It has been well established in the literature that the typical practice of a physician in rural and northern areas is not the same as those in urban regions1-4. Canadian studies produced to date have focused on physician migration2,5,6, distributions1,2,6, workloads5 and the provision of specific services in family practice4,5. However, there is a tendency in the Canadian literature to conflate rural and northern issues and although much of northern Ontario is rural, this is not exclusively the case. Although there are many definitions of what constitutes northern Ontario, it can be generally stated that northern Ontario constitutes over 90% of the land mass of Ontario with an area of more than 800 000 km2 and less than 7% of the population (Fig1)7. The rural areas of southern Ontario are primarily agricultural communities which stand in contrast to the often resource extraction economy-based rural northern communities where the principal industries are mining, forestry and hydroelectricity. While there have been several recent descriptive reports that have examined physician services in rural and northern Ontario1,2,4,5, none to date have done so with the explicit purpose of examining differences in physician populations between rural and urban regions of the northern and southern areas of the province.
Physician recruitment to rural and northern regions are a priority for the Ministry of Health and Long-term Care in Ontario8, which offers many programs designed to improve physician recruitment and retention in these underserviced communities9. In addition, a new medical school, the first in over 30 years, was established in Northern Ontario and began accepting students in 200510. The Northern Ontario School of Medicine (NOSM) is a joint initiative of Laurentian University in Sudbury and Lakehead University in Thunder Bay. One of the key rationales for establishing NOSM stems from evidence indicating that students from rural backgrounds who are trained in rural areas tend to practice in those areas11-13. Furthermore, recent comprehensive reviews of both grey and published literature outline numerous factors that affect physician recruitment and retention strategy and incentive effectiveness14-16. These reviews clearly identify that although financial and professional/organizational issues are important for retention, family/personal factors (eg housing, spouse/partner employment, child care, schools, lifestyle)17 and location/community factors (eg community infrastructure such as sports or cultural facilities, local transportation, climate, community isolation) are also important factors that influence retention. For example, Humphreys and associates have pointed out that longer duration of stay of physicians within a community is positively associated with physicians who are older, attended school locally, and living with family15. As a result, retention strategies which are supportive for 'empty-nest' physicians may not be as effective for those with young families. Having a solid understanding of who is likely to want to live in certain types of communities may be helpful in targeting recruitment and retention efforts in specific regions.
In this study, data from the College of Physicians and Surgeons of Ontario (CPSO) Annual Membership Renewal Survey were utilized to seek a better understanding of the demographic distribution of physicians across rural and urban areas of northern and southern Ontario. The CPSO is the licensing and regulatory body of physicians in Ontario. Its register contains verified demographic, credential and practice location information for all physicians in the province. On an annual basis, all physicians are required to renew their membership with the CPSO and participate in the survey. The survey boasts a 98% response rate providing an almost complete picture of physicians across Ontario. Descriptive statistics from the survey have been published by the CPSO in previous years18 but none have specifically examined rural-urban differences in northern and southern practices. This study aims to provide a more nuanced understanding of the distribution of the physician population across varying degrees of rurality in northern and southern regions so that this information may assist in the development of focused recruitment and retention strategies for communities with different physician demographic compositions.
Data and study population
Encrypted data from the 2007 CPSO Annual Membership Renewal Survey and the CPSO Register were employed. This is a report on the geographic distribution of the 22 688 GPs and specialists certified by the College of Family Physicians of Canada (CFPC) and the Royal College of Physicians and Surgeons of Canada (RCPSC) who responded to the survey and who had their primary practice address in Ontario.
Ethics and funding
Funding for this study was provided by the Laurentian University Research Fund and research ethics approval was granted by the Laurentian University Research Ethics Board.
Urban/rural categorization
The geographic location of the primary practice address was identified using the six-character postal code contained in the CPSO registration database. Primary practice postal codes were linked to Canadian census subdivisions (CSDs), employing Statistics Canada's Postal Code Conversion Files (PCCF). The data were coded for degree of rurality employing Statistics Canada's Metropolitan Area and Census Agglomeration Influenced Zones (MIZ) definitions19.
The MIZ approaches define census metropolitan areas (CMA) (population of at least 100 000) and census agglomerations (CA) (population of at least 10 000) as urban and all other areas as rural. These rural areas are then subdivided on the basis of proportions of rural residents who commute to work in urban centres. Statistics Canada classifies urban/rural locations into one of 5 zones19:
- Urban: Located within a Statistics Canada-defined CMA or CA, 88% of the population of Ontario resides in an urban area.
- Rural-Strong MIZ: ≥30% of the employed labour force living in the CSD works in any CMA/CA areas; 5% of Ontarians live in a rural-strong MIZ area.
- Rural-Moderate MIZ: ≥5%, but ≤30%, of the employed labour force living in the CSD works in any CMA/CA areas; 4% of Ontarians live in a rural-moderate MIZ area.
- Rural-Weak MIZ: >0%, but <5%, of the employed labour force living in the CSD works in any CMA/CA areas; 2% of Ontarians live in a rural-weak MIZ area.
- Rural-no MIZ: includes all CSDs that have a small employed labour force (<40 people), or any CSD that has no commuters to a CMA/CA areas; only 0.3% of Ontarians live in a rural-no MIZ area.
There is no universally accepted definition of 'rural' in Canada but, at present, many (rural) health researchers use the MIZ definitions, providing a standard method for defining and sub-dividing rural and the units can be linked to socio-demographic census information and many other Statistics Canada databases when needed. Since there were fewer than 15 physicians who had primary practice addresses in no MIZ areas, this category was combined with the weak MIZ category for analysis to avoid small cell disclosure.
Northern categorization
Similarly, there is no universally accepted boundary dividing northern and southern parts of the province. The Forward Sortation Area (FSA) of the Canadian postal codes were used to define the north. Based on this distinction, FSAs beginning with a 'P' are considered northern while all remaining FSAs (which begin with a K, L, M or N) represent southern Ontario. Geographically speaking, this divide stretches from the base of Georgian Bay (roughly 45o of latitude) and runs at a 45o angle toward the Quebec border (Fig1).
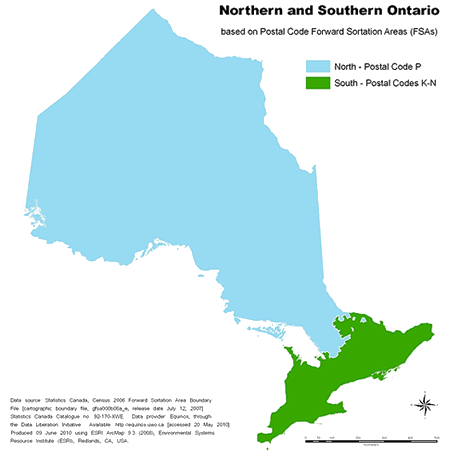
Figure 1: Map of Ontario divided into north and south regions, based on postal code geography.
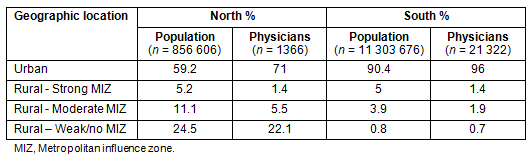
In accordance with this definition, 93% of Ontario's population resides in the south and 7% resides in the north20. The distribution of the population of Ontario that resides in northern and southern locations by MIZ category is outlined (Table 1).
Table 1: Geographic distribution of Ontario's population (2007) and Ontario physicians
Analysis
The data set represents the population of all physicians with primary practices in Ontario making the use of inferential statistics unnecessary. Data were used to examine the distribution of physician numbers, age, sex, international medical graduates (IMGs), and certification for physicians with primary practice addresses in the north versus the south across each of the MIZ categories.
Geographic distribution
Of the 22 688 Ontario based physicians, 1366 (6%) practiced primarily in northern regions. Of those northern physicians, 71.0% practiced in urban areas, 1.4% practiced in strong MIZ zones, 5.5% practiced in moderate MIZ and 22.1% practiced in weak/no MIZ areas. The vast majority of physicians (94%) had their primary practice located in southern Ontario. Over 96% of southern physicians practiced in urban areas, 1.4% practiced in strong MIZ areas, 1.9% practiced in moderate MIZ zones, and 0.7% practiced in weak MIZ areas (Table 1).
Certification
For the total physician population, certification is distributed as follows: 28.1% CFPC certified, 51.7% RCPSC certified and 20.2% were 'general practitioners' with no certification.
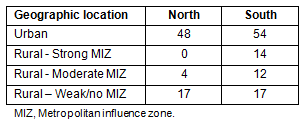
Differences were evident in the distribution physician certification in northern and southern practice locations. In the north, GPs and CFPC-certified FPs accounted for 62.2% of the physician population, compared to 47.5% in the south. It is clear from examining the MIZ categories that RCPSC-certified specialists were heavily concentrated in urban areas (Table 2). In the north, 48% of physicians in urban areas were RCPSC certified specialists, whereas 0%, 4% and 17% of the physicians practicing in strong MIZ, moderate MIZ and weak/no MIZ zones, respectively, were RCPSC certified specialists. A similar pattern was found in southern regions where 54% of the physicians in urban areas, 14% in strong MIZ zones, 12% in moderate MIZ areas and 17% found in weak/no MIZ locations were RCPSC certified specialists.
Table 2: Percent of Ontario physicians with Royal College of Physicians and Surgeons of Canada certification by location
Age
The mean ages of northern and southern physicians were 50.4 and 51.2 years, respectively. However, the age differences per MIZ category provide distinct age patterns across both northern and southern and rural and urban areas (Fig2). In northern locations, physicians tended to be younger in rural locations. The mean ages of northern physicians were: 51 years in the urban north, 41.3 years for north strong MIZ, 50 years for north moderate MIZ, and 49.1 years for north weak/no MIZ. For southern physicians, mean age steadily increased with increasing rurality. In the south, urban physicians had a mean age of 51.2 years, strong MIZ physicians were 51.9 years, moderate MIZ were 52.5 years and weak/no MIZ physicians were 52.3 years. The age distribution (histograms) of the physicians in each MIZ category were examined and no abnormalities found because each category was normally distributed.
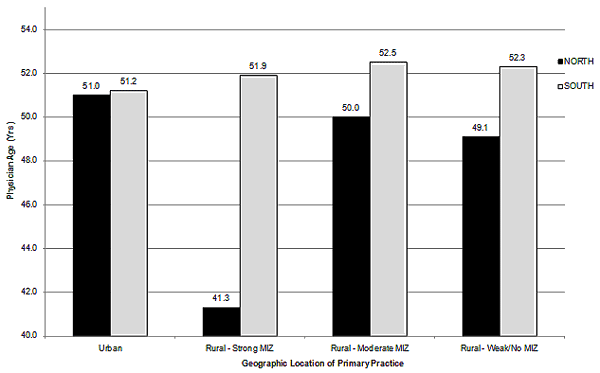
Figure 2: Mean age of physicians in Ontario 2007 by location
Sex
For the entire physician population in Ontario, 32.1% of the physicians were female. The proportion of female physicians was higher in southern locations than in northern locations. In the south, 32.5% of the physicians were female, whereas only 25.5% of northern physicians were female. Only in the most rural areas (ie weak/no MIZ) was there a higher proportion of female physicians in the north (27.8%), compared with the same rural category in the south (24.0%). A closer look at the MIZ categories indicated that in southern locations, the proportion of female physicians declined with increasing rurality, with 33.8%, 29.9% and 24.0% in strong, moderate and weak/no MIZ locations, respectively. In contrast, rural northern regions had higher proportions of female physicians compared to the urban north, with 31.6%, 26.7% and 27.8% in strong, moderate and weak/no MIZ, respectively, versus 24.6% females in urban north (Fig3).
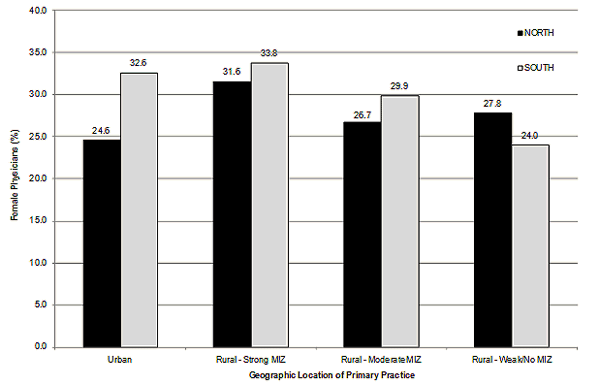
Figure 3: Percent of female physicians in Ontario 2007 by location
International medical graduates
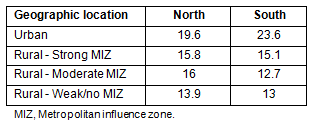
The proportion of international medical graduates (IMGs) among all Ontario physicians was 22.9%. The IMGs comprised 23.2% of all southern physicians and 18.1% of all northern physicians. A greater proportion of urban southern physicians were IMGs (23.6%) compared with physicians in northern urban centres (19.6%). Patterns of the distribution of IMGs were similar in southern and northern regions in that the proportion of IMGs decreased with increasing rurality; however, northern areas had slightly greater proportions of IMGs in moderate MIZ (16.0%) and weak/no MIZ (13.9%) areas than the corresponding MIZ areas in the south (12.7% and 13.0%, respectively) (Table 3).
Table 3: Percent of Ontario physicians in 2007 who were international medical graduates by location
Discussion
Mirroring the provincial population distribution, the present data showed a much greater proportion of physicians located in Ontario's southern regions and urban communities. The picture differs somewhat in Ontario's north. Although the number of physicians practicing in northern communities (6%) was proportionate to the population (7%), their distribution between urban and rural locations was disproportionate, with 71% of northern physicians in urban area where only 59% of the northern population resided. In rural locations, 1.4% of northern physicians practiced in strong MIZ areas, 5.5% in moderate MIZ area and 22.1% in weak/no MIZ area, where these physicians care for 5.2%, 11.1% and 24.5% of the northern population, respectively. This degree of discrepancy is not seen in the south. This finding suggests that the north may not be underserved due to the absolute physician-to-population ratio, but rather due to an imbalance in its distribution of physicians. Thus, recruitment and retention strategies in the north should focus more heavily on northern rural areas.
Additional regional differences were revealed in the Ontario physician population with regard to age, sex, certification and IMG status by further differentiating the rural-urban comparison from a northern versus southern perspective. There were more younger and male physicians in northern and rural areas. It appears that the trend of older physicians choosing to practice in a rural setting is occurring more often in the agricultural rural south than in the less populated, resource intensive, northern rural communities. Likewise, female physicians were more frequently found in the south with decreasing proportions of females with increasing degrees of rurality. In the northern areas of the province, although overall the proportion of female physicians were lower than in the south, there was a slight increase in the proportion of female physicians as rurality increased. Physicians certified by the RCPSC where distributed in clusters in the northern part of the province, with larger proportions located in urban areas as well as in the most rural areas; a distribution which corresponds with the location of hospitals in the north. The largest proportions of IMGs were found in urban areas and the proportions of IMGs decreased with increasing rurality. However, northern rural regions did tend to have a higher proportion of IMG physicians than in corresponding rural areas in the south.
One of the strengths of this study is that it examined the entire Ontario physician population and the physician workforce in Ontario is the largest in the country21,22. However, it is acknowledged that this current report is limited in that the focus is entirely on demographic information. There is a need to also look at other professional and community data that are essential in order to enhance retention and recruitment15. Future work should include rural-urban, northern-southern comparisons of hours worked per week, patient volume, clinical activities and open practice (ie accepting new patients into practice). In addition, the data from the CPSO survey only provide us with a cross-sectional view. They do not indicate how long those physicians have been in their current practice settings, nor do they provide information on what influenced their decisions to locate in one area or another. Future studies should focus on providing a longitudinal analysis of migration patterns coupled with data regarding the rationale behind physicians' decisions for relocation. Finally, the CPSO data conveniently lends itself to a Forward Sortation Area definition of north and south. However, this definition is slightly different from that used by Ontario's Local Health Integration Networks (Ontario's regional health authorities), which place the north-south divide slightly further north. With this in mind, the present findings cover a slightly larger area of northern Ontario, which includes the Muskoka area, Ontario's tourism hot spot, which is commonly considered a southern location. The present analysis could be repeated using alternative geographic definitions that are perhaps more applicable to the organizations or communities intending to use the information to inform policy and program development.
The results indicate that although there are similarities in the distribution of physician demographics in rural and urban areas, there are clear differences between the rural north and the rural south. Likewise, although there are some patterns that distinguish the south from the north, these areas are not homogeneous regions where the urban north is clearly different from the rural north. In considering the implications of these distinctions for the development of physician recruitment and retention initiatives and policies, the importance of accounting for these geographical differences becomes clearer. For example, in relation to the sex distribution of younger physicians, new graduates and undergraduates in medical school, it is clear that future cohorts of physicians entering the workforce will consist of increasingly larger proportions of females23. In general, northern rural areas have attracted more younger male physicians with females and older males found in higher proportions in southern urban and rural areas. If the predominantly female new graduates are to be encouraged to establish their practices in northern and rural regions, it is necessary to be sure that the recruitment and retention initiatives are geared specifically to attract and support this population.
Likewise, attracting IMGs to northern and rural regions may require some equally creative recruitment and retention initiatives which address their specific concerns and issues which may differ from those of non-IMG medical graduates. This may be of particular relevance given that Ontario has recently changed its incentive policy aimed at attracting IMGs to underserviced rural and northern regions. In past years, IMGs under the Postgraduate Return of Service Program were required to initially work in rural or northern communities24,25. In March 2010, that initial practice location restriction was eased, allowing return-of-service commitments to be completed in any Ontario community except Toronto and Ottawa - the two largest cities in the province25. International Medical Graduates are still eligible for other provincial initiatives that have been established to specifically attract physicians to rural and northern areas (eg the Northern and Rural Recruitment and Retention Initiative)26. However, given that IMGs are more likely to locate in southern and urban centres, it will be important to monitor if the change in the Postgraduate Return of Service Program results in a decline in the numbers of IMGs completing their return of service contracts in rural or northern regions.
Since no one single recruitment or retention strategy is likely to appeal to all physicians, multifaceted incentive programs, which recognize that different groups of physicians have different needs, are likely to be more successful than a 'one-size-fits-all approach' in attracting a broader spectrum of physicians to underserviced northern and rural regions.
Acknowledgements
The authors thank the College of Physicians and Surgeons of Ontario for providing access to the data used for this study. The CPSO was not involved in the design, conduct of the study, management, analysis or interpretation of the data, or the preparation, review or approval of the manuscript.
References
1. Tepper J, Schultz SE, Rothwell DM, Chan BT. Physician services in rural and northern Ontario. Toronto: Institute for Clinical Evaluative Sciences, 2005.
2. Pitblado, JR. Distribution and internal migration of Canada's physician workforce. Ottawa: Canadian Institute for Health Information, 2007.
3. Coyte PC, Catz M, Stricker M. Distribution of physicians in Ontario. Where are there too few or too many family physicians and general practitioners? Canadian Family Physician. 1997; 43: 677-683, 733.
4. Canadian Institute for Health Information. What do we know about family physicians who accept new patients? (Online) 2010. Available: http://secure.cihi.ca/cihiweb/products/aib_what_do_we_know_en.pdf (Accessed 13 July 2010).
5. Chan BT, Schultz SE. Supply and utilization of general practitioner and family physician services in Ontario. Toronto: Institute for Clinical Evaluative Sciences, 2005.
6. Chan BT, Schultz SE. Supply of physicians' services in Ontario. Toronto: Institute for Clinical Evaluative Sciences, 1999.
7. Ontario Tourism Marketing Partnership. Northern Ontario. (Online) 2010. Available: http://in.ontariotravel.net/regions/northern.aspx (Accessed 19 July 2010).
8. Ontario Ministry of Health and Long-term Care. Improving access to health care: McGuinty government helps recruit more doctors. (Online) 2010. Available: http://www.news.ontario.ca/mohltc/en/2010/03/improving-access-to-health-care.html (Accessed 19 March 2010).
9. Pong RW. Strategies to overcome physician shortages in northern Ontario: a study of policy implementation over 35 years. Human Resources for Health. (Online) 2008. Available: http://www.human-resources-health.com/content/6/1/24 (Accessed 8 December 2010).
10. Tesson G, Hudson G, Strasser R, Hunt D. The making of the Northern Ontario School of medicine: a case study in the history of medical education. Montreal, ON: McGill-Queen's University Press, 2009.
11. Heng D, Pong RW, Chan BTB, Degani N, Crichton T, Goertzen J et al. Graduates of northern Ontario family medicine residency programs practise where they train. Canadian Journal of Rural Medicine 2007; 12(3): 146-152.
12. Rourke JT, Incitti F, Rourke LL, Kennard M. Relationship between practice location of Ontario family physicians and their rural background or amount of rural medical education experience. Canadian Journal of Rural Medicine 2005; 10(4): 231-240.
13. Rabinowitz HK, Diamond JJ, Markham FW, Rabinowitz C. Long-term retention of graduates from a program to increase the supply of rural family physicians. Academic Medicine 2005; 80(8): 728-732.
14. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural Remote Health 9(2): 1060. (Online) 2009. Available: http://www.rrh.org.au/journal/region/5/North_America (Accessed 19 March 2010).
15. Humphreys J, Wakerman J, Pashen D, Buykx P. Retention strategies and incentives for health workers in rural and remote area: what works? Canberra, ACT: Australian Primary Health Care Resarch Institute, 2009.
16. Daniels ZM, VanLeit BJ, Skipper BJ, Sanders ML, Rhyn RL. Factors in recruiting and retaining health professionals for rural practice. Journal of Rural Health 2007; 23(1): 62.
17. Pong Rw, Chan BTB, Crichton T, Goertzen J, McCready W, Rourke J. Big cities and bright lights: rural- and northern-trained physicians in urban practice. Canadian Journal of Rural Medicine 2007; 12(3): 153-160.
18. College of Physicians and Surgeons of Ontario. 2006 Physician resources in Ontario: small triumphs, big challenges. College of Physicians and Surgeons of Ontario, 2007.
19. DesMeules M, Pong R, Lagace C, Heng D, Manuel D, Pitblado R et al. How healthy are rural Canadians? An assessment of their health status and health determinants. (Online) 2006. Ottawa, ON: Canadian Institute for Health Information. Available: http://www.phac-aspc.gc.ca/publicat/rural06/pdf/rural_canadians_2006_report_e.pdf (Accessed 16 September 2009).
20. Statistics Canada. Population and dwelling counts, for Canada and census subdivisions (municipalities). (Online) 2006. Available: http://www12.statcan.gc.ca/census-recensement/2006/dp-pd/hlt/97-550/Index.cfm?TPL=P1C&Page=RETR&LANG=Eng&T=301&S=3&O=D (Accessed 19 July 2010).
21. Tamblyn R, Abrahamowicz M, Dauphinee D, Wenghofer E, Jacques A, Klass D et al. Physician scores on a national clinical skills examination as predictors of complaints to medical regulatory authorities. JAMA 2007; 298(9): 993-1001.
22. Canadian Institute for Health Information. Health Indicators. Ottawa: CIHI, 2007.
23. College of Physicians and Surgeons of Ontario. Reaping the rewards - striving for sustainability: 2007 registration statistics and survey findings. (Online) 2007. Available: http://www.cpso.on.ca/uploadedfiles/policies/positions/resourceinitiative/Reaping%20the%20Rewards%20Survey_07.pdf?terms=2007+annual+survey (Accessed 9 July 2008).
24. Ontario Ministry of Health and Long-Term Care, Health Human Resources Policy Branch. Guidelines for return of services (ROS) for international medical graduates (IMGs), Repatriation Program and Registration Through Practice Assessment. (Online) 2007. Available: http://www.health.gov.on.ca/english/providers/ministry/recruit/repat/docs/ros_guidelines.pdf (Accessed 19 July 2010).
25. Ontario Ministry of Health and Long-Term Care. HealthForceOntario Postgraduate Return of Service Program. (Online) 2010. Available: http://www.health.gov.on.ca/english/providers/program/uap/uap_hfo_ros.html (Accessed 9 July 2010).
26. Ontario Ministry of Health and Long-term Care. HealthForceOntario Northern and Rural Recruitment and Retention Initiative (NRRR). (Online) 2010. Available: http://www.health.gov.on.ca/english/providers/program/uap/uap_hfo_nrrr.html (Accessed 9 July 2010).


