The high infant and child morbidity and mortality in most sub-Saharan African countries, and Nigeria in particular, is a prominent global concern often associated with inadequate health services and dysfunctional primary healthcare systems. Annually, approximately 10 million of the world's children aged 5 years and younger die from largely preventable disease1. In Nigeria, despite efforts to reduce the under-five mortality rate (U5MR) over the last decade, recent estimates are very high when compared with most other developing countries. For example, in 1999 Nigerian U5MRs were estimated as 178 per 1000 children, rising to 201/1000 in 2003 before declining to 138/1000 in 20072; however, (circa 2007) U5MRs from other countries were much lower. For example, the U5MR/1000 in Ghana was 80, in Kenya 73, Liberia 109, Namibia 69 and in Rwanda 1033.
The family is the basic social unit in Nigeria, consisting largely of patrilineal extended households where the male is the head of the household, leaving women with less autonomy in health issues. These differences are more pronounced in northern than southern Nigeria4-7. In northern Nigeria, women are predominantly engaged in agricultural work and petty trading, and are less likely to be engaged in professional, technical and managerial jobs than women in southern Nigeria. These discrepancies (ie the dominance of agricultural work among women) are more pronounced in rural areas due to the huge differences between the south and the north, an artifact of geoclimatical zones. For example, the southern and middle agroclimatic zones are endowed with more infrastructure and social services than the northern zones, partly due to a more active private sector. In addition, the southern zone has had a longer exposure to economic development and modern international links because of its geographical position7. This disparity is reflected in a number of health outcomes. For example, results from the 2008 Nigeria Demographic and Health Survey (DHS) showed that child mortality rates (deaths per 1000 children) ranged from a low of 32 in the south-west zone to 139 in the north-west zone. Total fertility rates were also generally higher among rural (6.3 children) compared with urban (4.7 children) women8.
Often rural women, particularly those from northern Nigeria, are subordinate to men as a result of sociocultural beliefs that women are 'inferior' to men. Despite efforts to ensure that women globally attain higher status in society and the family, women continue to experience challenges associated with low educational attainment and the inability to control resources4,5. Prior studies have demonstrated that women's status influences the health and mortality of their children9,10, generally concluding that the health of women and their children is largely determined by culturally and socially determined roles and expectations.
Many studies11-13 have used female headship of households as a proxy for access to resources, focusing on critical socioeconomic status outcomes such as poverty and income, with the key assumption that female-headed households (FHH) are poorer than male-headed households (MHH). Few studies have focused on household headship and reproductive health outcomes, which are critical markers of progress towards achieving Millennium Development Goals (MDGs) 4 and 5 that concern reductions in child and maternal mortality. The household status of rural Nigerian women, and rural northern Nigeria women in particular, need further investigation, particularly in areas related to reproductive health outcomes - an indicator of health service utilization. The south-north comparison is critical as the deadline of the MDGs approaches (the year 2015).
Against this background, this study examines the prevalence of and factors associated with child death among rural Nigerian women. Specifically, this article investigates the potential impact of the sex of the household head on child mortality. The article is also an attempt to further document the differences between Nigerian women in the north and the south, areas that are significantly different in terms of economic indicators and sociocultural beliefs. Using recent data, the study aims to provide evidence-based information for maternal and child health program planners and other policy-makers. Such information may assist in clarifying factors that attenuate the effects of interventions aimed at improving maternal and child health outcomes in Nigeria.
Data
Publicly available data from the 2008 Nigeria DHS (via MEASURE DHS; www.measuredhs.com) were used in this analysis. The MEASURE DHS program has collected, analyzed and disseminated representative data on population, health, HIV, and nutrition from more than 200 surveys in over 75 countries throughout Africa, Asia, the Near East, Latin America, and the Caribbean. It is funded by the United States Agency for International Development and includes contributions from other donors and participating countries. Demographic and health surveys typically have sample sizes of up to 33 000 households and provide data for a wide range of monitoring and impact evaluation indicators in the areas of population, health, and nutrition.
The core questionnaire for DHS emphasizes basic indicators and flexibility. It allows for the addition of special modules so that questionnaires can be tailored to meet host-country and donor-data needs. The standard DHS consists of a household questionnaire and a women's questionnaire, with a nationally representative sample of women aged 15-49 years interviewed. The household schedule collects a list of household members' information: age, sex, relationship to the head of the household, education, and parental survivorship and residence. In addition, household characteristics information collected includes the source of drinking water, toilet facilities, cooking fuel used, assets and the use of bed nets. Information is also collected on household members' nutritional status and anemia, with more recent DHS collecting data on HIV testing. Detailed information on reproductive health is also collected.
The sample design for the 2008 Nigeria DHS has been extensively discussed elsewhere8. In brief, it allowed for the generation of nationally representative data using the 2006 Nigeria Population and Housing Census (provided by the National Population Commission) as the sampling frame. The survey's primary sampling unit, referred to as a 'cluster', was defined on the basis of enumeration areas (EAs) from the 2006 census. The 2008 Nigeria DHS sample was selected using a stratified two-state cluster design consisting of 888 clusters (286 urban and 602 rural).
A representative sample of 36 800 households was selected, with a minimum target of 950 completed interviews per state for each of the 36 states and the Federal Capital Territory (FCT), Abuja. In each state, households were distributed proportionately among urban and the rural areas. In the second stage of selection, an average of 41 households was selected in each cluster by equal probability systematic sampling. All women aged 15-49 years who were either permanent residents of the households in the 2008 Nigeria DHS sample or visitors present in the households on the night before the survey were eligible to be interviewed. In a sub-sample of half of the households, all men aged 15-59 years who were either permanent residents of the households in the survey sample or visitors present in the households on the night before the survey were eligible to be interviewed. In addition, a sub-sample of one eligible woman in each household was randomly selected to be asked additional questions about domestic violence.
A total of 33 385 women from 34 070 households were finally interviewed in the 2008 Nigeria DHS. Approximately 69% of the households (n=23 346) were from a rural area. Approximately 69% of the total women interviewed (n=22 896) were from a rural area. The analysis was limited to the sample of 13 203 rural women (73% of a total of 18 028) who gave birth within the past 5 years. The 5 years prior to the survey corresponded to the reference period for the prevalence of children's death in the analysis.
Variables
The dependent variable in the analysis was the proportion of women who reported that their children aged 5 years or younger died in the 5 years prior to the survey. This was simply measured by all women whose children had died being represented by '1', and women whose children did not die as '0'.
The key independent variable was household headship: MHH and FHH was a proxy for leadership in decision-making on issues that affected the health of women, children and other household members. In the survey, the household head was defined as a person who was recognized as such by members of the household, including the respondent. The questionnaire asked for the relationship between each member of the household and the head (anyone who made decisions or the main breadwinner in the household). The FHH were defined as those where the female (with or without a male partner) was recognized by household members as head, likewise with the male head for MHH.
Twelve additional variables were considered in the analysis: individual age at the time of the survey; age at first marriage; parity; schooling; region of residence; occupation; wealth status (based on information on household assets); whether the woman received antenatal care (ANC) from a skilled provider for most recent pregnancy; ever use of family planning (FP); place of delivery for most recent birth; possession of vaccination card for most recent birth; and age of living children.
For age at the time of the survey, women were allocated to one of three age groups: 15-24, 25-34, and 35-49 years. Age at first marriage was categorized less than 16 years or 16 years or older. Parity was measured by the number of children ever born according to one of 4 categories: 1, 2-3, 4-5 and 6 or more. Schooling was defined according to educational level: none, primary, and those with secondary and higher education. Region of residence was based on Nigeria's 6 geopolitical zones (or group of states): north central, north east, north west, south east, south west and south south. For example, the north-west zone consists of Jigawa, Kaduna, Kano, Katsina, Kebbi, Sokoto and Zamfara States; whereas the south-south zone consists of Akwa Ibom, Bayelsa, Cross River, Delta, Edo and Rivers States. The FCT, Abuja, is located in the north-central zone. Apart from the already mentioned variations between northern and the southern regions, these zonal groupings are largely for administrative and political representation purposes (eg power sharing). The wealth index serves as a proxy for measuring long-term standard of living. It is based on data from the household's ownership of consumer goods, dwelling characteristics, type of drinking water source, toilet facilities and other characteristics related to a household's socio-economic status. To construct the index, the DHS used each of these assets and assigned a weight (factor score) generated through principal component analysis, and the resulting asset scores were standardized in relation to a standard normal distribution with a mean of '0' and standard deviation of '1'14. Antenatal care with skilled provider was defined as women reporting receiving ANC from a doctor, nurse/midwife or auxiliary midwife during most recent pregnancy ('1'), and those who did not receive ANC from skilled provider ('0'). Ever-use of FP (modern or traditional methods) was dichotomous (never-used/ever-used); whereas 'place of delivery for most recent birth' was categorized as women who gave birth at home (respondent's own home or 'other' home) or in a health facility. Women were also grouped according to possession of vaccination card for the child most recently born (yes/no). Age (in years) of living children was entered as a continuous variable (0, 1, 2 etc).
Data analysis
Two approaches were used in the analysis, using STATA v10 (www.stata.com). First, univariate models were used to examine for links between independent variables and the rural mothers' experience of child death. A χ² test determined associations between categorical variables and differences were deemed significant at p<0.05. Second, logistic regression was used to examine the impact of household headship on the experience of a child death, before and after controlling for other factors; 3 models were estimated in order to assess if this effect was robust after controlling for other variables. Associations between dependent and independent variables were estimated by odds ratio (OR) and 95% confidence interval (CI). Parity was found to be highly correlated with the age of a woman and was eliminated from the regression models. Variables that were significant based on a χ² test were eliminated from the multivariate regression models because they did not improve the model fit.
Descriptive characteristics of respondents
The distribution of rural women whose most recent birth occurred in the 5 years preceding the survey is presented according to selected background characteristics (Table 1). The majority of women (44%) were in the age group 25-34 years, followed by the youngest age group (28%) and the older women (27%; Table 1). The mean age of women was 29 years. More than half of the women (53%) were first married at 16 years or older and the remainder when they were 16 years or younger. Approximately 30% of women had given birth to 6 children or more and a similar percentage to 2-3 children; 16% and 24% had given birth to 1 child and 4-5 children, respectively. The mean number of children ever born was 4.3.
Table 1: Percentage distribution of rural women whose most recent birth occurred in the 5 years preceding the survey, according to selected characteristics, 2008 Nigeria Demographic and Health Survey8
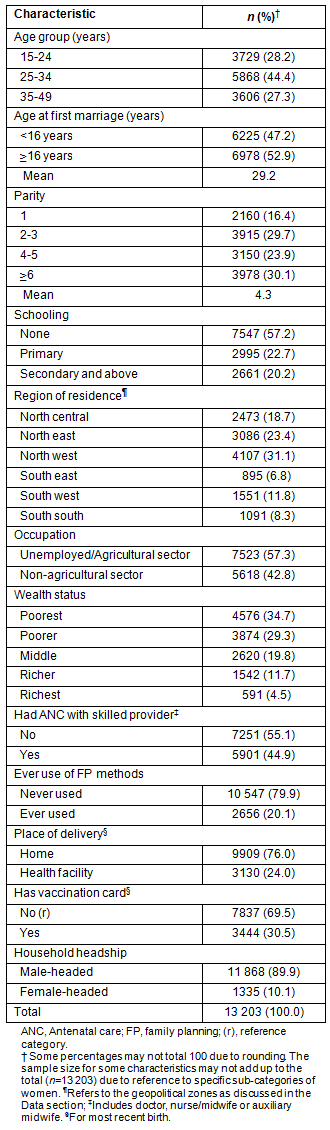
Many women (57%) had never been to school, and those with primary and secondary (and higher) schooling were 23% and 20%, respectively. The distribution of women by region of residence shows that more women were located in the north-west zone (31%) than north-east and north-central zones (23% and 18%, respectively). There were 12% of women in the south-west zone, and 8% and 7% in south-south and the south-east zones, respectively.
When women were classified according to occupation, 57% were unemployed or largely working in the agricultural sector, with the remainder working in the non-agricultural sector (Table 1). The distribution of women by wealth status (based on information on household assets) was 35% poorest, 29% poorer, 20% middle, 12% richer and the richest at 5%. Among all women, 26% were poorest and 14% were richest. Approximately 55% of women had not received ANC from a skilled provider for the most recent birth, and 80% had never used any FP. Home deliveries were more common (76%) than health facility deliveries (24%); and the possession of vaccination card was reported among 31% of women. The most important variable in this study was household headship, with only one in 10 households having a female head.
One of the key objectives of this study was to discover if reporting a child death varies according to selected socio-demographic characteristics. The distribution of women according to experiencing a child death is presented (Table 2), with approximately 43% of women whose most recent birth occurred in the 5 years preceding the survey reporting the death of a child. This percentage reporting varied according to selected background characteristics. For example, a significantly higher percentage of older women (63%) had lost a child, compared with the youngest women (23%). Similarly, more women (52%) who married at an early age (<16 years) had a lost a child, compared with women who married at 16 years or older (35%).
Table 2: Rural mothers (n=13 203) reporting a child death, according to selected characteristics, 2008 Nigeria Demographic and Health Survey8
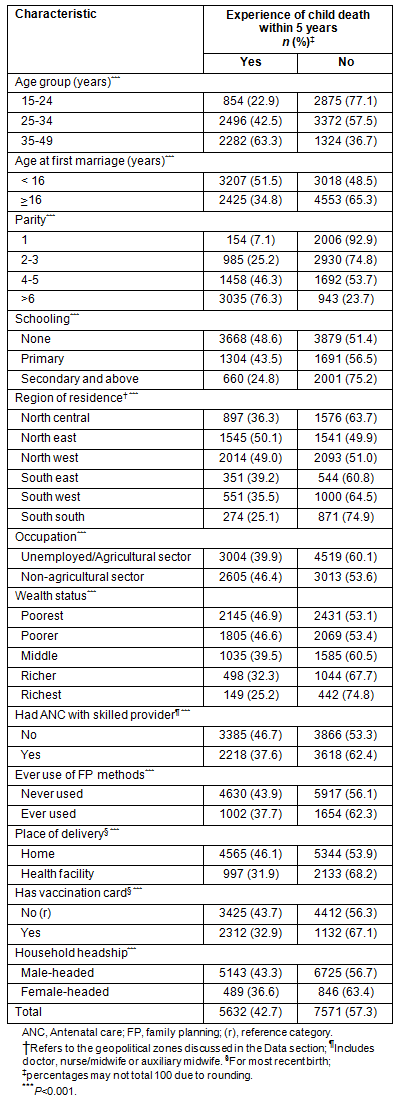
Women who had given birth to at least 6 children reported the highest percentage of child deaths (76%) compared with women of low parity (Table 2). As expected, illiterate women reported the highest percentage of child deaths (49%), compared with those who had some education. Nevertheless, the difference in reporting child deaths between women with primary and secondary schooling was small (49% vs 44%) but increased at the secondary schooling level (25%). Those women living in the north-east and the north-west zones recorded the highest proportion of child deaths (50% and 49%, respectively) compared with women in the southern zone. When women were grouped according to occupation, those employed in the non-agricultural sector had the highest percentage of reporting child deaths (46%), compared with women who were unemployed or employed in the agricultural sector (40%).
With respect to wealth status, women from the richest households had fewer child deaths (25%) than those from poorest households (47%). Generally, movement from lower socioeconomic status to highest was associated with a decline in the percentage of women reporting child deaths. Women who utilized health services recorded lower percentages of reporting child deaths than those who had never utilized some health services. For example, receiving ANC from a skilled provider was associated with a lower percentage of reporting child deaths (38%), compared with women who did not receive ANC from a skilled provider (47%). Approximately 38% of women who had ever used FP methods reported child deaths, compared with 44% who had never used FP. Women who delivered their most recent child at home had the highest percentage (46%) of reporting child death, compared with those who delivered in a health facility (32%). Possession of a vaccination card for the youngest child was associated with a lower prevalence of child deaths (33%), compared with those without vaccination cards. Notably, the percentage of women who resided in MHH had a significantly higher (43%) prevalence of child deaths than those from FHH (37%).
Multivariate results for occurrence of child death
The results of the regression of the effect of household headship are provided (Table 3). The baseline effect of household headship on reporting child death was estimated in Model 1; following this, other variables were controlled for in Models 2 and 3. Table 3 shows that women from FHH were 26% (95% CI 0.65, 0.84) less likely to experience child death than those from MHH. When age group, wealth status and occupation were controlled for in Model 2, the effect of household headship on reporting child death was in the same direction with the odds slightly increased (adjusted odds ratio [AOR] for FHH 0.77 [95% CI 0.68, 0.88]). Women aged 25-34 years were 2.80 times (95% CI 2.54, 3.09) more likely to report child death than those aged 15-24. Older women were associated with odds of reporting child death that were 6.49 times (95% CI 5.82, 7.23) higher, compared with the youngest women. Women who came from middle wealth status households were 32% less likely (AOR 0.68, 95% CI 0.61, 0.76) to report child deaths than those who came from poorer households. Women who came from richer and richest households were 54% (AOR 0.46, 95% CI 0.40, 0.52) and 74% respectively (AOR 0.26, 95% CI 0.21, 0.33) less likely to report child death than those from the poorest households. Compared with the unemployed or those working in the agricultural sector, being a non-agricultural sector worker was associated with odds of 1.33 (95% CI 1.23, 1.44) for reporting child death.
Table 3: Odds ratio (95% CI) for reporting child death among rural women whose most recent birth occurred in the 5 years preceding the survey, 2008 Nigeria Demographic and Health Survey8
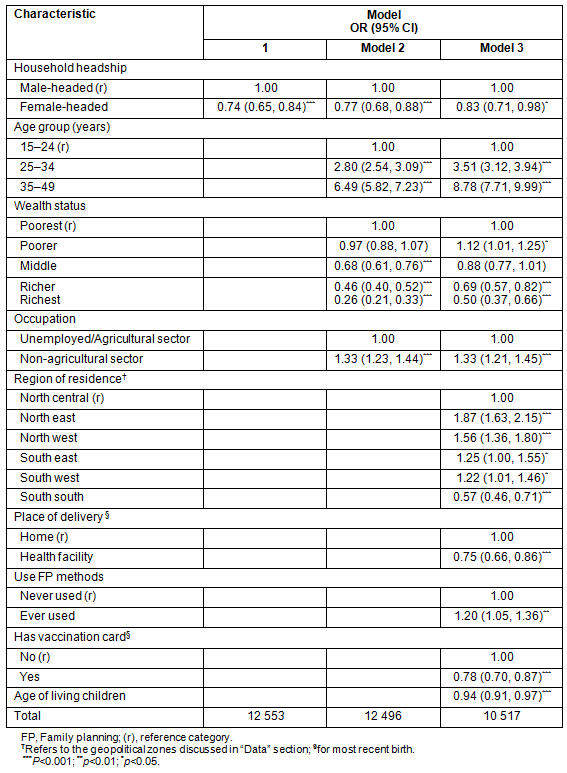
In Model 3, when region, place of delivery, ever use of FP, possession of vaccination cards and age of living children were controlled for, the effect of household headship and other controls was as robust as in Model 2 (Table 3). The odds for FHH were 0.83 (95% CI 0.71, 0.98). Women aged 25-34 years and 35-49 years were associated with higher odds (3.51 and 8.78, respectively) of reporting child death. The odds for wealth status showed that poorer women were 1.12 times more likely (95% CI 1.01, 1.25) to report child death than poorest women. The odds of women from richer households were 0.69 (95% CI 0.57, 0.82) whereas those from the richest households were 0.50 (95% CI 0.37, 0.66), compared with women from the poorest households. However, for women working in non-agricultural sector the odds were reduced: 1.33 (95% CI 1.21, 1.45). With the inclusion of region of residence in the full model, compared with women in the north-central region, women in the north-east region were 87% more likely to report child death (AOR 1.87, 95% CI 1.63, 2.15); whereas women in the north-west zones were 56% more likely to report child death (AOR 1.56, 95% CI 1.36, 1.80). Again, women in the south-east and south-west zones were 25% more likely (AOR 1.25, 95% CI 1.00, 1.55) and 22% more likely (AOR, 1.01, 1.46) to report child death than those in the north-central region. A lower likelihood of reporting child death was only observed among women in the south-south region (AOR 0.57, 95% CI 0.46, 0.71), compared with those in the north-central region. Women delivering at a health facility were 25% less likely (AOR 0.75, 95% CI 0.66, 0.86) to report child death than those delivering at home. Women who ever used FP were 20% more likely (AOR 1.20, 95% CI 1.05, 1.36) to report child death than those who had never used FP. However, women who possessed vaccination cards for their youngest children were 22% less likely (AOR 0.78, 95% CI 0.70, 0.87) to report child death. As the age of living children increased, the odds of reporting a child death reduced by 6% (AOR 0.94, 95% CI 0.91, 0.97). The other variables that were significant in the bivariate relationships did not improve the models and were finally excluded.
Discussion
This study investigated the effect of a number of socio-demographic and other factors related to health service utilization and household headship on reporting child deaths in rural Nigeria. The study found that child deaths are common among rural women, and therefore efforts should be made to strengthen health-service delivery and mobilize communities to utilize those services. At the bivariate level, all variables considered (eg age of the woman, age at first marriage, parity; Table 2), were found to be important in explaining child mortality. However, the effect of some of these variables did not improve the models. In the multivariate analysis, household headship, age of the woman, wealth status, occupation, region of residence, place of delivery, ever use of FP methods, possession of vaccination cards for youngest children, and age of living children were found to be significantly related to child mortality.
Women from FHH were less likely to report the death of a child than were women from MHH, and this could be due to women being able to discuss their maternal and child health needs freely with other women and the female household head. In addition, female household heads may understand maternal and child health problems better than male heads, and encourage other women to seek medical treatment or other advice for their sick children. In fact, 67% of the women from FHH were actually the head of their household. The plausible explanation for the lower prevalence of child deaths among these women is likely to be related to women's autonomy, for these women are expected to be autonomous in their choice and use of health services as well as decision-making related to maternal and child health-seeking behavior. For example, a study in Bangladesh15 based on data from over 188 000 households found that the children of FHH consumed a more diverse diet than those of MHH, consuming micro-nutrient- and protein-rich foods more often. Further, FHH were also more likely to achieve better child and maternal nutritional outcomes than MHH, which was thought to be due to prioritization of expenditures targeted at improved health and nutrition. The effect of women's autonomy on improving child survival has been well established9,10.
The present study also found that child mortality was higher among older than young women. This is consistent with the findings of many studies16-18 that higher educational attainment among younger women results in differences in maternal and child health-seeking behaviour. For example, the 2008 Nigeria DHS data show that young women (15-24 years) were 27.4% more literate than older women (40-49 years). This was a minor improvement from the 32.1% gap reported in the 2003 Nigeria DHS3. The higher experience of child mortality among older women points to the need for renewing efforts in female literacy, as a long term strategy. The fact that poorer women were more likely to report child deaths may be related to differences in health service utilization, particularly where perceived expenses (eg transport costs to health facilities, the purchase of medications) may hinder access and utilization6. However, it is not clear whether offering free health services such as ANC or maternal and child health care would lead to change, because transport costs, the physical inability to travel long distances and poor quality of care (particularly in the northern zone) would remain important barriers19.
The finding that women who worked in the non-agricultural sector were disadvantaged in experiencing child mortality suggests that women in wealthy households who do not need to work can spend more time with their children and therefore take better care of them. These results, however, may also be related to insignificant differences among women's occupation status in rural Nigeria, where the benefits of employment on health outcomes are immaterial because most women struggle to earn sufficient income, and dysfunctional health systems are prevalent. This was highlighted in an early study (1996)7 where it was found that household poverty, particularly in FHH, may be related to legal, regulatory, and cultural barriers that keep women disadvantaged relative to men in terms of access to health, financial resources, education, and agricultural extension services. For those who are employed, other studies have identified the widespread 'feminization' of income where women work longer hours than men to achieve the same standard of living20.
This study also found regional variations in reporting child death. The northern zone was disadvantaged compared with the south-south zone. This pattern has been observed in other studies focusing on reproductive health outcomes. For example, in 2000 in the rural Kano State of northern Nigeria, it was found that 12% of sampled women reported receiving ANC21. Similar results on low uptake of ANC services and FP were documented in this study. For those in the northern zone, this was associated with high illiteracy, and the socio-cultural beliefs and practices of women (eg requiring the husband's permission to use health services and purdah restrictions) that impede women's access to reproductive health services4,5. Due to high illiteracy levels, the counselling and educational materials used in communicating health messages must be audiovisual, interactive, and pictorial in order to reach uneducated women who are most at risk and therefore need to learn to identify and address maternal and child health problems. It is also important to recognize the strong cultural forces that lead women to seek advice from others in the community, and this suggests a need to strengthen sources of advice within the community. For example, the community mobilization of women's groups established for savings and credit activities may also provide an opportunity to communicate improved home-care practices and maternal and child health-seeking behaviour in these areas22. These efforts can be more effective if husbands or partners are involved in the process.
Another key finding was the lower likelihood of reporting child death among women delivering at health facilities, compared with those delivering at home. Qualitative studies from northern Nigeria have reported the following factors as critical to perpetuating the low utilization of health services (ie low uptake of ANC and supervised delivery): the perception that home deliveries are comfortable; a belief that facility-based deliveries are unnecessary; and cost21. Any program seeking to increase ANC uptake, supervised childbirth and maternal and child health services in rural settings should therefore communicate carefully the benefits of seeking access to formal health services.
Ever use of FP was associated with a higher chance of reporting child death. However, it may simply be that in resource constrained rural Nigeria, where the local health system may well be dysfunctional, ever use of FP is not a critical indicator. For FP services are available in only a few rural Nigerian health facilities where there are irregular supplies, few reported clients and few re-visits23. However, a strong health system that provides regular FP services to meet the reproductive health needs of women is one of the catalysts in reducing child mortality. Those who are not able to access FP due to culture, religion or non-availability of services are less likely to benefit from the child survival advantages associated with use of FP. Considering the challenges of accessing FP services in rural Nigeria, the majority of women who ever used FP may well be irregular users22.
Another factor associated with the utilization of health services was the possession of vaccination cards for the last child born. Women who had vaccination cards were found to be less likely to report child death; presumably their children were vaccinated according to schedule and so had a reduced risk of contracting diseases with high a child mortality. The present study also found that women with older living children were less likely to report child death, implying that once children pass the critical stages for early mortality, the survival advantage of their siblings increases24.
Limitations
Key limitations associated with these data are threefold. First, the retrospective nature of the data may be associated with recall bias, which is more pronounced for events that took place 5 years before the survey. The survey responses may also have been biased towards more 'don't know' or 'other' answers due to of high illiteracy levels among respondents (particularly in the northern zone), resulting in varying understanding of concepts. However, even with adequately trained interviewers such problems are inevitable. The survey was led by an experienced technical team who had the necessary skills to overcome such limitations; the survey also provides comprehensive information based on a national representative sample.
Second, the results cannot be generalized because the focus of the study was women who gave birth within the 5 years preceding the survey. Therefore, results regarding the prevalence of child deaths may not be applicable to all rural Nigerian women. For example, if examined child mortality rates were based on those that occurred 10 years before the survey, this could have increased the denominator or number of women. Third, the cross-sectional design of the study as well as associated analytical methods only provided evidence of statistical association - rather than causality - between independent variables and child death.
Nigeria has one of the highest child mortality levels in the world. Multiple explanations are required to account for this. After controlling for other variables, this study found that, among many other factors, household headship was a strong predictor. Programs aimed at addressing reductions in child mortality should focus on areas related to women's autonomy, such as increasing access to literacy programs and communication about good practices in maternal and child health-seeking behavior. Male involvement in these processes is essential, particularly in MHH where women may not have autonomy due to sociocultural beliefs. More studies are required in rural Nigeria in order to explore findings such as those related to the reported high child death rate among women who ever used FP. However, the results should be interpreted with caution, due to the uniqueness and paradoxes of life in Nigeria - a country with plentiful resources but a dysfunctional healthcare system.
References
1. UNICEF. Young child survival and development. (Online) 2007. Available: http://www.unicef.org/childsurvival/index_40850.html (Accessed 23 September 2010).
2. National Bureau of Statistics (NBS). Nigeria Multiple Indicator Cluster Survey 2007 Final Report. Abuja, Nigeria: NBS, 2007.
3. Macro International Inc. MEASURE DHS STATcompiler. (Online) 2010. Available: http://www.measuredhs.com (Accessed 13 November 2010).
4. Wall LL. Dead mothers and injured wives: the social context of maternal morbidity and mortality among the Hausa of Northern Nigeria. Studies in Family Planning 1998; 29: 341-359.
5. Erulkar AS, Bello M. The Experience of Married Adolescent Girls in Northern Nigeria. New York: The Population Council, 2007.
6. Babalola S, Fatusi A. Determinants of use of maternal health services in Nigeria - looking beyond individual and household factors. BMC Pregnancy and Childbirth 2009; 9: 43.
7. World Bank. Poverty in the midst of plenty: the challenge of growth with inclusion. Report no. 14733-UNI. Washington: Population and Human Resource Division, West Africa Department, World Bank, 1996.
8. National Population Commission (Nigeria), ICF Macro. Nigeria Demographic and Health Survey 2008. Abuja, Nigeria: Population Commission and ICF Macro, 2009.
9. Castle SE. Intra-household differentials in women's status: household function and focus as determinants of children's illness management and care in Rural Mali. Health Transition Review 1993; 3(2): 137-157.
10. Gupta DM. Death clustering mothers' education and the determinants of child mortality in Rural Pujab, India. Population Studies 1990; 44(3): 489-505.
11. Staten LK, Dufour DL, Reina JC, Spurr GB. Household headship and nutritional status: Female-headed versus male/dual-headed households. American Journal of Human Biology 1998; 10(6): 699-709.
12. Katapa RA. A comparison of female- and male-headed households in Tanzania and poverty implications. Journal of Biosocial Science 2006; 38(3): 327-339.
13. McDaniel A. Historical racial differences in living arrangements of children. Journal of Family History 1994; 19(1): 57-77.
14. Gwatkin DR, Rutstein S, Johnson K, Pande RP, Wagstaff A. Socio-economic differences in health, nutrition, and population. Washington, DC: World Bank, 2000.
15. Helen Keller International. Female decision-making power and nutritional status within Bangladesh's socio-economic context. Nutritional Surveillance Project Bulletin no. 20. Dhaka, Bangladesh: Hellen Keller International, 2006. Available: http://www.hki.org/research/NSP%20Bulletin%2020.pdf (Accessed 13 November 2010).
16. Buor D. Mothers' education and childhood mortality in Ghana. Health policy 2003; 64: 297-309.
17. Doctor HV. Women's schooling and religious affiliation in Malawi at the end of the twentieth century. International Journal of Educational Development 2005; 25(5): 481-492.
18. Caldwell JC. Education as a factor in mortality decline: an examination of Nigerian data. Population Studies 1979; 33: 395-413.
19. Gabrysch S, Campbell OMR. Still too far to walk: literature review of the determinants of delivery service use. BMC Pregnancy and Childbirth 2009; 9: 34.
20. Mberu BU. Household structure and living conditions in Nigeria. Journal of Marriage and Family 2007; 69: 513-527.
21. Adamu YM, Salihu HM. Barriers to the use of antenatal and obstetric care services in rural Kano, Nigeria. Journal of Obstetrics and Gynaecology 2002; 22(6): 600-603.
22. Tripathy P, Nair N, Barnett S, Mahapatra R, Borghi J, Rath S. Effect of a participatory intervention with women's groups on birth coutcomes and maternal depression in Jharkhand and Orissa, India: A cluster-randomized controlled trial. Lancet 2010; 375: 1182-1192.
23. Ameh C, Hofman JJ, van de Broek N. Baseline survey of primary health care and basic emergency and obstetric care health facilities in Katsina, Yobe and Zamfara States of northern Nigeria. Kano, Nigeria: PRRINN-MNCH Programme, 2009.
24. Madise N. Child mortality in Malawi: further evidence of death clustering within families. In: AR Powell, A Eleuther , A Mwageni, A Ankomah (Eds). Population dynamics: some past and emerging issues. Exeter: University of Exeter, Institute of Population Studies,1996; 27-35.
