The mental health of older adults is being discussed increasingly as the UK population ages. There is evidence that depression in older adults is strongly associated with reduced quality of life, with one study suggesting that only heart disease and arthritis have stronger associations1. It is associated with greater cognitive decline2 and with increased mortality3. Anxiety has similar negative effects in the older adult population, with studies demonstrating a relationship with reduced quality of life4 and increased mortality5.
In principle, a range of treatment options are available to the GP. They can prescribe medication, such as anti-depressants, and monitor and adjust the dosage as appropriate6. Consideration of the differing side-effect profiles and drug interactions appears to be particularly important when selecting this option for elderly patients7. They can direct the patient to a range of self-help materials available from libraries or on the internet (bibliotherapy), and a list of these has been made available to all GP practices in the area, as suggested by Whitfield et al8. They can suggest that the patient makes use of social groups and activities, possibly with the assistance of another agency9,10. Or they may refer the patient for psychotherapy, either directly to Clinical Psychology or through a psychiatric referral11. The effectiveness of psychotherapies for depression and anxiety in older adults has been demonstrated in past studies and reviews12-14 although the lack of referrals may be indicative of a reliance on psycho-pharmacotherapy. At present, little reliable information is available regarding the attitudes of GPs towards these options.
Despite the apparent evidence that psychotherapy is effective at reducing depression and anxiety in older adults, it appears that this does not lead to a majority of these patients being offered psychotherapy15. It may be that older adults are not making GPs aware of their psychological distress. There is some evidence that anxiety and depression in older adults are often unrecognised in primary care settings16,17. If recognised, GPs may be concerned that psychotherapy would not be an acceptable treatment option to their older adult patients, although evidence suggests that it is seen as both acceptable and effective by depressed older adults18,19.
The local conditions of the Scottish Highlands are different from other areas of the UK, as there is a great deal of sparsely populated land that gives the local GP practice a particularly vital role in delivering local health services. If GPs do refer patients to a specialist service, either the patient must travel to one of the few population centres or the specialist must travel to them. In either case, the journey time could be up to 5 hours. The most recent census data indicates that more than 50% of the population covered by NHS Highland is outside the major population centre. As a result, long waiting lists have sometimes characterised local clinical psychology services, as necessary travel time takes up valuable time with patients.
Until recently, older adults were seen within the generic Adult Mental Health psychology service. However, a dedicated Older Adults Psychology service was introduced in 2005 providing both neuropsychological assessments of patients with possible dementia of any age as well as psychotherapy for those aged over 65 years. It had no fixed referral pathway and would accept referrals from GPs, psychiatry, care homes or from other services. However, in the period from January 2008 to July 2008, the department received only 9 referrals for depression or anxiety from GPs. Given the high number of older adults residing in the area, and the national prevalence of significant depression and anxiety among this group20,21, there is a concern that many older adults in the area may not be getting the psychological treatments that could help them with their problems. Recent research has revealed this pattern of under-referring in NHS Greater Glasgow22.
The present study is designed to obtain further information about GPs' attitudes to psychotherapy within the rural Highlands. The present authors intended to discover what specific therapies they felt would most benefit their patients and which therapies they generally accessed. From one perspective, this may help rural departments structure their services around the wishes of those who refer to it. From another, it may show areas where GPs would benefit from information of the differing efficacies of the various treatments. While the study was intended to address local problems, the results may also be relevant in locations with similar demographics and geographical constraints.
The aims of the study were to:
- Gain an estimate of the prevalence of depression and anxiety in local GP clinics.
- Gain a snapshot of local GP's attitudes towards the different treatment options for depression and anxiety in older adults and their current use of these options.
- Elicit GP suggestions in regards to improvements to psychological services for older adults in the area.
Design
The study used a questionnaire to survey all GPs in the area. Confirmation was obtained from the local NHS ethics committee that the study did not require full ethics approval because it was a service evaluation involving only health professionals.
Participants
An NHS document provided the names and practise addresses of every GP in the three NHS Highland Community Health Partnerships (CHPs) and all 284 of these were invited to participate in the study. Each of these CHPs contains a mix of rural and urban areas. In order to preserve the anonymity of participants in an area where GP practices can be easily identified, further details of the practice location were not requested.
Materials
A questionnaire was designed specifically for this research. In producing this, the primary concerns were concision, clarity and the usefulness of questions in addressing the research aims, as it was hoped these features would help persuade GPs to return the questionnaire despite their busy schedules. A series of drafts were produced and discussed with the research team, and a range of amendments included in the final version. A mix of quantitative and qualitative questions was included to fit the individual aims of the study. The final version was shown to a GP who gave his opinion that the questions would be easily understood and completed by local GPs. No further pilot testing was undertaken in order to minimise delays.
The three questions were as follows:
Q 1: During the last week, how many older people did you treat for mild to moderate depression and/or anxiety?
This was included to give a rough estimate of the potential need in the area for some form of psychological input.
Q 2: How effective would you judge the following treatment options for Older People experiencing mild to moderate depression or anxiety?
Please tick the box at the end if you currently prescribe this treatment.
The GPs were provided with Likert scale from 1 ('Not at all effective') to 7 ('Extremely effective) for each option, that is pharmacological, psychological (eg cognitive behavioural therapy), social (eg groups) and bibliotherapy (eg self-help books). A box at the end of each scale allowed GPs to indicate if this treatment was currently prescribed. This question was included to assess the attitudes of GPs towards a range of commonly recommended treatment options for depression or anxiety. The 4 options were not intended to be mutually exclusive (for instance, the latter 3 options could all be expected to offer similar behavioural suggestions). The 'currently prescribe?' option was included to allow a comparison between beliefs of treatment efficacy and current practice.
Q 3: If you had an elderly patient whose problems seemed to have a psychological component, what would you need to make psychological input more available to them?
This question was left open to allow GPs to comment on current service requirements. A thematic content analysis was carried out to categorise the revealed themes23. The first author first familiarized himself with the responses. Themes were developed and coded as the responses were examined, then the entire set of responses was re-examined to ensure that no response was un-coded and that no themes had been mis-applied. The themes were then given names that briefly and clearly described the theme and examples were selected.
A further question relating to the 'understandability' of depression in older adults was also included. However, this was primarily used to inform a separate study and has therefore not been included in these analyses.
Procedure
Packages were sent to each practice in the area. A letter to the practice manager explaining the nature and importance of the project was included, and they were requested to pass on the remaining contents to the GPs in their practice. The inclusion of the practice manager was partly to facilitate the circulation of the questionnaires, but also in the hope that they might encourage the GPs to complete them.
Each GP received an envelope directly addressed to them. This included the questionnaire, an addressed return envelope and a participant information sheet. The information sheet again underlined the purpose and importance of the study, emphasised the minimum time required to complete and return it, and underlined that all responses would be anonymous (although coded by region).
Questionnaires were received from 119 GPs (46%) over a 4 month period, in equivalent proportions from the 3 main CHPs in the area.
Q.1 - During the last week, how many older people did you treat for mild to moderate depression and/or anxiety?
Although most GPs responded using a number or range of numbers, qualitative responses to this question were provided by 16 GPs, including 'Lots!', 'Don't keep this as a record' and 'Usually between 5 and 10'. The mid-point was accepted as an estimate where a range was provided, and in other cases the response was recorded but not included in analysis. The mean number of older adults with depression and/or anxiety treated by GPs in the previous week was 2.6 (s.d.= 3.08) with a range of 0-20. In total this amounted to 309 patients seen in the previous week by the 119 respondents
Q.2 - How effective would you judge the following treatment options for Older People experiencing mild to moderate depression or anxiety? Please indicate if you currently prescribe this treatment.
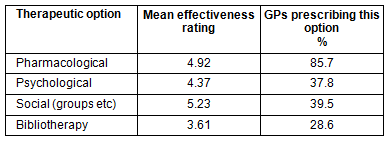
The GP respondents rated social therapies as most effective (mean= 5.23; s.d.=1.0) followed by pharmacology (mean= 4.92; s.d.=1.0), psychological therapies (mean= 4.37; s.d.=1.1) and bibliotherapy (mean=3.61; s.d.=1.2). Post-hoc t-tests (using a Bonferroni correction) revealed that all paired-comparisons were significant at the 1% significance level with the exception of the pharmacology- social comparison.
In contrast, the therapy prescribed by most respondents was psycho-pharmacotherapy, which was prescribed by 84%, while only 40% prescribed social therapies, 38% prescribed psychology and 29% prescribed bibliotherapy (Table 1).
Table 1: The GPs' ratings of therapy effectiveness and their current prescribing practice
Q.3 - If you had an elderly patient whose problems seemed to have a psychological component, what would you need to make psychological input more available to them?
A range of views were provided to this question. Initial examination suggested that a small number of key themes were being repeated by many participants. It was accepted that some GPs expressed more than one view and so the percentages given below refer to the number of GPs who reported a given theme. The full range of views is not provided in order to preserve anonymity but the major themes revealed were as follows (with examples):
- Theme 1 - Long waiting times 47%
- 'A psychological service that doesn't have such an enormous waiting list.'
- 'Because of the long waiting times I usually don't bother referring for specialist psychological help, instead relying on the input I can give as a GP.'
- Theme 2 - Local input 24%
- 'A local psychology service!'
- Theme 3 - A specialist older adult service 17%
- 'A psychologist who specialises in older people.'
- Theme 4 - Increased Community Psychiatric Nurse (CPN) availability 14%
- 'More CPN or equivalent.'
- Theme 5 - Faster referrals 5%
- 'Prompt referral service.'
Discussion
The results of this study suggest that GPs are aware of many more elderly patients with anxiety or depression than they currently refer to Clinical Psychology. More than 300 patient contacts involving mild to moderate depression or anxiety were reported in one week by the respondents. This is in stark contrast to the 9 referrals received from GPs in a 6 month period.
Also of interest were the GPs attitudes to different therapeutic options for mild to moderate depression or anxiety and how this compared with their practice. As might be expected, more GPs reported that they would prescribe pharmacological treatments than the 3 non-medication options (psychotherapy, social and bibliotherapy). However, the attitudes of the GPs towards these options were not consistent with their practice. When asked to give their impression of the relative effectiveness of the options, social interventions were rated the highest. Post-hoc analysis revealed that this was significantly higher than psychological and bibliotherapy interventions, although the difference between social and pharmacology options was not significant. These results suggest that GPs would have greater faith in a service which provided social assistance to older adults, such as groups. While this is not something provided directly from the psychology department at present, it is an approach that is supported by psychological theory and research at reducing depression9 and loneliness10. The cognitive-behavioural model highlights the importance of behavioural activation in depression and opportunities for exposure in anxiety. One of the possible consequences of this finding may be the involvement of psychology in such services to help obtain 'a foot in the door', or else adjust resources aimed at GPs to give them more of a social emphasis. In either case, the results suggest that GPs may be intuitively more aware of the risks of isolation on the mental health of the elderly than might have been expected from the low referral rate. Perhaps the lack of social resources is particularly salient in these remote communities.
This study was principally concerned with the attitudes GPs held, rather than the actions they performed, and the one question that did address their current behaviour was condensed to allow the form to be completed quickly. That we were able to show some discrepancy between GPs' judgment of treatment efficacy and their use of these treatments is one of the most interesting results we have uncovered, but further research is needed to test this conclusively. Our question used the phrase 'currently prescribe' and it is possible the use of the word 'prescribe' rather than 'offer' or 'refer' may have led clinicians to think in terms of medication rather than therapy. Also, the different therapy options we presented were given only brief descriptors, and we intended this to reflect the vocabulary used by GPs in their letters. However, their understanding of these words was not tested, and it is possible that the broad descriptors used (such as 'social') added confusion rather than clarity. The study would certainly have been strengthened had drafts of the questionnaire been given to a wider selection of GPs for comment.
The qualitative question was responded to enthusiastically and may ultimately have the greatest effect on the workings of the department. There was a clear misunderstanding of the difference between the Older Adults Psychology Service and the Adult Mental Health Service, and GPs clearly expected referrals to be met with the same extensive waiting lists as they would get in the latter. In this instance, they appeared to be unaware that a specialist service existed and that it currently operates with almost no waiting list at all. Following this response, it has become clear that the different referral options have not been fully explained to GPs and the most appropriate way of achieving this is currently being considered. It is of note that a recent US study in rural Illinois also concluded that availability of psychologists was again a major concern among primary care physicians24.
Equally clear was the GPs requests for a far more local service, a desire also expressed by elderly Highlands residents in a recent study25. This has generally been difficult to achieve in the area, but initiatives such as Guided Self Help Workers have begun to have an impact on the delivery of psychological services to remote areas. It is possible that such projects may be successfully adapted to the needs of older adults. These and the other recommendations from the GP have been passed on to relevant NHS managers, whose decisions may benefit from the perspectives of those working most directly with the public. Adequate provision of mental health services in rural areas may be difficult to achieve using the same service models as urban areas, but this study suggests that rural GPs would be keen to make use of local, dedicated older adults' services if they were made available.
Study limitations
This study received questionnaires from only half of the Highland GPs and, therefore, may have been affect by selection bias. As the Highlands consist of both rural and urban areas, the responses may reflect a mix of views from these two kinds of community. Additionally, the questionnaire used was piloted on few GPs and therefore the wording of some questions may have been confusing. Similar work in this area could be strengthened by introducing measures to increase the number of respondents and by categorizing responses according to their location, as well as conducting careful piloting of questionnaires before distribution.
The results from this study suggest that there are many more cases of mild to moderate depression or anxiety being seen by GPs in the area than are being referred to the Older Adults Clinical Psychology Service. The GPs indicated that they are more likely to deal with cases by prescribing medications than offering psychotherapeutic treatment options. However, the GPs rate social therapeutic options as highly as pharmacological options for effectiveness in treating these patients. Suggestions from GPs of improvements to the service indicate that many GPs are not fully aware of the service available, although many requested a local psychology service. This suggestion may reflect the difficulties in delivering psychotherapy in predominantly rural areas, although the overall results indicate that the GPs would like a suitable service for older adults they could refer to. The results have implications for future service development in similar rural areas.
References
1. Unützer J, Patrick DL, Diehr P, Simon G, Grembowski D, Katon W. Quality adjusted life years in older adults with depressive symptoms and chronic medical disorders. International Psychogeriatrics 2000; 12: 15-33.
2. Sachs-Ericsson N, Joiner T, Plant EA, Blazer DG. The influence of depression on cognitive decline in community-dwelling elderly persons. American Journal of Geriatric Psychiatry 2005; 13: 402-408.
3. Schulz R, Drayer RA, Rollman BL. Depression as a risk factor for non-suicide mortality in the elderly. Biological Psychiatry 2002; 52(3): 205-225.
4. Bourland SL, Stanley MA, Snyder AG, Novy DM, Beck JG, Averill PM et al. Quality of life in older adults with generalized anxiety disorder. Aging and Mental Health 2000; 4(4): 315-323.
5. Van Hout HPJ, Beekman ATF, De Beurs E, Comijs H, Van Marwijk H, De Haan M et al. Anxiety and the risk of death in older men and women. British Journal of Psychiatry 2004; 185(5):399-404.
6. Joint Formulary Committee. British national formulary 54. London: British Medical Association and Royal Pharmaceutical Society of Great Britain, 2007.
7. Pollock BG. Adverse reactions of antidepressants in elderly patients. Journal of Clinical Psychiatry 1999; 60(20): 4-8.
8. Whitfield G, Williams CJ, Shapiro DA. Assessing the take up and aceptability of a self-help room used by patients awaiting their initial outpatient appointment. Behavioural and Cognitive Psychotherapy 2001; 29: 333-343.
9. Niederehe G. Developing psychosocial interventions for depression in dementia: beginnings and future directions. Clinical Psychology: Science and Practice 2005; 12(3): 317.
10. Cattan M, White M, Bond J, Learmouth A. Preventing social isolation and loneliness among older people: a systematic review of health promotion interventions. Ageing & Society 2005; 25(1): 41-67.
11. Whitfield, Williams C. The evidence base for cognitve behavioural therapy in depression: delivery in busy clinical settings. Advances in Psychological Treatment 2003; 9: 21-30.
12. Frazer CJ, Christensen H, Griffiths KM. Effectiveness of treatments for depression in older people. Medical Journal of Australia 2005; 182: 627-632.
13. Pinquart M, Duberstein PR, Lyness JM. Treatments for later-life depressive conditions: a meta-analytic comparison of pharmacotherapy and psychotherapy. American Journal of Psychiatry 2006; 163(9): 1493-1501.
14. Hendriks GJ, Voshaar RCO, Keijsers GPJ, Hoogduin CAL, Balkom AJLMv. Cognitive-behavioural therapy for late-life anxiety disorders: a systematic review and meta-analysis. Acta Psychiatrica Scandinavica 2008; 117(6): 403-411.
15. Wei W, Sambamoorthi U, Olfson M, Walkup JT, Crystal S. Use of psychotherapy for depression in older adults. American Journal of Psychiatry 2005; 162(4): 711-717.
16. Stanley MA, Roberts RE, Bourland SL, Novy DM. Anxiety disorders among older primary care patients. Journal of Clinical Geropsychology 2001; 7(2): 105-116.
17. Martin L, Poss JW, Hirdes JP, Jones RN, Stones MJ, Fries BE. Predictors of a new depression diagnosis among older adults admitted to complex continuing care: implications for the depression rating scale (DRS). Age and Ageing 2008; 37: 51-56.
18. Kuruvilla T, Fenwick CD, Haque MS, Vassilas CA. Elderly depressed patients: what are their views on treatment options? Aging & Mental Health 2006; 10(2): 204-206.
19. Landreville P, Landry J, Baillargeon L, Guerette A, Matteau E. Older adults' acceptance of psychological and pharmacological treatments for depression. Journal of Gerontology: Psychological Sciences 2001; 56(5): 285-291.
20. Beekman AT, Copeland JR, Prince MJ. Review of community prevalence of depression in later life. British Journal of Psychiatry 1999; 174(4): 307-311.
21. Bryant C, Jackson H, Ames D. The prevalence of anxiety in older adults: Methodological issues and a review of the literature. Journal of Affective Disorders 2008; 109(3): 233-250.
22. Broomfield NM, Birch L. Primary care mental health teams: where are all the older people? Clinical Psychology Forum 2009; 198: 16-19.
23. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006; 3(2): 77-101.
24. Glasser M, Vogels L, Gravdal J. Geriatric depression assessment by rural primary care physicians. Rural and Remote Health 9:1180. (Online) 2009. Available: www.rrh.org.au (Accessed 22 December 2010).
25. King G, Farmer J. What older people want: Evidence from a study of remote scottish communities. Rural and Remote Health 9:1166. (Online) 2009. Available: www.rrh.org.au (Accessed 22 December 2010).
