Unpaid carers play an important role in society, and their contribution is becoming increasingly critical as a result of population ageing, predominantly in terms of the very old who are more likely to require care1. However, care provision is particularly problematic in rural areas, which generally have a higher ratio of older people than urban areas1-3. In addition to having a larger proportion of people needing care, rural areas are compromised by having fewer people of working age to provide care and support to older people1, as well as a shortage of viable residential care facilities4. As a result, older people in rural areas are more likely to be required to provide care to ageing partners and other family members.
As the number of older carers in rural areas increases, so too does their likelihood of experiencing social isolation, as there is a strong association between being a carer and being socially isolated in later life5. Being involved in caring responsibilities can result in the loss of social networks6, and for older carers this is exacerbated by factors associated with ageing, such as loss of paid work, relocation of family, and health and mobility issues7-10. Again, these issues are intensified in rural areas, where connections with other carers and support services are limited11,12.
A recent Australian government inquiry has highlighted the issue of social isolation among carers, recommending that this issue be an early priority for the newly established Australian Social Inclusion Board13. This inquiry resulted in the inception of a National Carer Recognition Framework, which is currently being developed in conjunction with local governments, carers and service providers, and will fill a major Australian policy gap. In particular, social isolation is a serious problem in an ageing population, because evidence suggests it can lead to poor health, depression, withdrawal, and a loss of self-esteem and confidence14. For carers, there are additional issues, with social isolation said to increase perceived caregiver burden15, and potentially lead to abuse of the care recipient16. Conversely, social networks can alleviate the stresses of caring17, and provide emotional comfort, release and understanding18. This highlights the critical importance of addressing the risks of social isolation associated with being an older carer, particularly for those living in rural areas.
In recognition of the significance of this problem, an increasing number of programs and interventions are being implemented internationally to address the issue. Some are designed to meet the needs of specific population groups, or to respond to a particular barrier or risk factor. These include face-to-face, individual or group programs, as well as those conducted via virtual means, such as the telephone or internet. The intention of this article is to explore these models and, in doing so, to identify the features of effective interventions. As such, the article aims to provide a particular framework for program planners to help build effective intervention models that best reduce social isolation and increase support for older, rural carers. It also aims to highlight the implications of these findings in terms of health and social policy relating to carers.
A literature review was undertaken using three approaches: (i) a search of peer reviewed journal articles located in online databases that included Informit (Rural Health, Health and Society, Family, APAIS, AMI), Ovid (AMED, Embase, Medline, PsycINFO), Proquest Health and Social Science, CSA Sociological and Social Science Abstracts, CINAHL and Expanded Academic ASAP; (ii) a search of selected government and research-based websites, both Australian and international; and (iii) an internet search using Google Scholar, used to locate 'grey literature' in the form of unpublished reports. Searches were limited to material published between 1999 and 2009, and keywords utilised both cumulatively and in isolation included carer/caregiver, rural, old/older, ageing, social exclusion/isolation/inclusion, support groups, support programs, social support, and models of care.
From the searches, 67 articles, book chapters and reports were identified and included in this review on the basis that they either examined barriers to social participation for rural and older people, or evaluated interventions which addressed social isolation and/or had a social component. Literature that did not meet one of these criteria was excluded from the review. The literature examined included review articles, program evaluations, small-scale qualitative and larger scale quantitative studies, which were carefully evaluated by the authors prior to inclusion to ensure that methods of evaluation, particularly in the case of unpublished reports, were academically rigorous. Due to the limited range of programs for rural older populations specifically, interventions trialed on both rural and older carers were reviewed.
Results and Discussion
The review is conducted in two sections. First, the literature in relation to the barriers to social participation for older and rural carers is explored in order to provide an understanding of the factors that result in social isolation among this group. The second section presents and analyses the features of effective models contributing to reduced social isolation.
Barriers to social participation for older rural carers
The literature highlights a range of barriers inhibiting social participation among older carers, which are exacerbated by residing in a rural area. First, older carers have limited time and motivation to maintain or create social networks, because they are often fully involved in their care activities and lack time to socialize, particularly if the dependency of the care recipient increases over time3,16. Thus, older carers may decide that available activities are simply not worth the time investment and cost16. Further, activities may not be appropriate to the needs of carers, particularly those who have different cultural values or beliefs from the majority, and this may be a particular barrier for those from CALD (culturally and linguistically diverse) backgrounds6,19.
Second, a lack of respite care limits the capacity of older carers to undertake social participation. Australian studies have noted that two-thirds of older carers do not have a substitute informal carer to call on9, and only 50% of older carers utilise respite care16. Low use of respite can be attributed to supply factors, such as poor availability, flexibility or suitability, the cost of care, and limited awareness of what is available16,20,21. It can also be attributed to demand factors, such as older carers choosing not to use respite due to personal or cultural values, the reluctance of the care recipient to enter respite, or previous adverse experiences with the service16,21. Caring may be seen as the responsibility of the family21, and as a result some older people are reluctant to define themselves as carers, particularly those from CALD backgrounds13,19. Accepting help or respite may result in feelings of embarrassment, weakness or guilt; with carers believing that respite time should be spent doing things which will benefit the care recipient16,20,22. Research has identified that for rural older carers, this sense of responsibility influences respite use and is a major contributor to social isolation23.
Third, even if respite is available and the carer wishes to be involved in social activities, there are a number of financial and personal limitations that inhibit social participation among older carers, and the literature highlights a number of issues associated with attending face-to-face support groups for both older and rural carers15,24-26. In terms of general social interaction, cost is a significant barrier, particularly as older carers are more likely to reside in low-income households or be unaware of their eligibility for government allowances6,9. Other practical barriers include reduced mobility, and poor physical and mental health related to caring stress20,27. Simply leaving the house may be seen as difficult, particularly if the care recipient needs to be cared for outside the home22. In addition, those who care for someone with problematic social behavior may fear the stigma that is associated with their interaction in a community setting27.
Many of these issues, such as lack of time or respite, or concerns about costs or stigma, may be even more apparent in a rural setting. Research has shown, for example, that rural carers demonstrate increased financial hardship, poorer health and experience more stressful events than non-carers28,29. In rural areas, geographical isolation, the distances between houses, extreme weather conditions, and limited public transport are more likely to be barriers to social participation12,15. While many rural carers report stronger social networks than those of urban carers29,30, they are less likely to have family support to draw on10,29. This is a significant barrier, because family support is instrumental in ensuring regular social participation for rural older caregivers31. However, even if family support is available, rural carers may be reluctant to rely on family members for fear of being a burden32.
Rural communities can be rich in social capital; however, the insular nature of some of these communities and the reluctance of rural carers to admit they have a problem prevents them from asking for and accepting help, and prevents help from being offered. In rural settings where resilience is valued, receiving help may be viewed as selfish and unnecessary33. Carers in rural areas may also isolate themselves and their care recipients, because of the stigma associated with mental illness33,34. Perceived stigma is also an issue for rural carers in utilising respite services, due to fear that services will be provided by a community member known socially to the carer32,35. Services are particularly difficult to deliver in rural communities, and there may not be the choice of and flexibility in services that exist in more populous regions20,28,36. In some cases, rural carers report better awareness of services and the quality of these services but, for the reasons discussed, this does not mean that they will be utilized30. These issues are compounded by the reluctance of rural people to seek assistance from 'outsiders'34.
Therefore, older carers in rural communities are at significant risk of social isolation, because there are considerable barriers to participating in social activities. While this suggests that there are numerous obstacles to addressing the issue of social isolation among older and rural carers, there are a range of programs and interventions designed to meet the specific needs of these groups. The next section draws on these programs, delivered in both face-to-face and virtual formats, in order to explore how they are designed to meet the social needs of older rural carers.
Six dimensions of effective models
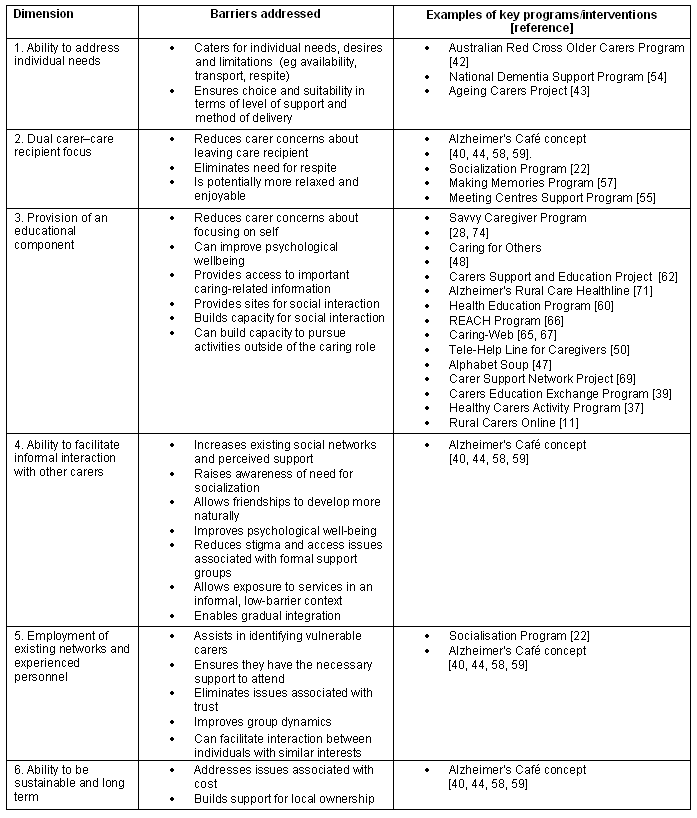
This review has identified a number of barriers to social participation for older rural carers. Guidelines for best practice, therefore, need to consider these barriers, while also identifying approaches to meet the needs of this increasing group. As such, this section highlights six key dimensions that need to underpin any social support program designed to meet the needs of rural older carers. Interventions must address individual needs, incorporate a dual carer-care recipient focus and/or an educational component, facilitate informal social interaction, utilise existing networks and experienced personnel, and be both sustainable and long term. These dimensions, as well as some examples of programs that address these, are presented in Table 1.
Ability to address individual needs: As noted in the literature, effective interventions must cater for the individual needs of carers, in terms of flexibility, frequency and timing37. Thus, in rural areas, fewer meeting times to avoid travel and transport difficulties might be more appropriate38,39, and given the lack of services, programs held on weekends when there are no professional services available may better meet the needs of older, rural carers40. Respite is also important, and needs to be both available and flexible37,41,42. For those new or potentially resistant to the concept of respite, it should be both gradually introduced through transitional arrangements and information sessions, as well as being cost-appropriate and suitable20,43. Given the financial issues that most rural older carers will experience, costs associated with programs need to be low or non-existent. Transport provision has also been identified as critical for face-to-face programs in rural areas, with the provision of paid or volunteer drivers effective in ensuring attendance40,44. Due to the identified problem of stigma and fear of lack of confidentiality associated with living in a small rural community, it may be that carers would prefer to attend programs outside their community; however, this will require additional transport options38,39.
Further, modes of delivery need to recognize the individual needs and preferences of older rural carers. For example, one-on-one support prior to attending group interventions may be required for socially isolated carers22, and virtual interventions and one-on-one volunteer befriending programs can be a first step in this regard45,46. Virtual interventions may be more convenient for older rural carers, because they cater for limited time, financial constraints, mobility issues and geographic isolation11,24,46-50. They also provide anonymity, which may result in a willingness to share personal details not shared in a face-to-face program24,26,46,48. Thus, the benefits of virtual support may need to be explained to rural older caregivers, who may have less experience of these modes of delivery26, and additional training may need to be provided.
The evidence suggests that virtual modes of delivery, particularly via the telephone, can be as effective as face-to-face support groups in providing support and education to rural caregivers24. However, evaluations suggest that the lack of face-to-face contact and the lack of a physical break from caring are a significant problem for older carers25,26,46,51-53. While one study has demonstrated that for 91% of older rural carers, videoconferencing was equally beneficial or nearly as beneficial as face-to-face interaction48, virtual interventions cannot provide physical contact. Thus, even in cases of geographical isolation, opportunities for physical contact should be considered26, because rural older caregivers may not identify travel as an obstacle if physical contact is important to them28.
Thus, multifaceted interventions that incorporate respite, transportation and companionship, and are delivered in both face-to-face and virtual formats, are particularly effective in targeting isolation in rural older carers15,42,43,54. A notable example of this is the Australian Older Carers Program42, which provided assistance to older carers through the development of integrated care plans, respite activities, volunteer support and cost effective brokering arrangements. The success of these interventions was attributed to their capacity to be needs-based and to present a coordinated approach to services and groups54. However, an evaluation of one such program identified that satisfaction levels were significantly lowered in older carers residing in rural areas due to poor availability of respite and reduced competence of program coordinators in these locations42.
Dual carer-care recipient focus: While respite is an integral component of programs targeting social isolation in older rural carers, even if it is available, many carers do not utilise it due to the associated feelings of distrust, guilt, fear or embarrassment. However, respite for carers does not necessarily involve being apart from the care recipient22. This suggests that a dual carer-care recipient focus is important, where both the carer and the care recipient can attend an activity37,43. This is particularly important for spousal carers, because relationship strain is reported when support services distinguish between the carer and the care recipient22. This focus also eliminates the need for respite, and allows the carer to take the care recipient out in a supportive environment without fear of stigma, and helps to build the confidence of the carer22,40,44,55,56.
Older carers may also feel more relaxed and able to socialise knowing that their care recipient is participating in an enjoyable activity21,22, and thus providing enjoyable activities for the care recipient to attend while at the same time running support groups for the carers has proved successful in increasing social support55,57. A noteworthy example of this dual carer-care recipient focus is the 'Alzheimer's café' concept, which has been successfully implemented in both rural and urban areas, and provides a location where carers and care recipients can congregate in a social setting40,44,58,59.
Provision of an educational component: The focus of any program or intervention is important. Certainly focusing on self-care for the carer may be problematic, for the evidence suggests that older rural carers may feel guilt and shame when taking 'time out' for such activities26, which suggests that targeted interventions that focus on the delivery of information and/or education may be better received. Examples of this include the Savvy Caregiver Program28, which provided training for Alzheimer caregivers in regard to self-care, strengthening resources and disease knowledge, and the Caring for Others program48, which sought to address psychological barriers restricting adaptive functioning. These approaches can be beneficial as interventions incorporating an educational, psychoeducational or cognitive-behavioral component can improve psychological wellbeing in older and rural carers15,24,28,48,60,61. This develops both the ability and confidence necessary to make life changes that reduce social isolation, such as increased use of respite and frequency of social interaction62.
Educational or health-based interventions also provide additional benefits in terms of social support, when conducted in a group setting11,15,37,60. Group settings can also be facilitated via virtual means, including educational videoconferences which involve attendance at a central location to take part in a multi-site videoconference47,63. Evaluations of psycho-educational interventions demonstrate positive health and social outcomes for carers, suggesting they are effective in meeting their need for social interaction. One intervention attributes decreased depression in rural older carers to the face-to-face contacts made in the training stage of the study28, and another suggests that psychoeducational interventions and standard support groups score similarly in terms of the wellbeing of older carers64, indicating that it may be the group component that is significant in reducing social isolation. However, apart from providing psychological benefits, the educational component may encourage participation because carers feel that it will benefit the care recipient in some way11, and this is therefore important in motivating them to attend. This was observed from the outcomes of one internet-based intervention targeting older rural caregivers, where over time participants used caregiving information pages less but increased their use of the email component to contact other carers65.
However, while psycho-educational programs are thus very effective, it may be that some older carers may instead value the opportunity to be involved in activities that are not directly focused on their caring responsibilities22,37, and these groups can also provide social benefits. One such example is the Rural Carers Online pilot program, which sought to increase social interaction among rural older carers through training in email and internet usage11. The program evaluation demonstrated broad outcomes that included increased access to social and professional networks, and stronger connections with family and community.
Ability to facilitate informal social interaction with other carers: As noted, programs that enable informal interaction with other carers can develop social networks and friendships, and reduce loneliness51,53,66,67. This can reduce social isolation42,48, and create greater perceived support through identification with a group42,48,63. In this way, social interaction both increases psychological wellbeing and increases both the desire and the capacity to socialise25,50,52. Other positive benefits include greater awareness of the need for self-care68, as well as the provision of new information and perspectives on other carers' experiences with services42,43,69. Carers are more likely to accept information from other carers as credible, and this may give them the needed confidence and knowledge to access these services43,70. Increased awareness and use of services will, in turn, allow more time for socialization.
However, interventions designed to build social interaction need to address the key barriers of access and stigma for rural populations15, and the evidence suggests that this is best achieved through informal environments. Programs such as the Alzheimer's café concept allow friendships to be made more easily, and provide a greater sense of ownership and identification with the group. The ability for gradual integration that these environments provide is also important. In the case of dual focus interventions, carers often attend on their own prior to bringing their care recipient44. The name and location of the intervention are also significant, because older rural men are often uncomfortable with 'support group' terminology because they feel they do not need support31. Similarly, use of the term 'carer' may alienate those who do not identify as carers, and also exclude former carers who are at risk of social isolation due to withdrawal of formal support12. In terms of location, meetings should be held in community facilities so they are not viewed as a medical intervention40,44. However, service providers can be invited to attend groups in an informal capacity, which provides easy access to, and raises awareness of rural services38, assists carers to become familiar with staff, creates trust and provides a form of outreach44. Thus, it may be that special provision for informal contact needs to be made in more targeted formal interventions if these benefits are to be achieved.
Employment of existing networks and experienced personnel: The fifth dimension that needs to be considered in designing effective programs for older rural carers is the consideration of existing social networks and agencies that already have a relationship with the carer, because these can be beneficial in ensuring initial attendance. Existing contacts can assist recruitment by identifying carers, encouraging them to attend interventions and ensuring they have the necessary practical support to do so22,43,45,59,63. This dimension may be particularly appropriate in the rural context, because it can eliminate problems in gaining trust34, promote program credibility50, and encourage carers to try more innovative programs69.
To maximize social interaction, interventions should be facilitated by experienced individuals, who are able to manage differences between individuals attending the group31,38,39,42,48. Furthermore, experienced personnel will be able to introduce carers to other carers with similar interests44, prevent the monopoly of groups by particular individuals38,39, and act as a trusted permanent contact40. Use of an experienced facilitator is particularly important in virtual settings due to the increased demands of group work in these environments, and the emotional impact of the abrupt end to sessions46,69.
Ability to be sustainable and long term: Finally, the issue of sustainability is critical, because while many interventions provide short-term social support, most carers are unable to sustain these networks on a long-term basis40. Thus, interventions need to identify avenues for ongoing social support that can be incorporated into the caring role43. Most of the interventions explored in this review have been short term, with few focusing on long-term outcomes, yet sustainability of programs is critical in terms of continued attendance and applicability. Cost associated with any program is a key issue that can be addressed through the use of volunteers and the donation of time. Resources can also be supplied by the community with, for example, funding gained from community grants38 or by registering a program as a charity40.
In relation to virtual interventions, technical support needs to be provided on an ongoing basis, as studies have noted that older rural carers can experience issues with equipment11,67. Further, the use of recycled computers may assist in keeping costs low11. The issue of internet connections is particularly problematic, because connectivity is often difficult and costly to obtain in rural areas11,71. In the same way, even teleconferencing costs may be prohibitive24,48,69. Thus, when considering the mode of program delivery, while virtual interventions may seem more cost-effective than sending professionals to rural communities, this may not be the case24.
Finally, rurality should be embraced, because living in a rural environment can be advantageous for carers, and may assist in achieving greater sustainability. Rural areas are notable for their community spirit, and positive aspects such as this should be drawn upon to create appropriate and sustainable support for rural areas72. For example, with regard to group-based interventions, a sense of local ownership can be built through creation of a local steering committee38,44. However, there is little research exploring how rurality can alleviate carer burden or how it is beneficial to their wellbeing73. Consideration of these dimensions in future interventions would be highly beneficial for rural older caregivers.
Table 1: Key dimensions of effective programs designed to address social isolation among rural and older carers11,22,28,37,39,40,42-44,47,48,50,54,55,57-60,62,65-67,69,71,74
 Conclusions
Conclusions
This review has identified six key dimensions important in designing interventions aimed at reducing the social isolation of rural older carers. However, there are considerable similarities between the issues experienced by older urban and older rural carers, because the literature suggests that older urban carers are similarly prone to issues associated with transport, perceived social isolation and limited access to respite. However, as a result of geographic location, older rural carers are more likely to experience issues associated with respite provision, particularly relating to availability and suitability, transport and the financial cost of attending services and interventions. Significantly, fears regarding loss of privacy and stigma in small communities may limit service utilisation, and result in the perception that services are not needed. Recent research has demonstrated that urban carers are more likely than rural carers to identify as socially isolated75, which may impact upon service utilisation, but does not necessarily mean that rural carers are not in need of social interaction. Consideration of these issues is integral to addressing social isolation in the rural context for older carers.
Based on the review findings, it is suggested that increasing social participation in rural older carers is a two-stage process. First, the barriers to attending an intervention must be removed. This includes addressing practical and logistical issues, as well as ensuring that the focus of the intervention is relevant to the carer and will attract their interest. The evidence suggests that, regardless of the level of support provided, it is unlikely that rural older carers will attend an intervention unless it has benefits for their care recipient, suggesting that this needs to be at the forefront of any intervention. Second, the intervention must maximize social opportunities, which can be achieved directly by allowing older rural carers to mingle in informal settings. The provision of learning opportunities is important as a focus for the intervention, although the social dimension is critical to achieving long-term outcomes. Effective interventions also include the integration of service providers in an informal capacity, because this can de-stigmatize and raise awareness of other support services. However, given the small scale and pilot nature of many of the interventions reviewed, which is a limitation of this study, there is clearly a need to assess the long-term effects of these interventions regarding continued attendance and applicability, as well as their long-term outcomes. Thus, these findings should be treated with caution in terms of their long term applicability.
In terms of limitations, it also should be recognized that although there is a large published literature outlining these programs, not all programs and models are published in the academic literature, and therefore may not be included in this review. Furthermore, the large majority of published interventions is quantitatively evaluated, and thus fails to capture the subjective views of the carers. There is also a scarcity of qualitative research examining the broad range of associated issues, such as the role of existing social networks, the level of care integration with other social and community groups, and the issues associated with accessing isolated, hidden carers, who are not utilizing services. Input of this nature is integral to developing interventions that reduce social isolation in rural older carers and will be both appropriate and sustainable, and achieve an improved quality of life for an increasingly vulnerable population.
However, this review has highlighted some key issues associated with targeting social isolation in older rural carers and is intended to provide a framework for building effective intervention models. In the Australian context, this has major policy implications, because the Australian Government is currently implementing a National Carer Strategy as part of a National Carer Recognition Framework based on the findings of recent inquiries. This strategy will guide government policies and programs relating to carer supports and services76. However, the inquiry on which this strategy is based13 does not highlight the specific issues faced by older and rural carers in any detail, referring only to an increased need for respite in the rural context. This is significant, because this review has highlighted that there are a number of related issues that will impact upon social interaction for older rural carers which need to be addressed in policy, both from a practical and financial perspective, in terms of delivering relevant and beneficial programs. Overarching policies addressing carers as a general population will not be relevant to all older rural carers, and recommendations need to be carefully considered in terms of how they can be applied successfully in the rural context.
Acknowledgements
The authors acknowledge 'annecto-the people network', who provided funding for the research on which this article is based.
References
1. United Nations. World Population Ageing 2009. New York: UN Department of Economic and Social Affairs, Population Division; 2009.
2. Kinsella K. Urban and rural dimensions of global population ageing: an overview. Journal of Rural Health 2001; 17: 314-22.
3. Australian Institute of Health and Welfare. Older Australia at a glance, 4th edn. Canberra, ACT: AIHW; 2007.
4. Snowball K. Multi-purpose services: a potential solution for rural health and aged care. Australian Journal of Rural Health 1994; 2(4): 37-40.
5. Findlay R. Interventions to reduce social isolation amongst older people: where is the evidence? Ageing & Society 2003; 23: 647-658.
6. Cockram J, Hancock P, Jarvis J. Supporting older carers of people with a disability: an evaluation of a respite care program in Western Australia. Asia Pacific Journal of Health Management 2007; 2(2): 58-62.
7. Social Exclusion Unit. A sure start to later life: ending inequalities for older people. London: Office for the Deputy Prime Minister, 2006.
8. Edwards B, Higgins D, Zmijewski N. The Families Caring for a Person with a Disability study and the social lives of carers. Family Matters 2007; 76: 8-17.
9. Australian Bureau of Statistics. A profile of carers in Australia (4448.0). Canberra, ACT: Australian Bureau of Statistics, 2008.
10. Vecchio N. The use of support systems by informal caregivers: an Australian experience. Australian Journal of Primary Health 2008; 14(3): 27-34.
11. Dow B, Moore K, Scott P, Ratnayeke A, Wise K, Sims J et al. Rural carers online: a feasibility study Australian Journal of Rural Health 2008; 16: 221-225.
12. Ford G. Life after placement: experiences of older rural caregivers after placing a family member into residential care. Rural and Remote Health 8:1030. (Online) 2008. Available: www.rrh.org.au (Accessed 2 September 2009).
13. Commonwealth of Australia. Who cares? Report on the inquiry into better support for carers. Canberra, ACT: Department of Communities, 2009.
14. Owen T. Working with socially isolated older people. British Journal of Community Nursing 2007; 12(3): 115-116.
15. Butler S, Turner W, Kaye L, Ruffin L, Downey R. Depression and caregiver burden among rural elder caregivers. Journal of Gerontological Social Work 2005; 46(1): 47-63.
16. O'Connell B, Bailey S, Walker A. Promoting the health and well being of older carers: a proactive strategy. Australian Health Review 2003; 26(2): 78-86.
17. Milne A, Hatzidimitriadou E, Chryssanthropoulou C, Owen T. Caring in later life: reviewing the role of older carers (Executive Summary). London: Help the Aged, 2007.
18. Watts J, Teitelman J. Achieving a restorative mental break for family caregivers of persons with Alzheimer's disease. Australian Occupational Therapy Journal 2005; 52: 282-292.
19. Liu K, Moyle W, Kellett U. The needs of Chinese-Australian family carers who care for older relatives with diabetes. Geriaction 2009; 27(1): 5-16.
20. Hancock P, Jarvis J, L'Veena T. Barriers to respite: a case study of a sub-group from an older carers program in Western Australia. Australian Journal of Primary Health 2006; 12(2): 113-23.
21. Jeon Y, Brodaty H, O'Neill C, Chesterson J. "Give me a break"- respite care for older carers of mentally ill persons. Scandinavian Journal of Caring Science 2006; 20: 417-426.
22. Hillier M. Rebuilding connections: creating opportunities for socially isolated older Australians. Melbourne, VIC: Brotherhood of St Laurence, 2007.
23. Reed D, Weicherding M. Factors of caregiver isolation in a rural midwest area. Home Health Care Services Quarterly 1999; 17(4): 13-24.
24. Brown R, Pain K, Berwald C, Hirschi P. Distance education and caregiver support groups: comparison of traditional and telephone groups. Journal of Head Trauma Rehabilitation 1999; 14(3): 257-268.
25. Smith T, Toseland R, Rizzo V, Zinoman M. Telephone caregiver support groups. Journal of Gerontological Social Work 2004; 44(1/2): 151-172.
26. Colvin J, Chenoweth L, Bold M, Harding C. Caregivers of older adults: advantages and disadvantages of internet-based social support. Family Matters 2004; 53(1): 49-57.
27. Tedman-Jones J, Knox M, Buys L. 'Just hanging on': the experiences of older carers of a family member with chronic mental illness. In: Proceedings, Social Change in the 21st Century Conference; 21 November 2003; Queensland University of Technology. 2003.
28. Smith S, Bell P. Examining the effectiveness of the Savvy Caregiver Program among rural Colorado residents. Rural and Remote Health 5:466. (Online) 2005. Available: www.rrh.org.au (Accessed 20 September 2009).
29. Edwards B, Gray M, Baxter J, Hunter B. The tyranny of distance? Carers in regional and remote areas of Australia. Canberra, ACT: Australian Institute of Family Studies, 2009.
30. Lucke J, Russell A, Tooth L, Lee C, Watson M, Byrne G et al. Few urban-rural differences in older carers' access to community services. Australian Health Review 2008; 32(4): 684-690.
31. Russell R. Social networks among elderly men caregivers. Journal of Men's Studies 2004; 13(1): 121-142.
32. Hansen E, Robinson A, Mudge P, Crack G. Barriers to the provision of care for people with dementia and their carers in a rural community. Australian Journal of Primary Health 2005; 11(1): 72-79.
33. Morgan D, Semchuk K, Stewart N, D'Arcy P. Rural families caring for a relative with dementia: barriers to use of formal services. Social Science & Medicine 2002; 55: 1129-1142.
34. Glueckauf R, Stine C, Bourgeois M, Pomidor A, Rom P, Young M et al. Alzheimer's Rural Care Healthline: linking rural caregivers to cognitive-behavioural intervention for depression. Rehabilitation Psychology 2005; 50(4): 346-354.
35. Blackstock K, Innes A, Cox C, Smith A, Mason A. Living with dementia in rural and remote Scotland: diverse experiences of people with dementia and their carers. Journal of Rural Studies 2006; 22: 161-176.
36. Bruen W, Howe A. Respite care for people living with dementia: "It's more than just a short break". Canberra, ACT: Alzheimer's Australia, 2009.
37. Hill K, Smith R, Fearn M, Rydberg M, Oliphant R. Physical and psychological outcomes of a supported physical activity program for older carers. Journal of Aging and Physical Activity 2007; 15: 257-271.
38. Smith D. CADS: Carer and Depression Support Group. Australian Journal of Primary Health 2006; 12(3): 9-11.
39. Hayman F. Helping carers care: an education programme for rural carers of people with a mental illness. Australasian Psychiatry 2005; 13(2): 148-152.
40. Minnema N. A cuppa in the country. Journal of Dementia Care 2008; 16(6): 20-21.
41. Hayes J. Respite for caregivers: a community based model in a rural setting. Journal of Gerontological Nursing 1999; 25(1): 22-26.
42. Hancock P, Jarvis J, L'Veena T. Older carers in ageing societies: an evaluation of a respite program for older carers in Western Australia. Home Health Care Services Quarterly 2007; 26(2): 59-84.
43. Cameron J. Who will look after her when I die? Report on the Ageing Carers of People with a Disability Project. Melbourne, VIC: Carers Victoria, 2005.
44. Bailey J, Moriarty J. Alzheimer's Society Derby Branch: a comprehensive programme of support for people with dementia and their carers. Dementia 2006; 5(2): 293-296.
45. Charlesworth G, Tzimoula X, Higgs P, Poland F. Social networks, befriending and support for family carers of people with dementia. Quality in Ageing 2007; 8(2): 37-44.
46. Shanley C. Supporting family carers through telephone-mediated group programs: opportunities for gerontological social workers. Journal of Gerontological Social Work 2008; 51(3/4): 199-209.
47. Paul L, Johnson A, Cranston G. A successful videoconference satellite program: providing nutritional information on dementia to rural caregivers. Educational Gerontology 2000; 26: 415-425.
48. Marziali E, Donahue P, Crossin G. Caring for others: internet health care support intervention for family caregivers of persons with Alzheimer's, stroke or Parkinson's disease. Families in Society 2005; 86: 375-383.
49. Buckwalter K, Davis L, Wakefield B, Kienzle M, Murray M. Telehealth for elders and their caregivers in rural communities. Family and Community Health 2002; 25(3): 31-40.
50. Dollinger S, Chwalisz K, Zerth E. Tele-Help Line for Caregivers (TLC): a comprehensive telehealth intervention for rural family caregivers. Clinical Gerontologist 2006; 30(2): 51-64.
51. Hartke R, King R. Telephone group intervention for older stroke caregivers. Topics in Stroke Rehabilitation 2003; 9(4): 65-81.
52. Larkin M. Group support during caring and post caring: the role of carers groups. Groupwork 2007; 17(2): 28-51.
53. Magnusson L, Hanson E, Nolan M. The impact of information and communication technology on family carers of older people and professionals in Sweden. Ageing & Society 2005; 25: 693-713.
54. Williams P, Grenade L. Meeting the challenge: a national approach to supporting people with dementia and their carers. Asia Pacific Journal of Health Management 2008; 3(1): 51-57.
55. Droes R, Meiland F, De Lange J, Vernooil-Dassen M, Van Tilberg W. The Meeting Centres Support Programme: an effective way of supporting people with dementia who live at home and their carers. Dementia 2003; 2(3): 426-433.
56. King S, Bellamy J. Who is caring for the carers? Sydney, NSW: Anglicare; 2008.
57. Brodaty H, Low L. Making Memories: pilot evaluation of a new program for people with dementia and their caregivers. Australasian Journal on Ageing 2004; 23(3): 144-146.
58. Capus J. The Kingston Dementia Cafe: the benefits of establishing an Alzheimer cafe for carers and people with dementia. Dementia 2005; 4(4): 588-591.
59. Mather L. Memory Lane Cafe: follow-up support for people with early stage dementia and their families and carers. Dementia 2006; 5(2): 290-293.
60. Toseland R, McCallion P, Smith T, Banks S. Supporting caregivers of frail older adults in an HMO setting. American Journal of Orthopsychiatry 2004; 74(3): 349-364.
61. Gal, lagher-Thompson D, Lovett S, Rose J, McKibbin C, Coon D, Futterman A et al. Impact of psychoeducational interventions on distressed family caregivers. Journal of Clinical Geropsychology 2000; 6(2): 91-110.
<, a, , , href='#ref62_cite141' name='cite_note-62'>62. Van Ast P, Larson A. Supporting rural carers through telehealth. Rural and Remote Health 7:623. (Online) 2007. Available: www.rrh.org.au (Accessed 15 September 2009).
63. Van Ast P. Supporting community carers via teleconferencing. Journal of Telemedicine and Telecare 2005; 11(2): 96-97.
64. Ducharme F, Levesque L, Giroux F, Lachance L. Follow-up of an intervention program for caregivers of a relative with dementia living in a long term care setting: are there any persistent and delayed effects? Aging & Mental Health 2005; 9(5): 461-469.
65. Pierce L, Steiner V, Govoni A, Hicks B, Thompson T, Friedemann M. Internet-based support for rural caregivers of persons with stroke shows promise. Rehabilitation Nursing 2004; 29(3): 95-103.
66. Bank A, Arguelles S, Rubert M, Eisdorfer C, Czaja S. The value of telephone support groups among ethnically diverse caregivers of persons with dementia. The Gerontologist 2006; 46(1): 134-138.
67. Pierce L, Steiner V, Govoni A, Hicks B, Thompson T, Friedemann M. Caregivers dealing with stroke pull together and feel connected. Journal of Neuroscience Nursing 2004b; 36(1): 32-39.
68. Golden M, Lund D. Identifying themes regarding the benefits and limitations of caregiver support group conversations. Journal of Gerontological Social Work 2009; 52(2): 154-170.
69. Shanley C, Roddy M, Cruysmans B, Eisenberg M. The humble telephone: a medium for running carer support groups. Australasian Journal on Ageing 2004; 23(2): 82-85.
70. Warmington R. Family carers' health and well being and community building capacity in rural areas. In: Proceedings, 7th National Rural Health Conference; 1-4 March 2003; Hobart, Tasmania, Australia. 2003.
71. Glueckauf R, Jeffers S, Sharma D, Massey A, Davis W, Wesley L et al. Telephone-based cognitive-behavioural intervention for distressed rural dementia caregivers. Clinical Gerontologist 2007; 31(1): 21-41.
72. Mental Health Council of Australia. Carers of People with Mental Illness Project: Final Report: Mental Health Council of Australia/Carers Association of Australia, 2000.
73. Baldwin C, Mackenzie J. Service needs and delivery following dementia diagnosis: evidence based review. Bradford: Bradford Dementia Group/Commission for Rural Communities, 2008.
74. Tompkins S, Bell P. Examination of a psychoeducational intervention and a respite grant in relieving psychosocial stressors associated with being an Alzheimer's caregiver. Journal of Gerontological Social Work 2009; 52: 89-104.
75. Tommis Y, Seddon B, Woods B, Robinson C, Reeves C, Russell I. Rural-urban differences in the effects on mental well-being of caring for people with stroke or dementia. Aging & Mental Health 2007; 11(6): 743-750.
76. Australian Government. Towards a National Carer Strategy: a discussion paper from the Australian Government. Canberra, ACT: Australian Government; 2010.

