Introduction
Among US rural counties, 65% lack adequate numbers of health professionals, with the distribution of physicians favoring urban areas1,2. Rural areas have significant health workforce shortages, rural residents are more dependent on public assistance programs and rural residents must travel farther to see a physician compared with their urban counterparts3,4. Physician specialists are not as plentiful as primary care (PC) physicians in rural settings5. Shortages also exist of other professions in rural areas, such as dentists6, nurses7 and mental health providers6-8. Overall, recruitment and retention of rural healthcare professionals remains a difficult problem and impacts on access to health care4,9-11.
The purposes of this exploratory study were to: (i) assess whether and to what extent US rural hospital chief executive officers (CEOs) experience similar regional health professions shortages; and (ii) identify to what extent they report similar or different regional issues in the recruitment and retention processes for rural communities. Glasser et al. assessed the extent of shortages by asking CEOs in Illinois their perspectives on rural healthcare workforce shortages12. The authors concluded that Illinois continues to experience shortages and suggested various recruitment and retention difficulties associated with the rural healthcare workforce. In a recent study comparing rural hospital CEOs' reported shortages of health professionals in Illinois and Arkansas, many common workforce shortage patterns were observed as well as similar issues related to recruiting and retaining healthcare professionals in rural areas13. The present study builds on this past work to assess to what extent rural health professions workforce shortages are reported nationally and to examine possible differences between professions and major geographic areas of the USA. Differences in the CEOs' ratings of attributes influencing recruiting and retention are also examined and their relationship to the extent of PC shortages assessed.
Methods
Survey sample
A multi-step process was used to identify and recruit rural hospital CEOs. First, a list of Area Health Education Center (AHEC) directors was obtained from the National AHEC office. The AHEC Directors were targeted because of familiarity with hospital leadership in their regions; they were sent a letter with a request to list rural hospitals in their area and the contact information for the hospital and CEO. Second, the rural hospitals identified through this process were combined with previously gathered information about rural hospitals from the Arkansas Department of Health and Human Services and Illinois rural CEOs identified through the Illinois Hospital Association. Once the national hospital list was developed, the 2003 Rural Urban Commuting Area (RUCA) codes were used to identify hospitals in an area designated as rural (having a RUCA code of 4 or higher). This resulted in a sample frame of 1031 rural hospitals. The RUCA codes and related ZIP code-RUCA code estimates have been developed by the US Department of Agriculture and the University of Washington. This approach uses a census tract-based classification scheme from the Bureau of the Census for urbanized area standard and place definitions, in combination with commuting information for a ZIP code to characterize its rural and urban status, that is, its degree of rurality and metro proximity. Codes assigned range from 1 (most urban) to 10 (most rural) with additional information indicated by decimals14.
All rural CEOs were mailed a survey using methods approved by the local Institutional Review Board. Respondents names were not requested. There were two mailings to hospital CEOs (June 2008, with follow-up 4 weeks later) and both contained self-addressed return envelopes.
Survey instrument
The three-page survey contained questions about whether or not physician shortages were present in the CEO's community, and physician needs by specialty. The CEOs were also asked to assess whether other health professionals were needed in their town or within a 48 km (30 mile) radius. Three questions were asked in relation to physician supply (capitals were used for emphasis to respondents) that concluded with a question about perceived shortage: (i) 'Number of physicians needed in this specialty in your TOWN'; (ii) 'Do people currently have trouble seeing doctors in this specialty?'; and (iii) 'Is there a shortage of doctors in this specialty WITHIN A 30 MILE RADIUS (yes or no)?'. Finally, the CEOs responded to 16 Likert-scaled questions regarding recruitment and retention of health professionals in rural areas. There were also open-ended questions about major needs in the community related to health issues and health professions student training at the hospital.
Analysis
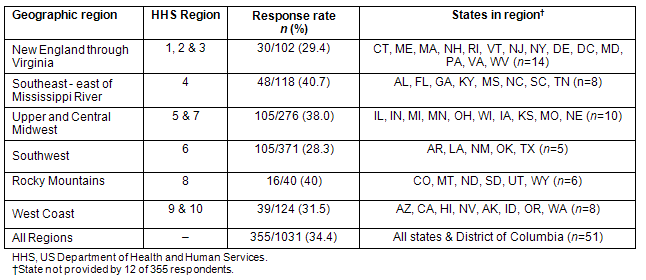
For description and analysis purposes, responding hospitals were assigned to major geographic areas based on US Department of Health and Human Services regions; SPSS v15 (SPSS Inc; Chicago, IL, USA; www.spps.com) was used for all analyses. Details on the geographic groupings are given, with response rates by region (Table 1). The overall response rate was 34.4% (355/1031).
Table 1: Geographic groupings information
Cross-tabulation was used to compare geographic regions related to shortages of physicians and other healthcare professionals. Primary care specialties were defined as family medicine (FM), general internal medicine (IM) and pediatrics (PEDS). Chi-square statistics were used to assess differences in the patterns of responses between regions. Analysis of variance was used to compare means on Likert-scale questions assessing recruitment and retention. Assessment of the magnitude and direction of the association of the correlation between extent of PC physician shortages in the community and the rating on each of the recruitment/retention factors (ranging from 1 to 5), was conducted using Spearman's Rho. In addition to looking at need for specific PC specialties, as a measure of the extent of the need for PC physicians a composite variable (ranging from 0 to 3) and based on the number of different types of PC physicians was operationalized. This PC shortage variable ranged from none of any type of PC physicians needed to all three PC specialties needed specifically valued as: 0 if no PC specialties were needed; 1 if one type of PC specialty was needed; 2 if two types of PC specialties were needed; and 3 if three types of PC specialties were needed.
Results
As shown in Table 1, response rates ranged from approximately 30% to 40% by region with an overall response rate of 34.4%. The highest response rate was in the southeastern states (40.7%) and the lowest response was in the Southwest (28.3%). At least 94% of the survey respondents were in locations that were designated Health Professions Shortage Areas (HPSAs) for one or more professions and/or were medically underserved populations; 3.9% reported no location; and 2.3% were in a location that is not a HPSA or is not medically underserved. Using the US Department of Health and Human Services, Centers for Medicare and Medicaid Services (CMS), 52% of all rural ZIP codes nationally15 were designated as PC shortage areas in 2007. A very similar percentage (49%) of the rural CEO survey respondents were located in CMS PC shortage ZIP codes. The percentage of CEO respondents in rural ZIP codes with RUCA14 codes of 4 and 5 was 29.3%, compared with 27.6% of rural ZIP codes being RUCA codes 4 and 5 nationally. Also, the percent of responding CEOs who were in ZIP codes with RUCA codes 6 and over was 69.1%, compared with 72.4% of all rural ZIP codes in the USA being RUCA codes 6 and over. The similarity of PC shortage and rurality patterns provides support for the survey respondents being representative of rural hospital CEOs.
Primary care physician shortages
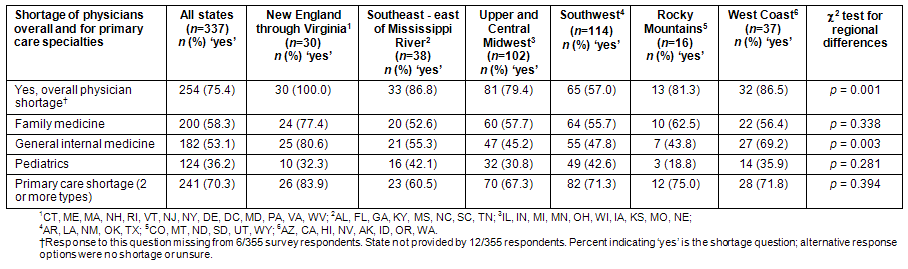
Overall physician shortages were reported by 75% of the responding CEOs (Table 2). There was considerable variations among regions, with 57% of Southwest area CEOs reporting shortages, compared with 100% of the CEOs in the New England through Virginia region. No statistically significant differences were observed in the percentage of CEOs reporting shortages of FM and PEDS physicians between regions, with national percentages of approximately 58% and 36%, respectively. However, there was a significant difference in reported shortages of general IM physicians, mainly due to the high reported need in the New England through Virginia area (approximately 81%; p = .003). Nationally 53.1% of respondents indicated a shortage of IM physicians. The percentage of CEOs reporting shortages of two or more PC specialties (FM, IM or PEDS) was 70.3% nationally, with no statistically significant regional variation (p = .394). However, the percentage of respondents reporting a shortage of IM physicians was higher for the New England through Virginia region (83.9%) than for all other regions.
Table 2: Rural hospital CEO responses regarding need for primary care physicians in their community: National Rural CEO Survey, Summer 2008
Specialty physician shortages
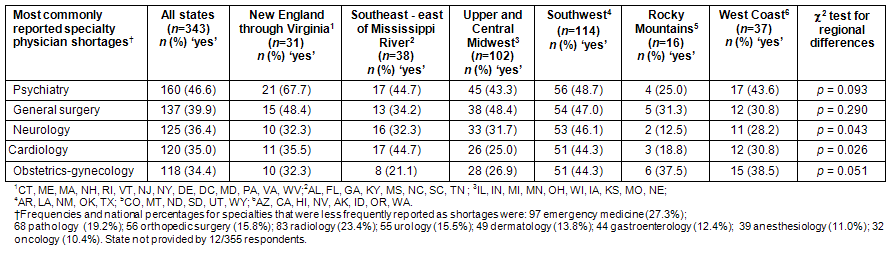
Overall, comparing information presented in Tables 2 and 3, there were fewer specialty physician shortages reported compared with adult PC physician shortages. The CEOs reported the highest specialty care shortages for psychiatry (46.6%) followed by general surgery (39.9%), neurology (36.4%), cardiology (35.0%) and obstetrics-gynecology (34.4%). These major specialty shortages showed considerable variation among regions; however, only for neurology and cardiology were differences among regions statistically significant (p < .05). Unlike other regions, the rural CEOs in the Southwest region consistently reported shortages of these 5 specialty types. In other regions, the extent of reported shortages was more variable among these 5 specialties. The need for psychiatry in rural areas was, proportionately, most often reported in the New England through Virginia region (67.7%). Other specialties reported as shortages less frequently ranged from 27.3% for emergency medicine to 10.4% for oncology.
Table 3: Rural hospital CEO responses regarding need for specialist physicians in their community: National Rural CEO Survey, Summer 2008
Other professions shortages
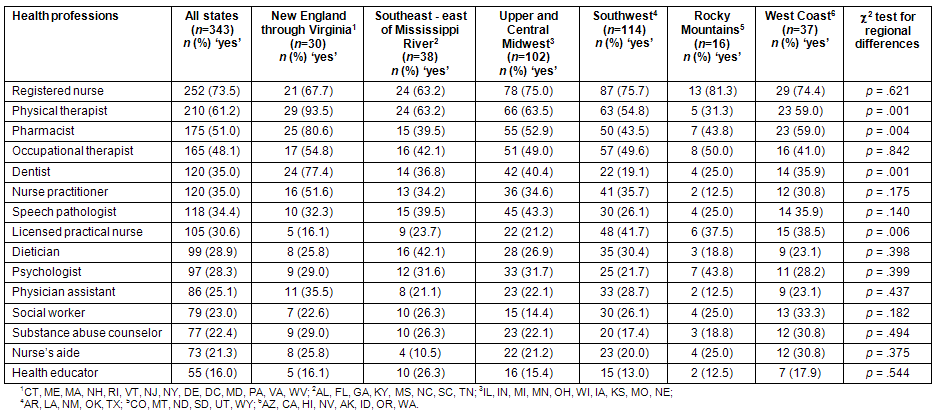
Marked variation in need for healthcare professionals was reported, ranging from approximately 73% for registered nurses (RNs) to 16% for health educators. The percentage of CEOs reporting a need for RNs in rural areas was almost 74% nationally, and 35% reported a need for nurse practitioners. Differences between CEO's ratings of need for both RNs and nurse practitioners were not statistically significant among regions (Table 4). Nationally, approximately 30% of CEOs reported a shortage of licensed practical nurses, which differed significantly among regions, with the 3 western regions showing higher reported shortages (p = .006). There was variation in physical therapist shortages, with 61.2% of CEOs reporting shortages nationally. However, the percentage for physical therapists was considerably higher in the New England to Virginia area (93.5%), and much lower in the Rocky Mountain States (31.3%). A similar pattern was observed for pharmacists, with rural CEOs from New England through Virginia reporting a much higher shortage for pharmacists (80.6%) than in other rural areas, compared with only approximately half of the CEOs reporting a shortage nationally.
Nationally, approximately one-third of the rural CEOs reported a shortage of speech pathologists, with no statistically significant differences among regions. The percentage indicating a shortage of other professions ranged from a high of 28.9% for dietitians to a low of 16% for health educators.
Table 4: Rural hospital CEO responses regarding other health professionals shortages in their community: National Rural CEO Survey, summer 2008
Primary care and other professions shortages
The possible relationship between reports of PC shortages and other healthcare professionals was examined by cross-tabulation of CEO reported shortages of two or more PC doctors with their indication of the need for other health professionals (Personal data, present authors, 2010). Those CEOs who responded that there was a shortage of PC physicians in their geographical areas were also more likely than CEOs not reporting PC shortages to report the need for: nurse practitioners, 39.5% versus 22.4% (p < .001); physician assistants 29.8% versus 13.1% (p < .001); pharmacists, 54.8% versus 40.2% (p = .011); and dentists, 39.5% versus 22.4% (p = .002). The CEOs in the reported shortage areas were also somewhat more likely to indicate a shortage of dental hygienists, 13.3% versus 6.5% (p = .064). Those CEOs not in PC shortage areas were more likely to report a shortage of nurse aids, 29.9% versus 16.9% (p = .006).
Comparison of ratings for recruitment and retention factors
The rural CEOs' views of issues in recruitment and retention of health professionals in their communities is summarized (Table 5). Overall, in relation to the health and status of the community, the CEOs most strongly agreed that health care is a major part of local economic development. Regionally, all CEOs tended to agree with this statement, although hospital administrators in the New England through Virginia and the Upper and Central Midwest regions more often agreed with this assessment, particularly in comparison with CEOs located southeast of the Mississippi River. Nationally, the CEOs also agreed that their communities were good places for a family and that doctors were well respected and supported in their communities. Although not rated quite as highly, the rural CEOs also generally positively evaluated their communities in agreeing that: community health professionals get along and work well together; people in their communities are friendly and supportive of each other; and healthcare providers and other sectors of the community work well together. However, the CEOs were neutral or below in their response to the statement that the overall health of the community is good. Most skeptical in this appraisal were CEOs in the regions southeast of the Mississippi River and New England through Virginia.
Table 5: Rural hospital CEO perceptions of recruitment and retention issues in their communities scores
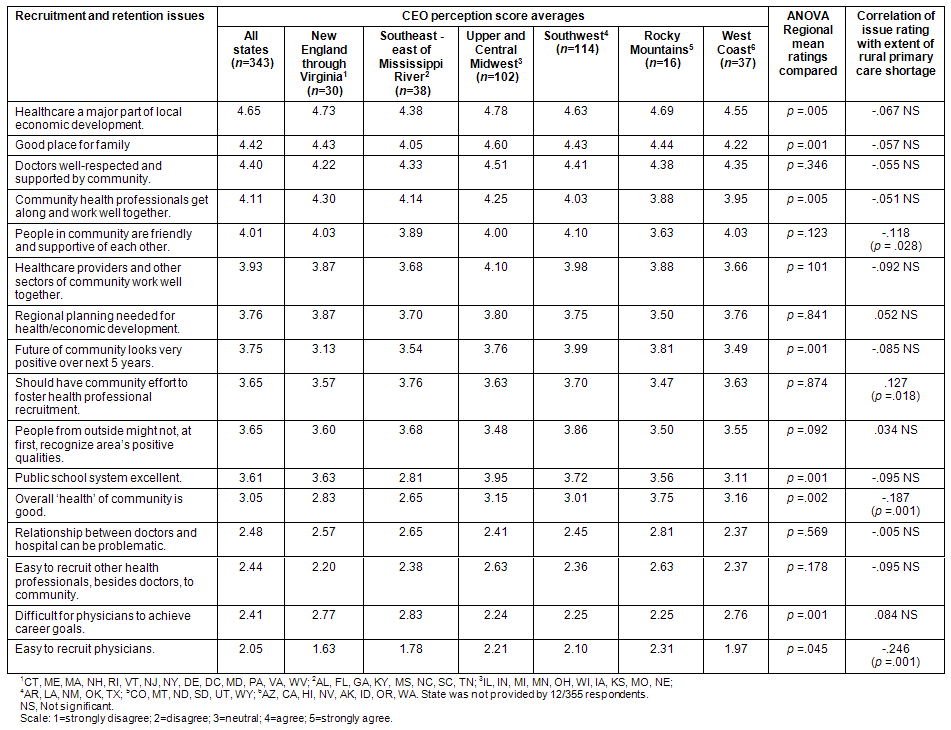
In terms of workforce development and outcomes, recruitment was a major concern. Nationally, the item that received the least positive evaluation by the CEOs was that it is easy to recruit physicians, with CEOs in New England through Virginia and southeast of the Mississippi River least likely to agree with this statement. The CEOs also expressed difficulty related to it being easy to recruit other health professionals to their communities. However, the respondents tended to disagree that once physicians were in the rural communities it would be difficult to achieve career goals.
Correlation between overall physician shortage and recruitment/retention factors
Three of the recruitment/retention factors were found to be significantly correlated with the extent of the reported PC shortage in the region (ranging from 0 to 3 PC specialty shortages); 2 items were negatively associated. Specifically, the higher the CEO's rating that people in the community were perceived as friendly and supportive of each other, the less likely was indication of PC shortages (r = -.118). Similarly, the higher the assessment that the overall health of community is good, the less likely were reported PC shortages (r = -.187). However, CEOs who were more likely to agree that community effort was needed to foster health professional recruitment were also more likely to report PC shortages in their community (r = .127).
Discussion
Nationwide and within distinct geographic regions in the USA, rural hospital CEOs participating in this exploratory study clearly agreed that physician and other healthcare professions shortages exist. The percentage of survey respondents indicating they had a PC physician shortage was approximately the same as the percentage of rural ZIP codes that are designated by CMS as PC shortage areas. This provides support that the survey respondents in this study were representative of rural hospital CEO perspectives. In addition, the current survey response rate (34%) was similar to the response rate (38%) in a national survey of CEOs16 commissioned by a national health care executive organization. Based on RUCA codes, the pattern with regard to rurality of survey respondent locations was similar to national rurality patterns.
Family medicine, general IM and psychiatric physicians were identified as the top three specialty shortages. States in the New England through Virginia region reported the highest shortages in rural areas for family and general IM physicians. Whether this is a pattern in the region or unique to the response pattern associated with CEOs participating in the survey will require more detailed regional studies. It did appear that those rural CEOs with the greatest shortages (physician and other professionals) were somewhat more likely to respond to the survey.
Even within PC specialties, there were differences in perceived need when comparing FM and IM with PEDS. For most regions, shortages of pediatricians were reported at a lower percentage than the other two PC specialties. This topic would be an interesting area to pursue in future research related to PC needs both nationally and within geographic regions of the country.
These findings at the national level related to shortages of family physicians are very similar to findings reported by the current authors in a study focusing on Illinois and Arkansas (58.3% in the present study compared with 57.4% in Illinois-Arkansas)13. Similarly, in a study of community health centers (CHCs), Rosenblatt et al.17 reported that the percentage of rural CHCs indicating that recruiting was very difficult for FM physicians was considerably higher than urban CHCs (41.8% and 20.8%, respectively, p <.001). For IM, the percent shortage in the current study was slightly higher (53.1%) than in the Illinois-Arkansas study (45.7%). Related to pediatrics, the reported shortages were again very similar (36.2% nationally vs 34.4% for Illinois-Arkansas). Bola and Pathman18 found, in a survey of community residents in the southeast of USA that approximately half (46.8%) did not believe there were enough doctors in their community, which is significantly lower than the 86.8% of CEOs who indicated an overall shortage of physicians in the states defined as southeast in the current study. This stems mainly from differences in the definition of 'shortage' and in the definition of the 'southeast' region or from the perceptions of residents about shortages and their willingness to use local health care. Regardless of specific geographic divisions or metrics used in the assessment of 'shortage', it is very clear from this study and other literature that the supply of physicians in most rural areas is less than adequate.
Our study also reinforces the concern that there is a shortage of specialty physicians in the USA. Cooper points out that the prevalence of conditions requiring specialty care is increasing19. Included in this is a 'serious and increasing shortage of psychiatrists nearly everywhere except in the larger urban areas' (p.764). In the present study, the highest specialty shortage reported by rural hospital CEOs was psychiatrists, approximately 47%, followed by general surgeons, approximately 40%. These findings are not surprising because only 7.4% of all psychiatrists practicing in 2005 were located in rural US areas (RUCA code 4 or greater) and only 14.2% of general surgeons practicing in 2005 were located in rural areas based on coding of practice address in the American Medical Association Masterfile (B Bowman; pers. comm., 2010).
With respect to shortages of other healthcare professionals, the four most frequently reported nationally were registered nurses, physical therapists, pharmacists and occupational therapists. Again, the percentages reported for these professions were highest in the New England through Virginia region. Whether this is unique to the respondents reporting in this study or is a pattern in the region would require a more detailed regional study. Overall, results are consistent with recent calls for training and placement of such health professionals as nurses and pharmacists to meet rural and underserved population needs.
For most attributes addressed in our study, ratings related to retention and recruitment issues were similar for CEOs in all regions. Some regional differences existed, but generally ratings followed the themes found important by Glasser et al.12. These themes were based on the perspectives of Illinois rural hospital CEOs using 16 Likert-scaled items (strongly disagree to strongly agree) inquiring about the importance of a variety of factors that prior literature had supported as relating to the recruitment and retention of physicians and other health professionals in rural communities. These included attractiveness related to the family environment, community spirit, and positive interactions between professionals and the community as well as among healthcare professionals. Attractiveness appears to consist of several components when common themes are assessed. However, a positive attitude towards schools was not ranked as highly in this national study as in the prior two state Illinois-Arkansas study13. However, there were some differences among regions related to the themes of future of the community, communication within the community, quality of public schools and cooperation within the community.
Overall, this and prior studies indicate that 'community culture' needs to be open, helpful and supportive of healthcare professionals. Cooperation among professionals and other sectors within the community is important for two reasons. First, it appears that the friendliness of people, the relationships between professionals and the hospital and the ability of community groups and other healthcare professionals to work well together are related to a perception of being respected and being able to achieve future goals. Second, candidates for employment may view regional or community planning as a sign of harmony and a common vision versus lack of consensus about a direction for the community. If candidates do not perceive these factors, then CEOs believe recruiting and retention are more difficult. An implication for CEOs seeking to improve their recruiting situation is that they should work with other community leaders on a long-term basis to improve key attributes of the community that contribute to strong public education systems, economic development and the overall quality of life.
Limitations
Certain limitations to the present study must be acknowledged. First, this study is based on a subset of rural hospitals in each state whose CEOs were willing to respond to the survey. If different rural hospitals had responded in each region, the findings could have changed; however, the response rates were adequate for a nationwide survey involving hospital CEOs. Second, additional information from other sources (such as turnover rates for positions, job advertisements placed or the length of time positions were open etc) that could be indicative of shortages should be used to verify the survey results. The CEOs assessed if a physician shortage existed, based on their individual view of the meaning of 'shortage'. The 'shortage' question did follow questions that asked and encouraged thought about the number needed and whether people had difficulty accessing a given type of physician. Whether or not there was need for other health professionals was also assessed by the responding CEO.
Conclusion
This study does lend support from a national sample to the belief that shortages of many professionals exist within rural healthcare settings/systems. Overall, this study offers additional evidence of the importance of strongly promoting PC in medical and all health professions education and in advancing policies that will develop an adequate supply of PC providers who will locate and stay in rural communities.
Acknowledgements
This study was supported in part by Project EXPORT Grant Number P20 MD000524 from the National Center on Minority Health and Health Disparities, National Institutes of Health. The article contents are solely the responsibility of the authors and do not necessarily represent the official view of the National Institutes of Health.
References
1. Probst JC, Moore CG, Glover SH, Samuels ME. Person and place: The compounding effects of race/ethnicity and rurality on health. American Journal of Public Health 2004; 94(10): 1695-1703.
2. National Rural Health Association. What's Different About Rural Health Care? (Online) no date. Available: http://www.ruralhealthweb.org/go/left/approximately -rural-health/what-s-different-approximately -rural-health-care/what-s-different-approximately -rural-health-care (Accessed 16 November 2009).
3. Arcury T, Gesler WM, Preisser JS, Sherman J, Spencer J, Perin J. The effects of geography and spatial behavior on health care utilization among the residents of a rural region. Health Service Research 2005; 40(1): 135-156.
4. Reschovsky JD, Staiti AB. Access and quality: Does rural America lag behind? Health Affairs 2005; 24(4): 1128-1139.
5. Rickets TC. Workforce issues in rural areas: A focus on policy equity. American Journal of Public Health 2005; 95(1): 42-48.
6. Knapp KK, Hardwick K. The availability and distribution of dentists in rural ZIP codes and Primary Care Health Professional Shortage Areas (PC-HPSA) ZIP codes: Comparison with primary care providers. Journal of Public Health Dentistry 2000; 60(1): 43-48.
7. Cramer M, Nienaber J, Helget P, Agrawal S. Comparative analysis of urban and rural nursing workforce shortages in Nebraska hospitals. Policy, Politics, and Nursing Practice 2006; 7(4): 248-260.
8. Baldwin LM, Patanian MM, Larson EH, Lishner DM, Mauksch LB, Katon WJ et al. Modeling the mental health workforce in Washington State: Using state licensing data to examine provider supply in rural and urban areas. Journal of Rural Health 2006; 22(1): 50-58.
9. National Rural Health Association. Physician recruitment and retention. (Online) 1998. Available: http://www.ruralhealthweb.org/go/left/policy-and-advocacy/policy-documents-and-statements/official-policy-positions/archived-policy-positions/archived-policy-positions (Accessed 16 November 2009).
10. National Rural Health Association. Rural Health Careers Pipeline: Kindergarten to 12th Grade Education. Rural Health Careers Pipeline series no.7. Official Policy Positions. (Online) 2006. Available: http://www.ruralhealthweb.org/go/left/policy-and-advocacy/policy-documents-and-statements/official-policy-positions/official-policy-positions (Accessed 16 November 2009).
11. Steinwald B. Testimony before the Committee on Health, Education, Labor, and Pensions, U.S. Senate. Primary Care Professionals: Recent Supply Trends, Projections, and Valuation of Services. (Online) 2008. Available: www.gao.gov/new.items/d08472t.pdf (Accessed 16 November 2009).
12. Glasser M, Peters K, MacDowell M. Rural Illinois hospital chief executive officers' perceptions of provider shortages and issues in rural recruitment and retention. Journal of Rural Health 2006; 22(1): 59-62.
13. MacDowell M, Glasser M, Fitts M, Fratzke M, Peters K. Perspectives on rural health workforce issues: Illinois-Arkansas comparison. Journal of Rural Health 2009; 25(2): 135-140.
14. The United States Department of Agriculture, Economic Research Service. Rural-Urban Commuting Area Codes. (Online) 2005. Available: http://151.121.68.30/Data/RuralUrbanCommutingAreaCodes (Accessed 16 November 2009).
15. US Department of Health & Human Services. From analysis of percent of rural population in each region living in an area defined as a CMS shortage area in 2004 - FY 2005. (Online) no date. Available: www.cms.hhs.gov/HPSAPSAPhysicianBonuses/ (Accessed 16 November 2009).
16. Khaliq AA, Thompson DM, Walston SL. Perceptions of hospital CEOs about the effects of CEO turnover. Hospital Topics 2006; 84(4): 21-7.
17. Rosenblatt R, Andrilla H, Curtin T, Hart G. Shortage of Medical Personnel in Coummunity Health Centers. Journal of the American Medical Association 2006; 295(9): 1042-1049.
18. Bola H, Pathman D. Are there enough doctors in my rural community? Perceptions of the local physician supply. Journal of Rural Health 2009; 25(2): 115-123.
19. Cooper RA. There's a shortage of specialists. Is anyone listening? Academic Medicine 2002; 77(8): 761-766.




