Dear Editor
Pain is a universal human experience, although not every person reacts to painful conditions in the same manner. There is wide acceptance that the ability to perceive painful stimuli is culture-free1; however, abundant clinical, anthropological and epidemiological evidence shows that the expression of clinical pain varies significantly according to cultural and other social factors2,3. Variability in pain experience has important clinical implications.
It is notable that pain is the most common complaint brought to physicians' offices4. In New Zealand, 81.7% of the population reported a pain experience5. Indeed, in a WHO international study, 22% of primary care patients in 14 countries reported persistent pain6. In the USA, pain causes 40 million medical visits annually and costs the country over $100 billion each year in healthcare expenditure and lost productivity7.
Inadequate treatment of pain is highly prevalent and has been well-documented among specific social stratas, age groups, and medical settings, and is particularly notorious among minority groups8. The worldwide neglect of pain has become a clinical, public health and fundamental human rights issue9.
Despite the medical importance of pain and its effects on wellbeing, the way pain is experienced, assessed and managed in rural and remote communities is largely unknown. Indeed, little is known about the pain experience and suffering of the estimated 28 million Indigenous people in the Andes, South America, who are mainly Quichua (Inca). The research aim was to explore how Quichuas in the Andes perceive, describe, and cope with pain.
The Quichua people of the Andes
Of the 28 million Indigenous people in the Andean region of South America10, most live in rural and mountainous regions. The Quichua are an Amerindian nation that once made up a large portion of the Tawantinsuyu, the Inca Confederation, which at its height included present-day Bolivia, Ecuador and Peru, as well as parts of Argentina, Chile and Colombia. In the 16th Century, Spanish armies invaded and subjugated the Confederation and imposed a regime of domination, land dispossession, and serfdom.
In present-day post-colonial Andean countries, there is a caste-like social stratification that marginalizes Indigenous people and supports institutionalized racism11. The ruling Latino group (those of mixed Spanish and Quichua ancestry who identify as 'white-civilized-westerners' and repudiate their Amerindian roots), have replaced the Spaniards as oppressors for the last 200 years. This long-lasting oppression and social exclusion has resulted in scandalously poor health among Indigenous people12 and transformed them into one of the most impoverished and dispossessed groups in the world13.
Methods
An exploratory qualitative/descriptive study was conducted in 1996 with a convenience sample of 40 Quichua adults (15 women and 25 men) in the northern highlands of Ecuador. Data were collected through structured interviews of approximately 3 hours length, using the Quichua questionnaire 'The Nature of Pain' (Nanay Jahua Tapuicuna), which was administered verbally by the researchers.
Results
The Quichua pain experience
The survey results indicate that the Quichuas' pain experience is complex and their strategies to cope with it are sophisticated. Although there are some commonalties with other societies, their pain experience has several remarkable distinctive elements.
The causes of pain: The Quichuas' multifactorial theory of pain causation consists of psychosocial and supernatural notions closely related to their theories of illness and worldview. Negative life events including the loss of loved ones, financial strains, and a failure to maintain good relationships with neighbors, are seen as important in originating illness, disease, and pain. The Quichuas' emphasis on psychosocial pain causes contradicts the view of local Ecuadorian Latino medical practitioners who consider the Quichua explanations of pain to originate from irrational or primitive beliefs (Table 1).
Table 1: The Quichua people's attribution of pain causation
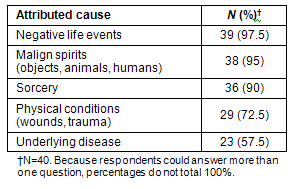
Vulnerability: The Quichua believe that those most prone to suffer from pain are those who are married, elderly, and women. This is consistent with published reports indicating that clinical pain is more prevalent among women and the elderly14,15. Concerns about raising a family and providing for it, educating children, running a business, taking care of domestic animals and cultivating lands were the main reasons for pain cited by married Quichuas. Every day difficulties, life events, and social and interpersonal friction, when severe, can all potentially contribute to the development of illness, disease and pain. Because single people in the Andes usually live with their parents, they are deemed to have no serious responsibilities and are thus considered protected from stresses, and so less susceptible to pain.
Emotions and pain: The role of strong emotional experiences in the origin of psychological or physical illnesses, including pain, is a salient feature, and is probably an ethos of the Quichua people of the Andes. There is strong agreement among them that pain can lead to depression, anxiety, irritability, fearfulness, tiredness, sleep disturbances, poor appetite, a range of serious diseases, and even death.
However, some of their attitudes towards pain could be labeled as stoic. For example, moaning and complaining about pain was considered a sign of weakness by two-thirds of our interviewees. Thinking about or remembering pain is therefore discouraged, because doing so will worsen or trigger the pain. For the extremely impoverished Quichua people of the Andes, 85% of whom live on $2 per day or less, and whose access to medical or psychiatric services is literally non-existent10, complaining about pain with the aim of obtaining medical care is a useless strategy. In rural and remote areas where the majority live, it is in one's interests to learn how to endure pain, or to ask the help of family members or traditional healers. Indeed, 87% responded that they could endure any kind of pain. However, for the health practitioner, usually an outsider, a Quichua patient may look defeated and passive in dealing with pain.
Pathways to care
The pathways to pain care preferred by the Quichua people are inclusive and pluralistic. They strongly embrace biomedicine and physicians as well as Quichua traditional medicine and traditional healers as sources of health care and pain control. Nonetheless, they have a preference for medicinal plants, rather than pharmaceutical products. What also makes them different from Western patients is their acceptance of family members and neighbors as valuable sources of care.
Conclusion
The Quichuas' pain experience is complex and their coping strategies sophisticated. What has been learned from the Quichuas' pain experience could contribute to improving cultural competence in cross-cultural clinical encounters. Indeed, a culturally-sensitive approach to patients could facilitate fruitful negotiations during the formulation of diagnoses, assist patient-doctor communication, and improve the planning of successful pain control strategies16. This will benefit health practitioners seeking to provide high-quality medical care in rural and remote communities worldwide.
Acknowledgement
The study was supported by a doctoral research award granted by Fonds FCAR, Québec, Canada. Many thanks to the Quichua people of Rumipamba in Imbabura, Ecuador for their support and participation. The authors' deepest gratitude goes to the late Mr Alberto Cacuango, a remarkable community leader and field research assistant, for his unconditional support of this study and his friendship. The authors thank Sioui Maldonado Bouchard for her assistance in reviewing English language usage.
Mario Incayawar1, MD, DESS, MSc and Jean-François Saucier2, MD, PhD
1Runajambi - Institute for the Study of Quichua Culture and Health
Otavalo, Ecuador
2Department of Psychiatry, Université de Montréal
Montreal, Canada
References
1. Zatzick DF, Dimsdale JE. Cultural variations in response to painful stimuli. Psychosomatic Medicine 1990; 52(5): 544-557.
2. Bates MS. Biocultural dimensions of chronic pain - implications for treatment of multi-ethnic populations. Albany, NY: State University of New York Press, 1996.
3. Good MJD. Pain as human experience - an anthropological perspective. Berkeley, CA: University of California Press, 1994.
4. Osterweis M, Kleinman A, Mechanic D. Pain and disability - clinical, behavioral, and public policy perspectives. Washington, DC: National Academy Press, 1987.
5. James FR, Large RG, Bushnell JA, Wells JE. Epidemiology of pain in New Zealand. Pain 1991; 44(3): 279-283.
6. Gureje O, Von Korff M, Simon GE, Gater R. Persistent pain and well-being: a World Health Organization study in primary care. JAMA 1998; 280(2): 147-151.
7. US Department of Health and Human Services, Management of Cancer Pain Guideline Panel, United States, Agency for Health Care Policy and Research. Management of cancer pain, no. 94-0592. Rockville, MD: US Department of Health and Human Services, Public Health Service, Agency for Health Care Policy and Research, 1994.
8. Todd KH, Samaroo N, Hoffman JR. Ethnicity as a risk factor for inadequate emergency department analgesia. JAMA 1993; 269(12): 1537-1539.
9. Brennan F, Carr DB, Cousins M. Pain management: a fundamental human right. Anesthesia and Analgesia 2007; 105(1): 205-221.
10. Incayawar M. Indigenous peoples of South America - inequalities in mental health care. In: K Bhui, D Bhugra (Eds). Culture and mental health - a comprehensive textbook. London, UK: Hodder and Arnold, 2007; 185-190.
11. Casagrande JB. Strategies for survival: the Indians of highland Ecuador. In: NE Whitten Jr (Ed.). Cultural transformations and ethnicity in modern Ecuador. Urbana, IL: University of Illinois Press, 1981; 260-277.
12. Incayawar M, Maldonado-Bouchard S. The forsaken mental health of the Indigenous Peoples - a moral case of outrageous exclusion in Latin America. BMC International Health and Human Rights 2009; 9(1): 27.
13. Berger TR. A long and terrible shadow - white values, native rights in the Americas, 1492-1992. Vancouver: Douglas & McIntyre, 1991.
14. Elliott AM, Smith BH, Penny KI, Smith WC, Chambers WA. The epidemiology of chronic pain in the community. Lancet 1999; 354(9186): 1248-1252.
15. Wilson JF. The pain divide between men and women. Annals of Internal Medicine 2006; 144(6): 461-464.
16. Kleinman A. Culture, illness, and care: clinical lessons from anthropological and cross-cultural research. Annals of Internal Medicine 1978; 88: 251-258.

