Context
The recruitment and retention of qualified health workers has been a crucial premise for health service delivery in the circumpolar region, as well as in other remote and rural areas for decades1. In fact, in the interests of achieving universal access to healthcare, as espoused by WHO's renewed commitment to primary health care2, rural recruitment and retention of health workers is crucial. This article describes how improved internships (pre-vocational training) for medical graduates have been applied as one way to recruit new physicians to northern Norway. It also provides a preliminary analysis of whether internship in Finnmark (Norway's most northern and remote county) encouraged more physicians to settle in northern Norway than could be expected from their place of origin, and also suggests the main characteristics of those more likely to stay.
When internship was established in Norway in 1954, the grounds were purely pedagogical: it replaced 18 months of the curriculum at the University of Oslo, the only medical school in the country at that time. The first year of the internship was taken in a hospital (6 months in surgical department and 6 months in internal medicine) and the last 6 months in primary care (PC), both under guidance and supervision of an experienced doctor.
At the beginning of the 1960s a serious shortage of doctors arose, particularly in rural areas, and the internship soon became a useful way to mitigate this crises. By sending interns to rural hospitals and to vacant positions in general practice in remote areas, the shortage was eased and vacant positions filled, albeit with young and inexperienced doctors.
For many years the bulk of internships were in small hospitals and general practice in rural and remote areas, particularly in the north. Because the number of new graduates in internship has more than doubled in the last decade, more placements have had to be established in urban areas. The percentage of interns is, however, still higher in the north. Rural areas and small hospitals are ranked as providing the best quality training3, allowing interns more interesting work without having to compete with the junior doctors in postgraduate specialist training as they do in the university hospitals.
The graduates do not apply for the internships as in ordinary employment; the system is more like a lottery. Graduates sign up for internship with the Norwegian Registration Authority for Health Personnel (SAFH) and each applicant is randomly assigned a number. Posts are chosen in chronological order: candidate 1 can choose any post in the country, while the unfortunate (last) candidate 450 must accept the post that is left. Posts in the most remote areas are usually last to be chosen.
Issue
Internships in Finnmark
Finnmark is the northernmost county in Norway, situated far beyond the Polar Circle. Covering an area greater than Switzerland it has approximately 73 000 inhabitants. There are 2 small but well equipped hospitals. One has 60 beds and 40 doctors, of which 8 (20%) are interns; the other has 100 beds and 63 doctors, of which 16 (25%) are interns.
The 19 municipalities (of which 15 have less than 5000 inhabitants) all offer comprehensive PC, and host approximately 20 interns each half-year (40/year). This is approximately 20% of the PC physician workforce.
Internships in Finnmark can be quite challenging, especially in PC. The long distances and harsh climate can make it difficult to transfer patients to a higher level of medical care. In remote communities PC physicians must cope with medical conditions that would be treated in hospital elsewhere, at least until the weather improves and transfer is possible. However, this makes the work more interesting and provides a very good training environment if guidance and supervision is appropriate.
The Norwegian rural health workforce crisis
Since internship was established, it has been the primary pathway for recruiting new physicians to rural positions. In earlier times the common career pathway was to work 3-5 years in a rural area after internship, before returning to the south for more senior positions. However, from the mid-1990s recruiting senior medical staff in this way failed because most of the young doctors returned to urban areas as soon as they were fully licensed. The resulting serious shortage of physicians in the north meant that by 1997 more than 30% of Finnmark's PC physician positions were vacant or filled by short-term replacements4, mostly flown in from Sweden or Denmark.
Fighting the crisis - the Finnmark intern support project
Starting in 1997, a new effort was made to retain interns in Finnmark: they were offered tutorials in groups, in addition to the day-to-day clinical supervision by their local GP. The groups met 3 times for 1-3 days during the 6-month period of their PC internship, with the first meeting at approximately 1 month after the beginning of service. The groups were encouraged to discuss the challenges they met during their difficult service and to share experience of solving these problems (Fig1). The meetings also provided opportunities to meet with peer interns from neighbouring municipalities in an attempt to overcome the professional and social isolation many faced.

Figure 1: Agenda for the first group meeting.
The project was conducted by an experienced GP and group tutor from the Chief County Medical Officer of Finnmark, and it was funded by The Ministry of Health. There were no baseline data available for the evaluation but interns in Nordland, the second most remote county, served as 'control group' from the beginning. While this initiative was heartily welcomed by the Finnmark interns and vacancy rates started to drop, shortages continued to rise in other counties. The project was therefore extended to other counties and the 'control group' was lost. From 2004, the group tutorial has been an integrated element of internship training throughout the country.
Analyzing characteristics and trends in the improved Finnmark internship: methods
Over the years of the improved internship scheme, data were collected from graduates serving PC internship in Finnmark between 15 January 1999 and 15 August 2006. Of the 267 interns in this period, complete records were obtainable for 233 (87.3%).
The following intern characteristics were recorded:
- place of origin (rural or urban, north or south, or abroad)
- graduating university
- place of first professional post after internship (primary or hospital/specialist care; rural, urban or foreign).
The common migration pattern for young people in Norway, especially in the north, is to move from rural/remote areas to central regions to seek higher education5. Medical graduates from the south of the country seldom apply for jobs in the north6. The present study examined whether internship in Finnmark encouraged more physicians to settle in northern Norway than could have been expected from their origin, and what factors were the main predictors of this.
Those who did not start to work as physician immediately after internship were excluded from most analyses. Their reason was recorded (eg maternity leave, military service, a long vacation).
The data were processed in SPSS (SPSS Inc; Chicago, IL, USA; www.spps.com. Differences were tested with a binominal test and Pearsons χ2 test. Significance was estimated at 5% (p<0.05 or confidence interval [CI] 95%). The predictors were tested by logistic regression, keeping 'Job in the North' , 'Job in PC North' and 'Job in PC' as the dependent variable and using 'southern upbringing' or 'southern graduation' as reference. Logistic regressions were adjusted for gender. Hosmer and Lemeshow's goodness-of-fit test showed that the models used were a good fit for the data.
Results
The data set consisted of 112 men (48%) and 121 women (52%). In all, 43 (18.5%) of the interns had grown up in northern Norway, while 150 (64.4%) came from the south of the country and 40 (17.2%) from abroad (Fig2).
The distribution of interns according to their graduating universities is shown (Fig3). The 84 interns (36%) who graduated from foreign universities is more than double the 40 (17.2%) who grew up abroad. This reflects the fact that many Norwegian students go to medical schools abroad due to an insufficient domestic education capacity. As a result, many Norwegian students are given scholarships and loans from the Norwegian Government to study abroad.
Of the 233 interns, 181 started work as a licensed physician immediately after their internship, and their place of first fully licensed physician position is shown (Fig4). Of the remaining 52 interns, 23 went into military service, 8 went on maternity leave and 21 had other reasons for not commencing work as a licensed physician.
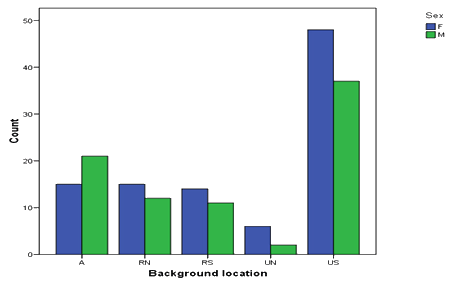
Figure 2: Finnmark interns by place of upbringing. RN, Rural north; RS, rural south; UN, urban north; US, urban south; A, abroad.
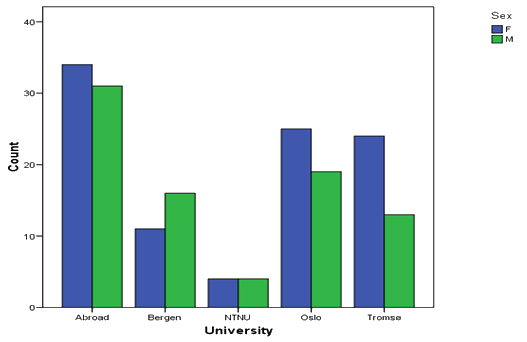
Figure 3: Distribution of Finnmark interns by graduating university.
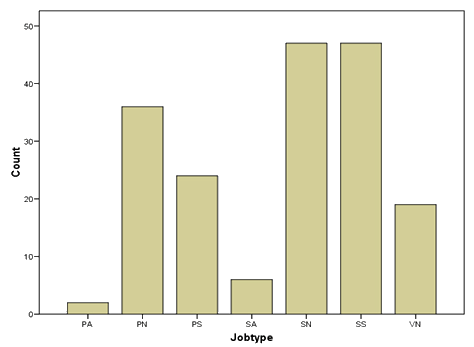
Figure 4: Finnmark interns' choice of first job as fully licensed physician. PA, Primary care post abroad; PN, primary care in north; PS, primary care in south; SA, specialist/hospital care abroad; SN, specialist/hospital care in north; SS, specialist care in south; VN, short term replacement in vacant primary care in the north.
While only 43 (18.5%) of the interns were brought up in northern Norway, as many as 83 (45.9%) took their first job there. Considering the aforementioned general trend of graduates of northern origin remaining in the south and very few of southern origin seeking jobs in the north, one would have expected no more than 18.5% of graduates to take up positions in the north. The difference between those expected to stay in the north on the basis of their origin and those who actually stayed, is highly significant (p<0.001). Of the 35 interns with a northern background who started work immediately, 31 (88.6%) took their first job in the north, which was significantly higher than for those in the total group (p<0.001). This corresponds to the logistic regression where northern upbringing also proved to be the most important predictor for taking a job in the north (Table 1).
Logistic regressions were generated to analyze predictors for job (Table 2) and location choices. Sub-grouping of background (rural and urban) did not add any significant information and was left out of the regressions to ensure more robust models.
Table 1: Cross-tabulation between background and first job in the north (or not)
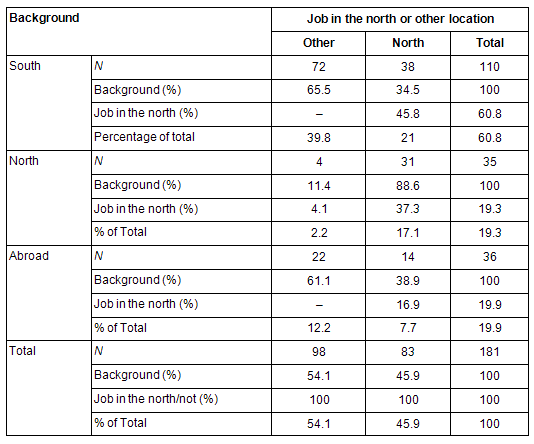
Table 2: Predictors for the first job after internship, expressed as odds ratio
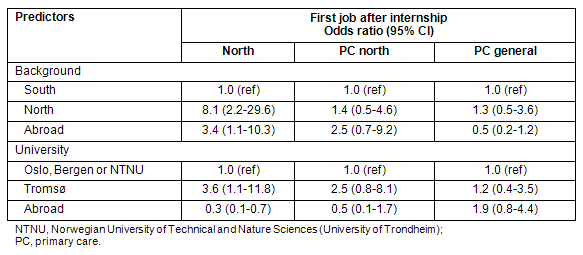
Interns brought up in the north were 8 times as likely to take their first job in the north as were those with a southern background and this is highly significant (CI 2.2-29.6). Interns from abroad were also significantly more inclined to start working in the north than their peer from southern Norway.
Interns who graduated from the University of Tromsø were 3.6 times more likely to take a job in the north than their counterparts from the 3 southern universities. Graduates from foreign universities, of which more than 50% were Norwegians who went abroad to study, were however significantly less prone to start working in the north.
Interns who grew up abroad or graduated from the University of Tromsø had a higher tendency to choose PC in the north (odds ratio 2.5), but this was not statistically significant (CI 0.7-9.2 and 0.8-8.1, respectively).
Of the 181 interns who started work immediately, 99 (54.7%) went into hospitals, while 62 (35.4%) chose PC. No significant predictor was found from the logistic regression for choosing PC in general.
Lessons learned
The most important finding in this study is that significantly more interns than could be expected from their origin took their first fully licensed physician job in the north. Given that this improvement coincided with the introduction of supported internships in the north, this fact was interpreted as an indication that internship in the north, when accompanied by adequate professional and social support, does promote recruitment. Although causality cannot be proved, this is a strong enough association to draw some recommendations.
Due to the random nature of the appointment system, many medical graduates who would never have applied for a rural job voluntarily are allocated a rural position. During internship they are exposed to rural life and the challenges of northern medical practice. Some enjoy these conditions enough to stay.
An additional 19 interns (10.5% of the workforce) stayed in the north for at least a few months as locums, and they were highly preferred to foreign locums by the municipalities.
Determinants for staying in the north
Several studies7,8 have shown that northern background graduates from the (northern) University of Tromsø are more likely (approximately 4:1) to start working in the north than their classmates who are brought up in the south. It is on this basis that students from the north are selected by this medical school. The present study confirms that graduation from the University of Tromsø is an independent predictor for seeking a job in the north among interns, but that northern upbringing is an even stronger predictor.
Another study showed that final year medical students from the University of Tromsø are much more willing to seek work in the north than their counterparts from a southern university (Oslo)6. The results of the present study not only confirm this, but also show that Oslo graduates serving their internship in Finnmark are more likely to seek jobs in the north (35.7%) than their average class mates (7.5%) (Fig5). This is another indication that internship in Finnmark influences a subsequent job location in the north.
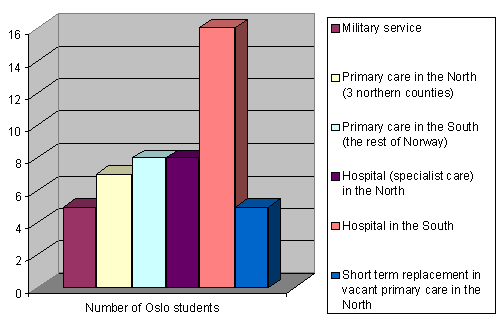
Figure 5: Destinations of Oslo-trained Finnmark interns.
Another interesting result is that interns brought up abroad were significantly more likely to start working in the north than their peers from southern Norway. This might indicate that foreign physicians coming to Norway are more prepared to take jobs where they are easy to find. And being far from family and friends already, foreign-trained interns may not have a strong preference for an urban location.
However, graduation from a foreign university in general makes taking a job in the north less likely. This could imply that Norwegian students graduating abroad, even with an internship in Finnmark, are not a good recruitment source for northern Norway.
Although interns brought up in northern Norway are much more likely to stay, it should be kept in mind that 38 of the interns (45.8%) who took their first job in the north did come from the south, and an additional 14 (16.9%) came from abroad. The appointment system for internships in Norway drives a lot of medical graduates who would never have chosen to work in the north to do so. Internship in the rural north exposes young doctors to challenging medical practice and living conditions. Given appropriate professional and social support, a certain proportion will decide to stay. In Australia, Hays et al. showed similarly that non-metropolitan attachments after graduation were particularly useful in influencing a rural career choice for medical graduates with no previous exposure to rural life or medical practice9.
Determinants for PC in the north and PC in general
The shortage of physicians in the north has been more critical for PC than for hospitals, and recruitment and retention of GPs has been a top priority for health authorities. While none of the present study's predictors were statistically significant, both foreign upbringing and graduation from the University of Tromsø gave a 2.5 times higher likelihood than the reference for taking up a PC job in the north, and both were close to statistical significance.
None of the predictors were significant for choosing PC in general, but it was shown that 34% of interns from Finnmark made this choice. That is significantly higher than the 15% national gain of new GPs during the same period10, p<0.001. This may be an indicator that internship in Finnmark also recruits to PC in general.
The interns in the present study were followed up by professional and social support. This support is likely to be a major factor in interns having the confidence to enjoy challenging service and the courage to endure it. A strong indicator for this is the significant drop in vacancies in Finnmark after the introduction of the intern support project11, and the reduced number of vacancies has remained constant since. The structured preparation for and continuous support in the Finnmark internship, along with licensing being dependent on internship completion, distinguishes this project from other less successful 'bonding models'12,13.
Experience during internship is, of course, not the only issue important to young physicians when they decide on a future career, and direct causality between internship in and recruitment to Finnmark is not claimed. The association is, however, striking and during the period of the present study most other factors (wages, working hours etc.) disfavored rural practice in the north. It can be confidently concluded, therefore, that internship in Finnmark has contributed to improved recruitment of physicians to the region.
The main points/recommendations from this study can be summarized as:
- Medical internship (compulsory service) in remote areas, accompanied by adequate professional and social support, may improve recruitment to further service in the area.
- The interns brought up or educated in the region are those most likely to make this choice. However, candidates from other areas who are allocated to internship in the north due to the random appointment system, have an increased probability for further work in the region.
Acknowledgements
The project was funded by The Ministry of Health and Care Services/The Directorate of Health. The analysis was supported by the World Health Organization program 'Increasing access to health workers in remote and rural areas through improved retention'. The National Center for Rural Medicine in Tromsø assisted with statistical analyses (postdoctoral scholar Tonje Braaten) and academic support.
References
1. Dolea C, Braichet JM, Shaw DMP. Health workforce retention in remote and rural areas: call for papers. Bulletin of the World Health Organisation 87(7). (Online) 2009. Available: http://www.scielosp.org/scielo.php?script=sci_arttext&pid=S0042-96862009000700002&lng=en. (Accessed 28 February 2010).
2. WHO. Primary health care - now more than ever. Geneva: WHO, 2009.
3. Norwegian Medical Association Internship Committee. Annual report. (Online) no date. Oslo: The Norwegian Medical Association. Available: www.legeforeningen.no (Accessed 29 April 2010).
4. Chief County Medical Officer of Finnmark. Annual report. (Online) no date. Vadso: Chief County Medical Officer of Finnmark. Available: http://www.helsetilsynet.no/templates/ArticleWithLinks____6466.aspx (Accessed 29 April 2010).
5. Carling J. Flyttemønster 1977-98 [Domestic migration patterns 1977-98]. (Online) 1999. Available: www.ssb.no/samfunnsspeilet/utg/9906/6.shtml (Accessed 30 March 2010). (In Norwegian)
6. Alexandersen Ø, Jørgensen E, Østerås J, Hasvold T. Medisinerutdanningen i Tromsø - sikrer den legerekrutteringen til Nord-Norge? [Medical school in Tromsø - does it ensure recruitment of phycisians to nothern Norway?]. Tidsskrift for den Norske Lægeforening 2004; 124(16): 2107-2196. (In Norwegian, English summary)
7. Forsdahl A, Grundnes O, Gamnes J, Hagland R, Ytrehus I. Hvor blir Tromsø-legene av? [Where do all the Tromsø doctors go?]. Tidsskrift for den Norske Lægeforening 1988; 108(15): 1225-1230. (In Norwegian)
8. Magnus JH, Tollan A. Rural doctor recruitment: does medical education in rural districts recruit doctors to rural areas? Medical Education 1993; 27: 250-235.
9. Hays RB. Choosing a rural practice career in Queensland. Australian Journal of Rural Health 1995; 3: 171-174
10. Taraldset A. Allmennleger-antall og utvikling 1995-2003 [General Practitioners (in Norway) - numbers and development 1995-2003]. Utposten 2003; 32(4): 34-35.
11. County Medical Officer of Finnmark. Helse- og sosialmeldinger for Finnmark [Annual reports from the County Medical Officer of Finnmark]. (Online) 2010. Available: www.helsetilsynet.no/templates/ArticleWithLinks____6466.aspx (Accessed 30 March 2010) (in Norwegian).
12. Cavender A, Alban M. Compulsory medical service in Ecuador: the physician's perspective. Social Science and Medicine 1998; 47(12): 1937-1946.
13. Dolea C, Stormont L, Shaw DMP, Zurn P, Braichet JM. Increasing access to health workers in remote and rural areas through improved retention. Geneva: WHO, 2009. Available: http://www.who.int/hrh/migration/background_paper.pdf (Accessed 30 March 2010).

