Pelvic organ prolapse is a common condition that can significantly affect a woman's life, including her sexual, urinary, and social functioning. In the USA, pelvic organ prolapse is often treated early to prevent any significant deterioration in patients' quality of life. In developing nations, however, pelvic organ prolapse is not treated as early, leading to increased burdens on the daily lives of women.
Pelvic organ prolapse is the failure of the anatomic structures of the pelvic floor to support pelvic viscera. It can cause sexual and urinary dysfunction, and can adversely affect quality of life. Millions of women suffer from pelvic organ prolapse worldwide, with an estimated lifetime prevalence of 30% to 50% in parous women1. One cross-sectional analysis of the Women's Health Initiative found the following incidence of prolapse in the USA: 14.2% reported uterine prolapse, 34.3% had bladder prolapse (cystocele), and 18.6% had rectal prolapse (rectocele). This study also found that uterine prolapse was more common in a Hispanic population2.
Symptoms of pelvic organ prolapse include the sensation of fullness or pressure, a protrusion of tissue from vaginal outlet, dysparuenia, urinary incontinence, and incomplete emptying with voiding. Risk factors for pelvic organ prolapse include multiparty, vaginal delivery, obesity, constipation, and aging1.
Identification of pelvic organ prolapse is difficult because many women are embarrassed by their symptoms. In the USA, questionnaires such as the Pelvic Floor Impact Questionnaire and the Pelvic Organ Prolapse Incontinence Sexual Questionnaire exist to evaluate the impact of pelvic organ prolapse on urinary and sexual functioning3,4. The current assessment tools were designed primarily for a Western patient population, and unfortunately do not adequately evaluate patients in rural nations, such as the Mayans in Guatemala.
In Guatemala, anecdotal evidence suggests that the daily activities of Mayan women contribute to and worsen the degree of pelvic organ prolapse. In general, these women have a higher parity, perform more manual labor, and may even be genetically predisposed to prolapse2. A culturally specific assessment tool is required to determine the extent to which pelvic organ prolapse affects the daily activities of Mayan women in rural Guatemala. It is important that the questionnaires used are not only condition-specific but also lifestyle-specific so that they are applicable to the population being evaluated.
The objective of the present study was to develop a culturally specific assessment tool to better evaluate how pelvic organ prolapse affects daily activities of Mayan women in rural Guatemala.
Study population
The study population consisted of 19 Guatemalan women with various degrees of pelvic organ prolapse who were evaluated at Clinica Ezell in Montellano, Guatemala 14-21 April 2007. Clinica Ezell is affiliated with Health Talents International, a non-profit Christian organization that performs monthly medical-surgical missions in Guatemala. Study participants were assessed by a team of board certified gynecologists from Washington, DC. Participants were evaluated for prolapse, urinary incontinence, and urinary retention. The ordinal staging system was used to determine the stage of pelvic organ prolapse.
Our patient population consisted of indigent Guatemalans living in rural areas near Montellano, a city located in the Suchitepequez province, southwest of the national capital, Guatemala City. The average life expectancy in Guatemala is 69.1 years5. The total fertility rate (births per woman) in Guatemala is 4.4 children. Forty-one percent of the births in Guatemala are attended by a skilled healthcare provider, which includes either a physician or a midwife5,6.
Our study population spoke Spanish and Quiché, a regional Mayan dialectic. In Guatemala, typical daily activities for women include caring for children, cooking, gathering water from nearby streams, and cleaning. Much of the rural population in Guatemala does not have access to running water, electricity, or motor vehicles. As a result these individuals often walk long distances, carry heavy loads of wood and water, and perform a large amount of manual labor.
Assessment tools
The assessment tool created was entitled a Culturally Specific Assessment Tool for Pelvic Organ Prolapse (CSAT-POP) (Appendix I). The assessment tool was based on a review of the literature regarding pelvic floor dysfunction, functional disability assessment tools, previous experience with post-operative evaluation modules, and expert opinion. The survey collected respondents' demographic information, obstetrics history, and assessed their pre-operative ability to perform culturally specific activities of daily living. Demographic information included age, BMI, diagnosis, surgical procedure and surgeon. Obstetrics history included gravida and parity, age at deliveries, location and attendants at birth.
The assessment of activities of daily living was based on the Pelvic Floor Impact Questionnaire7,8 and Lawton and Brody's Instrumental Activities of Daily Living (IADLs)9. These assessment tools used IADLs to help determine elderly or disabled persons' abilities to perform traditional tasks, including answering a telephone, shopping, food preparation, housekeeping, laundry, and handling finances. The IADLs used in the CSAT-POP reflect typical activities of rural Guatemalans. Seven culturally specific IADLs were assessed: (i) carrying water from the river to the village; (ii) washing clothes; (iii) gathering wood; (iv) taking care of children; (v) walking more than 30 min without rest; (vi) preparing food; and (vii) vigorous activities (running, carrying heavy loads, climbing). Determining which IADLs to evaluate was based on previous observations of rural Guatemalan life. A Likert scale was used to determine a patient's ability to perform daily activities. The scale consisted of: 1=Need no help; 2=Need some help; and 3=Unable to do at all. If the patient did not perform an activity, a score of zero was given for not applicable.
An on-site interpreter orally translated the CSAT-POP into Spanish and Quiché. This was essential because many of the patients were illiterate. The Institutional Review Board at The George Washington University School of Medicine and Health Sciences approved the assessment tool. In Guatemala, Clinica Ezell did not have an institutional structure to approve the assessment tool; however, the director of the clinic did give verbal permission to allow administration of the survey to patients. Patients gave oral consent to study participation.
Demographics
The mean age of the patient population was 49.2 ± 28 years. All patients were of Mayan descent and lived in rural Guatemala. The median parity was 6.8 years (range 1-11). The total number of births in our study population was 125. The average age of delivery was 25 years (range 17-43 years). Of the births, 71.2% occurred in the home, while 28.8% occurred at a hospital or medical facility. The gynecologic diagnoses of the study population (Table 1), and types of surgeries performed (Table 2) are provided.
Table 1: Gynecologic diagnoses of study population
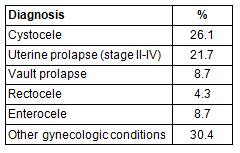
Table 2: Surgical procedures performed
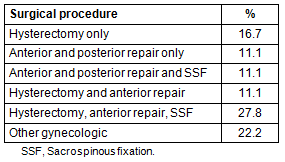
Culturally specific instrumental activities of daily living
In discussing their daily lives, our study population reported making tortillas, walking to rivers to collect water, using outside bathroom facilities, washing clothes, selling food such as sugar and bread, taking care of children, and walking as their primary form of transportation.
The CSAT-POP survey found the entire study population washed clothes, walked more than 30 min without rest, and prepared food on a daily basis. A majority of the study population did not gather wood daily; instead they stated that their husbands or children collected the wood (Fig1).
In assessing ability to perform IADLs with pelvic organ prolapse, participants reported needing the least amount of help with preparing food (84% required no help), washing clothes, and caring for children. The culturally specific IADLs that participants needed the most help with included performing vigorous activities, gathering wood, and carrying water, and 15-20% of the study population was unable to perform these activities on a daily basis. The IADL that the highest percentage of study participants reported being unable to perform was vigorous activity (Table 3; Fig1).
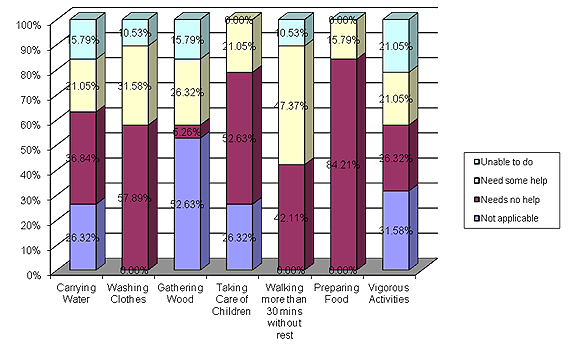
Figure 1: Pre-operative ability to perform culturally specific Instrumental Activities of Daily Living (IADL).
Table 3: Study participants' ability to perform culturally specific activities of daily living
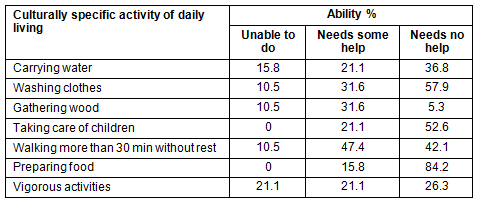
Discussion
The Guatemalan study population overall was multiparous and performed physically demanding activities on a daily basis. The CSAT-POP showed that study participants suffering from pelvic organ prolapse had difficulty walking long distances, carrying water, and engaging in vigorous activities. The survey also found that pelvic organ prolapse did not affect participants' ability to prepare food, the IADL that requires the least amount of physical force.
Limitations
The major limitations of this study are the patients' recall of their ability to perform activities, language barriers, and the small study population. To minimize recall bias participants were only asked to reflect on activities they performed daily in the past 3 months. Asking them about their daily routines also helped with recall. With respect to communication barriers, the CSAT-POP survey was directly translated into Spanish, which all but one of the participants spoke. However, the survey was not validated by an English version, and it is possible there was some misunderstanding with regard to our questioning. To minimize miscommunication, two qualified professional medical translators fluent in both Spanish and Quiché conducted the survey. Finally, the study population consisted of only 19 women. The study population was restricted by both the amount of time the researchers had in Guatemala, and that the patients were recruited by Health Talents International. Nevertheless, the authors believe that the women surveyed generally reflect the indigenous population of Guatemala because they shared parity and birth experiences, according to the data obtained. However, because the location of the clinic was in a mountainous region, it was not clear whether the daily activities of these women were more vigorous than those of the general Guatemalan population, potentially resulting in a greater burden of disease.
Conclusion
The CSAT-POP survey is the first to examine how pelvic organ prolapse affects culturally specific activities in rural Guatemalan women. While specific to Guatemala, the authors believe that the survey tool can be applied to a larger population, especially populations in other developing nations to allow for culturally specific evaluation of disease.
Understanding the burdens of disease in a cultural context allows physicians to better treat patients. In the case of Mayan women in rural Guatemala, the CSAT-POP allowed for better assessment of the effect of pelvic floor disorders on women's ability to perform daily activities. The survey will continue to be used by physicians in Guatemala when assessing patients for gynecologic surgery in future medical missions sponsored by Health Talents International.
References
1. Wein A, Kavoussi L, Novick A, Partin A, Peters C. Campbell-Walsh Urology, 6th edn. Philadelphia, PA: Saunders Elsvier, 2007.
2. Hendrix SL, Clark A, Nygaard I, Aragaki A, Barnabei V, McTiernan A. Pelvic Organ Prolapse in the Women's Health Initiative: gravity and gravidity. American Journal of Obstetrics and Gynecology 2002; 186(6): 1169-1166.
3. Rogers RG, Coates KW, Kammere-Doak D, Khalsa S, Qualls C. A short form of the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire (PISQ-12). International Urogynecology Journal and Pelvic Floor Dysfunction 2003; 14(3): 164-168.
4. Romero A, Hardart A, Kobak W, Qualls C, Rogers R. Validation of a Spanish version of the Pelvic Organ Prolapse Incontinence Sexual Questionnaire. Obstetrics and Gynecology 2003; 102(5Pt1): 1000-1005.
5. The World Bank. Guatemala Data Profile. World Development Indicators Database. (Online) 2007. Available: http://web.worldbank.org (Accessed 9 February 2011).
6. Central Intelligence Agency. The World Fact Book: Guatemala. (Online) 2007. Available: https://www.cia.gov/library/publications/the-world-factbook/geos/gt.html (Accessed 19 June 2007).
7. Bump RC, Mattiasson A, Bo K. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. American Journal of Obstetrics and Gynecology 1996; 175: 10-17.
8. Barber M, Kuchibhatla M, Pieper C, Bump R. Psychometric evaluation of 2 comprehensive condition-specific quality of life instruments for women with pelvic floor disorders. American Journal of Obstetrics and Gynecology 2001; 185(6): 1388-1395.
9. Lawton MP, Brody EM. Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist 1969; 9: 179-186.
_______________________
Appendix I: Culturally Specific Assessment Tool for Pelvic Organ Prolapse, Clinic Ezell, Guatemala

