In the public health service sector, chronic diseases are a serious economic and social burden, affecting individuals and entire communities. Chronic diseases increase the mortality rate and are a primary reason for the rising costs of medical care1-3. Great emphasis has been placed on the necessity for preventive measures and the promotion of health-related measures, according to Chronic Care Model (CCM), which is a guide to chronic care improvement4. These measures can slow down or even stop the process of chronic diseases5. According to the CCM guidelines, the most effective way to assess health care provided to chronically ill patients is to measure such elements as quality of life (an essential healthcare outcome or 'medical endpoint', which prevents relapses, alleviates symptoms and increases patients' satisfaction with health care), healthy behaviors and healthcare utilization6. Effective chronic illness management requires an appropriately organized delivery system linked with complementary community resources available outside the organization4.
Quality of life (QoL) is believed to be a multidimensional concept, and evaluated with regard to its physiological, psychological and social aspects7. The measure of QoL has often been used to determine health status and functional wellbeing of people suffering from chronic or specific diseases8. The nationwide initiatives improve QoL, promoting healthy behaviors and prevention of diseases among patients of all ages as main goals of public health9 as well as essential healthcare outcomes of CCM4.
Rural lifestyles are less comfortable than urban lifestyles, which may influence health-related quality of life10. However, information on this issue remains very scanty. Lifestyle, including health behaviors, is rated close to biological, genetic and social factors, as well as the availability and quality of medical care as the main determinant of health11. Both scientific studies and government programs concerning health concentrate on health-related behaviors demonstrated by individuals and whole communities as primary fundamentals of prevention programs12. Positive health habits have been proven to postpone mobility problems or disability in later life13. Research has described the situation of various behaviors occurring together to turn into certain lifestyles14. Studies have also investigated how the combination of particular behaviors contributes to specific health conditions15. Reports show that we can delay death by increasing the number of healthy behaviors and reducing the number of detrimental or risky ones16. Scientists predict that the average life span will decline unless the number of unhealthy behaviors is reduced17.
Residents of rural areas are being increasingly identified as people at risk of health disparities9. Rural areas are characterized by higher unemployment and more severe poverty, as well as lower levels of education, and more difficult access to health and social services18. Differences in health results of rural and urban dwellers can be caused by these factors19. Rural inhabitants have generally worse parameters of physical and mental health than their urban counterparts; for example, in the USA, the higher prevalence of chronic obstructive pulmonary disease and chronic health conditions, as well as a higher mortality rate (both general number of deaths and number of deaths as a consequence of unintentional injuries) have been noted in rural areas. The research involving adult rural residents suggests the importance of abode for social epidemiology and public health concerns20. Place of residence and geographical factors play a role in the assessment of health status, healthcare utilization and health service deficits, adequacy of health care and health-related behaviors. It has long been believed that where people live, work and relax either protects and promotes health or generates health hazards21. Rural residences themselves have proven to be a risk factor of obesity22, diabetes23 and cardiovascular diseases24. It has also been suggested that health-related behaviors of rural dwellers may differ from those demonstrated by people in urban areas. Researchers have shown that patients from both rural and urban regions tend to choose unhealthy behaviors rather than health-promoting ones25. For example, a low perception of risk has been observed in rural areas for heart disease, sun exposure and skin cancer26.
In 2011, 39.8% of the Polish population resided in rural areas (vs 38.2% in 2002); 25.6% of all medical practices and 22.6% of all consultations provided per year in medical practices were in rural parts of Poland. The life expectancy for 60-year-old rural residents is shorter than for their urban counterparts (rural areas - women 23.6 years, men 18.0 years; vs urban areas - 23.8 years and 18.9 years, respectively). In 2011, 197 800 people settled in rural regions, while 158 000 moved to urban areas27.
The purpose of this study was to describe rural and urban disparities in quality of life and health-related behaviors among chronically ill patients. The authors also wanted to identify variables related to the high QoL and health-related behavior levels in rural areas, including effects of healthcare utilization on health status and health-related behaviors.
Family doctors were recruited by the authors through regional Continuing Medical Education centers between January and June 2010. The chronically ill subjects were recruited as described below from patients of 434 family doctors between July 2010 and June 2012. The study comprised 1239 chronically ill primary care patients from rural areas in Poland (eligible patients; response rate: 62.0%). The analyzed group was compared with the urban group, homogeneous (with the same structure) in respect of gender and age (n=1886) (Fig1).
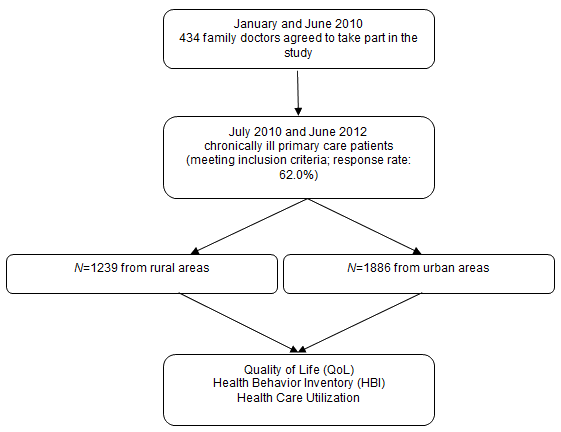
Figure 1: Flow chart of the study
The family doctors invited patients with age ≥18 years and a diagnosis of at least one chronic disease to participate anonymously in the study. A chronic disease was defined as a disease of long duration (longer than 3 months) and generally slow progression. Patients with the following criteria were excluded: active cancer disease (defined as cancer diagnosis under current treatment with radiotherapy or chemotherapy), moderate to severe dementia, severe mental disorders or any problems that hinder active participation in the intervention (eg non-Polish speaking patients). Those who agreed to take part in the project signed an informed consent form. The patients were given a questionnaire to complete at home and return in a closed envelope.
Power analysis
The χ2 goodness-of-fit test was used to check whether sample allocation was proportional in respect of gender, age, education and marital status. To unify the age and gender strata in rural and urban sub-samples, stratified random sampling with proportional allocation was performed in the urban sub-sample with reference to the frequency distribution in the rural sub-sample strata. A computer 'random number' generator from the statistical package R v2.10.1 (for Mac OS X Cocoa GUI) (http://cran.r-project.org/bin/macosx) was used for sampling. Then the urban sub-sample was used for calculations. Biased estimators were calculated on the basis of this sub-sample. The size of the rural sample was 1239, which means that the obtained estimator for any unknown population proportion has a probability of at least 0.95 of being no farther than d=0.028 from the population proportion. Respectively, for the size of urban sample (1886), the value of d=0.023.
Research tools
Quality of life (QoL) was measured using the Polish version of the World Health Organization Quality of Life Instrument Short Form (WHOQOL-BREF) developed by Wołowicka and Jaracz28. The WHOQOL-BREF is a generic QoL instrument that has been designed to be applied in different conditions or cultures29. It is a shorter version of the WHOQOL-100, developed by the WHO Group for the Research on Quality of Life. It is suggested that the WHOQOL-BREF provides a valid and reliable alternative to the assessment of domain profiles with the WHOQOL-100, and is especially sensitive to the health-related QoL status of those with chronic diseases29. The authors of this study employed the WHOQOL-BREF questionnaire because it had been validated for the Polish population. The first two questions (about satisfaction with QoL and health state) are analyzed separately. All answers are rated on a five-point Likert scale, where 1 is very dissatisfied and 5 is very satisfied. The WHOQOL-BREF can be used to measure quality of life in four domains: physical, psychological, social relationship and environment. The reliability of the Polish version of the WHOQOL-BREF questionnaire, measured with the α-Cronbach coefficient, is very high, which refers both to the parts evaluating particular domains (results from 0.69 to 0.81) and the questionnaire as a whole (0.90)29.
The Health Behavior Inventory (HBI) developed by Juczyński30 was used to measure four categories of health behaviors (HB) reported to promote health and prevent diseases: healthy eating habits (HEH), preventive behaviors (PB), positive mental attitudes (PMA) and health practices (HP) (α-Cronbach coefficient 0.85) (Table 3)30. Questions were answered using a five-point scale (where 1 is almost never and 5 is almost always), resulting in a total score of 24 to 120 (the higher the score, the greater number of health behaviors). Scores were also calculated for the four sub-scales (a result being the sum of all answers within a particular sub-scale was divided by six)30.
Ethics approval
The research was conducted in accordance with the principles of the Declaration of Helsinki. The study was approved by the Bioethical Commission of the Medical University in Wroclaw, Poland (approval no. KB-608/2011).
Statistical analysis
A distribution free method, Wilcoxon's rank sum test, was used to assess whether two populations had the same location (for quantitative variables). The analysis of qualitative variables was based on contingency tables and the χ2 test. Categorical variables were reported as frequencies (%) and continuous variables as means and standard deviations (SD) for normally distributed data and median (min, max, IQR) for data not normally distributed. The Spearman rank correlation test was applied to check correlations between the variables. Overall results of the WHOQOL-BREF and the Health Behavior Inventory did not have normal distribution, which was confirmed by the Shapiro-Wilk normality test.
Analysis of logistic regression was used to examine the impact of variables on odds ratio (OR) of QoL measured by the WHOQOL-BREF. The R v2.10.1 (see below) statistical software was used for all data analyses. The level of statistical significance was set at p<0.05 for all analyses.
The mean age was 61.8±15.0 years. The respondents were mostly women (61.3%, 759), married individuals (67.6%, 832), and those with vocational education (35.9%, 443). Accurate sociodemographic data of the patients are shown in Table 1. The top 10 diagnoses of the patients from rural and urban areas are presented in Table 2. The results of the WHOQOL-BREF and the HBI are presented in Table 3.
Table 1: Sociodemographic data of patients from rural and urban areas
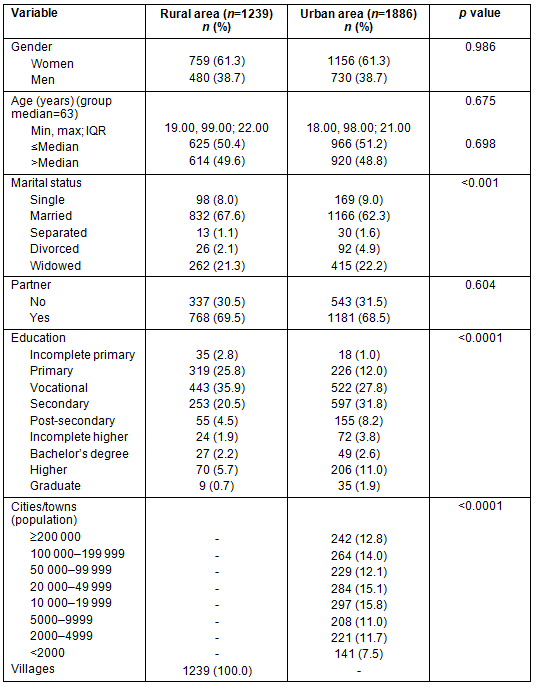
Table 2: Top 10 diagnoses in patients from rural and urban areas
(detected by multiple-choice questions with multiple answers)
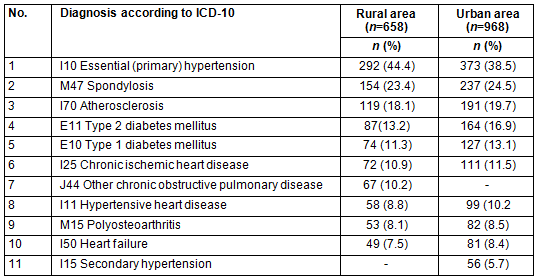
Table 3: WHOQOL-BREF and HBI results
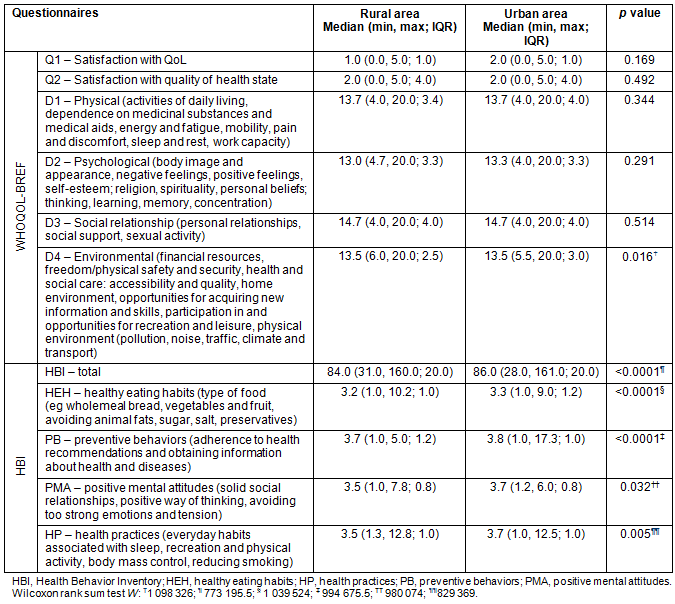
The mean score for questions regarding satisfaction with QoL was lower than for questions about satisfaction with health. The highest scores were obtained in Domain 3 (Social relationship) and the lowest in Domain 2 (Psychological). Only the results in Domain 4 (Environmental) were statistically significantly higher among patients from rural areas.
The highest scores within the HBI were observed in the PB category. The lowest scores were noted in HEH. All results of HBI were statistically significantly higher in patients from urban areas.
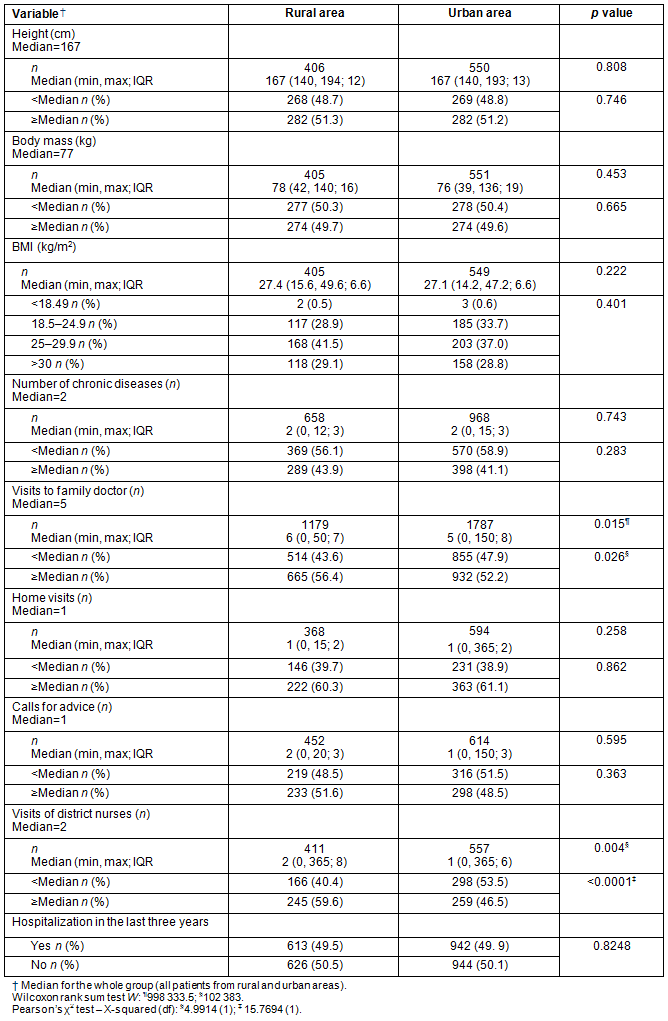
The analyzed descriptive variables are shown in Table 4. More visits to a family doctor and fewer visits of district nurses were observed among the rural patients. Statistically significant differences between the patients from rural and urban areas were only noted in healthcare utilization.
Table 4: Descriptive statistics of patients from rural and urban areas
Pictograms of correlation coefficients between the questionnaire outcomes and demographic and clinical data for patients from rural and urban areas are shown in Table 5. According to the results of correlations, in rural and urban areas, lower satisfaction with QoL and health was noted more often among patients who were younger, had life partners, had a higher education, had a low BMI, had a lower number of chronic diseases and used healthcare services less often. In urban areas, lower satisfaction with QoL and health was observed more often among patients having low body mass. Lower QoL scores within all domains were observed more often among older and shorter patients, those without life partners, with a lower education level, with a greater number of chronic diseases, who often visit family doctors, and who have more home visits, call for advice more often, are more often visited by district nurses, and had been hospitalized during the last 3 years. Additionally, lower scores were noted in domains D1, D2 and D3, mainly among urban patients with higher body mass and BMI, in domain D2 among urban women, and in domain D4 among urban women, rural patients with lower body mass and urban patients with higher body mass and BMI.
Table 5: Pictograms for correlation coefficients between the questionnaire outcomes, demographic and clinical data of patients from rural (r) and urban (u) areas
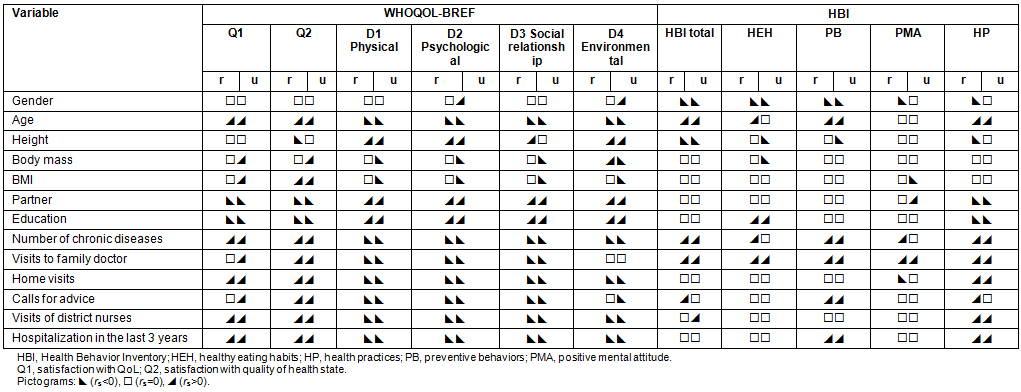
Low scores within the HBI and all four categories were more common among men, younger patients, those with a greater number of chronic diseases and who visit the family doctor less frequently. Additionally, lower scores were noted within the HBI mainly among taller patients, and those calling for advice less frequently; HEH in patients with lower education; PB in patients calling for advice less frequently, and not hospitalized during the last three years; PMA in patients having more home visits; HP in patients having fewer home visits, calling for advice and visited by district nurses less often, and not hospitalized during the last 3 years.
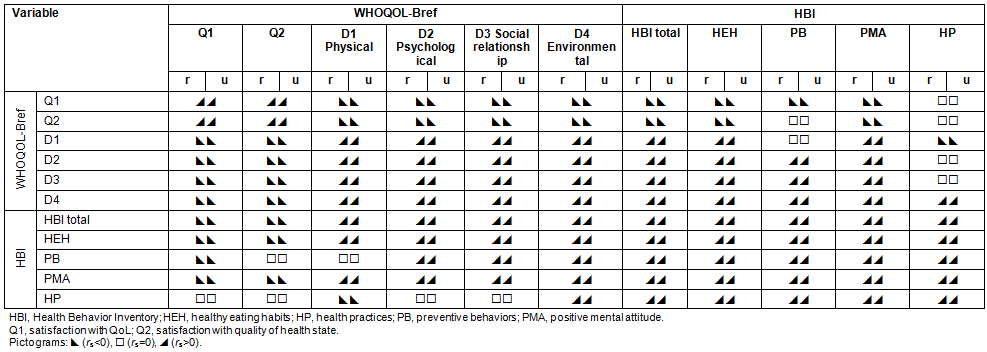
Pictograms of correlation coefficients between the questionnaire outcomes for patients from rural and urban areas are shown in Table 6. We found that all correlation coefficients between the questionnaire outcomes for patients from rural and urban areas had the same sign (both rural and urban were either positive, negative or zero). The strongest correlations in both groups within the WHOQOL-BREF were observed between D1 and D2 and D2 and D4. HB correlated strongest with D4. Within particular HB categories, the levels of HEH and PMA correlated strongest with D2 and the levels of PB and HP correlated with D4. Within the HBI, the strongest correlations were observed between the overall level of HB and PB. Within particular HB categories, the strongest correlations were noted between PMA and PB.
Table 6: Pictograms for correlation coefficients between the questionnaire outcomes of patients from rural (r) and urban (u) areas
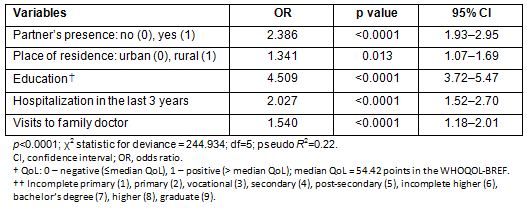
The results of logistic regression are presented in Table 7. Odds ratio for QoL (0(-) QoL ≤ median QoL (54.4 points), 1(+) QoL > median QoL (54.4 points)) was as follows: in the case of education level (graduate (9) vs incomplete primary (1)): OR9|1=4.509 (95% CI: 3.72-5.47), partner's presence (yes (1) vs no (0)): OR1|0=2.386 (95% CI: 1.93-2.95), hospitalization in the last 3 years (0 vs 4 hospitalizations): OR0|4=2.03 (95% CI: 1.52-2.70), visits to family doctor during last 12 months (0 vs 10 visits): OR 0|10=1.540 (95% CI: 1.18-2.01), place of residence (rural (1) vs urban (0)): OR1|0=1.341 (95% CI: 1.07-1.69).
Table 7: Coefficients of logistic regression for Quality of Life?
Discussion
International literature provides relatively little information on rural and urban disparities in QoL and health-related behaviors of chronically ill patients, or the influence of QoL and health-related behaviors on medical care utilization31.
Quality of Life and rural-urban disparities
Living in rural settings is recognized as a strong determinant of health-related QoL. While rural residence has positive impacts on mental health, it negatively affects physical health-related QoL. Other important contributors to a low physical health-related QoL include being retired or receiving social pension, long-term illness, and consulting a medical specialist. Higher education and access to medical specialist care improve QoL related to mental health32. However, statistically significant differences between the levels of satisfaction with QoL and satisfaction with health between the analyzed groups were not found. The only statistically significantly higher results in rural patients were noted within the environmental domain concerning: financial resources, freedom/physical safety and security, health and social care, accessibility and quality home environment, opportunities for acquiring new information and skills, participation in and opportunities for recreation/leisure, physical environment (pollution, noise, traffi and climate) and transportation. Also, Amarasinghe et al. implied that the surrounding environment may be a factor in deciding people's health and quality of life33. Breeze et al. concluded that policy should take into account both the community level interventions and those directed at individuals34.
It was noticed that the correlations between the analyzed variables and the declared satisfaction with QoL and health differed from the correlations between the variables and QoL results within particular domains. Older patients declare higher levels of satisfaction with QoL and health, but the correlations between the results of Physical and Psychological domains demonstrate higher satisfaction levels in the group of younger patients. Also, patients with a high level of healthcare utilization declared high levels of satisfaction with QoL and health, but correlations between the results of Physical and Psychological domains suggested higher results in the group of patients with low levels of healthcare utilization. Similar observations were made by Jakobsson et al., who noted lower QoL levels among patients often using healthcare services and higher QoL in patients with lower levels of healthcare utilization especially in primary care35.
Differences in the contributors to lower QoL between rural and urban areas included variables such as height, body mass and BMI. It may be associated with different social expectations in urban and rural areas. Analogous results and conclusions concerning QoL in the psychological domain were reported by Probst et al36..
Health-related behavior disparities
Unhealthy behaviors are typical of most patients, especially younger ones37, which was also confirmed by the findings. Rural areas themselves were a risk factor of low HB levels in this study. All results of HBI were statistically significantly higher in patients from urban areas, with the greatest differences observed within HEH and PB.
The review of literature concerning health-related behaviors also led to the conclusion that sociodemographic factors, such as gender and place of residence, play an important part in shaping health38, which was also supported by the results. It was also found that factors such as age, height, body mass, BMI, number of chronic diseases and level of health utilization may contribute to lower level of HB.
Residents of rural areas have lower results of HBI and are more likely to be obese than people from urban areas39. According to Liebman et al40., overweight and obesity in rural communities are caused by physical inactivity and unhealthy eating behaviors, such as drinking sweetened beverages and eating during other activities (eg while watching television). The majority of patients involved in this study were either overweight or obese. And yet, no statistically significant differences in body mass, height or BMI between rural and urban dwellers were found. It can be explained by the homogeneity of both groups in respect of gender, age and chronic diseases. Also, data provided by the Polish National Multicenter Health Survey (WOBASZ), which measured the influence of socioeconomic factors on the incidence of overweight and obesity in the Polish population, show that the occurrence of overweight does not depend on the place of residence11.
Some data demonstrate significant correlations between body mass and HB41. The presented results confirmed this factor only in the case of urban residents, whose higher levels of HEH were accompanied by lower body mass, and higher levels of PMA by a lower BMI. Similarly, in the study conducted by Kawalec et al. on a group of patients with overweight and obesity, body mass correlated negatively with healthy eating habits42.Theoretically, the awareness of being obese should lead to changes in one's lifestyle, but according to Bąk-Sosnowska and Zahorska-Markiewicz43, it appears that obese people perceive themselves as slimmer than they really are, and their body image remains the same despite weight reduction. Almost half of overweight subjects in the study carried out by Suliburska et al. did not make any effort to lose weight44.
Similar to other studies45,46, the one presented here shows that in rural populations, women and older patients have higher results in all HB categories, and those better educated have higher results in HEH.
Oyhenart et al47. assert that differences in eating habits may result from different educational backgrounds. The authors of this study concluded that a higher level of education correlates with a higher level of HEH and a lower level of HP.
Higher levels of health behaviors are observed among chronically ill patients. They more often take up health practices associated with rest, regular sleep, body mass control, limitation of smoking, and avoiding excessive physical effort48. The presented results proved that it refers mainly to chronically ill patients from rural areas, and the presence of chronic diseases has positive effects on the level of health behaviors.
Expected impact of the study
The presented findings can be useful for public health practitioners who are interested in developing population-level prevention-focused interventions, the aim of which is to improve the quality of health and health-related behaviors among rural chronically ill patients. The results may also help to understand how place of residence affects a person's health and increases the awareness of the need for the development of targeted public health interventions.
Limitations
Several salient points in this study are worth emphasizing. So far, very little research has been conducted in a rural primary care setting among chronically ill patients in Poland, even though they are frequent recipients of healthcare services. The findings presented here are based on the analysis of active users of healthcare services. The fact that the participants were selected with regard to chronic diseases gave the authors the opportunity to assess the influence of this variable on QoL and health behaviors. The authors did not consider the somatic status of the patients. Future research including somatic status would enable the analysis of correlations between health behaviors and the intensity of somatic complaints. Inclusion of a control group without chronic diseases in the study could also be of benefit.
Higher QoL may reduce the intensity of healthcare utilization among residents of rural and urban areas. In order to improve QoL of chronically ill patients from rural and urban areas, the relationships between physical and mental states, as well as environmental factors, should be taken into consideration. Educational programs promoting health behaviors should be primarily addressed to rural patients, men, younger individuals, patients with a lower number of chronic diseases, and those using healthcare services less often. The deciding factor about the level of HB demonstrated by rural and urban patients in all categories is the frequency of visiting a family doctor. Regular contact with a doctor, and receiving instructions about health promotion and prevention of diseases, enhances the chances of chronically ill patients changing their health behaviors.
Acknowledgements
The authors would like to thank all the patients who agreed to participate in the research, along with the managers of primary healthcare centers, where recruitment of respondents was conducted.
References
1. Starfield B, Shi L. Policy relevant determinants of health: an international perspective. Health Policy 2002; 60(3): 201-218.
2. Wolff JL, Starfield B, Anderson G. Prevalence, expenditures, and complications of multiple chronic conditions in the elderly. Archives of Internal Medicine 2002; 162(20): 2269-2276.
3. Starfield B. Primary care: balancing health needs, services and technology. Oxford: Oxford University Press, 1998.
4. Wagner EH, Austin BT, Davis C, Hindmarsh M, Schaefer J, Bonomi A. Improving chronic illness care: translating evidence into action. Health Affairs 2001; 20: 64-78.
5. Phillips G, Renton A, Moore DG, Bottomley C, Schmidt E, Lais S, et al. The Well London program - a cluster randomized trial of community engagement for improving health behaviors and mental wellbeing: baseline survey results. Trials 2012; 13: 105.
6. Cao WJ, Chen CS, Hua Y, Li YM, Xu YY, Hua QZ. Factor analysis of a health-promoting lifestyle profile (HPLP): application to older adults in Mainland China. Archives of Gerontology and Geriatrics 2012; 55(3): 632-638.
7. Brown J, Bowling A, Flynn TN. Models of quality of life: a taxonomy and systematic review of the literature. Report commissioned by European Forum on Population Ageing Research/Quality Life, University of Sheffield, 2004.
8. Melberg K. Farming, stress and psychological well-being: the case of Norwegian farm spouses. Sociologia Ruralis 2003; 43: 56-9.
9. US Department of Health and Human Services. Healthy People 2020. Available: http://www.healthypeople.gov/2020/default.aspx (Accessed 11 October 2012).
10. Gilbert LA. Women at midlife: current theoretical perspectives and research. Women & Therapy 2003; 14: 105-115.
11. Health 21 - health for all in the 21st century: The Health for All Policy Framework for the WHO European Region. Available: http://www.euro.who.int/en/publications/abstracts/health21-the-health-for-all-policy-framework-for-the-who-european-region (Accessed 11 October 2012).
12. US Department of Health and Human Services. Healthy People 2010. Available: http://www.healthypeople.gov/ (Accessed 11 October 2012).
13. Liao W-C, Li C-R, Lin Y-C, Wang C-C, Chen Y-J, Yen C-H, et al. Healthy behaviors and onset of functional disability in older adults: results of a National Longitudinal Study. Journal of the American Geriatrics Society 2011; 59(2): 200-206.
14. Conry MC, Morgan K, Curry P, McGee H, Harrington J, Ward M, et al. The clustering of health behaviours in Ireland and their relationship with mental health, self-rated health and quality of life. BMC Public Health 2011; 11: 692.
15. Wilsgaard T, Emaus N, Ahmed LA, Grimnes G, Joakimsen RM, Omsland TK et al. Lifestyle impact on lifetime bone loss in women and men. American Journal of Epidemiology 2009; 169(7): 877-886.
16. Shaw BA, Agahi N. A prospective cohort study of health behavior profiles after age 50 and mortality risk. BMC Public Health 2012; 12(1): 803.
17. Garrow JS, James WPT, Ralph A. Human nutrition and dietetics. London: Churchill Livingstone, 2000.
18. Moore C, Probst J, Tompkins M, Cuffe S, Martin A. Poverty, stress, and violent disagreements in the home among rural families. South Carolina Rural Health Research Center, 2005. Available: http://rhr.sph.sc.edu (Accessed 11 October 2012).
19. Filip RS, Zagorski J. Osteoporosis risk factors in rural and urban women from the Lublin Region of Poland. Annals of Agricultural and Environmental Medicine 2005; 12: 21-26.
20. Berke EM. Geographic Information Systems (GIS): recognizing the importance of place in primary care research and practice. Journal of the American Board of Family Medicine 2010; 23: 9-12.
21. Cummins S, Curtis S, Diez-Roux AV, Macintyre S. Understanding and representing 'place' in health research: a relational approach. Social Science & Medicine 2007; 65: 1825-1838.
22. Lutfiyya MN, Lipsky MS, Wisdom-Behounek J, Inpanbutr-Martinkus M. Is rural residency a risk factor for overweight and obesity for U.S. children? Obesity (Silver Spring) 2007; 15: 2348-2356.
23. Krishna S, Gillespie KN, McBride TM. Diabetes burden and access to preventive care in the rural United States. Journal of Rural Health 2010; 26: 3-11.
24. Schwartz F, Ruhil AV, Denham S, Shubrook J, Simpson C, Boyd SL. High self-reported prevalence of diabetes mellitus, heart disease, and stroke in 11 counties of rural Appalachian Ohio. Journal of Rural Health 2009; 25: 226-230.
25. The World Health Report 2008. Primary Health Care. World Health Organization, WHO Press, 2008.
26. Bury G, Dowling J. Community cardiac awareness teaching in a rural area: the potential for a health promotion message. Resuscitation 1996; 33: 141-145.
27. CSO - Central Statistical Office. Concise Statistical Yearbook of Poland 2012. Available: http://www.stat.gov.pl/cps/rde/xbcr/gus/oz_maly_rocznik_statystyczny_2012.pdf (Accessed 11 October 2012).
28. Wołowicka L, Jaracz K. Polska wersja WHOQOL - WHOQOL-100 i WHOQOL-Bref. In: L Wołowicka (Ed.). Quality of life in medical sciences. Poznań: Dział Wydawnictw Uczelnianych Akademii Medycznej, 2001.
29. Jaracz K, Kalfoss M, Górna K, Baczyk G. Quality of life in Polish respondents: psychometric properties of the Polish WHOQOL-Bref. Scandinavian Journal of Caring Science 2006; 20(3): 251-260.
30. Juczyński Z. Narz?dzia pomiaru w promocji i psychologii zdrowia. Pracownia Testów Psychologicznych, Warszawa, 2009.
31. Frohlich KL, Corin E, Potvin L. A theoretical proposal for the relationship between context and disease. Sociology of Health & Illness 2001; 23: 776-797.
32. Zagozdzon P, Kolarzyk E, Marcinkowski JT. Quality of life and rural place of residence in Polish women - population based study. Annals of Agricultural and Environmental Medicine 2011; 18(2): 429-432.
33. Amarasinghe A, D'Souza G, Brown Ch, Oh H, Borisova T. The influence of socioeconomic and environmental determinants on health and obesity: a West Virginia case study. International Journal of Environmental Research and Public Health 2009; 6: 2271-2287.
34. Breeze E, Jones DA, Wilkinson P, Bulpitt CJ, Grundy C, Latif AM, et al. Area deprivation, social class, and quality of life among people aged 75 years and over in Britain. International Journal of Epidemiology 2005; 34(2): 276-283.
35. Jakobsson U, Kristensson J, Hallberg IR, Midlöv P. Psychosocial perspectives on health care utilization among frail elderly people: an explorative study. Archives of Gerontology and Geriatrics 2011; 52(3): 290-294.
36. Probst J, Laditka S, Moore C, Harun N, Powell M. Depression in rural populations: prevalence, effects on life quality, and treatment seeking behavior. Rural Health Research Center 2005. Available: http://rhr.sph.sc.edu/report/SCRHRC_Depression_Rural_Exec_Sum.pdf (Accessed 01 October 2012).
37. Seo DC, Nehl E, Agley J, Ma SM. Relations between physical activity and behavioral and perceptual correlates among midwestern college students. Journal of American College Health 2007; 56(2): 187-197.
38. Carroll SL, Lee RE, Kaur H, Harris KJ, Strother ML, Huang TT. Smoking, weight loss intention and obesity-promoting behaviors in college students. Journal of the American College of Nutrition 2006; 25(4): 348-353.
39. Gacek M. Selected health habits of the group of women in the rural and urban environment according to their socio-economic and nutritional status. Problemy Higieny i Epidemiologii 2011; 92: 260-266.
40. Liebman M, Pelican S, Moore SA, Holmes B, Wardlaw MK, Melcher LM, et al. Dietary intake, eating behavior, and physical activity-related determinants of high body mass index in rural communities in Wyoming, Montana, and Idaho. International Journal of Obesity and Related Metabolic Disorders 2003; 27(6): 684-692.
41. Ostrowska L, Karczewski J, Szwarc J. Dietary habits as an environmental factor of overweight and obesity. Roczniki Państwowego Zakładu Higieny 2007; 58(1): 307-313.
42. Kawalec E, Reczek A, Porębska A, Brzostek T, Malinowska-Lipień I. Health-related behaviour of patients affected by obesity and overweight. Pielęgniarstwo XXI wieku 2011; 2(35): 27-33
43. Bąk-Sosnowska M, Zahorska-Markiewicz B. The imaginary picture of one's own body in overweight woman and its influence on weight reduction therapy. Endokrynologia, Otylosc i Zaburzenia Przemiany Materii 2009; 5(4): 192-197.
44. Suliburska J, Bogdański P, Pupek-Musialik D, Głód-Nawrocka M, Krauss H, Piątek J. Analysis of lifestyle of young adults in the rural and urban areas. Annals of Agricultural and Environmental Medicine 2012; 19(1): 135-139.
45. Binkowska-Bury M, Kruk W, Szymanska J, Marc M, Penar-Zadarko B, Wdowiak L. Psychosocial factors and health-related behavior among students from South-East Poland. Annals of Agricultural and Environmental Medicine 2010; 17(1): 107-113.
46. Łagowska K, Woźniewicz M, Jeszka J. Comparison of eating habits among students with admitted sex and level of physical activity. Roczniki Państwowego Zakładu Higieny 2011; 62(3): 335-342.
47. Oyhenart EE, Castro LE, Forte LM, Sicre ML, Quintero FA, Luis MA et al. Socioenvironmental conditions and nutritional status in urban and rural schoolchildren. American Journal of Human Biology 2008; 20(4): 399-405.
48. Kurowska K, Bialasik B. Health behaviors and coping with disease in patients of Accident and Emergency Ward (A&E WARD). Nowiny Lekarskie 2009; 2: 113-122.



