Current asthma management has reduced asthma mortality in Australia. The National Asthma Council (NAC) cites recent figures from the Australian Bureau of Statistics that show the asthma death rate to have fallen to its lowest in 5 years, from 454 deaths in 2000 to 422deaths in 20011. The NAC attributes the reduction in asthma mortality to better asthma management and education. Improved asthma management strategies include: increased general practitioner involvement; use of preventive medicine and asthma plans; and increased community awareness of asthma, meaning that 'people are getting help earlier'2.
In spite of these gains, the prevalence of asthma is increasing and the resultant morbidity is a significant burden on the community. It is estimated that between 45% and 55% of the total cost of asthma is related to lost productivity3. In 1999, in recognition of the burden of asthma, the Commonwealth Minister of Health identified asthma as an Australian National Health Priority Area.
It is widely acknowledged in the literature that improved management is the key to reducing the severity and frequency of asthma exacerbations and their associated mortality4. After widespread consultation and information gathering, the NAC published the National Asthma Strategy Implementation Plan 1999, a document that brought together current and proposed efforts to improve asthma health outcomes in a coordinated way5. While this work and much other literature focused on disease treatment and outcomes of the various treatment modalities,4,6 few publications addressed the implementation of asthma management models.
The Loddon Mallee region (LMR) of Victoria, Australia, is located in the north-west corner of the State. It has a diverse geographic area of approximately 60 000 km2, or 26% of the State, making it the largest of the 9 Victorian Department of Human Services (DHS) regions. In 1996, the population of the LMR was estimated at approximately 283 705. Bendigo, Mildura, Swan Hill and Echuca are the major cities in the region and they service the smaller towns and surrounding rural areas.
The prevalence of asthma in the LMR is approximately 1% higher than the Victorian average. Four local government areas in the LMR have close to double the State average hospital admission ratios for asthma7. In recognition of these issues, the regional DHS provided funding to the Bendigo Health Care Group's (BHCG) Collaborative Health, Education and Research Centre to research management of asthma in the region.
This paper describes the development of standardised documentation designed to assist health providers to manage asthma according to best practice.
The project
The aim of the project was to develop a regional asthma management model (RAMM) based on a uniform approach to management and which operationalised the recommendations of the National Asthma Campaign.
The project objectives were to:
- Identify best practice in management
- Develop a profile of current management strategies in the LMR
- Identify gaps between present practice and best practice in management
- Develop a framework for best practice in management
- Assist acute hospitals in the region to develop a strategy for implementing best practice in management.
The scope of this project covered the diverse LMR and involved key regional stakeholders, including health professionals from acute and community settings, health service providers, general practitioners, pharmacists, asthma educators and consumers.
Methods
Literature review
A review of the literature was undertaken to identify best practice. The MEDLINE and CINAHL databases were searched using key words 'asthma' and 'management'. The Cochrane Library was also searched to identify evidence-based best-practice asthma management.
Workbooks and subregional workshops
Identified aspects of best practice were used as the basis of questions developed into workbooks by the project team. The workbooks were designed to profile current asthma management practice in the LMR and to compare it with identified best-practice in the literature. The workbooks were distributed to all acute hospitals, community health centres and asthma educators in the region. Five subregional workshops obtained additional information from workbook respondents.
General practitioner survey
All general practitioners (GPs) working in the LMR were surveyed to identify their current range of asthma management strategies and to obtain their views on how management could be improved.
Consumer focus groups
Input was sought from people with asthma about their asthma management and ideas for its improvement. Due to the diversity of the region, consumers were accessed in a variety of ways. A focus group was held in an urban area and individual interviews were held in two rural/remote areas in the region.
Reference group and documentation design team
A multidisciplinary reference group provided guidance to the project. A documentation design team was convened to develop the asthma clinical pathway and to ensure it and other documentation reflected the diverse needs of the region.
Results
Of the 19 workbooks sent to individual acute hospitals 15 (78.9%) were completed and returned; 13 of 14 workbooks (92.8%) sent to individual community health centres were completed and returned. Fourteen of 15 asthma educators identified in the LMR were employed in the acute hospitals and community health centres that returned the workbooks; one asthma educator worked privately.
The number of people treated for asthma in EDs throughout LMR varied from 5 to more than 250 patients per year. Among workbook respondents, 29% stated that their hospital had no ED protocols for asthma, 36% used NAC guidelines, 21% used emergency nursing guidelines and the remaining 14% used protocols developed by the local GP or director of nursing. To the workbook question 'Should a formal ED protocol be implemented'?, 100% of respondents answered 'Yes'.
Of the 215 GP surveys distributed, 38 surveys (17.6%) were returned. The majority of GP respondents supported developing a uniform regional approach to asthma management based on NAC guidelines, but due to the low response rate, this finding must be viewed with caution.
Consumer focus groups identified panic associated with acute exacerbation of asthma. To increase confidence in management, consumers suggested that treating doctors/EDs provide patients and carers with written instructions regarding acute asthma attacks and advice on management strategies for the ensuing 24-48 hours.
Collation of data from consumer interviews, workbooks, and workshops, profiled current asthma management strategies in the region. This regional profile of asthma management practice was compared with identified best practice. Gaps in practice and services were identified and responsive recommendations formulated by the project team.
RAMM documentation
The RAMM provides guidance for standardised management of a person suffering an acute exacerbation of asthma in the community, through the ED and back to the community (Figure 1)8.
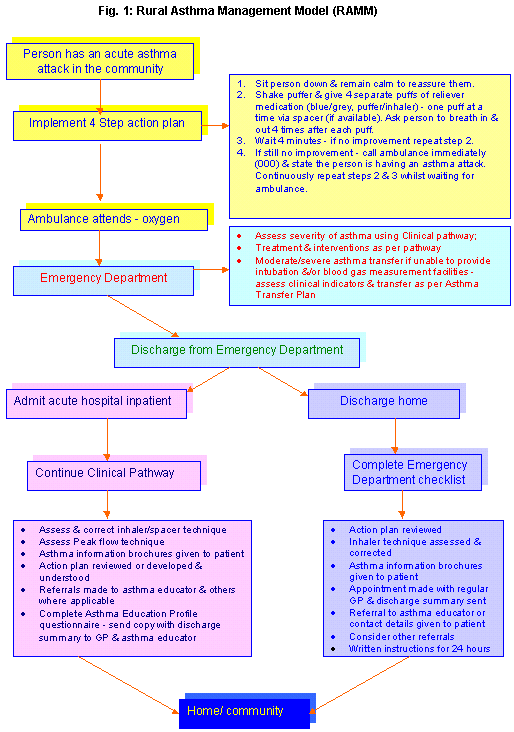
Figure 1: Rural Asthma Management Model (RAMM) developed for the Loddon Mallee region health services, Victoria, Australia.
Discussion in the workshops and with the project Advisory committee verified that regional EDs required a documentation package to standardise asthma assessment, management and transfer. A documentation package that included the Regional Asthma Clinical Pathway and Emergency Department (ED) Package was designed to assist regional health professionals achieve best practice asthma management.
Regional Asthma Clinical Pathway: A pathway was designed, based on the NAC, Scottish Intercollegiate Guidelines Network (SIGN)9,10, the Royal Children's Hospital, (Melbourne, Australia) asthma clinical pathway, the Western Hospital's (Melbourne, Australia) evidence-based clinical guidelines for Hospital Management of Acute Asthma, and advice and opinions from respected experts and clinicians. Levels of evidence for the pathway and guidelines for use are included in the RAMM. The regional asthma clinical pathway was developed as a template for use by all hospitals in the Loddon Mallee region.
The design team sent drafts of the pathway to key stakeholders for comment and modifications were made accordingly. The projects Reference group ratified the pathway. What resulted was a regional asthma clinical pathway designed by clinicians for clinicians. The pathway commences in the ED and flows through the inpatient setting to discharge planning and patient return to the community. Designed in stages rather than days, the pathway outlines interventions for each stage of asthma severity and allows the patient to move back or forward through the pathway depending on their individual needs.
ED Package:
The ED package developed by the project includes an ED Asthma Assessment Flow Chart with ED asthma discharge checklist, an Asthma Transfer Plan, and supporting laminated ED wall charts. Copies may be obtained by contacting the authors.
ED Asthma Assessment Flow Chart The ED Asthma Assessment flow chart outlined the process recommended for assessment and initial treatment of asthma, depending on the stage of severity. The flow chart included an asthma checklist for use before discharge from ED, as well as transfer advice according to available resources. The flow chart was designed for use in conjunction with the asthma clinical pathway, which commenced in the ED. A laminated A3 version of the flowchart was produced for ED wall display, as was supporting documentation in the form of an adaption of the NAC's laminated Emergency Management of Asthma chart that outlines assessment of asthma severity and initial treatment.
The ED asthma discharge checklist The ED asthma discharge checklist was designed to assist the transition from the ED to home for people with acute asthma who were not admitted to hospital. Stage one of the asthma clinical pathway includes a section for discharge and education of people with asthma in the ED. The checklist was designed to provide written information about asthma and instructions for management over the 24 hours subsequent to ED discharge.
Asthma Transfer Plan Rural Ambulance Victoria and critical care staff at BHCG developed an Asthma Transfer Plan. The plan was designed for use in conjunction with the asthma clinical pathway. The Asthma Transfer Plan outlined the criteria for transfer of a person with acute asthma. The Transfer Plan was developed as part of BHCG's Medical Retrieval process and listed an Advice and Retrieval Hotline number for the use of facilities that refer asthma patients to BHCG. A laminated A4 version of the Asthma Transfer Plan was produced for ED wall display.
Discussion
No data were gathered on the reasons for GP non-response to the workbooks, however the low response rate constrained interpretation of the results. In addition, requested GP review of the draft clinical pathway provided feedback that was, in part, contradictory. For example, approximately half the GPs commented that the pathway was too cluttered and too time consuming to be of practical use, however the other GPs found the pathway comprehensive and the guidelines useful. The multidisciplinary reference group and high response rate from regional hospitals and community health centres was believed to mitigate the low level of GP participation.
The ED is often the first point of contact for a person with an acute exacerbation of asthma. The lack of evidence based asthma management protocols in regional EDs was of concern, particularly as smaller rural hospitals often did not have the resources or facilities to treat severe or life-threatening asthma. There were no formal protocols for interhospital transfer of patients with asthma. The main issue identified through the workbooks and workshops was the need for standardised asthma documentation. Only one hospital in the region was using a clinical pathway to guide asthma management but the pathway had not been evaluated.
The ED package developed provides a quick reference of resources needed to manage different levels of asthma severity and enables prompt transfer from those facilities that do not have the required resources. Although the package was developed for use in regional EDs its evidence based content and easy to follow format allows it to be adapted to any ED. Likewise, the project did not attempt to impose a regional asthma clinical pathway but to develop an agreed pathway template in a common word processing format (Microsoft Word), which could be used by all regional hospitals. Hospitals were then free to include their Logo and agency-specific assessments or information.
The RAMM is currently being evaluated as the next stage of the project. The process of developing the RAMM also identified issues and subsequent recommendations that were outside the scope of this project. The recommendations were outlined in the project reports and mainly concerned community management issues such as management of acute asthma attacks by school teachers and sporting organisations in rural areas and raising asthma awareness in the community. These recommendations are currently being addressed in a collaborative project between BHCG, Bendigo Community Health and Bendigo and District Division of General Practice.
Conclusion
The Regional Asthma Management Model (RAMM) developed by the project provides regional hospitals with access to evidence-based documentation that will assist in managing people with asthma according to accepted best practice. The project brief was to develop the RAMM and to identify strategies to assist its implementation. An evaluation of the implementation and uptake of the RAMM has commenced. Key Performance Indicators include the increased use of asthma clinical pathways and increased referrals to asthma educators.
The methodology and outcomes of the RAMM reflect the geography of the region, with multiple service providers from different locations managing a person with asthma across a primary, secondary and tertiary continuum. The RAMM could be adapted easily to a metropolitan health environment.
The focus of the Australian health care system is now on health gain and disability reduction through effective disease management. The RAMM is one of the ways the LMR has addressed the National Health Priority areas.
Acknowledgments
This project was funded by the State Department of Human Services, Loddon Mallee region, Victoria, Australia.
References
2. Bauman A, for National Asthma Council, Australia. Latest statistical trends. Undated. Available from:
http://www.nationalasthma.org.au/publications/cam/trends.html (accessed January 2003).
3. National Asthma Campaign. National Asthma Council, Australia. Report on the cost of Asthma in Australia. Undated. Available from:
http://www.nationalasthma.org.au/publications/costs/exec.html (accessed January 2003).
4. Gibson PG, Coughlan J, Wilson AJ, Abramson M, Bauman A, Hensley MJ, Walters EH. Self-management education and regular practitioner review for adults with asthma (Cochrane Review). In: The Cochrane Library, Issue 4 2002. Oxford: Update Software.
5. National Asthma Campaign, National Asthma Strategy. Implementation Plan, 1999. South Melbourne, Australia: National Asthma Campaign, 1999.
6. Jenkins CR, Bauman AE. Asthma management plans: progress and problems. Medical Journal of Australia 1997; 166: 287-288.
7. Ansari Z, Carson N, Serraglio A, Barbetti T, Cicuttini F. Reducing demand on hospital services in Victoria: opportunities for targeted interventions. Health of Victorians, The Chief Health Officer's Bulletin 2001; 1: 28-31.
8. National Asthma Campaign. Asthma Management Handbook South Melbourne, Vic: National Asthma Campaign, 1998.
9. Scottish Intercollegiate Guidelines Network. Emergency management of acute asthma. Edinburgh: Royal College of Physicians, 1998.
10. Scottish Intercollegiate Guidelines Network. Primary care management of asthma. Edinburgh: Royal College of Physicians, 1999.



