The health workforce has been identified as the key to effective health services1,2. However, workforce shortages are the most commonly reported staff-related problem in health care, especially in resource-constrained countries3,4.
Among the many challenges facing Nigeria's health system is an acute shortage of competent healthcare providers. As a result of inadequate infrastructure locally and poor compensation packages, a sizeable number of physicians, nurses and other health professionals migrate to developed countries in search of fulfilling and lucrative positions5. Nigeria is a major health-staff-exporting nation, accounting for 22% of nurses who emigrated out of Africa between April 2000 and March 20016,7; however the true extent of this migration is masked by under-reporting. Whatever the extent, this has resulted to acute shortages of health staff in Nigerian health facilities, which has drastically reduced access to local health care.
The doctors and nurses who remain are reluctant to relocate to remote areas, including forest locations, where communication with other regions is poor and amenities for health professionals and their families are lacking. So the inequitable geographical distribution of healthcare professionals is compounded by a concentration of medical professionals in urban areas. While access to medical personnel may be readily available in cities, rural dwellers often have to travel considerable distances in order to obtain treatment.
Nigerian urban areas are also more attractive to healthcare professionals due to the social, cultural and professional advantages of urban work. Large metropolitan centers offer greater opportunities for career and educational advancement, better employment prospects for health professionals and their spouse, easier access to private practice (an important factor in Nigeria because public salaries are relatively low), lifestyle-related services and amenities, and better access to education for their children7,8. Rural and remote employment is usually regarded as having a low status, while urban positions are perceived as more prestigious.
In Nigeria scarce data on the availability, distribution, and trends in human resources for health (HRH) has been a barrier to effective HRH planning. However, while it has been established that in the Nigerian public sector there are 13 doctors, 92 nurses/midwives, and 64 community health workers (CHWs) per 100 000 population8, an urban Nigerian resident has a 3-fold greater access to doctors and there are twice as many nurses/midwives, compared with a rural resident. Attrition rates of between 1.3% and 2.3% are highest among doctors and pharmacists, with the attrition of doctors and nurses being highest at the primary care level. The attrition rate of doctors and nurses is much higher in rural areas, at triple and double the urban attrition, respectively.
The unavailability of physicians and nurses in rural areas often leads to a delay in seeking health care until symptoms become unbearable and the disease is advanced8. Transporting a seriously ill patient to an urban facility on poor roads may result in a delay makes the difference between life and death7.
This study aimed to determine factors that attract health workers to and retain them in remote rural areas in Ogun State, Nigeria. The study also explored differences or similarities in these factors between rural and urban health workers.
Study sites
Ogun State (otherwise known as the 'Gateway to Nigeria") was created in 1976 in the southwest of Nigeria. It borders Lagos State to the South, Oyo and Osun states to the North, Ondo State to the east and the republic of Benin to the west. The historic city of AbeokutaIts is its capital and largest urban centre9.
Ogun State's predominantly agro-ecological zones consist of rain forest and derived savannah vegetation. The state has a land area of 16 409 km2 with a population of approximately 5 million10, predominantly a homogenous group of Yoruba extraction. Yoruba is the primary language of these people, while English is the second and official language. Agriculture is the major industry9.
In terms of political administration, the state consists of 20 local government areas (LGAs), 4 of which were chosen as study sites: Ifo, Ewekoro, Ado-Odo/Ota and Abeokuta South. Ifo LGA has an estimated population of 100 00011 and is a rural-peri-urban setting consisting of residential and commercial areas. Ifo town is the administrative centre of the LGA, which has 11 wards. Ewekoro LGA is administered from the town of Itori. It has an area of 594 km² and the population was 55 156 in 200610. Ewekoro the location for the premier cement factory of Nigeria; however, the main occupation of residents is trading and farming12. The town of Ota, the capital of the Ado-Odo/Ota LGA, has an estimated 163 783 residents in the town and surrounding areas13. It has the third largest concentration of industry in Nigeria13. Abeokuta South is an LGA administered from Ake Abeokuta. It has an area of 71 km² and in 2006 had a population of 250 27810.
Health service
In compliance with its constitutional responsibility, Ogun State is greatly concerned with the maintenance of a functional primary healthcare system. One of the pioneer, model primary health care (PHC) centers in the country is situated in Pakoto, in Ifo LGA. This PHC center was established to meet the diverse health needs of the local population. In addition, tertiary, secondary and private hospitals are available throughout the state, and the efforts of these hospitals and clinics are complemented by the work of traditional birth attendants at community level.
In 2005 Ogun State's health workforce status per 100 000 population was14:
19 doctors
41 nurses
1.7 medical laboratory scientists
1 rehabilitation therapist
8 pharmacists
15 community health officers/community health extension workers (CHOs/CHEWs)
no radiographers or health records officers.
Study design
The quantitative aspect of the study employed a cross-sectional comparative methodology as a one-time survey with a comparison of factors between rural and urban health workers. Qualitative methods (unpublished data, authors) provided additional information to clarify some findings of the quantitative survey.
Study population and sampling technique
The study participants were drawn from every health worker designation, including facility managers, in the selected PHC facilities; however, auxiliary nurses and volunteer health workers were excluded. Inclusion criteria were that the health worker must have:
undergone formal training in a government-approved training institution and matched the WHO definition of a qualified health worker
been working in a primary health facility in Ogun state.
The total health workers sample size was based on a calculation of minimum sample size using a standard formula applied to the total health workforce in Ogun State. The minimum sample size was calculated as 86 and rounded up to 100 for both urban and rural LGAs to compensate for a 15% non-response rate. These 200 health workers were recruited for the study using multi-stage sampling technique.
Stage1: The 2 rural and 2 urban LGAs were selected by simple random sampling from the 20 LGAs in the state: Ifo and Ewekoro LGAs (rural) and Abeokuta South and Ota LGAs (urban).
Stage 2: Two wards were randomly selected in each of the 4 LGAs.
Stage 3: A total of 5 rural PHC centers and 6 urban PHCs were randomly selected. The rural and urban PCH centers were comparable in terms of health worker mix and services provided, so that the only factors of difference would be attraction and retention to work in rural Nigerian settings.
The selected rural PHC centers in Ifo and Ewekoro had an average health staff of 25 and 20, respectively; while the urban PHCs, Ota and Abeokuta South, averaged 20 and 30 health workers, respectively.
Following the permission of the Chairmen and PHC Directors of the respective LGAs, the health workers were approached through their facility managers. All those eligible to participate were recruited after an explanation of the study purpose and obtaining informed consent.
Data collection techniques and instruments
Data were collected between December 2009 and February 2010. A self-administered, pre-tested questionnaire was adapted from a data tool used in a previous study identified in the literature review15. The parameters listed in the data tool included respondents' work experience, whether or not they liked their current job and reasons for this, reasons for assuming their current job, likelihood to leave their current job, and motivators and de-motivators regarding attraction to and retention in work in rural settings.
Data management
The Epi Info v3.1 software (CDC; Atlanta, GA, USA; http://wwwn.cdc.gov/epiinfo/) was used for data entry, validation, cleaning and analysis. Frequency distributions were generated for all categorical variables and means and standard deviations were determined for the continuous variable. Chi-squared was used for testing significant differences between groups; p was set at <0.05.
Ethical considerations
Ethical approval was obtained from the Research and Ethics Committee of the College of Medicine, University of Lagos. Permission was granted by the Chairmen/PHC Directors of the LGAs. For each participant interviewed, informed consent was obtained.
One hundred questionnaires were distributed to urban LGA respondents and the same number to rural respondents, with 95 and 93 questionnaires returned, respectively. Four urban and 5 rural questionnaires incomplete and discarded, yielding a response rate of 91% and 88%, respectively.
The mean ages of rural and urban LGA respondents were 36.1 ± 10.04 and 36.8 ± 6.86 years, respectively. More than two-thirds of the health workers were female. Approximately 6 of 10 were married with approximately three-quarters having post-secondary education. More than half the respondents were either CHOs or CHEWs (Table 1).
More than two-thirds had worked for between 1 and 9 years. Approximately 6 of 10 workers in both groups had worked elsewhere prior to their current work. Concerning previous rural work experience, almost two-fifths of the rural workers and one-quarter of urban workers had previous rural work experience. Regarding previous urban work experience, over half the health workers in both groups had previous urban work experience. Less than one-fifth in both groups had both rural and urban work experience.
The most common reason for rural and urban respondents leaving former work was administrative transfer (56.1% and 44.4%, respectively); with other reasons including 'search for development opportunities' (19.3% and 26.9%), marriage (17.5% and 9.5%), better salary (1.8% and 15.9%) and cheaper accommodation (5.3% and 3.3%).
To account for differences in rural attraction and retention due to compulsory (administrative) or voluntary transfer, respondents were stratified into two groups for analysis. In the non-transfer (voluntary) group, a statistically significant rural-urban worker difference (p=0.036) existed with more rural participants liking their current work. However there was no significant difference (p=0.412) within the (administrative) transfer group. In the non-transfer group, for those who liked their current job, the reasons 'better staff relationships' (p=0.00053) and 'career development opportunities' (p=0.00045) were significantly different between rural and urban workers. For the transfer group, the only urban-rural worker difference was that the present job provided opportunities for better job prospects (Table 2). Among those who disliked their current job, the reasons given were not significantly different between the rural and urban groups, irrespective of transfer status (Table 2).
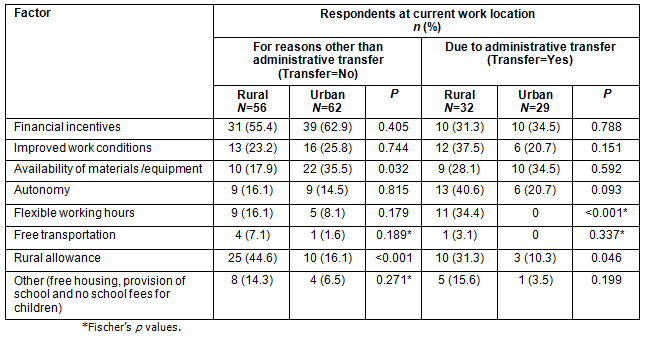
Regarding respondents' reasons for assuming their current employment, while availability of materials and equipment (p=0.032) and rural allowance (p=0.0007) were significantly different for rural and urban workers within the non-transfer group, the reasons did not differ significantly within the transfer group (Table 3).
Table 1: Demographic characteristics of respondents
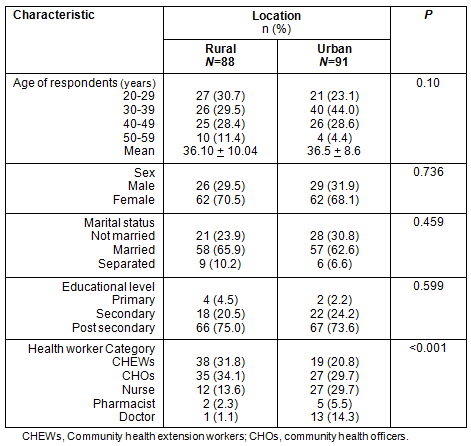
Table 2: Respondents' opinion of their current job
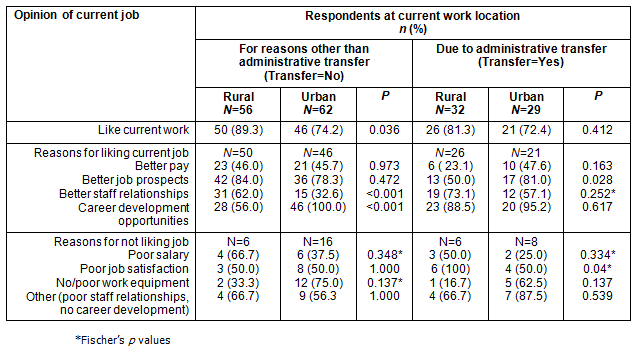
Table 3: Factors that attracted respondents to their current job
Factors that could motivate attraction to rural work among the non-transfer group included opportunities for career development, availability of equipment, flexible working hours (the ability to adjust their compulsory daily 8 hours work time according to the facility workload), rural allowance, staff relationship, safety and availability of good schools for children. However, some (mostly rural) respondents cited instances of having to recall those off duty to work when the workload was heavy, and having to send some workers off duty when the patient load was light.
More urban than rural health workers said that opportunities for career development, availability of materials/equipment and flexible work hours could attract them to work in rural areas, while more rural than urban health workers within the same group considered rural allowance, improved staff relationships, payment of children's school fees and adequate security could increase their willingness to work in rural settings. Significantly different factors within the transfer groups were rural allowance (p=0.002), accommodation (p=0.032) and staff relationships (p=0.011) (Table 4).
Major determinants of job retention within the non-transfer group included: financial incentives (eg salary doubled, rural allowance, guaranteed retirement scheme, and housing and vehicle loans), availability of materials/equipment, staff relationships and recognition of their work by the community. While for those in the transfer group, significantly different job retention determinants were rural allowance, recognition of their work by the community, accommodation, staff relationships and participatory supervision (Table 5).
Likelihood to leave a current job was explored as an indirect assessment of job satisfaction and likelihood of retention. More rural than urban health workers expressed a desire to continue in their current jobs and would be likely to return to their current jobs in the event of a break from work. Although more rural than urban workers expressed a desire to continue in the profession, this difference was not significant. However, significant differences (p<0.05), existed between the two groups with respect to the length of time the worker would like to stay in the profession and the likelihood of returning to the profession after a break.
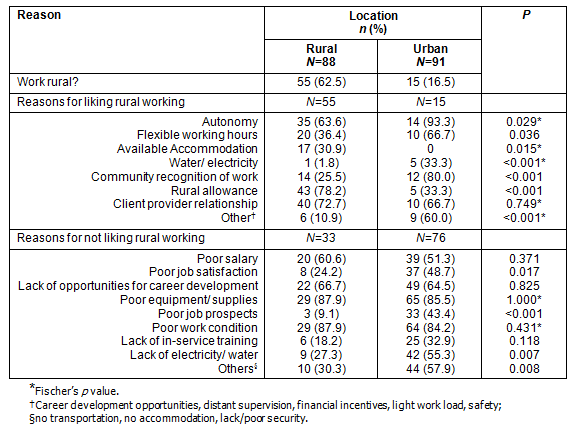
While 62.5% of rural workers expressed desire to continue to work in rural areas, only 16.5% of urban workers were willing to work in rural areas. Among those willing to work in rural areas, major reasons included: autonomy, available accommodation, rural allowance, flexible working hours, community recognition of work, and better client-provider relationships. For those unwilling to work in rural areas, major reasons cited included: poor equipment/supplies, lack of opportunities for career development, poor work condition, lack of electricity/water and poor salary (Table 6).
A multivariate analysis of these factors, however, revealed that the willingness to work and remain in rural areas was significantly affected by the age of respondents, previous work experience, and liking their present work. Younger respondents, those who had had previous work experience and those who liked their current work were more willing to work and remain in rural areas. Previous rural work experience had no significant relationship with willingness to work and remain in rural settings.
Table 4: Factors that may attract respondents to work in rural areas
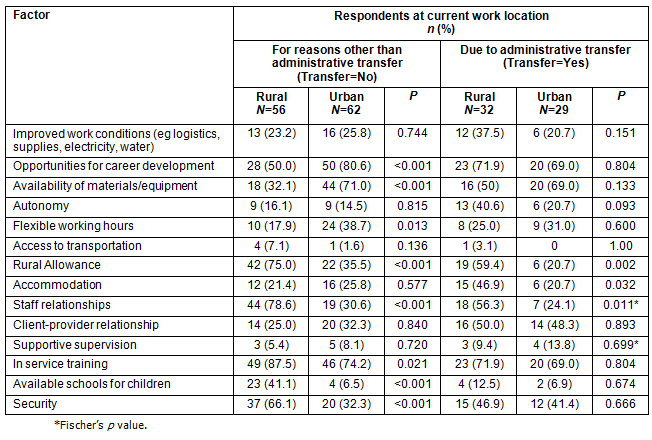
Table 5: Factors that may influence respondents to retain jobs in rural areas
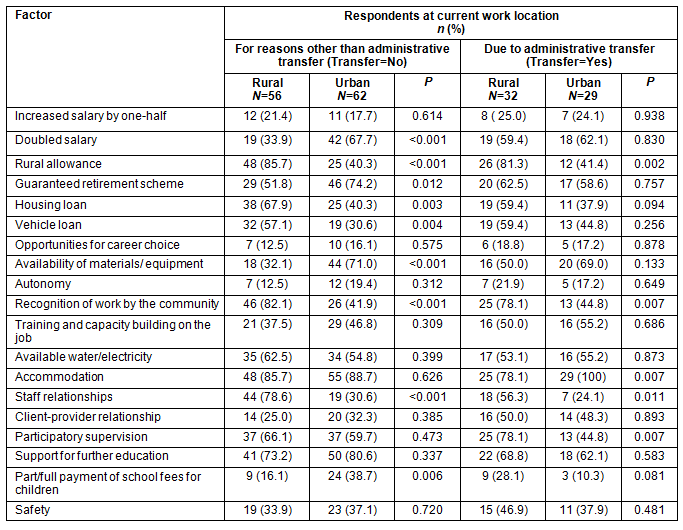
Table 6: Health workers' willingness and unwillingness to work in rural areas
Discussion
Nigeria faces a major challenge regarding its ability to provide and retain an adequate, competent health workforce in the right mix to provide health care in areas where services are most needed. This challenge is complicated by many global and disease obligations, such as the UN Health Millennium Development Goals (HMDGs); the Global Fund to fight HIV/AIDS, Tuberculosis and Malaria; the Roll Back Malaria Programme and the Polio Eradication Campaign, which has implications for human resources for health16.
In WHO's 2006 report to mark WHO Day, it called on governments, civilian societies, individuals and the entire international community to better understand and take action to plan for the production of skilled health workers, and to improve the working environment and wellbeing of health workers2. In response to this, Nigeria developed a National Human Resources for Health Policy14; however, it was silent on guidelines pertaining to rural health manpower development.
Findings from the present study have shown that attraction and retention motivators for rural work were similar for both groups. These included the availability of equipment and supplies, effective and efficient support systems, career development opportunities, and better living and family support systems. This supports the findings of previous studies which identified factors such as socio-demographics, career advancement opportunities, and working and living conditions17-23 . A multivariate analysis of motivational factors, however, revealed some significant differences among rural health workers, with the age of the health worker, their previous work experience and perception of their present work significantly influencing a willingness to work and remain in rural areas.
Younger respondents, and those who had previous work experience and expressed a liking for their current work were more willing to work and remain in rural areas. It may be that the younger health workers were mobile enough to relocate to rural and remote areas, being less likely to be married and therefore having fewer family ties. Previous work experience and liking their present work may have afforded opportunities to acquire work experience and this may subsequently influence willingness to work in rural areas - although willingness was not influenced by previous rural work experience. Being at a current work location due to compulsory administrative transfer or not did not significantly influence workers' willingness to work and remain in rural areas.
Study limitations
There are two limitations to this study. First, inadequate funds restricted scope of study to only 4 LGAs. Second, there was some difficulty in retrieving questionnaire from respondents.
Conclusion
The study findings revealed that working conditions, career development opportunities, and appropriate infrastructural issues are still core factors affecting an individual's motivation for rural work, regardless of the health worker's geographic origin. This calls for an urgent and comprehensive review, and accommodation of issues related to staff motivation if the HMDGs are to be realized. This would entail developing a comprehensive rural health work force improvement strategy which incorporates a coordinated intersectoral approach involving partnership among stakeholders in rural health development.
References
1. Joint Learning Initiative. Human resources for health. Overcoming the crisis. Cambridge, MA: Global health Initiative/Harvard University Press; 2004.
2. World Health Organization. The World Health Report 2006: working together for health. Geneva, World Health Organization, 2006.
3. Kirigia JM, Gbary AR, Muthuri LK, Nyoni J, Seddoh A. The cost of health professionals' brain drain in Kenya. BioMed Central Health Service Research 2006; 6: 89.
4. Muula AS, Panulo B Jr, Maseko FC. The financial losses from the migration of nurses from Malawi. BioMed Central Nursing 2006; 5: 9.
5. Awofeso N. Managing brain drain and brain waste of health workers in Nigeria. (Online) 2008. Available: http://www.who.int/bulletin/bulletin_board/82/stilwell1/en/ (Accessed 10 August 2008).
6. Nnamuchi O. The right to health in Nigeria. (Online) 2007. Available: http://www.abdn.ac.uk/law/documents/Nigeria_%20210808.pdf (Accessed 10 June 2008).
7. Uneke A, Ogbonna A, Ezeoha P, Oyibo F, Onwe B, Ngwu & Innovative Health Research Group. The Nigeria health sector and human resource challenges. The Internet Journal of Health 2008; 8(1). (Online) 2008. Available: http://www.ispub.com/journal/the_internet_journal_of_health/volume_8_number_1_5/article/the_nigeria_health_sector_and_human_resource_challenges.html
8. Chankova S, Nguyen H, Chipanta D, Kombe G, Onoja A, Ogungbemi K. Catalyzing human resources mobilization: a look at the situation in Nigeria. In, Proceedings, Global Health Council Annual Conference; 30 May 2007; Washington DC, 2007. (Accessed 2 February 2011).
9. Facebook. OGUN STATE... the gateway to Nigeria! Available: http://www.facebook.com/note.php?note_id=22661703845 (Accessed 7 February 2011).
10. Government of Nigeria. National Bureau of Statistics. (Online) 2010. Available: www.nigerianstat.gov.ng (Accessed 28 March 2010).
11. Wikipedia. Ifo. (Online) 2010. Available: http://en.wikipedia.org/wiki/Ifo (Accessed 21 December 2010).
12. Wikipedia. Ewekoro. (Online) 2010. Available: http://en.wikipedia.org/wiki/Ewekoro (Accessed 21 December 2010).
13. Wikipedia. Ota, Nigeria. (Online) 2010. Available: http://en.wikipedia.org/wiki/ota,_Nigeria (Accessed 14 March 2010).
14. Federal Ministry of Health Nigeria. Draft National Human Resources for Health Policy. Abuja: Government of Nigeria, 2007; 1-47.
15. Aiken LH, Patrician PA. Measuring organizational traits of hospitals: the revised nursing work index. Nursing Research 2000, 49(3): 146-153.
16. Gomez Sambo L. Crisis in Human Resources for Health in the African Region. African Health Monitor 2007; 7(1): 3.
17. Kotzee T, Couper ID. What interventions do South African qualified doctors think will retain them in rural hospitals of the Limpopo province of South Africa. Rural and Remote Health 6: 581. (Online) 2006. Available: www.rrh.org.au (Accessed 21 December 2010).
18. Sengooba F, Rahman S, Hongoro C, Rutebemberwa E, Mustafa A, Kielmann T et al. Health sector reforms and human resources for health in Uganda and Bangladesh: mechanisms of effect. Human Resources for Health 2007; 5: 3.
19. Willis-Shattuck M, Bidwell P, Thomas S, Wyness L, Blaauw D, Ditlopo P. Motivation and retention of health workers in developing countries: a systematic review. BioMed Central Health Service Research 2008; 8: 247.
20. Manafa O, McAuliffe E, Maseko F, Bowie C, MacLachlan M, Normand C. Retention of health workers in Malawi: perspectives of health workers and district management, Human Resources for Health 2009; 7: 65.
21. Agyepong IA, Anafi P, Asiamah E, Ansah E, Ashon D, Narh-Dometey C. Health worker (internal customer) satisfaction and motivation in the public sector in Ghana. International Journal of Health Planning and Management 2004; 19: 319-336.
22. Manongi R, Marchant T, Bygbjerg IC. Improving motivation among primary health care workers in Tanzania: a health worker perspective. Human Resources for Health 2006; 4: 6.
23. Reid S. Monitoring the effect of the new rural allowance for health professionals. Durban: Health Systems Trust, 2004; 1-7.

