Introduction
The nature of health service delivery and the experience of practising health professionals can vary in rural communities1. The rural physiotherapist is faced with unique challenges, different from an urban physiotherapist2-7. These challenges become more apparent when there is a need for the rural physiotherapist to extend their skills and knowledge to areas typically covered by a specialist physiotherapist. An example of this is when a rural physiotherapist is required to treat paediatric cases who, in an urban setting, would normally be seen by a specialist paediatric physiotherapist1-4,6-10. The effects of working in challenging conditions on the physiotherapist's confidence and belief in themselves to fulfil these demands are unknown.
Self-efficacy is the central component of the social learning theory conceptualised by Albert Bandura in 197710,11. The belief of self-efficacy is defined as 'a person's judgement of their capabilities to organise and execute designated courses of action required to attain designated levels of performance' (p.391)12. Bandura's key contentions with regards to the role of self-efficacy beliefs in human functioning is that 'people's level of motivation, affective states, and actions are based more on what they believe than on what is objectively true' (p.2)13.
Pajares found that human functioning is influenced by many factors, especially as the success or failure experienced as people engage in the myriad tasks that comprise their life naturally influences the decisions they make14. The knowledge and skills they possess play critical roles in what they choose to do and not do13,14. Individuals interpret the results of their attainments, just as they make judgments about the quality of the knowledge and skills they posses, hence allowing self-efficacy beliefs to also be seen as 'the confidence that people have in their ability to do the things they try to do' (p.3)14. Self-efficacy is assessed by asking individuals to report the level, generality, and strength of their confidence to accomplish a task or succeed in a certain situation14,15,16.
The availability of other health professionals to the rural physiotherapist becomes crucial to the physiotherapist's service delivery, professional support and interdisciplinary interaction. When considering Bandura's theory, in the case of a rural physiotherapist, low self-efficacy is possible because they face daily challenges and setbacks secondary to a lack of support, resources and services3,6,17,18. Physiotherapists working in such a demanding, poorly structured and unsupported environment are expected to have low levels of belief in their abilities, and poor coping strategies, thus causing them to develop low self-efficacy beliefs19,20. The clinical implications remain unclear. However it has been documented that physiotherapists suffer burnout when working in rural areas3,4,7,19-21.
Williams et al identified the challenges of working in a rural area as the lack of a career path, career development and specialisation7. A specialist physiotherapist is one who has achieved a required standard of practical, theoretical expertise and competence in a required area of special need or interest within a recognised area of physiotherapy 22-25. Professional acknowledgement identifies to other health professionals and to employers that the physiotherapist with specialist qualifications is one with advanced clinical competence who is up-to-date with current research and evidence-based practice in their field of work22,26,27. Career choice and development is an example of the power of self-efficacy to affect the course of life paths through choice-related processes28. The higher the level of the individual's self-efficacy, the wider the range of career options they seriously consider, the greater their interest in them, and the better they prepare themselves educationally for the occupational pursuits they choose, therefore resulting in greater success28. However, in the case of the physiotherapist working in a rural area, secondary to poor workforce structure and lack of support, the career option of specialisation is not considered achievable.
Rural physiotherapy is considered as a separate discipline of physiotherapy; however, the specialisation process of the rural physiotherapist is relatively new and is still undergoing institutional changes2,3,5-7,17,25,27,29. Paediatrics was chosen as an example of a specialist caseload because current paediatric rural services are fragmented, with access to care that is comprehensive and responsive to client's needs being difficult due to waiting lists and the need to travel limiting timely appropriate services30. Moreover, in rural areas where 85% of the physiotherapists were considered to be a generalist physiotherapist, paediatrics often contributed to a large majority (34%) of the caseload18. Roles for physiotherapy that extend the boundaries of scope of practice are often adopted out of necessity to solve service delivery and workforce problems31. However, the Australian Physiotherapy Association (APA) Code of Conduct and the Physiotherapists Board of Queensland (PBQ) Code of Practice, both share the view that a physiotherapist should avoid practising outside their scope of practice in an area in which they have poor confidence32,33. More specifically, the Code of Conduct highlights32:
APA members shall define their scope of practice according to current knowledge and competency standards, shall practice in a careful, honest and accountable manner and shall accept responsibility for the exercise of sound judgment. (p.2)
The APA and the PBQ share the view that a physiotherapist with low confidence in a clinical field outside their scope of practice, should refer on to a more suitably qualified practitioner with more experience32,33. However if the alternative is to not offer the service, going without the service also poses a risk because the potential for various therapeutic approaches may be missed by generalist rural physiotherapists. This may result in reduced functional independence and the emergence of secondary conditions or complications for the patient34,35. In turn, the physiotherapist is then faced with a professional dilemma: whether to treat outside their scope of practice in an area in which they do not feel competent. This can result in sub-standard and inadequate treatment, or treatment refusal due to a lack of skills; which in turn may lead to lack of self-efficacy beliefs, causing conflict with the code of ethics and giving rise to professional conduct issues32.
The purpose of this study was to measure the self-efficacy of physiotherapists working in rural settings, who undertake service delivery in the field of paediatrics among their normal caseload. The study also aimed to explore the possible existence of a lack of self-efficacy in the rural physiotherapy cohort as well as identify any contributing factors. It was hypothesised that low self-efficacy and confidence exists among generalist rural physiotherapists undertaking specialist paediatrics caseloads.
Methods
Design and subjects
This study was of descriptive, cross-sectional design. The target population was a sample of physiotherapists working in the north Queensland region of Australia, within a boundary extending north of and including Mackay, to the western border of Queensland. The inclusion criteria was physiotherapists working in areas with an Accessibility/ Remoteness Index of Australia (ARIA) classification providing four classes of 'moderately accessible', 'remote' or 'very remote'. The ARIA index score is based on the road distance from the closest service centres in each of these 4 classes. North Queensland was chosen due to its vast distances and the area's inclusion of the 4 ARIA classes, providing diversity.
The study inclusion criteria extended to physiotherapists who undertake specialist clinical caseloads where paediatric cases contribute to this caseload. The second criterion was later amended because it was difficult to determine, due to there being no record of specialist paediatric physiotherapists working in a rural area. It was also difficult to define where paediatric cases contributed to the case load because most rural physiotherapists work as a generalist and experience a wide variety of clientele in their caseload2-7,17.
Compiling the mailing list
The addresses of rural physiotherapists were obtained through the James Cook University (JCU) Physiotherapy contact database, as well as through a general search of the Yellow Pages® telephone directory. This was cross-checked against the APA's 'Find a Physio' website. There was considerable difficulty in obtaining an accurate database because contact details were often not updated to reflect an accurate picture of those physiotherapists working in a rural area. This can be attributed to high staff turnover and attrition in rural areas2-7,17. To comply with ethics requirements, once a contact number was obtained, the workplace was then contacted to obtain names of the physiotherapists currently working there, to ensure accuracy when addressing the envelopes. Physiotherapists are required to be registered to practise. However as the registration list may not accurately reflect work address and permission was not achieved to access the registration list filtered by postcode, this was not further pursued. Therefore, a sample size could not be determined with accuracy. The vast distances of the study area and the mobility of the workforce precluded face-to-face interviews. James Cook University Human Resource Ethics Committee provided ethical approval.
Questionnaire development
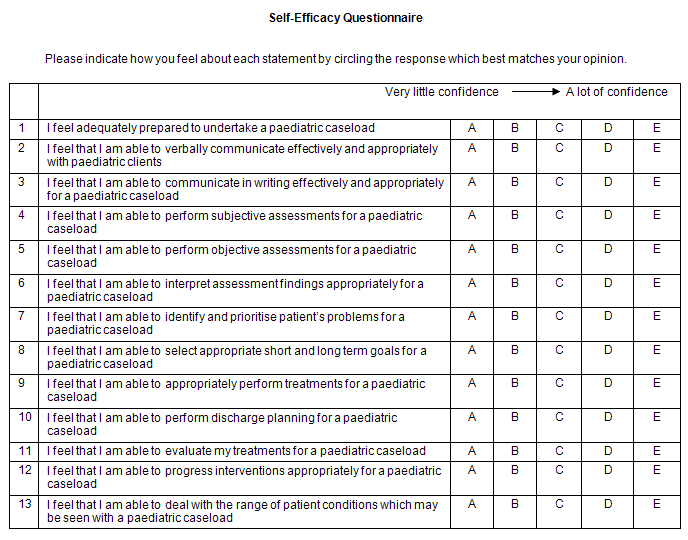
The questionnaire was designed in two parts and included 13 items specific to tasks undertaken in a paediatric physiotherapy practice domain (Appendix I). The first part was to obtain demographic and background details of the physiotherapist participant, while the second part was to obtain a quantitative picture of the self-efficacy scores of the participants with regards to working with paediatric caseloads. Self-efficacy was measured on a 5 point Likert scale ('very little confidence' to 'a lot of confidence'). Pajares has demonstrated that researchers assess self-efficacy beliefs by asking individuals to report the level, generality, and strength of their confidence to accomplish a task or succeed in a certain situation16. The self-efficacy questionnaire used was slightly modified from a previous JCU research project and is based on the ideas of Pajares, which determine that self-efficacy should be measured in terms of personal judgments of capability that vary across a realm of activity, different levels of task demands and under different circumstances, so as to not result in a generalised or global measurement16.
Data were collected over a 12 week period. Initially, 19 completed questionnaires were returned. Nine questionnaires were returned marked 'not at this address/return to sender'. A second mail-out of questionnaires was conducted to those who had not returned the questionnaire. A further 5 completed questionnaires were returned, with one marked 'not at this address/return to sender'. In total, 23 completed questionnaires were returned providing an overall response rate of 41% (23 of 56).
Validity and reliability
Traditionally self-efficacy has been measured by asking a yes/no-answer question about whether a person can perform at specific task to a certain level. The person is then asked to rate how confident they feel (as a percentage) in performing the task to the level indicated. Maurer and Pierce conducted a study which aimed to address whether a Likert-type measurement can be used as an alternative to this traditional measurement of self-efficacy36. The results indicated that Likert-type and traditional measures of self-efficacy have similar reliability-error variance, provide equivalent levels of prediction, and have similar factor structure and similar discriminability36. Overall, considering both practicality and the apparent similarity of empirical results using the two methods, a Likert scale offered an acceptable alternative method of measuring self-efficacy36. Maurer and Andrews compared three methods of measuring self-efficacy37. The three methods included traditional, Likert, and a simplified scale. Scores on the three scales had highly similar reliability and validity and were strongly related37. The Likert scale required 50% fewer participant responses than the traditional format, and provided more specific diagnostic information in line with the traditional method of measuring self-efficacy37. Robson and Neuman both agreed that the simplicity and ease of use of the Likert scale is its real strength38,39. The study does acknowledge the limitations of using this scale, especially as the scale may reveal little about the causes for answers. However, Dyer determined that attitude scales do not need to be factually accurate, they simply need to reflect one possible perception of the truth40. Dyer further demonstrated that respondents will not be assessing the factual accuracy of each item, but will be responding to the feelings which the statement triggers in them41.
Data analysis
Responses were coded according to common responses within each questionnaire. The format of these responses utilised a variety of levels of measurement including nominal data (non-numerical variables such as age or place of work) and ordinal data (within the Likert scale). Once coded, the data were analysed using SPSS v17 software (www.spss.com), using descriptive statistics and cross tabs to determine and compare relationships among variables.
Results and Discussion
The respondents were 56.5% female (n= 13) and 43.5% male (n= 10). The age of physiotherapists practising in rural locations ranged from 18 to ≥65 years. The age range distribution fell predominantly between 35 and 54 years.
Work practices
To explore work practices, information was obtained from respondents on the work setting, location in area of distribution, employment status, role description and duration of employment since graduation and in their current job. Ten respondents (44%) worked in a hospital, 11 (48%) worked in private practice, and two (9%) worked in a community health setting. None of the respondents reported working in outreach.
In agreement with past research, rural physiotherapy practice is more likely to involve a sole position (n=16, 70%), or one of a small group of clinicians (n=7, 30%)2-7,17. Eight respondents reported working in their current job for ≥10 years. Two respondents reported having worked ≥20 years since graduation in their current job. Of the 64% of respondents who reported working less than 10 years in their current job, the majority (36%) reported working 6-12 months, and 3-5 years, respectively (18%). The majority of respondents (65%) stated having a Bachelor Degree in Physiotherapy as their highest qualification.
The majority of respondents working in a small multi-disciplinary team demonstrated low self-efficacy when working with a paediatric caseload. This could be attributed to the keys issues identified by Wilson et al as those affecting the work ethic of rural physiotherapists35. Recruitment, retention, and lack of resources were identified, as was inadequate staffing35. Struber complements this, revealing the rural physiotherapy cohort to be a complex workforce that is fragmented by part-time work, multiple workplaces, and overlay within the public and private sector41. However, of the study participants, 78% worked full time compared with 22% who worked part time. Moreover, new graduates frequently fill vacancies and it is imperative that they develop advanced skills across a broad range of clinical and management areas very quickly4. In turn, Bent highlighted that such a position is not suitable for new graduates, despite their recruitment and, as such, the APA has found that many of the physiotherapists currently working in rural areas are inexperienced and lack the diversity of skills necessary to cope in such a demanding environment4. It may be that because of this lack of experience and necessary skills, these physiotherapists might have rated their self-efficacy as quite low.
In the questionnaire, the majority of respondents reported having worked ≥20 years since graduation; however, they still reported low levels of self-efficacy beliefs when working with paediatrics caseloads across all domains of the questionnaire, despite their wide experience. Logical arguments for this could be attributed to those issues identified by Struber41 of poor utilisation of professional development (PD) demonstrated among participants.
The majority of respondents reported undertaking further training and PD in musculoskeletal studies (30%), followed by neurological rehabilitation (13%), 4% each in cardiorespiratory, intensive care and alternative therapy, and 26% reporting further training in two or more of these areas. Four respondents (17%) reported undertaking no further training or PD at all, yet given the breadth of clinical areas and advances in physiotherapy this is surprising2-7,42. The APA introduced a compulsory system of continuing professional development (CPD) for all members in January 1999 in response to this issue43. However, the downfall of this strategy was that APA membership is not compulsory43. Because membership of the APA status was not collected in the questionnaire, the implications of this on the sample are unknown. Recently, the Australian Health Workforce Ministerial Council reached a consensus in the implementation of a national registration and accreditation scheme for health professionals in Australia44. The national scheme introduced from 1 July 2010 included requirements that registrants show participation in CPD activities in order for their registration to be renewed44. At present, the PD required to further develop skills unique to a specialist area of physiotherapy involves high cost and travel to major centres, where the PD available is usually metropolitan in context, rather than rural18.
Rural practice has been identified as being a distinct discipline, because physiotherapists working in rural locations are considered to be generalists who manage a broad range of clinical conditions across the age spectrum2-7,17. Therefore, the physiotherapist conducts an appropriate initial assessments of clients across the lifespan, establishes problem lists and employs collaborative goal setting. The study demonstrated that across the entire questionnaire (n=23), an average of 9 (of 16 sole practitioners), and an average of 6 (of 7) practitioners who work in a small group of clinicians were rated as having neutral and below levels of confidence concerning these components of initial assessment.
When asked if they felt adequately prepared to undertake a paediatric caseload, in the responses to self-efficacy question (SEQ) 1 the majority (74%) of respondents reported neutral levels of confidence and below. Similarly, 94% of the respondents with no further training or PD in paediatrics reported neutral levels of confidence and below. When asked if they felt able to appropriately perform treatments for a paediatric caseload (SEQ 9) the majority of respondents (65%) reported neutral levels of confidence and below. The lack of self-efficacy beliefs demonstrated concerning treatment of a paediatric client is well justified, because it has been established that the physiotherapist undertaking a paediatric clinical caseload requires specialist knowledge when treating a child or adolescent42,45. When asked if able to progress interventions appropriately for a paediatric caseload, the majority of respondents (78%) reported neutral levels of confidence and below. However, more concerning is that in contrast those respondents who have had further experience, 50% reported having neutral levels of confidence and below. This may reflect a need to travel to major centres to further develop skills unique to a specialised area of physiotherapy, and the PD available is usually metropolitan in context, rather than rural18. This raises the question of whether current PD and training in the area of paediatrics is appropriate and applicable to a rural context.
When asked if they felt able to perform discharge planning for a paediatric caseload ( SEQ10) the majority of respondents reported neutral levels of confidence and below (74%). The majority (74%) of respondents reported neutral levels of confidence and below with regard to preparation to undertake paediatric caseloads. Similarly, 94% of the respondents with no further training or PD in paediatrics reported neutral levels of confidence and below. This reflects current practice in paediatrics where discharge is often more complex than for adults because it involves greater need for a holistic approach that encompasses the child, the family and the natural setting in which the child lives, learns and plays46. Similarly, 94% of the respondents with no further training or PD in paediatrics reported neutral levels of confidence and below. This is generally reflected in current research. Battye and McTaggart found that most allied health professionals recruited for rural areas are dissatisfied with their preparation and workload3. In such circumstances, a high level of support is needed for those practising in rural areas, especially when the physiotherapist lacks experience and the diverse clinical skills needed to successfully practise in a rural area3,4,18.
When asked if able to progress interventions appropriately for a paediatric caseload (SEQ12), the majority of respondents (78.2%) reported neutral levels of confidence and below. Similarly, 88% of the respondents with no further training or PD in paediatrics reported neutral levels of confidence and below. When asked if they are able to deal with the range of patient conditions which may be seen with a paediatric caseload (SEQ13), the majority of respondents (68.5%) reported neutral levels of confidence and below. Similarly, 94% of the respondents with no further training or PD in paediatrics reported neutral levels of confidence and below. In this context the questionnaire explored the confidence and self-efficacy beliefs of a rural physiotherapist undertaking a paediatric initial assessment to incorporate effective communication, comprehensive subjective and objective assessments, interpretation of assessment findings, and prioritisation of those assessment findings. Other components included adequately performing treatments as well as selection of short- and long-term goals.
Across the entire questionnaire, an average of 9 (of 16 sole practitioners) and 6 (of 7 practitioners working as part of a small group of clinicians) were also rated as having neutral levels of confidence and below when working with a paediatric caseload. Similarly, 77% of respondents who reported having no further experience in paediatrics were reported as having neutral levels of confidence and below. This is in contrast with 47% of those respondents who have had further experience in paediatrics reporting neutral levels of confidence and below. Further experience was defined as previously working in paediatrics, covering paediatrics within a hospital rotation, or currently working with paediatrics clients.
Conversely, respondents were more likely to have higher levels of self-efficacy across more generic domains of paediatric physiotherapy . When asked if able to verbally communicate effectively and appropriately with paediatric clients, 87% of respondents reporting neutral levels of confidence and above (35% confident, 17% a lot of confidence). This appeared to be the only domain where the majority of respondents did not demonstrate a lack of self-efficacy. This can be attributed to the well-developed communication skills required when working as a physiotherapist. Communication and interpersonal skills are vital to competent and effective practice, especially in forming effective interaction with patients47.
In summary, common themes found across responses to SEQ and domains of the questionnaire demonstrated low levels of confidence and a lack of self-efficacy in rural physiotherapists when dealing with paediatric caseloads. Unexpectedly this was also found for respondents who had further experience or education in paediatrics. Past research has determined the majority of rural physiotherapists was considered to be a generalist, undertaking service delivery across a range of caseloads where paediatrics often contributed one-third of that caseload18. However, when the rural physiotherapist demonstrates a lack of self-efficacy beliefs in treating a paediatric client, it raises concern about the adequacy of competency standards and about conflicts with codes of conduct. This is particularly so when professional bodies and registration boards such as the APA and the PBQ, respectively, set codes of practice compelling physiotherapists to define their scope of practice according to current knowledge and competency standards. A physiotherapist with low confidence in a clinical field outside their scope of practice should refer on to a more suitably qualified practitioner with more experience to ensure the patient receives the best possible and most appropriate physiotherapy service.
Limitations
The study design has limitations. First, in terms of the choice of methodology, most general self-efficacy assessments consist of an omnibus-type instrument that attempts to measure a general sense of efficacy or confidence. Bandura argued that such general measures create problems of predictive relevance and are obscure regarding what is being assessed. General self-efficacy instruments provide global scores that de-contextualize the self-efficacy correspondence and transform self-efficacy into a generalized personality trait, rather than the context-specific judgment Bandura suggests12-14,16. Domain-specific assessments are more explanatory and predictive than omnibus measures and preferable to judgments, but they are inferior to task-specific judgments because the sub-domains can differ markedly in the skills required48. The study aimed to eliminate this by creating a scale that encompassed task-specific measurement of confidence12,13,14,16.
The true clinical implications remain unclear because the study design incorporated descriptive statistics only, which was conducted on a small sample. Should further in-depth analysis have been undertaken, it would not have revealed any statistically significant results as the sample size was too small. This, coupled with a lack of higher level evidence, does not provide the reader with the ability to draw clinical implications, but rather raises the findings as issues to be considered.
Initially, a mixed method approach was regarded as best for this study because multiple facets of the research question needed exploration. However, due to time constraints, once the self-efficacy data was collected by questionnaire, the thoroughness of the participants' answers was deemed sufficient to address the other study aims without need for semi-structured interviews. Further investigation can be undertaken to gain a more qualitative, information rich picture of this physiotherapy cohort, and to explore the reasons for their low self-efficacy beliefs.
Conclusion
Low levels of confidence and a lack of self-efficacy beliefs exists in rural physiotherapists working with paediatric caseloads. This trend was evident across all domains of the patient initial assessment, and was also a key issue demonstrated by sole practitioners and those rural physiotherapists working within a small multidisciplinary team. A lack of self-efficacy was also noticed unexpectedly among rural physiotherapists who had further experience or training in paediatrics physiotherapy practices. The consequences of low self-efficacy include poor confidence in the ability to practise as a physiotherapist, and a belief that one lacks the skills and attributes to do so. In turn, this can lead to issues with professional conduct, and ethical standards.
References
1. Australian Physiotherapy Association. Issues for rural and remote physiotherapists made flesh. Physiotherapy InMotion 2009; June: 18-19.
2. Australian Physiotherapy Association. Sole rural and remote physiotherapists. Australian Physiotherapy Association position statement, Victoria, NSW: APA. (Online) no date. Available: http://www.physiotherapy.asn.au/images/Document_Library/Position_Statements/sole_rural_and_remote_physiotherapists.pdf (Accessed 19 October 2010).
3. Battye KM, McTaggart K. Development of a model for sustainable delivery of outreach allied health services to remote north-west Queensland, Australia. Rural and Remote Health 3: 194. (Online) 2003. Available: www.rrh.org.au (Accessed 27 April 2006).
4. Bent A. Allied health in Central Australia: Challenges and rewards in remote area practice. Australian Journal of Physiotherapy 1999; 45(3): 203-212.
5. Fary R. Increased work value. The case for physiotherapy 2004. Physiotherapy Work Value Submission. Application P18 of 2003. Unknown publisher: 2004; 68-78.
6. Sheppard L, Nielsen I. Rural and remote physiotherapy: Its own discipline. Australian Journal of Rural Health 2005; 13(3): 135-136.
7. Williams E, D'Amore W, McMeeken J. Physiotherapy in rural and remote and regional Australia. Australian Journal of Rural Health 2008; 15(2): 380-386.
8. Australian Physiotherapy Association. Physiotherapy workforce in rural and remote Australia. Physiotherapy InMotion 2009; June: 16-17.
9. Australian Physiotherapy Association. The broader context of rural and remote health. Physiotherapy InMotion 2009; June: 18-19.
10. Bandura A. Self-efficacy: toward a unifying theory of behavioral change. Psychological Review 1977; 12(84): 191-215.
11. Schwoerer CE, May DR, Hollensbe EC, Mencl J. General and specific self-efficacy in the context of a training intervention to enhance performance expectancy. Human Resource Development Quarterly 2005; 16(1): 111-129.
12. Bandura A. Social foundations of thought and action - a social cognitive theory. Englewood Cliffs: Prentice Hall, 1986.
13. Bandura A. Self-efficacy: the exercise of control. New York: Freeman, 1997.
14. Pajares F. Overview of social cognitive theory and of self-efficacy. (Online) 2002. Available: http://www.emory.edu/EDUCATION/mfp/eff.html (Accessed 15 October 2009).
15. Sander P, Sanders L. Measuring confidence in an academic study: a summary report. Electronic Journal of Research in Educational Psychology and Psychopedagogy 2003; 1(1): 1-17. Available: http://www.investigacion-psicopedagogica.org/revista/articulos/1/english/Art_1_1.pdf
16. Pajares F. Current directions in self-efficacy research. In: M Maher, P Pintrich (Eds). Advances in motivation and achievement, vol 10. Greenwich: JAI Press, 1997; 1-49.
17. Arthur L, Sheppard L, Dare R. Redefining rural and remote physiotherapy practice. Australian Journal of Rural Health 2005; 13(1): 57.
18. Sheppard L. Work practices of rural and remote physiotherapists. Australian Journal of Rural Health 2001; 9(2): 85-91.
19. Lindsay R, Hanson L, Taylor M, McBurney H. Workplace stressors experienced by physiotherapists working in regional public hospitals. Australian Journal of Rural Health 2008; 16(4): 194-200.
20. Smith T, Cooper R, Brown L, Hemmings R, Greaves J. Profile of the rural and remote allied health workforce in Northern NSW and comparison with previous studies. Australian Journal of Rural Health 2008; 16(3): 156-163.
21. Australian Physiotherapy Association. APA Vision for Physiotherapy 2020. Melbourne, VIC: APA, 2005.
22. Carr J, Sheppard R. Clinical physiotherapy specialisation in Australia: some current views. Australian Journal of Physiotherapy 1996; 42(1): 10-14.
23. Durrell S. Expanding the scope of physiotherapy: clinical physiotherapy specialists in consultants' clinics. Manual Therapy 1996; 1(4): 210-213.
24. New Zealand Society of Physiotherapists, the Advanced Practitioners Working Party. Physiotherapy specialisation - the way forward. Auckland, New Zealand: New Zealand Society of Physiotherapists, 2008.
25. van de Meene LW. Towards the effective use of the specialist physiotherapist. Australian Journal of Physiotherapy 1988; 34(2): 83-87.
26. Chartered Society of Physiotherapy. Specialisims and specialists: guidance for developing the clinical specialist role. London: Chartered Society of Physiotherapy, 2001.
27. Jull G, Australian Physiotherapy Association. Specialist physiotherapists graduate in record numbers. Melbourne, VIC: APA, 2007.
28. Bandura A. Self-efficacy. Encyclopaedia of Human Behaviour, vol 4. San Diego, LA: Academic Press, 1994.
29. Bennett CJ, Grant MJ. Specialisation in physiotherapy: a mark of maturity. Australian Journal of Physiotherapy 2004; 50(1): 3-5.
30. Australian Physiotherapy Association. Submission to the Parliamentary Standing Committee Enquiry into the Developmental Needs of 0-3 Year Olds in WA. Presented to the Principal Research Officer of Community Development and Justice Standing Committee, Legislative Assembly Parliament House, Perth, Western Australia; 1 February 2009.
31. Maher P. Extending scope of practice boundaries. Physiotherapy InMotion 2009; June: 5.
32. Australian Physiotherapy Association. Australian Physiotherapy Association - Code of Conduct. Melbourne, VIC: APA, 2001. Available: http://www.physiotherapy.asn.au/images/APA_Corporate_Documents/apa_code_of_conduct.pdf (Accessed 19 October 2010).
33. Physiotherapists Board of Queensland. Physiotherapists Board of Queensland - Code of Practice. Brisbane, QLD: PBQ, 2005.
34. Lazarus SS, Page CM, Barcome DF. Rehabilitation services in rural and remote communities: delivery by hospital based and local teams. Archive of Physical Medical Rehabilitation 1984; 65(7): 383-387.
35. Wilson KG, Seguin N, Goodman A, Greene G, Pole M. Rural and remote health professionals' satisfaction with a rehabilitation mobile outreach program. Archive of Physical Medical Rehabilitation 1999; 80(3): 332-338.
36. Maurer TJ, Pierce HR. A comparison of Likert scale and traditional measures of self-efficacy. Journal of Applied Psychology 1998; 83(2): 324-329.
37. Maurer T, Andrews KD. Traditional, Likert, and simplified measures of self-efficacy. Educational and Psychological Measurement 2000; 60(6): 965-973.
38. Robson C. Real world research: a resource for social scientists and practitioner-researchers. Oxford: Blackwell, 1993.
39. Neuman WL. Social research methods: qualitative and quantitative approaches. Boston: Allyn & Bacon 2000.
40. Dyer C. Beginning Research in Psychology. Oxford: Blackwell, 1995.
41. Struber J. Recruiting and retaining allied health professionals in rural and remote Australia: why is it so difficult? The Internet Journal of Allied Health Sciences and Practice 2004; 2(2): 1-11.
42. Fary R. Increased work value. The case for physiotherapy 2004. Physiotherapy Work Value Submission. Application P18 of 2003. Unknown publisher: 2004; 68-78.
43. Australian Physiotherapy Association. APA Continuing Professional Development Scheme. (Online) 2009. Available: http://www.physiotherapy.asn.au/index.php/prof-dev/about-cdp-scheme (Accessed 15 November 2009).
44. Physiotherapy Board of Queensland. Registrants Update Newsletter. Brisbane, QLD: PBQ, June 2009; 3-4.
45. Heriza CB, Sweeney JK. Paediatric physical therapy. Part 1. Practice scope, scientific basis and theoretical foundation. Infants and Young Children 1994; 7(2): 20-32.
46. Cherry DB. Paediatric physical therapy: philosophy, science, and techniques. Paediatric Physical Therapy 1991; 30(2): 70-76.
47. QAA. Subject benchmark statements - Health care programmes: Physiotherapy. (Online) 2009. Available: http://www.qaa.ac.uk/academicinfrastructure/benchmark/health/physio-final.asp (Accessed 15 October 2009).
48. Page-Bucci H. The value of Likert scales in measuring attitudes of online learners. (Online) 2003. Available: http://www.hkadesigns.co.uk/websites/msc/reme/likert.htm (Accessed 22 October 2009).
_____________________________