Dental decay (caries) is a widespread disease among Aboriginal communities and it has a particularly severe impact on children and their wellbeing1,2. For example, decayed and painful teeth greatly inhibit an ability to eat healthy foods, directly influencing nutrition and ultimately systemic health. Recent general health examinations conducted by medical and nursing personnel in the Northern Territory found oral health problems to be the most common condition affecting Aboriginal children, with 43% of those examined having caries3.
In young children, due to the thin layer of enamel on primary teeth, dental caries can progress more quickly than in adult teeth, causing severe pain, destruction of the dentition, and systemic infection. Often the only treatment possible is multiple extractions under general anaesthesia in hospital or a day-stay unit4-6. Such a situation is of great concern, given the limited availability of resources, including dental personnel, in many Aboriginal communities.
In recognition of the extent and severity of this disease, its high hospitalisation rates and its impact on childhood nutrition, socialisation and schooling, the control of dental caries has been identified as a key indicator in the reduction of Aboriginal disadvantage7. Yet the oral health of Aboriginal children is worsening rather than improving under current approaches. This group has twice the level of dental caries in both their primary and permanent teeth compared with their non-Aboriginal counterparts, as well as higher levels of untreated decay8. Many Aboriginal communities face this burden of oral disease with very limited or no access to dental services, and current workforce statistics indicate that most dentists work in private practices that are based in the major cities9. Few Aboriginal controlled community health services are funded to provide dental care and those that do have great difficulty in attracting and retaining dental professionals, particularly in rural and remote communities.
The purpose of this review was to collate published material to provide readers with a single publication that describes the prevalence and experience of dental caries, and more importantly, that documents the disparity in dental caries experience between Aboriginal and non-Aboriginal Australian children, by state and over time. It is anticipated that such a resource will provide useful information for evidence-based program planning and policy-making in Aboriginal oral health.
Medline was the primary database used in the literature search. Other databases included: PubMed, Web of Science, and Google Scholar. Articles were also retrieved using the 'similar articles' feature in PubMed and via cascading the references of reviewed articles. National and State department of health websites were also searched for relevant publications. In Medline, articles were retrieved using the MeSH terms* and keywords: prevalence*, dental caries*, oral health*, prevention and control*, child*, adolescent*, population groups*, Aboriginal and Indigenous. In the initial selection phase 1811 article abstracts were screened and included if they reported oral health information for Australian Aboriginal children. Following this screening process, 73 full-length articles were retrieved and the inclusion and exclusion criteria were applied. Articles were included in the review if they reported information on either caries prevalence rates or experience scores. Articles were excluded if the study sample was special needs children, or caries statistics were reported only for children over 12 years of age. This led to 15 articles being included for the review.
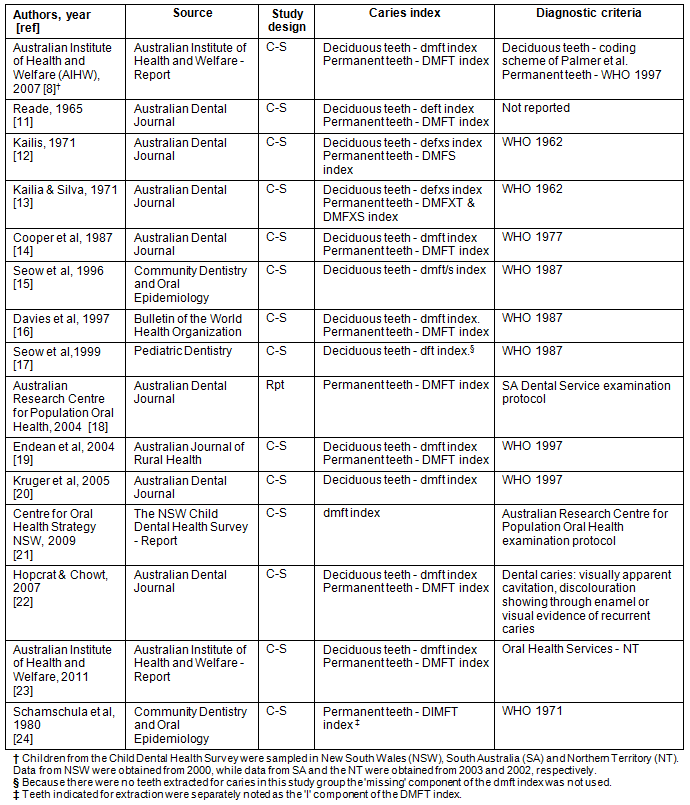
Information is provided on the selected study characteristics (Table 1). Data were extracted for children up to 18 years of age; however, for comparative purposes across studies, the main focus is on the WHO benchmark ages of 5-6 years for the primary dentition, and 12-year-olds for the permanent dentition10. Information on caries statistics for non-Aboriginal children was also obtained and matched by age, location and time.
Table 1: Study characteristics8,11-24
Primary dentition
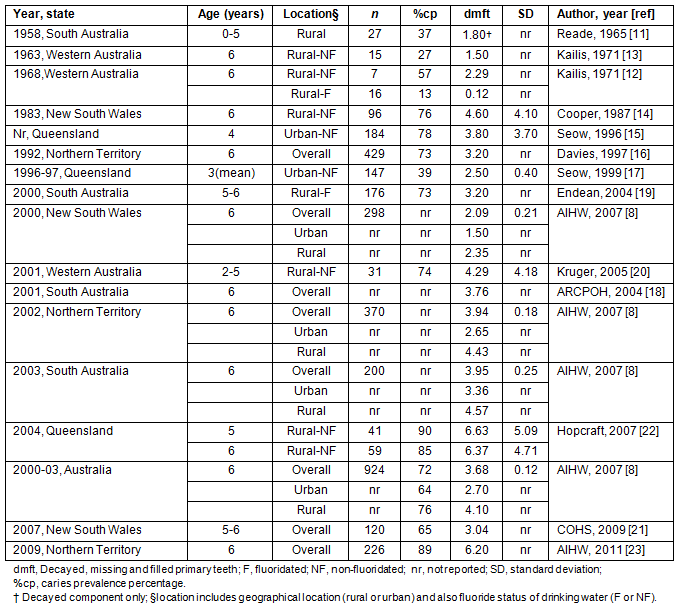
Caries statistics for the primary dentition of Australian Aboriginal children aged 2 to 6 years are given8,11-23 (Table 2), organized chronologically according to year of data collection and geographical location.
It was observed that there were very low caries prevalence (13%) and experience (0.12) among 6-year-old Aboriginal children living in rural fluoridated Western Australia in 196812. Since that time, it appears that caries rates have increased considerably. For example, caries prevalence among 6-year-olds in rural non-fluoridated Western Australia in 1963 was 27% with a mean dmft (decayed, missing and filled primary teeth) of 2.07, and in 2004 was 85% among 6-year-olds (dmft=6.37) in rural non-fluoridated Queensland13,22.
A report by the Australian Institute of Health and Welfare gave national pooled caries estimates for 6-year-old Aboriginal children (caries prevalence=72%, mean dmft score=3.68). This report also highlighted an urban-rural disparity in caries statistics, with rural Aboriginal children having the poorer oral health. Such a trend was observed within and across States8.
Queensland and the Northern Territory had the highest levels of dental caries. Ninety precent of 5-year-old Aboriginal children in rural Queensland had dental caries (dmft = 6.63, SD=5.09)22. In the Northern Territory in 2009, a similar proportion of 6-year-olds had caries and a mean dmft score of 6.2023. This is a 57% increase from 2002 when the mean dmft score was 3.94 (SE=0.18). In, New South Wales (NSW), a 45% increase in caries experience was observed, among 5-6-year-olds, between 2000 and 2007 (dmft scores of 2.09 and 3.04, respectively)8,21.
Table 2: Caries prevalence percentage and experience (dmft) in the primary dentition
of Australian Aboriginal children by year of data collection and State8,11-23
Permanent dentition
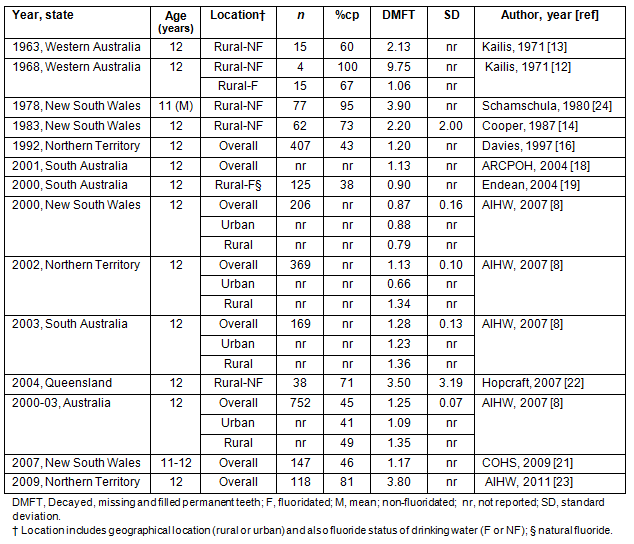
The caries statistics for the permanent dentition of Aboriginal children aged 11 to 12 years are presented8,12-14,16,18,19,21-24 (Table 3). Caries prevalence rates were observed to have decreased over time, while the experience rates (DMFT, Decayed, Missing and Filled Permanent Teeth) have remained largely constant at approximately 1.00. The 2007 AIHW report on oral health of Aboriginal children, reported a national caries prevalence of 45% and mean DMFT score of 1.25 (SE=0.07). However, Queensland and the Northern Territory had relatively higher caries prevalence and experience rates. In the Northern Territory, a 236% increase in caries experience was observed between 2002 (mean DMFT=1.13) and 2009 (mean DMFT=3.80)8,23. In 2007, data from Queensland showed a caries prevalence of 71% and mean DMFT score of 3.50. In NSW, mean DMFT scores decreased between 1978 and 2000, from 3.90 to 0.87. However, since 2000 a 34% increase in caries experience was observed in NSW with a mean DMFT score of 1.17 recorded in 20078,21.
Urban-rural differences in caries experience were similar to the primary dentition, where rural children experienced considerably more dental caries. The exception was NSW, where urban 12-year-olds had a mean DMFT score of 0.88, compared with 0.79 for their rural counterparts8.
Table 3: Caries prevalence percentage and experience (DMFT) in the permanent dentition
of Australian Aboriginal children by year of data collection and State8,12-14,16,18,19,21-24
Dental caries disparities
Caries statistics were compared between Australian Aboriginal and non-Aboriginal children, by time and State8,13-22,24-28 (Tables 4 & 5). In 1963, more non-Aboriginal 6- and 12-year-olds had dental caries compared with their Aboriginal counterparts. Since then the situation has reversed.
Over time, caries prevalence estimates for young Aboriginal children (Table 4) have either not changed or increased. However, a decrease was observed among non-Aboriginal children. A similar pattern was observed for caries experience (dmft), with scores remaining relatively unchanged or increasing over time for Aboriginal children. The relative difference in dmft scores between Aboriginal and non-Aboriginal 6-year-olds (matched for location and time) was relatively unchanged between 1983 and 2007, with Aboriginal children having approximately double the caries experience of non-Aboriginal children. National estimates for primary dentition show that during the 2000-2003 period 72% of Aboriginal children aged 6 years had dental caries, whereas this figure was only 37% for non-Aboriginal children, the difference being 35 percentage points. In terms of caries experience, Aboriginal 6-year-olds had a mean dmft score of 3.68 which was 2.38 times higher than that for non-Aboriginal children (dmft=1.54).
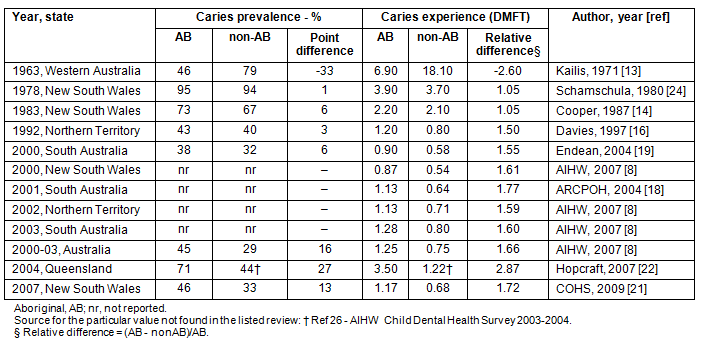
There was a major decrease in mean DMFT scores for non-Aboriginal 12-year-olds (Table 5) from 18.10 in 1963 to 0.75 in 2000-038,13. Twelve-year-old Aboriginal children residing in Queensland were observed to have a three-fold higher (relative difference=2.87) caries experience (DMFT=3.50) compared with their non-Aboriginal counterparts (DMFT=1.22)22. The 2000-2003 national estimates of caries experience (DMFT) for Aboriginal 12-year-olds was 1.25, and for their non-Aboriginal counterparts it was 0.75, with the relative difference indicating 1.66 times higher caries experience in Aboriginal children8. However, this magnitude of disparity was not as large as that observed for the primary dentition. Caries prevalence rates in 2000-2003 for Aboriginal and non-Aboriginal 12-year-olds were 45% and 29%, respectively; a 16 percentage point difference.
Table 4: Comparison of primary dentition (6-year-old) caries
statistics between Aboriginal and non- Aboriginal children8,13-18,21-26
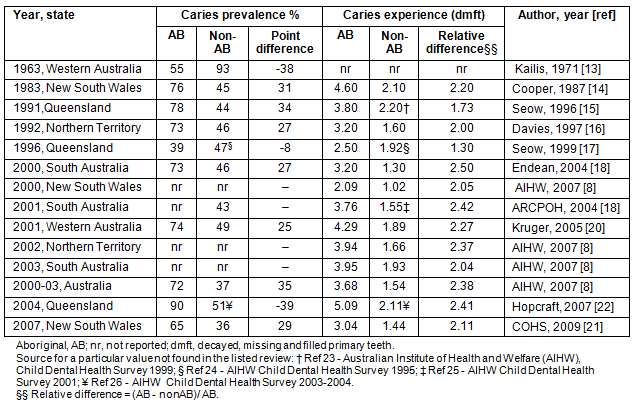
Table 5: Comparison of permanent dentition (12-year-old) caries
statistics between Aboriginal and non- Aboriginal children8,13,14,16,18,19,21,22,24,26
Discussion
This literature review collates published evidence on caries prevalence and experience rates in the Australian Aboriginal child population. The main points emerging from this review on the distribution of caries prevalence and experience in Australian Aboriginal children are:
- consistent inequality, over time and location, in caries rates between Aboriginal and non-Aboriginal children
- geographical (urban-rural) variation in caries rates
- a higher prevalence and more severe caries in young children.
The European colonization of Australia had severe negative effects on the Indigenous population and was characterised by dispossession, physical ill-treatment, social disruption, population decline, economic exploitation, codified discrimination, and cultural devastation. The consequences of these actions, which were in part the product of misguided and discriminatory laws, have resulted in today's Aboriginal communities being the most disadvantaged by all measures of healthy living29. An example of this disadvantage is the well-documented fact that Aboriginal people continue to experience worse health outcomes than their non-Aboriginal counterparts30.
Historically, Aboriginal communities had very little dental caries11. However, it is clear from this review that, at present, dental caries is a major health problem among Aboriginal children, particularly in the primary dentition. The global decline in caries rates since the 1960s has not yet reached the Aboriginal community, resulting in dental health inequalities31,32. No single factor can be identified as the reason for this; instead, it is more likely to be explained by a complex interaction of factors such as: as social isolation; cultural perceptions of oral health; misguided policy; lack of access to health services; inadequate education; remote location; inadequate housing and living conditions; no access to fluoride; and exposure to a Westernised diet33.
Potential reasons for urban Aboriginal children having better caries rates than their rural counterparts include: access to fluoridated water; access to and timely dental visits; supportive school dental services; better education systems and social support networks; and better environmental conditions.
As expected, higher caries rates were reported in the primary dentition of Aboriginal children. A reason for this is because primary teeth are made up of thinner dental tissue so the disease progresses more aggressively. Other reasons include: young children being dependent on others for their oral hygiene needs, and healthy behaviour development. This reality coupled with other risk factors such as diet, socioeconomic situation, environment and health behaviour, make Aboriginal children a high risk group. It also highlights the general lack of effective oral health interventions targeted to this group.
A recent comprehensive oral health intervention study among Aboriginal children aged 18-47 months in the Northern Territory, Australia, tested the effect of a community-oriented primary healthcare intervention on dental caries and oral health behaviours. The intervention included fluoride varnish applications, training of primary-care workers, and oral health promotion at the individual, family and community levels. The study reported a significant decrease in the primary outcome of dental caries but not the secondary outcomes of health behaviour change or community health promotion34,35. A possible reason for the lack of behaviour change in this population is the deeply embedded and overwhelming disadvantage that is experienced on a daily basis. The Aboriginal way of life was altered by the negative influence of the social, political and economic environment that existed during the first two centuries of colonisation. As such environments were the outcome of misguided politics they are amendable to change. The Commission on the Social Determinants of Health identified these upstream factors (social norms, policies and practices) as the main drivers of health inequality36.
It is apparent from this review, that studies on dental caries rates in Australian Aboriginal children are relatively few, with small sample sizes and limited national representation. Caries experience also varied widely within the samples examined, as is shown by the large standard deviations in dmft/DMFT rates. This suggests that some of the children had very high levels of dental caries when compared with the rest of the sample. These findings highlight the need for new and well-planned epidemiological studies which could provide reliable and valid statistics. Apart from these issues, a major factor that made interpretation complex and reduced the comparability and generalizability, was the variation in the research methodology and diagnostic criteria across studies.
Interventions to close the increasing gap in oral health inequalities needs to be evidence based, culturally competent, community based, focused on upstream influences (those at the community or population level rather than individual level), and involve key stakeholders such as the government and local communities. Oral health inequality is a complex issue affected by an interaction of social, behavioural, political, economic, cultural and biologic systems. To better understand this area, future analysis will require a systems approach, which integrates individual systems or functioning units into the larger complex hierarchical system with all interacting forces that influence action to produce real-world outcomes37. However, it is important to reflect on the factors which greatly reduced the dental caries levels of non-Aboriginal children. In part this can be attributed to the community water fluoridation programs and the widespread use of fluoride toothpaste. While this is only part of the picture, it does offer a preventive strategy which can be implemented quickly in many Aboriginal communities.
Both caries prevalence and experience are evidently higher in the primary dentition. Rural Queensland and the Northern Territory have much higher caries rates among both 6- and 12-year-olds. Rural Aboriginal children are generally at a disadvantage compared with their urban counterparts. The magnitude of disparity in caries rates between Aboriginal and non-Aboriginal Australian children appears to be relatively unchanged over time, with an indication that it is increasing. This raises the issue of health inequity and the need to fund practical, culturally appropriate and sustainable preventive programs.
Acknowledgment
The authors thank Dr Rahila Ummer Christian for her assistance in data extraction, preparation of the tables and commenting on the manuscript.
References
1. Sheiham A. Dental caries affects body weight, growth and quality of life in pre-school children. British Dental Journal 2006; 201(10): 625-626.
2. Filstrup SL, Briskie D, da Fonseca M, Lawrence L, Wandera A, Inglehart MR. Early childhood caries and quality of life: child and parent perspectives. Pediatric Dentistry 2003; 25(5): 431-440.
3. Australian Institute of Health and Welfare and Department of Health and Ageing. Progress of the Northern Territory Emergency Response child Health check Initiative:update on results from the Child Health Check and follow-up data collections. Cat no IHW28. Canberra, ACT: AIHW, 2009.
4. Tennant M, Namjoshi D, Silva D, Codde J. Oral health and hospitalization in Western Australian children. Australian Dental Journal 2000; 45(3): 204-207.
5. Kruger E, Dyson K, Tennant M. Hospitalization of Western Australian children for oral health related conditions: a 5-8 year follow-up. Australian Dental Journal 2006; 51(3): 231-236.
6. Jamieson LM, Roberts-Thomson KF. Dental general anaesthetic trends among Australian children. BMC Oral Health 2006; 6: 16.
7. Steering Committee for the Review of Government Service Provision. Overcoming Indigenous Disadvantage: Key Indicators 2009. Canberra, ACT: Productivity Commission, 2009.
8. Australian Institute of Health and Welfare, Dental Statistics and Research Unit. Oral health of Aboriginal and Torres Strait Islander children. Dental Statistics and Research Series AIHW cat no DEN167. Canberra, ACT: AIHW, 2007.
9. Chrisopoulos S, Nguyen T. Trends in the Australian dental labour force, 2000 to 2009: Dental labour force collection, 2009. Dental Statistics and Research Series no. 61. Canberra, ACT: AIHW, 2012.
10. World Health Organization. Oral health surveys - basic methods. Geneva: World Health Organization, 1997.
11. Reade PC. Dental observations on Australian aborigines, Koonibba, South Australia. Australian Dental Journal 1965; 10(5): 361-370.
12. Kailis DG. Dental conditions observed in Australian aboriginal children resident in Warburton and Cundeelee missions, Western Australia (August, 1968). Australian Dental Journal 1971; 16(1): 44-52.
13. Kailis DG, Silva DG. Prevalence of dental caries in Australian aboriginal children resident in Carnarvon, Western Australia. Australian Dental Journal 1971; 16(2): 109-115.
14. Cooper MH, Schamschula RG, Craig GG. Caries experience of aboriginal children in the Orana region of New South Wales. Australian Dental Journal 1987; 32(4): 292-294.
15. Seow WK, Amaratunge A, Bennett R, Bronsch D, Lai PY. Dental health of aboriginal pre-school children in Brisbane, Australia. Community Dentistry and Oral Epidemiology 1996; 24(3): 187-190.
16. Davies MJ, Spencer AJ, Westwater A, Simmons B. Dental caries among Australian Aboriginal, non-Aboriginal Australian-born, and overseas-born children. Bulletin of the World Health Organization 1997; 75(3): 197-203.
17. Seow WK, Amaratunge A, Sim R, Wan A. Prevalence of caries in urban Australian aborigines aged 1-3.5 years. Pediatric Dentistry 1999; 21(2): 91-96.
18. Australian Centre for Population Oral Health. Oral Health of Aboriginal Australians. Australian Dental Journal 2004; 49(3): 151-153.
19. Endean C, Roberts-Thomson K, Wooley S. Anangu oral health: the status of the Indigenous population of the Anangu Pitjantjatjara lands. Australian Journal of Rural Health 2004; 12(3): 99-103.
20. Kruger E, Dyson K, Tennant M. Pre-school child oral health in rural Western Australia. Australian Dental Journal 2005; 50(4): 258-262.
21. Centre for Oral Health Strategy NSW. The New South Wales Child Dental Health Survey 2007. Sydney, NSW: NSW Department of Health, 2009.
22. Hopcraft M, Chowt W. Dental caries experience in Aboriginal and Torres Strait Islanders in the Northern Peninsula Area, Queensland. Australian Dental Journal 2007; 52(4): 300-304.
23. Australian Institute of Health and Welfare. Dental health of Indigenous children in the Northern Territory: findings from the Closing the Gap Program. Cat no IHW41. Canberra, ACT: AIHW, 2011.
24. Schamschula RG, Cooper MH, Adkins BL, Barmes DE, Agus HM. Oral conditions in Australian children of Aboriginal and Caucasian descent. Community Dentistry and Oral Epidemiology 1980; 8(7): 365-369.
25. Australian Institute of Health and Welfare Dental Statistics and Research Unit. The Child Dental Health Survey, Australia 1999: Trends across the 1990s. Cat no DEN 95. Adelaide, SA: University of Adelaide, 2003.
26. Australian Institute of Health and Welfare Dental Statistics and Research Unit. The Child Dental Health Survey, Australia 1995. Adelaide, SA: University of Adelaide, 1997.
27. Australian Institute of Health and Welfare Dental Statistics and Research Unit. Socioeconomic differences in children's dental health: The Child Dental Health Survey, Australia 2001. Cat no DEN152. Canberra, ACT: AIHW, 2006.
28. Australian Institute of Health and Welfare Dental Statistics and Research Unit. Dental health of Australia's teenagers and pre-teen children: the child dental health survey, Australia 2003-04. Cat no DEN199. Canberra, ACT: AIHW, 2009.
29. Gardiner-Garden J. From dispossession to reconciliation. Research paper no 27, 1998-99. Canberra, ACT: Department of the Parliamentary Library - Information and Research Services, 1999.
30. Australian Institute of Health and Welfare. The health and welfare of Australia's Aboriginal and Torres Strait Islander people, an overview 2011. Cat no IHW42. Canberra, ACT: AIHW, 2011.
31. Carr LM. Dental health of children in Australia 1977-1980. Australian Dental Journal 1982; 27(3): 169-175.
32. Burt BA. The future of the caries decline. Journal of Public Health Dentistry 1985; 45(4): 261-269.
33. Gracey M. Historical, cultural, political, and social influences on dietary patterns and nutrition in Australian Aboriginal children. American Journal of Clinical Nutrition 2000; 72(5Suppl): 1361S-1367S.
34. Roberts-Thomson KF, Slade GD, Bailie RS, Endean C, Simmons B, Leach AJ et al. A comprehensive approach to health promotion for the reduction of dental caries in remote Indigenous Australian children: a clustered randomised controlled trial. International Dental Journal 2010; 60(3Suppl2): 245-249.
35. Slade GD, Bailie RS, Roberts-Thomson K, Leach AJ, Raye I, Endean C et al. Effect of health promotion and fluoride varnish on dental caries among Australian Aboriginal children: results from a community-randomized controlled trial. Community Dentistry and Oral Epidemiology 2011; 39(1): 29-43.
36. Commission on the Social Determinants of Health. Closing the gap in a generation: health equity through action on the social determinants of health. Geneva: World Health Organization, 2008.
37. Chattopadhyay A. Systems Thinking. Oral Health Epidemiology Principles and Practice. Boston, MA: Jones and Bartlett, 2010; 383-392.
Correction: A correction was made to the reference citations in Table 1 on 11 February 2013.

