Paralysis agitans or Parkinson's disease (PD) is a significant neurological condition and the most common neurodegenerative disorder after Alzheimer's disease1-4. It can contribute to or coexist with dementia and other neurodegenerative conditions. Presentation varies among differing ethnicities and geographic locations and may also be due to exposure to certain chemicals4. Men have a greater incidence and prevalence of PD worldwide. In Australia, males represent 51% of the PD population2.
At the request of Parkinson's Australia, Access Economics researched the prevalence, cost and burden of PD in Australia2. The review discussed the difficulty of estimating PD prevalence in Australia because no community two-phase studies have occurred (screening followed by detailed medical examination to confirm diagnosis)2. In 2005 Access Economics estimated the Australian PD prevalence in to be 54 700 (265 per 100 000), with a further 15 000 cases undiagnosed. On the basis of the number of PD medication prescriptions that estimation was believed to be conservative2. The 2005 incidence was estimated to be 8900 cases by analysing prevalence data, remission and risk of mortality data. The report cited that 18% of known cases were in those under 65 years and that the prevalence of PD was expected to rise2. Peters et al used a three-step algorithm to examine GP estimation of patients with idiopathic PD and estimated the prevalence to be 145 per 100 000 in Queensland, Australia5. They cited McCann et al who estimated the prevalence of PD in the rural town of Nambour on Queensland's Sunshine Coast to be 415 per 100 0006. Both Access Economics and Peters et al highlighted the difficulty of making an accurate estimation of prevalence and noted a paucity of studies.
Parknison's disease has a strong genetic link, yet other risks including environmental factors such as exposure to heavy metals and pesticides are suggested to influence the onset7. Both European3 and Australian5 meta-analyses concluded that rural living is a statistically significant risk factor. Factors linking PD with rurality include the use of pesticides, herbicides and transition metal exposure (in agricultural and mining practices)3,7 where neurotoxity theories are espoused. Stress and the use of bore (groundwater) and well water are also noted in rural areas. Whether rural living itself increases exposure to other unknown neurotoxins or whether urban living is protective is yet to be established. Paradoxically, smoking and caffeine ingestion have exhibited protective characteristics for PD3,7-9. A risk factor summary is provided (Table 1).
Table 1: Major environmental risk factors for Parkinson's disease
(adapted from Pankratz and Faroud; and Access Economics2,10)

Literature review reveals a dearth of Australian publications that outline the specific problems of People with Parkinson's (PWP) in rural and regional (RR) Australia. The greater density of neurologists in metropolitan areas highlights the relative disadvantage of PWP in RR areas because of its greater rural incidence. The impact of limited facilities and access to medical and allied health professionals (AHP) is yet to be fully explored, especially with respect to the ready availability of pharmacological and non-pharmacological treatment options. It is theorized that such limitations hinder diagnosis and the management of PWP in RR areas, especially in the early stages of the disease. The Parkinson's Australia 2008-2009 Federal budget submission emphasised this, and a major recommendation was to improve the plight of PWP in rural and remote areas and to assess the availability of rural neurologists11.
Some epidemiological studies have been conducted in Australia5,12-15 and significant to the present study is a 2005 state-wide postal/telephone survey of GPs examining the incidence and prevalence of PD, in both rural and metropolitan areas5. Peters et al found that Australian GPs in metropolitan areas had greater access to and support from neurologists. This study also showed a substantial portion of PWP relied solely on their GP for support, and approximately 90% of surveyed GPs stressed the need for postgraduate training in neurodegenerative disorders5.
While there is no cure for PD, the largest hurdle in PD management in Australia is in establishing multidisciplinary care teams for functional management of the condition2. This is also significant in rural Australia with its well-recognized deficiency of some AHP, as well as medical practitioners.
Literature review
Literature was sourced through MEDLINE, EMBASE, MEDITEXT and Google Scholar databases for the time period 1990-2009. Clinical Information Access Program (CIAP), Australian Institute of Health and Welfare and NSW Department of Health websites, the Australasian Journal of Neuroscience, Australian Doctor and the Australian Journal of Rural Health were also searched manually for relevant articles. Articles on rurality and regional healthcare delivery relating to PD, particularly in the Australian literature, were also reviewed.
Key search words included:
- Parkinson's
- rural; regional; remote; Australia
- incidence; prevalence
- intervention; risk factors
- healthcare; allied health; treatment; general practice.
Participant recruitment
Three pamphlets were produced, designed to advertise the project to PWP, carers and rural GPs. The pamphlets gave information about the purpose of the study and what was involved in being a participant. In addition, two advertisements were placed in the local newspaper inviting the participation of AHP and the telephone book was searched for AHP contact details for personal invitation. Pamphlets were distributed to GPs through the Riverina Division of General Practice newsletter.
Ethics approval allowed access to the database of the Wagga Wagga Parkinson Support Group (WWPSG) after written approval from the President, and the researchers were able to send personal letters of invitation with the pamphlets. Preliminary talks were also given to three meetings of the WWPSG. The WWPSG also distributed pamphlets to their members at meetings and via mailed newsletters.
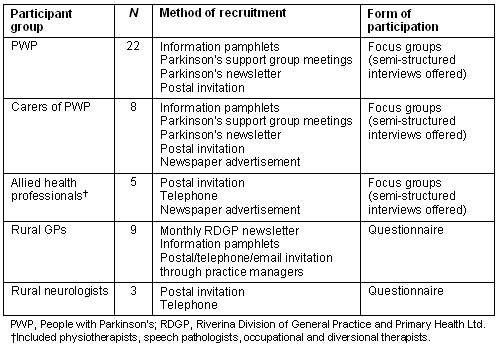
Participants were able to choose either focus group participation or questionnaire response, according to their availability and preference. The 47 participants recruited represented five groups: PWP, their carers, AHP, rural GPs and rural neurologists (Table 2).
Table 2: Recruitment and participation type of participant groups
Data collection
Focus groups: A separate set of focus group questions were designed for each of the non-medical groups (PWP, carers and AHP). Each set contained 7 questions (8 for carers):
- People with Parkinson's: questions covered diagnosis, problems with medication, frequency of medical visits, roles of GPs and neurologists, interaction with AHP and available supports. The question set for PD participants contained four prompts for each question in order to obtain maximum information.
- Carers: carers were asked to describe their role in caring for their PWP and to describe major obstacles and difficulties. Their input was sought on problems related to current treatment strategies and on what they found to be most and least effective. Information about available supports was also sought, as well as what they would like to see done about management of PD in the local community.
- Allied health professionals: the allied health focus group was asked similar questions to those for the carers group.
Focus group discussion was recorded and notes were taken by the researcher. All participants were asked to sign a consent form granting permission for the recording at the commencement of each session. They were also given a revocation form to use if they later wished the recording to be destroyed.
Following data collection, qualitative methods were used to analyse each group's responses by categorising responses into themes.
Questionnaire: A separate questionnaire was designed for the neurologists and GPs invited to be part of the research. This questionnaire combined Yes/No tick boxes, rating scales and space for free comment. The GPs' and neurologists' questionnaires consisted of 9 and 11 questions, respectively. The GP questionnaire enquired about contact with PD patients, confidence in diagnosis and management, problems encountered and knowledge of allied health service supports (Fig1); and the neurologist questionnaire enquired about numbers of PD patients seen, issues encountered, modes of treatment, impact of rural shortages of neurologists and their awareness of the financial burden to PD patients (Fig2). The neurologists were also asked to comments on issues that needed addressing in local communities for PD sufferers.

Figure 1: Example: Q5. GP questionnaire

Figure 2: Example: Q4. Neurologist questionnaire
People with Parkinson's groups
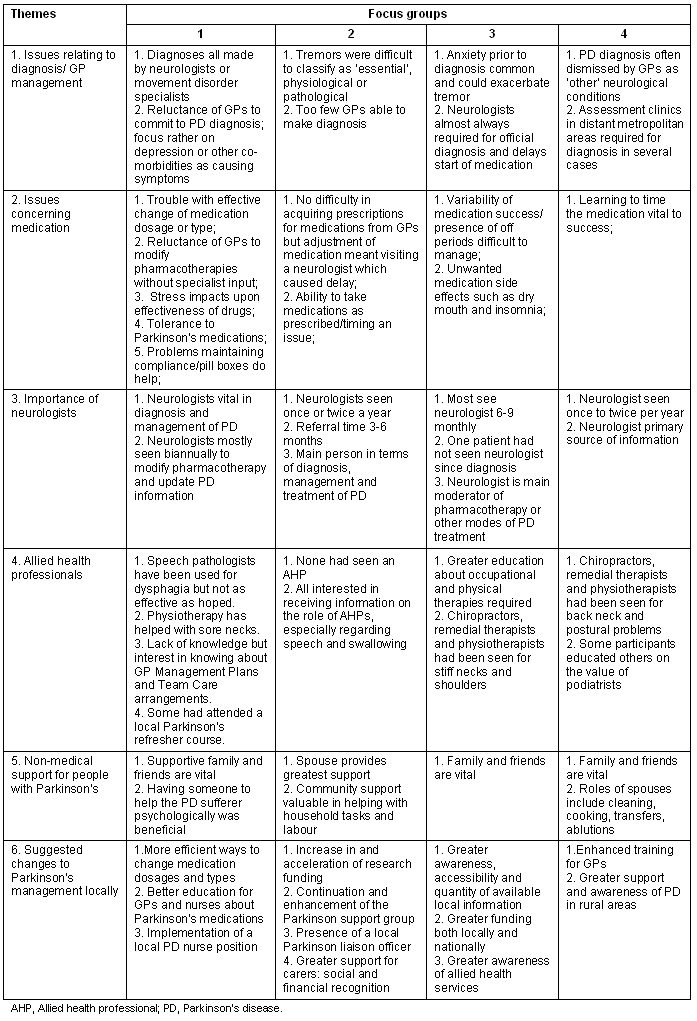
Four focus groups of PWP were conducted. It was also the researchers' perception that the PWP and carers' focus groups often served to enhance education for participants as they learnt from others' experiences. The theme areas from the PWP group are discussed and summarised (Table 3), with questions asked about diagnosis and medication, frequency of medical visits, the roles of GPs and neurologists, interaction with AHP and available supports.
Diagnosis: As expected, most PWP participants reported a resting tremor as the first or most distinguishable symptom preceding diagnosis, and this was often the catalyst for seeking medical help. However, there were a considerable number of participants who complained of irregular balance, shuffle or one-sided sway (with one upper or lower limb not compliant with total body movement) prior to diagnosis.
A substantial number of participants noted loss of smell (and to a lesser extent, taste) as a significant event in their disease progression which could precede PD diagnosis by several years. The literature review included current studies investigating role of dopamine secreting cells and their proximity to and influence on olfactory centres16-18. Stem cell studies for PD are investigating the potential benefits of olfactory cells16.
Neurologists were almost always the medical professional who made the initial the diagnosis of PD and many of the PWP participants had been referred to neurology clinics in Sydney (the state capital) for this reason.
Medication issues: Two issues arose:
- The precise timing of PD medication was problematic, especially during a hospital admission or in nursing homes because staff appeared to not understand the importance of exact dosing times for this condition.
- While rural GPs willingly provided prescriptions, they seemed reluctant to adjust medication doses. Hence, dosage manipulation was often delayed by 6 to 12 months while PWP waited for a neurologist's appointment.
Role of the general practitioner: The PWP focus groups related disappointing experiences regarding GPs' knowledge and awareness of the disease. Some PWP reported frustration after a consultation, having self-diagnosed PD but finding the GP ignored this as a potential diagnosis. They felt diagnoses were delayed due to clinicians' inability to recognise the symptom set. Ultimately the GP role involved writing prescriptions and providing referrals to specialists and other health professionals. While the PWP would prefer the GP to manage their PD in greater depth, they recognised the demands of rural general practice. Further training and refresher courses were suggested to assist GPs to deal with patients with PD.
Importance of the neurologist: The regional study area had only one neurologist, with two others 90 min drive to the south and six in Canberra, 3 hours to the east. The local neurologist was invariably the one who modified pharmacotherapy type and dosage and provided the most up-to-date PD information for patients and carers. This meant that delays of 6 to 12 months were common for patients requiring definitive management changes.
Role of allied health professionals: The AHPs most frequently visited were physical, speech and occupational therapists, with chiropractors and remedial therapists also utilized for 'sore backs' and 'stiff necks'. While physiotherapists were consulted for a wide range of motor disturbances, dysphagia was the most common reason for visiting speech pathologists. Occupational therapists, often working in conjunction with physiotherapists, dealt with the impact of PD motor disturbances at home and work. Considerable variability in the knowledge of AHPs and their roles in treatment was noted in the PWP focus groups.
Supports required and issues to be addressed: The PWP received most support from family and friends. Few received any community supports.
Participants alluded to loss of earnings and the need to travel for medical diagnosis and treatment as impacting negatively on their financial situation. Access Economics found that the financial burden of PD over a lifetime is comparable with that of cancer2. The longer one has PD, the greater the financial demands with implicitly less income from work2.
All PWP focus groups requested greater funding for research. As well refresher neurological courses suggested for GPs and AHP, a regional Parkinson's specialist nurse and/or Parkinson's liaison officer was regarded as a high priority need.
Table 3: Summary: People with Parkinson's focus groups regarding medical and allied health roles in Parkinson's disease
Carers group
Carers were asked to describe their role in caring for their person with PD and to describe the major difficulties and current treatment strategies most and least effective. Input was also sought about available supports and improvements to the management of PD in the local community.
Roles of carers: Carers, most often spouses, were responsible for household chores and assisting the PWP with activities of daily living such as cooking, using knives (anecdotally reported to be dangerous at times), cleaning, washing (particularly hanging clothes to dry), ablutions and mobility. Preventing falls and accidents due to motor disturbances was an important carer role that pervaded all other activities.
Major problems in dealing with people with Parkinson's: Carers reported that despite the physical demands of care, their greatest difficulty was dealing with the psychological changes of PD. Symptoms such as depression and social withdrawal quickly became more debilitating than the physical symptoms and impacted significantly on the carer, placing stress on the spousal relationship. One carer who had previously been a nurse said that what was expected of carers was overwhelming, stating 'Nothing prepared me for this'. There was consensus among carers of having experienced 'being thrown in the deep end' and also their sense of carrying an 'immense responsibility'. They also reflected profound fear of the unknown for their PWP and a loss of trust in others. They empathised with their PWP's frustration due to loss of mobility and noted this to be worse in 'off periods'. Carers stated that maintenance of a routine was important because their PWP became easily distressed when routine was disrupted. Consequently carers' ability for spontaneity (eg meeting friends for coffee) was reduced.
Issues surrounding treatment of Parkinson's disease locally: There was general consensus on the lack of understanding and public awareness of PD, particularly in RR areas. Carers felt that more publicity was needed due to the higher PD incidence in this population. Vigorous support was given for the concept of a specialist Parkinson's nurse in the region, a Parkinson's liaison officer, or preferably both.
Recommendations from carers about Parkinson's disease management: Carers were adamant that there was an urgent need for readily available respite facilities. While many in this group were aware of respite opportunities from home-care nurses locally, there was a demonstrated need for greatly increased respite services. They also noted that if GPs could coordinate a multidisciplinary approach to help manage the PWP, then this would greatly reduce the responsibility carried by the carer.
Allied health professionals group
The AHP group were asked about the AHP role, interventions and future directions.
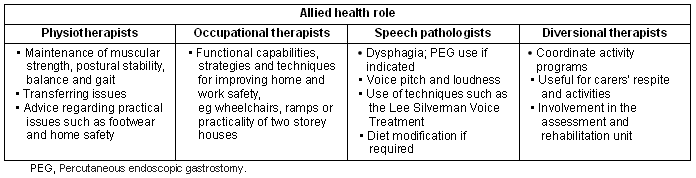
Roles of allied health professionals: AHPs stressed that all disciplines could help enhance and consolidate the functional capabilities of PWP. There was unanimous agreement that the greatest problem in allied health management of RR PWP was the lack of early referrals. The National Institute for Health and Clinical Excellence (NICE) clinical guidelines for PD outlines several benefits of allied health services19, validating the with AHPs' discussion. The AHP focus group discussion is summarized (Table 4).
Table 4: Role perspective of allied health therapists
Allied health professionals emphasised that PWP living in RR communities were not aware or adequately educated regarding the potential benefits of allied health interventions, particularly if implemented early in the disease. This was believed to be due to insufficient PD referrals from all health professionals, the absence of some services locally, the non-existence of a PD coordinator and/or liaison officer, and the geographic distance between health providers. The PWP focus groups also highlighted lack of awareness of the range of services offered by AHP and referral options in GP management plans.
Successful techniques for dealing with people with Parkinson's regionally: Allied health professionals emphasised that while pharmacological intervention is necessary in PD, it overshadowed the benefits of other treatment modalities, especially with early referral. All allied health disciplines involved in the present investigation agreed that while biomechanical and physical approaches are useful, their efficacy is enhanced by a cognitive behavioural approach that requires PWP to set their own goals for self-motivated change.
The Access Economics' Report suggested that team-based approaches are vital in PD management2. This approach was particularly validated in the focus group attended by members of the Aged Care Assessment Team (ACAT).
Allied health and Parkinson's disease in the future: A number of practical recommendations were made by AHPs, including the development of a regional Parkinson's clinic and/or PD service coordinator. One participant said that a proposal for such a clinic (in approximately 2005) had been rejected due to the lack of funds available. It was suggested that a monthly clinic could operate within the local ACAT facilities offering attending PWP a variety of appointments and assessments in a single visit. A database of PD patients could be formulated from PWP who attended the clinic to monitor local data and disease progression more efficiently.
Other recommendations included a greater focus on a team-centred approach and earlier assessment and intervention by AHP. Mapping of suitable local services for PWP and their carers was also suggested.
Rural general practitioners
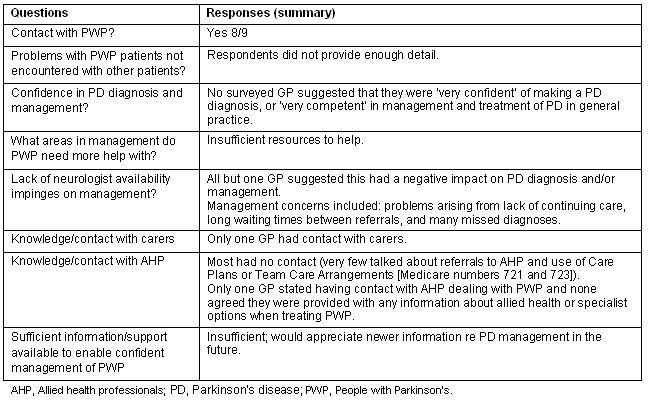
The Riverina Division of General Practice and Primary Health Ltd (RDGP) provided the contact details of area practices for mailing out GP questionnaires. Although all RDGP identified practices were contacted by phone, postal mail, email, in person, or a combination of these methods, and on more than one occasion, the response rate among GPs was low (n = 9, <20%), as had been anticipated20. A broad summary of the small return of questionnaires is provided (Table 5). It is of interest that Buetow et al's random sample of 500 PD patients in New Zealand found that GPs had too limited information on the perceived needs of PD patients and did not involve the patient21. Similarly Peters et al found that more than 50% of GPs surveyed were not confident in treating the disease5.
Table 5: Findings from rural GP questionnaire
Rural neurologists
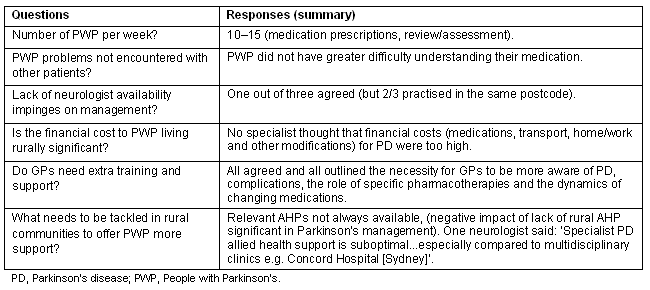
All three full-time neurologists based in the GSAHS region replied to the questionnaire regarding the delivery of health care to PWP. All stated they saw 11-15 PWP per week, mainly for pharmacological prescription, review and assessment. Referrals for various forms of therapy, especially speech and physical modalities, was the second most often reported specialist activity with PD patients. The neurologists scored the 5 closed questions in Item 4 of the questionnaire similarly (Table 6).
Table 6: Findings from rural neurologist questionnaire
Limitations
The largest group of respondents was PWP (28/49, 57%), and Kitzinger suggests that this is inevitable because such a group has a vested interest in the study22. The PWP database used (WWPSG) included all people in local and surrounding areas known to have a diagnosis of PD, even those not attending meetings or receiving monthly newsletters. This sampling method may have missed some potential participants.
In addition, the PWP group had a vested interest in the project and this could have influenced some findings. Morgan said that in a qualitative process such groups are not only more likely to participate, but also to participate in discussion23. Further, PWP who had more adequate transportation or support were more likely to have attended the focus groups. The average age of those in PWP focus groups was well over 60 years (although some had been diagnosed in their 40s), so group homogeneity may have resulted in a lack of diversity in responses22-24.
However this study aimed for an in-depth understanding of the experience of PWP and those caring for and treating them. The researchers aimed to find such people within the study area and time-frame (24 weeks), and Greenhalgh and Taylor25 confirm this to be a reasonable approach.
General practitioner participation was not expected to be high20 (anecdotally reported through general practice managers) and attempts to increase GP participation were unsuccessful. The RDGP newsletter limited publicised recruitment to one issue, although the researchers requested greater exposure. Direct phone calls to practice managers did not increase the response rate significantly.
It also would have been of value to approach the further six neurologists 3 hours to the east of the town to broaden responses, but this was not possible due to time restraints.
This study provides a microcosmic view of the issues revealed by the literature available on RR Australia's healthcare delivery to PWP and their carers. It highlighted a lack of health staff, funding and information for relevant stakeholders, as well as the PWP' desire for increased input from GPs and the ancillary sector.
While the investigation did not directly compare RR with metropolitan Parkinson's delivery, it was inferred from participant groups that regional areas are less well equipped in terms of medical staff and facilities, and that this hinders efficient PD diagnosis, management and treatment.
The findings have relevant implications for various Parkinson stakeholders, whose knowledge of local available services was surprisingly limited, with a few exceptions. The investigation noted the desire of all participant groups to have a PD liaison officer in the region, to act as an intermediary between PWP, their carers and allied and medical health providers.
The authors urge future research into PD in Australia to help develop practical resources for PWP and their carers.
Finally, the authors received feedback from the CEO of Parkinson's New South Wales who provided comments from the audience to a poster presentation at The Parkinson's Australia Conference 2008, including:
I have had Parkinson's disease for over 12 years and have not had a full understanding of PD as I live in the country [a rural area] and this information is not available to us. I leave here today with a lot more knowledge and understanding.
Acknowledgements
The authors appreciate the Wagga Wagga Parkinson's Support Group for local PD data. They also thank Parkinson's Australia for the grant that allowed attendance at the National Australian Parkinson's Conference. The authors also thank the University of New South Wales for the opportunity to undertake this study as part of an independent learning project.
References
1. Burch D, Sheerin F. Parkinson's disease. Lancet 2005; 365: 622-627.
2. Access Economics for Parkinson's Australia. Living with Parkinson's disease; challenges and positive steps for the future. (Online) 2007. Available: http://www.parkinsonsnsw.org.au/assets/attachments/documents/AE-Report_2011.pdf (Accessed 11 June 2008).
3. Dick FD, De Palma G, Ahmadi A, Scott NW, Prescott GJ, Bennett J et al, for the Geoparkinson Study Group. Environmental risk factors for Parkinson's disease and parkinsonism: the Geoparkinson study. Occupational and Environmental Medicine 2007; 64: 666-672.
4. De Lau LML, Schipper CMA, Hofman A, Koudstaal PJ, Breteler MMB. Prognosis of Parkinson Disease. Archives of Neurology 2005; 62: 1265-1269.
5. Peters CM, Gartner CEL, Traficante R, Reid WGJ, O'Sullivan DJ, Williamson PM. The Sydney multicentre study of Parkinson's disease: progression and mortality at 10 years. Journal of Neurology, Neurosurgery and Psychiatry 1999; 67: 300-307.
6. McCann SJ, Le Couteur DG, Green AC, Brayne C, Johnson AG, Chan D et al. The epidemiology of Parkinson's Disease in an Australian population. Neurobiology 1998; 17: 310-317.
7. Couteur DG, McLean AJ, Taylor MC, Woodham BL, Board PG. Pesticides and Parkinson's disease. Biomedicine & Pharmacotherapy 1999; 53: 122-130.
8. Galvan A, Wichmann T. Pathophysiology of Parkinsonism. Clinical Neurophysiology 2008; 119(7): 1459-1474.
9. Pankratz N, Foroud T. Genetics of Parkinson disease. Genetics 2007; 9(12): 801-811.
10. Pankratz N, Foroud T. Genetics of Parkinson disease. Genetics 2007; 9(12): 801-811.
11. Parkinson's Australia. Federal Budget Submission. (Online) 2008. Available: www.parkinsons.org.au (Accessed 2 February 2009).
12. Mehta P, Kifley A, Wang JJ, Rochtchina P, Sue CM. Population Prevalence and incidence of Parkinson's disease in an Australian community. Internal Medicine Journal 2007; 37: 812-814.
13. Chan DK, Cordato D, Karr M, Ong B, Lei H, Liu et al. Prevalence of Parkinson's disease in Sydney. Acta Neurologica Scandinavica 2005; 111: 7-11.
14. Hely MA, Morris JGL, Traficante R, Reid WGJ, O'Sullivan DJ, Williamson PM. The Sydney multicentre study of Parkinson's disease: progression and mortality at 10 years. Journal of Neurology, Neurosurgery and Psychiatry 1999; 67: 300-307.
15. Reider CR, Hubble JP. Test-retest reliability of an epidemiological instrument for Parkinson's disease. Journal of Clinical Epidemiology 2000; 53: 863-865.
16. Murrell W, Wetzig A, Donnellan M, Fe'ron F, Burne T, Meedeniya A et al. Olfactory mucosa is a potential source for autologous stem cell therapy for Parkinson's disease. Stem Cells 2008; 26(8): 2183-2192.
17. Doty RL, Stern MB, Pfeiffer C, Gollomp SM, Hurtig HI. Bilateral olfactory dysfunction in early stage treated and untreated idiopathic Parkinson's disease. Journal of Neurology, Neurosurgery, and Psychiatry 1992; 55: 138-142.
18. Stefano K, Pagano F, Impagnatiello F, Girelli M, Cova L, Grioni E et al. Isolation and Characterization of Neural Stem Cells from the Adult Human Olfactory Bulb. Stem Cells 2000; 18(4): 295-300.
19. The National Institute for Health and Clinical Excellence. CG35 Parkinson's disease: NICE guideline. (Online) 2006. Available: http://www.nice.org.uk/Guidance/CG35/NiceGuidance/pdf/English (Accessed 8 October 2008).
20. Barclay S, Todd C, Finlay I, Grande G, Wyatt P. Not another questionnaire! Maximizing the response rate, predicting non-response and assessing non-response bias in postal questionnaire studies of GPs. Family Practice 2002; 19: 105-111.
21. Buetow S, Giddings LS, Williams L, Nayar S. Perceived unmet needs for health care among Parkinson's Society of New Zealand members with Parkinson's Disease. Parkinsonism and Related Disorders 2008; 14(6): 495-500.
22. Kitzinger J. Introducing Focus Groups. BMJ 1995; 311: 299-302.
23. Morgan DL. Focus groups as qualitative research (2nd edn). London: Sage,1997.
24. Kitzinger J. The methodology of focus groups: the importance of interaction between research participants. Sociology of Health and Illness 1994; 16(1): 103-121.
25. Greenhalgh T, Taylor R. How to read a paper: Papers that can go beyond numbers (qualitative research). BMJ 1997; 315: 740-743.
