by health researchers as a tool to reach agreement among experts on controversial subjects, research agendas or clinical guidelines for several decades24. Among the more common approaches is the Delphi method, where topic experts reach consensus through several rounds of prioritization exercises composed of self-administered questionnaires and anonymous ranking processes25. In contrast, the nominal group technique brings together experts in a face-to-face meeting to collaborate using structured prioritizing exercises. Both techniques have been considered transparent and democratic in the development of health research agendas25-27. Similarly, Glaser's state-of-the-art consensus process uses a small group of experts who identify additional experts using a snowball technique. Next, the expert panel collectively engages in iterative rounds of revisions to a position paper, based on the most current research on a particular topic or practice. Glaser's approach also includes strategies to ensure knowledge translation28.
An Indigenous consensus method
While Western consensus methods are focused on practical applications of health knowledge and consensus building, and are thus conceptually compatible with Indigenous epistemologies, there are also aspects that render them inappropriate for use in Aboriginal health research. Foremost, the emphasis on clinical and academic experts is problematic in Aboriginal research. 'Experts' have shallow histories in Aboriginal communities, and are linked to colonialism and the legitimization of outsiders who speak for Aboriginal people while devaluing Aboriginal knowledge and thus effectively silencing Aboriginal perspectives29,30.
In contrast, the ATKC consensus approach shifts the focus from expert panels to communities of practice and policy-makers; individuals with a lived experience and deep understanding of Aboriginal communities, e-health applications, policies and politics. Figure 1 provides a conceptual representation of the communities of practice involved in the development of the research agenda. Value of community knowledge was acknowledged in the literature review (prepared for consensus participants as a reference tool), which included academic works, as well as the ATKC toolkit, a web-based repository of grey literature. Finally, in the spirit of a commitment to respectful consultation, the authors refrained from using majority rule ranking systems to prioritize the research agenda. Instead, a small community-based executive group, the ATKC Council, focused and prioritized the research agenda using several cycles of consensus. Consensus was considered to be achieved when no new ideas or issues were tabled during a discussion and participants voiced agreement with all prioritized items.
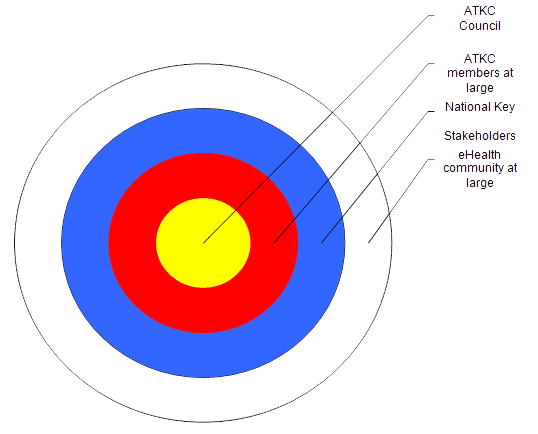
Figure 1: Conceptual model of the key groups involved in the consensus process
Description of the Aboriginal Telehealth Knowledge Consensus method
The Council members and researchers collaboratively developed an Indigenous approach to consensus building, primarily designed to incorporate Aboriginal values and culturally congruent group processes. This ATKC consensus process places less emphasis on the knowledge of experts in the traditional Western sense, rather it invites the perspective of those who are most affected by e-health, community members and communities of practice. Additional voices were then added: those who influence Aboriginal e-health at a policy level, those who educate healthcare professionals, researchers and, last but not least, those who were interested in contributing to Aboriginal e-health in the future.
Elements of existing consensus processes that are congruent with Aboriginal cultural values were incorporated; however, with substantial modifications. For example, in the Delphi approach, a single facilitator is charged with interacting with an anonymous group. The ATKC process in contrast emphasizes a participatory approach. As such a dedicated core group of individuals, the ATKC Council were charged with collecting, reviewing and prioritizing findings from various lines of evidence that included interviewing and polling communities of practice and broadly reviewing the literature. Specifically, the ATKC consensus process involved the following 7 cycles:
Cycle 1: Initiation: The ATKC council identified a research lead (MM) who then guided a face-to-face discussion with six ATKC council members to broadly identify the scope of the research agenda, the spectrum of stakeholders that would be consulted and appropriate ethical frameworks. A composite list was created and projected on a screen for review, discussion and modification until consensus was reached.
Cycle 2: Questionnaire-supported methodology development: Based on the cycle 1 consensus, the researchers created a questionnaire designed to formally collect council members' views regarding: (i) the most significant information needs related to Aboriginal e-health; (ii) key stakeholder groups to be consulted; (iii) existing resource materials; and (iv) models for ethical Aboriginal research. Consistent with the Delphi process, council members then completed a self-administered, electronically distributed questionnaire. Based on the results, an interim report was produced including a research plan with research tools and a list of key informants with strategic geographic, cultural and sector representation.
Cycle 3: Methodology consensus meeting: Council members provided feedback and reached consensus on the research plan during a telephone discussion. The discussion included a research ethics review followed by feedback on the practical aspects of the project such as completeness of key informant list and resource materials and refinement of the key stakeholder interview tools.
Cycle 4: National Key Stakeholder consultations: All interviews were conducted by one Aboriginal researcher (AS). Of the 25 identified key informants, a total of 15 people (60%) agreed to participate in semi-structured telephone interviews. Those who declined participation cited lack of time. Participants had considerable expertise in the area of Aboriginal e-health as leaders of Aboriginal organizations and communities, communities of practice, health policy-makers and/or as academics. The researcher took detailed notes and read back longer answers for verification. Furthermore, a survey was distributed to participants at an ATKC sponsored workshop and 11 out of 15 surveys (73%) were returned. Interview and survey questions were designed to identify information and research needs of diverse stakeholders. A thematic analysis of the interviews and surveys was then conducted. Responses were grouped into categories and summarized.
Cycle 5: Validation of findings in context of current literature: A draft report was completed based on the interview data, questionnaires and literature review. The ATKC council reviewed the report and prioritized the research agenda based on the stakeholder consultation in context of the literature review during a 'round robin' teleconference. Consensus was reached and incorporated into a second draft.
Cycle 6: Validation with community of practice: Next, as an additional level of verification the second draft report was reviewed by the ATKC members at large during a face-to-face meeting of 14 members of the community of practice. One of the researchers (MM) presented each research agenda domain for discussion, modification and finalization until consensus was reached.
Cycle 7: Dissemination and knowledge translation: The report was then adjusted based on the feedback of round 6, and the current paper was drafted and reviewed by the ATKC council.
Results
A total of 40 participants contributed to the research agenda, as part of the survey and interview process and the ATKC review and consensus process. Our analysis revealed that e-health research priorities fall into 6 distinct topical areas. These included: (i) ethical principles for Aboriginal e-health research; (ii) internet-based national information for Aboriginal e-health initiatives; (iii) research related to e-health education and professional development; (iv) sustainability; (v) best practices; and (vi) broader applications and impact of e-health on Aboriginal culture and communities.
Ethical principles for Aboriginal e-health research
Many participants emphasized that a focus on Aboriginal research ethics was of utmost importance to the research agenda, because Aboriginal communities are weary of research due to past negative experiences. A significant body of literature supports the notion that Aboriginal health research must be driven by Aboriginal community needs and interests29-31. In the case of e-health, research must have direct relevance to the applications of telehealth within the community. If academic researchers are involved, they must take a collaborative, partnership-based approach. Partnership models may vary according to the needs and interest of the involved communities and organizations. Participants agreed that researchers should build on existing principles on ethical Aboriginal research such as (but not limited to) those outlined in Table 1. Generally, ethical guidelines should be based on respect for Aboriginal values and knowledge and employ a PAR approach.
Table 1: Ethical models for Aboriginal research

Internet-based national information for Aboriginal e-health initiatives
Aboriginal e-health and telemedicine initiatives are currently in various developmental stages and it is difficult to get an up-to-date, broad overview of these projects in Canada. Basic statistical, demographic and service information is of particular interest and web-based central access to this information is desirable. Research questions are provided (Table 2).
Table 2: Internet-enabled access to baseline research and communication

Research and development of educational resources to enable Aboriginal e-health initiatives
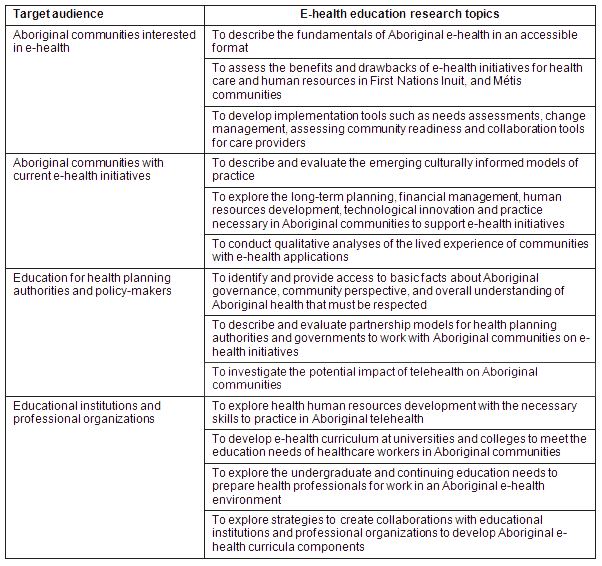
Stakeholders identified a broad range of educational materials that are urgently required to promote the benefits of e-health in Aboriginal communities to government employees, policy-makers, Aboriginal community leaders, health professionals and educators. An overview of the research and development priorities in the area of education and professional development is provided (Table 3).
Table 3: Research and development priorities for e-health education resources
Sustainability models
Participants expressed that sustainability is an important issue for Aboriginal e-health initiatives. There is significant interest by community leaders and policy-makers to learn more about how, for example, telehealth programs can be sustained and expanded over time. The associated research priorities are listed (Table 4).
Table 4: Research priorities related to sustainability of Aboriginal e-health initiatives

Best practices
E-health and telehealth is evolving within mainstream clinical or hospital environments, and the existing models and standards for practice are tailored to these environments. Consequently, there is a need for community-based Aboriginal models of practice and culturally competent models of care that respect the cultural background of Aboriginal patients. Cultural considerations must be a priority to ensure successful integration of telehealth applications at the community level. Best-practice research is required.
Table 5: Research priorities for the development of best practices

Broadening the horizon of Aboriginal telehealth
Research that goes beyond the videoconferencing application is seen as a key requirement for an Aboriginal telehealth research agenda. A broader look at e-health and various telehealth applications is necessary to expand the use of ICT to address the unique health disparities in Aboriginal communities at a national level. The health sector must learn more about applications that are less known but have the capacity to support the health goals of Aboriginal communities, as listed (Table 6).
Table 6: Research priorities to expand e-health and track its impact

Discussion
Our research shows that the successful development of Aboriginal e-health applications is contingent upon knowledge exchange with various stakeholders on a broad spectrum of topics, which go beyond medical and information technology research. There was clear and immediate consensus that Aboriginal research ethics and protection of Aboriginal knowledge must be addressed before research can begin, because past research often exploited Aboriginal communities and failed to acknowledge Aboriginal perspectives and values. Such research was often an extension of colonial practices. Outside experts with little or no understanding of Aboriginal people and communities were commonly in control of all aspects of research projects. Without an emphasis on a two-way knowledge exchange between communities and researchers, research rarely had a positive impact on Aboriginal health. 'Research fatigue' is a common sentiment in Aboriginal communities 30-32. However, over the past decade, many Aboriginal communities have made major advances to take control of the research process and meaningful collaborative health research is occurring more commonly31,33,34. These have the potential to serve as models for future e-health research.
A reoccurring theme was the emphasis on knowledge exchange and there was a call for a central organization, such as ATKC, to facilitate the exchange between communities of practice. An internet-based portal was seen as a tool to facilitate sharing of basic information related to Aboriginal e-health initiatives, as well as to facilitate connection and communication between communities of practice not only within Canada, but also among Indigenous people worldwide. While ATKC has begun to respond to these suggestions, further development of their portal and open access are necessary. New resources will be necessary to accomplish this.
Education needs are multifold, ranging from basic e-health information for community decision-makers, to educating governmental policy makers on how to effectively collaborate with Aboriginal communities and understand the realities of remote community life. Furthermore, university curricula need to be updated to include e-health in order to prepare providers for practice in rural and remote areas.
Stakeholders voiced considerable interest in sustainable models. However economic analyses show that measuring cost-benefit is slow and expensive and it is very difficult to relate health outcomes directly to specific e-health applications35. Furthermore, Canada's free market approach to the development of broadband has disadvantaged Aboriginal communities by setting the 'standard of access as those consumers who can afford it'36. Sustainability will thus be difficult to attain until Canada shows a clear commitment to deploy and maintain broadband technology and thus close the digital divide in Aboriginal communities. Similar to stakeholder research elsewhere, there was also considerable interest in increasing knowledge related to a broad range of emerging applications37. This underscores the need for research that supports the capacity of communities and providers to tailor e-health to their specific and varied needs. Lastly, and perhaps most important, research is required on the interplay between Aboriginal cultures and e-health, including how the practice of e-health and its applications should be adapted to support Aboriginal people's aspirations in health care and self-determination in general; and how cultural safety can be best attained for patients as well as the impact of the adoption of e-health on Aboriginal communities, culture and health.
Aboriginal e-health research has at this point received relatively little attention from funding agencies and researchers. Furthermore, the evolving nature of e-health and divergent provincial e-health strategies make national research projects difficult to realize and research has been largely limited to project based studies. Partnerships among Aboriginal communities, governments and academic researchers are necessary to move this research agenda forward. Improved communication and coordination of e-health research between Aboriginal communities and collaboration with a national advocacy body for Aboriginal e-health will be a key requirement of success. The ATKC is a young national organization with an emergent role. Given the interdisciplinary and complex nature of Aboriginal e-health research, ATKC should consider exploring its role in facilitating research partnerships. The ATKC may also develop its position in facilitating dialogue in Indigenous e-health research priorities with other countries. A web-based Indigenous e-health portal committed to free, open access knowledge exchange is urgently needed to expand e-health information sharing between Indigenous e-health communities of practice worldwide.
The Aboriginal Telehealth Knowledge Consensus method
The Indigenous consensus method developed as part of this project employed an Aboriginal epistemology and placed an unmistakable emphasis on local Aboriginal knowledge, which has frequently been relegated to the periphery in research methods and discourse. This Indigenous research method allowed the research collaborators to reach consensus on a relatively obscure, under-researched topic quickly and effectively. The authors believe this model can be adapted to other Indigenous consensus based research.
Limitations
Participants were recruited from the 10 provincial and 3 territorial regions of Canada; however, given the diversity of Aboriginal cultures, it is unlikely that the full nuances of research priorities in each of these regions has been collected. Initially the consultation with stakeholders focused on the 'sharp end of e-health', that is telehealth applications. However it was quickly realized that stakeholders were concerned about information gaps to a broad spectrum of e-health issues. Priorities for Aboriginal perspectives on health informatics such as electronic medical records are not covered in our project. However, the authors believe that issues related to Aboriginal electronic health records, including ownership, access and control, must be part of a broader political discussion that addresses cross-jurisdictional issues related to Aboriginal health. These issues are of a fundamental political nature and cannot be addressed in this consensus process.
Conclusion
An ATKC consensus process was successfully applied to reach consensus on an Aboriginal e-health research agenda, demonstrating the potential of Indigenous research approaches for defining levels of agreement on complex topics. The resulting conceptual map for e-health research can be used as a springboard for partnership-based research initiatives involving Aboriginal communities, governments and researchers, and may be of interest to Indigenous e-health researchers at an international level.
Acknowledgements
The authors thank all who participated in this study and the ATKC members for reviewing and commenting on the results. Also thanked are the ATKC Council and Ernie Dal Grande for their support of this initiative; and Health Canada's First Nations and Inuit Health Branch, eHealth Solutions Unit and the Northern Ontario School of Medicine for providing necessary resources this project.
References
1. Statistics Canada. 2006 Census: Aboriginal peoples in Canada in 2006: Inuit, Métis and First Nations, 2006 Census. Ottawa, Ontario: Statistics Canada, 2006.
2. Muttitt S, Vigneault R, Loewen L. Integrating telehealth into Aboriginal healthcare: the Canadian experience. International Journal of Circumpolar Health 2004; 63(4): 401-414.
3. Brave Heart MYH, De Bruyn LM. The American Indian holocaust: healing historical unresolved grief. American Indian and Alaska Native Mental Health Research 1998; 8(2): 56-78.
4. Waldram JB, Herring DA, Young TK. Aboriginal health in Canada: historical, cultural and epidemiological perspectives, 2nd edn. Toronto: University of Toronto; 2006.
5. Wieman C. Improving the mental health status of Canada's Aboriginal youth. Journal of the Canadian Academy of Child and Adolescent Psychiatry 2006; 15(4): 157-158.
6. Warry W. Unfinished dreams: community healing and the reality of Aboriginal self-government. Toronto: University of Toronto; 1998.
7. Eysenbach G. What is e-health? Journal of Medical Internet Research 2001; 3(2): e20.
8. Ontario Government. New directions: Aboriginal health policy for Ontario. Ottawa, Ontario: Ministry of Health, 1994.
9. Gibbons MC. A Historical overview of health disparities and the potential of ehealth. Journal of Medical Internet Research 2005; 7(5): e50.
10. Crompton S. Off-reserve Aboriginal Internet users. Canadian Social Trends 2004; 8: 10-17.
11. Peddle K. Telehealth in Context: Socio-technical Barriers to Telehealth use in Laborador, Canada. Computer Supported Cooperative Work 2007; 16(6): 595-614.
12. Gagnon MP, Duplantie J, Fortin J, Landry R. Implementing telehealth to support medical practice in rural/remote regions: what are the conditions for success? Implementation Science. (Online) 2006. Available: http://www.implementationscience.com/content/1/1/18 (Accessed 19 August 2009).
13. Ho K, Jarvis-Selinger S. Identification of best practices for evidenced-based telehealth in British Columbia. (Online) 2005. Available: http://www.cst-sct.org (Accessed 19 August 2009).
14. Jennett PA, Affleck Hall L, Hailey D, Ohinmaa A, Anderson C, Thomas R et al. The socio-economic impact of telehealth: a systematic review. Journal of Telemedicine and Telecare 2003; 9(6): 311-320.
15. Ramirez R, Aitkin H, Jamieson R, Richardson D. Harnessing ICTs: a Canadian First Nations experience. K-Net case study on health. Ottawa, Ontario: International Development Research Centre on behalf of the Institute for Connectivity in the Americas (IDRC/ICA); 2004.
16. Downing R. Bridging Aboriginal digital and learning divides: report on Office of Learning Technologies support to Aboriginal Communities. Ottawa, Ontario: Government of Canada; 2002.
17. Elias B, O'Neil J, Sanderson D. The politics of trust and participation: a case study in developing First Nations and university capacity to build health information systems in a First Nations context. Journal of Aboriginal Health 2004; 1: 68-78.
18. Jin A, Martin D, Maberley D, Dawson K, Seccombe D, Beattie J. Evaluation of a mobile diabetes care telemedicine clinic serving Aboriginal communities in Northern British Columbia, Canada. International Journal of Circumpolar Health 2004; 63(Suppl 2): 124-128.
19. Health Canada. First Nations health care in transition: the Alberta story - finding new ways to improve client health. (Online) 2005. Available: http://www.hc-sc.gc.ca/fniah-spnia/services/ehealth-esante/alta_clients-eng.php (Accessed 26 April 2005).
20. Health Canada. Alberta First Nations telehealth program. (Online) 2005. Available: http://www.hc-sc.gc.ca/fniah-spnia/services/ehealth-esante/tele/ab-eng.php (Accessed 27 April 2005).
21. Shore JH, Bloom JD, Manson SM, Whitener RJ. Telepsychiatry with rural American Indians: issues in civil commitments. Behavioral Science & the Law 2008; 26: 287-300.
22. Canadian Society of Telehealth. Aboriginal Telehealth Knowledge Circle. (Online) 2009. Available: http://www.cst-sct.org/en/index.php?module=pagemaster&PAGE_user_op=view_page&PAGE_id=97 (Accessed 19 August 2009).
23. Canadian Institutes of Health Research. CIHR Guidelines for Health Research Involving Aboriginal People. (Online) 2007. Available: http://www.cihr-irsc.gc.ca/e/documents/ethics_aboriginal_guidelines_e.pdf (Accessed 19 August 2009).
24. Eldredge JD, Harris MR, Ascher MT. Defining the Medical Library Association research agenda: methodology and final results from a consensus process. Journal of the Medical Library Association 2009; 97(3): 178-185.
25. Fink A, Kosecoff J, Chassin M, Brook RH. Consensus methods: characteristics and guidelines for use. American Journal of Public Health 1984; 74(9): 979-983.
26. Kellum JA, Mehta RL, Levin A, Molitoris BA, Warnock DG, Shah SV et al. Development of a clinical research agenda for acute kidney injury using an international, interdisciplinary, three-step modified Delphi process. Clinical Journal of the American Society of Nephrology 2008; 3(3): 887-894.
27. Vella K, Goldfrad C, Rowan K, Bion J, Black N. Use of consensus development to establish national research priorities in critical care. BMJ 2000; 320(7240): 976-980.
28. Glaser EM. Using behavioral science strategies for defining the state-of-the-art. Journal of Applied Behavioral Science 1980; 16(1): 79-92.
29. Ermine W, Sinclair R, Jeffery B. The ethics of research involving Indigenous peoples. Report of the Indigenous Peoples' Health Research Centre to the Interagency Advisory Panel on Research Ethics. Saskatoon, SK: Indigenous Peoples' Health Research Centre, 2004; 272.
30. Smith LT. Decolonizing methodologies: research and Indigenous peoples. New York: St Marten's, 1999.
31. Maar M, Sutherland M, McGregor L. A regional model for ethical engagement: The First Nations Research Ethics Committee on Manitoulin Island. In: JP White, S Wingert, DB Maxim (Eds). Aboriginal policy research moving forward, making a difference. Toronto: Thompson Education, 2007.
32. Warry W. Doing unto others: applied anthropology, collaborative research and native self-determination. Culture 1990; 10(1): 61-73.
33. Jacklin K, Kinoshameg P. Developing a participatory aboriginal health research project: 'Only if it's going to mean something'. Journal of Empirical Research on Human Research Ethics 2008; 3(2): 53-68.
34. Cranley Glass K, Kaufert J. Research ethics review and Aboriginal community values. Can the two be reconciled? Journal of Empirical Research on Human Research Ethics 2007; 2(2): 25-40.
35. Jones R, Rogers R, Roberts J, Callaghan L, Lindsey L, Campbell J et al. What is eHealth (5): a research agenda for ehealth through stakeholder consultation and policy context review. Journal of Medical Internet Research 2005; 7(5): e54.
36. Perley S, O'Donnell S. Broadband video communication research in First Nations communities. In: Proceedings, Canadian Communication Association Annual Conference; 1-3 June 2006: National Research Council Canada, 2006; 1-21.
37. Bahaadini K, Yogesan K, Wootton R. Health staff priorities for the future development of telehealth in Western Australia. Rural and Remote Health 9: 1164. (Online) 2009. Available: www.rrh.org.au (Accessed 15 December 2009).
Abstract
Introduction: In Canada, telehealth has been successfully implemented in a number of Aboriginal communities with subsequent improvements to access to health care and quality of life. However, there are many knowledge gaps that limit our understanding of the broad range of Aboriginal e-health issues; a research agenda is urgently required. The objective of this research was to develop an Aboriginal e-health research agenda designed to address the substantial knowledge gaps that impede e-health deployment and adoption particularly in rural and remote Aboriginal communities in Canada. A consensus method based on Aboriginal culture, values and approaches to consensus was developed to achieve this.
Methods: In this consensus methodology, a core group of Aboriginal telehealth leaders, led by a research facilitator, engaged in an iterative process of individual and group review of research data. The reviewed data included stakeholder interview data, questionnaires, literature and other resources and was prioritized in order to develop recommendations for an Aboriginal e-health research agenda.
Results: A total of 40 stakeholders including Aboriginal Telehealth Knowledge Circle (ATKC) members, communities of practice and regional, provincial and federal leaders and policy-makers participated in the consensus process. The research recommendations showed a high degree of consistency among stakeholders. Participants reached consensus on 6 areas: research ethics, internet-based e-health services data, educational resources, sustainability models, best practices and exploration of innovative applications.
Conclusions: An ATKC consensus process was successfully applied to reach consensus on an Aboriginal e-health research agenda, demonstrating the potential of Indigenous research approaches for defining levels of agreement on complex topics. The resulting conceptual map for e-health research can be used as a springboard for partnership-based research initiatives involving Aboriginal communities, governments and researchers, and may be of interest to Indigenous e-health researchers at an international level.
Key words: Aboriginal people, Aboriginal research ethics, Canada, consensus methods, e-health, Indigenous research methods, research agenda, telehealth.



