Faecal incontinence (FI), the involuntary loss of liquid or solid stool with or without the patient's awareness, may cause embarrassment, loss of self-respect, psychiatric disorders, and withdrawal from the community1. Little systematic research of this socially disabling condition has been conducted to determine either the true burden on individuals and communities or the results of treatment in northern Australia.
Community prevalence of FI has been reported to range between 8% and 11% in South Australia and New South Wales2-4. Faecal incontinence is a leading reason for nursing home placement in Australia where up to 72% of residents have the condition5. In studies conducted at the Colorectal and Urogynaecology outpatient clinics of the Townsville Hospital (TTH) in North Queensland more than one in five patients reported FI1,6.
Biofeedback is a safe, conservative first-line treatment for FI7. The Townsville Hospital, a publicly funded regional hospital with an extensive rural catchment area, operates a nurse-run holistic biofeedback program for patients with FI, constipation or pelvic pain8,9.
A Cochrane review of biofeedback for the treatment of FI found no evidence that any method of biofeedback or pelvic floor exercises provided better outcomes than any other conservative treatment method10. Standard care including diary and symptom questionnaire, structured assessment, patient teaching, emotional support, lifestyle modifications, management of FI and urgency control was a method that provided equivalent results11. When telephone assisted support for remote patients was compared with face-to-face biofeedback protocol for regional patients, no significant outcome differences were found12.
This clinical study was designed to assess two exercise regimens, the efficacy of biofeedback program components for FI (L Bartlett, K Sloots; unpubl. data, 2005-2006) and whether treatment outcomes (ie FI severity or quality of life [QOL]) differed between rural and regional participants.
Participants
Clinic patients were eligible to participate in the study if their FI had persisted for at least 6 months and had failed to respond to standard treatment recommended by their GP. Further eligibility criteria included being at least 18 years of age and not pregnant; and having no terminal illness, mental illness or gastrointestinal stoma. Participants were referred by a colorectal surgeon following anorectal physiologic assessment including manometry and endoanal ultrasound. They attended the biofeedback program between January 2005 and October 2006 and signed informed consent forms.
Ethics
Ethics approval was granted by Townsville Health Service District Human Research Ethics Committee (47/04) and James Cook University (H1950). The Australian New Zealand Clinical Trials Registry number is ACTRN12610000258055.
Study procedure
Faecal incontinence patients on the TTH biofeedback waitlist were initially telephoned, had the study explained to them and were invited to participate. An information pack about the study and biofeedback treatment with appointment dates and a bowel chart were mailed to them. Treatment included 5 outpatient sessions: 4 at weekly intervals, 4 weeks home practice of techniques learnt, then an assessment session. Detail of the study procedure is provided (Fig1).
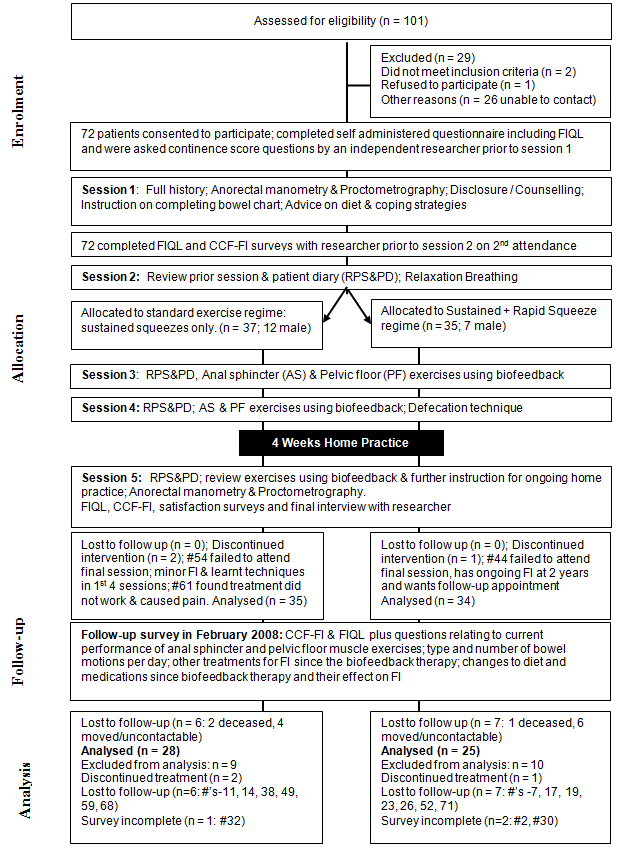
Figure 1: Participants' progress through the study
Participants met with the researcher immediately prior to the initial biofeedback session and completed a self administered FI questionnaire1, including the 29 question Fecal Incontinence Quality of Life Scale (FIQL) survey tool13. The researcher completed the Cleveland Clinic Florida Fecal Incontinence Score (CCF-FI)14 with them. Session one with the biofeedback therapist included documenting: relevant medical, surgical, obstetric and medication history; and bowel problems and habits. Diet, fibre, and fluid intake were discussed together with the aim of therapy and the establishment of treatment goals and instructions given to record food, fluid, supplement intake and medications used in the patient diary. Anorectal function and proctometrographic evaluation were assessed using clinic manometric equipment15,16. The therapist presented coping strategies and dietary advice8. The pre-treatment bowel chart was reviewed and comprehensive instructions were given to accurately record daily bowel accidents and toileted motions using the Bristol Stool Form Scale17. Immediately before session two, participants repeated the FIQL and CCF-FI with the researcher. The biofeedback therapist then reviewed the previous week's diary and bowel chart with the patient noting the impact of any dietary or coping modifications used, before instructing each patient in slow relaxation (diaphragmatic) breathing. Patients had the rectal probe and the balloon inserted, prior to inflating the balloon to sensory threshold. Lying in the supine position with one hand lightly resting on the upper abdomen to monitor diaphragmatic movement and rate of breathing, each participant practiced relaxation breathing for 5-10 min. Visual biofeedback was provided from the clinic computer monitor with verbal feedback from the therapist to improve the technique9. Patients were instructed to practise relaxation breathing at home at least twice per day and complete the bowel chart for the following week.
Before session three the biofeedback therapist was advised the exercise regimen to which the patient had been randomised; that is: standard exercises (sustained pelvic floor and anal squeeze exercises) or alternative exercises (rapid and sustained pelvic floor and anal squeeze exercises)18.
In session three the previous sessions' therapy components were reviewed and amended. Anal sphincter and pelvic floor muscle exercises were taught according to the relevant exercise regimen. Participants were coached to link the changes in pressures seen on the computer monitor with the exercises performed and sensations felt. The aims of the exercises and techniques were to reduce urgency and frequency, and to improve sensitivity, anorectal co-ordination and continence. Patients were asked to perform their individual prescribed exercises at home (Fig2).
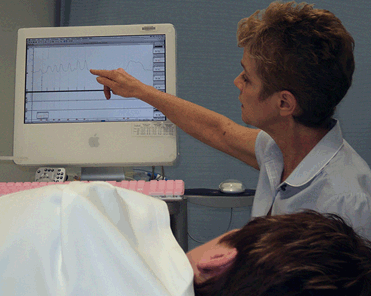
Figure 2: Rapid and sustained anal sphincter squeeze instruction.
A review of all components of previous treatment sessions (bowel charts, exercises, monitoring of dietary, medication, and fluid or supplement changes) was conducted by the biofeedback therapist in session four. The number and strength of prescribed exercises was increased as appropriate for the individual. A defecation technique, using a combination of the toileting position, relaxation breathing and evacuation technique was taught to assist with stool fragmentation and incomplete evacuation. Participants were then given written and verbal instructions on all components for their 4 week home practice.
At the fifth session, patients' home practice and bowel charts were reviewed with the biofeedback therapist; anorectal function was reassessed, and suggestions made for future improvements. Patients who felt they needed further support were able to book a follow-up appointment. At the completion of the fifth session the researcher reassessed severity of symptoms, the effect of FI on QOL and satisfaction with treatment outcomes; and also conducted a short semi structured interview to elicit participants' opinions about: the reasons for the delay in seeking treatment for FI; advice they would give fellow FI sufferers; suggestions they could provide to improve FI disclosure; and usefulness of a home biofeedback device.
In February 2008 all participants were mailed a follow-up survey.
Statistical analysis
Data were analysed on an intention-to-treat basis and patients who failed to complete the program were treated as missing. Numerical data are given as mean value and standard deviation (SD) or median value and interquartile range (IQR), depending on the distribution. Comparisons between characteristics were undertaken using χ² tests and χ² tests for trend, non-parametric Wilcoxon tests, and t-tests. Statistical analyses were conducted using SPSS for Windows v17 (SPSS Inc; Chicago, IL, USA; www.spss.com). Throughout the analyses p<0.05 was considered statistically significant.
Participants
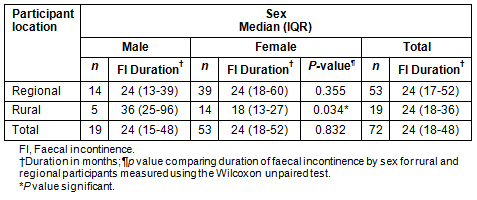
Of 101 consecutive patients with FI referred for biofeedback, 72 participants (19 male), mean age 62.1 years (95%CI 38.3-85.9), were both eligible and consented to participate. Twenty participants (6 male) had previously undergone bowel surgery, 12 for colorectal cancer (5 male). The surgery performed on these participants was: anterior resection, 11 (9 for low rectal carcinoma, 1 for diverticulitis, 1 for prolapse); segmental colectomy, 5 (carcinoma 1; diverticulitis 2; ischaemia of colon 1; rectal prolapse 1); and total proctocolectomy with ileal J-pouch anastomosis, 4 (carcinoma 2; diverticulitis 1; constipation 1). Eight participants (4 male) reported difficulty with rectal emptying. Of the 53 female patients, 38 (72%) had external anal sphincter defects; 13 had been surgically repaired prior to biofeedback referral, 26 had difficult vaginal deliveries requiring forceps or vacuum extraction, 5 women had vaginal repair surgery only and 10 women had both vaginal repair surgery and difficult vaginal deliveries. Fifty-three participants (14 male) lived within 30 min drive of the clinic (median 7.8 km, IQR: 5.7-12.0) while 19 (5 male) travelled up to 903 km (median 339 km, IQR: 136-388) from rural locations (p<0.001) to attend the clinic. Female participants were younger than male participants, and significantly so for regional residents (p=0.044, Table 1). Overall, participants had suffered from FI for a median duration of 24 months (IQR 18-48) with rural women reporting FI for a significantly shorter period before seeking treatment than their regional counterparts (p=0.034, Table 2). There were no adverse events as a result of treatment.
Table 1: Participants' ages according to sex and location
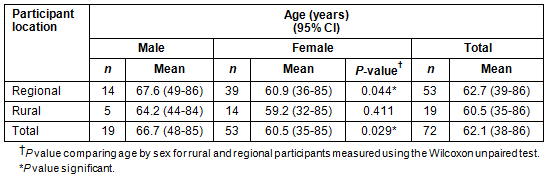
Table 2: Participants' duration of faecal incontinence according to sex and location
Baseline data
Pre-existing medical conditions and prior surgical history known to be risk factors for FI were similar for rural and regional participants. Rural participants reported poorer general health than regional participants (p=0.004) and lower QOL with regard to lifestyle (p=0.028, Table 3). Rural participants also presented with more severe FI than regional participants (CCF-FI, Table 3), significantly so for males (p=0.044).
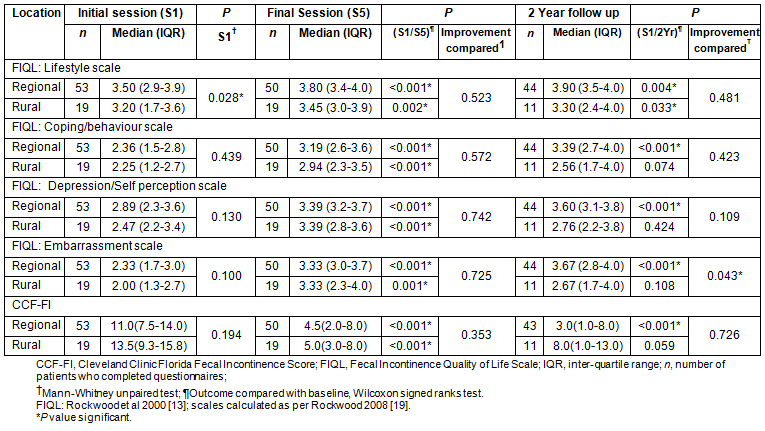
Table 3: Quality of life and faecal incontinence severity over study period, according to location13,19
Participants who failed to complete treatment
Sixty-nine participants completed all 5 treatment sessions (median duration 8 weeks). Three patients (all regional) failed to attend the final session: one with minimal FI (CCF-FI=1 and FIQL=4 for each scale) advised he had acquired sufficient skills in the first 4 sessions and did not need to continue; a second suffered post-surgery bowel dysfunction (following treatment for diverticulitis) and found the exercises exacerbated the pain and was not prepared to continue; the third did not provide a reason, but at the 2 year follow up requested further sessions with the biofeedback therapist.
Results at completion of treatment
Between the initial and final treatment sessions there were significant reductions in incontinent episodes (median of 4[1-11.5] to 1[0-2.3] per week, p<0.001) and stool frequency (median of 13[8-28] to 12[8-20] bowel motions per week, p=0.007) as recorded in participants' bowel charts. The CCF-FI reduced significantly (11.5 to 5.0, p<0.001) with 86% (59/69) of participants reporting improved continence. The FIQL subscales improved significantly (Lifestyle, 3.4 to 3.8; Coping, 2.3 to 3.1; Depression, 2.8 to 3.4; Embarrassment, 2.2 to 3.3; all p<0.001). There was also a significant improvement in the patients' subjective measures of their bowel control over the period of treatment, from a median of 3.0/10 (1.8-4) to a median of 7.5/10 (6.3-8.6), p<0.001, (0=worst, 10=best). Objective anorectal manometry and proctometrographic measures, undertaken at baseline and at the final biofeedback session were significantly improved for maximum squeeze pressure (median: 59.2-67.3 mmHg, p<0.001) and volume of initial sensation (median: 28-20 mL, p=0.027); marginally different for mean resting pressures (median: 34.6-32.0, p=ns [not significant]); and reduced for volume at first urge (median: 73.5-60 mL, p=ns) and maximum tolerable volume (150-125 mL, p=0.023). There were no significant differences in any objective measure between rural and regional participants (Table 4). Participants were very satisfied with the treatment program, with their median rating being 9 (7.5-10) out of a maximum of 10. They also rated individual components of the program from very to extremely helpful (Fig3).
Table 4: Anorectal physiology pre- and post-treatment, according to location
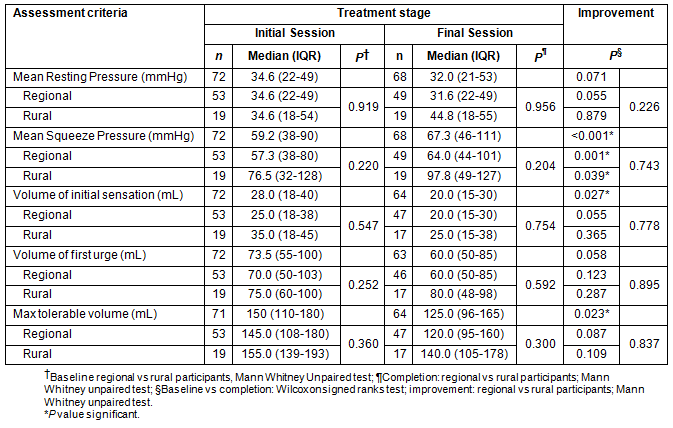
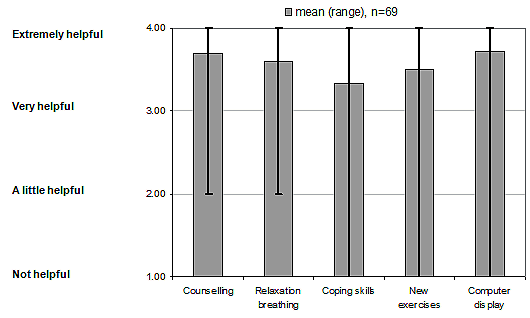
Figure 3: Participant rating of treatment components.
While improvement in rural participants' FIQL and CCF-FI scores over the course of treatment had been marginally better than that of regional participants, there were no significant differences in subjective or objective treatment outcomes between regional or rural participants at the final treatment session.
Final interview
At the session five interviews at least a quarter of participants (33% rural, 25% regional) reported they had sought help for their bowel leakage as soon as it occurred, while more than a third (45% rural, 40% regional) had sought help within 12 months. However, more than a quarter of participants (22% rural, 35% regional) did not seek help for more than a year. The reasons patients gave for the delay in obtaining treatment included: believing the problem would go away (26 patients, 6 rural); being too embarrassed to seek help (11 patients, 2 rural); being given poor advice by a GP, for example that nothing could be done, or that it was a normal problem after a 10lb baby (11 patients, 3 rural); just coping with the problem (13 patients, 2 rural); thinking FI was a normal part of aging (6 patients, 2 rural); believing they were the only one with the problem and not knowing it was treatable (5 patients, 2 rural); and experiencing previous unsuccessful treatments such as medication, anal stretching or fistula operations (11 patients, 5 rural).
More than 83% of the participants (15 rural, 45 regional) sought initial help from their GP, 4% (2 rural, 1 regional) from hospital doctors and 7% (2 rural, 3 regional) from their colorectal surgeon. Over 91% were directly referred to the colorectal surgeon; the remainder had colonoscopy or other investigations before referral to the colorectal surgeon.
All participants attending the final session reported that they would advise a friend in a similar situation not to wait, but seek help immediately, with 53% specifically citing the biofeedback program, 14% their GP and 2% their specialist.
When asked for recommendations to facilitate patient disclosure of FI to doctors, suggestions included: asking patients directly about FI (54%: 14/19 rural; 22/48 regional, p=0.039); listening to patients (39%: 10/19 rural; 16/48 regional); exhibiting empathy (24%: 8/19 rural; 8/48 regional, p=0.028); providing advice about FI risk factors (24%, 6/19 rural; 11/48 regional); recommending biofeedback (18%: 2/19 rural; 11/48 regional); surveying patients (7%); shortening biofeedback waitlists (6%); providing private FI treatment facilities (6%); GP referral to specialist (4%); and more education about available treatment for FI for GPs and hospital doctors (12%: 4/19 rural; 4/48 regional). Patients were asked 'Would a confidential survey, completed in the waiting room that you handed straight to the GP aid discussion of this or other potentially embarrassing problems?' 86% of those asked (15/17 rural; 29/34 regional) said it was a good idea; 5 patients (1 rural) said they would not use it because they had good communication with their GP; one person thought a general consultation was too short to deal with an additional issue, but it could prompt a future discussion; while another would prefer to fill it in at home for use at a subsequent consultation.
More than 78% of participants had never seen information about FI in the community; those who had seen such information cited their pharmacy, community nurse, speakers at an older women's network, or the internet.
Over 97% of patients reported that the biofeedback program was very/extremely helpful. Five patients mentioned they were confident doing their exercises in the clinic with biofeedback, but were concerned that they were not doing them correctly at home. Of the 49 who were asked if they would be interested in trialling a home biofeedback device (with an anal sensor), 44 said they would because it would 'be motivating'; 'be good to see an improvement'; or confirm they were doing the exercises correctly. Other qualitative feedback supported the satisfaction scores.
Two year follow up
Fifty-nine participants (12 rural) responded to the February 2008 survey. Thirteen participants were lost to follow up; three were deceased (1 rural) and ten (6 rural) could not be contacted. For regional participants FIQL and CCF-FI scores continued to improve (Table 3), although these results were not significantly different from their final treatment session, with 44% (19/43) reporting no faecal leakage. In contrast rural participants' FIQL scores had declined over time, and with the exception of the FIQL lifestyle scale (p=0.033) they were not significantly better than the pre-treatment scores (Table 3). For responding rural women, improvement in FI severity was maintained at the 2 year follow up; however, the three rural men who answered FI severity questions had reverted to pre-treatment levels. Only 18% (2/11) of rural respondents reported no faecal leakage. Of the 33 patients (9 rural) who reported still having some faecal leakage 14 (2 rural) reported mostly staining, 14 (6 rural) reported moderate faecal losses and 1 (regional) reported loss of a large amount of stool. There were no significant differences in results during the treatment program between the rural patients who responded to the 2 year questionnaire and those who did not.
Since completion of the biofeedback therapy, five survey respondents had sought additional help for their FI. New treatments included silicone anal implants (1 rural, 1 regional), stoma (2 rural) and additional medication (1 rural). Eleven participants (1 rural) requested further biofeedback sessions.
There were no significant differences between rural and regional participants in the number of exercises they performed or their confidence in performing these exercises, although rural participants performed their exercises more frequently. Additionally, stool type for rural participants was looser (p=0.033), they reduced food intake before going out (p=0.005), avoided travelling (p=0.045) particularly by aeroplane or train (p=0.002), and had more faecal urgency (p=0.048) and avoided visiting friends marginally more often (p=0.033). When asked directly, they reported feeling more depressed (p=0.048), felt less healthy (p=0.015), enjoyed life less (p=0.031), were more afraid to have sex (p=0.031), and were more likely to avoid going out to eat (p=0.001).
Discussion
The major findings of this study were that the biofeedback treatment program significantly improved continence and QOL for both regional and rural participants. While FI severity and QOL had continued to improve in regional participants 2 years later, for rural participants FI severity and QOL had regressed to pre-treatment levels.
Many people enjoy living in rural locations due to higher general wellbeing, personal safety and community connection20. Rural participants reported poorer general health than regional participants prior to treatment, which has been previously described in rural populations21. Poorer rural health has been linked to lower levels of education, employment and income, occupational risks, higher levels of hypertension, high cholesterol, asthma, diabetes and risky behaviour such as smoking and alcohol abuse, reduced access to health services, and driving long distances21,22.
Rural female participants sought help earlier than regional women despite their FI severity scores not being significantly different. This is possibly due to the greater inconvenience to their lifestyle which involves more planning and the need to travel further, with less access to toilets. In comparison with regional participants, rural participants avoided travelling, going out to eat, visiting friends, were more afraid to have sex, were more depressed and enjoyed life less, all of which could explain their reduced sense of wellbeing.
While significant improvement of FI severity and QOL in both rural and regional participants was achieved during treatment, the QOL of rural participants failed to be maintained over time. As there was no difference in exercise maintenance at the 2 year follow up, poorer rural QOL could be due to other reasons, such as a change in diet, reduced social interaction or lower tolerance of the impact of FI on QOL. Rural diet tends to be very different from urban diet, including more meat, biscuits and cakes23. Thus the dietary changes rural individuals needed to make may have been more difficult to maintain over the long term in their rural setting. Further research is required to investigate this issue.
Men and women who reside in rural northern Queensland may be required to perform heavy physical work (eg farmers and cane growers). Heavy lifting has been shown to put stress on pelvic floor muscles24 which may in turn contribute to FI25. Additionally, in the long term, regular heavy physical work or the long working hours of primary producers may reduce the likelihood of performing prescribed exercises at the end of a tiring day, compared with people in more sedentary professions who can perform them at any time26.
Disclosure of taboo subjects can be seen as socially risky, and people are less likely to disclose embarrassing information, particularly to close friends, relatives or respected associates such as GPs27, especially if they believe the consequences will be negative6,28. By not admitting an urgent need to access toilet facilities to prevent bowel leakage, rural participants' social or informal support networks may fail22. To maintain post-treatment QOL improvements, rural participants may require referral to a counsellor at the end of biofeedback treatment, or longer term biofeedback clinic support by way of a home biofeedback device, a telephone helpline, newsletter, or webpage.
Participants reported that disclosure of FI to their doctor was embarrassing and many delayed seeking help. Most thought that an 'embarrassing topic survey tool' available in their GP's surgery may have assisted them to disclose their FI earlier, or the GP to ask patients with risk factors whether they had FI, directly and with empathy. They felt this would enable disclosure and facilitate treatment, while maintaining the professional doctor-patient relationship. An embarrassing topic survey tool is currently being assessed.
The short treatment program (5 x 1.5 hour sessions over 8 weeks), which is comparable with other biofeedback programs7,29, may not be sufficiently supportive for rural patients in the long term. A similar program in Sydney, Australia with 5 monthly sessions, used telephone assisted support between initial and final face-to-face sessions for rural/remote patients and found no difference in results between that method and full clinic attendance for regional participants12. The treatment duration of that study was twice the length of this study, even though the number of sessions was equivalent. Advantages of the longer treatment duration may include greater time for patients to practise techniques learnt, greater opportunity to present problems to the therapist and for the therapist to customise treatment. However this may be at the cost of building a strong therapist-client relationship, patient focus and motivation in the short term.
For rural participants to maintain similar long-term improvement in continence and QOL to regional participants, an additional follow-up session with the biofeedback therapist and ongoing local support by continence advisors should be investigated for these patients. A telephone helpline, newsletter, or webpage may also be beneficial.
Acknowledgements
This study was supported by a Program Grant from James Cook University. Lynne Bartlett was supported by the George Roberts scholarship from the Cancer Council, Queensland.
References
1. Ho YH, Muller R, Veitch C, Rane A, Durrheim D. Faecal incontinence: an unrecognised epidemic in rural North Queensland? Results of a hospital-based outpatient study. Australian Journal of Rural Health 2005; 13(1): 28-34.
2. Kalantar JS, Howell S, Talley NJ. Prevalence of faecal incontinence and associated risk factors; an underdiagnosed problem in the Australian community? Medical Journal of Australia 2002; 176(2): 54-57.
3. Lam TCF, Kennedy ML, Chen FC, Lubowski D, Talley NJ. Prevalence of faecal incontinence: obstetric and constipation risk factors: a population based study. Colorectal Disease 1999; 1: 197-203.
4. Hawthorne G. Measuring Incontinence in Australia 2006. Canberra: Commonwealth of Australia; 2006.
5. Australian Institute of Health and Welfare. Australian incontinence data analysis and development. AIHW cat no DIS44. Sydney, NSW: AIHW, 2006; 119.
6. Bartlett L, Nowak M, Ho YH. Reasons for non-disclosure of faecal incontinence: a comparison between two survey methods. Techniques in Coloproctology 2007; 11(3): 251-257.
7. Norton C, Kamm MA. Anal sphincter biofeedback and pelvic floor exercises for faecal incontinence in adults--a systematic review. Alimentary Pharmacology & Therapeutics 2001; 15(8): 1147-1154.
8. Sloots K, Bartlett L. Practical strategies for treating postsurgical bowel dysfunction. Journal of Wound, Ostomy, and Continence Nursing 2009; 36(5): 522-527.
9. Sloots K, Bartlett L, Ho YH. Treatment of postsurgery bowel dysfunction: biofeedback therapy. Journal of Wound, Ostomy, and Continence Nursing 2009; 36(6): 651-658.
10. Norton C, Cody JD, Hosker G. Biofeedback and/or sphincter exercises for the treatment of faecal incontinence in adults. Cochrane Database of Systematic Reviews 2006; 3: CD002111.
11. Norton C, Chelvanayagam S, Wilson-Barnett J, Redfern S, Kamm MA. Randomized controlled trial of biofeedback for fecal incontinence. Gastroenterology 2003; 125(5): 1320-1329.
12. Byrne CM, Solomon MJ, Rex J, Young JM, Heggie D, Merlino C. Telephone vs. face-to-face biofeedback for fecal incontinence: comparison of two techniques in 239 patients. Diseases of the Colon and Rectum 2005; 48(12): 2281-2288.
13. Rockwood TH, Church JM, Fleshman JW, Kane RL, Mavrantonis C, Thorson AG, et al. Fecal Incontinence Quality of Life Scale: quality of life instrument for patients with fecal incontinence. Diseases of the Colon and Rectum 2000; 43(1): 9-16.
14. Jorge JM, Wexner SD. Etiology and management of fecal incontinence. Diseases of the Colon and Rectum 1993; 36(1): 77-97.
15. Tuteja AK, Rao SS. Review article: Recent trends in diagnosis and treatment of faecal incontinence. Alimentary Pharmacology & Therapeutics 2004; 19(8): 829-840.
16. Bharucha AE. Update of tests of colon and rectal structure and function. Journal of Clinical Gastroenterology 2006; 40(2): 96-103.
17. Heaton K, Thompson W. Diagnosis. In: K Heaton, W Thompson (Eds). Irritable bowel syndrome. Oxford: Health Press, 1999; 27.
18. Bartlett L, Sloots K, Nowak M, Ho Y-H. Biofeedback for faecal incontinence: a randomized control study comparing exercise regimen. Diseases of the Colon and Rectum 2011; (in press).
19. Rockwood T. The author replies. Diseases of the Colon and Rectum 2008; 51(9): 1434.
20. Cummins R, Davern M, Okerstrom E, Lo S, Eckersley R. Australian Unity Wellbeing Index: special report on city and country living. Report 12.1. Geelong, VIC: Deakin University, 2005.
21. Australian Institute of Health and Welfare. Australia's health 2010. Australia's Health series no. 12. Cat. no. AUS 122. Canberra, ACT: AIHW, 2010.
22. Davis S, Bartlett H. Healthy ageing in rural Australia: issues and challenges. Australasian Journal on Ageing 2008; 27(2): 56-60.
23. Dobson A, Mishra G, Brown W, Reynolds R. Food habits of young and middle-aged women living outside the capital cities of Australia. Australian and New Zealand Journal of Public Health 1997; 21(7): 711-715.
24. Jorgensen S, Hein HO, Gyntelberg F. Heavy lifting at work and risk of genital prolapse and herniated lumbar disc in assistant nurses. Occupational Medicine 1994; 44(1): 47-49.
25. Norton C, Chelvanayagam S. Causes of faecal incontinence. In: C Norton, S Chelvanayagam (Eds). Bowel Continence Nursing. Beaconsfield: Beaconsfield Publishers 2004; 23-32.
26. O'Kane GM, Craig P, Black D, Sutherland D. Riverina men's study: a preliminary exploration of the diet, alcohol use and physical activity behaviours and attitudes of rural men in two Australian New South Wales electorates. Rural and Remote Health 8: 851. (Online) 2008. Available: http://rrh.org.au (Accessed 11 February 2011).
27. Bartlett L, Nowak M, Ho YH. Impact of fecal incontinence on quality of life. World Journal of Gastroenterology 2009; 15(26): 3276-3282.
28. White T. Consumer Disclosure and Disclosure Avoidance: A Motivational Framework. Journal of Consumer Psychology 2004; 14: 1441-1451.
29. Heymen S, Jones KR, Ringel Y, Scarlett Y, Whitehead WE. Biofeedback treatment of fecal incontinence: a critical review. Diseases of the Colon and Rectum 2001; 44(5): 728-736.


