Introduction
The Antarctic external environment is extremely cold, dark and isolated during winter1. Over-wintering personnel are isolated from the rest of the world, separated from family and friends and privacy can be severely compromised compared with one's normal environment2.
The psychological aspects of over-wintering are identified as the most difficult to cope with3. It has been claimed that as many as 50% of the people who over-winter in Antarctica suffer from depression, irritability, insomnia, and cognitive problems ('the over winter syndrome')2,4. These complaints have been attributed to the isolation and confinement, as well as low external temperature and a lack of daylight during the winter5. A drop in mood and an increase in discomfort are often reported following the midpoint of the isolation experience3. This is referred to as the 'third quarter phenomenon'6. Sandal7 observed the third quarter phenomenon in relation to reduced coping with stress, but only in land-based Antarctic personnel, not in personnel stationed on ships. She attributed the phenomenon to difficulties in interpersonal relationships.
The psychological difficulties may also relate to changes in diurnal biological rhythms. The midwinter absence of daylight and the constant daylight during summer is a challenge to the maintenance of normal diurnal rhythm. Changes in the biological normal diurnal rhythm will effect sleep and may also influence mood and performance8,9. The way to deal with this challenge is to maintain a strict and fixed work schedule and day-night routine. If this is effective the diurnal rhythm of cortisol will follow the normal pattern, a rise in the morning, and a decrease in the evening10.
There are few studies into cortisol rhythms among personnel working in Antarctica, and their results differ. One study of Antarctic personnel showed that the 24 hour rhythm of cortisol (measured in urine) was maintained during the Antarctic year11, while another study of participants in a Greenpeace expedition showed a free-running circadian rhythm of cortisol, even when the participants had knowledge of time12. However there is no information on work schedule and day-night routine in these studies.
The British Antarctic Survey (BAS) has established fixed schedules for the organisation of work and leisure time, meal times and day-night routines. The base commander is instructed to follow these procedures for all personnel at the station. If these procedures are followed, a normal diurnal cortisol rhythm is expected in BAS over-wintering personnel. If this is the case, there should also be low levels of the 'over winter syndrome'.
The aim of the study was to: (i) discover whether personnel at 2 BAS stations in Antarctica followed a normal diurnal cortisol rhythm during over-wintering, measured by repeated saliva sampling; (ii) establish levels of 'over winter syndrome'; and (iii) analyze to what extent diurnal rhythm was related to performance, as evaluated by the base commander and subjective health complaints (mood, sleep, and unspecific health complaints).
Methods
Participants
In total, 55 healthy individuals who over-wintered at 2 British Antarctic Stations between 1999 and 2007 participated in the study. Of the participants, 32 were located at Halley (29 men and 3 women) with a mean age of 33.38 (8.17) years and 23 were located at Rothera (20 men and 3 women) with a mean age of 28.86 (3.34). They were all recruited from the personnel working at the 2 stations, with 55 of 61 individuals (90.2%) participating in the study. The BAS and the SCAR Working Group on Human Biology and Medicine approved the study, which was conducted in accordance with the Declaration of Helsinki.
British Antarctic Stations involved in the project
Rothera research station (67°34'S, 68°8'W) is located on the west side of the Antarctic Peninsula, and Halley research station (75°35'S, 26°30'W) is located further south. Rothera is the principal BAS logistics centre for support of Antarctic field science, and the main British station for field work. During winter the population is approximately 19. At Halley there are usually approximately 14-16 over-wintering personnel. Most of the winter personnel are technical specialists who are required to keep the station and scientific experiments running. Depending on how far south the research stations are located, the winter period starts in March or April and ends in October or early November. Full winter climatic conditions with total isolation are from May to August for Rothera and from early April to the end of September for Halley.
As an organisation, BAS tries to instil in all parts of their workforce the need to maintain 'normal' working, eating, and sleeping periods, and they have established fixed schedules for the organisation of work and leisure time, meal times and day-night routines. In pre-deployment meetings scientists are made aware that, despite time pressures, it is important to respect the support staff for whom the station is their long term home. At the pre-deployment briefing conference for all new staff, the need for 'normal' timing is stressed. This is given even greater emphasis in the lifestyle workshops of the briefing conference. Base commanders are strongly encouraged to maintain such normal hours with a degree of discipline. Doctors and base commanders discuss the need to hold this firm routine when they meet at their own two-day workshop. The term 'base commander' is used instead of 'station leader' in an attempt to support good discipline, although the powers of the base commander are as limited as any station leader or manager.
Procedure and instruments
The data were collected as part of the SOAP project (Selection of Antarctic Personnel), where the aim was to investigate whether it is possible to identify psychological factors that should be considered in the selection of personnel for service in the Antarctic and other extreme environments13. The personnel volunteer for the service, and have been selected based on interviews and a general medical examination. In addition to the normal routine, the participants in the present study were also screened with questionnaires, and saliva was collected immediately after their arrival at the station (mid-March), at midwinter (the end of June or beginning of July), and in the week before their departure (the end of October).
All personnel keep the same rhythm (wake at approximately 08.00 h, local time), except for one person who works night shift as a watchperson. Every person performs this role for a week and that person was omitted from testing. There has been no evidence of effects from differences in latitude or due to the fact that Rothera has 3 hours of twilight in midwinter (at this time personnel usually remain indoors at both locations due to the poor weather).
Cortisol was measured in saliva. A salivette sampling device (DPC Norway, Brakkerøya, Drammen) was used for collecting saliva and written information on the procedure was managed by the base doctor, who also observed that all participants followed the procedure strictly. Participants were instructed to collect saliva immediately after awakening, 15 and 45 min after waking, and at 15.00 h and 22.00 h on 3 consecutive days. They were also instructed not to eat, drink, or brush their teeth one hour prior to the collection of saliva.
The same procedure was followed immediately after arrival at the station (mid-March), midwinter (end of June or beginning of July), and during the week before departure (mid-October). When possible, samples were centrifuged to separate the saliva from the cotton, to avoid the small chance that the cotton surface may interact with the sample. Tubes were kept frozen (-18oC) throughout the winter period, including during transport back to the UK, and later to Norway for analysis. Luminescence ImmunoAssay-kit (IBL, Hamburg, Germany) was used to assay salivary cortisol, and the coefficients of variation for low and high commercial controls were 2.6-18.8%, and 1.6-14.4% for intra-assay and 12.8-10.9% for inter-assay.
The questionnaires included standardized measures of Subjective Health Complaints (SHC)14, Positive and Negative Affect (PANAS)15, depression (Burnam screen for depression)16, and information on age, gender, occupation, and education. The SHC were measured immediately after arrival at the station, midwinter, and in the week before departure. The PANAS and Burnam screen for depression were measured only at midwinter.
The SHC inventory was used to measure subjective health complaints14. The questionnaire consists of 29 items and measure the degree of subjective somatic and psychological complaints experienced the last 30 days. Severities were scored on a four-point scale from 0 (not at all) to 3 (serious). The inventory yields 5 subscales in addition to the sum score, but only 3 were used in this study: (i) musculoskeletal complaints (headache, neck pain, upper back pain, low back pain, arm pain, shoulder pain, migraine, and leg pain); (ii) pseudoneurology (palpitation, heat flushes, sleep problems, tiredness, dizziness, anxiety, and depression); and (iii) gastrointestinal complaints (heartburn, epigastric, discomfort, ulcer/non-ulcer dyspepsia, stomach pain, gas discomfort, diarrhoea, and constipation). The scale has high validity and reliability14.
Affect was measured using the PANAS15, where each scale consists of 10 words that describe different feelings and emotions. The words included in the positive affect (PA) scale are: attentive, interested, alert, excited, enthusiastic, inspired, proud, determined, strong and active. The words included in negative affect (NA) scale are: distressed, upset-distressed, hostile, irritable-angry, scared, afraid-fearful, ashamed, guilty, nervous, and jittery. The participants were asked to indicate on a five-point scale ranging from 1 ('very slightly or not at all') to 5 ('extremely'), to what extent they have felt this way during the past week. The scale has high validity and reliability15
Depression was measured with the Burnam Screen for Depression16, version of the Center for Epidemiologic Studies-Depression Scale (CES-D). The Burnam Screen for Depression (Burnam) consist of 6 items derived from the original CES-D version17 and 2 items from the National Institute of Mental Health's Diagnostic Interview Schedule (DIS)18. The questions from CES-D are about feelings during the past week (I felt depressed, my sleep was restless, I enjoyed life, I had crying spells, I felt sad, I felt that people disliked me), answered on a four-point scale (1 = 'rarely or none of the time', 2 = 'some or a little of the time' [1-2 days], 3 = 'occasionally or moderate amount of days' [3-4 days], and 4 = 'most or all of the time' [5-7 days]). The two questions from the DIS are about periods of depressed affect during the past year ('In the past year, have you had two weeks or more during which you felt sad, blue, or depressed or lost pleasure in things that you usually cared about or enjoyed? Have you had two or more years in your life when you felt depressed or sad most days, even if you felt okay sometimes? If yes, have you felt depressed or sad much of the time in the past year?')The answer is yes or no18. The scale has high reliability and validity16. The final score is obtained from a complex weighting system; high scores are interpreted as depression, the cut-offs for depression vary16. The present study calculated the sum score on depression, but also examined the scores on the single items in the scale.
Performance and adaptation were measured with the base commander's evaluation just before departure. All participants were rated for psychological functioning, social adaptability, and work performance during the winter. This is a standard interview based on 20 statements covering: energy and enthusiasm, reliability, common sense, ability to work unsupervised, joining in base activities, helping others with their work, communicating with others, tact and co-operation, personal cleanliness, leadership, organising social events, doing his/her job, health and ailments, being miserable and depressed, excess alcohol consumption, aggressive behaviour, complaining about things, being inappropriately cheerful, irritating others, and shirking duties. The base commanders are asked to rate how much they agree with each of the statements on a scale of 1 to 10. Based on the sum score all participants were classified as either 'poorly adapted', 'moderately well adapted' or 'exceptionally well adapted'.
Statistical analyses
The software SPSS for Windows v 15.0 (SPSS inc; Chicago, IL, USA; www.spps.com) was used for the statistical analysis. The mixed model routine was used to model fixed effects for day, time of day, and period for the cortisol measures. To model the repeated nature of the data, a variable identifying the measures at a specific time of day for the given individual was constructed. Thus, for example, the first measures each day for the individuals were considered to be correlated with an autoregressive (AR1) structure. This construct also provided almost equidistant data and the autoregressive covariance structure gave the best model fit compared with the other covariance structures (lowest Aikaikes value). To control for the repeated measures the same day for the individuals, a random factor for individuals was included.
Due to the small sample size data from the two stations were aggregated. There were no significant differences found between the 2 stations in cortisol, scores on subjective health complaints, depression, or affect. There was one exception which was ignored as a chance event: personnel at Halley had a significant (p=0.03) higher cortisol in the evening (1.03 nmol/L) compared with Rothera (0.55 nmol/L) as measured on the second day of the week before departure.
Period differences in diurnal rhythm of cortisol were tested by contrasting cortisol levels from the first week after arrival at the station with those during midwinter and the week before departure. In order to see the effect of base commander's evaluation, subjective health complaints, depression, positive and negative affect on the cortisol rhythm in the different periods, the specific variables were added to stratified models (stratified by period), one at the time. Furthermore, the base commander's evaluation was included as a categorical variable in the stratified models, where the category 'moderately well adapted' was used as the reference value.
Age and gender were adjusted for in the models and p-values less than 0.05 were considered statistically significant.
To make the cortisol data normally distributed a log transformation was used in the analysis of all data on cortisol19. Cortisol values higher than 7 nmol/L (2 samples) and morning samples with a delay of more than 15 min were adjusted or excluded from the analysis (13 samples). The three morning samples (at awakening, and 15 and 45 min after awakening) were used to calculate the cortisol awakening response (CAR). The samples taken 45 min after awakening, at 15.00 h and 22.00 h were used to calculate the mean level for decrease during the day, and the samples taken at 22.00 h (evening sample) were used as a single measure of recovery.
Repeated measures of variance, with Bonferroni corrections, were used to explore differences in SHC at arrival, during midwinter, and before departure.
Results
Diurnal rhythm of cortisol
The participants had a normal diurnal rhythm of cortisol, with the characteristic peak level in the morning and a normal and gradual decrease towards the evening, at arrival, during midwinter, and before departure from the base. The awakening time was 08.00 h, local time, on an average. Local time at Halley was GMT -3 hours, at Rothera GMT -4 hours.
Approximately half-way through their stay (midwinter) the participants had significantly lower CAR (estimate: -.28 [SEM=.06], p<.001) and a significantly lower level for cortisol decrease during the day (estimate: .17 [SEM=.08], p=.04) compared with cortisol levels at arrival. There were no differences in cortisol levels in the evening (estimate: -.03 [SEM=.18], p=.88) (Fig1).
The week before departure the participants had significantly lower CAR (estimate: -.13 [SEM=.06], p=.04), significantly lower level for cortisol decrease during the day (estimate: -.37 [SEM=.08], p<.001), and significantly lower evening levels (estimate: -.69 [SEM=.18], p<.001) compared with cortisol levels at arrival (Fig1).
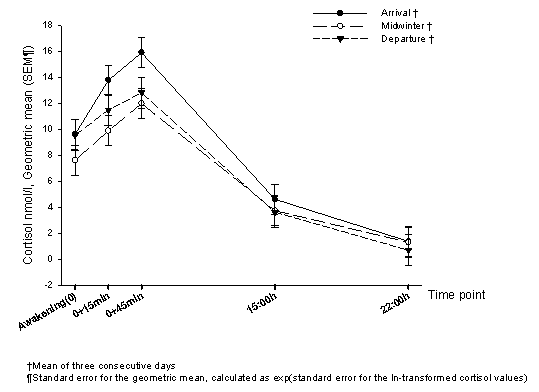
Figure 1: Cortisol levels (geometric mean and standard error of the mean) in the three periods: arrival, midwinter and departure.
Subjective health complaints, depression, positive-and negative affect
There were no significant changes in SHC (sum score, musculoskeletal complaints, gastrointestinal complaints, or pseudoneurology) during their stay in Antarctica (Table 1).
The mean score on the Burnam Screen for depression was .73 (sd=1.27) with a range from -.62 to 6.04. Independent of high or low cut-off points, 32 participants (58.2%) qualified for 'depressive symptoms' according to this scale.
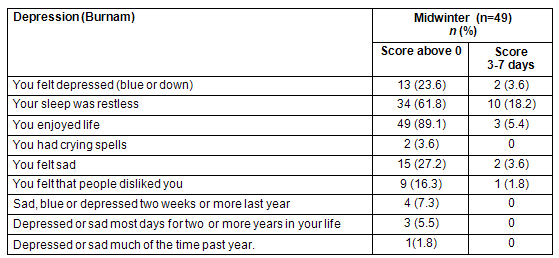
There were no corresponding high scores for depressive symptoms during midwinter on the SHC. There was no significant increase in pseudoneurology, which includes questions on mood. Therefore the scores on single items from both the Burnam screen for depression and the pseudoneurology scale from SHC were examined (Tables 2,3). According to Burnam screen for depression, 13 (23.6%) of the participants reported that they had felt depressed some or a little of the time, while 2 (3.6%) reported they had felt depressed occasionally or a moderate amount of days. In all, 18 (39.1%) scored above 0 using the SHC score on depression, and 4 (8.7%) reported that they had some (score 2) or serious (score 3) depression during the last 30 days.
Table 1: Mean score, standard deviation and percentage of personnel reporting subjective health complaints at arrival, midwinter and departure
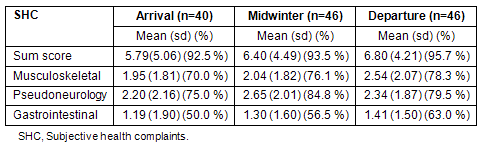
Table 2: Participants reporting pseudoneurological complaints at arrival, midwinter and departure
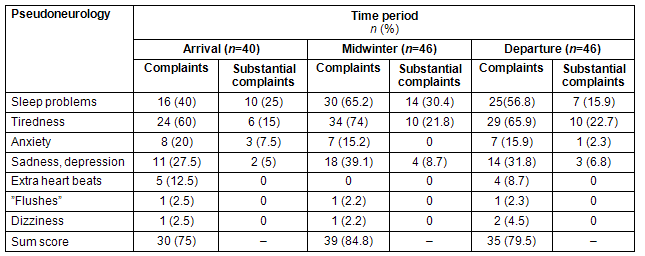
Table 3: Participants reporting depression (Burnam screen for depression) at midwinter
The main contributor to the high scores on depressive symptoms were sleep problems; with 34 (62%) participants reporting little or some of the time on the Burnam screen for depression, and 30 (65.2%) scoring above 0, with 14 (30.4%) reporting some or serious problems on the SHC score on sleep problems. There were also high scores on tiredness on the SHC, with 34 (74%) of the participants scoring above 0 and 10 (21.8%) reporting some or serious problems (Table 2). However, the differences from the arrival scores were slight, with a slight increase in the number of participants reporting sleep problems, tiredness, and depression during midwinter.
At midwinter the mean score on PA were 33.74 (sd=7.18) with a range from 10 to 50, and the mean score on NA were 13.29 (sd = 3.60) with a range from 10 to 23.
Subjective health complaints, affect, depression and diurnal rhythm of cortisol
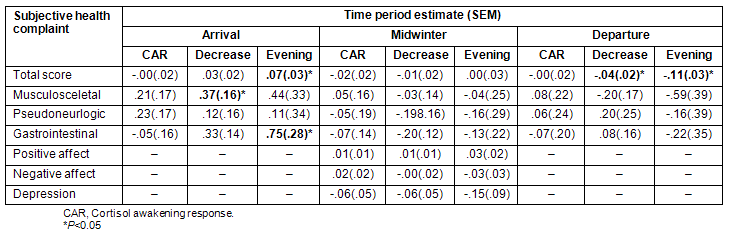
At arrival, a high score on SHC sum score and gastrointestinal complaints where associated to high cortisol levels in the evening (22.00 h) (Table 4). At arrival, a high score on musculoskeletal complaints was associated with a higher mean level for cortisol decrease during the day (Table 2). There were no significant associations between SHC and CAR at arrival.
At midwinter there were no significant associations between SHC and cortisol (Table 4). The week before departure high score on SHC sum score was associated with low level for cortisol decrease during the day and low cortisol levels in the evening, indicating a low mean cortisol level across the day.
Positive affect, negative affect, and depression were not associated to cortisol measured at midwinter (Table 4).
Table 4: Multilevel estimates and standard error for the cortisol response after awakening, cortisol decrease (slope) during the day and cortisol level in the evening (22.00 h) at arrival, midwinter and departure when subjective health complaints (total score, musculoskeletal, pseudoneurology, and gastrointestinal), positive affect, negative affect, and depression (Burnam) were added to stratified models one at the time
Base commander's evaluation
In total, 6 participants (11.3%) were evaluated as 'poorly adapted', 33 (62.3%) were evaluated as 'moderately well adapted', and 14 (26.5%) were evaluated as 'exceptionally well adapted' according to the base commander's evaluation.
Base commander's evaluation and diurnal rhythm of cortisol
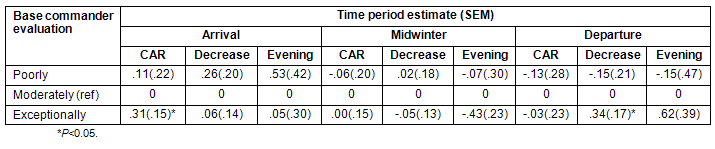
Participants evaluated as 'exceptionally adapted' had significantly higher CAR at arrival and a steeper decrease during the day the last week before departure when participants evaluated as 'moderately adapted' were used as reference (Table 5).
Table 5: Multilevel estimates and standard error of the cortisol response after awakening, cortisol decrease (slope) during the day and cortisol level in the evening and the association with the base commander's evaluation when personnel evaluated as 'moderately well adapted' were used as reference value
Discussion
The main finding is that in spite of the isolation, the extreme external environment, the continuous lack of daylight midwinter, and the midnight sun during summer, disruption of the diurnal cortisol rhythm was not observed. The participants had the normal peak level in the morning, and the normal and gradual fall towards evening both during the period of extreme external darkness outside, and during the summer with no or little darkness during the night. There were no significant differences between the stations in spite of the difference in latitude. There are no significant latitude effects on seasonal affective disorder in North America20
The levels of cortisol were higher at all measurement points immediately after arrival at the Antarctic stations. These values cannot be considered 'baseline' or 'normal' values because the high CAR at arrival were obtained in a period of high activity at the research stations where routines have to be established in a novel and challenging environment. In addition to the high activity level and work burden, there is also constant daylight and low external temperatures. This period is generally considered to be the most stressful part of the stay2. Participants evaluated as exceptionally well adapted had a significantly higher cortisol awakening response at arrival and a greater decrease during the day at departure compared with participants evaluated as moderately adapted. These results fit the assumption that high activation may be good for performance21.
Despite the normal cortisol rhythm that did not indicate any over-winter syndrome, more than half of the participants (58%) qualified for 'depressive symptoms' on the Burnam scales at midwinter. The results are in accordance with other studies from Antarctica4. However, examination of the single items in the SHC and Burnam scales indicates that the high scores were due to sleep problems. Comparison of SHC scores from these participants with normative data from Norway22 confirms that the difference is made by sleep complaints.
It was mainly sleep problems that were higher than the normative data from Norway22. Although sleep problems occurring under these circumstances may be a valid complaint, they do not support the concept of an 'over winter syndrome'. The concept also lacks support from our scores for mood, PA, NA and the maintenance of a normal diurnal rhythm.
The BAS routines adhere strictly to the maintenance of a regular schedule, with fixed times for meals and job routines. The results suggest that this is important for the maintenance of normal rhythms and wellbeing. In general, performance is also maintained at a high or acceptable level, as judged from the base commander's reports. Finally, the BAS personnel are highly selected. They are self-selected in that they volunteer for the expedition, and they are selected for the service by a BAS panel with considerable operational experience. Personnel also go through an extensive medical examination before being accepted for over-wintering service.
The general finding of a reasonably healthy population is also supported from the other SHC scores, at all three measuring points the participants scored lower on health complaints than the average scores in the Norwegian population22. The participants also have better scores on PA and NA compared with normative data from the UK23. However, due to the small sample size there is a risk for type II error in the analyses.
Conclusion
The participants in this study were able to maintain cortisol rhythm during the winter. There were no changes in SHC during their stay and in general the average score on SHC, PA and NA were better compared with average scores in normative data. The only signs of an 'over winter syndrome' was the score on depressive symptoms measured at midwinter, which instead appeared to be due to subjective sleep problems and tiredness. High scores on SHC were related to high cortisol levels in the evening at arrival and low cortisol levels in the evening at departure. Depression, PA and NA were not associated with the cortisol rhythm. Adaptation was related to high cortisol awakening response and cortisol decrease during the day in participants rated as exceptionally well adapted.
Acknowledgements
The authors acknowledge the BAS Personnel Department for processing, distribution and collection of SOAP input data forms; the wintering staff who took part in the study; Nina Konglevoll for technical assistance, Eli Nordeide, Randi F Espelid and Nina Harkestad for the analysis of cortisol. The study was supported by grants from BAS/BASMU and Unifob health.
References
1. Bradbury J. Utter isolation in a cold climate: the Antarctic challenge. Lancet 2002; 359(9312): 1130.
2. Palinkas L.A. Going to extremes: the cultural context of stress, illness and coping in Antarctica. Social Science and Medicine 1992; 35(5): 651-664.
3. Décamps G, Rosnet E. A longitudinal asseement of psychological adaptation during a winter-over in Antarctica. Environment and Behavior 2005; 37: 418-435.
4. Palinkas LA, Suedfeld P. Psychological effects of polar expeditions. Lancet 2008; 371(9607): 153-163.
5. Palinkas LA, Houseal M, Rosenthal NE. Subsyndromal seasonal affective disorder in Antarctica. Journal of Nervous and Mental Disorders 1996; 184(9): 530-534.
6. Bechtel RB, Berning A. The third-quarter phenomenon: do people experience discomfort after stress has passed? In: AA Harrison, YA Clearwater, CP McKay (Eds). From Antarctica to outer space: life in isolation and confinement. New York: Springer-Verlag, 1991; 261-266.
7. Sandal GM. Coping in Antarctica: is it possible to generalize results across settings? Aviation, Space and Environmental Medicine 2000; 71(9 Suppl): A37-43.
8. Sack RL, Auckley D, Auger RR, Carskadon MA, Wright KP Jr, Vitiello MV et al. Circadian rhythm sleep disorders: part I, basic principles, shift work and jet lag disorders. An American Academy of Sleep Medicine review. Sleep 2007; 30(11): 1460-1483.
9. Costa G. The impact of shift and night work on health. Applied Ergonomics 1996; 27(1): 9-16.
10. Weitzman ED, Fukushima D, Nogeire C, Roffwarg H, Gallagher TF, Hellman L. Twenty-four hour pattern of the episodic secretion of cortisol in normal subjects. Journal of Clinical Endocrinology and Metabolism 1971; 33(1): 14-22.
11. Griffiths PA , Folkard S, Bojkowski C, English J, Arendt J. Persistent 24-h variations of urinary 6-hydroxy melatonin sulphate and cortisol in Antarctica. Experientia 1986; 42(4): 430-432.
12. Kennaway DJ, Van Dorp CF. Free-running rhythms of melatonin, cortisol, electrolytes, and sleep in humans in Antarctica. American Journal of Physiology 1991; 260(6Pt2): R1137-1144.
13. Grant I, Eriksen HR, Marquis P, Orre IJ, Palinkas LA, Suedfeld P et al. Psychological selection of Antarctic personnel: the 'SOAP' instrument. Aviation, Space and Environmental Medicine 2007; 78(8): 793-800.
14. Eriksen HR, Ihlebaek C, Ursin H. A scoring system for subjective health complaints (SHC). Scandinavian Journal of Public Health 1999; 27(1): 63-72.
15. Watson D, Clark LA, Tellegen A. Development and validation of brief measures of positive and negative affect: the PANAS scales. Journal of Personal Social Psychology 1988; 54(6): 1063-1070.
16. Burnam MA, Wells KB, Leake B, Landsverk J. Development of a brief screening instrument for detecting depressive disorders. Medical Care 1988; 26(8): 775-789.
17. Radloff L. The CES-D scale: A self-report depression scale for research in the general population. Application of Psychological Measures 1977; 1: 385-401.
18. Robins LN, Helzer JE, Croughan J, Ratcliff KS. National Institute of Mental Health Diagnostic Interview Schedule. Its history, characteristics, and validity. Archives of General Psychiatry 1981; 38(4): 381-389.
19. Tabachnick BG, Fidell LS. Using multivariate statistics. Boston: Pearson/Allyn and Bacon, 2007; 980.
20. Mersch PP, Middendorp HM, Bouhuys AL, Beersma DG, van den Hoofdakker RH. Seasonal affective disorder and latitude: a review of the literature. Journal of Affective Disordorders 1999; 53(1): 35-48.
21. Ursin H, Eriksen HR. The cognitive activation theory of stress. Psychoneuroendocrinology 2004; 29(5): 567-592.
22. Ihlebaek C, Eriksen HR, Ursin H. Prevalence of subjective health complaints (SHC) in Norway. Scandinavian Journal of Public Health 2002; 30(1): 20-29.
23. Crawford JR, Henry JD. The positive and negative affect schedule (PANAS): construct validity, measurement properties and normative data in a large non-clinical sample. British Journal of Clinical Psychology 2004; 43(Pt 3): 245-65.
Abstract
Introduction: The diurnal rhythm of saliva cortisol and its association to adaptation, performance and health were examined in personnel over-wintering at two British Antarctic stations.
Methods: In total, 55 healthy individuals (49 males, 6 females) participated in the study. Cortisol in saliva was sampled on 3 consecutive days (at awakening, 15 and 45 min after waking, at 15.00 h, and 22.00 h) immediately after arrival at the station, midwinter, and the last week before departure. Subjective health complaints were also measured at arrival, midwinter, and the last week before departure, while depression (Burnam screen for depression) and positive and negative affect (PANAS) were measured at midwinter only. At the end of the winter appointment, base commanders evaluated the performance of all personnel.
Results: The variations in external light (darkness during winter, midnight sun during arrival and departure) did not influence the diurnal rhythms. The normal peak level in the morning, and the normal and gradual fall towards the evening were observed at arrival, midwinter, and before departure. Immediately after arrival the cortisol values were relatively high and correlated positively with base commander's evaluation of performance. During midwinter, approximately 58% scored for depression on the Burnam scale. However, when examining these data more closely, only 4 participants (7%) reported depression, the main reason for the high score on the depression scale was related to sleep problems and tiredness.
Conclusions: There was no indication that over-wintering led to any disturbance in the diurnal rhythm of cortisol in British Antarctic personnel. There were no other indications of any 'over-wintering syndrome' than reports of subjective sleep problems and tiredness.
Key words: adaptation, cortisol, extreme environment, sleep problems, subjective health complaints, tiredness.
You might also be interested in:
2008 - Correction, article no. 824: Attracting psychiatrists to a rural area - 10 years on






