Editor's Note
The Chalmers Oration is an annual event celebrating the achievements of Professor John Chalmers AM, the Foundation Chair in Medicine at the Flinders University School of Medicine, South Australia.
This article is based on the 2010 Chalmers Oration delivered by Dr Tom Calma on 15 August 2010 in Adelaide, South Australia at Flinders University. The 2010 Oration is reproduced in Rural and Remote Health because of the importance of Indigenous health to this journal, and the groundbreaking role that Dr Tom Calma and the Close the Gap Campaign has played in making a difference to the health of Indigenous Australians, especially those who live in rural and remote Australia.
Paul Worley
Editor in Chief
Rural and Remote Health
-------------------------
Acknowledgement of the traditional owners
Thank you, Elder David Copley for your welcome to country. I acknowledge your people, the Kuarna people, the traditional owners of the land on which we are meeting and I pay my respects to the Elders and especially to Kuarna children and youth who will be the future Elders and holders of your knowledge, culture, language and heritage.
Introduction
This presentation is made from the perspective of several roles. The first is my 2004 to 2010 role as former Aboriginal and Torres Strait Islander Social Justice Commissioner. In that role I was convenor of the 'Close the Gap Campaign for Indigenous Health Equality' (the Close the Gap Campaign; http://www.closethegap.com.au/), which is the main topic of this Oration. The second is my role as National Coordinator for 'Tackling Indigenous Smoking', held since March 2010. The third is my role as National Patron of the Poche Centres for Indigenous Health, an exciting new venture that also involves Flinders University.
As I begin I am aware of the illustrious speakers and friends who have gone before me, among them Professor Fiona Stanley, former Prime Minister Malcolm Fraser, and Dr Lowitja O'Donoghue. A decade ago Dr O'Donoghue's Oration was entitled 'Indigenous Health - hopes for a new century'. It is my hope that the following presentation on Indigenous health and the Close the Gap Campaign will demonstrate that her expression of hope was justified.
There is no doubt that the situation of Indigenous health has improved in the past 10 years. Indigenous health equality is now firmly on the agenda with the establishment of a Federal Minister for Indigenous Health, and the National Indigenous Health Equality Council, thanks to the activities of the Close the Gap Campaign and many Aboriginal and Torres Strait Islander health activists, such as Dr O'Donoghue. She and those like her have, since the late 1960s, worked unceasingly for Indigenous people and it could be said that the Close the Gap Campaign stands on their shoulders.
It is vital to acknowledge this, and the fact that the earliest heroes of the Aboriginal cause have been calling for improvements to Indigenous health since the 1920s. This history and their legacy must never be forgotten. We cannot afford to be complacent for there is still much to be done. Because of this, my own Oration entitled 'What's needed to Close the Gap?' must inevitably focus on current deficits. However my goal is to paint, as Dr O'Donoghue did 10 years ago, a picture of hope rather than despair.
If the name of the Close the Gap Campaign is unfamiliar it is because, like an iceberg, much of the Campaign's activity is beneath the public face. Due to the nature of our work, most lobbying efforts and representation at meetings are necessarily in Canberra or eastern-states focused. And because our efforts involve close work with government, confusion often arises because the Australian Government and the Council of Australian Governments' (COAG) Indigenous initiatives are branded 'Closing the Gap'1. There is a fine distinction here ('Close' vs 'Closing'), and although this is in part testament to the success of the Campaign, from the outset I must distinguish the Close the Gap Campaign's approach from the Australian governments' 'Closing the Gap' efforts. This is more than just a point of definition, for in that fine space of difference lies the answer to my question: 'What is needed to Close the Gap?'
However, first let us establish the human rights foundation of the Campaign. The Close the Gap Campaign's goal is to close the health and life expectancy gap between Aboriginal and Torres Strait Islander and non-Indigenous Australians within a generation. This in itself is an answer to the question, because it contains the following features:
- The adoption by Australian governments of a comprehensive national plan of action focusing on a wide range of health conditions and health determinants, that is properly resourced and has the goal of achieving health equality by 2030.
- The national plan will be developed and implemented in partnership with Aboriginal and Torres Strait Islander peoples and their representatives.
- The plan will define ambitious yet realistic benchmarks and targets.
- The plan will not only include an expansion of the role of Aboriginal Community Controlled Health Services for the delivery of primary health care to Indigenous Australians, but also increase the access of Indigenous Australians to mainstream health services.
That is what is needed to close the gap. However, to understand the rationale for the Campaign, a closer look at the gap itself is needed.
The persistent gap
'The gap' of course refers to the difference in life expectancy and health status between Indigenous and non-Indigenous Australians. The official estimation of the original 17 year life expectancy gap was revised in 2009 to 11.5 years for males and 9.7 years for females2. Either way, the gap is sizeable. The Campaign refers to this as the '10-17 year gap' because other than acknowledging that it exists we cannot say precisely how wide it is, apart from that it is large - at least 10 years large!
Although the gap cannot be quantified precisely, we do know that a series of smaller gaps underlie the life expectancy gap: Indigenous Australians die younger and at faster rates of the same conditions. The Indigenous standardised mortality rates for the five main groups of chronic diseases for the years 2001 to 2005, when compared with that of the non-Indigenous population, show that we're dying at 10 times the rate of other Australians for certain conditions (Fig1)3.
Heart disease is the single biggest killer of Indigenous Australians and this represents a burden of unnecessary suffering. The word 'unnecessary' is the key here, for we are all going to die some day, and sickness touches us all. However our task is to eliminate as much unnecessary sickness and death as is possible, in this case among the Indigenous population. The suffering is clearly unnecessary, as can be seen by comparing mortality and morbidity rates for the Australian Indigenous and non-Indigenous populations. This also applies to the significantly higher rates of communicable diseases among Indigenous peoples (Fig2)4.

Figure 1: Indigenous standardised mortality rates (SMR; as multiples of the rate in the non-Indigenous population): Main causes 2001-20053.

Figure 2: Communicable diseases in Indigenous peoples, reported as multiples of the rates in the non-Indigenous population (2004-2005)4.
In fact, in addition to high rates of chronic and communicable diseases, there are a number of disturbing indicators and trends that reveal an entrenched health crisis in the Indigenous population, notably:
- High rates of poor health among Indigenous infants does not bode well for the future adult population. Despite infant mortality decreasing in the past decade, recent increases in low birth weight babies predicts poor adult health in survivors.
- High rates of unhealthy and risky behaviour, including an increased prevalence of substance abuse and alcohol and tobacco use.
With a significant proportion of Indigenous peoples in younger age groups (the result of a recent Indigenous 'baby boom'), the additional challenge to programs and services is to keep up with the future demands of a burgeoning Indigenous population (Fig3). It is clear that unless substantial steps are taken now, the gap could widen. There is no room for complacency or a blinkered reliance on trends and other data. If the gap is to close, action is required now.
Let us be clear at this point that, as established in the literature, there is no genetic 'wild card' contributing to the poorer health of Indigenous people. We are dying from, and being disabled by, conditions and diseases that in the non-Indigenous population are preventable, curable and otherwise manageable. The health gap is man-made. Not by action but by a failure to act when action is needed. We die younger because we were treated differently in the past, and we are treated differently now (Fig4). Indeed the biggest divide of all that underlies the health gap, is a divide between the opportunities of black and white Australians to be healthy.
This is a most important understanding, particularly for those who blame Indigenous peoples for their own poorer health, for instance for the rates of tobacco smoking. For while it is true that we are all ultimately responsible for the choices we make, it is equally true that for a variety of reasons Indigenous Australians have had fewer health choices than other Australians. The good news is that as the gap is 'man-made', its closing is also within our collective will and power.
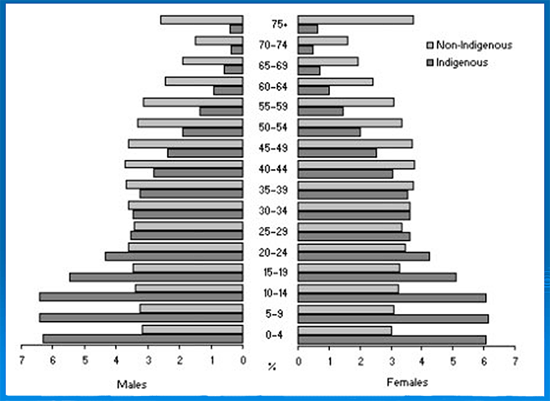
Figure 3: Indigenous and non-Indigenous age structures5.
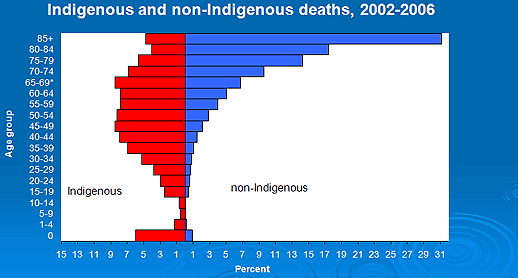
Figure 4: Life-expectancy: most Indigenous deaths occur in the middle adult ages2.
Access to health services - or lack of it
Nowhere is the Indigenous lack of opportunity to be healthy seen more clearly than in relation to access to health services. In the 2004-2005 health survey6, for example, 21% of Indigenous Australians reported they had needed to go to a dentist in the last 12 months but had not gone, and 15% had needed to go to a doctor but had not gone. Reported reasons for not accessing health care included 'lack of availability of services', 'transport and distance to services', 'cost', and 'language and cultural barriers'. A higher proportion of Indigenous people in non-remote areas reported 'cost' as a reason for not seeking health care; while for those in remote areas, 'transport/distance' and 'the service not being available' were more commonly reported.
Another factor impacting on the use of health services is the relatively few Indigenous health professional available to deliver those services. As services such as Dr Noel Hayman's State government community clinic in Inala, Queensland, have demonstrated, an Indigenous face behind the desk or an Indigenous nurse to consult with can make a huge difference in Indigenous peoples' perceptions of health services. However in 2006, Indigenous Australians were under-represented in almost all health-related occupations and comprised only 1% of the health workforce despite being 2.5% of the Australian population2.
Indigenous students continue to be under-represented among those completing courses in the health disciplines. While the situation is improving with initiatives such as the Poche Centres for Indigenous Health at Flinders University, this strategy can partially address workforce demands. Action is still required to secure Indigenous peoples' full participation in the delivery of health services to Indigenous communities, and indeed to all Australians.
A lack of access to primary healthcare services is reflected damningly in other statistics. In 2005-2006, Indigenous males and females were more than twice as likely as other males and females to have been hospitalised, with the greatest differences in hospitalisation rates for people 25 years and over2. Most of this difference was due to high rates of care for renal dialysis and other potentially preventable hospitalisations (ie causes detectable by adequate primary health care). Indigenous Australians were hospitalised for care involving dialysis at 14 times the rate of other Australians, and for potentially preventable hospitalisations at 5 times the rate of other Australians. In other words, missed opportunities to access primary health care results in unnecessary hospitalization.
Not only is hospitalization a personal trauma, it also burdens the community with significant and unnecessary cost. There is, therefore, a compelling cost-benefit argument for achieving Indigenous health equality, if indeed any further argument is necessary. It is worth reflecting on the economic argument here, for the whole thrust of recent reforms has been financially motivated. If people are seen earlier by doctors they can be kept out of expensive hospital beds, which are often associated with expensive travel and dislocation from community and family. To the Indigenous community, it seems that Australian policy-makers have just discovered this in the past 5 years! However, for Indigenous Australians the situation and its required solutions goes far beyond economics. It goes to the heart of how we are treated, and have been treated. In terms of the health system, this means missing out on access to services most Australians take for granted.
The human rights framework and Closing the Gap in Indigenous health
While I've hinted that the answer to the question in our title lies in the difference between the Close the Gap Campaign and the Australian Governments' Closing the Gap efforts, there is a simpler way of expressing this difference. The Close the Gap Campaign is based on the rights of Indigenous Australians, particularly the right to health. Indeed, the Campaign's approach is the first articulated expression of the right to health in a policy setting, internationally. As such, it has received a significant amount of attention and approval internationally, particularly from the UN. And so, in relation to the question 'What is needed to Close the Gap?' I also answer 'A human rights based approach'.
Such an approach is characterised by:
- Planning to achieve equality and equality of opportunity in relation to health in an ambitious but realistic manner.
- The use of targets and benchmarks in the plan.
- Indigenous Australians having the opportunity to participate as partners in planning, including planning for the implementation of the plan, and the delivery of services under that plan.
So how is this approach formulated? Australia is a signatory to the 1966 International Covenant on Economic, Social and Cultural Rights7, one of the primary legal expressions of the UN's fundamental 1948 Universal Declaration on Human Rights. Article 12 of the 1966 Covenant is the primary human rights law expression of the right to health, stating that everyone has the right to 'enjoy the highest standard of physical and mental health'7. This right is ensured by providing opportunities to be healthy: that is, health services and a key range of goods and services that support good health (adequate food, potable water supplies, sanitation etc). However crucially, because non-discrimination is a fundamental element of human rights law, a state is obliged to ensure or provide equal opportunities to be healthy regardless of human differences, such as race and sex. And a state that does not provide equal opportunities to be healthy is legally required to institute a response referred to as 'progressive realisation' - that is, to ensure that equality of opportunity is achieved as soon as possible. The Close the Gap Campaign's approach is an example of progressive realisation in action.
Australia is also a signatory to the UN's 1965 International Convention on the Elimination of All Forms of Racial Discrimination8. The Convention obliges governments to enact 'special measures' in the form of differential treatment aimed at achieving substantive equality or equality 'in fact', or equality outcomes for the disadvantaged race. Special measures can be thought of as a legally required 'catch up'. As with progressive realisation, such a catch up also requires planning, partnership and the use of equality benchmarks and equality targets. The special measures, however, go beyond ensuring equality of opportunity in relation to the enjoyment of human rights into the future (as progressive realisation aims to do). It also aims to address past injustices.
In Australia, the higher rates of chronic disease among Aboriginal and Torres Strait Islander peoples are the result of significant historical neglect and racial discrimination, such as in life on mission and government reserves with poor diet and minimal health services. Or from being paid wages in tobacco, as Aboriginal people were until the 1960s in some cases - imagine if this were the case today! In this situation, specific measures are appropriate to compensate for the chronic disease burden of Australian Indigenous peoples, in order to equalize their rates of chronic disease with that of the non-Indigenous population - in other words, to catch up.
The Close the Gap Campaign could be said to be a two-pronged catch up because it:
- Provides a catch up (or levelling out) in relation to the chronic and communicable diseases that are a legacy of the past.
- Provides equal opportunities to be healthy into the future, so Indigenous Australians enjoy the same opportunities as other Australians to see doctors and to make choices for health, and also enjoy the health benefits of a similar standard of housing and community services.
Other rights inform the Close the Gap approach. Self-determination, the right of Indigenous peoples, has many dimensions. However, within the broader context of the post-colonial nation state it is basically the right to self-governance. Aboriginal Community Controlled Health Services are an expression of Aboriginal and Torres Strait Islander peoples' right to self-determination. They are best placed to ensure culturally appropriate health services are delivered to the communities they serve, which includes the use of traditional healing practices, where appropriate. In the latter they are also an expression of Aboriginal and Torres Strait Islander peoples' cultural rights. The Close the Gap Campaign supports Aboriginal Community Controlled Health Services as the preferred services for health delivery to Indigenous Australians, while also recognising that Aboriginal and Torres Strait Islander people must also have the same opportunity to access 'mainstream' health services that exist for other Australians.
Finally, one of the great wisdoms of human rights is that they are inter-related: one right cannot be denied without impacting on other rights. The associations between education, employment or income, adequate housing and good or bad health, are well documented. And the Close the Gap Campaign advocates that not only social but also cultural determinants must be included in the scope of a plan for health equality, or otherwise addressed in a broader effort to achieve Indigenous health equality. Cultural determinants can be understood as the social determinants of health that are unique to Aboriginal and Torres Strait Islander peoples in both positive terms (the positive health impacts and resilience associated with membership of strong Aboriginal and Torres Strait Islander cultures), and negative terms (what results from racism being directed at a particular group). Thus, for example, the Campaign encompasses efforts towards reconciliation and tackling racism as health measures; it acknowledges the potentially positive health impacts of constitutional change, the strengthening of Native Title, and the preservation of Indigenous languages.
With the finalisation of the United Nations' 2007 Declaration on the Rights of Indigenous Peoples, the human rights framework in an indigenous context has now been significantly articulated9. In Australia this was foreshadowed by my 2005 Social Justice Report10. This is the foundation of the Close the Gap Campaign.
The Close the Gap Campaign
From a hopeful beginning...
The human and corporate foundation of the Close the Gap Campaign is a collective of peak Indigenous and mainstream health bodies, health professional bodies, NGOs and other institutions (Fig5). The Campaign is lead by a Steering Committee that operates by consensus, taking direction from an Indigenous Leadership Group (Fig6). The first meeting of the Campaign Steering Committee was held after the Social Justice Report10 was tabled in the Australian Parliament in March 2006. Following this, in April 2007 the Campaign was launched by patrons, Olympians Catherine Freeman and Ian Thorpe (Fig7).

Figure 5: Close the Gap Campaign Steering Committee membership

Figure 6: Close the Gap Campaign Steering Committee Indigenous leadership.

Figure 7: Close the Gap Campaign patrons, Olympians Catherine Freeman and Ian Thorpe at the Campaign launch in April 2007.
The Campaign has operated through difficult times and under two governments. Campaign partners, both Indigenous and non-Indigenous, have reached a point of trust and commitment to see the process through. There is no funding from government - the membership donates funds for operational costs, and the Australian Human Rights Commission hosts the secretariat. Significant funding support from Oxfam Australia enabled Campaign establishment and the rapid advancement of its objectives.
Beyond official partners, the Campaign has the pledged support of over 140 000 Australians to 'Close the Gap', and this wide community support is evidenced by the 570 community events that marked national Close the Gap Day on 25 March 2010. In August 2009, the National Rugby League became the first sporting code to join the Campaign, dedicating an annual round of matches to Close the Gap.
...To great steps forward
In August 2007, the Federal Opposition under the leadership of Kevin Rudd signalled its support for the Close the Gap approach in its Indigenous affairs election platform. As a result, 'Closing the Gap' entered the policy lexicon. Following the election of the Rudd Labor Government, many aspects of the Close the Gap Campaign became official government policy. Since then, Australian governments through a number of COAG commitments have adopted elements of the Close the Gap approach. In December 2007, COAG adopted a target to 'achieve Aboriginal and Torres Strait Islander life expectancy equality within a generation'1. This was supported by the target to 'halve the mortality rate of under 5 year old Aboriginal and Torres Strait Islander children within 10 years'. By mid-2009, a total of 6 COAG 'Closing The Gap' targets had been announced (Fig8). That was our first great success.

Figure 8: Council of Australian Governments (COAG) Closing the Gap targets1.
Close the Gap National Indigenous Health Equality Summit and its Statement of Intent
The next great step forward was heralded by the Close the Gap National Indigenous Health Equality Summit (the Summit), hosted by the Campaign in March 2008. The Summit culminated in Prime Minister Rudd, the Minister for Health and Ageing, the Minister for Families, Housing, Community Services and Indigenous Affairs, and the Federal Opposition Leader signing the Close the Gap Statement of Intent with Indigenous health leaders, and a key commitment11 follows:
...we commit:
To developing a comprehensive, long-term plan of action, that is targeted to need, evidence-based and capable of addressing the existing inequities in health services, in order to achieve equality of health status and life expectancy between Aboriginal and Torres Strait Islander peoples and non- Indigenous Australians by 2030.
The Statement of Intent is the only formal bi-partisan agreement in Indigenous affairs at the Australian national level. It will soon achieve actual national status as it has since been signed by the governments and oppositions of Western Australia, Queensland, Victoria, the Australian Capital Territory and New South Wales, with a commitment to sign received from the South Australian (SA) Premier.
Since the Summit, 'Close the Gap' branded programs from Australian governments have reached funding of approximately $5 billion, of which $1.6 billion is specifically targeted to closing the gap in life expectancy within a generation, the biggest single injection of funding into Indigenous health in history. However, progress has been slower in other areas because much of the Campaign's subsequent work has been with the Australian government to facilitate implementation of the Statement of Intent commitments amid massive reform to the health system. These reforms, in turn, have occurred in the context of an even larger national reform agenda encompassing seven areas of national interest, one of which is to address Indigenous disadvantage.
Close the Gap Campaign Steering Committee sub-targets
Coinciding with the adoption by COAG of the target to achieve Aboriginal and Torres Strait Islander health equality within a generation, the Close the Gap Steering Committee developed a range of sub-targets. These supported the COAG targets but took them further. The sub-targets were developed by Aboriginal and Torres Strait Islander health experts and stakeholders over 6 months in 2007-2008, and are known as the Close the Gap National Indigenous Health Equality Targets (Close the Gap targets)12. Finalising the targets was the primary purpose of the Summit and they were published and presented to the Federal Health Minister in July 2008.
Further Campaign developments in Indigenous health
In the 2 years since the Summit, great change has taken place in Aboriginal and Torres Strait Islander health, mainstream health and Indigenous affairs. In particular:
- The establishment of the National Health and Hospital Reform Commission in February 2008
- The establishment of the National Indigenous Health Equality Council in March 2008
- The National Indigenous Reform Agreement in November 2008
- The National Integrated Strategy for Closing the Gap in Indigenous Disadvantage (Integrated Strategy) in June 2009
- The seven 'closing the gap' National Partnership Agreements (NPAs) associated with the Integrated Strategy (this partnership is not the type advocated by the Campaign because it is between Australian governments without involving Indigenous people and their representatives) including:
- The NPA on closing the gap in Indigenous health outcomes with a focus on chronic disease, which includes measures to increase Aboriginal and Torres Strait Islander's access to both Aboriginal Community Controlled Health Services and mainstream GPs and primary health care services, and to health checks and social marketing programs.
- The NPA on Indigenous early childhood development which focuses on child and maternal health.
- The NPA on closing the gap in Indigenous health outcomes with a focus on chronic disease, which includes measures to increase Aboriginal and Torres Strait Islander's access to both Aboriginal Community Controlled Health Services and mainstream GPs and primary health care services, and to health checks and social marketing programs.
- The appointment of a Minister for Indigenous Health in June 2009
- The development of the Health and Hospital Network (finalised May 2010) and the broad shift in health system emphasis towards primary and preventative health
- A draft National Preventative Health Strategy in September 2009
- The establishment of 'Medicare Locals' and the National Primary Health Care Strategy in May 2010
- The launch of the National Congress of Australia's First Peoples in April 2010.
The Close the Gap Campaign Steering Committee was actively involved in the majority of the reform processes associated with these developments. I am involved with the $1.6 billion NPA on closing the gap in Indigenous health outcomes, through overseeing a greater than $100 million program aimed at drastically reducing the rates of smoking in the Indigenous population. When deciding what is needed to Close the Gap, significantly reducing smoking is vital. Currently, Indigenous smoking rates are approximately 50% overall and up to 80% in some communities, with tobacco smoking alone responsible for almost 20% of all deaths13. Aboriginal and Torres Strait Islander peoples are nearly three times as likely as the non-Indigenous population to be daily smokers, and smoking is the primary cause of chronic conditions and diseases among Indigenous Australians. Research also indicates an earlier age of uptake of tobacco use among children of Aboriginal and Torres Strait Islander descent than their non-Indigenous counterparts.
If the smoking rate among Indigenous Australians was reduced to the rate of the non-Indigenous population, approximately 420 Aboriginal and Torres Strait Islander lives would be saved each year, equating to an additional 4 years life expectancy. Tackling smoking in the Indigenous population is a major initiative and represents a great opportunity to effect change and achieve far-reaching and lasting outcomes.
With the support of Indigenous Health Minister Warren Snowdon, the Close the Gap Steering Committee convened the 'Close the Gap, Making it Happen' workshop in June 2010 to focus on the development and implementation of a plan for Aboriginal and Torres Strait Islander health equality within a generation. The meeting was significant in foreshadowing a national plan for Indigenous health equality.
In terms of a partnership for health equality, the creation of the National Congress of Australia's First Peoples' in April 2010 heralds a new dawn for Indigenous affairs in Australia. The model for the Congress was developed by an Indigenous steering committee under my leadership after extensive, year-long community consultations. It will be partnered by an Ethics Council. In this and other developments the Australian Government has taken significant steps forward in working with us and giving us a voice on the policies and laws that affect us, including those relating to health planning. However, we are still waiting for the development of a formal partnership.
Philanthropy in Indigenous health
The work of philanthropists involves a second type of partnership. The role of philanthropy in Indigenous health is vital because it can significantly accelerate essential developments, particularly those where government support is limited or too restrictive to enable innovative initiatives.
This type of partnership is exemplified by the work of philanthropists Greg and Kay Poche. The Poche's partnership with Flinders University to advance Indigenous healthcare worker education is consistent with the aims of the Campaign. Such a partnership is also crucial to many of the recent developments in Indigenous health for, as we have established, a strong Indigenous health workforce is needed to Close the Gap.
In a March 2010 initiative, the Poches donated $10 million to Flinders University for the establishment of the Poche Centre for Indigenous Health in Adelaide SA and Alice Springs in the Northern Territory (NT; in collaboration with Charles Darwin University), for which I am National Patron. The principal objectives of this initiative are to:
- increase the number of Indigenous students studying medicine, nursing and other health profession courses
- improve understanding of Indigenous health and wellbeing by all health professionals
- foster health research by Indigenous researchers and health workers
- increase research that leads to improvements in Indigenous health.
Results are already apparent. The Faculty of Health Sciences has drafted a Faculty Commitment on Aboriginal and Torres Strait Islander Health that will include initiatives to build a culturally safe faculty environment. In addition, a significant number of applications have already been received from Indigenous students for 2011 entry into medicine at both Flinders University NT and SA.
There are many other opportunities for Indigenous health initiatives philanthropy, similar to the Poche Centre's Network, including investing in developments such as the Functional Electrical Stimulation (FES) suit led by Mr Graham Calma, in collaboration with faculty of Flinders and Adelaide Universities.
Finally, while the Close the Gap Campaign continues to work behind the scenes with government, it is also willing to criticize government when necessary, as it did this year in its 'Shadow Report to the Prime Minister's Annual Report to Parliament' on efforts to Close the Gap, repeating the call for a inclusive planning processes and a partnership approach to Indigenous health initiatives.
Conclusion
In conclusion, the answer to the question 'What is needed to Close the Gap?' is and can only be, 'A human rights based approach to Indigenous health'. Such an approach includes a bold and ambitious plan and partnership between Indigenous Australians and their representative Australian governments.
The personal dimension of the current crisis should never be forgotten. Indeed it injects a sense of urgency into our efforts. For Indigenous peoples, the health gap is not experienced as a table of statistics but as suffering and pain for those with poorer health, and grief and trauma for those who care for them - their communities. In this way, the damage from health inequality is not just inflicted on individuals.
We have all heard about 'dying' Indigenous languages, of our cultures being 'under stress', and the lack of leadership in some communities. These are not discrete issues but deeply related to health. Poor health and early and unnecessary death wreaks havoc among us, impacting on our emotional and social equilibrium. Poor physical health is one in a constellation of other related factors contributing to our disturbingly higher rates of mental health issues. Health status therefore significantly affects our capacity to be educated as children and young people. It affects our ability to later hold jobs and earn decent wages for the care of our children.
The drive for Indigenous health equality is a matter of great personal concern to Indigenous Australians. It's about our happiness as individuals and families; it's about our children, our parents and our grandparents, our communities, our languages and our cultures.
And for the nation, this state of affairs presents a profound challenge. It asks, 'What does it mean to be an Australian?' and 'What does this country stand for?'. For although we live in one of the wealthiest and healthiest nations on earth, we have tolerated profound inequality among ourselves that continues to this day. It is this persistent inequality that condemns our First Peoples to the life and health status of those living in the developing world.
While I have no doubt that things are improving, we were and still are a society deeply divided - a nation that has not yet faced up to its past, and one still in need of reconciliation. There is work to be done! This involves a national effort to reconcile us, to bring us together in expectation of what it is to live in this great nation: health and happiness, and respect and esteem from each other and the government we create together. In so doing, I believe it is essential to acknowledge the racial discrimination and neglect of the past. If we are to move forward together as one nation, the dark legacy of the past that dwells in today's poorer health of Indigenous Australians has to be acknowledged - and rectified.

Figure 9: Text from Australian Prime Minister Kevin Rudd's acknowledgement of the 'ills of the past' in his Apology to the Stolen Generations, Parliament of Australia, 13 February 2008.
Just as Prime Minister Rudd's acknowledgement of the ills of the past (Fig9) in his 'Apology to the Stolen Generations' is helping to generate a new era in Indigenous affairs, only by acknowledging the past can we move forward together to a future in which black and white Australians truly do stand together as brothers and sisters, enjoying an equally high standard of physical and mental health. This is the challenge ahead of us: to set in motion a planning process and a partnership to support, develop and implement 'What is needed to Close the Gap'.
References
1. COAG. Closing the Gap for Indigenous Australians. (Online) 2008. Available: http://www.coag.gov.au/coag_meeting_outcomes/2008-10-02/index.cfm#gap (Accessed 5 August 2010).
2. Australian Bureau of Statistics. Experimental Life Tables for Aboriginal and Torres Strait Islander Australians, 2005-2007, ABS cat no 3302.0.55.003. (Online) 2009. Available: www.abs.gov.au (Accessed 23 August 2010).
3. Australian Institute of Health and Welfare. Australia's Health 2008: Table 3.4, ABS cat no 8903.0. Canberra, ACT: AIHW, 2008.
4. Australian Institute of Health and Welfare and Australian Bureau of Statistics. The Health and Welfare of Australia's Aboriginal and Torres Strait Islander Peoples 2008: Table 7.34, ABS cat no 4704.0. Canberra, ACT: ABS & AIHW, 2008.
5. Australian Bureau of Statistics. Population Characteristics, Aboriginal and Torres Strait Islander Peoples 2006 (unnumbered graph), ABS cat no 4713.0. Canberra, ACT: ABS, 2008; 15.
6. Australian Institute of Health and Welfare and Australian Bureau of Statistics. The Health and Welfare of Australia's Aboriginal and Torres Strait Islander Peoples 2008, ABS cat no 4704.0. Canberra, ACT: ABS & AIHW, 2008.
7. Office of the United Nations High Commissioner for Human Rights. International Covenant on Economic, Social and Cultural Rights, adopted 16 December 1996. (Online) 1996-2007. Available: http://www2.ohchr.org/english/law/cescr.htm (Accessed 5 August 2010).
8. Office of the United Nations High Commissioner for Human Rights. International Convention on the Elimination of All Forms of Racial Discrimination, adopted 21 December 1965. (Online) 1996-2007. Available: http://www2.ohchr.org/english/law/cerd.htm (Accessed 5 August 2010).
9. United Nations. Declaration on the Rights of Indigenous Peoples. (Online) 2007. Available: http://www.un.org/esa/socdev/unpfii/en/drip.html (Accessed 5 August 2010).
10. Calma T. Social Justice Report. (Online) 2007. Available: http://www.hreoc.gov.au/social_justice/sj_report/sjreport07/index.html (Accessed 5 August 2010).
11. Australian Human Rights Commission. Close the Gap: Indigenous Health Equality Summit Statement of Intent. (Online) 2008. Available: http://www.hreoc.gov.au/social_justice/health/statement_intent.html (Accessed 5 August 2010).
12. Human Rights and Equal Opportunity Commission. Close the Gap National Indigenous Health Equality Targets. (Online) 2008. Available: http://www.hreoc.gov.au/social_justice/health/targets/health_targets.pdf (Accessed 5 August 2010).
13. Vos T, Barker B, Stanley L, Lopez A. Burden of disease and injury in Aboriginal and Torres Strait Islander peoples: summary report. Brisbane, QLD: Centre for Burden of Disease and Cost-Effectiveness, School of Population Health, University of Queensland, 2007.
