Introduction
Within years Germany will face a shortage of general practitioners (GPs), an issue that already exists in some rural regions1. By 2010, approximately 15 600 GPs will have to be replaced in Germany due to their retirement2. This is important because the population is aging and there is an increase in chronic diseases3. There are several reasons for the shortage of GPs. Fewer medical students are deciding to work in patient care, even fewer in general practice and fewer still in general practice in rural areas. However, this trend is not limited to Germany4-6.
In preceding studies, mainly medical students and residents were asked about their attitude to working as a GP in rural areas7-9. Data on job satisfaction from GPs in rural areas has also been made available10,11. Qualitative studies of German GPs regarding working conditions in rural areas are rare. The opinions of GPs appear to be particularly relevant in this context for, from the perspective of occupational sociology, members of a profession have a latent influence on the job orientation of students12. The more satisfied members of a profession are, the more attractive a profession appears to be for the next generation12. To explore the attractiveness of rural doctors' profession, it is important to determine positive and negative aspects of GPs' work in rural areas.
The meaning of 'rural' in the German political context means a 'sparsely populated area with sub-standard density value regarding population, housing and jobs'13. However, there is no consistent definition for the word 'rural' in the context of German health care. For the purpose of this project, rural is defined as a geographic area with less than 5000 inhabitants.
The aim of this study was to explore the 'pros and cons' in the work of GPs in rural areas from the GPs' perspective, and to identify possible measures to counteract a future shortage of rural GPs in Germany.
Method
Design of the study
A qualitative study consisting of semi-structured interviews was chosen to allow intensive analysis of individual opinions, attitudes and needs among the target group. Semi-structured interviews are an established qualitative research method for collecting information from particular groups, for instance professional target groups.
Sample
Within a symposium organised by the Department of General Practice and Health Services Research at the University Hospital of Heidelberg14, GPs were informed about the study and invited to take part in the interviews. A mixed sample in terms of sex, age, number of years in practice, urban or rural setting, solo practice or group practice was selected from the interested GPs. Individual appointments for interview were arranged by telephone.
Interview grid
The interviews were carried out between May and August 2008 in the GP's practice or in the Department of General Practice and Health Services Research, University Hospital of Heidelberg, Germany. The interviews were semi-structured and conducted by a sociologist (IN), who is experienced in conducting interviews. They were based on key questions and lasted 45-60 min each. All interviews were recorded digitally and transcribed verbatim.
Five topics were developed on the basis of literature research15-17. As a warm-up, questions were asked about the motivational reasons for 'choosing the profession of a GP' and the 'job satisfaction of GPs'. The main questions followed concerning the 'image of the GP profession in society', 'recruitment problems for GPs' and the 'attractiveness of the GP profession in rural areas'. Each topic area covered three issues.
As the focus of this article is the 'attractiveness of the GPs' profession in rural areas', the questions from this relevant set of topics are listed:
- What are the advantages of working as a GP in a rural area?
- What are the disadvantages of working as a GP in a rural area?
- How could the attractiveness of a GP's profession in rural areas be increased in order to recruit young doctors for employment in rural areas?
In addition, relevant aspects of the responses from the other topics were included in the analysis. The GPs had the opportunity to answer openly and precisely without being interrupted by further questions, except when something was unclear.
Ethics approval
The ethics committee of the Heidelberg Medical School informed the researchers that approval is not necessary for a study which does not involve patient data.
Data analysis
Analysis was carried out using the ATLAS.ti software (www.atlasti.com. Key issues were identified, summarised, labelled as codes and sorted into main categories and sub-categories, based on qualitative content analysis, as described by Mayring18. Using this approach, qualitative content analysis has developed procedures of inductive category development. Each category was attributed to a quotation19. Interviews and analysis were conducted simultaneously, so that the researchers could control for topic saturation. Two authors (IN and SJ) independently reviewed transcripts to confirm that the codes were comprehensive and reproducible. Disagreements during this process were discussed until consensus was reached. The quotations cited in this article were translated by author IN from German into English and cross-checked by author SJ.
Results
In total, 16 interviews were conducted. The characteristics of the 16 interviewees are summarised (Table 1).
The findings are presented on the basis of deductive and inductive categories. The main inductive categories 'personal level', 'professional level' and 'regional/ structural level' were formed beside the deductive categories 'positive aspects' and 'negative aspects', which were derived from the key questions. An overview of the main categories 'personal level', 'professional level' and 'regional/structural level' and their sub-categories is provided (Table 2).
Table 1: Characteristics of participating GPs
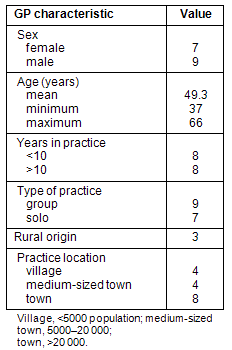
Table 2: Attractiveness of the GPs' profession in rural areas
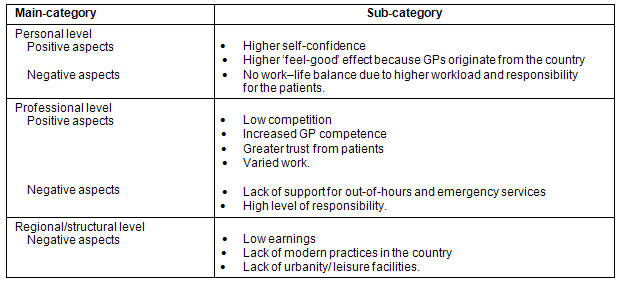
Personal level
Positive aspects: The respondents mentioned that GPs in rural areas have a higher level of self-confidence than GPs from urban areas. This is the result of a better social standing and increased authority.
You can use this authority, for example when someone in the country comes to you with a triviality and you tell him so, what you say is better understood and accepted here than in town. You are more self-confident as a GP in a rural area due to the authority and good social standing. (GP 8)
The GPs who grew up in rural regions particularly appreciated the rural environment and felt attached to their home. The 'feel-good' effect of those GPs seemed very high when returning to the rural area and opening a practice there:
I love the country, grew up in the country. Opening a practice here was thus the only thing that came into consideration for me. I feel very happy here - happier than in an urban environment. (GP 15)
Negative aspects: The workload of practising as a GP in a rural area is considered higher than that of a GP in an urban area. The responsibility of being available for patients around the clock constitutes a large burden for country doctors, which influences their work-life balance in a negative way:
...I found that the work of a country doctor carries a large burden because you have nobody around to give you a bit help. Yes, when emergency medical services are concerned, emergency doctors. But when it's really precarious, when it comes to the crunch, it always takes too long for the ambulance to travel to rural areas. It's a big responsibility that you have to bear in rural areas. (GP 1)
Professional level
Positive aspects: The GPs highlighted the low level of competition among GPs in the rural regions. While their workload increases due to having many patients, the worry about competition is considerably reduced:
They don't have the problem with the competition that we have in town. There's an oversupply in towns, a high density of doctors.... And then they have to really slog away in order to make a living. And they don't have this problem because the patients have no choice but to go to this place. (GP 3)
The competence of the GP is valued more highly in rural areas. In urban areas, people are basically focused on the specialist:
You have a better status in the country. Here, you are really a doctor. In town, the specialist is regarded more highly. When the doctor says something, it is also accepted - most of the time. The relationship has always been good in the country. Here you still have authority. (GP 7)
Usually the GP is the only doctor in the village and thus has an important function as provider of care. Often, patients trust a GP's opinion and advice completely:
In towns, they [patients] are more preoccupied with themselves or better informed. In the country, what you say is believed, whereas here in town the patient goes to a colleague and gets a second opinion. They don't have that opportunity in the country. (GP 10)
Therapeutic limitations, often mentioned by GPs practising in urban areas, do not appear to be a problem for GPs in rural areas. In contrast, they regard the work as more varied:
You can do everything in the country, even surgery is sometimes on the agenda. (GP 8)
In the country you drive roughly 20 minutes to the next orthopaedist. I get to see these illnesses and that widens my knowledge base. (GP 9)
Negative aspects: The lack of support for out-of-hours and emergency services is a considerable challenge for doctors in rural areas. The result is a high level of pressure due to the large amount of work and a high level of responsibility, which could make the work of rural doctors unattractive:
You are always under a high level of pressure as a GP in a rural area because there is a lot of work due to the lack of support. The stress and the high level of responsibility are negative factors associated with being a GP in a rural area. (GP 9)
Regional/ structural level
The regional/structural level covers local problem factors that were taken up by doctors from both urban and rural areas.
Negative aspect: Considering the regional attachment to a rural area, the low earnings count as a major drawback. The respondents from rural and urban areas regarded this as a disincentive to work in a rural area. The many hours of overtime as well as regular home visits are not adequately remunerated, according to the respondents:
And that's what's so unfair about it. It's been like that for decades in the country. You don't get more money for home visits and we finance it through our health insurance contributions. (GP 14)
Additionally, the absence of modern practice equipment is a disincentive. Younger GPs especially attach a great deal of importance on having an attractive practice, which contributes to feeling good at work. The younger respondents held the opinion that older rural doctors have old-fashioned practices and these offer no incentive to prospective successors:
But taking on a run-down practice in the country isn't the hit, of course. And if you haven't got the money to make a nice practice out of it, it makes the matter even more unattractive. (GP 16)
The absence of attractive leisure activities is viewed very negatively by GPs from urban areas. They prefer the city life which includes more leisure facilities. The GPs from urban areas believed this could be a major drawback for young people:
I would miss city life in the country. I greatly value being able to say in the evening, 'OK, I'm going to the cinema now or for a glass of wine round the corner'. I think the young doctors miss city life in the country.... (GP 8)
Measures to increase attractiveness in rural areas
Measures suggested by the GPs to increase the attractiveness of practising as GP in a rural area are reported (Table 3).
Table 3: Measures to increase attractiveness in rural areas

Personal level
The majority of the respondents thought that GPs' dissatisfaction is an important factor influencing the job orientation of medical students. The dissatisfaction of practising GPs could be transferred to medical students and in this way increases the shortage of GPs in rural areas. The 'complaining mentality' of GPs increases the problem. More motivation and optimism on the part of physicians was thought to be necessary for an increased level of job satisfaction:
We [GPs] and especially those in the country should generally be more positively-minded and also communicate this thinking to young doctors. It's no wonder that nobody wants to go to the country when all the doctors moan. I can't talk! I do some complaining now and then as well. (GP 2)
Professional level
Besides job satisfaction, for most respondents the promotion of modern group practices in rural areas was an important aspect of addressing young doctors' needs. To work within a team permits exchange with colleagues on a professional level. Furthermore, it is possible to share emergency medical services in a group practice, thus lessening the high workload.
Yes, that's right, more modern group practices would be best I think. Where you can stand in for each other and where you have room on the one hand but can also share the obligations nicely on the other hand. That would naturally be ideal but then you would naturally have to find someone who also has this intention. (GP 9)
Regional/ structural level
Specifically approaching young doctors originating from a rural region to work as GPs in the country was believed to be an important aspect of recruitment. People who grew up in a rural area would more often decide to move to a rural region and practise there as a GP.
No, it's too stressful for me in town. I'm not a city person. They should just approach young doctors from the country to recruit them for a rural practice. (GP 16)
Discussion
The shortage of GPs in rural areas was an important issue for all interviewed GPs, not only those practising in a rural area, but also those from urban areas. Three main categories were derived from the interviewees' discussion: personal level, professional level and regional/structural level. Most of the positive aspects were found on the professional level: a higher regard for the work of a GP making the profession of being a GP in a rural area attractive. This combined positively with a low level of competition, a higher level of competence and the varied work. Negative aspects were predominantly apparent on the regional/structural level: low earnings, the lack of modern group practices and few leisure facilities were all factors highlighted negatively by the GPs. In part, our results were similar to the findings of an Australian study where only a minority of interviewed medical students could imagine working in a rural area when they originate from urban area8. The reasons for not wanting to work as a GP in a rural area referred to having lower career opportunities (not mentioned by our GPs as a negative aspect), and having a better quality of life in urban areas due to more leisure facilities. This latter point was also highlighted by our interviewed GPs.
Measures to counteract the lack of GPs in rural areas referred to all three levels, according to the present study interviewees. Regarding the personal level, they thought that more optimism on the part of GPs in rural areas could increase the attractiveness of their profession. According to Daheim's sociological theory on career choice behaviour, existing members of a profession have an enormous influence on the job orientation of the next generation12. The more satisfied are members of a profession, the more attractive their profession seems to the next generation. In future more motivation, optimism and a resulting satisfaction on the part of doctors in rural areas could be improved by enhancement of the benefits of working as a doctor in a rural area.
Regarding the professional level, the present interviewees proposed modern group practices to increase exchange on a professional level. Group practices offer several advantages, among them that the financing of the practice is easier because costs are shared. Moreover, they allow professional exchange among colleagues and greater possibilities of sharing out-of-hours and emergency services, thus leading to a better work-life balance and higher satisfaction among individual GPs. This may have another effect on the professional level, because the doctor has more time to attend to the patients' concerns. A Canadian study similarly found that the promotion of group practices could increase the attractiveness of working as a GP in a rural area20.
With regard to the regional/structural level, the present interviewees recommended the recruitment of young doctors originating from rural areas for employment in rural areas. The approach of a 'return-of-service program' is similar to the findings of previous studies that recommended medical students who come from undersupplied regions should be supported because they are more eager to return to rural regions than students from urban areas9,21,22.
A systematic review of the financial incentives provided for physicians practising in rural areas showed that 'return-of-service programs' were successful in short-term recruitment but less successful in long-term retention22. In Germany, previous attempts by the Associations of Statutory Health Insurance Physicians to acquire young physicians for employment in rural areas by offering financial incentives had moderate success only23. In general, most international research shows that financial incentives do not guarantee more doctors being attracted to rural areas22,24. The present GPs thought that origin (urban or rural), personal experiences and individual interests such as young physicians' preference for leisure facilities, are more important and should be focused on in order to counteract the future lack of GPs in rural areas.
Strengths and limitations
This article is the first German qualitative study on the attractiveness of the GP profession with a focus on practising in rural areas, and also on the related problem of recruiting young doctors to rural general practice. The main strength of the study is the sample, which was balanced in terms of gender, time of practising, structure of the practice and region. A further strength is that, in the data analysis, various professionals (a sociologist and physicians) were involved, increasing the inter-subjective view that is desired for qualitative studies.
A limitation of the study is that only four GPs interviewed actually practised in a rural region, three of whom originated from a rural area. However, also interviewing GPs who practised in small and large towns helped to obtain a well-balanced view of the problem of recruiting young doctors in rural areas.
Conclusion
In conclusion, our data provides new insights into the attractiveness of GPs' profession especially in rural areas. The insights gained are therefore beneficial in the development of future measures to counteract the shortage of rural doctors in Germany. Financial incentives are regarded as insufficient to attract enough young physicians to open a practice in a rural area. Future action is required at the personal, professional and regional levels. Furthermore, the origin (urban or rural) of medical student should be considered a relevant predicting factor for their recruitment to rural practice.
Study implications
Recruiting more medical students for employment as GPs in rural areas will be a major future challenge. In order to ensure the availability of primary health care throughout Germany, this challenge must be tackled in a variety of ways. The data from this study provides a starting point.
Acknowledgements
This work was supported by the Baden-Wuerttemberg Ministry of Science, Research and Art, Stuttgart, Germany, within the project 'Competence Centre General Practice Baden-Wuerttemberg'.
References
1. Die Senatorin für Arbeit, Frauen, Gesundheit, Jugend und Soziales. Sicherstellung der hausärztlichen Versorgung in Deutschland. Primärversorgung in Deutschland im Jahr 2020. (Online) 2007. Available: http://www.arztrecht.de/publikationen/krankenhaus/Landesgesundheitsministerkonferenz_Beschluss.pdf (Accessed 5 August 2009). (in German)
2. Korzilius H. Allgemeinmedizin: verkanntes potential. Deutsches Ärzteblatt 2005; 102: 34-35. (in German)
3. Landeszentrale für Politische Bildung Baden-Württemberg 2008. Bevölkerung: die Menschen des Landes. (Online) 2000. Available: www.lpb-bw.de/publikationen/politischelandeskunde/bevoelkerung.pdf (Accessed 6 August 2009). (in German)
4. Wendt C. Gesundheitssysteme im internationalen Vergleich. Ein Überblick über den Forschungsstand. Gesundheitswesen 2006; 68: 593-599.
5. Smith DM. Barriers facing junior doctors in rural practice. Rural and Remote Health 5: 348. (Online) 2005. Available: www.rrh.org.au (Accessed 14 April 2010).
6. McGlone SJ, Chenoweth IG: Job demands and control as predictors of satisfaction in general practice. Medical Journal of Australia 2001; 175(2): 85-86.
7. Lu DJ, Hakes J, Bai M. Rural intentions. Factors affecting the career choices of family medicine graduates. Canadian Family Physician 2008; 54(7): 1016-1017.
8. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9: 1083. (Online) 2009. Available: www.rrh.org.au (Accessed 14 April 2010).
9. Pretorius RW, Milling DA, McGuigan D. Influence of rural background on medical student's decision to specialize in family medicine. Rural and Remote Health 8: 928. (Online) 2008. Available: www.rrh.org.au (Accessed 14 April 2010).
10. Gardiner M , Sexton R , Durbridge M, Garrard K. The role of psychological well-being in retaining rural general practitioners. Australian Journal of Rural Health 2005; 13(3): 149-155
11. Miedema B, Hamilton R, Fortin P, Easley P, Tatemichi S. The challenges and rewards of rural family practice in New Brunswick, Canada: lessons for retention. Rural and Remote Health 9: 1141. (Online) 2009. Available: www.rrh.org.au (Accessed 14 April 2010).
12. Daheim H. Der Beruf in der modernen Gesellschaft. Versuch einer soziologischen Theorie beruflichen Handelns. Köln, Berlin: Kiepenheuer & Witsch Verlag, 1970. (in German)
13. Ministerium für Ernährung und Ländlichen Raum 2009. Ländlicher Raum. (Online) no date. Available: http://www.landwirtschaft-bw.info/servlet/PB/menu/1158374_l1/index.html (Accessed 24 February 2010). (in German)
14. Szecsenyi J, Wiesemann A, Stutzke O, Mahler C. 'Tag der Allgemeinmedizin' - ein Beitrag zur Entwicklung einer gemeinsamen regionalen Plattform zwischen Hausarztpraxen und Universitätsabteilungen. Zeitschrift für Allgemeinmedizin 2006; 82: 449-455.
15. McGlone SJ, Chenoweth IG. Job demands and control as predictors of satisfaction in general practice. Medical Journal of Australia 2001; 175: 85-86.
16. Compton MT, Frank E, Elon L, Carrera J. Changes in medical U.S. medical students' speciality interests over the course of medical school. Journal of General Internal Medicine 2008; 23(7): 1095-1100.
17. Buddeberg-Fischer B, Stamm M, Marty F. Attraktivitätssteigerung der Hausarztmedizin - Ansichten und Vorschläge von praktizierenden Hausärzten. Primary Care 2007; 7(42- 43): 639-641.
18. Mayring P. Qualitative Inhaltsanalyse. Grundlagen und Techniken. Weinheim: Beltz Verlag, 2008. (in German)
19. Krippendorff K. Content analysis. An introduction to its methodology. Beverly Hills, CA: Sage, 1980.
20. Rouke J. Increasing the number of rural physicians. Canadian Medical Association Journal 2008, 178(3): 322-325.
21. Sullivan M. Why are fewer medical students choosing family medicine as career choice? Memorial University of Newfoundland, Canada. (Unpublished thesis) Available: http://www.artc-hsr.ca/Documents%20linked%20to/Thesis%20summary%20Melissa%20Sullivan.pdf
22. Sempowski IP. Effectiveness of financial incentives in exchange for rural and under serviced area return-of-service commitments: systematic review of the literature. Canada Journal of Rural Medicine 2004, 8: 82-88.
23. Hartmannbund - Verband der Ärzte Deutschlands e.V. Der Politik auf die Sprünge helfen. (Online) 2008. Available: http://www.journalmed.de/newsview.php?id=21332 (Accessed 12 August 2009). (in German)
24. Pathman DE, Konrad TR, Ricketts TC III. The comparative retention of National Health Service Corps and other rural physicians. JAMA 1992; 268: 1552-1558.

