Many innovations in health for rural populations, such as telemedicine, have addressed poor access to specialised services due to distance, but do not take account of poor utilisation of services for cultural or linguistic reasons. On the other hand, studies focussing on ethnic disparities in health have been criticised for focussing on culture as a sole explanatory variable at the expense of other variables1. This often leads to a situation where ethnicity is seen as the cause of health disparities, rather than an effect resulting from differences in the uptake of preventive measures and health service utilisation.
Lack of attention to how issues of culture and language (with exception of studies of Indigenous people) may impact on health service utilisation in rural areas in part reflects sampling difficulties. Some rural communities are relatively homogenous, others have small numbers of people from a wide range of backgrounds and others have concentrations of particular populations from the same background. In view of this, working with communities where there are significant concentrations of specific ethnic populations may be a useful way of developing models to understand how cultural differences impact on attitudes to health and health service provision in a rural environment. In addition to providing information about specific communities, this may also provide a basis for understanding what issues may affect other culturally and linguistically diverse groups.
In this paper we compare health utilisation among Filipinas (women born in the Philippines) living in remote and rural parts of Queensland to their urban counterparts. Making an urban/rural comparison within particular ethnic groups enables differences in health service utilisation to be discussed separately from culture.
Access to health services will be discussed in terms of the framework outlined by McKinley et al.2.
- Knowledge (Availability) is measured in terms of consumers' knowledge about the services and consumers' confidence in being able to use the medical care they require.
- Accessibility is considered in terms of their location to the consumers in relation to the services (distance) and being able to physically get to them (transport).
- Affordability is measured in terms of the extent to which cost is seen as a barrier to service use.
- Accommodation is measured in terms of the extent to which service delivery arrangements are able to accommodate consumers' needs and the extent to which doctors' attitudes are seen to be accommodating of those needs.
The four dimensions listed inform a fifth dimension; Acceptability which is measured in terms of the perceived need for improvement in the service delivery arrangements and consumers' satisfaction with the arrangements. It would be expected that cultural and linguistic issues would primarily affect Knowledge and Accommodation. It might be expected that women living urban areas would have access to a wider range of services at a primary care level than women in rural communities. This may result in improved knowledge and possibly better Accommodation among urban women compared to rural women. Differences in Accessibility and Affordability would be expected to be affected by location. Access to services in rural areas may be more difficult and dependent on personal transport.
Method
Sample
The sample was recruited as part of the University of Queensland component of the Australian Longitudinal Study of Women's Health(ALSWH)3. The first phase of the study has consisted of exhaustive sampling of Filipinas involved in community organisations and their social contacts. This methodology enabled extensive sampling of the community, as defined by cultural affiliation, rather than by factors like geographic location3. This was supplemented through the use of factories and church groups.
The population distribution of Filipinas in Queensland is clustered with high population densities in Brisbane and adjacent coastal areas, Far North Queensland (Cairns and Townsville), and Mt Isa. Sampling for the ALSWH concentrated on these three population centres and surrounding rural and remote areas. Study centres were established in Brisbane coastal regions and Far North Queensland in 1996 and in Mt Isa in 1997. The sample consisted of women from Brisbane, the Gold Coast, the Sunshine Coast, Cairns and surrounds, Townsville and surrounds and Mt Isa. In-depth interviews were conducted with 139 women and a further 90 women attended focus groups. Most of the women lived in urban or semi-urban areas (n = 391) and 90 lived in areas designated as rural or remote areas by Queensland Health. All women included in the rural and remote sample were eligible for the Queensland patient transfer assistance scheme by air for some services regardless of whether their area of residence was classified as rural or remote, that is they lived over 1000 km away from tertiary services or lived in areas eligible for other reasons. The overall response rate was 87% and 83%.
Instruments
Telephone protocol
Publicity through community groups and attendance at meetings meant that many women were aware of the study and had met the research team prior to being asked to participate in the study. In some cases women were invited to participate directly in the study over the telephone, using contact information obtained from community organisations or personal contacts. The protocol invited women to participate and explained what was entailed and the voluntary nature of participation. In addition, researchers' affiliations, the source of contact details, the nature and scope of the study and reasons for involving Filipinas were outlined.
Interview protocol
A semi-structured interview protocol was developed based on a review of qualitative and quantitative data collected in the first half of 1996 by the research team and the reference group. Six major areas of interest were identified which required further clarification or more in-depth investigation. Areas identified included immigration experience; recognition of qualifications and access to employment and professional development; social support in Australia and in the Philippines; relationship issues; perceptions and use of health services, and cultural perspectives on health and staying healthy.
Questionnaire
The questionnaire was used to collect baseline data on the health of Filipinas and is the basis for the recruitment of cohorts for the longitudinal component of the study. It consists of items about immigration status derived from the Longitudinal Study of Immigrants to Australia (LSIA), Mothers in a New Country (MINC) study, and the main section of the study by the University of Newcastle, and contains sections on mental health, health and health service utilisation, life events, life stages, settlement experience, and language and demographics. The questionnaire was pre-tested and reviewed by the members of the reference group, who suggested that sensitive health issues (eg domestic violence) be removed. Questions about income were replaced by a question about health care cards, and questions on eye and dental care were added. Questions about domestic violence were modified to address injury in general.
Procedure
At the outset, women were informed that the study was part of a national women's health initiative, and that participation required completing an interview/workshop and an initial questionnaire. They were also informed that they might be asked to participate in further stages of the study. Women were asked to consent separately to participation in the current questionnaire and interview, taping of the interview, future contact by the study team, and the provision of additional personal details to make contacting them easier. Women were informed that their participation was voluntary, that they had the right not to answer any particular questions, and that they could withdraw from the study at any stage. The study was approved by the ethics committee at University of Queensland.
Results and Discussion
Quantitative data
All statistical analyses compared health status among Filipinas living in urban areas to Filipinas living in remote rural/areas. SPSS was used to conduct Chi-square analyses. The percentage of women reporting difficulties with access to health services is shown (Table 1).
Table 1: Differences in access to health services between remote/rural and urban women
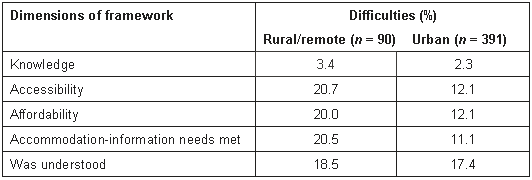
Women in remote/rural areas reported a greater degree of difficulty in accessing doctors at their last visit (c2 = 4.4, df = 1; p = 0.04) and getting their information needs accommodated (c2 = 5.3, df=1; p = 0.02) than women living in urban areas did. There were no differences between women living in rural/remote and urban areas in knowing where to go (c2 = 0.3, df = 1; p = 0.58), ability to afford treatment (c2 = 3.7, df = 1; p =0.06) and in being understood (c2 = 0.05, df = 1; p = 0.82).
In order to ascertain whether women's perceptions of access to health care affected their actual use, differences in health service utilisation were also tested. Women in remote/rural areas were more likely than women living in urban areas to have been admitted to hospital in the last year for reasons other than having a baby (c2 = 5.5, df = 1; p = 0.02). There were no statistical differences in morbidity (except high blood sugar) suggesting that differences in the rate of hospitalisation may reflect the fact that there are limited alternative options for care in remote/rural areas. This may also be true in regard to preventive behaviour. Remote/rural women were more likely than urban women to have had a pap smear (c2 = 8.7, df = 1; p = 0.04) but there were no differences in the number of women who had had a pap smear in the last 2 years (c2 = 0.9, df = 1; p = 0.34).
Rural women expressed greater problems with access and accommodation. The differences in accommodation were only due to difficulty getting their information needs met rather than in being understood. Rural women were also more likely to hospitalised but differences were not detected in preventive care. Analysis of the qualitative data was used to explore these differences in greater detail.
Qualitative data
Greater difficulty accessing health care among remote/rural women was also reflected in the qualitative data. The major health service issues identified by Filipinas in remote/rural areas were associated with geographic location rather than ethnicity. These included: lack of bulk billing doctors, difficulty in accessing female doctors, difficulty in accessing specialists, travel and cost associated with visiting specialists, long waiting times in outpatients (only option for after hours care), young inexperienced doctors, transience of medical staff and difficulty in gaining a second opinion in town. Generally all of the issues raised referred to access, although there was a perceived trade-off between the affordability of services and access to them.
Lack of bulk billing doctors and young and inexperienced doctors
Interestingly, although the quantative data did not suggest differences in affordability, the qualitative data did suggest that there were differences in the cost of services. Lack of bulk billing doctors did not appear to be an issue for urban women but women in remote and rural areas reported that few general practitioners bulk billed and most charged above the amount refunded by Medicare. Rural/remote women appeared to trade off the financial costs of visiting the doctor with the perceived severity of the illness and risk of delaying treatment. Changes in patterns of health service use may be the reason that the quantitative data did not pick up differences in affordability.
Remote/rural women perceived that there was a large gap in the quality of public and private services but this did not appear to be an issue for urban women. This is partly due to the fact that doctors in public facilities in remote/rural areas were more likely to be young, inexperienced and unfamiliar with the community5. Rural and remote women tended to attend the few 'free' services when they wanted to get prescriptions (eg for the pill or antibiotics), but not when they believed that they or their families had serious health problems. This pattern of health utilisation may reflect the fact that many types of medication, only available by prescription in Australia, are available over the counter in the Philippines. Attending medical services in these cases was seen as a necessary step in the process of self-prescription rather than a health intervention in itself.
Lack of Access to Female Doctors: In general, Filipinas in all areas reported shame and reluctance to talk to or be examined by male doctors in regard to gynaecological issues. However,in the full population of the ALSWH, all women in rural and remote areas found it more difficult to access female doctors. A shortage of female doctors mean that even women who have regular GPs were unlikely to get regular check ups because their doctors are male. This also led to difficulties when women who were reluctant to see a male doctor required a second opinion.
A few women did attend male doctors for pap smears and other gynaecological problems. This was largely because options for obstetrics and gynaecology were seriously limited so most women tended to be attended by a male doctor during pre-natal care and during birth. While many women found this disturbing and embarrassing they had no other option. Positive experiences during this process meant that women were less reluctant to discuss gynaecological problems with male doctors, especially those that they had a pre-existing clinical relationship with and often were prepared to visit male doctors who were recommended by personal acquaintances.
Waiting: Lack of appropriately trained doctors and geographic isolation meant that local doctors in remote and rural areas were often overworked, waiting times are long and after hours services often limited to hospital outpatients6. Long waits for hospital and GP visits were a major issue for rural and remote women but were less important for urban women. While most women recognised that waiting in outpatients or casualty was determined by priorities, their sense of priorities was often different from health workers. For example, people were sometimes served first for reasons other than medical urgency and this could be misunderstood.
- I had been waiting in the hospital for hours with my daughter who was really sick. This man came in. He was drunk and swearing. He had a dirty bandage on his arm but there was nothing wrong with him, only drunk. He got served straight away. I was really mad. I wanted to go up and say, 'Is this a hospital for everyone or only the drunks?'
Anxiety and frustration about waiting periods were exacerbated because people only attended Accident and Emergency when they believed that they, or a family member, were experiencing a health crisis. This also affected perceptions of the type of treatment that was appropriate. The length of the wait was seen as a determinant of the intensity of the treatment. Many women complained that they had waited for hours only to be told to go home or to 'take a Panadol'. Most of the cases where this occurred involved women presenting at outpatients with children with diarrhoea or vomiting. This could suggest that women were not sure how to manage these problems at home and at what point they should present to the hospital.
Waiting is also a regular feature of visits to GPs and there was a perception that delays in services were not always equitable. In some cases women complained that there was preferential treatment in GPs with some people waiting for less time than others. These apparent inequities tended to relate to different strategies that people used to deal with delays, for example, calling first to see how far the doctor is running behind and showing up five minutes before the appointment. Uncertainty about when they would actually see the doctor meant that women working as domestics or in hospitality had to take time off to see the doctor or refuse work if they worked on call.
Specialist Services and travel assistance: The impact of geographic isolation was most evident in discussions about specialist services. Specialist services were usually delivered by visiting specialists or the nearest central hospital, depending on the urgency of the visit or whether there was an appropriate visiting specialist. This meant that there were often long waits for specialists, and this often precluded access to specialist services where this model of treatment was not appropriate.
Filipinas were more affected by geographic disadvantage because they were less likely to drive and had greater difficulty navigating their eligibility for travel assistance. Assistance to travel to specialist services was provided through the patient transfer assistance scheme. The funding granted for travel was at the discretion of the referring hospital and varied considerably depending on the fitness of the patient for travel, the need for accompanying persons, and the nature of the treatment. For example, one woman received airfares to visit a cardiac specialist in Townsville, while another received payment for mileage to drive her daughter to Townsville to an ear, nose and throat specialist. The method of payment varied according to the method of travel, so that air tickets were provided up-front, but compensation for mileage only occurred after the journey had taken place. The need to pay costs up-front posed some financial difficulty for some of the women. Lack of transparency in the system raised concerns about equity because it was not always clear what women were entitled to and why some women received different treatment than others. Inconsistencies in treatment are added to by the fact that funding for patient transfers is decided by the referring hospital. This meant that a person who lived in Mt Isa, who was admitted directly to another hospital and then transferred back to Mt Isa, may have received different treatment to a patient who was referred from Mt Isa to the same hospital with the same complaint.
Women who had operations performed by specialists resident in other centres were not funded to visit the specialist who actually performed the operation if there was a relevant visiting specialist. In general, women did not find this policy problematic and felt that there was little disruption to continuity of care due to effective hand over. However sometimes women found it threatening to change doctors if the problem was particularly sensitive, for example a gynaecological problem, because it meant repeating the process of building up trust and breaking down cultural barriers to effective communication.
Conclusion
Access to health services and getting their information needs Accommodated were more problematic for Filipinas living in remote/rural areas than women in other parts of the state. The qualitative data suggested that there were also differences in the Affordability and Acceptability of services although no significant differences were detected using quantitative items. There were no differences in Knowledge between remote/rural Filipinas and urban Filipinas however Filipinas in remote/rural areas experienced greater barriers in getting their information needs met.
Differences in the use of health services were mainly due to lack of bulk billing doctors, young and inexperienced doctors, after hours services, specialist services and lack of female doctors. Long waiting times and short consultations meant that women were often unable to get the information they needed. These problems are common to all women living in rural and remote areas and largely reflect limitations in services7-9. However these limitations were exacerbated because of differences in expectations about health services and providers, lack of information and explanation about the way different health problems are treated in Australia and lack of transparency in the way access to services and resources are facilitated10. In some cases barriers to health service use were also exacerbated by Filipinas involvement in domestic and hospitality work where they were unable to take the time to visit health services10.
Much of the disadvantage experienced by Filipinas in remote and rural communities was a function of structural differences in health services. However there were also differences in access to information, which in conjunction with these structural differences did affect the acceptability of services. Filipinas although generally aware of many of the services that did exist in the community did not have access to information that would aid in self-management (eg information about when to present at casualty for conditions like diarrhoea). Improving consumers' understanding of management strategies may improve community perceptions of health care systems, reduce the burden on health care workers and improve quality of care.
Acknowledgements
This work has been supported by the Australian Commonwealth Department of Health and Aged care as part of the Australian Longitudinal Study on Women's Health. It was also supported by an Australian National Health and Medical Research Council Sidney Sax Fellowship. We would like to acknowledge the co-operation of The University of Newcastle and our colleagues of Australian Centre for International & Tropical Health & Nutrition. We would also like to thank health workers, our advisory group and Filipino organisations throughout Queensland for their time and goodwill.
References
1 McKinley RK, Manku-Scott T, Hastings AM, French DP, Baker R. Reliability and validity of a new measure of patient satisfaction with after hours primary medical care in the United Kingdom: development of a patient questionnaire. BMJ 1997; 314: 193-198.
2 Ahmad WIU. The trouble with culture. In: D Kelleher, S Hillier (Eds). Researching cultural differences in health. London: Routledge, 1996; 190-219.
3. Dobson A, Manderson L, Schofield M, Williams G. Women's health Australia: establishment of the Australian Longitudinal Study of Women's Health. Journal of Women's Health 1996; 5: 467-472.
4. Manderson L, Kelaher M, Williams G, Shannon C. The politics of community: negotiation and consultation in research on women's health. Human Organization 1998; 57: 222-239.
5. Elliott-Schmidt R, Strong J. The concept of well-being in a rural setting: understanding health and illness. Australian Journal of Rural Health 1997; 5: 59-63.
6. Coakes SJ, Kelly GJ. Community competence and empowerment: strategies for rural change in women's health services planning and delivery. Australian Journal of Rural Health 1997; 5: 26-30.
7. Brown W, Young AF, Byles JE. Tyranny of distance? The health of mid-age women living in five geographical areas of Australia. Australian Journal of Rural Health 1999; 7: 148-156.
8. Young AF, Dobson AJ, Byles JE. Access and equity in the provision of general practitioner services in Australia. Australian and New Zealand Journal of Public Health. 2000; 24: 474-480.
9. Young AF, Dobson AJ, Byles JE. Determinants of general practitioner use among women in Australia. Social Science and Medicine 2001; 53: 1641-1651.
10. Kelaher M, Williams G, Manderson L. Health issues among Filipino women in remote Queensland, Australia. Australian Journal of Rural Health 2001 9: 150-157.


