Globally, educators in higher education are using distance education more and more as an education approach1-4. The advantages of distance education are that it makes education available to students in remote areas and to those with family or work commitments that prohibit attendance at extended on-site education programs2,3,5,6.
Graduates of Christian Medical College (CMC), Vellore, India, have a 2-year service obligation to work in small hospitals mainly located in rural areas. The Fellowship in Secondary Hospital Medicine (FSHM) program is a year-long blended on-site and distance learning program, designed by CMC to support its graduates working in such hospitals7. CMC aspired through the FSHM program, designed as a blend of distance learning modules, contact sessions, project work and networking, to provide educational opportunities for these junior doctors working in geographically remote areas.
The purpose of this paper is to present a description and evaluation of the combined role in the program of the distance learning modules, structured for active learning, and the contact sessions, to develop knowledge and skills for these junior doctors to practice effectively in rural hospitals in India. The role of project work and networking is important and will be addressed in another publication7,8.
FSHM setting and description
Medical graduates in India: Medical graduates in India obtain the MBBS degree (equivalent to a US MD degree) after five and a half years of medical training, which includes a 1-year rotating internship. These MBBS graduates would be a junior doctor in India. They can practice as a general practitioner after registration with the Medical Council of India9.
Secondary hospitals: Graduates of CMC, a tertiary care center, have a 2-year service obligation to work in secondary hospitals, which are small hospitals mainly located in rural areas7. These hospitals have between 20 and 200 beds, with a generalist practice of medicine, surgery, pediatrics, and obstetrics and gynecology; limited laboratory support; and local community-based programs such as antenatal care and tuberculosis programs. These graduates face many challenges while working in these hospitals, such as lack of academic and social support and academic isolation7,10. Other challenging factors include the type of knowledge and skills required to practice at secondary hospitals (eg providing effective patient management with limited laboratory support); the type of cases seen in secondary hospitals which depends on the prevalence of disease patterns in the area where the secondary hospital was located, (eg kala-azar (leishmaniasis) in Bihar, falciparum malaria in the east and north-east, and sickle cell disease in the tribal belts11-13). Graduates also faced difficulties in following standard guidelines for treatment because of limited patient economic resources, limited lab support, and limited/lack of referral support. Most of these graduates choose not to work in these smaller hospitals after their service obligation. Many such hospitals are closing because of lack of staff10,14. This is affecting the health care of the nation, especially in rural areas where these hospitals are located.
Lack of rural physicians is a global problem15,16. Providing rural physicians with academic and social support has been suggested as a measure for retention of a rural health workforce15,17,18. CMC aspired, through the FSHM program, to provide support to these junior doctors working in rural hospitals and help them develop the knowledge and skills to practice effectively in their hospitals. What these junior doctors learned through the FSHM program could be applicable to rural hospitals similar to the ones in which they were placed for their service obligation.
FSHM program: Distance education has been successful in providing such educational opportunities to students located in geographically remote areas3. However, distance learning needs to be adequately supported with supervised clinical work for knowledge to be translated into practice19. Other challenges of distance learning are providing adequate interaction among students and between faculty and students; and the high dropout rate20,21. Thus, the FSHM program was designed by CMC as a blend of 15 paper-based distance learning modules focused on providing the academic resources to develop knowledge to practice in rural hospitals; three contact sessions at CMC, which focused on developing the necessary skills; project work focused on improving local health services; and networking between peers and with faculty to provide academic and social support and reduce potential isolation.
Distance learning modules: The purpose of the 15 modules was to help students develop the knowledge to practice at secondary hospitals in the following areas: anesthesia for obstetric emergencies; ear, nose and throat problems; infectious diseases, neonatology; nephrology; neurology; obstetric ambulatory care; obstetric emergency care; ophthalmology; orthopedics; pediatrics; primary trauma care; respiratory/tuberculosis; surgery; and toxicology.
Each module included an introduction, learning activities with feedback, readings, tutor graded assignments, references and a feedback form to be completed by the student. The modules also provided patient management protocols, algorithms, relevant X-rays and other appropriate images such as CT scan. Modules were designed to promote active learning by students reflecting on practice, with support and feedback by tutors. The time required for each module was 4 hours per week for 2 weeks. The distance learning modules were developed using the Open University (OU) UK distance learning approach, which emphasizes active learning and feedback22. An example of a module on infectious disease is provided in Appendix I. These were paper-based printed modules sent to the junior doctors at their rural hospitals by postal service.
Contact sessions: The purpose of the contact sessions was skills building, student support and networking. Clinical skill development was in the following areas: acute trauma care; critical care; dermatology; ear, nose and throat; general medicine; microbiology; neonatology; obstetrics and gynecology; orthopedics; pathology; pediatrics; plastic surgery; rheumatology; radiology; and surgery. The first contact session was at the beginning of the FSHM program, the second was in the middle and the third was at the end. The first two contact sessions were 1 week in duration, while the third was 3 days long.
The FSHM students were graduates with MBBS degrees and were thus licensed to practice. They were already trained in certain skills to enable them to practice. However, based on the needs assessment for the FSHM program, certain specific skills were identified to be important, some of which needed reinforcement, such as cardiopulmonary resuscitation, while other skills such as neonatology resuscitation needed to be taught. These skills were addressed in the contact sessions. Students were assessed in the FSHM program on the tutor-graded assignment at the end of each module and with a final examination, which included multiple-choice questions and an objective structured clinical examination.
Faculty development was integral for development of distance learning modules and for teaching in the contact sessions. Evaluation of the distance learning modules and contact sessions was conducted both for accountability and improvement23.
Evaluation methods
Evaluation of the distance learning modules, supported with contact sessions, was done using mixed methods, a combination of qualitative and quantitative approaches with a major focus on the qualitative approach, using two written surveys with students and faculty and one focus group discussion with students. The FSHM students for 2007-2008 and 2008-2009, and faculty members for the FSHM program, were included in the evaluation study. The evaluation was done after 2 years of implementation of the year-long FSHM program.
Written surveys: Two written surveys were administered, one to all FSHM students (n=16) for 2008-2009 after they were awarded the fellowship and one to faculty (from CMC and secondary hospitals) (n=34). The surveys included structured questions that yielded quantitative data as well as open-ended questions that yielded comments. The structured questions focused on rating the effectiveness of the distance learning modules and contact sessions in developing the knowledge and skills to practice in secondary hospitals. The open-ended questions were used to obtain views of students and faculty regarding strengths of the distance learning modules and contact sessions, and recommendations for improvement.
Focus group: One focus group was conducted with 2008-2009 students (n=7) at the end of the program. The students were selected by the authors to represent genders, different secondary hospitals and different states of the country. The purpose of the focus group was to explore, through open-ended questions, the effectiveness of the distance learning modules and contact sessions and to collect qualitative data to provide a rich portrayal of the benefits of the program and recommendations for change.
Data analysis
Quantitative data analysis was done using the Statistical Package for the Social Sciences v11 (SPSS; http://www.spss.com) and is reported as frequency distributions. Qualitative data analysis was done through inductive content analysis as described earlier7.
Evidence for validity of surveys was gathered as described in an earlier paper24. To help ensure validity of the qualitative data analysis, triangulation, member check, thick description and audit trail, as recommended by Barzansky et al25, was used as previously described7.
Ethics approval
Institutional approval was obtained from the Christian Medical College-Vellore, for design and evaluation of a curriculum, consistent with CMC policies. Institutional Review Board approval was also obtained from the review board at the University of Illinois-Chicago (UIC), where the first author did this project, in partial completion of her Masters of Health Professions Education (MHPE) leadership degree. The approval number was 2009-0579 from the Office for the Protection of Research Subjects, UIC, Chicago.
Results
All 16 students of the 2008-2009 class completed the survey. Of 45 faculty involved with the program, 34 completed the survey (response rate, 76%). After discussion between reviewers, 100% agreement was reached for themes, and comments were assigned to themes for all data.
The quantitative and qualitative data reported below is summarized in Table 1 and Table 2 respectively.
Table 1: Quantitative data of student and faculty responses to survey questions regarding effectiveness of distance learning modules and contact sessions
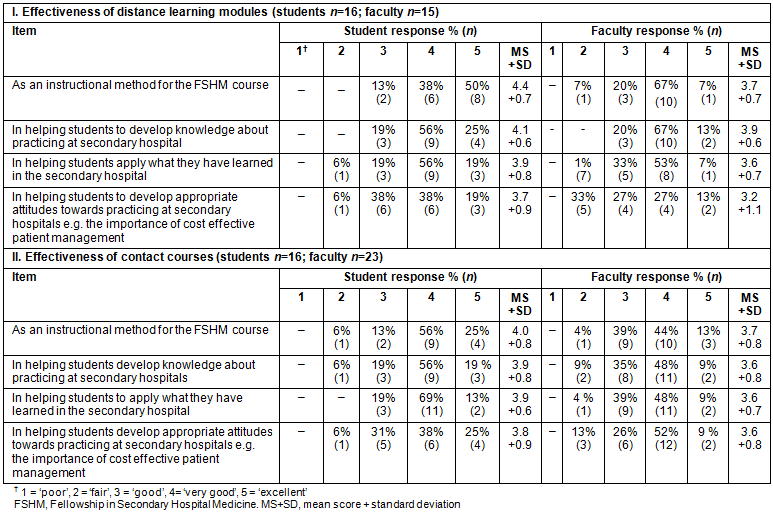
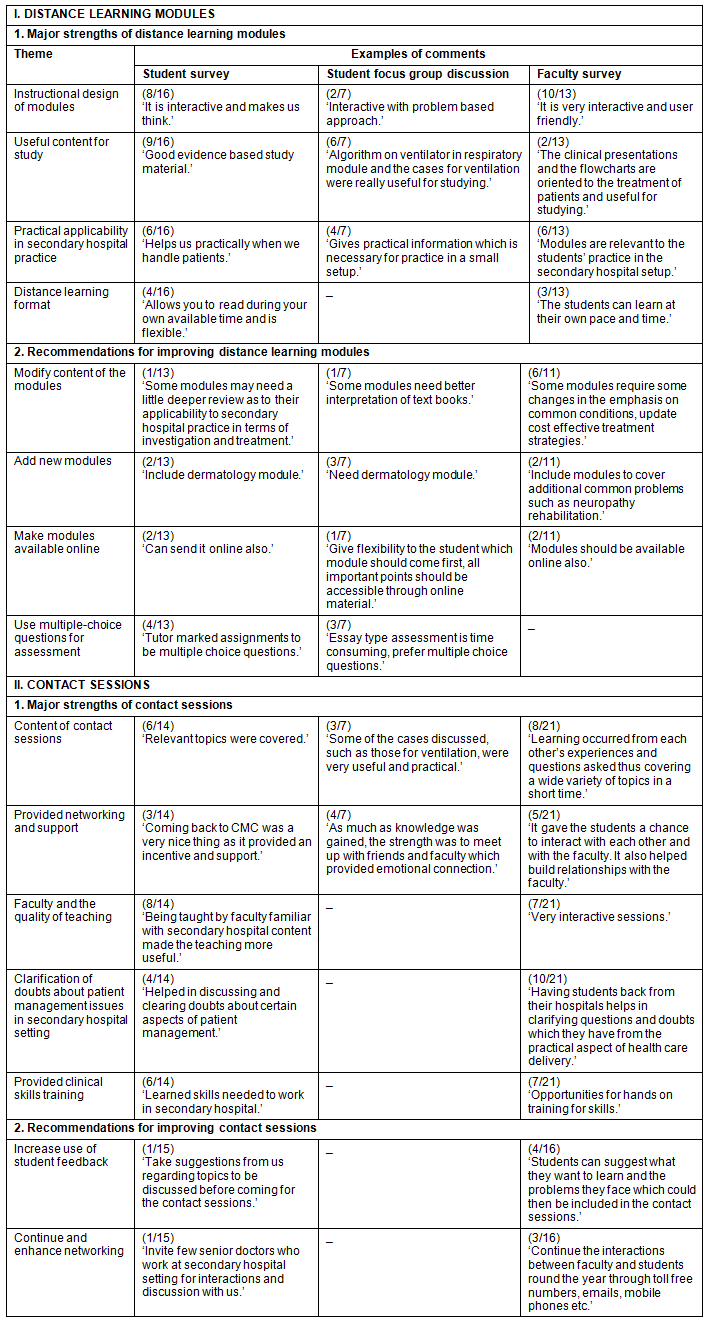
Table 2: Qualitative data analysis of comments from students and faculty to open-ended questions in survey and focus group discussion
Distance learning modules
The vast majority of students (81%) and faculty (80%) rated the distance learning modules as 'very good'/'excellent' in helping students develop the knowledge to practice in secondary hospitals.
Major themes identified in student and faculty responses to the open-ended questions about strengths of the distance learning modules, from greatest to least frequency, were instructional design, which was interactive, user friendly and made students think; useful content with practical applicability in secondary hospitals; and distance learning format providing flexibility and accessibility. Recommendations for improvement were to modify the content of modules to provide a deeper review; add new modules such as a module on dermatology; make modules available online; and use multiple-choice questions for assessment rather than essay questions.
All seven focus group members commented that the distance learning modules helped them in providing patient care in their day-to-day practice. One student commented, 'We would have read something in the module; then you see cases and can remember what you need'. Focus group participants gave various examples of cases they could manage because of what they learned in the distance learning modules, such as providing cost-effective management of patients with dog bite and typhoid, pediatric nephrotic syndrome, tetanus, organophosphorus poisoning and HIV; management of patients presenting with ectopic pregnancy; and giving anesthesia for cesarean sections.
Contact sessions
Most students (88%) and faculty (87%) rated the contact sessions 'good'/'very good' in helping students to apply what they have learned in secondary hospitals.
Major themes identified from student and faculty responses to open-ended questions on strengths of contact sessions, from greatest to least frequency, were content of contact sessions that was useful and practical; provided networking and support; clarification of doubts regarding patient management issues in secondary hospital settings; and provided clinical skills training.
Recommendations for improvement were increase use of students' feedback to improve the contact sessions and continue and enhance networking.
All seven students in the focus group commented that the contact sessions had been useful for them in providing patient care. Participants gave examples of specific skills learned in contact sessions that they were able to use in their secondary hospitals, such as starting an intra-osseous line for children, performing an emergency cricothyroidectomy, interpretation of electrocardiograms, managing patients with cardiac problems, providing basic life support to patients brought to the emergency room, doing intra-articular taps, and performing neonatal resuscitation.
This evaluation study provides evidence that the distance learning modules, supported by contact sessions, helped junior doctors develop the knowledge and skills to practice effectively in rural hospitals in India, based on the perspectives of the students and the faculty. The junior doctors felt that the blended program helped them to provide improved patient care and they gave specific examples of cases they could manage after going through the program.
Based on suggestions made, the distance learning modules have been reviewed and updated; new modules have been included. In addition, the FSHM program has been created on CMC's learning management system, through which the students can access resource materials. This is currently being developed for mobile phone use and being pilot tested by FSHM students to enable them to access information in time and on the go26.
A limitation of this study is that evaluation of outcomes is based on self-reports by students and faculty. Nevertheless, this study reflects the perspectives of two groups, students and faculty, using multiple methods of data collection, with consistent results among the two groups and data collection methods.
The advantages of distance learning are its accessibility, flexibility and availability as a lasting resource3,5. This is reflected from this study in which the identified strengths of the distance learning modules were accessibility, flexibility and use as an academic resource. Active learning with feedback maximizes the learning experience27,28, which is emphasized in these distance learning modules. Distance learning modules, combined with contact sessions, provide supervised skills training for providing effective patient care in hospitals19 and provides both academic and social support for the students5. This is reflected in this study's results, showing that the 15 paper-based distance learning modules, supported with three contact sessions, which provided academic and social support, enabled the students to provide effective patient care in their rural hospitals.
The next step in program evaluation would be to ask when the blended education works and when does it not. A scientifically rigorous evaluation research would be critical to provide evidence for contribution of the blended education towards retention of doctors in rural hospitals and improved community health.
The authors would thus suggest using carefully prepared distance learning modules, supported with contact sessions, for supporting junior doctors and enabling them to practice effectively in rural hospitals.
Acknowledgement
The authors thank the FSHM students and faculty for their participation and CMC Vellore for supporting the study. Thanks to Janet Grant, Open University UK, for setting up the distance learning program and FAIMER (Foundation for Advancement of International Medical Education and Research) for awarding the IFME (International Fellowship in Medical Education) Fellowship to one of the authors, which enabled the author to undertake this study as part of the thesis work for the MHPE (Masters in Health Professions Education) program at UIC, Chicago.
References
1. Treloar CJ. Evaluation of a national and international distance education program in clinical epidemiology. Medical Education 1998; 32: 70-75.
2. Sargeant JM, Purdy RA, Allen MJ, Nadkarni S, Watton L, O'Brien P. Evaluation of a CME problem-based learning internet discussion. Academic Medicine 2000; 75: S50-52.
3. Grimes EB. Use of distance education in dental hygiene programs. Journal of Dental Education 2002; 66: 1136-1145.
4. Le TT, Rait MA, Jarlsberg LG, Eid NS, Cabana MD. A randomized controlled trial to evaluate the effectiveness of a distance asthma-learning program for pediatricians. Journal of Asthma 2010; 47: 245-250.
5. Stanton F, Grant J. Approaches to experiential learning, course delivery and validation in medicine. A background document. Medical Education 1999; 33: 282-297.
6. Cravener PA. Faculty experiences with providing online courses. Thorns among the roses. Computers in Nursing 1999; 17: 42-47.
7. Vyas R, Zachariah A, Swamidasan I, Doris P, Harris I. Integration of academic learning and service development through guided projects for rural practitioners in India. Medical Teacher 2011; 33: e401-e407.
8. Vyas R, Zachariah A, Swamidasan I, Doris P, Harris I. A networking approach to reduce academic and social isolation for junior doctors working in rural hospitals in India. Education for Health 2012; 25(1): 70-74.
9. Biswas R, Sarkar N, Umakanth S, Singsit J, Hande M. Medical education and the physician workforce of India. Journal of Continuing Education in the Health Professions 2007; 27: 103-104.
10. Zachariah A. Secondary hospitals. Project for Foundation for Advancement of International Medical Education and Research (FAIMER) Institute, 2000.
11. Kate S. Health problems of tribal population groups from the state of Maharashtra. (Online) 2000. Available: http://sickle.bwh.harvard.edu/india_scd.html (Accessed 10 July 2012).
12. Director General of Health Services Ministry of Health and Family Welfare Government of India. National vector borne disease control programme. (Online) 2007. Available: http://nvbdcp.gov.in/kala-azar.html (Accessed 10 July 2012).
13. Kakkilaya BS. Malaria in India. (Online) 2012. Available: http://www.malariasite.com/malaria/MalariaInIndia.htm (Accessed 21 February 2014).
14. Mullan F. Doctors for the world: Indian physician emigration. Health Affairs (Millwood) 2006; 25: 380-393.
15. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 21 February 2014).
16. Pathman DE, Konrad TR, Ricketts TC. Medical education and the retention of rural physicians. Health Services Research 1994; 29: 39-58.
17. Curran V, Rourke J. The role of medical education in the recruitment and retention of rural physicians. Medical Teacher 2004; 26: 265-272.
18. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9: 1083. (Online) 2009. Available: www.rrh.org.au (Accessed 21 February 2014).
19. Sanders J. Distance education: can it go the distance? Imprint 2007; 54(5): 33-34.
20. Butterworth K, Hayes B, Zimmerman M. Remote and rural: do mentors enhance the value of distance learning continuing medical education? Education for Health (Abingdon) 2011; 24(3): 539.
21. Grimes EB. Use of distance education in dental hygiene programs. Journal of Dental Education 2002; 66(10): 1136-1145.
22. Grant J. 2002. Guidelines for producing a distance-learning course. (Unpublished).
23. Fitzpatrick JL, Sanders JR, Worthen BR. Program evaluation. Alternative approaches and guidelines. Boston: Pearson Education, 2002.
24. Vyas R, Tharion E, Satishkumar S. Improving the effectiveness of physiology record books as a learning tool for first-year medical students in India. Advances in Physiological Education 2009; 33: 329-334.
25. Barzansky B, Berner E, Beckman CR. Evaluation of a clinical program. Applying the concept of trustworthiness. Evaluation and the Health Professions 1985; 8: 193-208.
26. Vyas R, Albright S, Walker D, Zachariah A, Lee M. Clinical training at remote sites using mobile technology: an India-USA partnership. Distance Education 2010; 31(2): 211-226.
27. King A. From sage on the stage to guide on the side. College Teaching 1993; 41: 30-35.
28. Bransford J, Brown A, Cocking R. How people learn: brain, mind, experience and school. Washington, DC: National Academies, 2000.
_____________________
Appendix I: Sample of the distance learning module on infectious disease from the Fellowship in Secondary Hospital Medicine program.

