The shortage of doctors in rural areas of Australia is well documented and much that has been written focuses on the recruitment and retention of rural general practitioners1-4. However, there has been less discussion about the shortage of rural specialist medical practitioners5. The Australian Medical Workforce Advisory Committee (AMWAC) compiled a considerable body of research and made observations and recommendations about minimum requirements for sustainable specialist services in rural Australia6,7. However, the relationship between the availability of experienced hospital-employed medical officers (HMOs) and the problem of retention and recruitment of rural medical specialists has not been identified. This paper aims to explore this relationship as it applies to rural public hospitals, by examining the historical situation at rural North West Regional Hospital (NWRH) in Tasmania, Australia in 1996-2000.
Context
NWRH is a 160-bed, public hospital situated in Burnie, on the rural north-west coast of Tasmania, an island state off south-east mainland Australia (Figure 1). Over the 2-year period 1996 to 1997, seven of 23 specialist medical staff at NWRH resigned. Of these resignations, only two were due to retirement. Concurrent with the seven vacancies the resignations created were two long-standing vacancies in urology and anaesthetics, which were covered by locum staff. The author was appointed to NWRH as Medical Director during 1996 and was subsequently directed by the Regional Director (NW Tasmania), Department of Health and Community Services, to review of the hospital's specialist workforce with the aim of understanding and addressing the reasons for the loss of specialists at the hospital.
Informal interviews with both specialists who resigned and specialists who remained at NWRH revealed the most common reason for resignation was the onerous workload, particularly on-call and after-hours, with inadequate HMO support. Other issues included insufficient administrative support staff, low morale within NWRH, and family reasons. A literature review was undertaken, focusing on medical specialist retention issues in rural Australia, but not restricted to hospitals. Of particular interest were the relevant volumes of the Australian Medical Workforce Advisory Committee findings, which are based on a large body of national research6,7.
The author coordinated the recruitment of medical specialists to NWRH over the 4-year period, 1996-2000. During this process many medical specialists were interviewed and 16 specialists were subsequently recruited. Potential and actual recruits indicated that the presence of an HMO, especially an HMO who was a specialist-in-training, was a pivotal factor in deciding whether to accept a position at NWRH. During this time, the HMO workforce at the hospital was restructured.
Figure 1: Map of Tasmania, Australia, showing Burnie, the location of North West Regional Hospital.
Hospital-employed medical officers
The HMOs at NWRH were full-time staff, often on secondment from tertiary referral teaching hospitals in Australian capital cities, who were employed to assist specialists in their work. The HMOs were a diverse group of doctors ranging from those in their first post-graduate year to those with many years of experience. Their clinical capacities, therefore, also encompassed a wide range. While the purpose of HMO employment may have been to support the specialist medical staff, HMOs also have vocational needs and important considerations for their employing hospitals include providing the appropriate level of supervision and support; the tension of service versus training opportunities; and whether or not HMOs are overseas trained.
These HMO requirements were met at NWRH due to the wealth of training opportunities at this rural hospital and a specialist staff who were well aware of their responsibilities towards their HMOs. Clear evidence of this was in the gradual but steady increase in the number of HMOs sent to NWRH by seconding hospitals.
Sustainability of specialist services
The AMWAC Sustainable Specialists Services Report6, discusses the requirements to establish and sustain specialist medical services in Australia, including rural Australia. Briefly, AMWAC determined that three major issues are critical to the sustainability of specialist services:
- Demand and supply factors: including population demographics and geographic isolation.
- Infrastructure requirements: including facilities and services such as nursing and allied health.
- Critical mass: the number of similar and associated medical specialists working together.
The first two factors identified by AMWAC are beyond the scope of this reflection; however, the third issue, critical mass, will be analysed.
Critical mass
AMWAC recommends6 that at any one location a critical mass of similar (in specialty and seniority) specialists is necessary to ensure:
- ...reasonable hours of work, the ability to take time out knowing patients will be well cared for, timely access to peers with whom they can have supportive consultations, adequate remuneration, the ability to do research, the ability to participate in professional enhancement activities such as conferences, and continuing education.
In other words, critical mass can be said to consist of three parts: (i) workload; (ii) peer support; and (iii) professional enhancement. Further, AMWAC recommends that a critical mass of two similar specialists (or in some specialties such as paediatrics, orthopaedics and psychiatry a minimum of three specialists) is required in order to ensure sustainability.
While it is difficult to generalise due to the diversity of the NWRH HMO group, it is fair to say that almost all HMOs provided some degree of support for rural specialists. What did become clear was that the presence of a senior or post-graduate year-4 HMOs or specialist-in-training HMOs was most effective in supporting 'critical mass' and sustainability among the specialists.
Workload
The presence of HMOs in adequate numbers, especially senior or specialist-in-training HMOs, can reduce the basic and after-hours workload of a rural specialist and ensure their regular time off duty. Table 1 provides a rating scale developed at NWRH to assess the after-hours workload of each specialty, adjusted according to the seniority of the HMO support.
Table 1: After-hours workload for each specialty at North West Regional Hospital, Tasmania, Australia, 1998-2000
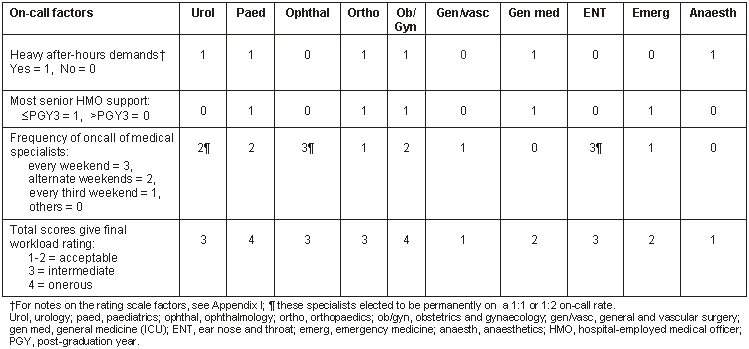
Basic workload: The basic workload of a given population is described by AMWAC, along with identified supply and demand factors that determine the number of specialists that may be required in a given area6. In some situations it is not possible to recruit an adequate number of specialists; in other situations the patient population does not support two specialists yet the workload is too great for a single specialist. Both these situations occurred at NWRH, and it was found that in response the HMO staff was able to assist by attending to emergencies, seeing outpatients and assisting in the care of inpatients. As well as relieving the specialists' workload, this also allowed specialists more uninterrupted time for their other clinical work.
While this may seem to be promoting HMOs to act substitutes for specialists, the intention was simply to support existing specialists by making their workload more manageable and allowing them a balance of other professional activities. This strategy contributed to NWRH specialist retention and improved recruitment of other specialists.
After-hours workload: The burden of on-call, after-hours work for specialists at the NWRH was a major issue due to the frequency of time spent on-call and the nature of call-outs (patient problems).
Frequency of on-call Typically in rural areas, as was the case at the NWRH, there are few specialists in each medical field, necessitating frequent on-call periods for existing specialists. Most specialists at NWRH were on call every weekend or every second weekend throughout the year (Table 1). In some circumstances HMO staff can reduce a high frequency of on-call periods for specialists, for example if the hospital permits an HMO to be on-call with supervision via telephone advice from a specialist at a more distant hospital. This strategy was permitted at NWRH for sole specialists in ENT, urology and ophthalmology.
Nature of call-outs The nature of on-call varies according to the medical specialty and is influenced by the type of call outs and their frequency; this can be measured in terms of 'heavy on-call demands'6 (Table 1). At NWRH, calls from the hospital to specialists commonly resulted in the specialist having to travel in to the hospital. When call-outs are the result of time-critical emergencies (eg paediatric and obstetric emergencies), the need for specialists to be physically available 'at the drop of a hat' makes the burden of on-call particularly onerous because it interferes with normal family life.
In contrast, where a senior or specialist-in-training HMO was working, the specialists' workload was alleviated because the HMO could reduce the requirement for the specialist to attend the hospital in person by:
- Acting on telephone advice from the specialist on call
- Attending to time-critical emergencies
- Making complex clinical decisions
- Performing a number of procedures without direct supervision.
Thus, rather than increasing the number of specialists, the presence of a senior HMO can contribute substantially to relieving a specialist's after-hours workload.
Peer support
According to AMWAC, having a minimum number of similar specialists at each location is necessary for peer support6. Improvements in communication technology have made timely consultation betweem peers easier, and the value of a senior HMO as a source of peer support was not identified by AMWAC. United Kingdom research has shown HMOs to be highly knowledgeable, even to the extent that HMO specialists-in-training are often more 'knowledgeable' than their consultant8. While medical knowledge is not the only thing required for peer support, the experience at NWRH was that HMOs did provide specialists with peer support, especially in regard to isolated clinical decisionmaking.
Professional enhancement
Professional enhancement encompasses such activities as continuing education, conference attendance and research. Professional development and continuing medical education is becoming mandatory for maintaining specialist registration in Australia. At NWRH, local opportunities to attend to professional development were limited. The presence of HMOs, particularly if the HMO was a specialist-in-training, provided an increased number of interested participants for such activities as journal clubs, teaching opportunities and an eager pair of hands to assist with local research endeavours, or in audit activities. Engaging in professional enhancement activities not only fulfills specialists' registration requirements but it also improves the quality of working life and was highly regarded by specialists at NWRH.
Conclusion
The value of the HMO in the recruitment and retention of rural specialists has not been well described in the past. The three 'critical mass' issues of workload, peer support and professional enhancement have been identified in national workforce studies undertaken by AMWAC as being vital to sustainable specialist services in Australia. This personal view of events at NWRH 1996-2000 has demonstrated that senior HMOs can impact positively on these sustainability issues. The most important contribution of HMOs was the mitigation of the after-hours workload of rural specialists. It is suggested that HMO staffing could be justifiably added to AMWAC's 'compendium of requirements' for sustainable specialist services.
Much is being done in Australia to improve the number of medical professionals in rural areas. It is recognised that exposure to a rural environment during medical school and as an HMO specialist-in-training encourages medical specialists to consider working in rural areas. An additional factor in the recruitment and retention of specialists in rural areas is when specialist-in-training HMO positions are increased in number and supported by rural hospitals.
Acknowledgements
Work on this manuscript was carried out while the author was an employee of the Department of Health and Human Services, Tasmania, Australia, and completed as a freelance consultant in health services management. The observations made and opinions expressed are those of the author and are not necessarily held by the Department of Health and Human Services, Tasmania, or by the medical staff at the North West Regional Hospital, Burnie, Tasmania. There is no conflict of interest or potential conflict of interest to declare.
References
1. Kamien M. Staying or leaving rural practice: 1996 outcomes of rural doctors' 1986 intentions. Medical Journal of Australia 1998; 169: 318-321.
2. Western Australian Health Department. Report of the Ministerial Inquiry into the Recruitment and Retention of Country Doctors in Western Australia. Perth, WA: Western Australian Health Department, 1987.
3. South Australian Health Commission, Royal Australian College of General Practitioners (SA), Australian Medical Association (SA). Review of general medical practice in South Australia. Third report: country general practice. Adelaide, SA: South Australian Health Commission, 1992.
4. Strasser R. Rural general practice in Victoria: the report from a study of the attitudes of Victorian rural general practitioners to country practice and training. Moe, Vic: Monash University Centre for Rural Health, 1992.
5. Bruening MH, Maddern GJ. A profile of rural surgeons in Australia. Medical Journal of Australia 1998; 169: 324-326.
6. Australian Medical Workforce Advisory Committee. The medical workforce in rural and remote Australia. AMWAC report 1996.8 Sydney, NSW: Australian Medical Workforce Advisory Committee, 1996.
7. Australian Medical Workforce Advisory Committee. Sustainable specialist services: a compendium of requirements, AMWAC Report 1998.7 Sydney, NSW: Australian Medical Workforce Advisory Committee, 1998.
8. Grant J, Marsden. Primary knowledge, medical education and consultant expertise. Medical Education 1988; 22: 173-179.
Appendix I: Factors used in rating scale for workload in Table 1
Factor 1
Identified by specialist colleges as having heavy on-call demands:
An estimation made by each specialty's College and reported by Australian Medical Workforce Advisory Committee 6 was used as an indication of the number and nature of specialist recalls to the hospital.
Factor 2
Seniority of HMO support:
HMO seniority relates to the number of years post-graduation (ie Post-Graduate Year (PGY) 1 is PGY1, Post-Graduate Year 2 is PGY2 etc. PGY4 or above (PGY4+) senior HMOs and/or specialists-in-training. The distinction between HMOs above and below PGY3 was that in the opinion of NWRH specialists, HMOs of 3 years post-graduate experiance or below required substantial on-site supervision from the specialist. PGY4+ are either specialists-in-training or more experienced HMOs who were deemed to require less on-site supervision.
Factor 3
Rate of on-call for medical specialists:
The frequency of on-call time for each specialist at NWRH was rated according to the corresponding number of weeks not on-call. For example, 1:1 means on-call all week and every weekend all year round; 1:2 means on-call every second weekend. The nature of the on-call system at NWRH permitted some consultants to go on leave or off call without on-site locum cover because supervisory advice could be obtained from a larger medical centre, and patients could be transferred there without disadvantaging their care.
