The Australian Government's Rural Clinical Training and Support (RCTS) program has made an outstanding contribution to rural communities over a decade or more. This article presents a rich picture of the successes and challenges in the 17 Australian rural clinical/regional medical schools (RCS/RMS). The research shows how they are improving access to university medical education for rural people, creating a university presence that is integrated in rural communities and producing more rural clinicians. While Australian universities offer a variety of undergraduate and graduate medical programs, it takes a minimum of 10 years to fully train a rural medical practitioner. The present research discusses the number of medical students on long-term clinical placements each year in rural health services and reveals why graduates are being attracted to rural practice.
Rural researchers argue there is a need to rigorously evaluate the impact of interventions and policies that aim to redress the inequitable distribution of healthcare professionals to rural and remote areas and to find good strategies to guide future practice and policy1. This article presents a snapshot evaluation of the achievements of the innovative medical education programs offered through Australian RCS and RMS and proposes an agenda to increase the momentum to build the rural health workforce.
Background
In response to the national rural health agenda initiated in the 1990s, Australian rural health policy has been strongly focused on building the rural health workforce2. The National Rural Health Agenda highlighted inequities in the health outcomes of rural communities with limited access to health services and unequal distribution of health professionals. In 2013, Australia has more doctors per density of population than the UK, New Zealand, USA and Canada3. The number of medical specialists is increasing but the workforce is not evenly distributed, with fewer medical graduates living and practising in rural areas. Rural communities are still reliant on international medical graduates and specialists who fly or drive to rural areas, and thousands of rural patients are transported to cities for treatment each year.
The more remote the community, the more likely it is to be underserved4. There are only 2.5 doctors per 1000 residents working in regional and rural Australia, in contrast to Australian capital cities, with more than four doctors per 1000 residents, one of the highest rates in the world5. Between 2007 and 2011 there was a 17% increase in the number of medical practitioners registered in Australia but little improvement in the rural workforce shortage6.
Over the past decade there has been a massive expansion of Australian medical student training from 1320 domestic and 267 international graduates in 2005 to 2994 domestic and 497 international graduates in 2013. A total of 3668 students commenced medical studies in 20137. Australia now has one of the highest rates of medical graduates in the OECD3. Despite similar numbers of medical students per capita in rural and regional settings and in capital cities, government investment in regional training has not yet produced its intended outcome, an end to the rural and regional medical shortage.
In 2000, the then Commonwealth Department of Health and Ageing (now Department of Health) announced the establishment of an RCS funding program and invited universities to deliver medical education in rural communities. By 2012, a total of 16 university medical schools had established rural programs, creating an extensive national network of RCS and RMS in each state and territory, funded through the RCTS program.
The aim of this study was to explore the achievements and challenges of RCS and RMS. The research question was, 'What are the achievements and challenges of the RCS in relation to key reporting parameters' (Appendix I).
This descriptive study entailed semi-structured interviews with key informants from 17 RCS/RMS programs. To obtain relevant data, participants in this study needed to be those with key responsibilities for the strategic development and implementation of the program within each university. Therefore purposive sampling was used to invite participants from each clinical school. Interviews were conducted with each director or senior staff member. In some cases a delegate was nominated because the director had been newly appointed. One school declined to participate in the interview, so information was sourced from the medical school website. Key informant interviews were used to represent the broadest and most complete knowledge of the RCS program. Key informants were also in a position to supply additional quantitative material relating to their program.
The interview was designed using both closed and open-ended questions. It was decided to use the nine RCTS program funding parameters (Appendix I) as a framework to formulate the questions. Questions asked, for example, about how many students were placed for 12 months or more each year, the percentage of total domestic students that have spent a minimum of 12 months at a RCS, and the length and types of placements available. Respondents were asked whether they had been able to meet each funding parameter, to identify key strategies for success, and to comment on the challenges they experienced.
A single interviewer (JG) conducted all the interviews to allow constant horizontal comparison between interviews. Interview data were organised into thematic categories, and analysed by the research team. Key themes and comments that were consistent or that brought up new themes were summarised. The summary was then posted on the shared list server to encourage participants to comment and to eliminate any conflict of interest. These findings were then presented at an open forum where clinical school directors and managers could make comments and validate the data presented regarding their program.
Ethics approval
This article is an evaluation of the different strategies implemented by medical schools in the national program and as such did not require ethics approval.
Sixteen Australian medical schools have established eighteen rural clinical schools/regional medical schools. Figure 1 shows not only RCTS funded main and minor sites but also those sites established through the Australian Government's University Department of Rural Health (UDRH) and Dental Training Expanding Rural Placements (DTERP) programs.
All the medical schools have established multiple rural and remote sites where they have student clinical placements widely distributed across rural and remote Australia. Prior to these programs, there were no long-term rural medical placements in rural and remote Australia.
Table 1 shows Australian universities with RCS and the year each was established. Notably, Monash and Flinders universities established rural clinical schools prior to the RCS funding program. New medical schools such as Deakin University, University of Wollongong, University Western Sydney and University of Notre Dame (Fremantle, Western Australia) may not be in a position to report for several years on the number of graduates into rural practice. However, these programs report innovative approaches to rural medical education.
Table 1: Year of establishment of Australian rural clinical schools
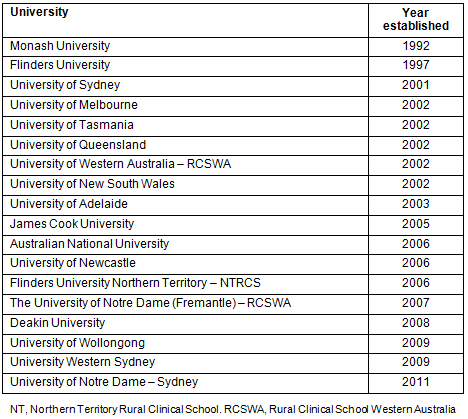
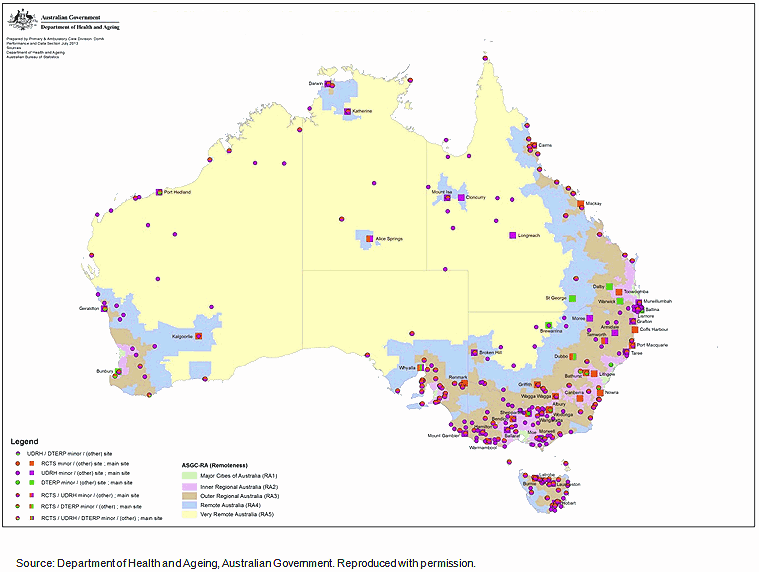
Figure 1: Rural Clinical Training and Support, University Department of Rural Health and Dental Training Expanding Rural Placements programs: major and minor sites.
Parameter 1 - Delivering rural experiences to enhance the workforce
A total of 1224 medical students were reported to have spent a minimum of 1 year in a rural clinical placement in 2012. Universities with more than 100 rural student placements per annum were Monash, Queensland, Flinders, James Cook and Deakin. The smallest number of student placements per annum was from Flinders University in the Northern Territory and University of Notre Dame (Fremantle), which have unique programs delivering learning experiences in remote communities.
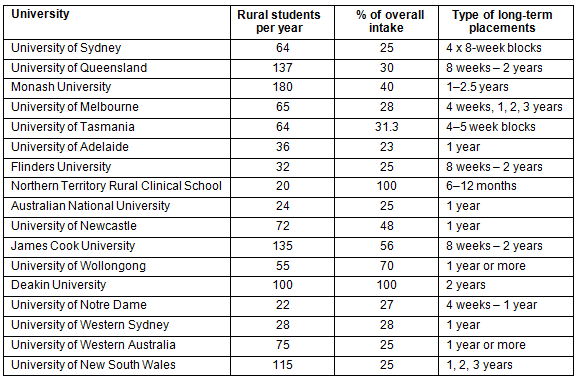
The length of rural placements range from short-term 4-8-week rotations (previously Rural Undergraduate Support and Coordination program funding, now administered by RCS) to longitudinal immersions of 6 months or 1, 2 or 3 years. Table 2 shows the number of medical students undertaking long-term rural placements, the percentage of the annual overall intake, and the type of long-term clinical placements. All rural clinical schools provide placements in hospitals, community and primary care settings.
There are many different approaches to attract students to apply for rural placements. Most schools select students using a preference system, which selects the most interested students; others use incentives to attract students. Several schools reported that the high-quality learning and clinical experiences are promoted by word of mouth from students who enjoy their rural placements, building a culture of competition to get into the RCS. Attractiveness of RCS placements is based on perceived value of the placement rather than on remoteness of the placement. Some RCS and RMS are also managing to increase opportunities for rural clinical placements in collaboration with nursing, paramedic and allied health programs.
Table 2: Rural clinical schools: long-term rural placements
Parameter 2 - Ensuring high-quality rural experiences
Responses to the interviews revealed that all schools seek to minimise the financial burden of rural placements by providing rent-free or subsidised accommodation in high-quality, furnished houses or units and by offering subsidies for travel. Several schools have purchased land and built student accommodation, including some large-scale student apartments, in close proximity to clinics or hospitals. In this way RCS/RMS contribute to the economic development of small towns even in regions, such as mining towns, where this is a major cost. Schools also support student learning by providing internet connections and information technology, video-conferencing systems and seamless access to rural general practices and health services. Several schools care for the wellbeing of students by providing counselling, defensive driving classes, health and fitness memberships and support for families.
The quality of the learning experience is integral to each school's curriculum. Many schools offer longitudinal integrated placements so that the students benefit from extended contact with patients, multiple opportunities to practice skills, and ongoing mentoring relationships. Ongoing evaluation of these experiences is core to each RCS and consistently shows that students highly value their learning experiences.
Medical students' experience of community is also purposefully nurtured. Students are immersed in their local rural community where they have orientation to the community and, during the year, receive feedback from the community.
Parameter 3 - Supporting rural academics/teachers and building training capacity
The most common and important strategy in support of rural clinical academics has been to recruit staff from local rural general practitioners and specialists. This strategy has created many new clinical academics in rural areas, which is likely to retain and expand the clinical workforce. It has been important to pay realistic salaries. Some schools reported that they provide rural salary incentives or flexible payment options and limit the administrative burden that comes with university appointments. All schools reported that they provide adjunct academic status for clinicians who teach students but are not directly employed by the school. This has been another successful strategy, creating academic career opportunities for rural clinicians where previously none existed.
There are numerous strategies for supporting rural academics as clinical teachers. All RCS and RMS have a strong commitment to professional development, with some universities offering postgraduate courses to academics and clinical teachers. All schools also reported that they have clinically active academic staff who are supported to undertake research.
Additional capacity is built through formalising clinical placements through written agreements, memoranda of understanding with hospitals and health services and through international collaboration and staff exchanges.
Parameter 4 - Rural student recruitment
One of the most important funding parameters is to develop strategies for recruitment of students with rural backgrounds, because rural-origin students are more likely to be attracted to rural practice8.
Most RCS have a rural student recruitment strategy that includes attending careers expo events, but strategies vary according to local needs and conditions. Some RCS promote the university in rural areas. For example, the University of Sydney has a Discovery Bus, and the University of WA visits all rural high schools to support students wanting to gain entry into medicine9. In general, there is a lack of a clear pathway for rural high school students wanting to study medicine. Findings highlighted a need to increase engagement, with RCS undertaking systematic activities with high schools and primary schools.
Scholarships are offered to many rural students and in some universities there is a bonus point system for rural background applicants through initiatives such as the Dean's Rural List.
Several universities have rural people involved in the selection process. Some medical schools select for rural background through an admission policy that requires 25% rural intake, but more work is needed to change outdated medical admission policies and processes. Several RCS reported a sense of frustration because they have little influence on the admission decisions regarding entry into medical school, whereas others have direct input into policy decisions.
RCS and RMS provide substantial support for the rural student clubs, which include rural medical student members.
Parameter 5 - Community engagement and collaboration
This parameter requires universities to:
- build partnerships, develop and maintain advisory groups: All schools have some form of community advisory board or committee, a range of community groups using the RCS facilities and buildings for meetings and events, and extensive media exposure. One respondent suggested that an important aspect of community engagement was to focus on partnerships that are genuinely mutually beneficial and dialogue beyond just arranging activities. Another stressed the importance of several key factors including presence, persistence, consistence and support. Several schools reported having local champions as a key strategy.
- engage with the community for positive rural experiences for students: Various community engagement strategies were reported. One school claimed the community sets the direction for education and research. Most schools said they had support of local government and the RCS is integrated in their region's planning processes. Five schools said their students undertake a mandated community project. One school reported they have established a community ombudsman portfolio and others have community members who are involved in student admissions and rural scholarship selection. In all rural areas, students and staff are involved in sports and community activities. However, few schools approached community engagement in a systematic way. Only three schools reported how they seek to understand the community needs, research the demographics and health status for a community engagement plan.
- work collaboratively with other key stakeholders: All schools have well-established collaborations with health services, non-government organisations, other educational institutions and professional groups that use local facilities and expertise. These relationships are essential to successful clinical placements and student wellbeing.
Parameter 6 - Progressing the rural health agenda
The establishment of the RCS program has substantially influenced the rural health agenda and there are strong partnerships for research with rural workforce agencies in each state.
Several schools have established partnerships with major research centres and they encourage and mentor early-career researchers and PhD students. Strategic and applied research is being undertaken to influence health policy. Research studies have a wide range of fields including epidemiology and population health, Aboriginal health, aged care, mental health and suicide prevention, farming families and climate change. Rural academics publish in prominent journals and have established this journal, Rural and Remote Health, which is now funded by RCS and RMS across Australia.
Each school has formed valuable partnerships with rural organisations and receives recognition from the university for driving rural health policy. Rural health is integrated throughout the curriculum in several universities, but not all, because some schools are still quite marginalised from the central medical school based in the city. Some RCS academics have been appointed to leadership roles within the university and in other high-profile and leadership positions in key organisations locally and nationally. Schools collaborate with key stakeholders to undertake innovative projects in rural health practices such as tele-health consulting.
Parameter 7 - Aboriginal and Torres Strait Islander health
This parameter of the program aims to increase opportunities for Aboriginal and Torres Strait Islander students and provide all medical students with a comprehensive understanding of Aboriginal and Torres Strait Islander health issues. All schools provide cultural awareness for staff and students and activities with the communities. Some schools have a high profile in the community during NAIDOC (National Aborigines and Islanders Day Observance Committee) week and partnerships with organisations such as the Australian Indigenous Doctors' Association and the Leaders in Indigenous Medical Education Network. Several RCS have specific programs to support Indigenous students and have successfully employed Aboriginal academics. Some schools find it difficult to attract Indigenous staff and are concerned about depleting other organisations. Therefore, they work with local groups for simulation sessions for Aboriginal health workers and Aboriginal guest lecturers. A couple of RCS are undertaking research about Indigenous health; for example, the RCS in Western Australia has a National Health and Medical Research Council centre in collaboration with Aboriginal research partners.
Some RCS and RMS programs are based in areas with high Indigenous populations and have good institutional strategies designed to suit their local contexts. Three schools said they have established Indigenous reference groups and this was seen as a key strategy for long-term engagement, attracting role models, building trust and mutual respect. One RCS is undertaking a review to address institutional racism, and another has a memorandum of understanding with its university's School of Indigenous Health. One school provides all fifth-year students a placement with an Aboriginal medical service for 5 weeks whilst others reported they have been working or co-locating with Aboriginal-controlled community health organisations/Aboriginal medical services. Two schools have established partnerships for retaining young rural Aboriginal people in school and work. One RCS delivers an annual Indigenous Entry Pathway and Preparation for Medicine program. One school provided funding to build infrastructure for an Aboriginal health clinic in general practice.
Parameter 8 - Monitoring and progressing evidence base
This parameter seeks collection of data regarding the workforce outcomes from rural clinical training activity with evidence supporting the positive effect of rural clinical medical training on the rural health workforce.
Seven of the nine rural clinical schools that were established prior to 2006 were able to report on the number of graduates in rural training but by 2012 only five schools had developed annual tracking processes for their graduates into rural practice, hence these data were inconclusive. Several newer schools are currently developing an alumni graduate destination database to track where graduates are practising.
The Medical Schools Outcomes Database and Longitudinal Tracking (MSOD) project began collecting data in 200610. All RCS reported that they have been involved. In the future these data will be a valuable source of information on the rural medical training pathway. Several universities focus their evaluation and research on the quality of education, impact of rural placements on the community and career intentions, and recruitment and retention of staff11. In 2005, RCS collaborated to design a national survey of RCS students, which has resulted in four publications that show the factors that attract students to rural placements and that rural-origin students are ten times more likely to practise in rural areas8,12-14.
Parameter 9 - Maximising rural expenditure
All universities understand that RCTS funding is 'ring fenced' - this is specified in the contract with the Commonwealth Department of Health and Ageing (now Department of Health). It was reported that 98% of full-time equivalent staff are located in rural, regional settings. All RCS reported strategies to tightly monitor travel and accommodation expenses, which are an inevitable aspect of a rural program. All RCS invest in local real estate and purchase local goods as well as employing local administrative and academic staff.
Discussion
RCS and RMS deliver the medical curriculum in rural and regional environments and are now integral structures within university medical schools throughout Australia. Each is unique, evolving in response to local community needs. Through targeted community engagement they have built effective regional networks with health services and regional training providers. The RCTS program has enabled local construction and furnishing of high-quality teaching and learning facilities and student accommodation in dozens of rural and regional locations across Australia. Innovative clinical training programs have been developed including distributed learning models, community-based longitudinal integrated clerkships, rural specialty-based clinical training and interprofessional practice models15.
Through the success of the RCS, more than a third of medical students each year are now undertaking a minimum of 1 year's clinical training in rural and regional Australia. However, the key informants identified that there are very limited opportunities for medical graduates to continue their training in rural and regional Australia. So the current investment only addresses the first part of the medical training continuum as rural and regional graduates are being forced back to capital cities for postgraduate training. The rural workforce shortage cannot be solved without regional postgraduate training programs, key recommendations of Health Workforce Australia's Health Workforce 2025 and the Australian Government review of health workforce programs6.
There continues to be not enough general practitioners and medical specialists in rural and regional Australia. The growing trend towards sub-specialisations is resulting in a shortage of generalists, particularly in rural Australia2.
There is a need for funded rural and regionally based internships and rural generalist and specialist training posts and pathways. RCTS programs are well positioned to offer vertically integrated medical education and some RCS and RMS have provided leadership in the development of innovative solutions such as the Mt Gambier community-based junior doctor program, the Monash Gippsland health education model and the Mountain 2 Murray intern program. Monash University, Deakin University and the University of Melbourne are working to produce a cost-effective solution to tackle the critical shortage of postgraduate training opportunities in Victoria. This will allow medical graduates to complete their training in the regions and avoid forcing them back to a capital city at such a critical time of their careers and lives. The proposal is based on creation of regional health and medical education centres, leveraging existing university RCS facilities and staff. These centres will be hubs for a network of training centres in smaller centres.
Vertically integrated training delivers a pathway for a medical graduate to a rural career with the training largely or exclusively undertaken in a rural environment. There is an opportunity and expectation that different levels of learners and clinicians learn from one another in a 'two-way' learning process. A broader definition involves all health professions within a team to learn together about priority health issues and health systems.
This continuum of training could be managed by medical schools for professional entry students, in collaboration with the Postgraduate Medical Councils, medical colleges and vocational GP or specialist training providers. The current poorly coordinated training pathway contributes to the problems identified in the Health Workforce 2025 report and the Australian Government review of health workforce programs6:
- Funding comes from a mix of state and federal sources.
- There is value in addressing the educational continuum, both from a pedagogical and workforce perspective, through continuous educational planning rather than in three separately funded and unlinked processes.
- Coordinated regional training will address issues around geographic distribution and will promote a better balance between generalist, specialist and subspecialist training.
Limitations
This article represents the views of key informants, and although these are broadly representative of the RCS program they may not include the perspective of all rural providers. However, it claims only to be an evaluation of the specific program of which the key informants had oversight. As the interview questions focused on key performance indicators, the report has a bias towards positive outcomes. It is more than a decade since the program commenced, hence it is timely to report these findings.
Building on the outstanding success of the RCTS program as reported by key informants, this article proposes a more coherent approach to rural medical education through vertically integrated rural health training and support programs. The RCTS program delivers different approaches within universities to deliver contextualised rural clinical education programs. There is no doubt that RCS and RMS are producing more medical graduates with a passion for rural health practice. In the future they may facilitate the development of a seamless rural clinical training pipeline linking undergraduate and postgraduate medical education for a sustainable Australian rural medical workforce.
References
1. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural Remote Health 9(2): 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 25 November 2013).
2. Worley P, Murray R. Social accountability in medical education - an Australian rural and remote perspective. Medical Teacher 2011; 33(8): 654-658.
3. OECD. Health data 2013. (Online) 2013. Available: http://www.oecd.org/health/healthdata (Accessed 25 November 2013).
4. Russell DJ, Humphreys JS, Ward B, Chisholm M, Buykx P, McGrail M, et al. Helping policy-makers address rural health access problems. Australian Journal of Rural Health 2013; 21(2): 61-71.
5. Australian Institute of Health and Welfare. Medical workforce 2011. Cat. no. HWL 49. Canberra, ACT: AIHW, 2013.
6. Health Workforce Australia. Health workforce 2025 - doctors, nurses and midwives. vol. 1. (Online) 2012. Available: http://www.hwa.gov.au/sites/uploads/FinalReport_Volume1_FINAL-20120424.pdf (Accessed 31 August 2015).
7. Medical Deans of Australia and New Zealand. Medical student statistics. (Online) 2013. Available: http://www.medicaldeans.org.au/statistics/annualtables (Accessed 31 August 2015).
8. Walker JH, Dewitt DE, Pallant JF, Cunningham CE. Rural origin plus a rural clinical school placement is a significant predictor of medical students' intentions to practice rurally: a multi-university study. Rural Remote Health 12: 1908. (Online) 2012. Available: www.rrh.org.au (Accessed 25 November 2013).
9. Emery A, Hurley S, Williams J, Pougnault S, Mercer A, Tennant M. A seven-year retrospective analysis of students entering medicine via a Rural Student Recruitment program in Western Australia. Australian Journal of Rural Health 2009; 17(6): 316-320.
10. Kaur B, Roberton DM, Glasgow NJ. Evidence-based medical workforce planning and education: the MSOD project. Medical Journal of Australia 2013; 198(10): 518-519.
11. Jones M, Humphreys JS, McGrail MR. Why does a rural background make medical students more likely to intend to work in rural areas and how consistent is the effect? A study of the rural background effect. Australian Journal of Rural Health 2012; 20(1): 29-34.
12. DeWitt DE, McLean R, Newbury J, Shannon S, Critchley J. Development of a common national questionnaire to evaluate student perceptions about the Australian Rural Clinical Schools Program. Rural Remote Health 5(3): 486. (Online) 2005. Available: www.rrh.org.au (Accessed 25 November 2013).
13. Krahe LM, McColl AR, Pallant JF, Cunningham CE, Dewitt DE. A multi-university study of which factors medical students consider when deciding to attend a rural clinical school in Australia. Rural Remote Health 10(3): 1477. (Online) 2010. Available: www.rrh.org.au (Accessed 25 November 2013).
14. McLean RG, Pallant J, Cunningham C, DeWitt DE. A multi-university evaluation of the rural clinical school experience of Australian medical students. Rural Remote Health 10(3): 1492. (Online) 2010. Available: www.rrh.org.au (Accessed 25 November 2013).
15. Walters L, Greenhill J, Richards J, Ward H, Campbell N, Ash J, et al. Outcomes of longitudinal integrated clinical placements for students, clinicians and society. Medical Education 2012; 46(11): 1028-1041.
_________________________
Appendix I: Rural clinical school program funding parameters



