Beginnings
The Rural Undergraduate Support and Coordination (RUSC) program (1997-2011) developed rural clinical placements for Australian medical students to provide an inspiration for future rural work. In the late 1990s the University of Adelaide, South Australia, had a large enrolment of Malaysian students sponsored by their government and bonded to return to their national health service. The challenges for these Malaysian graduates of working in tropical rural settings prompted the introduction of an International Health (IH) course, which included 'tropical medicine'. An initial course was developed in 1998 by RUSC academics Drs Owen Lewis and Jonathan Newbury, in the then Department of General Practice. Course content included disease-specific topics, public health, Indigenous health worker training and consideration of philosophical and religious issues.
The IH course was first delivered as a 2 week option in the 6th year mid-year break in 1999. It contained a series of short lectures and problem-based learning sessions with a short-answer examination on the final day. The IH course has evolved since 1999 and continues to be delivered every year.
Developing world electives
The University of Adelaide, like many other medical schools, has encouraged senior students to undertake international electives. The emerging risk of HIV in South Africa first prompted pre-departure planning1. A North American evaluation of developing world elective experience revealed positive and negative effects:
- limited usefulness to the community of short-term placements
- lack of education goals compared with other parts of the students' curriculum
- a failure to address community needs
- unexpected ethical dilemmas emerging
- the emergence of the disparaging term 'medical tourism'2.
Such effects may harm the student and their host community and precipitated the need for pre-departure courses2 to mitigate negative effects and facilitate self-reflection after the experience.
Curriculum
The need for a systematic approach to a global health curriculum was acknowledged both in Australia3 and debated in the medical literature4,5. Understanding the breadth of global health included an awareness of recent changes, for example the migration of medical workforce and the threat of pandemic influenza A H1N14 led to development of standard curriculum frameworks6 and persistent calls for global health to be incorporated in all medical curricula5,7. Despite this impetus, medical schools vary widely in what is offered as IH curriculum and, indeed, even accepting IH as a necessary part of their medical curriculum4.
University of Adelaide course
Initial evaluation of the University of Adelaide course content and the number of students enrolled demonstrated the perceived value of the course and ensured its place in the MBBS curriculum. When Dr Lewis returned to Nepal in 2003, Dr Gillian Laven joined as course coordinator and IH was expanded to 3 weeks, offered to 4th, 5th and 6th year medical students and repeated twice a year. The name of the course was changed to International Primary Health Care (IPHC) to reflect the focus on primary health care, including preventive care and the prevalence of 'chronic conditions of the industrialised world' in the developing world7,8.
Course content
The aim of IPHC is to provide students with a greater understanding of the social determinants of health. These include health issues related to poverty, powerlessness, lack of access to resources and health education - concepts that are equally relevant in Australian rural and remote locations and the developing world. The IPHC course is provided as a 'pre-departure training course'2 for students intending to work in Indigenous communities in Australia and internationally. However, there is value in all students understanding these concepts, even if their career will be in urban locations, providing peripatetic service to remote communities or refugee populations, or to returning travellers7.
The course seminars are designed to be interactive rather than traditionally didactic, to provide knowledge about developing world health issues, and strategies for relieving the health burden experienced by individuals and communities. Where possible the structure is progressive:
- from foundation seminars in the first week (eg Global Review of Major Causes of Health & Illness, and Child Health)
- followed by disease principles (eg TB, HIV and Malaria) in the second week
- to final week application of knowledge gained (eg Royal Flying Doctor Service, Refugee Health, Travel Medicine and Vicarious Trauma).
Australian community examples include Indigenous communities throughout urban and rural Australia and immigrant and refugee communities. In the period 2008-2009, 171 000 migrants entered Australia under the skilled and family streams of Australia's migration program, a further 670 000 arrived for specific work, business, entertainment, sporting, holiday or study on temporary visas. A smaller number (13 507) entered on humanitarian grounds9.
The use of presenters who are currently practising in IH makes the course relevant and authoritative. However, the logical sequence and flow of the seminars is often difficult to maintain due to the inclusion of presenters whose work takes them to rural areas in Australia and internationally.
Currently this progressive learning IPHC course covers the 3 competency domains recommended by the American Society for Tropical Medicine and Hygiene Committee on Medical Education7:
- Burden of global disease
- Travellers medicine
- Immigrant health.
Importantly, the course has a total of 40 contact hours over 3 weeks, which exceeds the Society's recommended student exposure to global health7.
In 2009, oral health was added to the IPHC curriculum because a 2008 examination of the medical curriculum found that medical students were exposed to only 2 hours of oral health. It was determined that graduating MBBS students need to understand the burden of oral disease, to be able to differentiate between deciduous and permanent dentition and between an ulcer and oral carcinoma10.
Educational assessment
All students participate in a group exercise to design and present a development program proposal (an intervention). The course provides students with an understanding of the complex inter-related problems in a community as they are guided through the process of gathering, sorting and organising information and selecting a focal community problem to address. The groups then develop a strategy to address the focal problem that includes lower level activities that contribute to higher level objectives. The proposals include the logical framework (outlining the program's strategy), a narrative outline of the program's background, rationale and implementation, and a budget. These development program proposals are prepared in both oral and on-line (Wiki) formats and presented to two academics who provide constructive feedback and assess the proposal according to pre-determined criteria.
Course evaluation was designed to understand why students selected the IPHC course. For although the IPHC course was designed to be a pre-vocational course for international students, it has also become a pre-departure course for domestic students, and not always those in their final year.
Medical students at all Australian medical schools are required by RUSC agreements to undertake a minimum of 4 weeks in an Australian rural or remote area. Students are also encouraged and supported to undertake an international placement. Although approximately two-thirds of IPHC students are in their final (6th) year, the remainder of students are spread across 4th and 5th year.
The evaluations have revealed that undertaking IPHC supports students because it:
[provides the] opportunity to learn about diseases specific to 3rd world medicine. To gain an idea of the type of work I could do in the developing world in the future.
...addresses many issues of healthcare that
should be covered[sic] are not covered in the standard curriculum. In my opinion, IPHC should be made compulsory in [sic] as a 3-week component in 4th year.
Student statements such as these support 'global health' being a core component in medical education4; however, the debate continues on what constitutes appropriate global health training for medical students.
It is acknowledged that some students select IPHC for reasons other than interest or for vocational or placement preparation:
Initially, I chose IPHC because of the predictable hours and doing something different - instead of general practice. Now, it has turned out to be one of the best rotations in my clinical years - I think is essential and should be incorporated into the core curriculum.
At present IPHC or 'global health' is the University of Adelaide option for those who have an 'interest in social justice issues' and those who are 'very passionate about Indigenous & developing world health. Interested in public health'.
And while the majority say it provides 'a greater understanding of public health in different global locations', and is suited to those 'Interested in working in rural/remote/international places', there will always be students who are allocated to it by default. Because without exposure there cannot be change, as educators the course coordinators are satisfied that some students select IPHC simply because 'friends recommended it'.
However some students elect to take IPHC for more informed reasons:
I felt that the public isn't aware of the problems other areas of the world is facing, and the impact they're going to make in a global situation. I want to be the educator to the public and hopefully, be able to make a small difference if possible.
Conclusion
The definition of 'global health' is evolving with more common usage11. Global health includes drawing distinctions from public health, with its roots in tropical and infectious diseases and IH with its emphasis on policy and individual developing world countries, rather than taking a global perspective11. In 2011 the IPHC course was re-named 'Global Health'. However, it still '...encompasses environmental, political, economic and social dynamics and diseases that affect individuals or communities across countries'4. Current presenters (from Africa, Antarctica, Australia, India, Malaysia, Nepal, and Papua New Guinea) continue to provide a multinational focus and emphasise the need for cooperative multidisciplinary solutions (Appendix I). In this way students continue to be prepared whether pre-departure for their international elective, for the care of returning travellers, the health of immigrants and refugees, or simply to gain knowledge about the burden of global disease.
Acknowledgements
Initial advice on course construction was generously given by Professor Anthony Radford who continues to teach in the course when he is available. The authors remain indebted to him. Dr Owen Lewis constructed the first course and delivered most of the teaching until his return to Nepal. The teaching of medical students in rural, remote and international health as described in this report has been supported by the Rural Undergraduate Support and Coordination grants from the Australian Government's Department of Health and Ageing to the University of Adelaide, 1997-2011. The authors are indebted to the large number of clinicians and academics who have presented in the course over a number of years. Ms Marie Dodman (previously) and Ms Yvonne Speir (currently) provide invaluable administrative support. The positive response of the medical students who have selected the course have kept the authors enthused and make it a highlight of their academic year.
References
1. Wilkinson D, Symon B. Medical students, their electives, and HIV. Unprepared, ill advised, and at risk. BMJ 1999; 318: 139-140.
2. Petrosoniak A, McCarthy A, Varpio L. International health electives: thematic results of student and professional interviews. Medical Education 2010; 44(7): 683-689.
3. Australian International Health Institute. Global health in the undergraduate medical curriculum. Occasional Seminar Series. Melbourne, VIC: University of Melbourne, 2003.
4. Brewer TF, Saba N, Clair V. From boutique to basic: a call for standardised medical education in global health. Medical Education 2009; 43(10): 930-933.
5. Drain P, Primack A, Hunt D, Fawzi W, Holmes K, Gardner P. Global health in medical education: a call for more training and opportunities. Academic Medicine 2007; 82(3): 226-230.
6. Rowson M. Global Health Studies. London: Medact, 2001.
7. Houpt E, Pearson R, Hall T. Three domains of competency in global health education: recommendations for all medical students. Academic Medicine 2007; 82(3): 222-225.
8. Oswald N. Doctors for the 21st century:The contribution primary medical care could make. Education for Health 1996; 9(1): 37-44.
9. Australian Government, Department of Immigration and Citizenship. Fact sheet 4 - More than 60 years of post-War migration 2010: (Online) 2010. Available: http://www.immi.gov.au/media/fact-sheets/04fifty.htm#today (Accessed 5 May 2011).
10. Laven G, Newbury J, Burgess V. A taste of oral health in undergraduate medicine. In: Proceedings, 11th National Rural Health Conference; 13-16 March 2011; Perth, WA; 2011.
11. Koplan JP, Bond CT, Merson MH, Reddy SK, Rodriguez MH, Sewankambo NK, et al. Towards a common definition of global health. Lancet 2009; 373: 1993-1995.
____________________
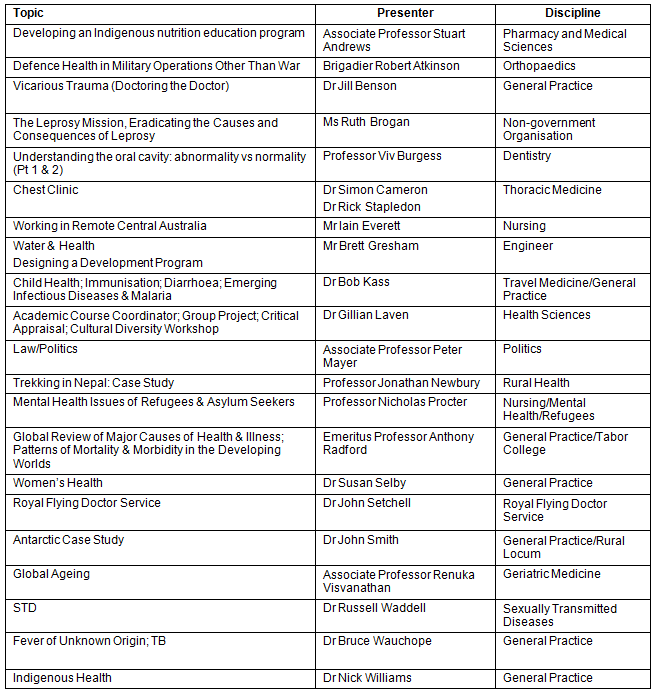
Appendix I: International Primary Health Care course topics, presenters and their health disciplines