Andhra Pradesh was the first State in independent India to be formed on a purely linguistic basis; Hyderabad is its capital. It is the fifth largest State in India in terms of both area and population. It has an area of 275 068 km1. Three-quarters (76%) of the population of Andhra Pradesh live in rural areas. Although Andhra Pradesh is predominantly an agricultural State, the State has changed rapidly in recent times. The contribution of the agricultural sector to the State domestic product declined from 43% in 1980-1981 to 35% in 1996-1997. The sex ratio is 995 females for every 1000 males in rural areas but only 954 females for every 1000 males in urban areas. Two-thirds (67%) of males and almost half (46%) of females aged 6 years and over are literate. Seventy-six percent of children aged 6-14 years attend school. Seventy-four percent of Andhra Pradesh households have electricity, and 52% have piped drinking water. The total fertility rate declined substantially from 4.6 children per woman in 1971 to 2.5 children per woman in 1997, dropping by 2.1 children in 26 years. The infant mortality rate declined from 106 per thousand live births in 1971 to 63 in 1997, a decline of 41%.
'Health for all by 2000 AD' through primary health care was declared in 1978 in the Alma Ata Declaration. Among its signatories, which included India, this Declaration accelerated development of and strengthened family welfare and Maternal and Child health (MCH) programs, encouraged new strategies and provided more health facilities in order to achieve the goal. Included in the Declaration's aims was that by the year 2000 all people of the world would have obtained a sufficient level of health to permit socially and economically productive lives. On World Health Day in 2002, WHO launched the slogan 'Move for Health'. The Indian Government had already shifted emphasis from family planning programs to family welfare programs, in order to provide a wider scope for promoting MCH programs to improve the heath of mothers and their young children.
The importance of maternal and child health services
In preventive medicine, MCH is defined as field of work related to the physical, mental and emotional health of women immediately before, during and after childbirth; and of infants and young children. Health services begin at the time of conception. Pre-natal, intra-natal and post-natal supervision of the mother promotes and periodically supervises her nutritional state. Avoidable complications of pregnancy are prevented or treated. Intra-natal services provide skilled care and attention by trained midwives during childbirth. Post-natal checks on the mother's health after delivery, which include family planning services, make it possible for a gynaecologist to diagnose and prevent some of the chronic and disabling conditions common in women. Child health services aim for the prevention of acute illness and disease that will disrupt the child's early years. Child health development programs now include the promotion of vigorous and healthy growth and development in children2.
MCH seeks to address the high risks that women in many contexts face in relation to child bearing. MCH programs emphasise the need for pregnant women to receive adequate prenatal care that protects them against the avoidable complications of pregnancy, and allows them to undergo a safe delivery, and to receive adequate postnatal care. Maternal health is significantly associated with the health status of children, which can be measured in the form of a reduction in either mortality or risks to child survival2,3. Childhood immunisation is a most important facet of MCH. Success in child immunisation programs leads to child survival4-6; however, the utilisation of MCH mainly depends on the socioeconomic characteristics of the community.
Delivery of health services in Andhra Pradesh is mainly governed by the National Health Policy, which was approved by the parliament in 1983. The National Health Policy places a major emphasis on ensuring primary health care to all by the year 2000 AD: (i) nutrition for all segments of the population; (ii) immunisation programs; (iii) maternal and child health care; (iv) the prevention of food adulteration and maintenance of water quality, supply and sanitation; (v) environmental protection; (vi) school health programs; (vii) occupational health services; (viii) prevention and control of endemic diseases.
Active community participation has been considered one of the most important supportive activities for successful implementation of health programs. After the Indian Government committed itself to the attaining goal of 'Health for all by 2000 AD', the Government concentrated on the largely neglected rural population. By March 1992, there were 1247 primary health centres, 10 568 sub-centres, 83 postpartum program units, and 131 urban family welfare centres in the State, providing health and family welfare services to the population7.
In 1992, the Indian government embarked on the first of two nation-wide surveys, the National Family Health Surveys (NFHS-I and NFHS-II)8,9. In Andhra Pradesh, the mothers of 93% children born in the 3 years preceding NFHS-II (1995-1998) received at least one antenatal check-up, and the mothers of 80% of these children received at least three antenatal check-ups. For 82% of these children, the mothers received the recommended number of tetanus toxoid vaccinations, and 81% of mothers received iron and folic acid (IFA) supplementation. Coverage by all three interventions was lower for women in disadvantaged socio-economic groups than for other women. Coverage was also low for women who already had four or more children8.
In 1948 the World Health Organization was fully established as a 'specialised agency' of the United Nations; its first World Assembly gave priority to programs for the developing world, such as the eradication and control of malaria, tuberculosis and venereal diseases, and the promotion of maternal and child health services. The unborn child is totally dependent on the mother; after birth, it depends completely on the immediate social environment of the family and of the mother in particular. Therefore since she is the first and most important health care agent of her child and she should be given the highest priority in any health care program. The importance of MCH services (primarily health services but generally regarded as welfare services) can never be exaggerated.
Objectives
This article examines MCH input, its utilisation and its output in the period 1992-1998. Attempts were also made to identify the background characteristics of respondents that effect better utilisation and better MCH in Andhra Pradesh.
The specific objectives were:
- To study the rural-urban differential in MCH input and net change.
- To study urban-rural differential in MCH utilisation and net change.
- To study the urban-rural differential in MCH outcomes and net change.
- To examine the factors influencing the net change in MCH utilisation and outcome.
The data for the present study were collected from National Family Health Surveys (NFHS-I in 1992 and NFHS-II in 1998). The NFHS collected data from 4276 ever-married women in the age group 13-49 years in 1992 (NFHS-I) and 4032 ever-married women in the age group 15-49 years in 1998 (NFHS-II). The following variables were selected for the present study:
- Health infrastructure: (i) Access to health facility within village; (ii) mobile unit; (iii) availability of trained birth attendant; (iv) village health guide; (v) electricity facility.
- Health input regarding antenatal care, postnatal care and childcare: (i) Women received antenatal check up at home from health worker; (ii) women provided with IFA tablets; (iii) assistance during delivery by doctor, nurse, dai (a woman who traditionally attends deliveries in villages); (iv) percentage of women supplied with vaccination card; (v) child provided with vaccination by public sector; (vi) respondents supplied with contraceptive method.
- Utilisation regarding maternal and child health: (i) Respondent went for antenatal care visit outside home; (ii) place of delivery: public or private; (iii) respondents gave full vaccination to their child within 12-23 months; (iv) percentage of children taken to health facility or providers for treatment of fever, acute respiratory infections and diarrhoea.
- Maternal and child health outcomes: (i) Neo-natal mortality; (ii) postnatal mortality; (iii) infant mortality; (iv) child mortality; (v) child under 5 years-of-age mortality; (vi) prevalence of diarrhoea, bloody diarrhoea, acute respiratory infections (ARI); (vii) use of contraception; (viii) delivery complication; (ix) low birth weight baby.
Results and Discussion
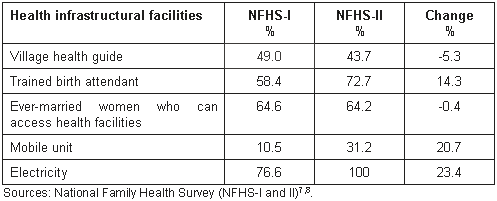
The comparison of health infrastructure facilities between NFHS-I and NFHS-II are shown (Table 1). In the time between NFHS-I and NFHS-II, the percentage of village health guides decreased by over 5% while trained birth attendants increased by 14%. The change in accessibility of the health facility was negligible. Additional health services provided through mobile units increased by 21% and total electrification increased by 23%. This increase means that electricity is widely available, which may have a significant effect on improving the health of the State as a whole.
Table 1: Percentage change in health infrastructure facilities in Andhra Pradesh, India, between NFHS-I and NFHS-II
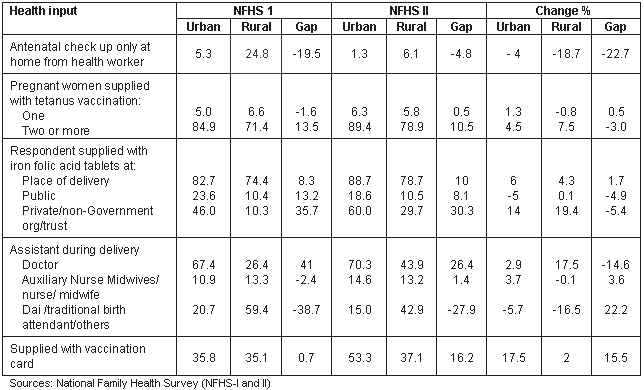
Rural-urban differentials in health input in Andhra Pradesh during NFHS-I and NFHS-II is presented (Table 2). The data indicate that in both urban and rural areas the incidence of antenatal check up 'only at home from the health worker' decreased. In rural areas, it may have been that more women were attending health centres for antenatal care, because it was impossible for the auxiliary nurse midwives (ANM) to provide antenatal care at home for all women in the 8-10 villages under their care. In urban areas, the decrease in home antenatal checks may have been because more women visited urban family welfare centres, general hospitals or maternity centres for their antenatal care.
Supply of tetanus toxoid vaccination to pregnant women increased overall. More women had two or more vaccinations during their pregnancy, rather than only one. The urban-rural differential in pregnant respondents supplied with two tetanus vaccinations decreased from 13.5% to 10.5% during the intra-survey period 1992-1998.
The percentage supply of IFA tablets increased in both rural and urban areas, however, the urban-rural gap also increased during this time.
In both rural and urban areas, during delivery the women had the assistance of a doctor or ANM, rather than trained birth attendants or dais (net change of -14.6%, 3.6% and 22.2%, respectively), indicating wide differences in the percentage of deliveries conducted by trained persons in both urban and rural areas. More urban women were supplied with a vaccination card, but there was no change in the low rate for rural women. Women in rural areas were less likely to have a Western-trained health professional in attendance at delivery, but this availablity improved over the research period.
A positive net change in health input occurred during 1992-1998 but urban rural differentials still existed in Andhra Pradesh. Mothers in rural areas not provided with antenatal care and delivery by trained persons may be more likely to develop postnatal complications that endanger their lives.
Table 2: Percentage change in urban and rural health input in Andhra Pradesh, India, between NFHS-I and NFHS-II
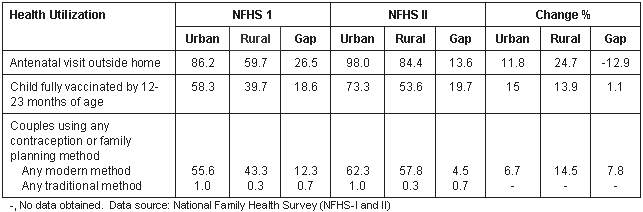
The urban-rural differential in health utilisation is shown (Table 3). There was an increase in antenatal visits outside home, in both urban and rural areas, but the increase was greater in the rural area. This may have been due to a decrease in antenatal check up only at home by health workers (Table 1). In 1993, Jagdish C Bhatia revealed that Andhra Pradesh women living in rural areas without even a subcentre for healthcare had the highest levels of maternal mortality9. The urban-rural differential decreased from 26.5% (1992) to 13.6% (1998).
There was an increase in the immunisation rate of children of 12-23 months of age but the urban-rural differential increased from 18.6% in 1992 to 19.7% in 1998 despite net change in both urban and rural areas. The use of contraception increased among couples using 'any modern method', this inter-survey increase in health consciousness was, however, relatively higher in rural areas. Regarding the use of contraception, there was a trend of increase in both rural and urban areas, but the percentages of use were higher in urban areas in both the surveys. The urban-rural differential in couples using any modern method decreased from 12.3% to 4.5% by 1998, whereas there was no change in the urban-rural differential for total couples using any traditional method. This indicated a net change in health utilisation although urban-rural differentials still existed in health utilisation in Andhra Pradesh.
Table 3: Percentage change in urban and rural health utilisation in Andhra Pradesh, India, between NFHS-I and NFHS-II
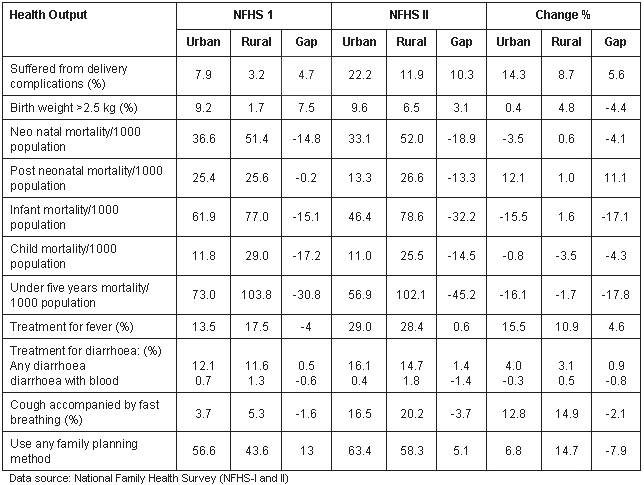
The urban-rural differential in health output is presented (Table 4). Respondents reporting delivery complications increased by more than 14% and 8% in urban and rural areas, respectively. There was a 5% increase in the number of birthweights of over 2.5 kg in rural areas, but the increase was negligible in urban areas, which could be due to malnutrition, lack of proper care and anaemia in the mother. In the 7 years, neonatal mortality decreased in urban areas but there was a slightly increase in rural areas. There was a decrease in the neonatal mortality rate of 3% in urban areas, but a slight increase in rural areas. There was an increase in post-neonatal mortality in both urban and rural areas. Infant mortality decreased by more than 15% in urban areas but increased by 1.6% in rural areas.
The child mortality and under-5 years mortality declined in both urban and rural areas. The treatment of fever increased both in urban and rural areas. The treatment of diarrhoea increased in both urban and rural areas, but diarrhoea with blood declined negligibly in urban areas. There was an increase of 13% in urban areas and 15% in rural areas in a cough accompanied by fast breathing.
There was an overall increase in the total number of respondents who used any family planning method, representing an increase of 7% in urban areas and 15% in rural areas in the intra-survey period. The rural increase is more than two-fold that in urban areas. Urban-rural differentials in respondents suffering from delivery complications increased from 4.7% to 10.3% in the years between the surveys.
The urban-rural differentials increased negatively in neonatal mortality, post-neonatal mortality, infant mortality, child mortality and under-five mortality. The probability of child mortality was increased by low maternal educational levels, short birth intervals and rural residence. Women with greater exposure to formal education are more likely to seek care than those with lower educational levels or no exposure to formal education10. Antenatal care and delivery assistance can improve the health of both mother and child.
The urban-rural differential in treatment for fever was -4% in 1992 and increased to 0.6% in 1998. The urban-rural differentials in treatment for any diarrhoea increased positively, whereas the treatment for diarrhoea with blood and cough accompanied by fast breathing increased negatively. The urban-rural differential in total respondent use of any family-planning method decreased from 13% to 5.1% between 1992 and 1998. Overall, there was a net change in health output, but urban-rural differentials still existed and mortality was still higher among those in rural areas, compared with urban areas.
Table 4: Percentage change in urban and rural health output in Andhra Pradesh, India, between NFHS-I and NFHS-II
A study in South India indicated there are differences between educated mothers and uneducated mothers in treatment-seeking for their children11. In another study, conducted in 1993 in the Ludhiana slums in India, it was observed that the relationship between education and poverty influences the achievement of complete immunisation12. Socioeconomic conditions, education, nutrition and healthcare are often key determinants of women's health and survival13.
In the present study it was observed that among background characteristics of respondents, the educational level of the mother is consistently related to net change in the number of respondents whose children were fully immunised within 12-23 months, and in the number of respondents who had taken their children to a health facility for treatment of diarrhoea. As the level of maternal education increased, the percentage of net change in MCH indicators also increased.
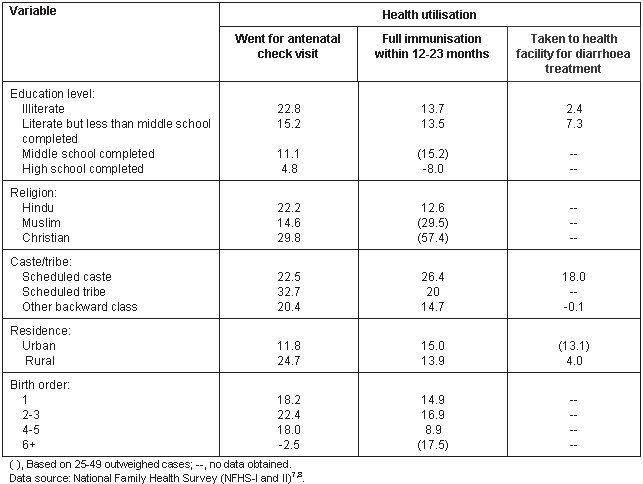
The background variables affecting the percentage of net change in health utilisation is given (Table 5). There was a positive change in the utilisation of health services overall. The increase in antenatal check ups (ANC) was relatively high in the case of those who are illiterate; however, full immunisation in children of 12-23 months was highest in the case of the children of mothers with middle school completed.
Utilisation of ANC by religion showed that Christians were the highest users (29.8%), which could have been due to missionary activities; Muslim women had the lowest (14.6%). Immunisation among children of 12-23 months by religion was highest among Christians (57.4%) and lowest among Hindus (12.6%).
Utilisation of ANC by caste/tribe was highest in case of the scheduled tribes (32.7%), followed by the scheduled caste (22.5%), and lowest 20.4% among other backward class (ie scheduled castes and tribes excluded). Immunisation among children of 12-23 months by caste/tribe was highest among the scheduled caste (26.4%) followed by the scheduled tribes (20%) and lowest among 'other backward class' (14.7%).
The utilisation of ANC was greater in rural areas than in urban areas. This may have been due to the home visits of ANM in rural areas. Full immunisation among urban children of 12-23 months was higher than among those in rural areas. The utilisation of ANC by birth order was found to be highest in case of mothers of children whose birth orders was 2 or 3. As birth order increased after 2 or 3, the mother's ANC decreased. The immunisation among children of 12-23 months by birth order was highest in the case of those with a birth order of 6+, followed by those with a birth order of 2 or 3, and lowest in those whose birth order was 4 or 5.
Table 5: Background variables affecting percentage change in health utilisation in Andhra Pradesh, India, between NFHS-I and NFHS-II
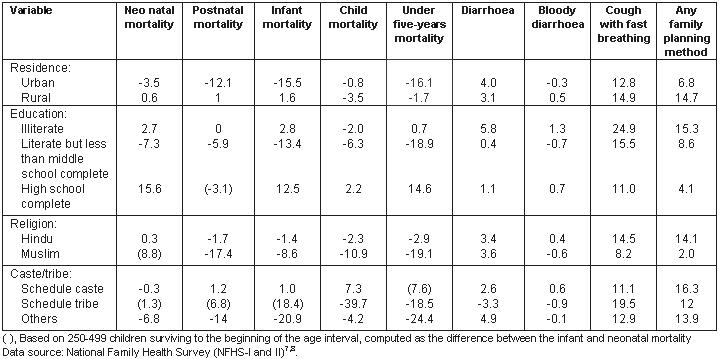
Background variables affecting percentage net change in health outcomes is presented (Table 6). The percentages of neonatal, postnatal, infant, child and under-5 years mortality decreased in urban areas and marginally decreased in rural areas. Among illiterates there was a negligible increase in neonatal and infant mortality. There was an unexpected 16% increase in neonatal mortality and 15% increase in under 5 years mortality among the children of respondents who had completed high school and above.
Among Hindus and Muslim the overall mortality declined but the decline was significant in post-neonatal mortality and under 5 years mortality among Muslims. In case of caste, although neonatal mortality declined slightly, it increased among the other identified age groups.
Among scheduled tribes, infant mortality increased but thereafter child mortality among those under 5 years suffering from diarrhoea decreased. Among other or general castes, all types of mortality decreased. In the case of children suffering from diarrhoea there was an increase among both urban and rural people and among illiterates; although the prevalence was higher when compared with literates, children suffering from diarrhoea increased among both Hindus and Muslims, scheduled and general castes. However, a decline trend in the prevalence of diarrhoea was observed among the children of scheduled tribeswomen. A decline trend was evident among the percentage suffering from bloody diarrhoea in most categories, but there was a marginal increase in its prevalence among the children in rural areas, illiterates, Hindus and scheduled caste respondent's children. The prevalence of bloody diarrhoea increased in all categories but was considerably higher among the children of rural women, illiterate or literate up-to-middle-school women, among Hindus and scheduled caste women. The percentage of women protected from pregnancy by contraception increased in all categories.
Table 6: Background variables affecting percentage change in health outcome in Andhra Pradesh, India, between NFHS-I and NFHS-II
Conclusions
Health facilities, except for village health guides, in rural Andhra Pradesh increased during the 7 years from NFHS-I (1992) to NFHS-II (1998). Andhra Pradesh was one of the most successful Indian States in providing MCH, even though urban-rural differentials still existed. Health input, utilisation and output showed a positive net change, which indicated an improvement in health facilities in the time between NFHS-I and NFHS-II. The increase in health facilities and their utilisation contributed to positive health indicator output. However, there was no major difference in background characteristics according to the output of health indicators.
There was an increase in health input, utilisation and output during the intra-survey period. At the same time contraceptive use greatly increased.
Overall, urban-rural differentials still existed and the Indian Government must take the necessary steps to improve MCH programs, including the provision of information and education campaigns, and sending dedicated health personnel to remote and inaccessible rural areas in order to reduce child mortality.
References
1. Caldwell JC. Education as a factor in mortality decline: an examination of Nigerian data. Population Studies 1979; 33: 395-413.
2. Kanitkar T. Development of maternal and child health services in India. In: Srinivasan K, Saxena PC, Kanitkar T (Eds). Child in India. Bombay: Himalaya, 1979.
3. Cleland J, Van Ginnekam J. Maternal education and child survival in developing countries: the search for pathway of influence. Social Science and Medicine 1988; 27: 1357-1368.
4. UNICEF. First call for children: world declaration and plan of action from the world summit for children. New York: UNICEF, 1990.
5. Kim-Farley R, for the Expanded Programme on Immunization Team. Global immunization. Annual Review of Public Health 1992; 13: 223-237.
6. Grant JP. The state of the world's children. New York: Oxford University Press for UNICEF, 1993.
7. Directorate of Health Services, Andhra Pradesh. Handbook of health statistics. Hyderabad: Government of Andhra Pradesh, 1993.
8. International Institute for population sciences (IIPS). National Family Health Survey: Andhra Pradesh Report, 2000. In: Srinivasan PC, Kanitkar S, Kanitkar T (Eds). Child in India. Bombay: Himalaya, 1979.
9. International Institute for population sciences (IIPS). National Family Health Survey: Andhra Pradesh Report. Bombay: IIPS, 1994.
10. Wolff RB. Maternal education and community context in maternal and child health behaviour in Nigeria, Vol.9. Ann Arbour, MI: University Microfilms International, 1993; 250.
11. Caldwell JC, Reddy PH, Caldwell P. The social component of mortality decline: an investigation in South India employing alternative methodologies. Population Studies 1983; 37: 185-205.
12. Panda P, Benjamin AI, Zachariah P. Health Status of Under-fives in a Ludhiana Slum, Health and Population Perspectives and Issues 1993; 16: [no pp].
13. United Nations. Reproductive rights and reproductive health: a concise report. Geneva: UN, 1995.

