Introduction
Chronic diseases have become an increasing global concern, and are prevalent in low-income communities in South Africa1. South African health systems are bearing the double burden of infectious and chronic diseases in low-income, rural communities2, and it has been shown that chronic diseases are increasing among older adults3. Physical activity has been associated with the prevention and reduction of such diseases4-5. While in South Africa concern has been expressed regarding high levels of physical inactivity, it has been estimated that 3.3% of the adult burden of disease may be explained by physical inactivity, which was ranked ninth among risk factors for attributable deaths6. However, despite the apparent rise in the burden of chronic diseases in South Africa7-9, there are limited data on the role of physical activity in preventing and reducing chronic diseases in these settings10-12.
School- and community-based physical activity interventions, including those targeting older adults, have been widely reported in the literature. Programs for schools are typically implemented within the existing school infrastructure and include a curriculum, environmental, or parent component, or a combination of these13-18. Programs for older adults also tend to be implemented within existing community infrastructure, and are often peer-led. Evaluations of interventions in older adults have reported not only increases in habitual levels of physical activity19, but also improvements in blood pressure20, physical function20-22, emotional state23, functional health and wellbeing21, and increased satisfaction with body appearance and function19. There is less information, however, on critical enabling factors or barriers to the implementation of such programs.
In recent years, qualitative methods have been used frequently in both outcome and process evaluations to understand program attributes such as cultural relevance24, feasibility18, and implementation25-27. However, the majority of this qualitative literature is from developed countries, and although a number of the studies were conducted with low-income groups24,26, there remains a gap in literature from low- and middle-income countries, such as South Africa. Furthermore, while a number of studies cited earlier reports on interventions in low-income settings, very few of these were from African settings. There is also a paucity of data from low-income, rural settings because the majority of interventions are implemented in urban areas.
The Discovery Healthy Lifestyle Programme
The Discovery Healthy Lifestyle Programme (DHLP), a corporate social investment project funded by a major national private health insurer, was implemented in 2006. This program was based on the Community Health Intervention Programmes (CHIPs) which have been active in low-income urban communities in the Western Cape region since 1997. The CHIPs are physical activity-based health promotion programs, based on a life-course approach, and form part of the Sports Science Institute of South Africa's (SSISA) Outreach Division. These programs were developed in response to the apparent rise in chronic diseases, relatively low prevalence of health-enhancing physical activity, and the lack of fitness facilities in low-income and previously marginalised communities28. The school-based component of the CHIPS has previously been shown to be effective in an urban setting29.
The village of Mafarana in South Africa's Limpopo Province was selected as one of the pilot settings for the DHLP because most of the province consists of rural communities, making it an effective contrast to the urban settings of the Western Cape. Furthermore, there was an existing collaboration between program funders and the Limpopo Department of Health in the Mopani District, who had already increased efforts to prevent chronic diseases. Two rural communities in this district were selected to participate in the pilot program. One, Mafarana, was the intervention community and the other, Motupa, served as a 'delayed-intervention' community. A brief overview of demographic information for the Limpopo province is provided (Table 1).
The two CHIPs programs that were implemented as part of the DHLP were 'Healthnutz' for children and 'Live it Up' for older adults (>60 years). Although these two CHIPs programs have generally been implemented separately, and not necessarily in the same communities in the Western Cape, for the purposes of the DHLP, the two programs were implemented together. Details of these programs are outlined in the logic model (Fig1).
Table 1: Limpopo demographic information30
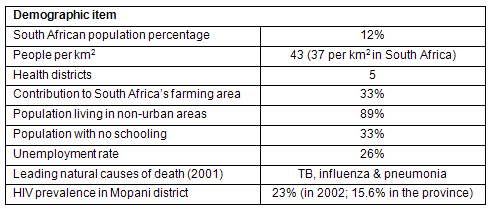

Figure 1: The Discovery Healthy Lifestyle Programme logic model.
The DHLP aligns with Pender's health promotion model31, a conceptual framework that is used to understand the complex way individuals interact with their interpersonal and physical environments when changing their health behaviour. This model has been used previously in relation to physical activity and chronic diseases31.
Aim
The aims of this qualitative evaluation were to: (i) assess the process by which the DHLP was implemented; (ii) assess the acceptability and feasibility of the program; and (iii) gain insight into the enabling factors and barriers to implementation that may have impacted on outcomes of physical activity participation and awareness of the role of physical activity for health. Although the program outcomes were assessed quantitatively (hence the inclusion of a delayed-intervention community), this article focuses on the qualitative evaluation. Systematic monitoring data were not collected for this program, thus limiting information about the fidelity of the intervention. Due to the lack of reliable monitoring data and the paucity of research on evaluation of physical activity interventions in South Africa or other low-income, rural settings, this evaluation was largely exploratory in nature.
Methods
Data were collected through semi-structured focus groups, situational analyses, informal community observations and informal interviews with program coordinators (nurses from the provincial Department of Health in the Mopani district). These data collection methods, which draw on ethnographic approaches, have been recommended for evaluations of community-based programs that aim to encourage community participation32. It was believed that qualitative methods would provide a richer understanding of the contextual factors surrounding the implementation of the program, owing to the exploratory, descriptive and flexible nature of qualitative research that contributes to and expands our understanding of social processes33.
Semi-structured focus groups were chosen, rather than in-depth interviews, because the researchers believed a more flexible group process would elicit community views and issues affecting the implementation of the DHLP. The research team acknowledged the unfamiliarity of community members with research, making the naturalistic quality of focus groups34 a less threatening option than one-on-one interviews.
A total of seven visits were made to the community by at least one member of the research team at each visit. Details of these visits are outlined (Table 2). The visits provided a number of valuable opportunities for the researchers to observe the community setting and to speak with program coordinators. While these observations and conversations were not necessarily of the depth required for ethnographic research, they nevertheless played an important part in contextualising the DHLP and providing insight into the implementation process. This was particularly relevant as an essentially urban program was being implemented for the first time in a rural setting.
Table 2: Details of research visit
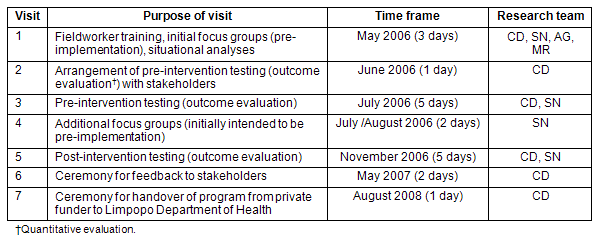
A total of six focus groups (Table 3) were conducted in the communities (total n=45), either at schools or health clinics. Two focus groups (n=8, n=12) with leaders (of the Healthnutz program) and teachers were conducted during their training, just prior to program implementation; all those undergoing training were invited to participate in the focus groups. One focus group was conducted with teachers from the school in the delayed-intervention community (n=6), and this took place at the school. An additional two focus groups were conducted approximately 1 month after implementation: one with Live it Up members (n=8) and the other with chronic disease support group members in the delayed-intervention community (n=8). For both these focus groups, nurses at the clinics involved in the program invited members of the chronic disease support groups to participate in the focus groups. One focus group (n=3) was conducted 4 months after implementation with nurses and a community leader from the intervention community to assess their impressions of the program's progress in their community.
Table 3: Focus group details
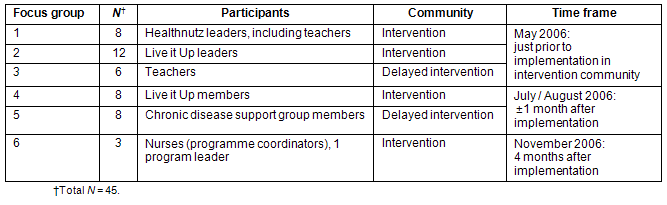
The purpose of the focus groups in the delayed-intervention community was to gain insight into the issues under investigation, and to determine (qualitatively) the similarities of and differences between the two community settings. The 1 month delay in the initial round of evaluation focus groups was due to logistical and institutional constraints, as well as the fact that program implementation was given priority.
The focus group guide questions covered the following issues:
- the importance of physical activity
- expectations and perceptions of the program/s, and whether any similar programs currently exist in their community
- perceptions of the leader's training
- community factors that may enable or inhibit the successful implementation of the programs.
Focus groups with leaders and teachers were conducted in English, whereas others were conducted in the home language of the participants (Xitsonga or Northern Sotho) by a member of the research team fluent in these languages. Notes of group discussions were taken by trained, local fieldworkers (from both the intervention and delayed-intervention communities) as opposed to recording the discussions by audio or video, because the latter may have inhibited participation. Note-taking was deemed more culturally appropriate by members of the research team after consultation with the program implementers. Notes taken in participants' home language were translated into English; all notes were then collated to generate summaries of the discussions.
Situational analysis was conducted on the physical activity environment of each school (n=3), with specific focus on the implementation of physical activity and sport in the timetable, the availability of sporting equipment and facilities, and the distribution and accessibility of healthy food at the school. This involved a combination of direct observation and consultation with a member of the school staff, such as the school principal or teacher in charge of sport, who also facilitated the observation. These were conducted by a member of the research team using a tool developed for use in South African settings, for 30-45 min duration in each school.
Members of the research team responsible for qualitative data analysis were aware from the outset that the type of data to be collected may not have had sufficient rigour for qualitative data analysis, such as discourse or conversation analysis. However, owing to the exploratory nature of the evaluation, the team agreed that content (thematic) analysis would be sufficient to uncover the relevant contextual issues impacting on the program's implementation. The focus group summaries were analysed for content by the members of the research team and then validated by informal interviews with program coordinators (n=3) and community observations.
The synopses derived from the focus groups, situational analysis, observations and interviews were grouped according to the following framework themes for findings presentation:
- challenges within communities
- perceptions of the importance of physical activity and healthy lifestyles
- views of the DHLP, including the training received by the leaders
- factors perceived to be contributing to or inhibiting the success of the DHLP.
Ethical approval for this research was obtained from the Research Ethics Committee in the Faculty of Health Sciences, University of Cape Town (REC ref: 486/2005). All participants consented to their involvement in the research.
Results
Challenges within communities
A brief description of the socioeconomic characteristics of these communities will help contextualise the circumstances in which the DHLP was implemented. From observations of the community settings, it was evident that these rural communities faced socioeconomic and health inequalities, and were under-resourced and under-served. During the period in which the research took place (2006-2008), a lack of access to basic amenities such as potable water, sanitation and electricity was observed. Although these facilities were available at public health clinics, they were not available at schools or in most homes. A rain water tank served as the only source of potable water at all the schools.
Although participating communities were in close proximity (35-40 km, approximately 30 min drive on roads in reasonably good condition) to the town of Tzaneen (one of Limpopo's largest towns), there was limited access to health services. In 2006, there were reportedly 9600 people to one clinic in the Mopani District35. Health concerns in the community, according to clinic staff and community members (in focus groups), included the prevalence of HIV/AIDS in the district, as well as chronic diseases, with high blood pressure being the primary concern.
Other community challenges emerged in focus group discussions. Public transport, although available, was regarded as unreliable and costly. However, it was often used instead of walking due to the safety concerns of community members (eg the fear of being assaulted or robbed). Transport to and from the clinic was reported to be particularly challenging for older adults who had limited mobility, because many did not live within reasonable walking distance of the clinic.
Further challenges reported in the focus groups by older adults included childminding responsibilities, which were expected of them because many mothers worked away from home. Older adults also experienced financial stress due to poverty, particularly if their minimal government-issued pension (equivalent to approximately US$130 per month in 2008) was used by other family members who were unemployed. Some respondents also mentioned that they experienced food insecurity (insufficient food, food that was irregularly available or of a poor quality), resulting in poor nutritional status.
Perceptions of the importance of physical activity and healthy lifestyles
At program commencement, leaders and Live it Up members were of the opinion that physical activity was only for younger persons, and that it could be described as 'running and jumping around'. One older adult felt that it would give them 'an opportunity to exercise like white people', suggesting that 'exercise' was typically associated with the more affluent lifestyle 'white people' have historically enjoyed in South Africa.
It was evident in the focus group discussions with leaders and members that their participation in the program provided an opportunity to identify the benefits of physical activity for older adults, such as increased flexibility, strengthening of the bones and joints, reduction in pains, aches and cramps, improved blood circulation, stress reduction, and 'keeping them young'. Many were of the opinion that regular physical activity had decreased in rural areas, and that they were walking less than in previous years. It was noted that manual labour tasks had decreased due to developments such as increased access to resources (eg purchasing already chopped wood or buying maize meal instead of grinding their own).
Barriers to physical activity and sport in the school environment
Within the school environment, participants expressed the view that children had become less physically active, partly due to the inclusion of physical education in the 'Life Orientation' (LO) curriculum, following its phasing out as a stand-alone subject from 2004 as part of the revised national curriculum. Life Orientation has four learning outcomes: health promotion (including nutrition), social development, personal development, and physical development (including physical activity). Discussions with principals and teachers revealed that as physical activity was only one of the four LO components, it was subsequently allocated less time and attention. As a result teachers required assistance and support to find ways to include physical activity and nutrition education into the LO curriculum.
In addition, during the situational analyses schools were observed to be in great need of sporting equipment, appropriate uniforms and adequately developed facilities. Although large open spaces were available in the school grounds, these were not ideal for physical activity or organised sport because poor surface quality (sandy soil containing stones) increased the risk of injury and was unsuitable for field markings. In the focus group discussions teachers reported that the inadequacy of equipment and facilities severely hindered the implementation and practice of organised sport.
Teachers also mentioned the difficulty of transporting children to compete with other schools, due to large geographical distances; and because many children had no birth certificate they could not be classified into age groups for participation in organised competitions. Such difficulties in participating in organised sport impacted negatively on the establishment of a culture of physical activity in the school environment.
Views of the Discovery Healthy Lifestyle Programme
The DHLP was believed to be well received in both communities on the basis of the researchers' interactions with community members and stakeholders, continued participation and apparent support of the program (the term 'stakeholders' refers here to political, religious, traditional and tribal community leaders). Many believed that there was a great need for such programs. Despite some initial apprehension due to the novelty of the program in a rural area, respondents were positive about the DHLP and confident about its successful implementation. The perceived value of the program related to both health and psychosocial outcomes.
From a health perspective, focus group participants believed that the information and health education would increase their knowledge about the importance of physical activity and healthy lifestyles. They also believed the program would assist in the reduction of chronic diseases and other adverse health outcomes, as well as improving their own chronic conditions. In terms of psychosocial outcomes, program participants saw the program as providing social interaction, a sense of belonging and unity, and improved quality of life and longevity.
The leaders were positive in the focus groups, and seemingly empowered by the training. This increased their self-efficacy as role models and agents of change. They maintained that the training increased their understanding of physical activity and healthy lifestyles, and their ability to relay the benefits to others in their community. They also believed that the training had positively altered their perception of physical activity, and that future involvement in the program would continue to enhance their knowledge and skills.
Perceptions of the successful implementation of the Discovery Healthy Lifestyle Programme
Initial indicators of successful implementation of the DHLP (specifically the Live it Up program) included the positive change in respondents' perceptions of physical activity, increased awareness of the importance of physical activity and the adoption of healthier lifestyles. These emerged in the focus group conducted with Live it Up members approximately 1 month after the program was implemented. Further indications of program success were mainly from informal observation and interviews during stakeholder feedback and handover ceremonies (visits 6 and 7). While limited specific data were collected, the information gathered from these visits give some indication of the positive way in which the program was received by stakeholders.
Program implementers perceived the Live it Up program component to be growing, and this was evident at the time of the stakeholder feedback ceremony (6 months after post-intervention testing at visit 6) when Live it Up participants from the delayed-intervention community provided an exercise demonstration. This indicated the program had been implemented in the community as planned, which was considered a sign of program growth, and suggested sustainability. There were, however, some concerns about the Healthnutz intervention because some schools were having difficulty incorporating the program into the school timetable. Nonetheless, teachers were positive about the program and its value for their learners, staff and school.
At the stakeholder feedback ceremony, selected findings from the outcome evaluation were presented, with an emphasis on the progress of the research, and the importance of the research for the program. All stakeholder groups were represented, including the academic institutions involved in the evaluation, program managers (CHIPs and SSISA) and funders (Discovery), program implementers, program participants and leaders, as well as community leaders such as tribal and religious leaders, and members of local government. Representatives from all stakeholder groups expressed satisfaction with the progress of the program, and community and local government representatives in particular voiced their support and their desire to see the program continue and expand in their district. At the time of visit 6 it was also evident from discussion with program implementers and stakeholders that even the evaluation was seen as value-adding to the program, an encouraging finding for future research in similar rural communities.
Positive sentiments expressed during visit 6 were echoed even more strongly at the seventh visit, at which the ownership of the program was transferred from corporate funders to the Department of Health. Just prior to this event, 60 Department of Health nurses had received training to implement the program in their clinics as part of the wider dissemination to other communities in the district. Representatives from the delayed-intervention community (where the program was implemented after the completion of the research) were also present, which was encouraging to the researchers.
The observations made at the stakeholder feedback and handover ceremonies confirmed that the program is perceived as acceptable and feasible within these communities, in spite of the challenges to implementation. At these events it was apparent that communities (including community members, leaders and local government) had been mobilised by their involvement in the DHLP, which increased the likelihood of its sustainability. This was an important outcome of the original community development approach.
Certain characteristics of these two communities - being under-resourced and under-served rural settings - seemed to have positively influenced the implementation of the DHLP. The paucity of resources and infrastructure meant that little had been done to raise the profile of physical activity prior to implementation of the DHLP. Comments from participants suggested this increased their receptiveness to the DHLP and enabled an increase in their levels of activity despite inadequate resources. The involvement of local government in the formative and implementation program phases, with their existing awareness of the effect of chronic diseases, paved the way for an extensive and participative consultation process with key stakeholders in the district. Community interaction suggested that the consultation process encouraged greater ownership of and involvement in the program. Both members and leaders were identified as role models in their communities, with the potential to change the social norms associated with physical activity and healthy lifestyles.
Alignment of the Discovery Healthy Lifestyle Programme with the health promotion model
With regard to Pender's health promotion model mentioned previously, Figure 2 outlines the main components of this model and indicates areas of alignment of this model with the DHLP.
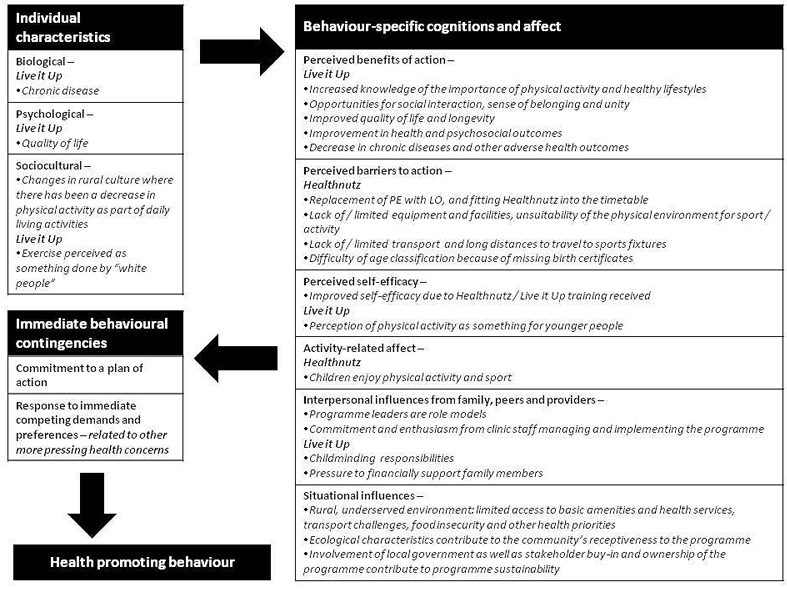
Figure 2: Health promotion model.
Discussion
The findings of this study suggest that through enhancement of knowledge, transfer of appropriate skills and the provision of an enabling environment, participation in physical activity can be effectively promoted, in both children and older adults. This study showed that there is a need for physical activity-based health promotion programs, such as the DHLP, even in rural communities where activity may still form a part of everyday household and work-related activities. The DHLP was feasible and accessible to the targeted rural communities because it made use of existing community strengths and assets, such as existing governmental networks and programs. Furthermore, the program was financially viable because it required minimal, inexpensive equipment for the successful implementation, and utilised existing infrastructure within the healthcare or education sectors.
The lessons learnt from this study highlight that key role players and community leaders should be included and acknowledged because they can influence, mobilise and encourage community members to identify, own and implement interventions. This concept of community participation is a key principle of successful health promotion practice24,32, and has been shown to be vital to successful implementation and sustainability of the DHLP.
The empowerment of communities has been identified as a key function of health promotion36. Within the DHLP, not only were leaders empowered as role models and agents of change in their communities, but also program participants were empowered through the opportunity to take increased responsibility for their health. The consultation process was also empowering for community stakeholders, resulting in a greater sense of ownership and involvement in the program. The empowerment of community members through program participation has been shown to be particularly important in South African settings37.
A further lesson from the present findings is that older adults may have the responsibilities of child minding and providing financially for their families. In this case it meant they had less time for program participation than program planners had envisaged. Consideration also needs to be given to the limited mobility of older adults, particularly if they must travel relatively large distances in rural areas. Therefore, health interventions such as physical activity participation should be associated with regular clinic visits and existing chronic disease support group meetings.
The findings of this study also showed that the intervention investigated had to compete with other pressing health and social issues (such as HIV/AIDS, crime and safety, unemployment, poverty and access to basic amenities such as electricity, water and sanitation) for time, attention, resources and energy. However this should not overshadow the appropriateness of and need for such a program.
Health promoters should be encouraged to include the promotion of physical activity for chronic disease prevention as part of a comprehensive approach to promoting healthy lifestyles in low-income, rural communities. Physical activity as part of health promotion could serve as a vehicle for community development and mobilisation; and Ridde's argument36 that health promotion should address social and health inequalities, has relevance for the DHLP in rural communities where socioeconomic and health inequalities persist.
In analysing the benefits of a program such as the DHLP, it is important to also focus on benefits other than the physiological, and this was relevant for Live it Up and Healthnutz. For older adults, many of the psychosocial benefits identified by respondents were similar to those reported elsewhere19,23. Within the school environment, the Healthnutz program was believed to be valuable by raising the profile of physical activity and emphasising the importance of healthy lifestyles for teachers and learners, as well as building the capacity of teachers, particularly in the area of LO. The potential impact on other educational and social outcomes warrants further study, as these could be important to key role players, as well as to school teachers and principals.
Limitations
The limitations of this study include the small sample size and the relatively short period of evaluation. A follow-up study after a number of years would provide more specific insights into and data on the factors promoting or hindering the success of such an activity promotion program. In addition, the authors acknowledge that there were challenges associated with the rigour of this evaluation. These challenges included the remote, rural setting and the geographical distance from members of the research team, and the pressure to 'implement versus evaluate' that can be experienced in corporately-funded programs. A further challenge was the novelty of this type of research in such rural communities. The resulting unfamiliarity with monitoring and evaluation procedures limited the availability of systematic monitoring data. These challenges highlight the importance of using ethnographic methods in future research that can more accurately capture the community-level data required.
Conclusions
The DHLP was well received by the stakeholders. Although the evaluation was relatively basic, it was perceived by stakeholders to add value to the program. This study presented a unique opportunity to assess the implementation and sustainability requirements of programs in environments with limited resources, a considerable burden of infectious and chronic diseases, and extensive socioeconomic challenges. The evaluation, therefore, contributes to the understanding of implementing and evaluating physical activity-based programs aimed at preventing and treating chronic disease in low-income, rural settings.
Acknowledgements
The authors thank the representatives of the Limpopo Department of Health in the Mopani District for their enormous assistance with the Discovery Healthy Lifestyle Programme, and particularly the logistical aspects of this research. Funding for this research was provided by Discovery Corporate Social Investment.
References
1. World Health Organisation. Global strategy on diet, physical activity and health. (Online) 2004. Available: http://www.who.int/dietphysicalactivity/en/ (Accessed 31 July 2009).
2. Tollman SM, Kahn K, Sartorius B, Collinson MA, Clark SJ, Garenne ML. Implications of mortality transition for primary health care in rural South Africa: a population-based surveillance study. Lancet 2008; 372(9642): 893-901.
3. Kahn K, Garenne ML, Collinson MA, Tollman SM. Mortality trends in a new South Africa: hard to make a fresh start. Scandinavian Journal of Public Health 2007; 69(Suppl): 6-34.
4. Booth FW, Chakravarthy MV, Gordon SE, Spangenburg EE. Waging war on physical inactivity: using modern molecular ammunition against an ancient enemy. Journal of Applied Physiology 2002; 93(1): 3-30.
5. Patel D, Lambert EV, de Silva R, Liberto F, Nossel C, Gaziano T. Fitness-related activities as part of an incentive-based wellness program and chronic medical claims and admission: Vitality Insured Persons. Medicine and Science in Sports and Exercise 2008; 40(5): S106.
6. Joubert J, Norman R, Lambert EV, Groenewald P, Schneider M, Bull F et al. South African Comparative Risk Assessment Collaborating Group. Estimating the burden of disease attributable to physical inactivity in South Africa in 2000. South African Medical Journal 2007; 97(8 Pt 2): 725-731.
7. Senekal M, Steyn NP, Nel JH. Factors associated with overweight/obesity in economically active South African populations. Ethnicity and Disease 2003; 13(1): 109-116.
8. Walker AR, Walker BF, Segal I. Some puzzling situations in the onset, occurrence and future of coronary heart disease in developed and developing populations, particularly such in sub-Saharan Africa. Journal of the Royal Society for the Promotion of Health 2004; 124(1): 40-46.
9. Kruger HS, Puoane T, Senekal M, van der Merwe MT. Obesity in South Africa: challenges for government and health professionals. Public Health Nutrition 2005; 8(5): 491-500.
10. Levitt NS, Steyn K, Lambert EV, Reagon G, Lombard CJ, Fourie JM et al. Modifiable risk factors for Type 2 diabetes mellitus in a peri-urban community in South Africa. Diabetic Medicine 1999; 16(11): 946-950.
11. Kruger HS, Venter CS, Vorster HH, Margetts BM. Physical inactivity is the major determinant of obesity in black women in the North West Province, South Africa: the THUSA study. Transition and Health During Urbanisation of South Africa. Nutrition 2002; 18(5): 422-427.
12. Steyn K, Levitt NS, Hoffman M, Marais AD, Fourie JM, Lambert EV et al. The global cardiovascular diseases risk pattern in a peri-urban working-class community in South Africa. The Mamre study. Ethnicity and Disease 2004; 14(2): 233-242.
13. Luepker RV, Perry CL, McKinlay SM, Nader PR, Parcel GS, Stone EJ et al. Outcomes of a field trial to improve children's dietary patterns and physical activity. The Child and Adolescent Trial for Cardiovascular Health. CATCH collaborative group. Journal of the American Medical Association 1996; 275(10): 768-776.
14. Going S, Thompson J, Cano S, Stewart D, Stone E, Harnack L et al. The effects of the Pathways Obesity Prevention Program on physical activity in American Indian children. Preventive Medicine 2003; 37(6-Pt 2): S62-69.
15. Verstraete SJ, Cardon GM, De Clercq DL, De Bourdeaudhuij IM. A comprehensive physical activity promotion programme at elementary school: the effects on physical activity, physical fitness and psychosocial correlates of physical activity. Public Health Nutrition 2007; 10(5): 477-484.
16. Angelopoulous PD, Milionis HJ, Grammatikaki E, Moschonis G, Manios Y. Changes in BMI and blood pressure after a school based intervention: the CHILDREN study. European Journal of Public Health 2009; 19(3): 319-325.
17. Kain J, Leyton B, Cerda R, Vio F, Uauy R. Two-year controlled effectiveness trial of a school-based intervention to prevent obesity in Chilean children. Public Health Nutrition 2009; 12(9): 1451-1461.
18. Naylor PJ, Macdonald HM, Zebedee JA, Reed KE, McKay HA. Lessons learned from Action Schools! BC - an 'active school' model to promote physical activity in elementary schools. Journal of Science and Medicine in Sport 2006; 9(5): 413-423.
19. Wilcox S, Dowda M, Griffin SF, Rheaume C, Ory MG, Leviton L et al. Results of the first year of active for life: translation of 2 evidence-based physical activity programs for older adults into community settings. American Journal of Public Health 2006; 96(7): 1201-1209.
20. Kolbe-Alexander TL, Lambert EV, Charlton KE. Effectiveness of a community-based low intensity exercise program for older adults. Journal of Nutrition, Health and Aging 2006; 10(1): 1-29.
21. Moore-Harrison TL, Johnson MA, Quinn ME, Cress ME. An evidence-based exercise program implemented in congregate-meal sites. Journal of Physical Activity and Health 2009; 6(2): 247-251.
22. Bunout D, Barrera G, Avendano M, de la Maza P, Gattas V, Leiva L et al. Results of a community-based weight-bearing resistance training programme for healthy Chilean elderly subjects. Age and Ageing 2005; 34(1): 80-83.
23. Shin Y. The effects of a walking exercise program on physical function and emotional state of elderly Korean women. Public Health Nursing 1999; 16(2): 146-154.
24. Feathers JT, Kieffer EC, Palmisano G, Anderson M, Janz N, Spencer MS et al. The development, implementation, and process evaluation of the REACH Detroit Partnership's Diabetes Lifestyle Intervention. Diabetes Educator 2007; 33(3): 509-520.
25. Jancey JM, Clarke A, Howat PA, Lee AH, Shilton T, Fisher J. A physical activity program to mobilize older people: a practical and sustainable approach. Gerontologist 2008; 48(2): 251-257.
26. Rosecrans AM, Gittelsohn J, Ho LS, Harris SB, Naqshbandi M, Sharma S. Process evaluation of a multi-institutional community-based program for diabetes prevention among First Nations. Health Education Research 2008; 23(2): 272-286.
27. Lytle LA, Ward J, Nader PR, Pedersen S, Williston BJ. Maintenance of a health promotion program in elementary schools: results from the CATCH-ON study key informant interviews. Health Education and Behaviour 2003; 30(4): 503-518.
28. Draper CE, Kolbe-Alexander TL, Lambert EV. Factors contributing to the success of a physical activity-based health promotion programme: a retrospective evaluation. Journal of Physical Activity and Health 2009; 6(5): 578-588.
29. Draper CE, de Kock L, Grimsrud AT, Rudolph M, Nemutandani MS, Kolbe-Alexander TL et al. Evaluation of the implementation of a school-based physical activity intervention in Alexandra township, South Africa. South African Journal of Sports Medicine 2010; 22(1): 12-19.
30. Statistics South Africa. Provincial Profile 2004 - Limpopo. (Online) 2004. Available: http://www.statssa.gov.za/Publications/Report-00-91-09/Report-00-91-092004.pdf (Accessed 31 July 2009).
31. Shin Y, Yun S, Pender NJ, Jang H. Test of the health promotion model as a causal model of commitment to a plan for exercise among Korean adults with chronic disease. Research in Nursing and Health 2005; 28(2): 17-125.
32. Aronson RE, Wallis AB, O'Campo PJ, Whitehead TL, Schafer P. Ethnographically informed community evaluation: a framework and approach for evaluating community-based initiatives. Maternal and Child Health Journal 2007; 11(2): 97-109.
33. Marshall C, Rossman GB. Designing qualitative research, 2nd edn. Thousand Oaks, CA: Sage, 1995.
34. Kitzinger J. Focus groups with users and providers of health care. In: C Pope and N Mays (Eds). Qualitative research in health care 2nd edn. London: BMJ Books, 2000; 20-29.
35. Mopani District Municipality. Mopani District Municipality: Reviewed integrated development plan for 2007/8 (Online) 2006. Available: http://www.mopani.gov.za/docs/2007-2008IDP.pdf (Accessed 31 July 2009).
36. Ridde V. Reducing social inequalities in health: public health, community health or health promotion? Promotion and Education 2007; 14(2): 63-67.
37. Smith MA, Garbharran H, Edwards MJ, O'Hara-Murdock P. Health promotion and disease prevention through sanitation education in South Africa Zulu and Xhosa women. Journal of Transcultural Nursing 2004; 15(1): 62-68.






