It has been established that childhood obesity continues into adulthood with adverse consequences for health1-3. The prevalence of childhood obesity in both developed and developing countries has risen in recent decades to epidemic rate4, including even Greece, where there is a long tradition of healthy diet5. In the last decade, childhood obesity in Greece has been estimated at between 6.1 and 14.8%6-9.
Many factors are involved in this public health problem, most commonly an imbalance between calorie intake and energy consumption10. Genetic factors contribute to some extent11,12 but sedentary behaviour, changes in dietary habits and a lack of physical activity are the main issues13,14. Socioeconomic factors may also influence the development of childhood obesity15 and within-country variation has been reported16.
The primary objective of this study was to estimate the prevalence of obesity in children and adolescents on the island of Kalymnos, a remote Greek island in the eastern Aegean Sea. The secondary objective was to assess influencing factors for the presence of increased weight in this group.
Population study
An epidemiological cross-sectional study was conducted on schoolchildren aged between 8 and 16 years from two primary and two secondary public schools on the island of Kalymnos. Children were selected by simple random allocation to achieve a representative sample.
Anthropometric measurements
Measurements took place in the schools during September 2010. In a standardized procedure weight was measured using an electronic scale precise to 0.1 kg (Seca 770; Seca, Hamburg, Germany; www.seca.com) on students wearing light clothing and no shoes. Their height was estimated using wall-mounted measuring tapes available at the schools; the barefoot children stood with their heads, backs and buttocks on the vertical line of the height gauge. Finally, parental weight and height were self-reported.
Questionnaire
Due to limited human and financial resources, information was collected via a self-reported questionnaire designed by the authors. The questions were written so a person with moderate education could understand them, and with the exception of questions about age and parental somatometrics they were of a closed type to restrict options. A small pilot study was conducted to improve the questionnaire.
The questionnaire was presented and explained to the teachers (so they were able to assist if necessary) and then distributed to the children, accompanied by written instructions and telephone numbers for use if clarification was necessary. It was suggested that children and parents should complete the questionnaire at home and returned it within 3 days.
The questionnaire was divided into three sections:
- Children's fields: date of birth, sex, daily duration of television watching or playing video games, out-of-school sporting activities, ownership of computer or mobile phone, hours of sleep (<6, 6-8, 8-10, >10 hours/ 24 hours), access to the internet at home, history of breastfeeding and time of initiation of solid food.
- Parental fields: age group, height, weight, level of education (<6, 6-9, 9-12, >12 years), profession and smoking status.
- A plain dietary history of the children according to the following fields: weekly consumption of fast-food, consumption of sugar-sweetened soft drinks, consumption of meat, fish, vegetables and fruit.
Ethical considerations
Permission for the study was obtained from the Greek Educational Institute and the Ministry of Education. The Directors of primary and secondary education in Kalymnos were informed about this study. The written consent of a parent was necessary for the children to participate.
Definitions
Body Mass Index (BMI) was calculated as weight in kilograms divided by height in meters squared. The nutritional status (overweight and obesity) was defined according to the International Obesity Task Force (IOTF) standards, based on the measurements of children from 6 countries17. Parents were defined as overweight if their BMI was over 25, and obese if their BMI was over 30.
Statistical analysis
Categorical data are presented as absolute and relative frequencies while continuous data as mean ± standard deviation (SD). The sample size was estimated using precision analysis. It was assumed that the prevalence of obesity was 8 ± 3.5%; based on this assumption, 230 subjects were needed to create a 95% confidence interval (CI). Assuming 10% of the children would not participate, the sample was set at 253 children. Children with increased weight were considered to be both obese and overweight.
Initially a univariable analysis was performed, estimating the unadjusted odds ratios (OR) in order to reveal possible associations between the students' increased weight and potential factors. For categorical data with more than two classes, apart from unadjusted OR compared with a reference level, an overall χ2 test was performed. Multivariable logistic regression analysis was further performed for factors statistically significant at the 20% level in univariable analysis so as to estimate the adjusted OR. The best-fit model was selected by a backward stepwise process and likelihood ratio method as the selective criterion18. Data analysis was performed by using SPSS v13.0 (www.spss.com).
The participants were 232 schoolchildren (91.6% participation rate) and their characteristics are presented (Table 1). The children's mean age was 12.2 ± 2.6 years and 43.9% (n=102) were male. All were of Greek origin. Their mean BMI was 20.7 ± 3.8. In total, 20.6% (n=48) of the participants were classified as overweight and 8.1% (n=19) were obese; 45.6% (n=106) were exposed to tobacco smoke at home. The majority of the children (85.9%) had been breastfed, and 58.4% of the mothers were engaged in housekeeping at home. Finally, 8.6% of the mothers and 25% of the fathers were obese.
In the univariable analysis, increased childhood weight was associated only with maternal obesity (Table 2); specifically, the odds of increased weight in children with obese mothers were 2.46 (95%CI 1.34-4.51) higher. No other variable was statistically significant in the univariable analysis.
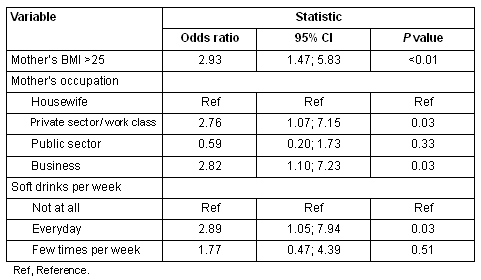
The adjusted odds ratios from the best-fit model are presented (Table 3). Apart from maternal obesity, the mother's occupation and the child's weekly consumption of soft drinks were statistically significant factors. Comparing each mother's occupation class with the housewife class, it was estimated that the odds of children's increased weight were 2.76 (95%CI 1.07-7.15) higher for private sector/ working class and 2.82 (95%CI 1.10-7.23) for business class, taking into account the other variables. Clearly, the chance of increased weight was significantly higher in these two classes. Participants who consumed soft drinks daily had 2.89 (95%CI 1.05-7.94) higher odds of having increased weight compared with the students who had rare soft drink consumption, after adjusting for other model terms.
Table 1: Study population characteristics
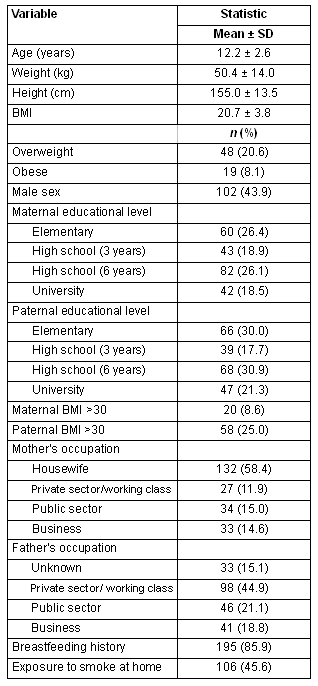
Table 2: Univariable association between increased weight and potential factors
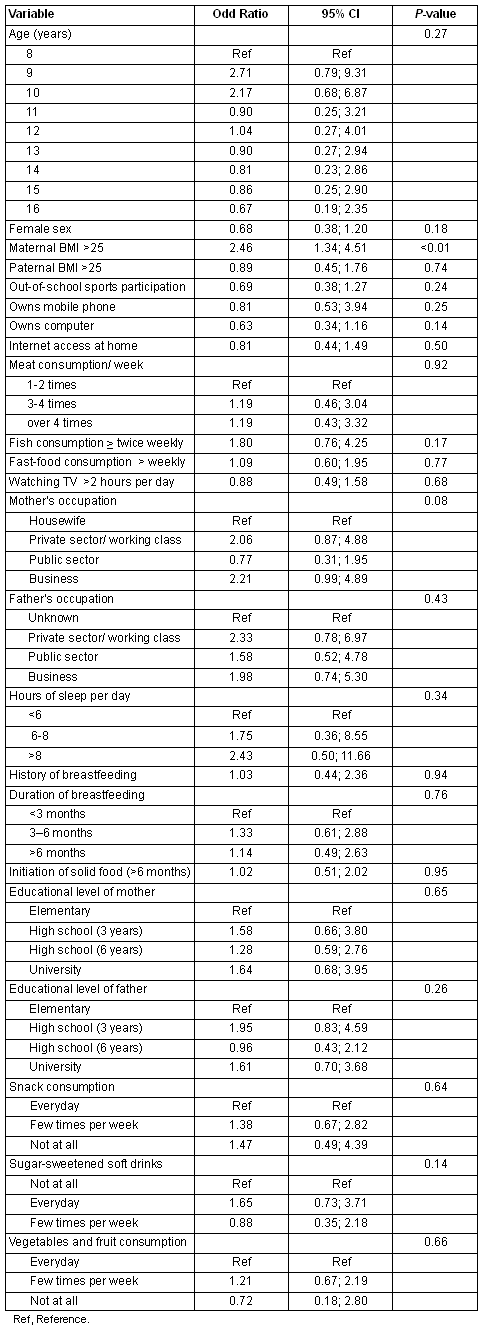
Table 3: Adjusted odds ratios of the best-fit model
Discussion
The prevalence of childhood obesity on the island of Kalymnos was 8.1%, similar to previous studies in Greece6-9. The prevalence of obese and overweight children combined was 28.7%, suggesting almost one-third of the island's children have increased weight. That this public health problem has infiltrated even this remote region could be due to the recent development of tourism changing the way of life and dietary habits of island dwellers.
In agreement with other studies, maternal obesity enhanced the probability of increased weight in children19,20. Obesity in one or both parents probably influences the child's risk of obesity because of shared genes or environmental factors within families. Parents are role models for their children and their habits can affect children's behaviour in terms of calorie intake and amount of physical activity13.
Evidence is limited regarding specific food or dietary patterns that contribute to excessive calorie intake in children and adolescents13. However, it is clear that large portions of food and beverages, eating meals from fast-food restaurants, frequent snacking on energy-dense foods and consuming beverages with added sugar contribute to excess energy intake in children and adolescents13. Evidence is mounting regarding the association of consuming sugar-sweetened drinks with weight gain in children and adolescents21-23. The present study confirms this relationship with the finding that consumption of soft drinks every day was more frequent in children with elevated weight.
Physically active children are likely to remain physically active into adolescence and adulthood. Certainly children and adolescents' participation in physical activities may have a beneficial effect on their body weight14. That no such association was found in the present study may be due to the lack of data on the duration and intensity of out-of-school athletic activities. A more detailed questionnaire may clarify this result.
Regarding the association of sedentary behaviour with obesity, several studies have found a positive correlation between obesity and media use24-26. In particular, media use and television watching reduce physical activity and metabolic rate. The consumption of calories may increase due to children eating snacks and other food in front of the television, leading to an unhealthy way of life. This study, however, found no correlation of sedentary life with participants' weight increase.
As has been seen in other studies, socioeconomic status influences the prevalence of obesity in children15,27,28. In the present study increased weight was dependent on the mother's occupation, but independent of the father's occupation and parental education levels. The probability of increased weight in children whose mothers were occupied with home duties was lower than for any other maternal occupation, suggesting that these mothers had more time to manage their children's diet.
Whether feeding practices during the first year of life (ie any breastfeeding, duration of breastfeeding, age of solid food introduction) influence the nutritional status of older children is controversial29,30, and the present results do not support any such association. Of note, however, is that the majority of participating children had been breastfed for a minimum period of 3 months with solid food commenced after 6 months of age.
Finally, several investigations have found a positive correlation between smoking during pregnancy and children's increased weight and blood pressure later in life31. Moreover, many studies have also indicated that smoking is associated with glucose intolerance, insulin resistance, dyslipidemia (increased low-density lipoprotein [LDL] cholesterol and decreased high-density lipoprotein [HDL] cholesterol), endothelial dysfunction, as well as a hyper-coagulation and an unhealthy body fat distribution, which are all related to the development of the metabolic syndrome32. There is also evidence that children's passive exposure to smoke may contribute to the reduction of the HDL and to a positive correlation between BMI and the daily time of exposure to tobacco smoke33,34. However, in the present study an association between smoke exposure at home and obesity was found to be not statistically significant.
Limitations
The study has some limitations. First, parental self-reporting and partial self-reporting of the children's data could have influenced the study's results. It is also necessary to take into account recall bias, especially regarding feeding practices during the first year of life. The questionnaire was designed by the authors and its validity and reliability was not tested. However, the questions were written in a clear and understandable way, although the restriction imposed by the use of closed questions must also be considered. In addition, a cross-sectional study may provide evidence of associations but not proof of causality. Finally, these results cannot be generalised to other populations.
Despite these limitations, the strong points of this study are its high participation rate (due to the positive relationship between Kalymnos medical staff and the island people) and the representative sample of children from the island.
The prevalence of obesity among Kalymnian children and adolescents is high. According to the present results, dietary habits, and maternal BMI and socioeconomic status appear to exert the highest influencing effect. Given the well known consequences of obesity, useful interventions at both school and home include fostering healthier dietary habits among family members, and also increasing in physical activity.
References
1. Wright CM, Parker L, Lamont D, Craft AW. Implications of childhood obesity for adult health: findings from thousand families cohort study. BMJ 2001; 323: 1280-1284.
2. Field AE, Cook NR, Gillman MW. Weight status in childhood as a predictor of becoming overweight or hypertensive in early adulthood. Obesity Research 2005; 13: 163-169.
3. Freedman DS, Khan LK, Serdula MK, Dietz WH, Srinivasan SR, Berenson GS. Inter relationships among childhood BMI, childhood height, and adult obesity: the Bogalusa Heart Study. International Journal of Obesity Related Metabolic Disorders 2004; 28: 10-16.
4. Lobstein T, Baur L, Uauy R, IASO International Obesity Taskforce. Obesity in children and young people: a crisis in public health. Obesity Review 2004; 5(Suppl1): 4-104.
5. Manios Y, Magkos F, Christakis G, Kafatos AG. Twenty-year dynamics in adiposity and blood lipids of Greek children: regional differences in Crete persist. Acta Pediatrica 2005; 94: 859-865.
6. Mihas K, Toyntas G, Alevizos A, Gizlis B, Konsyantinou E, Panagiotakos DB et al. Epidemiological elements in obesity among adolescents in an urban area. Results of VYRONAS study. Primary Health Care 2006; 18(3): 149-157.
7. Krassas GE, Tsametis C, Baleki V, Constantinidis T, Unluhizarci K, Kurtoglu S et al. Balkan Group for the Study of Obesity. Prevalence of overweight and obesity among children and adolescents in Thessaloniki-Greece and Kayseri-Turkey. Pediatric Endocrinology Review 2004; 1(Suppl3): 460-464.
8. Karayiannis D, Yannakoulia M, Terzidou M, Sidossis LS, Kokkevi A. Prevalence of overweight and obesity in Greek school-aged children and adolescents. European Journal of Clinical Nutrition 2003; 57(9): 1189-1192.
9. Tokmakidis SP, Kasambalis A, Christodoulos AD. Fitness levels of Greek primary schoolchildren in relationship to overweight and obesity. European Journal of Pediatrics 2006; 165(12): 867-874.
10. US Department of Health and Human Services. The Surgeon General's Call to Action to Prevent and Decrease Overweight and Obesity. Rockville, MD: Public Health Service, Office of the Surgeon General, 2001.
11. Le Stunff C, Fallin D, Bougneres P. Paternal transmission of the very common class I INS VNTR alleles predisposes to childhood obesity. Nature Genetics 2001; 29: 96-99.
12. Dietz WH, Gortmaker SL. Do we fatten our children at the television set? Obesity and television viewing in children and adolescents. Pediatrics 1985; 75: 807-812.
13. Institute of Medicine. Preventing childhood obesity - health in the balance. Washington, DC: National Academies, 2005.
14. Strong WB, Malina RM, Blimkie CJ, Daniels SR, Dishman RK, Gutin B et al. Evidence based physical activity for school-age youth. Journal of Pediatrics 2005; 146: 732-737.
15. Garn SM, Clark D. Nutrition, growth, development, and maturation: findings of the Ten State Nutritional Survey of 1968-70. Pediatrics 1975; 56: 306-319.
16. Lahti-Koski M, Taskinen O, Simila M, Mannisto S, Laatikainen T, Knekt P et al. Mapping geographical variation in obesity in Finland. European Journal of Public Health 2008; 18(6): 637-643.
17. Cole TJ, Bellizzi MC, Flegal KM, Dietz DH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320: 1240-1243.
18. Agresti A. Building and applying logistic regression models. In: A Agresti (Ed.). An introduction to categorical data analysis. New Jersey: John Wiley, 2007; 137-172.
19. Bouchard C. Childhood obesity: are genetic differences involved? American Journal of Clinical Nutrition 2009; 89(Suppl): 1494S-501S.
20. Whitaker RC, Write JA, Pepe MS, Seidel DS, Dietz WH. Predicting obesity in young adulthood from childhood and parental obesity. New England Journal of Medicine 1997; 337: 869-873.
21. Ludwig DS, Peterson KE, Gortmaker SL. Relation between consumption of sugar-sweetened drinks and childhood obesity: a prospective, observational analysis. Lancet 2001; 357: 505-508.
22. Welsh JA, Cogswell ME, Rogers S, Rockett H, Mei Z, Grummer-Strawn LM. Overweight among low-income preschool children associated with the consumption of sweet drinks: Missouri 1999-2002. Pediatrics 2005; 155: e223-e229.
23. Malik VS, Schulze MB, Hu FB. Intake of sugar-sweetened beverages and weight gain: a systematic review. American Journal of Clinical Nutrition 2006; 84: 274-288.
24. Dietz WH, Gortmaker SL. Do we fatten our children at the television set? Obesity and television viewing in children and adolescents. Pediatrics 1985; 75: 807-812.
25. Gortmaker SL, Must A, Sobol AM, Peterson K, Colditz GA, Dietz WH. Television viewing as a cause of increasing obesity among children in the United States, 1986-1990. Archives of Pediatric and Adolescent Medicine 1996; 150(4): 356-362.
26. Crespo CJ, Smit E, Troiano RP, Bartlett SJ, Macera CA, Andersen RE. Television watching, energy intake, and obesity in US children: results from the third National Health and Nutrition Examination Survey, 1988-1994. Archives of Pediatric and Adolescent Medicine 2001; 155(3): 360-365.
27. Strauss RS, Knight J. Influence of the home environment on the development of obesity in children. Pediatrics 1999; 103: e85.
28. Lamerz A, Kuepper-Nybelen J, Wehle C, Bruning N, Trost-Brinkhues G, Brenner H et al. Social class, parental education, and obesity prevalence in a study of six-year-old children in Germany. International Journal of Obesity 2005; 29: 373-380.
29. Baughcum AE, Burklow KA, Deeks CM, Powers SW, Whitaker RC. Maternal Feeding Practices and Childhood Obesity. Archives of Pediatric and Adolescent Medicine 1998; 152: 1010-1014.
30. Brophy S, Cooksey R, Gravenor MB, Mistry R, Thomas N, Lyons RL et al. Risk factors for childhood obesity at age 5: analysis of the Millennium Cohort Study. BMC Public Health 2009; 9: 467.
31. Oken E, Huh YS, Taveras EM, Taveras M, Rich-Edwards JW, Gillman MW. Associations of Maternal Prenatal Smoking with Child Adiposity and Blood Pressure. Obesity Research 2005; 13(11): 2021-2028.
32. Xie B, Palmer PH, Pang Z, Sun P, Duan H, Johnson CA. Environmental tobacco use and indicators of metabolic syndrome in Chinese adults. Nicotine and Tobacco Research 2010; 12(3): 198-206.
33. Neufeld E, Mietus-Snyder M, Beiser A, Baker A, Newburger J. Passive cigarette smoking and reduced HDL cholesterol levels in children with high-risk lipid profiles. Circulation 1997; 96: 1403-1407.
34. Wojciak RW, Mojs E, Gajewska E. The assessment of exposure on passive smoking in obese children. Przegl Lek 2009; 66(10): 677-679.
